Abstract
Objective
Circulatory shock is a life-threatening syndrome resulting in multiorgan failure and a high mortality rate. The aim of this consensus is to provide support to the bedside clinician regarding the diagnosis, management and monitoring of shock.
Methods
The European Society of Intensive Care Medicine invited 12 experts to form a Task Force to update a previous consensus (Antonelli et al.: Intensive Care Med 33:575–590, 2007). The same five questions addressed in the earlier consensus were used as the outline for the literature search and review, with the aim of the Task Force to produce statements based on the available literature and evidence. These questions were: (1) What are the epidemiologic and pathophysiologic features of shock in the intensive care unit? (2) Should we monitor preload and fluid responsiveness in shock? (3) How and when should we monitor stroke volume or cardiac output in shock? (4) What markers of the regional and microcirculation can be monitored, and how can cellular function be assessed in shock? (5) What is the evidence for using hemodynamic monitoring to direct therapy in shock? Four types of statements were used: definition, recommendation, best practice and statement of fact.
Results
Forty-four statements were made. The main new statements include: (1) statements on individualizing blood pressure targets; (2) statements on the assessment and prediction of fluid responsiveness; (3) statements on the use of echocardiography and hemodynamic monitoring.
Conclusions
This consensus provides 44 statements that can be used at the bedside to diagnose, treat and monitor patients with shock.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Guidelines for the hemodynamic management of patients with circulatory shock and their implications for management [1] were developed in 2006 by a team of 25 experts in the field of shock and a jury of 11 individuals representing five critical care societies. In these guidelines, five specific questions were addressed: (1) What are the epidemiologic and pathophysiologic features of shock in the intensive care unit (ICU)? (2) Should we monitor preload and fluid responsiveness in shock? (3) How and when should we monitor stroke volume or cardiac output in shock? (4) What markers of the regional and microcirculation can be monitored, and how can cellular function be assessed in shock? (5) What is the evidence for using hemodynamic monitoring to direct therapy in shock?
Since the publication of the 2006 guidelines [1], data from several observational and randomized clinical trials (RCTs) have been published that provide new evidence for the optimal management of patients with circulatory shock. In this paper, the term shock refers to circulatory shock.
Consensus methodology
An international team of 12 experts in the field of shock was invited by the European Society of Intensive Care Medicine to form a Task Force to evaluate new evidence and to revise the guidelines as judged appropriate. Four types of statements were used for the consensus—statements of facts, recommendations, best practice and definitions (for example, definition of shock).
Statements of facts are used to summarize an important topic discussed in the consensus when facts, rather than actions, are discussed and agreed.
Indications to act or not to act on a specific issue are written in the form of a “recommendation” or “best practice statement”. Although the formal GRADE (Grading of Recommendations Assessment, Development and Evaluation) system of evidence review with the generation of evidence profiles was not conducted, in making their recommendations the Task Force members took into account the principles of the GRADE system. This system classifies recommendations as strong (Level 1) or weak (Level 2) [2] based on the certainty of Task Force members that following given recommendation will result in more good than harm. Panelists were also aware that strength of the GRADE system recommendation depends on the quality of underlying evidence (certainty in the estimates of effects), balance of benefits and harms, costs and values and preferences of the interested parties. When the panel judged that a specific recommendation should be issued, but there was either no reasonable alternative or sufficient indirect reasoning not to commit time and resources to formal evidence review, best practice statements were issued.
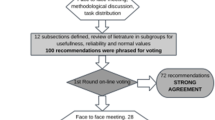
A modified Delphi approach was used to achieve consensus. For each of the five questions included in the 2006 guidelines [1], five pairs of experts of the consensus group were assigned the task of reviewing the new clinical trial data and presenting their findings at a consensus conference. During the conference, held in Brussels in March 2014, the evidence and recommendations were reviewed and discussed by the entire group and consensus reached.
A medical writer (Sophie Rushton-Smith) was present at the conference in Brussels and recorded the minutes of the discussion. These were used to complete the contributions of the authors and to draft the first version of the manuscript.
A conference call was held in August 2014. To complete the process by taking into account the latest papers published (up to 1 October 2014), members of the Task Force communicated with each other via emails and telephone conversations. The findings are presented in this report. While the same five questions of 2006 were used as the basis to search and discuss available literature, the present report has been written without retaining the order of the answers to the five questions of the 2006 consensus. This decision was based on the obvious overlap between answers to the different questions and to provide a more readable manuscript. The main differences between the 2007 report of Antonelli et al. [1] and this consensus are summarized in Tables 1 and 2. The statements issued in 2014 by the Task Force are summarized in Tables 3, 4, 5 and 6.
Definition, pathophysiology, features and epidemiology of shock
Definition
Shock is best defined as a life-threatening, generalized form of acute circulatory failure associated with inadequate oxygen utilization by the cells. It is a state in which the circulation is unable to deliver sufficient oxygen to meet the demands of the tissues, resulting in cellular dysfunction. The result is cellular dysoxia, i.e. the loss of the physiological independence between oxygen delivery and oxygen consumption, associated with increased lactate levels. Some clinical symptoms suggest an impaired microcirculation, including mottled skin, acrocyanosis, slow capillary refill time and an increased central-to-toe temperature gradient.
Pathophysiology and features of shock
Shock is a clinical state of acute circulatory failure [3] that can result from one, or a combination, of four mechanisms [4]. The first of these is a decrease in venous return due to a loss of circulating volume (i.e. due to internal or external loss of fluids). The second is a failure of the pump function of the heart that results from a loss of contractility (resulting from ischemia, infarction, myopathy, myocarditis) or a major arrhythmia (such as ventricular tachycardia or a high degree A-V block). The third is an obstruction due to pulmonary embolism, tension pneumothorax or cardiac tamponade. The fourth is loss of vascular tone that results in maldistribution of blood flow (due to sepsis, anaphylaxis or spinal injury). The features of each of these four types of shock often overlap, and patients admitted with one type of shock can develop other types of shock. For example, patients hospitalized with hemorrhagic shock due to trauma or with cardiogenic shock occasionally develop septic shock [5, 6].
Epidemiology
Up to one-third of patients admitted to the ICU are in circulatory shock [7], and early recognition of the condition is vital if subsequent tissue injuries are to be avoided. Shock can be categorized according to the underlying cause, including septic shock, cardiogenic shock, anaphylactic shock and shock associated with burns, trauma and hemorrhage. In the 1,679 ICU patients in the European Sepsis Occurrence in Acutely Ill Patients II (SOAP II) trial, septic shock was the most frequent cause of shock, accounting for 62 % of cases, followed by cardiogenic shock (17 %) and hypovolemia (16 %) [8].
Septic shock is the most severe manifestation of sepsis, with reported case-fatality rates in the range of 40–50 %, reaching as high as 80 % [9]. Limited data are available on the epidemiology of septic shock, particularly in low-income countries [9], but the literature suggests that its incidence is increasing [10–20]. The reported incidence of septic shock in patients admitted to the ICU varies between 6.3 and 14.7 % [1, 21].
Cardiogenic shock has most commonly been studied in the setting of acute myocardial infarction; the incidence in this population has remained fairly constant at between 6 and 9 %, over the past several decades [6, 22–25]. In a multinational observational study of 65,119 patients hospitalized for an acute coronary syndrome between 1999 and 2007, 4.6 % developed cardiogenic shock, and the in-hospital case-fatality rate was 59.4 % [26].
The definition, pathophysiology, features and epidemiology of shock
-
We define circulatory shock as a life-threatening, generalized form of acute circulatory failure associated with inadequate oxygen utilization by the cells. Definition.
-
As a result, there is cellular dysoxia, associated with increased blood lactate levels. Statement of fact.
-
Shock can be associated with four underlying patterns, of which three are associated with a low flow state (hypovolemic, cardiogenic, obstructive) and one is associated with a hyperkinetic state (distributive). Statement of fact.
-
Shock can be due to a combination of processes. Statement of fact.
Diagnosis of shock
General considerations
The diagnosis of acute circulatory failure is based on a combination of clinical, hemodynamic and biochemical signs. The clinical signs of shock typically include arterial hypotension (although this is not always present), associated with signs of altered tissue perfusion, visualized through the three ‘windows’ of the body [27]: the peripheral window (skin that is cold, clammy and blue, pale or discolored); the renal window (decreased urine output: <0.5 mL/kg/h); the neurologic window (altered mental characterized by obtundation, disorientation and confusion). The presence of low blood pressure should not be a prerequisite for defining shock: compensatory mechanisms may preserve blood pressure through vasoconstriction [28], while tissue perfusion and oxygenation are already decreased significantly [29].
General considerations
-
Shock is typically associated with evidence of inadequate tissue perfusion on physical examination. The three organs readily accessible to clinical assessment of tissue perfusion are the:
-
skin (degree of cutaneous perfusion);
-
kidneys (urine output);
-
brain (mental status).
-
Statement of fact.
-
We recommend routine screening of patients at risk to allow earlier identification of impending shock and implementation of therapy. Recommendation. Level 1; QoE low (C).
-
We recommend frequent measurement of heart rate, blood pressure, body temperature and physical examination variables (including signs of hypoperfusion, urine output and mental status) in patients with a history and with clinical findings suggestive of shock. Best practice.
Hypotension and shock
The diagnostic accuracy of a systolic blood pressure of <95 mmHg associated with acute blood loss was assessed by Stern et al. in a systematic evaluation of physical findings in patients with hypovolemia [30]. A random effects model produced a sensitivity of 13 % for moderate blood loss and 33 % for severe blood loss. The authors therefore concluded that a systolic blood pressure of <95 mmHg is not a sensitive measure for ruling out moderate or significant blood loss. A decrease in cardiac output is associated with significant vasoconstriction, leading to decreased peripheral perfusion to maintain arterial pressure [28]. The presence of hypotension is generally included in the diagnosis of septic shock, but several studies have actually shown that preserved blood pressure can be associated with markers of inadequate tissue perfusion, such as decreased central venous oxygen saturation (ScvO2) and significantly increased concentrations of blood lactate [31]. In addition, persistent hypotension in patients with septic shock without increased lactate levels may a have limited impact on mortality [32].
