Abstract
Summary
The effect of whole body-electromyostimulation in community-dwelling women ≥70 with sarcopenic obesity was heterogeneous, with high effects on muscle mass, moderate effects on functional parameters, and minor effects on fat mass. Further, we failed to determine a supportive effect of additional protein-enriched dietary supplementation in this albeit predominately well-nourished group.
Introduction
The aim of the study was to determine the effect of whole-body electromyostimulation (WB-EMS) on sarcopenic obesity (SO) in community-dwelling women more than 70 years with sarcopenic obesity.
Methods
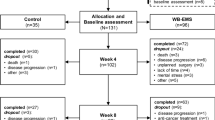
Seventy-five community-dwelling women ≥70 years with SO were randomly allocated to either a WB-EMS-application with (WB-EMS &P; 24.9 ± 1.9 kg/m2) or without (WB-EMS; 25.2 ± 1.8 kg/m2) dietary supplementation (150 kcal/day, 56 % protein) or a non-training control group (CG; 24.7 ± 1.4 kg/m2). WB-EMS consisted of one weekly session of 20 min (85 Hz, 350 μs, 4 s of strain–4 s of rest) performed with moderate to high intensity. Primary study endpoint was the Sarcopenia Z-Score constituted by skeletal muscle mass index (SMI, as assessed by dual energy X-ray absorptiometry), grip strength, and gait speed, and secondary study endpoint was body fat (%).
Results
Sarcopenia Z-score comparably increases in the WB-EMS and the WB-EMS&P-group (p ≤ .046). Both groups differ significantly (p ≤ .001) from the CG which deteriorated significantly (p = .006). Although body fat changes were most pronounced in the WB-EMS (−0.9 ± 2.1; p = .125) and WB-EMS&P (−1.4 ± 2.5; p = .028), reductions did not statistically differ (p = .746) from the CG (−0.8 ± 2.7; p = .179). Looking behind the covariates, the most prominent changes were determined for SMI, with a significant increase in both EMS-groups (2.0–2.5 %; p ≤ .003) and a decrease in the CG (−1.2 ± 3.1 %; p = .050) with significant between-group differences (p = .001).
Conclusion
WB-EMS is a safe and attractive method for increasing muscle mass and functional capacity in this cohort of women 70+ with SO; however, the effect on body fat is minor. Protein-enriched supplements did not increase effects of WB-EMS alone.


Similar content being viewed by others
References
Stenholm S, Harris TB, Rantanen T, Visser M, Kritchevsky SB, Ferrucci L (2008) Sarcopenic obesity: definition, cause and consequences. Curr Opin Clin Nutr Metab Care 11:693–700
Zamboni M, Mazzali G, Fantin F, Rossi A, Di Francesco V (2008) Sarcopenic obesity: a new category of obesity in the elderly. Nutr Metab Cardiovasc Dis NMCD 18:388–395
Zoico E, Di Francesco V, Guralnik JM, Mazzali G, Bortolani A, Guariento S, Sergi G, Bosello O, Zamboni M (2004) Physical disability and muscular strength in relation to obesity and different body composition indexes in a sample of healthy elderly women. Int J Obes Relat Metab Disord 28:234–241
Clynes MA, Edwards MH, Buehring B, Dennison EM, Binkley N, Cooper C (2015) Definitions of Sarcopenia: associations with previous falls and fracture in a population sample. Calcif Tissue Int 97:445–452
Janssen I, Heymsfield SB, Ross R (2002) Low relative skeletal muscle mass (sarcopenia) in older persons is associated with functional impairment and physical disability. J Am Geriatr Soc 50:889–896
Milte R, Crotty M (2014) Musculoskeletal health, frailty and functional decline. Best Pract Res Clin Rheumatol 28:395–410
Malafarina V, Uriz-Otano F, Iniesta R, Gil-Guerrero L (2012) Sarcopenia in the elderly: diagnosis, physiopathology and treatment. Maturitas 71:109–114
Batsis JA, Barre LK, Mackenzie TA, Pratt SI, Lopez-Jimenez F, Bartels SJ (2013) Variation in the prevalence of sarcopenia and sarcopenic obesity in older adults associated with different research definitions: dual-energy X-ray absorptiometry data from the National Health and Nutrition Examination Survey 1999-2004. J Am Geriatr Soc 61:974–980
