Abstract
Summary
This study revealed the time course of osteoporotic vertebral fracture by magnetic resonance imaging using a simple classification. Signal changes were associated with the compression degree and mobility of the fractured vertebral body. This classification showed sufficient reliability in categorizing magnetic resonance imaging findings of osteoporotic vertebral fractures.
Introduction
Magnetic resonance imaging (MRI) is useful in diagnosing osteoporotic vertebral fractures (OVFs). This study investigated the time course of OVFs by MRI using a simple classification.
Methods
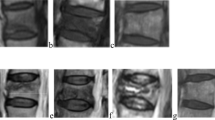
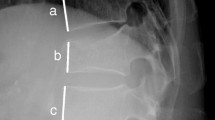
This multicenter cohort study was performed from 2012 to 2015. Consecutive patients with ≤2-week-old OVFs were enrolled in 11 institutions. MRI was performed at enrollment and at 1-, 3-, 6-, and 12-month follow-up. Signal changes on T1-weighted imaging (T1WI), T2WI, and short τ inversion recovery (STIR) were classified according to signal intensity. Height and angular motion of vertebral bodies were also measured.
Results
The 6-month follow-up was completed by 153 patients. At enrollment, fractured vertebrae signal changes were 43 % diffuse and 57 % confined low on T1WI; on T2WI, 56, 24, and 5 % were confined low, high, and diffuse low, respectively; on STIR, 100 % were high. On T1WI, diffuse low remained most common (90 % at 1 month and 60 % at 3 months) until 6 and 12 months, when most were confined low (54 and 52 %, respectively). On T2WI, confined low remained most common (decreasing to 41 % at 12 months). On STIR, high signal change was shown in 98, 87, and 64 % at 3, 6, and 12 months, respectively. At 3, 6, and 12 months, diffuse low signal change was associated with significantly lower vertebral height, and high signal change was associated with significantly greater angular motion.
Conclusions
MRI signal changes were associated with the compression degree and angular motion of fractured vertebrae. This classification showed sufficient reliability in categorizing MRI findings of OVFs.






Similar content being viewed by others
References
Johnell O, Kanis J (2005) Epidemiology of osteoporotic fractures. Osteoporos Int 16:6–10
Statistics Bureau Home Page. http://www.stat.go.jp/english/. Accessed 26 Jul 2015
Pfirrmann CW, Metzdorf a, Zanetti M, et al. (2001) Magnetic resonance classification of lumbar intervertebral disc degeneration. Spine (Phila Pa 1976) 26:1873–1878
Krege JH, Siminoski K, Adachi JD, et al. (2006) A simple method for determining the probability a new vertebral fracture is present in postmenopausal women with osteoporosis. Osteoporos Int 17:379–386
Huang C, Ross PD, Wasnich RD (1996) Vertebral fracture and other predictors of physical impairment and health care utilization. Arch Intern Med 156:2469–2475
Kado DM, Browner WS, Palermo L, et al. (1999) Vertebral fractures and mortality in older women: a prospective study. Study of Osteoporotic Fractures Research Group. Arch Intern Med 159:1215–1220
Nevitt MC, Ettinger B, Black DM, et al. (1998) The association of radiographically detected vertebral fractures with back pain and function: a prospective study. Ann Intern Med 128:793–800
Lenchik L, Rogers LF, Delmas PD, Genant HK (2004) Diagnosis of osteoporotic vertebral fractures. Am J Roentgenol 183:949–958
Toyone T, Toyone T, Tanaka T, et al. (2006) Changes in vertebral wedging rate between supine and standing position and its association with back pain: a prospective study in patients with osteoporotic vertebral compression fractures. Spine (Phila Pa 1976) 31:2963–2966
McKiernan F, Faciszewski T (2003) Intravertebral clefts in osteoporotic vertebral compression fractures. Arthritis Rheum 48:1414–1419
Mehta JS, Reed MR, McVie JL, Sanderson PL (2004) Weight-bearing radiographs in thoracolumbar fractures: do they influence management? Spine (Phila Pa 1976) 29:564–567
Oner FC, Van Gils APG, Dhert WJ a, Verbout a J (1999) MRI findings of thoracolumbar spine fractures: a categorisation based on MRI examinations of 100 fractures. Skelet Radiol 28:433–443
Cho T, Matsuda M, Sakurai M (1996) MRI findings on healing process of vertebral fracture in osteoporosis. J Orthop Sci 1:16–33
Kanchiku T, Imajo Y, Suzuki H, et al. (2013) Usefulness of an early MRI-based classification system for predicting vertebral collapse and pseudoarthrosis after osteoporotic vertebral fractures. J Spinal Disord Tech 27:61–65
Tsujio T, Nakamura H, Terai H, et al. (2011) Characteristic radiographic or magnetic resonance images of fresh osteoporotic vertebral fractures predicting potential risk for nonunion: a prospective multicenter study. Spine (Phila Pa 1976) 36:1229–1235
Heini PF (2005) The current treatment—a survey of osteoporotic fracture treatment. Osteoporotic spine fractures: the spine surgeon’s perspective. Osteoporos Int 16(Suppl 2):S85–S92