The definition of circulatory shock emerging from this consensus conference does not therefore require the presence of hypotension. Rather, the definition of shock as ‘life-threatening, generalized form of acute circulatory failure associated with inadequate oxygen utilization by the cells’ usually includes, but is not limited to, the presence of hypotension.
Hypotension and shock
-
We recommend that the presence of arterial hypotension [defined as systolic blood pressure of <90 mmHg, or mean arterial pressure (MAP) of <65 mmHg, or a decrease of ≥40 mmHg from baseline], while commonly present, should not be required to define shock. Recommendation. Level 1; QoE moderate (B).
Plasma lactate, mixed venous oxygen saturation and central venous oxygen saturation and other perfusion markers
In experimental models of acute circulatory failure induced by arterial hypoxemia, low hemoglobin levels, obstructive shock and septic shock, the onset of decreased oxygen utilization relative to oxygen demand is characterized by increasing lactate levels [33, 34] and decreased regional and microcirculatory perfusion [35, 36]. Additionally, the results of limited clinical studies have shown that inadequate oxygen is associated with increased lactate levels [37–39].
Hyperlactatemia is indeed typically present in cases of acute circulatory failure, indicating abnormal metabolism. The usual cut-off value is 2 mEq/L (or mmol/L), but lactate levels of >1.5 mmol/L in patients with septic shock are associated with increased mortality [40]. Although generally increased lactate levels are associated with abnormal oxidative phosphorylation and inadequate oxygen utilization [38, 39], other mechanisms may also increase lactate levels in the presence of adequate tissue oxygenation [41–43].
The prognostic value of lactate levels exceeds that of blood pressure [32, 44, 45]. While hyperlactatemia is associated with worse outcome in any type of shock, a correct interpretation also depends on the type of shock, i.e. septic shock versus hemorrhagic shock [46].
From a metabolic perspective, elevations in blood lactate concentration may be due to increased production, a decreased clearance or a combination of the two. As elevated plasma lactate forms part of the definition of shock, the argument to measure it as a diagnostic marker of shock is circular. Many studies have confirmed the association between initial serum lactate level and mortality independently of clinical signs of organ dysfunction in patients not only with severe sepsis [47], but also those in cardiogenic shock [48].
An early decrease in blood lactate levels may indicate the resolution of global tissue hypoxia and has been associated with a decreased mortality rate [49]. Two studies proposed ‘lactate-based management’ of ICU patients [50, 51]. Jones et al. [50] studied 300 patients, of whom more than 80 % had septic shock, who were treated to normalize central venous pressure (CVP) and MAP; additional management to normalize lactate clearance compared with management to normalize ScvO2 did not result in different rates of hospital mortality. Jansen et al. [51] showed, in patients with hyperlactatemia (>3.0 mEq/L) on ICU admission, that lactate-guided therapy (with the aim of decreasing lactate by ≥20 % every 2 h for the initial 8 h) in comparison with no lactate-guided therapy (in which the treatment team had no knowledge of lactate levels other than the admission level) reduced hospital mortality when predefined risk factors were adjusted (hazard ratio 0.61, 95 % confidence interval 0.43–0.87; P = 0.006). These authors demonstrated a reduced rate of organ failure—but no reduced mortality—in the lactate group compared with the control group in the early observation period (between 9 and 72 h). Lactate levels between the control and lactate groups were similar over a 3-day period. In clinical practice, we suggest serial measurements of lactates and/or base deficit to evaluate not only the outcome and prognosis but also to guide therapy; lactate measurements can be performed every 2 h in the first 8 h and every 8–12 h thereafter.
In the context of hyperlactatemia and mixed venous oxygen saturation (SvO2), ScvO2 can provide important information about the balance between oxygen transport and oxygen demand. For example, in the context of septic shock, low ScVO2 indicates an inadequacy of oxygen transport, especially in the context of hyperlactatemia. In patients with low ScVO2 values (<70 %), Rivers et al. showed that early goal-directed therapy (EGDT) aimed at increasing the ScVO2 to >70 % was associated to a better outcome than a different protocolized treatment not using this measurement to guide therapy [31]. In their study, the mean baseline values of ScVO2 were 49 and 48 % for the control and EGDT groups, respectively. Two recent multicenter RCTs, the ProCESS and the ARISE trials, failed to reproduce similar results. In these studies, patients had a lower mortality and higher mean baseline ScvO2 values (71 % for the ProCESS trial and 73 % for ARISE trial) [52, 53] compared to the Rivers et al. study [31]. In addition, in both the ProCESS and ARISE trials, clinicians well trained in management of septic shock and well aware of available resuscitation goals and techniques treated the control groups.
In practice, a high ScvO2 value in the context of hyperlactatemia is of limited use. One of the limitations of ScvO2 is that normal/high values cannot discriminate if the oxygen transport is adequate, as it may remain ‘blind’ to local hypoperfusion.
The venoarterial carbon dioxide difference (pCO2 gap), which measures the difference in the partial pressure of carbon dioxide (pCO2) between mixed or central venous blood and arterial blood, is a marker that can be used to identify patients who are under-resuscitated. Values of >6 mmHg suggest an insufficient blood flow in the tissues even when the ScvO2 is >70 % [54, 55].
Although all shock states are associated with systemic inflammation either early or later in the course of circulatory failure, and markers of systemic inflammation have been associated with mortality in such cases, the levels of these mediators are generally higher in septic patients [56–59]. However, even in patients with septic shock, lactate levels have a better prognostic value than other markers [60]. There is a lack of evidence that other biomarkers of an early hyper-inflammatory response (e.g. interleukin-1 receptor agonist, intercellular adhesion molecule 1, tumor necrosis factor-α, caspase 3 and interleukin-8) predict early complications, particularly in septic shock [61].
Good animal and human data are available on the role of mediators in the evolution of shock, but current outcome data do not support the routine use of these mediators as biomarkers in the diagnosis and staging of shock.
Plasma lactate, mixed venous oxygen saturation and central venous oxygen saturation and other perfusion markers
-
We recommend measuring blood lactate levels in all cases where shock is suspected. Recommendation. Level 1; QoE low (C).
-
Lactate levels are typically >2 mEq/L (or mmol/L) in shock states. Statement of fact.
-
We recommend serial measurements of blood lactate. The rationale is to guide, monitor and assess. Recommendation. Level 1; QoE low (C).
-
In patients with a central venous catheter (CVC), we suggest measurements of central venous oxygen saturation (ScvO2) and venoarterial difference in PCO2 (V-ApCO2) to help assess the underlying pattern and the adequacy of cardiac output as well as to guide therapy. Recommendation. Level 2; QoE moderate (B).
How and when to monitor cardiac function and hemodynamics in shock
The three main reasons for monitoring cardiac function in circulatory shock are for:
-
Identifying the type of shock.
-
Selecting the therapeutic intervention.
-
Evaluating the patient’s response to therapy.
Identification of the type of shock
Identifying the main mechanism responsible for shock—hypovolemic, cardiogenic, obstructive, or distributive [4, 62]––is of paramount importance. Context analysis (trauma, infection, chest pain, etc.) and clinical evaluation which focuses on skin perfusion and jugular vein distension usually orient diagnosis to the type of shock, but complex situations may exist (e.g. cardiac tamponade in a patient with trauma or septic shock in a patient with chronic heart failure) in which a diagnosis is more difficult. Hence, additional hemodynamic measurements are often needed to ascertain the type of shock, especially in complex situations or in patients with comorbidities. Distributive shock is usually characterized by an elevated cardiac output, while the other types of shock are associated with low cardiac output. Hypovolemic shock is associated with low blood pressures and volumes, while these are increased in cardiogenic shock. Obstructive shock is associated with increased pulmonary artery pressure and dilated right-sided cavities. Tamponade, a form of obstructive shock, is associated with compression of all cavities, and thus with elevated intracardiac pressures but small cardiac volumes. In general, hemodynamic variables such as CVP can be useful in identifying the type of shock. However, unless in the extreme ranges of the variables (such as a CVP of 0 mmHg in the case of a history of bleeding), they should always be interpreted together with other variables.
Evaluation of cardiac output, cardiac function and preload is essential when attempting to identify the type of shock and can be obtained using various techniques. Echocardiography allows rapid characterization of the type of shock and is now proposed as the first-line evaluation modality [4]. This information can be obtained rapidly, usually in less than 2 min, even by physicians with minimal training [63]. The situation may evolve over time, however, and repeated echocardiographic evaluations are not always feasible. Hence, a combination of echocardiography with other technologies is often warranted. Advanced hemodynamic monitoring may not be needed in non-severe episodes of shock that rapidly respond to initial therapy based on clinical evaluation and echocardiography. In cases of severe shock and in complex conditions, advanced hemodynamic monitoring is useful for identifying the factor(s) which contribute(s) most to the hemodynamic disturbances and on which therapy should focus. Continuous or semi-continuous measurements of cardiac output and/or SvO2 are particularly useful as these can be nurse driven.
Identification of the type of shock
-
We recommend efforts to identify the type of shock to better target causal and supportive therapies. Best practice.
-
We recommend further hemodynamic assessment (such as assessing cardiac function) to determine the type of shock if the clinical examination does not lead to a clear diagnosis. Best practice.
-
We suggest that, when hemodynamic assessment is needed, echocardiography is the preferred modality to initially evaluate the type of shock as opposed to more invasive technologies. Recommendation. Level 2; QoE (B).
-
We recommend not to use a single variable for the diagnosis and/or management of shock. Best Practice.
-
In complex patients we suggest to additionally use pulmonary artery catheterization or transpulmonary thermodilution to determine the type of shock. Recommendation. Level 2; QoE low (C).
Selection of the therapeutic intervention
Target for blood pressure in the management of shock
Aggressive fluid resuscitation should be avoided and hypotension tolerated in trauma patients with penetrating injury—until the bleeding is surgically stopped [64]. No equivalent guidelines are available for patients with blunt trauma. Regarding cardiogenic shock, no clinical studies have investigated the optimal blood pressure level, and guidelines no longer recommend a target blood pressure [65]. Blood pressure should be individualized for all patients. There is evidence, however, that a mean MAP of around 65 mmHg is sufficient in most patients with septic shock [51, 66–69], although in patients with a history of hypertension, a higher MAP is associated with a lower risk of acute kidney injury [70]. Therefore, clearly the arterial blood pressure level must be individualized. Vasopressors may have to be used if fluid resuscitation is not sufficient, or they may be indicated to maintain the desired value of MAP. In-dwelling arterial catheters allow continuous arterial blood pressure monitoring and at the same time allow for regular blood gas analysis. This is particularly important in patients not responding to the initial therapy. Central venous access may be required and preferred to peripheral venous access when patients admitted to the ICU require vasopressor infusions [71].