Börjesson M, Hellenius ML, Jansson E, Karlson J, Leijon M, Staehle A, Sundberg CJ, Taube T (2010) Physical activity in the prevention and treatment of disease. Swedish Institute of Health, Stockholm
Pedersen BK, Saltin B (2006) Evidence for prescribing exercise as a therapy in chronic disease. Scand J Med Sci Sports 16:3–63
Goisser S, Kemmler W, Porzel S, Volkert D, Sieber CC, Bollheimer LC, Freiberger E (2015) Sarcopenic obesity and complex interventions with nutrition and exercise in community-dwelling older persons—a narrative review. Clin Interv Aging 10:1267–1282
Statistisches-Bundesamt (2006) Gesundheit in Deutschland [Health in Germany]. Gesundheitsberichterstattung des BundesBerlin
Clark DO (1999) Physical activity and its correlates among urban primary care patients aged 55 years or older. J Gerontol B Psychol Sci Soc Sci 54:S41–S48
Chodzko-Zajko WJ, Proctor DN, Fiatarone Singh MA, Minson CT, Nigg CR, Salem GJ, Skinner JS (2009) American College of Sports Medicine position stand. Exercise and physical activity for older adults. Med Sci Sports Exerc 41:1510–1530
AHHS (2008) Physical activity guidelines for Americans. Oklahoma Nurse 53:25
Kemmler W, Schliffka R, Mayhew JL, von Stengel S (2010) Effects of Whole-Body-Electromyostimulation on Resting Metabolic Rate, Anthropometric and Neuromuscular Parameters in the Elderly. The Training and ElectroStimulation Trial (TEST). J Strength Cond Res 24:1880–1886
Kemmler W, Birlauf A, von Stengel S (2010) Einfluss von Ganzkörper-Elektromyostimulation auf das Metabolische Syndrom bei älteren Männern mit metabolischem Syndrom. Dtsch Z Sportmed 61:117–123
Kemmler W, von Stengel S (2013) Whole-body electromyostimulation as a means to impact muscle mass and abdominal body fat in lean, sedentary, older female adults: subanalysis of the TEST-III trial. Clin Interv Aging 8:1353–1364
Kemmler W, Bebenek M, Engelke K, von Stengel S (2014) Impact of whole-body electromyostimulation on body composition in elderly women at risk for sarcopenia: the Training and ElectroStimulation Trial (TEST-III). Age (Dordr) 36:395–406
Cruz-Jentoft AJ, Baeyens JP, Bauer JM et al (2010) Sarcopenia: European consensus on definition and diagnosis: report of the European Working Group on sarcopenia in older people. Age Ageing 39:412–423
WHO (1995) Physical status: the use and interpretation of anthropometry. Report of a WHO expert committee. In: Organization. WH (ed) World Health Organ Tech Rep SerGeneva, pp p. 1-452
Janssen I, Baumgartner RN, Ross R, Rosenberg IH, Roubenoff R (2004) Skeletal muscle cutpoints associated with elevated physical disability risk in older men and women. Am J Epidemiol 159:413–421
Borg E, Kaijser L (2006) A comparison between three rating scales for perceived exertion and two different work tests. Scand J Med Sci Sports 16:57–69
Peters DM, Fritz SL, Krotish DE (2013) Assessing the reliability and validity of a shorter walk test compared with the 10-Meter Walk Test for measurements of gait speed in healthy, older adults. J Geriatr Phys Ther 36:24–30
Johnson JL, Slentz CA, Houmard JA, Samsa GP, Duscha BD, Aiken LB, McCartney JS, Tanner CJ, Kraus WE (2007) Exercise training amount and intensity effects on metabolic syndrome (from Studies of a Targeted Risk Reduction Intervention through Defined Exercise). Am J Cardiol 100:1759–1766
Kemmler W, Riedel H (1998) Körperliche Belastung und Osteoporose—Einfluß einer 10monatigen Interventionsmaßnahme auf ossäre und extraossäre Risikofaktoren einer Osteoporose. Dtsch Z Sportmed 49:270–277
Fahrenberg J, Myrtek M, Wilk D, Kreutel K (1986) Multimodal assessment of life satisfaction: a study of patients with cardiovascular diseases. Psychother Psychosom Med Psychol 36:347–354