McKiernan F, Jensen R, Faciszewski T (2003) The dynamic mobility of vertebral compression fractures. J Bone Miner Res 18:24–29
Daniel A, Sven KT, Von Der HN, et al. (2014) Non-union of osteoporotic vertebral fractures—identification and treatment of an underestimated pathology in elderly patients with persistent back pain. Acta Orthop Belg 80:444–450
Baker LL, Goodman SB, Perkash I, et al. (1990) Benign versus pathologic compression fractures of vertebral bodies: assessment with conventional spin-echo, chemical-shift, and STIR MR imaging. Radiology 174:495–502
Meyers SP, Wiener SN (1991) Magnetic resonance imaging features of fractures using the short tau inversion recovery (STIR) sequence: correlation with radiographic findings. Skelet Radiol 20:499–507
Kim H-J, Yi J-M, Cho H-G, et al. (2014) Comparative study of the treatment outcomes of osteoporotic compression fractures without neurologic injury using a rigid brace, a soft brace, and no brace: a prospective randomized controlled non-inferiority trial. J Bone Joint Surg Am 96:1959–1966
Goodwin VA, Hall AJ, Rogers E, Bethel A (2016) Orthotics and taping in the management of vertebral fractures in people with osteoporosis: a systematic review. BMJ Open
Oner F, Ramos L, Simmermacher R, et al. (2002) Classification of thoracic and lumbar spine fractures: problems of reproducibility: a study of 53 patients using CT and MRI. Eur Spine J 11:235–245
Kanchiku T, Taguchi T, Kawai S (2003) Magnetic resonance imaging diagnosis and new classification of the osteoporotic vertebral fracture. J Orthop 8:463–466
Yao L, Lee JK (1988) Occult intraosseous fracture: detection with MR imaging. Radiology 167:749–751
Deutsch AL, Mink JH (1989) Magnetic resonance imaging of musculoskeletal injuries. Radiol Clin N Am 27:983–1002
Vogler JB, Murphy WA (1988) Bone marrow imaging. Radiology 168:679–693
Smith SR, Williams CE, Davies JM, Edwards RH (1989) Bone marrow disorders: characterization with quantitative MR imaging. Radiology 172:805–810
Zanetti M, Bruder E, Romero J, Hodler J (2000) Bone marrow edema pattern in osteoarthritic knees: correlation between MR imaging and histologic findings. Radiology 215:835–840
Dunn AJ, Campbell RSD, Mayor PE, Rees D (2008) Radiological findings and healing patterns of incomplete stress fractures of the pars interarticularis. Skelet Radiol 37:443–450
Mcnally EG, Goodman R, Burge P (2000) Original article the role of MRI in the assessment of scaphoid fracture healing : a pilot study. Eur Radiol 1928:1926–1928
Ryu CW, Han H, Lee YM, Lim MK (2009) The intravertebral cleft in benign vertebral compression fracture: the diagnostic performance of non-enhanced MRI and fat-suppressed contrast-enhanced MRI. Br J Radiol 82:976–981
Sarli M, Pérez Manghi FC, Gallo R, Zanchetta JR (2005) The vacuum cleft sign: an uncommon radiological sign. Osteoporos Int 16:1210–1214. doi:10.1007/s00198-005-1833-4
Malghem J, Maldague B, Labaisse MA, et al. (1993) Intravertebral vacuum cleft: changes in content after supine positioning. Radiology 187:483–487
Jimenez-Boj E, Nöbauer-Huhmann I, Hanslik-Schnabel B, et al. (2007) Bone erosions and bone marrow edema as defined by magnetic resonance imaging reflect true bone marrow inflammation in rheumatoid arthritis. Arthritis Rheum 56:1118–1124
Mahnken AH, Wildberger JE, Adam G, et al. (2005) Is there a need for contrast-enhanced T1-weighted MRI of the spine after inconspicuous short τ inversion recovery imaging? Eur Radiol 15:1387–1392
Diamond TH, Clark WA, Kumar SV (2007) Histomorphometric analysis of fracture healing cascade in acute osteoporotic vertebral body fractures. Bone 40:775–780
Bailey CS, Urquhart JC, Dvorak MF, et al. (2014) Orthosis versus no orthosis for the treatment of thoracolumbar burst fractures without neurologic injury: a multicenter prospective randomized equivalence trial. Spine J 14:2557–2564
Shamji MF, Roffey DM, Young DK, et al. (2014) A pilot evaluation of the role of bracing in stable thoracolumbar burst fractures without neurological deficit. J Spinal Disord Tech 27:370–375
Hoshino M, Tsujio T, Terai H, et al. (2013) Impact of initial conservative treatment interventions on the outcomes of patients with osteoporotic vertebral fractures. Spine (Phila Pa 1976) 38:E641–E648
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None.
Funding
This study was funded by the Japan Orthopedics and Traumatology Research Foundation, Inc. (grant no. 270).
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Takahashi, S., Hoshino, M., Takayama, K. et al. Time course of osteoporotic vertebral fractures by magnetic resonance imaging using a simple classification: a multicenter prospective cohort study. Osteoporos Int 28, 473–482 (2017). https://doi.org/10.1007/s00198-016-3737-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-016-3737-x