Target blood pressure in circulatory shock
-
We recommend individualizing the target blood pressure during shock resuscitation. Recommendation. Level 1; QoE moderate (B).
-
We recommend to initially target a MAP of ≥65 mmHg. Recommendation. Level 1; QoE low (C).
-
We suggest to tolerate a lower level of blood pressure in patients with uncontrolled bleeding (i.e. bleeding patients from a road traffic accident) without severe head injury. Recommendation. Level 2; QoE low (C).
-
We suggest a higher MAP in septic patients with a history of hypertension and in patients who improve with higher blood pressure. Recommendation. Level 2; QoE moderate (B).
-
We recommend arterial and CVC insertion in cases of shock unresponsive to initial therapy and/or requiring vasopressor infusion. Best practice.
Therapeutic interventions to improve perfusion
When tissue perfusion is judged inadequate, interventions aimed at improving perfusion can be considered. Vasopressors (together with fluid resuscitation) are often needed to restore blood pressure. The question then is how to select between the manipulation of preload (fluids), inotropic stimulation and modulation of afterload to improve flow and perfusion? Clinical examination is often of limited value. The detection of preload responsiveness can be achieved through the use of several different indices [72], but the presence of preload responsiveness does not imply that fluids can be administered safely or that they should be administered at all. Determination of filling pressures, measured invasively by pulmonary artery catheter (PAC) or estimated non-invasively by echocardiography, and measurements of extravascular lung water with transpulmonary thermodilution provide important information on the risks associated with fluid administration (see "Monitoring Preload and Fluid Responsiveness" for further details).
Evaluation of cardiac function is crucial when deciding on whether inotropic agents have a place in the therapy of a given patient. Cardiac function may be altered when cardiac output is normal or even when elevated, as is often the case in myocardial depression in sepsis. In a trial involving more than 200 patients with septic shock, Vieillard-Baron et al. [73] observed that several patients presented a left ventricular ejection fraction (LVEF) of close to 40 % even though their cardiac index was higher than 3 L/min/m2. Conversely, several patients had a low cardiac output but preserved cardiac function—and inotropic stimulation should not be used in these patients. In 46 patients with septic shock, Bouferrache et al. [74] observed that echocardiographic assessment of myocardial function and preload responsiveness often led to different interventions than those guided by the resuscitation goals proposed by the Surviving Sepsis Campaign (SSC) [75]. In this study, the authors found that agreement on the indication (or absence of indication) for inotropic administration occurred in 34 (74 %) of the patients, but that the evaluation of LVEF suggested the use of inotropic agents in 11 patients for whom the SSC guidelines suggested otherwise. The reverse situation occurred in only one patient. These authors therefore suggested that resuscitation should be guided by measurements of LVEF rather than by the SSC criteria. These data should, however, be interpreted with caution as no analysis of patient outcome was performed. The study simply illustrates that LVEF and oxygen saturation evaluate two different aspects of the hemodynamic state, with LVEF evaluating myocardial contractility and ScvO2 evaluating the adequacy of cardiac output according to oxygen utilization. Hence, inotropic agents should be given only when the altered cardiac function is accompanied by a low or inadequate cardiac output and signs of tissue hypoperfusion are present. The aim of the therapeutic options mentioned above is to increase oxygen delivery (DO2) to improve tissue perfusion. It therefore needs to be emphasized that the ultimate goal is the improvement of tissue perfusion—not the achievement of any specific DO2 value, which ultimately could lead to patient’s harm [76].
Therapeutic interventions to improve perfusion
-
We recommend early treatment, including hemodynamic stabilization (with fluid resuscitation and vasopressor treatment if needed) and treatment of the shock etiology. Best practice.
-
We suggest that inotropic agents should be added when the altered cardiac function is accompanied by a low or inadequate cardiac output and signs of tissue hypoperfusion persist after preload optimization. Recommendation. Level 2; QoE low (C).
-
We recommend not to give inotropes for isolated impaired cardiac function. Recommendation. Level 1; QoE moderate (B).
-
We recommend not to target absolute values of oxygen delivery in patients with shock. Recommendation. Level 1; QoE high (A).
Evaluation of response to therapy
The aim of providing hemodynamic support in cases of acute circulatory failure is often to increase cardiac output in order to improve tissue perfusion or decrease pulmonary capillary pressure. What measurements should therefore be performed to evaluate the effects of these interventions? While the ultimate goal is resolution of the signs of tissue hypoperfusion (e.g. oliguria, lactate levels), these may lack sensitivity or take time to improve.
The evaluation of cardiac output and cardiac function can be helpful in evaluating the impact of therapeutic interventions.
How can the effect of fluids be evaluated? Fluids are expected to improve the hemodynamic state by increasing stroke volume and cardiac output. Accordingly, changes in cardiac output by at least 10–15 % (to ascertain that these changes are not due to measurement variability) are used to define a positive response to fluids [77]. When cardiac output is not measured, surrogate measurements can be used, such as changes in end-tidal CO2 in mechanically ventilated patients [78, 79]. Alternatively, resolution of the signs of preload dependency indicates a positive response to fluids. Changes in arterial pressure are unpredictable [80, 81] and depend on vascular tone [82]. Even though pulse pressure is related to stroke volume, changes in pulse pressure cannot reliably predict response to fluids [81]. Of note, an increase in CVP or in end-diastolic volume only reflects the fact that preload was effectively manipulated, but these measurements are not helpful in identifying patients who experience an increase in cardiac output in response to fluid administration.
Evaluation of the response to inotropic agents in patients who do not respond to the initial therapy requires assessment of cardiac function and/or measurements of cardiac output. When present, a rise in SvO2 suggests an increase in cardiac output, but an increase can also occur with significant alterations in SvO2, especially when the SvO2 is close to the normal range and/or when oxygen consumption (VO2) concomitantly increases, which is the typical pattern of response in shock states characterized by VO2 dependency [83, 84]. Under these conditions, changes in pulse pressure also do not relate to changes in cardiac output [80].
Evaluation of response to therapy
-
We do not recommend routine measurement of cardiac output for patients with shock responding to the initial therapy. Recommendation. Level 1; QoE low (C).
-
We recommend measurements of cardiac output and stroke volume to evaluate the response to fluids or inotropes in patients that are not responding to initial therapy. Recommendation. Level 1; QoE low (C).
-
We suggest sequential evaluation of hemodynamic status during shock. Recommendation. Level 1; QoE low (C).
Monitoring preload and fluid responsiveness
Optimal fluid management is one of the cornerstones of hemodynamic management in shock. Both hypovolemia and hypervolemia are harmful states, and attempts have to be made to administer the fluids in the best possible way. Therefore, the first questions physicians should ask themselves are: (1) whether the clinical problem at hand can be (partially) resolved by increasing cardiac output and (2) whether fluid resuscitation will be effective to achieve this target.
Preload, along with afterload and cardiac contractility, is an important determinant of cardiac output. Preload has been defined as myocardial stretch imposed by ventricular filling at the end of the diastole. While fluid resuscitation should not be delayed, efforts should be made to assess if a patient will respond to fluids. Ideally, in cases of shock, a clinician should be able to use a measure of preload to determine whether a patient requires additional fluids to increase cardiac output. CVP and pulmonary artery occlusion pressure (PAOP) are the most commonly used estimates of right ventricular (RV) and LV preloads, respectively. Volumetric parameters, assessed by transpulmonary thermodilution, and end-diastolic ventricular volumes, determined by echocardiography, are also used to evaluate preload [72]. However, each of these pressure and volume measurements has their limitations. Dynamic measures of assessing whether a patient requires additional fluid to increase stroke volume (i.e. assessing fluid responsiveness) have been proposed in an effort to improve fluid management. The principle behind dynamic measures is that changes in intrathoracic pressure imposed by mechanical ventilation impact on venous return and subsequent cardiac output. During a positive pressure breath, RV filling has been shown to decrease by 20–70 %, leading to a decrease in stroke volume that can be amplified by an increasing degree of hypovolemia [85, 86]. This finding indicates that dynamic measures allow the discrimination of preload-dependent and preload-independent hemodynamic situations (i.e. these measures identify the position of a patient’s individual Frank–Starling curve). Different dynamic measures are currently available and can be routinely assessed at the bedside using standard and minimally invasive hemodynamic monitoring systems. These include the assessment of pulse pressure variation (PPV) and stroke volume variation (SVV) via the arterial line or non-invasively by plethysmography, as well as of aortic flow variation and vena cava collapsibility or distensibility determined by Doppler and other modalities of echocardiography [87–89]. The need for additional fluid may also be evaluated by observing the response to a volume challenge. Following the rapid administration of a bolus of intravenous fluid (i.e. 500 mL in <30 min) or a passive leg-raising test (which is akin to a fluid load, as venous return increases), cardiac output immediately increases in patients who are fluid-responsive [3, 77, 90].
