Abstract
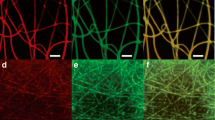
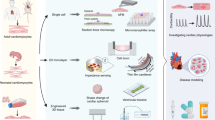
Due to the unique physicochemical properties exhibited by materials with nanoscale dimensions, there is currently a continuous increase in the number of engineered nanomaterials (ENMs) used in consumer goods. However, several reports associate ENM exposure to negative health outcomes such as cardiovascular diseases. Therefore, understanding the pathological consequences of ENM exposure represents an important challenge, requiring model systems that can provide mechanistic insights across different levels of ENM-based toxicity. To achieve this, we developed a mussel-inspired 3D microphysiological system (MPS) to measure cardiac contractility in the presence of ENMs. While multiple cardiac MPS have been reported as alternatives to in vivo testing, most systems only partially recapitulate the native extracellular matrix (ECM) structure. Here, we show how adhesive and aligned polydopamine (PDA)/polycaprolactone (PCL) nanofiber can be used to emulate the 3D native ECM environment of the myocardium. Such nanofiber scaffolds can support the formation of anisotropic and contractile muscular tissues. By integrating these fibers in a cardiac MPS, we assessed the effects of TiO2 and Ag nanoparticles on the contractile function of cardiac tissues. We found that these ENMs decrease the contractile function of cardiac tissues through structural damage to tissue architecture. Furthermore, the MPS with embedded sensors herein presents a way to non-invasively monitor the effects of ENM on cardiac tissue contractility at different time points. These results demonstrate the utility of our MPS as an analytical platform for understanding the functional impacts of ENMs while providing a biomimetic microenvironment to in vitro cardiac tissue samples.

Heart-on-a-chip integrated with mussel-inspired fiber scaffolds for a high-throughput toxicological assessment of engineered nanomaterials






Similar content being viewed by others
References
Walser T, Limbach LK, Brogioli R, Erismann E, Flamigni L, Hattendorf B, et al. Persistence of engineered nanoparticles in a municipal solid-waste incineration plant. Nat Nanotechnol. 2012;7(8):520.
Simeonova PP, Erdely A. Engineered nanoparticle respiratory exposure and potential risks for cardiovascular toxicity: predictive tests and biomarkers. Inhal Toxicol. 2009;21(sup1):68–73.
Yokel RA, MacPhail RC. Engineered nanomaterials: exposures, hazards, and risk prevention. J Occup Med Toxicol. 2011;6(1):7.
Gwinn MR, Vallyathan V. Nanoparticles: health effects—pros and cons. Environ Health Perspect. 2006;114(12):1818.
Stampfl A, Maier M, Radykewicz R, Reitmeir P, Göttlicher M, Niessner R. Langendorff heart: a model system to study cardiovascular effects of engineered nanoparticles. ACS Nano. 2011;5(7):5345–53.
Lin C-X, Yang S-Y, Gu J-L, Meng J, Xu H-Y, Cao J-M. The acute toxic effects of silver nanoparticles on myocardial transmembrane potential, I Na and I K1 channels and heart rhythm in mice. Nanotoxicology. 2017;11(6):827–37.
Mueller NC, Nowack B. Exposure modeling of engineered nanoparticles in the environment. Environ Sci Technol. 2008;42(12):4447–53.
Sun H, Xia M, Austin CP, Huang R. Paradigm shift in toxicity testing and modeling. AAPS J. 2012;14(3):473–80.
Grosberg A, Alford PW, McCain ML, Parker KK. Ensembles of engineered cardiac tissues for physiological and pharmacological study: heart on a chip. Lab Chip. 2011;11(24):4165–73.
Grosberg A, Nesmith AP, Goss JA, Brigham MD, McCain ML, Parker KK. Muscle on a chip: in vitro contractility assays for smooth and striated muscle. J Pharmacol Toxicol Methods. 2012;65(3):126–35.
Shim J, Grosberg A, Nawroth JC, Parker KK, Bertoldi K. Modeling of cardiac muscle thin films: pre-stretch, passive and active behavior. J Biomech. 2012;45(5):832–41.
McCain ML, Agarwal A, Nesmith HW, Nesmith AP, Parker KK. Micromolded gelatin hydrogels for extended culture of engineered cardiac tissues. Biomaterials. 2014;35(21):5462–71.
Lind JU, Busbee TA, Valentine AD, Pasqualini FS, Yuan H, Yadid M, et al. Instrumented cardiac microphysiological devices via multimaterial three-dimensional printing. Nat Mater. 2017;16(3):303.
Lind JU, Yadid M, Perkins I, O’Connor BB, Eweje F, Chantre CO, et al. Cardiac microphysiological devices with flexible thin-film sensors for higher-throughput drug screening. Lab Chip. 2017;17(21):3692–703.
