Abstract
Background
Criteria to assess the appropriateness of prescriptions might serve as a helpful guideline during professional training and in daily practice, with the aim to improve a patient’s pharmacotherapy.
Objective
To create a comprehensive and structured overview of existing tools to assess inappropriate prescribing.
Method
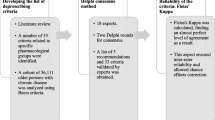
Systematic literature search in Pubmed (1991–2013). The following properties of the tools were extracted and mapped in a structured way: approach (explicit, implicit), development method (consensus technique, expert panel, literature based), focused patient group, health care setting, and covered aspects of inappropriate prescribing.
Results
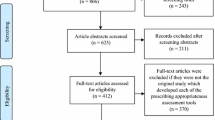
The literature search resulted in 46 tools to assess inappropriate prescribing.Twenty-eight (61%) of 46 tools were explicit, 8 (17%) were implicit and 10 (22%) used a mixed approach. Thirty-six (78%) tools named older people as target patients and 10 (22%) tools did not specify the target age group. Four (8.5%) tools were designed to detect inappropriate prescribing in hospitalised patients, 9 (19.5%) focused on patients in ambulatory care and 6 (13%) were developed for use in long-term care. Twenty-seven (59%) tools did not specify the health care setting. Consensus methods were applied in the development of 19 tools (41%), the others were based on either simple expert panels (13; 28%) or on a literature search (11; 24%). For three tools (7%) the development method was not described.
Conclusion
This overview reveals the characteristics of 46 assessment tools and can serve as a summary to assist readers in choosing a tool, either for research purposes or for daily practice use.


Similar content being viewed by others
References
Barber N (1995) What constitutes good prescribing? BMJ 310(6984):923–925
Shelton PS, Fritsch MA, Scott MA (2000) Assessing medication appropriateness in the elderly: a review of available measures. Drugs Aging 16(6):437–450
Spinewine A, Schmader KE, Barber N, Hughes C, Lapane KL, Swine C, Hanlon JT (2007) Appropriate prescribing in elderly people: how well can it be measured and optimised? Lancet 370(9582):173–184
Donabedian A (1981) Advantages and limitations of explicit criteria for assessing the quality of health care. Milbank Mem Fund Q Health Soc 59(1):99–106
Campbell SM, Cantrill JA (2001) Consensus methods in prescribing research. J Clin Pharm Ther 26(1):5–14
Chang CB, Chan DC (2010) Comparison of published explicit criteria for potentially inappropriate medications in older adults. Drugs Aging 27(12):947–957
Kaur S, Mitchell G, Vitetta L, Roberts MS (2009) Interventions that can reduce inappropriate prescribing in the elderly: a systematic review. Drugs Aging 26(12):1013–1028
Levy HB, Marcus EL, Christen C (2010) Beyond the Beers criteria: A comparative overview of explicit criteria. Ann Pharmacother 44(12):1968–1975
Dimitrow MS, Airaksinen MS, Kivela SL, Lyles A, Leikola SN (2011) Comparison of prescribing criteria to evaluate the appropriateness of drug treatment in individuals aged 65 and older: a systematic review. J Am Geriatr Soc 59(8):1521–1530
Parsons C, Johnston S, Mathie E, Baron N, Machen I, Amador S, Goodman C (2012) Potentially inappropriate prescribing in older people with dementia in care homes: a retrospective analysis. Drugs Aging 29(2):143–155
Mimica Matanovic S, Vlahovic-Palcevski V (2012) Potentially inappropriate medications in the elderly: a comprehensive protocol. Eur J Clin Pharmacol 68(8):1123–1138