Despite the fact that current guidelines as well as important clinical trials have used measures of preload to guide fluid resuscitation, clinicians should be cautious when using such measures. Importantly, any measure of preload, particularly if it is a one-time measurement, should not be taken out of context with respect to the measures of other variables and the patient’s overall clinical condition. For example, a normal individual with a normal vascular volume has a very low CVP and does not require additional fluid; alternatively, some patients with high measures of preload pressure may benefit from additional fluids. Thus, changes in these parameters following interventions may be much more useful than a single measurement. Unfortunately, poor correlations between estimates of preload (whether pressures or volumes) and predictions of fluid responsiveness have been widely reported. For example, in normal healthy volunteers, both CVP and PAOP are poor predictors of preload, cardiac performance and changes in cardiac performance following fluid loading compared with measurements of end-diastolic ventricular volumes. End-diastolic ventricular volumes have also been found to provide superior estimates of preload compared with CVP and PAOP in diverse groups of critically ill patients [91]. Nonetheless, there may be clinical settings, such as severe congestive heart failure or hypovolemia, where titration of fluid therapy based on CVP and PAOP may be helpful [92]. Notably, measurements of ventricular volumes are not always easy to obtain (especially on the right side of the heart), are associated with costs and time delays and are operator-dependent. A number of studies have shown that dynamic measures of fluid responsiveness are better predictors of fluid responsiveness than static parameters in mechanically ventilated patients. PPV and SVV, for example, have proven to be good predictors of fluid responsiveness in sedated mechanically ventilated patients without spontaneous breathing activities and in sinus rhythm. Dynamic measures do have several limitations, however. Importantly, patients must be on fully controlled mechanical ventilation without spontaneous efforts, which is seldom the case in ICU patients. In addition, these parameters are affected by the magnitude of the employed tidal volume. Finally, most of the evaluations involving dynamic measures have included relatively stable patients, such as post-cardiac surgery patients, and the extent to which these measures are useful in other potentially unstable populations is uncertain. Few studies evaluating measures of fluid responsiveness have specifically focused on the spontaneously breathing patient. Not surprisingly, the measurement of PPV had no predictive value in the subgroup of patients with spontaneous breathing activity [93]. However, reductions in right atrial pressures by at least 1 mmHg during a spontaneous inspiration have been shown to be a reasonable predictor of fluid responsiveness [94–96]. Passive leg-raising (e.g. 45° elevation for 4 min while maintaining the trunk supine) results in an increase in RV and LV preload. Such a test may help in predicting individual fluid responsiveness during spontaneous and positive pressure breaths while avoiding the hazards of unnecessary fluid loading [97, 98].
Monitoring preload and fluid responsiveness
-
Optimal fluid management does improve patient outcome; hypovolemia and hypervolemia are harmful. Statement of fact.
-
We recommend to assess volume status and volume responsiveness. Best practice.
-
We recommend that immediate fluid resuscitation should be started in shock states associated with very low values of commonly used preload parameters. Best practice.
-
We recommend that commonly used preload measures (such as CVP or PAOP or global end diastolic volume or global end diastolic area) alone should not be used to guide fluid resuscitation. Recommendation. Level 1; QoE moderate (B).
-
We recommend not to target any ventricular filling pressure or volume. Recommendation. Level 1; QoE moderate (B).
-
We recommend that fluid resuscitation should be guided by more than one single hemodynamic variable. Best practice.
-
We recommend using dynamic over static variables to predict fluid responsiveness, when applicable. Recommendation. Level 1; QoE moderate (B).
-
When the decision for fluid administration is made, we recommend to perform a fluid challenge, unless in cases of obvious hypovolemia (such as overt bleeding in a ruptured aneurysm). Recommendation, Level 1; QoE low (C).
-
We recommend that even in the context of fluid-responsive patients, fluid management should be titrated carefully, especially in the presence of elevated intravascular filling pressures or extravascular lung water. Best practice.
Monitoring cardiac function and cardiac output
Echocardiography
Echocardiography cannot provide continuous hemodynamic data. Nevertheless, it is the best bedside method to assess cardiac function repeatedly. Echocardiography can help the ICU physician in three ways: (1) better characterization of the hemodynamic disorders; (2) selection of the best therapeutic options (intravenous fluids, inotropes and ultrafiltration); (3) assessment of the response of the hemodynamic disorders to therapy.
Doppler echocardiography provides an estimation of stroke volume and hence cardiac output using the calculation of the velocity–time integral (VTI) of the subaortic blood flow and the area of the duct crossed by this flow. Since the area of the subaortic tract does not change over time, it is sufficient to follow short-term changes in VTI in order to assess changes in stroke volume.
Doppler echocardiography provides measurements of LVEF, which depends mainly on LV contractility and LV afterload. Thus, LVEF is not a precise marker of LV contractility but rather reflects the way the heart is able to adapt to the actual loading conditions with its intrinsic contractility. This is particularly important in shock patients in whom LV afterload can change markedly over a short period. Therefore, the LVEF must be correctly interpreted to take into account the systolic arterial pressure. Visual estimation of LVEF provides values very close to those measured by the orthogonal plan method [99], and this measurement can be obtained by most ICU physicians, even those who are moderately experienced with echocardiography [100].
LV filling pressures are best evaluated using analysis of the transmitral flow with pulsed Doppler echocardiography and the tissue Doppler imaging of the mitral annulus [101]. Analysis of transmitral flow allows measurement of the peak Doppler velocities of early (E) and late diastolic flow (A). The E/A ratio has been proposed as an estimation of the LV filling pressure [102], but this measurement is affected by diastolic function. Early diastolic mitral annular velocity (E′) measured with tissue Doppler imaging evaluates diastolic function in a load-independent manner [103]. The combination of tissue Doppler imaging and pulsed Doppler echocardiography of transmitral flow allows calculation of the E/E′ ratio, which is considered to be one of the best echocardiographic estimates of LV filling pressure [103, 104]. However, echocardiography provides only a semi-quantitative estimate of LV filling pressures. Although an E/E′ value of <8 is a good predictor of low LV filling pressure and an E/E′ value of >15 is a good predictor of high LV filling pressure, a value between 8 and 15 cannot reliably predict the LV filling pressure [105]. This is not a minor issue as most E/E′ values are between 8 and 15 in critically ill patients [104, 106].
Echocardiography also provides dynamic parameters of preload responsiveness through analysis of the respiratory variability of VTI [88] or the inferior or superior vena cava diameter [88, 107] or through the response of VTI to passive leg-raising [98, 108].
Doppler echocardiography provides an estimation of RV function through comparison of the RV end-diastolic area (RVEDA) with the LV end-diastolic area (LVEDA). A RVEDA/LVEDA ratio of between 0.6 and 1 suggests the presence of moderate RV dilatation, and a ratio >1 suggests the presence of severe RV dilatation. Some authors have defined acute cor pulmonale as the combination of a RVEDA/LVEDA ratio >0.6 and the presence of a paradoxical septal motion [109–111].
Pulmonary artery catheter
The PAC provides the ICU physician with information on important hemodynamic variables [e.g. right atrial pressure, pulmonary artery pressure (PAP), PAOP and cardiac output) and tissue perfusion variables (e.g. SvO2, oxygen utilization, oxygen delivery, oxygen extraction and PvCO2]. All of these variables can be useful in the management of patients with shock.
Right atrial pressure and PAP are particularly useful for managing patients with shock associated with RV dysfunction and/or acute respiratory distress syndrome (ARDS). PAOP is assumed to reflect the LV end-diastolic pressure. Correct measurements and appropriate interpretation of PAOP represent a difficult challenge, especially in patients receiving positive end-expiratory pressure (PEEP) [112, 113] or in the presence of intrinsic PEEP [113], where the measured PAOP overestimates the transmural PAOP.
Cardiac output can be measured intermittently according to the thermodilution principle after cold bolus injections. This is classically considered as the reference method, although it suffers from a number of methodological limitations, such as tricuspid regurgitation. The semi-continuous thermodilution method is based on the intermittent and automatic heating of blood by means of a proximal thermal filament and the recording of the temperature changes using a distal thermistor. The results obtained with continuous thermodilution agree with those provided by the intermittent technique, except for high values of cardiac output, which can be underestimated by the continuous method [114]. This technique presents the advantage of a continuous display of cardiac output and avoids repeated manipulations of the catheters and bolus injections. The major limitation is that it does not enable real-time monitoring of cardiac output as it averages several successive cardiac output measurements.
The PAC can also provide intermittent or continuous measurements of SvO2 and intermittent measurements of PvCO2; both variables are helpful in assessing the adequacy of the cardiac output for oxygen (O2) utilization and for the clearance of carbon dioxide (CO2) produced by cellular metabolism.
The main limitation of the PAC is its invasiveness, which explains in part the decline in its use during the past decade when less invasive hemodynamic techniques have been developed. Nevertheless, the PAC can still be helpful for the management of shock states refractory to the initial treatment, especially those with RV dysfunction or with complex circulatory conditions in which the knowledge of PAP, PAOP and oxygenation parameters is believed to be important for identifying the main disorders. Monitoring with a PAC is commonplace in the ICU setting despite the lack of high-quality data to support its benefits [115]. While the availability of cardiac output and other hemodynamic variables obtained using a PAC can improve the diagnosis and management of circulatory instability, the device can also cause complications and provide inaccurate measurements, and the data can be difficult to interpret [116].
Published evidence on the use of PACs in the ICU is conflicting, with some early non-randomized trials suggesting increased rates of mortality and morbidity and longer hospital stays. The results of a prospective study with propensity-matched groups showed that patients receiving a PAC had a higher rate of 30-day death, higher hospital costs and increased duration of ICU stay compared with patients who did not receive a PAC [116]. Analysis of data from an observational study in over 4,000 patients undergoing non-cardiac surgery revealed an increase in the rate of postoperative major cardiac and non-cardiac complications in those who underwent perioperative right heart catheterization [117]. In contrast, two recent studies, both of which used propensity scores to account for illness severity, reported similar outcomes in critically ill patients with or without a PAC [118, 119]. In a retrospective study of 119 consecutive patients with ARDS, monitoring with a PAC was not an independent predictor of death [120].
The impact of PAC on mortality and morbidity in critically ill patients has also been reported in several, more recent RCTs [121–124]. One study involving 201 patients reported no difference in mortality related to PAC use, but more fluids were given in the first 24 h to the PAC group, and the rates of acute renal failure and thrombocytopenia 3 days after randomization were greater in this group [121]. Similarly, in 676 patients with shock and/or ARDS, the use of a PAC did not significantly improve morbidity or reduce mortality [122]. Harvey et al. reported that they found no evidence of benefit or harm with the use of a PAC in a study of 1,041 ICU patients [123]. Wheeler et al. conducted a randomized trial in 1,000 patients with ARDS or acute lung injury with the aim of comparing hemodynamic management guided by PAC and by CVC [124]. These authors reported that there were no differences in 60-day mortality, time on the ventilator or days spent in the ICU, but the PAC group did have a higher rate of catheter-related complications, largely arrhythmias [124]. Shah et al., in a meta-analysis of the efficacy and safety of the PAC in 5,051 critically ill patients (13 RCTs) [125], reported that the use of a PAC was not associated with an increased rate of death or length of hospitalization, but the results also failed to demonstrate improved survival associated with PAC use.
