Abstract
Purpose
LCZ696 (sacubitril/valsartan), an angiotensin receptor neprilysin inhibitor, is indicated for chronic heart failure (HF) and reduced ejection fraction (HFrEF) to reduce the risk of cardiovascular death and hospitalization for HF. Following oral administration, LCZ696 provides systemic exposure to valsartan and sacubitril (a prodrug), and its metabolite sacubitrilat (the active neprilysin inhibitor, formerly named as LBQ657), which is eliminated primarily via renal route. Since renal dysfunction is a common comorbidity in patients with HF, two open-label studies assessing the effect of mild, moderate, and severe renal impairment were conducted.
Methods
Patients with mild (N = 8; creatinine clearance [CrCl] 50 to ≤80 mL/min), moderate (N = 8; CrCl 30 to <50 mL/min), and severe (N = 6; CrCl <30 mL/min) renal impairment and matching healthy subjects (CrCl >80 mL/min) for each severity group were enrolled to assess the pharmacokinetics of LCZ696 analytes following administration of LCZ696 400 mg once daily (QD) on days 1 and 5.
Results
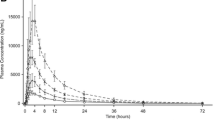
The steady-state Cmax and AUC0–24h of sacubitril and valsartan were unchanged in patients with renal impairment compared with healthy subjects. However, the steady-state Cmax of sacubitrilat was increased by ∼60 % in patients irrespective of degree of renal impairment; half-life increased from 12 h (in healthy subjects) to 21.1, 23.7, and 38.5 h, respectively; and AUC0–24h was increased 2.10-, 2.24-, and 2.70-fold, respectively, in patients with mild, moderate, and severe renal impairment.
Conclusion
Renal dysfunction increases exposure to sacubitrilat while not impacting sacubitril and valsartan exposure. LCZ696 was generally well tolerated in patients with renal impairment.


Similar content being viewed by others
References
Gu J, Noe A, Chandra P, Al-Fayoumi S, Ligueros-Saylan M, Sarangapani R, Maahs S, Ksander G, Rigel DF, Jeng AY, Lin TH, Zheng W, Dole WP (2010) Pharmacokinetics and pharmacodynamics of LCZ696, a novel dual-acting angiotensin receptor-neprilysin inhibitor (ARNi). J Clin Pharmacol 50(4):401–414
Shi J, Wang X, Nguyen J, Wu AH, Bleske BE, Zhu HJ (2016) Sacubitril is selectively activated by carboxylesterase 1 (CES1) in the liver and the activation is affected by CES1 genetic variation. Drug Metab Dispos 44(4):554–559. doi:10.1124/dmd.115.068536
McMurray JJV, Packer M, Desai AS, Gong J, Lefkowitz MP, Rizkala AR, Rouleau JL, Shi VC, Solomon SD, Swedberg K, Zile MR (2014) Angiotensin-neprilysin inhibition versus enalapril in heart failure. N Engl J Med 371(11):993–1004. doi:10.1056/NEJMoa1409077
Ayalasomayajula S, Langenickel T, Chandra P, Wolfson E, Albrecht D, Zhou W, Parasar P, Rajman I, G S (2016) Effect of food on the oral bioavailability of the angiotensin receptor neprilysin inhibitor sacubitril/valsartan (LCZ696) in healthy subjects. Int J Clin Pharmacol Ther (Accepted)
Flarakos J, Du Y, Bedman T, Al-Share Q, Jordaan P, Chandra P, Albrecht D, Wang L, Gu H, Einolf HJ, Huskey SE, Mangold JB (2016) Disposition and metabolism of [C] Sacubitril/Valsartan (formerly LCZ696) an angiotensin receptor neprilysin inhibitor, in healthy subjects. Xenobiotica: 1-15 DOI 10.3109/00498254.2015.1014944
Michel MC, Foster C, Brunner HR, Liu L (2013) A systematic comparison of the properties of clinically used angiotensin II type 1 receptor antagonists. Pharmacol Rev 65(2):809–848. doi:10.1124/pr.112.007278
7 Novartis Entresto™ (sacubitril and valsartan): US pescribing information. 2015. http://www.pharma.us.novartis.com. Accessed 21 Nov 2015.