Hanlon JT, Schmader KE, Ruby CM, Weinberger M (2001) Suboptimal prescribing in older inpatients and outpatients. J Am Geriatr Soc 49(2):200–209
Simonson W, Feinberg JL (2005) Medication-related problems in the elderly : defining the issues and identifying solutions. Drugs Aging 22(7):559–569
Robertson KE (1996) Process for preventing or identifying and resolving problems in drug therapy. Am J Health Syst Pharm 53(6):639–650
Wehling M (2009) Multimorbidity and polypharmacy: how to reduce the harmful drug load and yet add needed drugs in the elderly? Proposal of a new drug classification: fit for the aged. J Am Geriatr Soc 57(3):560–561
Haque R (2009) ARMOR: A Tool to Evaluate Polypharmacy in Elderly Persons. Annals of Long-Term Care 17(6):26–30
Sloane PD, Gruber-Baldini AL, Zimmerman S, Roth M, Watson L, Boustani M, Magaziner J, Hebel JR (2004) Medication undertreatment in assisted living settings. Arch Intern Med 164(18):2031–2037
Aronson JK (2004) Rational prescribing, appropriate prescribing. Br J Clin Pharmacol 57(3):229–230
Beers MH, Ouslander JG, Rollingher I, Reuben DB, Brooks J, Beck JC (1991) Explicit criteria for determining inappropriate medication use in nursing home residents. Arch Intern Med 151(9):1825–1832
Beers MH (1997) Explicit criteria for determining potentially inappropriate medication use by the elderly. An update Arch Intern Med 157(14):1531–1536
Fick DM, Cooper JW, Wade WE, Waller JL, Maclean JR, Beers MH (2003) Updating the Beers criteria for potentially inappropriate medication use in older adults: results of a US consensus panel of experts. Arch Intern Med 163(22):2716–2724
McLeod PJ, Huang AR, Tamblyn RM, Gayton DC (1997) Defining inappropriate practices in prescribing for elderly people: a national consensus panel. CMAJ 156(3):385–391
Hanlon JT, Schmader KE, Samsa GP, Weinberger M, Uttech KM, Lewis IK, Cohen HJ, Feussner JR (1992) A method for assessing drug therapy appropriateness. J Clin Epidemiol 45(10):1045–1051
Malone DC, Abarca J, Hansten PD, Grizzle AJ, Armstrong EP, Van Bergen RC, Duncan-Edgar BS, Solomon SL (2003) Lipton RB (2004) Identification of serious drug-drug interactions: results of the partnership to prevent drug-drug interactions. J Am Pharm Assoc 44(2):142–151
Taylor LK, Kawasumi Y, Bartlett G, Tamblyn R (2005) Inappropriate prescribing practices: the challenge and opportunity for patient safety. Healthc Q 8:81–85
Terrell KM, Perkins AJ, Dexter PR, Hui SL, Callahan CM, Miller DK (2009) Computerized decision support to reduce potentially inappropriate prescribing to older emergency department patients: a randomized, controlled trial. J Am Geriatr Soc 57(8):1388–1394
Matsumura Y, Yamaguchi T, Hasegawa H, Yoshihara K, Zhang Q, Mineno T, Takeda H (2009) Alert system for inappropriate prescriptions relating to patients' clinical condition. Methods Inf Med 48(6):566–573
Barenholtz Levy H (2003) Self-administered medication-risk questionnaire in an elderly population. Ann Pharmacother 37(7–8):982–987
American Geriatrics Society Updated Beers Criteria for Potentially Inappropriate Medication Use in Older Adults (2012) J Am Geriatr Soc 60(4):616–631
Wenger NS, Shekelle PG (2001) Assessing care of vulnerable elders: ACOVE project overview. Ann Intern Med 135(8 Pt 2):642–646
Shekelle PG, MacLean CH, Morton SC, Wenger NS (2001) Acove quality indicators. Ann Intern Med 135(8 Pt 2):653–667
Wenger NS, Roth CP, Shekelle P (2007) Introduction to the assessing care of vulnerable elders-3 quality indicator measurement set. J Am Geriatr Soc 55(Suppl 2):S247–252