Kemmler W, Weineck J, Kalender WA, Engelke K (2004) The effect of habitual physical activity, non-athletic exercise, muscle strength, and VO2max on bone mineral density is rather low in early postmenopausal osteopenic women. J Musculoskelet Neuronal Interact 4:325–334
Volkert D, Kreuel K, Heseker H, Stehle P (2004) Energy and nutrient intake of young-old, old-old and very-old elderly in Germany. Eur J Clin Nutr 58:1190–1200
Honaker J, King G, Blackwell M (2011) Amelia II: a program for missing data JSS 45:1-47
Alison P (2002) Missing data. Sage Publication, Thousand Oaks
Holm S (1979) A simple sequentially rejective multiple test procedure. Scand J Stat 6:65–70
Fielding RA, Vellas B, Evans WJ et al (2011) Sarcopenia: an undiagnosed condition in older adults. Current consensus definition: prevalence, etiology, and consequences. International working group on sarcopenia. J Am Med Dir Assoc 12:249–256
Kemmler W, Teschler M, Goisser S, Bebenek M, von Stengel S, Bollheimer LC, Sieber CC, Freiberger E (2015) Prevalence of sarcopenia in Germany and the corresponding effect of osteoarthritis in females 70 years and older living in the community: results of the FORMoSA study. Clin Interv Aging 10:1565–1573
Tieland M, Borgonjen-Van den Berg KJ, van Loon LJ, de Groot LC (2012) Dietary protein intake in community-dwelling, frail, and institutionalized elderly people: scope for improvement. Eur J Nutr 51:173–179
D-A-CH (2013) (Deutsche Gesellschaft für Ernährung): D-A-CH Referenzwerte. Referenzwerte der Nährstoffzufuhr. D-A-CH 1. Auflage, 5. korrigierter Nachdruck
WHO (2007) Protein and amino acid requirements in human nutrition: report of a joint WHO/FAO/UNU expert consultation. Geneva
Bauer J, Biolo G, Cederholm T et al (2013) Evidence-based recommendations for optimal dietary protein intake in older people: a position paper from the PROT-AGE Study Group. J Am Med Dir Assoc 14:542–559
Nowson C, O’Connell S (2015) Protein requirements and recommendations for older people: a review. Nutrients 7:6874–6899
American Dietetic A, Dietitians of C, American College of Sports M, Rodriguez NR, Di Marco NM, Langley S (2009) American College of Sports Medicine position stand. Nutrition and athletic performance. Med Sci Sports Exerc 41:709–731
Tipton KD (2008) Protein for adaptation to exercise training. EJSS 8:107–118
Peterson MD, Sen A, Gordon PM (2011) Influence of resistance exercise on lean body mass in aging adults: a meta-analysis. Med Sci Sports Exerc 43:249–258
Mavros Y, O’Neill E, Connerty M, Bean JF, Broe K, Kiel DP, Maclean D, Taylor A, Fielding RA, Singh MA (2015) Oxandrolone augmentation of resistance training in older women: a randomized trial. Med Sci Sports Exerc 47:2257–2267
Liu CJ, Latham NK (2009) Progressive resistance strength training for improving physical function in older adults. Cochrane Database Syst Rev CD002759
Lopopolo RB, Greco M, Sullivan D, Craik RL, Mangione KK (2006) Effect of therapeutic exercise on gait speed in community-dwelling elderly people: a meta-analysis. Phys Ther 86:520–540
Acknowledgments
We like to thank the “Bayerische Forschungsstiftung” (Munich, Germany) that supported the FORMOsA-Project. We further acknowledge the support of miha-bodytec (Gersthofen, Germany), Nutricia (Erlangen, Germany), and physiomed (Leipersdorf, Germany).
Trial registration number
NCT02356016 on www.clinicaltrials.gov
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
None.
Rights and permissions
About this article
Cite this article
Kemmler, W., Teschler, M., Weissenfels, A. et al. Whole-body electromyostimulation to fight sarcopenic obesity in community-dwelling older women at risk. Resultsof the randomized controlled FORMOsA-sarcopenic obesity study. Osteoporos Int 27, 3261–3270 (2016). https://doi.org/10.1007/s00198-016-3662-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00198-016-3662-z