Transpulmonary thermodilution devices
Transpulmonary thermodilution devices are considered to be less invasive than the PAC, but they still require insertion of a CVC and femoral arterial catheter. These devices combine transpulmonary thermodilution and pulse contour analysis.
Transpulmonary thermodilution provides intermittent measurements of cardiac output after a cold bolus injection into a central vein and detection of changes in the blood temperature in the femoral artery. The technique has been compared favorably with pulmonary thermodilution in critically ill patients, including some in shock [126]. Transpulmonary thermodilution also provides intermittent measurements of: (1) global end-diastolic volume, a volumetric marker of cardiac preload; (2) cardiac function index, a marker of systolic function of the heart; (3) extravascular lung water, a quantitative index of pulmonary edema.
Arterial pulse wave analysis measures cardiac output by placing sensors placed directly into the femoral artery catheter which record the arterial pressure waveform through the femoral artery catheter. Determination of pulse contour cardiac output uses proprietary algorithms based on the relationship between stroke volume and arterial pressure waveform, which is influenced by the resistive and elastic characteristics of the arterial system. Intermittent transpulmonary thermodilution cardiac output measurements are used to calibrate the pulse contour cardiac output, and good agreement with thermodilution cardiac output has been reported in hemodynamically unstable patients [127]. However, there is a potential drift with time, making recalibration mandatory. After a 1-h calibration-free period, recalibration may be encouraged in patients with septic shock who are receiving vasopressors [128].
The clinical interest for such real-time cardiac output monitoring is to improve diagnostics so that patients in whom cardiac output is dropping can be identified early and to be able to follow the short-term changes in cardiac output during dynamic tests or therapeutic challenges. Because such devices provide numerous important hemodynamic variables, transpulmonary thermodilution can be helpful in patients with shock refractory to initial treatment and especially in cases of associated ARDS because of the assessment of extravascular lung water.
Lithium dilution monitor
This system uses the lithium dilution method to calibrate an arterial waveform analysis system. The technique has been validated against pulmonary artery thermodilution in humans [129], and agreement remains acceptable for up to 4 h after calibration in critically ill patients [130]. The system needs a lithium bolus injection for its calibration. The best calibrations are achieved, as is true for any intermittent technique, by averaging more measurements (i.e. 2–3 boluses) [131]. The device can be used to measure and track cardiac output continuously in patients with shock. In complex patients it has the limitation of measuring fewer hemodynamic variables than the PAC and the transpulmonary thermodilution systems.
Uncalibrated arterial pulse contour analysis monitors
Several devices provide real-time cardiac output measurements by deriving the arterial pressure waveform recorded from an artery catheter (radial or femoral). These devices use proprietary algorithms that analyze the characteristics of the arterial pressure waveform and use this analysis, along with patient-specific demographic information, to determine continuous cardiac output and PPV and/or SVV. A theoretical advantage is that these devices can be used with a radial artery catheter and do not need calibration. However, the reliability of uncalibrated devices is still debated in the case of shock, particularly septic shock [132–134]. More importantly, the fact that these devices do not provide important variables, such as filling pressures or transpulmonary thermodilution variables (global end-diastolic volume, extravascular lung water, etc.), represents a disadvantage compared with PAC or transpulmonary thermodilution devices.
Recently developed systems use the pulse contour analysis and the volume clamp method to monitor cardiac output in real-time using an inflatable cuff wrapped around a finger connected to a monitor. This non-invasive method should be used during the perioperative period. However, the value of this technique in the context of shock patients and/or patients receiving vasopressors is questionable, as confirmed by results from clinical studies which showed no agreement with thermodilution cardiac output [135] or velocity time integral [136] for estimating either absolute values of cardiac output or for tracking changes in cardiac output during therapy. In addition, patients with shock often need an arterial catheter for their routine management.
Esophageal Doppler
The use of esophageal Doppler is aimed at monitoring cardiac output by continuously measuring the blood flow in the descending thoracic aorta. This method takes advantage of the anatomical proximity of the thoracic descending aorta and the esophagus. With this technique, a flexible probe of small diameter is introduced into the esophagus. The tip of the probe is equipped with a Doppler transducer that records the velocity of red blood cells passing into the descending thoracic aorta. To obtain flow from velocity measurements, the diameter of the descending aorta must be taken into account.
Most commercialized devices do not measure the aortic diameter, but rather they estimate it from nomograms based on the patient’s height, weight and age. With these devices, the aortic diameter is thus considered to be a constant in a particular patient. In patients with shock receiving resuscitation, this assumption represents an important limitation of using such devices because the aortic diameter depends on the transmural aortic pressure, such that changes in MAP result in changes in aortic diameter [137]. A practical limitation of the technique is that the probe moves easily into the esophagus when the patient is moving. Thus, continuous monitoring of cardiac output requires frequent replacement of the probe. Esophageal Doppler is more suitable for the operating theater than for the ICU. Unfortunately, esophageal Doppler can only provide blood flow measurements, which limits its potential for hemodynamic monitoring in the context of shock in comparison with other monitoring devices, such as the PAC or transpulmonary thermodilution.
Bioreactance
Bioreactance is a non-invasive technique used for monitoring cardiac output in real-time which uses skin surface electrodes placed on the patient’s chest and neck that apply a low-amplitude, high-frequency electrical current which traverses the thorax. The signal is recorded by other electrodes on the skin surface, with a time delay called a phase shift. The underlying scientific rationale is that the higher the cardiac stroke volume, the more significant these phase shifts become. In critically ill patients, including those with shock, a poor agreement between thermodilution cardiac output and bioreactance cardiac output has been reported in two studies [138, 139].
Monitoring cardiac function and cardiac output
-
Echocardiography can be used for the sequential evaluation of cardiac function in shock Statement of fact.
-
We do not recommend the routine use of the pulmonary artery catheter for patients in shock. Recommendation. Level 1; QoE high (A).
-
We suggest PAC in patients with refractory shock and RV dysfunction. Recommendation. Level 2; QoE low (C).
-
We suggest the use of transpulmonary thermodilution or PAC in patients with severe shock especially in the case of associated acute respiratory distress syndrome. Recommendation. Level 2; QoE low (C).
-
We recommend that less invasive devices are used, instead of more invasive devices, only when they have been validated in the context of patients with shock. Best practice.
Monitoring the microcirculation
Several techniques are available to evaluate the microcirculation in critically ill patients. These show some relation between altered microcirculation and poor outcome. In experimental conditions, shock states have been associated with a decrease in perfused capillary density and an increase in the heterogeneity of microcirculatory perfusion, with non-perfused capillaries in close vicinity to perfused capillaries [140].
The use of metabolic parameters for the assessment of regional microcirculatory perfusion is promising. Tissue CO2 represents the balance between local production and removal; thus, a rising value likely reflects a decrease in local blood flow rather than an increased local production of CO2. When associated with arterial CO2, tissue CO2 allows determination of the gradient or the PCO2 gap, which is inversely related to the proportion of perfused capillaries [141]. An occlusion test with near-infrared spectroscopy may help to evaluate indirectly the dynamic response of the microcirculation to an occlusion, even if the link between vasoreactivity, microcirculation and tissue oxygenation is still not clearly established. The evaluation of StO2 [tissue (muscle) oxygen saturation] changes in response to a vascular occlusion test provides two additional parameters: the StO2-deoxygenation rate (DeOx), which has been related to the local metabolic rate and local blood flow distribution, and the StO2-reoxygenation rate (ReOx). In a population of septic shock patients with restored MAP, decrements in DeOx and ReOx were found to be associated with a longer ICU stay, and impaired DeOx was associated with no improvement in organ failures after 24 h [142]. The ReOx rate seen on reperfusion is an measure of both the limb’s oxygen content and the capacity to recruit arterioles and venules (‘microvascular reserve’) [143].
Microvideoscopic techniques, such as orthogonal polarization spectral and sidestream dark field imaging, can directly evaluate microvascular networks covered by a thin epithelium, such as the sublingual microcirculation. They take into account the heterogeneity of microvascular perfusion. The following parameters have been suggested [144]: (1) a measure of vessel density (total or perfused vessel density); (2) two indices of vascular perfusion (proportion of perfused vessels and microcirculatory flow index); (3) a flow heterogeneity index. These indices evaluate how many vessels are perfused, the quality of the flow and whether non-perfused areas are located next to well-perfused areas. Using these techniques, microvascular alterations, similar to those reported in experimental conditions, have been observed in patients with septic [145], cardiogenic [146], and hemorrhagic [147] shock.
One goal of the management of patients with shock within the first hours after admission is to ensure adequate tissue perfusion and cellular metabolism. In a prospective observational study, early improvement in microvascular perfusion in response to goal-directed therapy was associated with an improvement in organ function [148]. These data strongly suggest that microcirculatory alterations are implicated in the development of organ failure. In a randomized, double-blind, crossover study by Hernandez et al. [149] in patients with pressor-dependent septic shock and hyperlactatemia, increasing oxygen delivery for 90 min by infusion of dobutamine did not alter lactate clearance, regional flow (measured by gastric tonometry PCO2) or microcirculatory flow (measured by sublingual imaging
The use of microcirculatory markers of tissue perfusion will require further large-scale studies to assess their potential benefit in microcirculation-oriented or microcirculation-guided management and/or therapy of early shock resuscitation. In summary, these techniques need further exploration and are not presently recommended as targets for resuscitation.
Monitoring microcirculation
-
We suggest the techniques to assess regional circulation or microcirculation for research purposes only. Recommendation. Level 2; QoE low (C).