Mann E, Bohmdorfer B, Fruhwald T, Roller-Wirnsberger RE, Dovjak P, Duckelmann-Hofer C, Fischer P, Rabady S, Iglseder B (2012) Potentially inappropriate medication in geriatric patients: the Austrian consensus panel list. Wien Klin Wochenschr 124(5–6):160–169
Schwalbe O, Freiberg I, Kloft C (2007) The beers criteria–an instrument to optimise the pharmacotherapy of geriatric patients. Med Monatsschr Pharm 30(7):244–248
Laroche ML, Charmes JP, Merle L (2007) Potentially inappropriate medications in the elderly: a French consensus panel list. Eur J Clin Pharmacol 63(8):725–731
Lindblad CI, Hanlon JT, Gross CR, Sloane RJ, Pieper CF, Hajjar ER, Ruby CM, Schmader KE (2006) Clinically important drug-disease interactions and their prevalence in older adults. Clin Ther 28(8):1133–1143
National Committee for Quality Assurance (NCQA) (2008) HEDIS - High Risk Medications (DAE-A) and potentially harmful Drug-Disease Interactions (DDE) in the Elderly. www.ncqa.org/tabid/598/Default.aspx. assessed 10.02.2011
Rognstad S, Brekke M, Fetveit A, Spigset O, Wyller TB, Straand J (2009) The Norwegian General Practice (NORGEP) criteria for assessing potentially inappropriate prescriptions to elderly patients. A modified Delphi study. Scand J Prim Health Care 27(3):153–159
Rancourt C, Moisan J, Baillargeon L, Verreault R, Laurin D, Gregoire JP (2004) Potentially inappropriate prescriptions for older patients in long-term care. BMC Geriatr 4:9
Barry PJ, Gallagher P, Ryan C, O'Mahony D (2007) START (screening tool to alert doctors to the right treatment)–an evidence-based screening tool to detect prescribing omissions in elderly patients. Age Ageing 36(6):632–638
Gallagher P, Ryan C, Byrne S, Kennedy J, O'Mahony D (2008) STOPP (Screening Tool of Older Person's Prescriptions) and START (Screening Tool to Alert doctors to Right Treatment). Consensus validation. Int J Clin Pharmacol Ther 46(2):72–83
Gallagher P, O'Mahony D (2008) STOPP (Screening Tool of Older Persons' potentially inappropriate Prescriptions): application to acutely ill elderly patients and comparison with Beers' criteria. Age Ageing 37(6):673–679
Holt S, Schmiedl S, Thurmann PA (2010) Potentially inappropriate medications in the elderly: the PRISCUS list. Dtsch Arztebl Int 107(31–32):543–551
Holt S, Schmiedl S, Thürmann PA (2011) PRISCUS-Liste potenziell inadäquater Medikation für ältere Menschen. http://priscus.net/download/PRISCUS-Liste_PRISCUS-TP3_2011.pdf. Accessed 01.02.2011
Winit-Watjana W, Sakulrat P, Kespichayawattana J (2008) Criteria for high-risk medication use in Thai older patients. Arch Gerontol Geriatr 47(1):35–51
Zhan C, Sangl J, Bierman AS, Miller MR, Friedman B, Wickizer SW, Meyer GS (2001) Potentially inappropriate medication use in the community-dwelling elderly: findings from the 1996 Medical Expenditure Panel Survey. JAMA 286(22):2823–2829
Maio V, Del Canale S, Abouzaid S (2010) Using explicit criteria to evaluate the quality of prescribing in elderly Italian outpatients: a cohort study. J Clin Pharm Ther 35(2):219–229
American Medical Directors Association (AMDA) Top 10 Particularly Dangerous Drug Interactions in Long Term Care. AMDA. http://www.amda.com/tools/clinical/m3/topten.cfm. Accessed 07.04. 2011
Raebel MA, Charles J, Dugan J, Carroll NM, Korner EJ, Brand DW, Magid DJ (2007) Randomized trial to improve prescribing safety in ambulatory elderly patients. J Am Geriatr Soc 55(7):977–985