Feinberg AW, Feigel A, Shevkoplyas SS, Sheehy S, Whitesides GM, Parker KK. Muscular thin films for building actuators and powering devices. Science. 2007;317(5843):1366–70.
Agarwal A, Goss JA, Cho A, McCain ML, Parker KK. Microfluidic heart on a chip for higher throughput pharmacological studies. Lab Chip. 2013;13(18):3599–608.
McCain ML, Sheehy SP, Grosberg A, Goss JA, Parker KK. Recapitulating maladaptive, multiscale remodeling of failing myocardium on a chip. Proc Natl Acad Sci. 2013;110(24):9770–5.
Nesmith AP, Agarwal A, McCain ML, Parker KK. Human airway musculature on a chip: an in vitro model of allergic asthmatic bronchoconstriction and bronchodilation. Lab Chip. 2014;14(20):3925–36.
Wang G, McCain ML, Yang L, He A, Pasqualini FS, Agarwal A, et al. Modeling the mitochondrial cardiomyopathy of Barth syndrome with induced pluripotent stem cell and heart-on-chip technologies. Nat Med. 2014;20(6):616.
Pham QP, Sharma U, Mikos AG. Electrospinning of polymeric nanofibers for tissue engineering applications: a review. Tissue Eng. 2006;12(5):1197–211.
Badrossamay MR, McIlwee HA, Goss JA, Parker KK. Nanofiber assembly by rotary jet-spinning. Nano Lett. 2010;10(6):2257–61.
Badrossamay MR, Balachandran K, Capulli AK, Golecki HM, Agarwal A, Goss JA, et al. Engineering hybrid polymer-protein super-aligned nanofibers via rotary jet spinning. Biomaterials. 2014;35(10):3188–97.
Deravi LF, Sinatra NR, Chantre CO, Nesmith AP, Yuan H, Deravi SK, et al. Design and fabrication of fibrous nanomaterials using pull spinning. Macromol Mater Eng. 2017;302(3):1600404.
Liu Y, Ai K, Lu L. Polydopamine and its derivative materials: synthesis and promising applications in energy, environmental, and biomedical fields. Chem Rev. 2014;114(9):5057–115.
Lin Q, Gourdon D, Sun C, Holten-Andersen N, Anderson TH, Waite JH, et al. Adhesion mechanisms of the mussel foot proteins mfp-1 and mfp-3. Proc Natl Acad Sci. 2007;104(10):3782–6.
Lee H, Rho J, Messersmith PB. Facile conjugation of biomolecules onto surfaces via mussel adhesive protein inspired coatings. Adv Mater. 2009;21(4):431–4.
Chuah YJ, Koh YT, Lim K, Menon NV, Wu Y, Kang Y. Simple surface engineering of polydimethylsiloxane with polydopamine for stabilized mesenchymal stem cell adhesion and multipotency. Sci Rep. 2015;5:18162.
Ku SH, Park CB. Human endothelial cell growth on mussel-inspired nanofiber scaffold for vascular tissue engineering. Biomaterials. 2010;31(36):9431–7.
Dhand C, Barathi VA, Ong ST, Venkatesh M, Harini S, Dwivedi N, et al. Latent oxidative polymerization of catecholamines as potential cross-linkers for biocompatible and multifunctional biopolymer scaffolds. ACS Appl Mater Interfaces. 2016;8(47):32266–81.
Choi W, Lee S, Kim SH, Jang JH. Polydopamine inter-fiber networks: new strategy for producing rigid, sticky, 3D fluffy electrospun fibrous polycaprolactone sponges. Macromol Biosci. 2016;16(6):824–35.
Della Vecchia NF, Luchini A, Napolitano A, D’Errico G, Vitiello G, Szekely N, et al. Tris buffer modulates polydopamine growth, aggregation, and paramagnetic properties. Langmuir. 2014;30(32):9811–8.
Klosterman L, Ahmad Z, Viswanathan V, Bettinger CJ. Synthesis and measurement of cohesive mechanics in polydopamine nanomembranes. Adv Mater Interfaces. 2017;4(10):1700041.
Patel K, Singh N, Yadav J, Nayak JM, Sahoo SK, Lata J, et al. Polydopamine films changes their physiochemical and antimicrobial properties with change in reaction conditions. Phys Chem Chem Phys. 2018;20(8):5744–55.
Hotaling NA, Bharti K, Kriel H, Simon CG. DiameterJ: a validated open source nanofiber diameter measurement tool. Biomaterials. 2015;61:327–38.
Chan FK-M, Moriwaki K, De Rosa MJ. Detection of necrosis by release of lactate dehydrogenase activity. In: Snow A, Lenardo M, editors. Immune homeostasis. Methods in molecular biology (methods and protocols), vol. 979. Totowa: Humana Press; 2013. p. 65–70.