Notes
Refers also to the statements related to ‘general considerations’ and ‘plasma lactate, mixed venous oxygen saturation and central venous oxygen saturation and other perfusion markers’ discussed in the section "Diagnosis of shock")
References
Antonelli M, Levy M, Andrews PJ, Chastre J, Hudson LD, Manthous C, Meduri GU, Moreno RP, Putensen C, Stewart T, Torres A (2007) Hemodynamic monitoring in shock and implications for management. International Consensus Conference, Paris, France, 27-28 April 2006. Intensive Care Med 33:575–590
Atkins D, Best D, Briss PA, Eccles M, Falck-Ytter Y, Flottorp S, Guyatt GH, Harbour RT, Haugh MC, Henry D, Hill S, Jaeschke R, Leng G, Liberati A, Magrini N, Mason J, Middleton P, Mrukowicz J, O’Connell D, Oxman AD, Phillips B, Schunemann HJ, Edejer T, Varonen H, Vist GE, Williams JW Jr, Zaza S, Grade Working Group (2004) Grading quality of evidence and strength of recommendations. BMJ 328:1490
Weil MH, Henning RJ (1979) New concepts in the diagnosis and fluid treatment of circulatory shock. Thirteenth annual Becton, Dickinson and Company Oscar Schwidetsky Memorial Lecture. Anesth Analg 58:124–132
Vincent JL, De Backer D (2013) Circulatory shock. N Eng J Med 369:1726–1734
Schulman AM, Claridge JA, Carr G, Diesen DL, Young JS (2004) Predictors of patients who will develop prolonged occult hypoperfusion following blunt trauma. J Trauma 57:795–800
Babaev A, Frederick PD, Pasta DJ, Every N, Sichrovsky T, Hochman JS, Investigators N (2005) Trends in management and outcomes of patients with acute myocardial infarction complicated by cardiogenic shock. JAMA 294:448–454
Sakr Y, Reinhart K, Vincent JL, Sprung CL, Moreno R, Ranieri VM, De Backer D, Payen D (2006) Does dopamine administration in shock influence outcome? Results of the Sepsis Occurrence in Acutely Ill Patients (SOAP) Study. Crit Care Med 34:589–597
De Backer D, Biston P, Devriendt J, Madl C, Chochrad D, Aldecoa C, Brasseur A, Defrance P, Gottignies P, Vincent JL (2010) Comparison of dopamine and norepinephrine in the treatment of shock. N Eng J Med 362:779–789
Jawad I, Luksic I, Rafnsson SB (2012) Assessing available information on the burden of sepsis: global estimates of incidence, prevalence and mortality. J Glob Health 2:010404
Brun-Buisson C, Doyon F, Carlet J, Dellamonica P, Gouin F, Lepoutre A, Mercier JC, Offenstadt G, Regnier B (1995) Incidence, risk factors, and outcome of severe sepsis and septic shock in adults. A multicenter prospective study in intensive care units. French ICU Group for Severe Sepsis. JAMA 274:968–974
Salvo I, de Cian W, Musicco M, Langer M, Piadena R, Wolfler A, Montani C, Magni E (1995) The Italian SEPSIS study: preliminary results on the incidence and evolution of SIRS, sepsis, severe sepsis and septic shock. Intensive Care Med 21[Suppl 2]:S244–S249
Brun-Buisson C, Doyon F, Carlet J (1996) Bacteremia and severe sepsis in adults: a multicenter prospective survey in ICUs and wards of 24 hospitals. French Bacteremia-Sepsis Study Group. Am J Respir Crit Care Med 154:617–624
Alberti C, Brun-Buisson C, Burchardi H, Martin C, Goodman S, Artigas A, Sicignano A, Palazzo M, Moreno R, Boulme R, Lepage E, Le Gall R (2002) Epidemiology of sepsis and infection in ICU patients from an international multicentre cohort study. Intensive Care Med 28:108–121
Annane D, Aegerter P, Jars-Guincestre MC, Guidet B, Network CU-R (2003) Current epidemiology of septic shock: the CUB-Rea Network. Am J Respir Crit Care Med 168:165–172
Flaatten H (2004) Epidemiology of sepsis in Norway in 1999. Crit Care 8:R180–R184
Linde-Zwirble WT, Angus DC (2004) Severe sepsis epidemiology: sampling, selection, and society. Crit Care 8:222–226
Brun-Buisson C, Meshaka P, Pinton P, Vallet B, Group ES (2004) EPISEPSIS: a reappraisal of the epidemiology and outcome of severe sepsis in French intensive care units. Intensive Care Med 30:580–588
Silva E, Pedro Mde A, Sogayar AC, Mohovic T, Silva CL, Janiszewski M, Cal RG, de Sousa EF, Abe TP, de Andrade J, de Matos JD, Rezende E, Assuncao M, Avezum A, Rocha PC, de Matos GF, Bento AM, Correa AD, Vieira PC, Knobel E, Brazilian Sepsis Epidemiological S (2004) Brazilian Sepsis Epidemiological Study (BASES study). Crit Care 8:R251–R260
van Gestel A, Bakker J, Veraart CP, van Hout BA (2004) Prevalence and incidence of severe sepsis in Dutch intensive care units. Crit Care 8:R153–R162
Vincent JL, Sakr Y, Sprung CL, Ranieri VM, Reinhart K, Gerlach H, Moreno R, Carlet J, Le Gall JR, Payen D, Sepsis Occurrence in Acutely Ill Patients I (2006) Sepsis in European intensive care units: results of the SOAP study. Crit Care Med 34:344–353
Quenot JP, Binquet C, Kara F, Martinet O, Ganster F, Navellou JC, Castelain V, Barraud D, Cousson J, Louis G, Perez P, Kuteifan K, Noirot A, Badie J, Mezher C, Lessire H, Pavon A (2013) The epidemiology of septic shock in French intensive care units: the prospective multicenter cohort EPISS study. Crit Care 17:R65
Goldberg RJ, Gore JM, Thompson CA, Gurwitz JH (2001) Recent magnitude of and temporal trends (1994-1997) in the incidence and hospital death rates of cardiogenic shock complicating acute myocardial infarction: the second national registry of myocardial infarction. Am Heart J 141:65–72
Goldberg RJ, Samad NA, Yarzebski J, Gurwitz J, Bigelow C, Gore JM (1999) Temporal trends in cardiogenic shock complicating acute myocardial infarction. N Eng J Med 340:1162–1168
Hands ME, Rutherford JD, Muller JE, Davies G, Stone PH, Parker C, Braunwald E, The MILIS Study Group (1989) The in-hospital development of cardiogenic shock after myocardial infarction: incidence, predictors of occurrence, outcome and prognostic factors. Journal of the American College of Cardiology 14:40–46 discussion 47-48
Holmes DR Jr, Bates ER, Kleiman NS, Sadowski Z, Horgan JH, Morris DC, Califf RM, Berger PB, Topol EJ (1995) Contemporary reperfusion therapy for cardiogenic shock: the GUSTO-I trial experience. The GUSTO-I Investigators. Global Utilization of Streptokinase and Tissue Plasminogen Activator for Occluded Coronary Arteries. J Am Coll Cardiol 26:668–674
Awad HH, Anderson FA Jr, Gore JM, Goodman SG, Goldberg RJ (2012) Cardiogenic shock complicating acute coronary syndromes: insights from the Global Registry of Acute Coronary Events. Am Heart J 163:963–971
Vincent JL, Ince C, Bakker J (2012) Clinical review: circulatory shock—an update: a tribute to Professor Max Harry Weil. Crit Care 16:239
van Genderen ME, Bartels SA, Lima A, Bezemer R, Ince C, Bakker J, van Bommel J (2013) Peripheral perfusion index as an early predictor for central hypovolemia in awake healthy volunteers. Anesth Analg 116:351–356
Soller BR, Ryan KL, Rickards CA, Cooke WH, Yang Y, Soyemi OO, Crookes BA, Heard SO, Convertino VA (2008) Oxygen saturation determined from deep muscle, not thenar tissue, is an early indicator of central hypovolemia in humans. Crit Care Med 36:176–182
Stern SA, Dronen SC, Birrer P, Wang X (1993) Effect of blood pressure on hemorrhage volume and survival in a near-fatal hemorrhage model incorporating a vascular injury. Ann Emerg Med 22:155–163
Rivers E, Nguyen B, Havstad S, Ressler J, Muzzin A, Knoblich B, Peterson E, Tomlanovich M (2001) Early goal-directed therapy in the treatment of severe sepsis and septic shock. N Eng J Med 345:1368–1377
Hernandez G, Castro R, Romero C, de la Hoz C, Angulo D, Aranguiz I, Larrondo J, Bujes A, Bruhn A(2011) Persistent sepsis-induced hypotension without hyperlactatemia: Is it really septic shock? J Crit Care 26:435.e9–14
Cain SM (1965) Appearance of excess lactate in aneshetized dogs during anemic and hypoxic hypoxia. Am J Physiol 209:604–608
Zhang H, Spapen H, Benlabed M, Vincent JL (1993) Systemic oxygen extraction can be improved during repeated episodes of cardiac tamponade. J Crit Care 8:93–99
Zhang H, Smail N, Cabral A, Cherkaoui S, Peny MO, Vincent JL (1999) Hepato-splanchnic blood flow and oxygen extraction capabilities during experimental tamponade: effects of endotoxin. J Surg Res 81:129–138
van Genderen ME, Klijn E, Lima A, de Jonge J, Sleeswijk Visser S, Voorbeijtel J, Bakker J, van Bommel J (2014) Microvascular perfusion as a target for fluid resuscitation in experimental circulatory shock*. Crit Care Med 42:e96–e105
Ronco JJ, Fenwick JC, Tweeddale MG, Wiggs BR, Phang PT, Cooper DJ, Cunningham KF, Russell JA, Walley KR (1993) Identification of the critical oxygen delivery for anaerobic metabolism in critically ill septic and nonseptic humans. JAMA 270:1724–1730
Bakker J, Vincent J-L (1991) The oxygen supply dependency phenomenon is associated with increased blood lactate levels. J Crit Care 6:152–159
Friedman G, De Backer D, Shahla M, Vincent JL (1998) Oxygen supply dependency can characterize septic shock. Intensive Care Med 24:118–123
Wacharasint P, Nakada TA, Boyd JH, Russell JA, Walley KR (2012) Normal-range blood lactate concentration in septic shock is prognostic and predictive. Shock 38:4–10
Jansen TC, van Bommel J, Bakker J (2009) Blood lactate monitoring in critically ill patients: a systematic health technology assessment. Crit Care Med 37:2827–2839
Hotchkiss RS, Karl IE (1992) Reevaluation of the role of cellular hypoxia and bioenergetic failure in sepsis. JAMA 267:1503–1510