Lechevallier-Michel N, Gautier-Bertrand M, Alperovitch A, Berr C, Belmin J, Legrain S, Saint-Jean O, Tavernier B, Dartigues JF, Fourrier-Reglat A (2005) Frequency and risk factors of potentially inappropriate medication use in a community-dwelling elderly population: results from the 3C Study. Eur J Clin Pharmacol 60(11):813–819
Bachyrycz A, Dodd MA, Priloutskaya G (2012) Development and dissemination of a statewide system to minimize use of Potentially Inappropriate Medications (PIMs). Med Care 50(11):993–996
Centre of Medicare and Medicaid Services (CMS) (2006) List of unnecessary Medications Used in Residents of Long-Term Care Facilities http://www.cms.gov/Regulations-and-Guidance/Guidance/Transmittals/downloads/R22SOMA.pdf. Accessed 22.03. 2011
Naugler CT, Brymer C, Stolee P, Arcese ZA (2000) Development and validation of an improving prescribing in the elderly tool. Can J Clin Pharmacol 7(2):103–107
Sloane PD, Zimmerman S, Brown LC, Ives TJ, Walsh JF (2002) Inappropriate medication prescribing in residential care/assisted living facilities. J Am Geriatr Soc 50(6):1001–1011
Kolzsch M, Bolbrinker J, Huber M, Kreutz R (2010) Potentially inappropriate medication for the elderly: adaptation and evaluation of a French consensus list. Med Monatsschr Pharm 33(8):295–302
Frohnhofen H, Michalek C, Wehling M (2011) Assessment of drug treatment in geriatrics with the new FORTA criteria. Dtsch Med Wochenschr 136(27):1417–1421
Cantrill JA, Sibbald B, Buetow S (1998) Indicators of the appropriateness of long-term prescribing in general practice in the United Kingdom: consensus development, face and content validity, feasibility, and reliability. Qual Health Care 7(3):130–135
Lipton HL, Bero LA, Bird JA, McPhee SJ (1992) The impact of clinical pharmacists' consultations on physicians' geriatric drug prescribing. A randomized controlled trial. Med Care 30(7):646–658
Winslade NE, Bajcar JM, Bombassaro AM, Caravaggio CD, Strong DK, Yamashita SK (1997) Pharmacist's management of drug-related problems: a tool for teaching and providing pharmaceutical care. Pharmacotherapy 17(4):801–809
Hamdy RC, Moore SW, Whalen K, Donnelly JP, Compton R, Testerman F, Haulsee P, Hughes J (1995) Reducing polypharmacy in extended care. South Med J 88(5):534–538
Owens NJ, Fretwell MD, Willey C, Murphy SS (1994) Distinguishing between the fit and frail elderly, and optimising pharmacotherapy. Drugs Aging 4(1):47–55
Basger BJ, Chen TF, Moles RJ (2008) Inappropriate medication use and prescribing indicators in elderly Australians: development of a prescribing indicators tool. Drugs Aging 25(9):777–793
Basger BJ, Chen TF, Moles RJ (2012) Validation of prescribing appropriateness criteria for older Australians using the RAND/UCLA appropriateness method. BMJ Open 2(5)
Brown NJ, Griffin MR, Ray WA, Meredith S, Beers MH, Marren J, Robles M, Stergachis A, Wood AJ, Avorn J (1998) A model for improving medication use in home health care patients. J Am Pharm Assoc (Wash) 38(6):696–702
New South Wales Therapeutic Advisory Group (2007) Indicators for Quality Use of Medicines in Australian Hospitals. http://www.ciap.health.nsw.gov.au/nswtag/documents/publications/indicators/manual.pdf. Accessed 01.05. 2011
Oborne CA, Batty GM, Maskrey V, Swift CG, Jackson SH (1997) Development of prescribing indicators for elderly medical inpatients. Br J Clin Pharmacol 43(1):91–97
Oborne CA, Hooper R, Swift CG, Jackson SH (2003) Explicit, evidence-based criteria to assess the quality of prescribing to elderly nursing home residents. Age Ageing 32(1):102–108
Lee SS, Schwemm AK, Reist J, Cantrell M, Andreski M, Doucette WR, Chrischilles EA, Farris KB (2009) Pharmacists' and pharmacy students' ability to identify drug-related problems using TIMER (Tool to Improve Medications in the Elderly via Review). Am J Pharm Educ 73(3):52