Ahn S, Chantre CO, Gannon AR, Lind JU, Campbell PH, Grevesse T, et al. Soy protein/cellulose nanofiber scaffolds mimicking skin extracellular matrix for enhanced wound healing. Adv Healthcare Mater. 2018:1701175. https://doi.org/10.1002/adhm.201701175.
Sheehy SP, Pasqualini F, Grosberg A, Park SJ, Aratyn-Schaus Y, Parker KK. Quality metrics for stem cell-derived cardiac myocytes. Stem Cell Rep. 2014;2(3):282–94.
Pasqualini FS, Sheehy SP, Agarwal A, Aratyn-Schaus Y, Parker KK. Structural phenotyping of stem cell-derived cardiomyocytes. Stem Cell Rep. 2015;4(3):340–7.
Tran QH, Le A-T. Silver nanoparticles: synthesis, properties, toxicology, applications and perspectives. Adv Nat Sci Nanosci Nanotechnol. 2013;4(3):033001.
Lee KJ, Jun BH, Kim TH, Joung J. Direct synthesis and inkjetting of silver nanocrystals toward printed electronics. Nanotechnology. 2006;17(9):2424.
Beltran-Huarac J, Zhang Z, Pyrgiotakis G, DeLoid G, Vaze N, Demokritou P. Development of reference metal and metal oxide engineered nanomaterials for nanotoxicology research using high throughput and precision flame spray synthesis approaches. NanoImpact. 2018;10:26–37.
DeLoid GM, Cohen JM, Pyrgiotakis G, Demokritou P. Preparation, characterization, and in vitro dosimetry of dispersed, engineered nanomaterials. Nat Protoc. 2017;12(2):355.
DeLoid GM, Cohen JM, Pyrgiotakis G, Pirela SV, Pal A, Liu J, et al. Advanced computational modeling for in vitro nanomaterial dosimetry. Part Fibre Toxicol. 2015;12(1):32.
DeLoid G, Cohen JM, Darrah T, Derk R, Rojanasakul L, Pyrgiotakis G, et al. Estimating the effective density of engineered nanomaterials for in vitro dosimetry. Nat Commun. 2014;5:3514.
Taurozzi JS, Hackley VA, Wiesner MR. Ultrasonic dispersion of nanoparticles for environmental, health and safety assessment—issues and recommendations. Nanotoxicology. 2011;5(4):711–29.
Dvir T, Timko BP, Brigham MD, Naik SR, Karajanagi SS, Levy O, et al. Nanowired three-dimensional cardiac patches. Nat Nanotechnol. 2011;6(11):720.
Liebscher J, Mrówczyński R, Scheidt HA, Filip C, Hădade ND, Turcu R, et al. Structure of polydopamine: a never-ending story? Langmuir. 2013;29(33):10539–48.
Xie J, Michael PL, Zhong S, Ma B, MacEwan MR, Lim CT. Mussel inspired protein-mediated surface modification to electrospun fibers and their potential biomedical applications. J Biomed Mater Res A. 2012;100((4):929–38.
Zangmeister RA, Morris TA, Tarlov MJ. Characterization of polydopamine thin films deposited at short times by autoxidation of dopamine. Langmuir. 2013;29(27):8619–28.
Boudreau-Béland J, Duverger JE, Petitjean E, Maguy A, Ledoux J, Comtois P. Spatiotemporal stability of neonatal rat cardiomyocyte monolayers spontaneous activity is dependent on the culture substrate. PLoS One. 2015;10(6):e0127977.
Jawad H, Boccaccini AR, Ali NN, Harding SE. Assessment of cellular toxicity of TiO2 nanoparticles for cardiac tissue engineering applications. Nanotoxicology. 2011;5(3):372–80.
Mallik A, Bryan S, Puukila S, Chen A, Khaper N. Efficacy of Pt-modified TiO2 nanoparticles in cardiac cells. Exp Clin Cardiol. 2011;16(1):6.
Schwerdt A, Zintchenko A, Concia M, Roesen N, Fisher K, Lindner LH, et al. Hyperthermia-induced targeting of thermosensitive gene carriers to tumors. Hum Gene Ther. 2008;19(11):1283–92.
Bostan HB, Rezaee R, Valokala MG, Tsarouhas K, Golokhvast K, Tsatsakis AM, et al. Cardiotoxicity of nano-particles. Life Sci. 2016;165:91–9.
Duan Y, Liu H, Zhao J, Liu C, Li Z, Yan J, et al. The effects of nano-anatase TiO2 on the activation of lactate dehydrogenase from rat heart. Biol Trace Elem Res. 2009;130(2):162–71.