Bakker J, Nijsten MW, Jansen TC (2013) Clinical use of lactate monitoring in critically ill patients. Ann Intensive care 3:12
Jansen TC, van Bommel J, Mulder PG, Rommes JH, Schieveld SJ, Bakker J (2008) The prognostic value of blood lactate levels relative to that of vital signs in the pre-hospital setting: a pilot study. Crit Care 12:R160
Howell M, Donnino M, Clardy P, Talmor D, Shapiro N (2007) Occult hypoperfusion and mortality in patients with suspected infection. Intensive Care Med 33(11):1892–1899
Jansen TC, van Bommel J, Mulder PG, Lima AP, van der Hoven B, Rommes JH, Snellen FT, Bakker J (2009) Prognostic value of blood lactate levels: does the clinical diagnosis at admission matter? J Trauma 66:377–385
Mikkelsen ME, Miltiades AN, Gaieski DF, Goyal M, Fuchs BD, Shah CV, Bellamy SL, Christie JD (2009) Serum lactate is associated with mortality in severe sepsis independent of organ failure and shock. Crit Care Med 37:1670–1677
Revelly JP, Tappy L, Martinez A, Bollmann M, Cayeux MC, Berger MM, Chiolero RL (2005) Lactate and glucose metabolism in severe sepsis and cardiogenic shock. Crit Care Med 33:2235–2240
Nguyen HB, Rivers EP, Knoblich BP, Jacobsen G, Muzzin A, Ressler JA, Tomlanovich MC (2004) Early lactate clearance is associated with improved outcome in severe sepsis and septic shock. Crit Care Med 32:1637–1642
Jones AE, Shapiro NI, Trzeciak S, Arnold RC, Claremont HA, Kline JA, Emergency Medicine Shock Research Network I (2010) Lactate clearance vs central venous oxygen saturation as goals of early sepsis therapy: a randomized clinical trial. JAMA 303:739–746
Jansen TC, van Bommel J, Schoonderbeek FJ, Sleeswijk Visser SJ, van der Klooster JM, Lima AP, Willemsen SP, Bakker J (2010) Early lactate-guided therapy in intensive care unit patients: a multicenter, open-label, randomized controlled trial. Am J Respir Crit Care Med 182:752–761
Pro CI, Yealy DM, Kellum JA, Huang DT, Barnato AE, Weissfeld LA, Pike F, Terndrup T, Wang HE, Hou PC, LoVecchio F, Filbin MR, Shapiro NI, Angus DC (2014) A randomized trial of protocol-based care for early septic shock. N Eng J Med 370:1683–1693
The ARISE Investigators and the ANZICS Clinical Trials Group (2014) Goal-directed resuscitation for patients with early septic shock. N Eng J Med 371:1496–1506
Vallet B, Pinsky MR, Cecconi M (2013) Resuscitation of patients with septic shock: please “mind the gap”! Intensive Care Med 39:1653–1655
Vallee F, Vallet B, Mathe O, Parraguette J, Mari A, Silva S, Samii K, Fourcade O, Genestal M (2008) Central venous-to-arterial carbon dioxide difference: an additional target for goal-directed therapy in septic shock? Intensive Care Med 34:2218–2225
de Werra I, Jaccard C, Corradin SB, Chiolero R, Yersin B, Gallati H, Assicot M, Bohuon C, Baumgartner JD, Glauser MP, Heumann D (1997) Cytokines, nitrite/nitrate, soluble tumor necrosis factor receptors, and procalcitonin concentrations: comparisons in patients with septic shock, cardiogenic shock, and bacterial pneumonia. Crit Care Med 25:607–613
Geppert A, Steiner A, Zorn G, Delle-Karth G, Koreny M, Haumer M, Siostrzonek P, Huber K, Heinz G (2002) Multiple organ failure in patients with cardiogenic shock is associated with high plasma levels of interleukin-6. Crit Care Med 30:1987–1994
Pinsky MR, Vincent JL, Deviere J, Alegre M, Kahn RJ, Dupont E (1993) Serum cytokine levels in human septic shock. Relation to multiple-system organ failure and mortality. Chest 103:565–575
Wanner GA, Keel M, Steckholzer U, Beier W, Stocker R, Ertel W (2000) Relationship between procalcitonin plasma levels and severity of injury, sepsis, organ failure, and mortality in injured patients. Crit Care Med 28:950–957
Marecaux G, Pinsky MR, Dupont E, Kahn RJ, Vincent JL (1996) Blood lactate levels are better prognostic indicators than TNF and IL-6 levels in patients with septic shock. Intensive Care Med 22:404–408
Rivers EP, Jaehne AK, Nguyen HB, Papamatheakis DG, Singer D, Yang JJ, Brown S, Klausner H (2013) Early biomarker activity in severe sepsis and septic shock and a contemporary review of immunotherapy trials: not a time to give up, but to give it earlier. Shock 39:127–137
Weil MH, Shubin H (1971) Proposed reclassification of shock states with special reference to distributive defects. Adv Exp Med Biol 23:13–23
Beraud AS, Rizk NW, Pearl RG, Liang DH, Patterson AJ (2013) Focused transthoracic echocardiography during critical care medicine training: curriculum implementation and evaluation of proficiency*. Crit Care Med 41:e179–e181
Bickell WH, Wall MJ, Pepe PE, Martin RR, Ginger VF, Allen MK, Mattox KL (1994) Immediate versus delayed fluid resuscitation for hypotensive patients with penetrating torso injuries. N Eng J Med 331:1105–1109
O’Gara PT, Kushner FG, Ascheim DD, Casey DE Jr, Chung MK, de Lemos JA, Ettinger SM, Fang JC, Fesmire FM, Franklin BA, Granger CB, Krumholz HM, Linderbaum JA, Morrow DA, Newby LK, Ornato JP, Ou N, Radford MJ, Tamis-Holland JE, Tommaso CL, Tracy CM, Woo YJ, Zhao DX, Anderson JL, Jacobs AK, Halperin JL, Albert NM, Brindis RG, Creager MA, DeMets D, Guyton RA, Hochman JS, Kovacs RJ, Kushner FG, Ohman EM, Stevenson WG, Yancy CW, American College of Cardiology Foundation, American Heart Association Task Force on Practice G (2013) 2013 ACCF/AHA guideline for the management of ST-elevation myocardial infarction: a report of the American College of Cardiology Foundation/American Heart Association Task Force on Practice Guidelines. Circulation 127:e362–e425
LeDoux D, Astiz ME, Carpati CM, Rackow EC (2000) Effects of perfusion pressure on tissue perfusion in septic shock. Crit Care Med 28:2729–2732
Bourgoin A, Leone M, Delmas A, Garnier F, Albanese J, Martin C (2005) Increasing mean arterial pressure in patients with septic shock: effects on oxygen variables and renal function. Crit Care Med 33:780–786
Dubin A, Pozo MO, Casabella CA, Palizas F Jr, Murias G, Moseinco MC, Kanoore Edul VS, Palizas F, Estenssoro E, Ince C (2009) Increasing arterial blood pressure with norepinephrine does not improve microcirculatory blood flow: a prospective study. Crit Care 13:R92
Asfar P, Meziani F, Hamel JF, Grelon F, Megarbane B, Anguel N, Mira JP, Dequin PF, Gergaud S, Weiss N, Legay F, Le Tulzo Y, Conrad M, Robert R, Gonzalez F, Guitton C, Tamion F, Tonnelier JM, Guezennec P, Van Der Linden T, Vieillard-Baron A, Mariotte E, Pradel G, Lesieur O, Ricard JD, Herve F, du Cheyron D, Guerin C, Mercat A, Teboul JL, Radermacher P, for the SEPSISPAM Investigators (2014) High versus low blood-pressure target in patients with septic shock. N Eng J Med 370:1583–1593
Asfar P, Teboul JL, Radermacher P (2014) High versus low blood-pressure target in septic shock. N Eng J Med 371:283–284
Ricard JD, Salomon L, Boyer A, Thiery G, Meybeck A, Roy C, Pasquet B, Le Miere E, Dreyfuss D (2013) Central or peripheral catheters for initial venous access of ICU patients: a randomized controlled trial. Crit Care Med 41:2108–2115
Marik PE, Monnet X, Teboul JL (2011) Hemodynamic parameters to guide fluid therapy. Ann Intensive Care 1:1
Vieillard-Baron A, Prin S, Chergui K, Dubourg O, Jardin F (2003) Hemodynamic instability in sepsis: bedside assessment by Doppler echocardiography. Am J Respir Crit Care Med 168:1270–1276
Bouferrache K, Amiel JB, Chimot L, Caille V, Charron C, Vignon P, Vieillard-Baron A (2012) Initial resuscitation guided by the Surviving Sepsis Campaign recommendations and early echocardiographic assessment of hemodynamics in intensive care unit septic patients: a pilot study. Crit Care Med 40:2821–2827
Dellinger RP, Levy MM, Rhodes A, Annane D, Gerlach H, Opal SM, Sevransky JE, Sprung CL, Douglas IS, Jaeschke R, Osborn TM, Nunnally ME, Townsend SR, Reinhart K, Kleinpell RM, Angus DC, Deutschman CS, Machado FR, Rubenfeld GD, Webb S, Beale RJ, Vincent JL, Moreno R, Surviving sepsis Campaign Guidelines Committee including The Pediatric Subgroup (2013) Surviving Sepsis Campaign: international guidelines for management of severe sepsis and septic shock, 2012. Intensive Care Med 39:165–228
Hayes MA, Timmins AC, Yau EH, Palazzo M, Hinds CJ, Watson D (1994) Elevation of systemic oxygen delivery in the treatment of critically ill patients. N Eng J Med 330:1717–1722
Cecconi M, Parsons AK, Rhodes A (2011) What is a fluid challenge? Curr Opin Crit Care 17:290–295
Monge Garcia MI, Gil Cano A, Gracia Romero M, Monterroso Pintado R, Perez Madueno V, Diaz Monrove JC (2012) Non-invasive assessment of fluid responsiveness by changes in partial end-tidal CO2 pressure during a passive leg-raising maneuver. Ann Intensive Care 2:9
Monnet X, Teboul JL (2013) End-tidal carbon dioxide and arterial pressure for predicting volume responsiveness by the passive leg raising test: reply to Piagnerelli and Biston. Intensive Care Med 39:1165
Monnet X, Letierce A, Hamzaoui O, Chemla D, Anguel N, Osman D, Richard C, Teboul JL (2011) Arterial pressure allows monitoring the changes in cardiac output induced by volume expansion but not by norepinephrine. Crit Care Med 39:1394–1399