Newton PF, Levinson W, Maslen D (1994) The geriatric medication algorithm: a pilot study. J Gen Intern Med 9(3):164–167
Johnson KA, Nye M, Hill-Besinque K, Cody M (1995) Measuring of impact of patient counseling in the outpatient pharmacy setting: development and implementation of the counseling models for the Kaiser Permanente/USC Patient Consultation Study. Clin Ther 17(5):988–1002
Bergman-Evans B (2006) Evidence-based guideline. Improving medication management for older adult clients. J Gerontol Nurs 32(7):6–14
Drenth-van Maanen AC, van Marum RJ, Knol W, van der Linden CM, Jansen PA (2009) Prescribing optimization method for improving prescribing in elderly patients receiving polypharmacy: results of application to case histories by general practitioners. Drugs Aging 26(8):687–701
Albert SM, Colombi A, Hanlon J (2010) Potentially inappropriate medications and risk of hospitalization in retirees: analysis of a US retiree health claims database. Drugs Aging 27(5):407–415
Ruggiero C, Dell'Aquila G, Gasperini B, Onder G, Lattanzio F, Volpato S, Corsonello A, Maraldi C, Bernabei R, Cherubini A (2010) Potentially inappropriate drug prescriptions and risk of hospitalization among older, Italian, nursing home residents: the ULISSE project. Drugs Aging 27(9):747–758
Passarelli MC, Jacob-Filho W, Figueras A (2005) Adverse drug reactions in an elderly hospitalised population: inappropriate prescription is a leading cause. Drugs Aging 22(9):767–777
Dedhiya SD, Hancock E, Craig BA, Doebbeling CC, Thomas J 3rd (2010) Incident use and outcomes associated with potentially inappropriate medication use in older adults. Am J Geriatr Pharmacother 8(6):562–570
McCombs JS, Liu G, Shi J, Feng W, Cody M, Parker JP, Nichol MB, Hay JW, Johnson KA, Groshen SL, Nye MT (1998) The Kaiser Permanente/USC Patient Consultation Study: change in use and cost of health care services. Am J Health Syst Pharm 55(23):2485–2499
Lipton HL, Bird JA, Bero LA, McPhee SJ (1993) Assessing the appropriateness of physician prescribing for geriatric outpatients. Development and testing of an instrument. J Pharm Technol 9(3):107–113
Hamilton H, Gallagher P, Ryan C, Byrne S, O'Mahony D (2011) Potentially inappropriate medications defined by STOPP criteria and the risk of adverse drug events in older hospitalized patients. Arch Intern Med 171(11):1013–1019
Conflicts of interest
The authors declare that they have no conflicts of interest.
Contributions of authors statement (with relevance to the ICMJE Guidelines)
C. P. Kaufmann: Contribution to the study design and the analysis and interpretation of data, involvement in the literature search, manuscript writing, final approval of the version to be published.
R. Tremp: Contribution to the study design and the analysis and interpretation of data, conducted the literature search and the mapping of the different tools.
K.E. Hersberger: Manuscript review and final approval of the version to be published.
M.L. Lampert: Contribution to the study design and the analysis and interpretation of data, manuscript review and final approval of the version to be published
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kaufmann, C.P., Tremp, R., Hersberger, K.E. et al. Inappropriate prescribing: a systematic overview of published assessment tools. Eur J Clin Pharmacol 70, 1–11 (2014). https://doi.org/10.1007/s00228-013-1575-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00228-013-1575-8