Sheng L, Wang X, Sang X, Ze Y, Zhao X, Liu D, et al. Cardiac oxidative damage in mice following exposure to nanoparticulate titanium dioxide. J Biomed Mater Res A. 2013;101(11):3238–46.
Savi M, Rossi S, Bocchi L, Gennaccaro L, Cacciani F, Perotti A, et al. Titanium dioxide nanoparticles promote arrhythmias via a direct interaction with rat cardiac tissue. Part Fibre Toxicol. 2014;11(1):63.
Chen J, Dong X, Xin Y, Zhao M. Effects of titanium dioxide nano-particles on growth and some histological parameters of zebrafish (Danio rerio) after a long-term exposure. Aquat Toxicol. 2011;101(3-4):493–9.
Carlson C, Hussain SM, Schrand AM, Braydich-Stolle LK, Hess KL, Jones RL, et al. Unique cellular interaction of silver nanoparticles: size-dependent generation of reactive oxygen species. J Phys Chem B. 2008;112(43):13608–19.
AshaRani P, Low Kah Mun G, Hande MP, Valiyaveettil S. Cytotoxicity and genotoxicity of silver nanoparticles in human cells. ACS Nano. 2008;3(2):279–90.
Han X, Gelein R, Corson N, Wade-Mercer P, Jiang J, Biswas P, et al. Validation of an LDH assay for assessing nanoparticle toxicity. Toxicology. 2011;287(1-3):99–104.
Altunbek M, Culha M. Influence of plasmonic nanoparticles on the performance of colorimetric cell viability assays. Plasmonics. 2017;12(6):1749–60.
Interagency Research Animal Committee. US government principles for the utilization and care of vertebrate animals used in testing, research and training. 2010;13. https://grants.nih.gov/grants/olaw/references/phspol.htm#USGovPrinciples. Accessed Dec 2010.
National Research Council. Guide for the care and use of laboratory animals. Washington, D.C.: National Academies Press; 2010.
US Department of Health and Human Services. Code of federal regulations: title 9: part 1: chapter 1: subchapter A: animal welfare. 2009;1.
Acknowledgements
The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. The engineered nanomaterials used in the research presented in this publication have been procured or synthesized and characterized by the Engineered Nanomaterials Resource and Coordination Core (ERCC) at the Center for Nanotechnology and Nanotoxicology at Harvard School of Public Health, part of the NIEHS/NHIR consortium. The authors also acknowledge the graphic works provided by Michael Rosnach. The authors also thank Dr. Patrick Campbell for providing information about the guidelines followed for animal experiments.
Funding
This work was supported by the Wyss Institute for Biologically Inspired Engineering at Harvard University. For the development and characterization of 3D nanofibrous MPS platform, this research was performed in part at the Harvard University Materials Research Science and Engineering Center (MRSEC) under NSF Award No. DMR-1420570 and the Harvard Center for Nanoscale Systems (CNS), which is a member of the National Nanotechnology Infrastructure Network (NNIN) under NSF Award No. 1541959. Research reported in this publication was supported by National Institute of Environmental Health Sciences of the National Institutes of Health under Award Number (NIH grant number U01ES027272) as part of the Nanotechnology Health Implications Research (NHIR) Consortium.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Research involving human participants and/or animals
The Faculty of Arts and Sciences (FAS) of Harvard University maintains an Institutional Animal Care and Use Committee (IACUC) as required by the Public Health Service (PHS) Policy on Humane Care and Use of Laboratory Animals. All protocols for animal experiments done in this study were approved by IACUC at Harvard University. All animals were appropriately housed prior to use. On arrival to our animal facility, neonatal rat pups used in the study and their dams were housed in clean, ventilated microisolator cages in a climate-controlled, automatic light cycle-equipped room with dam having free access to food and fresh water. All research personnel handling animals were appropriately qualified and trained by Harvard’s Office of Animal Resources under the direction of the Attending Veterinarian. Our euthanasia method for the pups is consistent with the recommendations of the 2013 American Veterinary Medical Association (AVMA) Guidelines on Euthanasia for rodents. All rats used in this study were cared for and used in a manner that complies with the US Government Principles for the Utilization and Care of Vertebrate Animals Used in Testing, Research, and Training [63]; the Guide for the Care and Use of Laboratory Animals [64]; and the Animal Welfare Act/Regulations [65].
Additional information
Published in the topical collection Analytical Developments in Advancing Safety in Nanotechnology with guest editors Lisa Holland and Wenwan Zhong.
Rights and permissions
About this article
Cite this article
Ahn, S., Ardoña, H.A.M., Lind, J.U. et al. Mussel-inspired 3D fiber scaffolds for heart-on-a-chip toxicity studies of engineered nanomaterials. Anal Bioanal Chem 410, 6141–6154 (2018). https://doi.org/10.1007/s00216-018-1106-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00216-018-1106-7