Brookman LJ, Rolan PE, Benjamin IS, Palmer KR, Wyld PJ, Lloyd P, Flesch G, Waldmeier F, Sioufi A, Mullins F (1997) Pharmacokinetics of valsartan in patients with liver disease. Clin Pharmacol Ther 62(3):272–278. doi:10.1016/S0009-9236(97)90029-1
Waldmeier F, Flesch G, Muller P, Winkler T, Kriemler HP, Buhlmayer P, De Gasparo M (1997) Pharmacokinetics, disposition and biotransformation of [14C]-radiolabelled valsartan in healthy male volunteers after a single oral dose. Xenobiotica 27(1):59–71. doi:10.1080/004982597240767
Cleland JG, Carubelli V, Castiello T, Yassin A, Pellicori P, Antony R (2012) Renal dysfunction in acute and chronic heart failure: prevalence, incidence and prognosis. Heart Fail Rev 17(2):133–149. doi:10.1007/s10741-012-9306-2
Doogue MP, Polasek TM (2011) Drug dosing in renal disease. Clin Biochem Rev 32(2):69–73
Hsiao HL, Langenickel TH, Greeley M, Roberts J, Zhou W, Pal P, Rebello S, Rajman I, Sunkara G (2015) Pharmacokinetic drug–drug interaction assessment between LCZ696, an angiotensin receptor neprilysin inhibitor, and hydrochlorothiazide, amlodipine, or carvedilol. Clin Pharmacol Drug Dev 4(6):407–417. doi:10.1002/cpdd.183
Cockcroft DW, Gault MH (1976) Prediction of creatinine clearance from serum creatinine. Nephron 16(1):31–41
Levey AS, Bosch JP, Lewis JB, Greene T, Rogers N, Roth D (1999) A more accurate method to estimate glomerular filtration rate from serum creatinine: a new prediction equation. Modification of Diet in Renal Disease Study Group. Ann Intern Med 130(6):461–470
Munar MY, Singh H (2007) Drug dosing adjustments in patients with chronic kidney disease. Am Fam Physician 75(10):1487–1496
Prasad P, Mangat S, Choi L, Chen S, Chen B, Bernardo A, Frame D, Sperelakis R, Lau A (1997) Effect of renal function on the pharmacokinetics of valsartan. Clin Drug Invest 13(4):207–214
Ito S, Satoh M, Tamaki Y, Gotou H, Charney A, Okino N, Akahori M, Zhang J (2015) Safety and efficacy of LCZ696, a first-in-class angiotensin receptor neprilysin inhibitor, in Japanese patients with hypertension and renal dysfunction. Hypertens Res 38(4):269–275. doi:10.1038/hr.2015.1
Acknowledgments
The authors would like to thank Dr. Sreedevi Boggarapu (Novartis Healthcare Pvt Ltd, Hyderabad) for providing medical writing support and editorial assistance with this manuscript and for the collation and incorporation of comments from all the authors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Two studies (EudraCT numbers: 2007-005480-96 [study 1] and 2007-005482-36 [study 2]) were conducted in compliance to the ethical principles originated from the Declaration of Helsinki, as well as Good Clinical Practices and applicable local regulatory requirements. The study protocols were approved by the Institutional Review Boards or Independent Ethics Committees including Ärztekammer Nordrhein (Germany) and Ethics Committee of the Clinical Center of Serbia (Serbia) for both the studies, and Ethics Committee under Federal Service on surveillance in healthcare and social development (Russia) for study 2. All the subjects provided written informed consent before enrolment in the study.
Disclosures
SA, TL, JP, DA, PP, IR, and GS are full-time employees of Novartis and eligible to receive Novartis stocks. PC was an employee of Novartis at the time of conduct of this study.
Rights and permissions
About this article
Cite this article
Ayalasomayajula, S.P., Langenickel, T.H., Jordaan, P. et al. Effect of renal function on the pharmacokinetics of LCZ696 (sacubitril/valsartan), an angiotensin receptor neprilysin inhibitor. Eur J Clin Pharmacol 72, 1065–1073 (2016). https://doi.org/10.1007/s00228-016-2072-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-016-2072-7