Pierrakos C, Velissaris D, Scolletta S, Heenen S, De Backer D, Vincent JL (2012) Can changes in arterial pressure be used to detect changes in cardiac index during fluid challenge in patients with septic shock? Intensive Care Med 38:422–428
Monge Garcia MI, Gil Cano A, Gracia Romero M (2011) Dynamic arterial elastance to predict arterial pressure response to volume loading in preload-dependent patients. Crit Care 15:R15
Vincent JL, Roman A, De Backer D, Kahn RJ (1990) Oxygen uptake/supply dependency. Effects of short-term dobutamine infusion. Am Rev Respir Dis 142:2–7
Monnet X, Julien F, Ait-Hamou N, Lequoy M, Gosset C, Jozwiak M, Persichini R, Anguel N, Richard C, Teboul JL (2013) Lactate and venoarterial carbon dioxide difference/arterial-venous oxygen difference ratio, but not central venous oxygen saturation, predict increase in oxygen consumption in fluid responders. Crit Care Med 41:1412–1420
Perel A, Pizov R, Cotev S (1987) Systolic blood pressure variation is a sensitive indicator of hypovelemia in ventilated dogs subjected to graded hemorrhage. Anesthesiology 67:498–502
Perel A, Pizov R, Cotev S (2014) Respiratory variations in the arterial pressure during mechanical ventilation reflect volume status and fluid responsiveness. Intensive Care Med 40:798–807
Michard F, Chemla D, Richard C, Wysocki M, Pinsky M, Lecarpentier Y, Teboul J-L (1999) Clinical use of respiratory changes in arterial pulse pressure to monitor the hemodynamic effects of PEEP. Am J Respir Crit Care Med 159:935–939
Feissel M, Michard F, Mangin I, Ruyer O, Faller JP, Teboul JL (2001) Respiratory changes in aortic blood velocity as an indicator of fluid responsiveness in ventilated patients with septic shock. Chest 119:867–873
Cannesson M, Besnard C, Durand P, Bohe J, Jacques D (2005) Relation between respiratory variations in pulse oximetry plethysmographic waveform amplitude and arterial pulse pressure in ventilated patients. Crit Care 9:R562–R568
Vincent JL, Weil MH (2006) Fluid challenge revisited. Crit Care Med 34:1333–1337
Michard F, Alaya S, Zarka V, Bahloul M, Richard C, Teboul JL (2003) Global end-diastolic volume as an indicator of cardiac preload in patients with septic shock. Chest 124:1900–1908
Magder S (1998) More respect for the CVP. Int Care Med 24:651–653
Heenen S, De Backer D, Vincent J (2006) How can the response to volume expansion in patients with spontaneous respiratory movements be predicted? Crit Care 10:R102
Magder S, Georgiadis G, Cheong T (1992) Respiratory variations in right atrial pressure predict response to fluid challenge. J Crit Care 7:76–85
Magder S (2004) Clinical usefulness of respiratory variations in arterial pressure. Am J Resp Crit Care Med 169:151–155
Magder S, Lagonidis D, Erice F (2002) The use of respiratory variations in right atrial pressure to predict the cardiac output response to PEEP. J Crit Care 16:108–114
Monnet X, Rienzo M, Osman D, Anguel N, Richard C, Pinsky M, Teboul J (2006) Passive leg raising predicts fluid responsiveness in the critically ill. Crit Care Med 34:1402–1407
Lamia B, Ochagavia A, Monnet X, Chemla D, Richard C, Teboul JL (2007) Echocardiographic prediction of volume responsiveness in critically ill patients with spontaneously breathing activity. Intensive Care Med 33:1125–1132
McGowan JH, Cleland JG (2003) Reliability of reporting left ventricular systolic function by echocardiography: a systematic review of 3 methods. Am Heart J 146:388–397
Cholley BP, Vieillard-Baron A, Mebazaa A (2006) Echocardiography in the ICU: time for widespread use! Intensive Care Med 32:9–10
Vignon P, AitHssain A, Francois B, Preux PM, Pichon N, Clavel M, Frat JP, Gastinne H (2008) Echocardiographic assessment of pulmonary artery occlusion pressure in ventilated patients: a transoesophageal study. Crit Care 12:R18
Vanoverschelde JL, Robert AR, Gerbaux A, Michel X, Hanet C, Wijns W (1995) Noninvasive estimation of pulmonary arterial wedge pressure with Doppler transmitral flow velocity pattern in patients with known heart disease. Am J Cardiol 75:383–389
Nagueh SF, Middleton KJ, Kopelen HA, Zoghbi WA, Quinones MA (1997) Doppler tissue imaging: a noninvasive technique for evaluation of left ventricular relaxation and estimation of filling pressures. J Am Coll Cardiol 30:1527–1533
Bouhemad B, Nicolas-Robin A, Benois A, Lemaire S, Goarin JP, Rouby JJ (2003) Echocardiographic Doppler assessment of pulmonary capillary wedge pressure in surgical patients with postoperative circulatory shock and acute lung injury. Anesthesiology 98:1091–1100
Ommen SR, Nishimura RA, Appleton CP, Miller FA, Oh JK, Redfield MM, Tajik AJ (2000) Clinical utility of Doppler echocardiography and tissue Doppler imaging in the estimation of left ventricular filling pressures: a comparative simultaneous Doppler-catheterization study. Circulation 102:1788–1794
Combes A, Arnoult F, Trouillet JL (2004) Tissue Doppler imaging estimation of pulmonary artery occlusion pressure in ICU patients. Intensive Care Med 30:75–81
Vieillard-Baron A, Chergui K, Rabiller A, Peyrouset O, Page B, Beauchet A, Jardin F (2004) Superior vena caval collapsibility as a gauge of volume status in ventilated septic patients. Intensive Care Med 30:1734–1739
Maizel J, Airapetian N, Lorne E, Tribouilloy C, Massy Z, Slama M (2007) Diagnosis of central hypovolemia by using passive leg raising. Intensive Care Med 33:1133–1138
Vieillard-Baron A, Schmitt JM, Augarde R, Fellahi JL, Prin S, Page B, Beauchet A, Jardin F (2001) Acute cor pulmonale in acute respiratory distress syndrome submitted to protective ventilation: incidence, clinical implications, and prognosis. Crit Care Med 29:1551–1555
Boissier F, Katsahian S, Razazi K, Thille AW, Roche-Campo F, Leon R, Vivier E, Brochard L, Vieillard-Baron A, Brun-Buisson C, Mekontso Dessap A (2013) Prevalence and prognosis of cor pulmonale during protective ventilation for acute respiratory distress syndrome. Intensive Care Med 39:1725–1733
Lheritier G, Legras A, Caille A, Lherm T, Mathonnet A, Frat JP, Courte A, Martin-Lefevre L, Gouello JP, Amiel JB, Garot D, Vignon P (2013) Prevalence and prognostic value of acute cor pulmonale and patent foramen ovale in ventilated patients with early acute respiratory distress syndrome: a multicenter study. Intensive Care Med 39:1734–1742
Pinsky M, Vincent JL, De Smet JM (1991) Estimating left ventricular filling pressure during positive end-expiratory pressure in humans. Am Rev Respir Dis 143:25–31
Teboul JL, Pinsky MR, Mercat A, Anguel N, Bernardin G, Achard JM, Boulain T, Richard C (2000) Estimating cardiac filling pressure in mechanically ventilated patients with hyperinflation. Crit Care Med 28:3631–3636
Jacquet L, Hanique G, Glorieux D, Matte P, Goenen M (1996) Analysis of the accuracy of continuous thermodilution cardiac output measurement. Comparison with intermittent thermodilution and Fick cardiac output measurement. Intensive Care Med 22:1125–1129
Hall JB (2005) Searching for evidence to support pulmonary artery catheter use in critically ill patients. JAMA 294:1693–1694
Connors AF Jr, Speroff T, Dawson NV, Thomas C, Harrell FE Jr, Wagner D, Desbiens N, Goldman L, Wu AW, Califf RM, Fulkerson WJ Jr, Vidaillet H, Broste S, Bellamy P, Lynn J, Knaus WA (1996) The effectiveness of right heart catheterization in the initial care of critically ill patients. SUPPORT Investigators. JAMA 276:889–897
Polanczyk CA, Rohde LE, Goldman L, Cook EF, Thomas EJ, Marcantonio ER, Mangione CM, Lee TH (2001) Right heart catheterization and cardiac complications in patients undergoing noncardiac surgery: an observational study. JAMA 286:309–314
Murdoch SD, Cohen AT, Bellamy MC (2000) Pulmonary artery catheterization and mortality in critically ill patients. Br J Anaesth 85:611–615
Sakr Y, Vincent JL, Reinhart K, Payen D, Wiedermann CJ, Zandstra DF, Sprung CL (2005) Sepsis Occurrence in Acutely Ill Patients I. Use of the pulmonary artery catheter is not associated with worse outcome in the ICU. Chest 128:2722–2731
Vieillard-Baron A, Girou E, Valente E, Brun-Buisson C, Jardin F, Lemaire F, Brochard L (2000) Predictors of mortality in acute respiratory distress syndrome. Focus on the role of right heart catheterization. Am J Respir Crit Care Med 161:1597–1601
Rhodes A, Cusack RJ, Newman PJ, Grounds RM, Bennett ED (2002) A randomised, controlled trial of the pulmonary artery catheter in critically ill patients. Intensive Care Med 28:256–264
Richard C, Warszawski J, Anguel N, Deye N, Combes A, Barnoud D, Boulain T, Lefort Y, Fartoukh M, Baud F, Boyer A, Brochard L, Teboul JL; French Pulmonary Artery Catheter Study G (2003) Early use of the pulmonary artery catheter and outcomes in patients with shock and acute respiratory distress syndrome: a randomized controlled trial. JAMA 290:2713–2720
Harvey S, Harrison DA, Singer M, Ashcroft J, Jones CM, Elbourne D, Brampton W, Williams D, Young D, Rowan K, Collaboration PA-Ms (2005) Assessment of the clinical effectiveness of pulmonary artery catheters in management of patients in intensive care (PAC-Man): a randomised controlled trial. Lancet 366:472–477
The National Heart, Lung, and Blood Institute Acute Respiratory Distress Syndrome (ARDS) Clinical Trials Network, Wheeler AP, Bernard GR, Thompson BT, Schoenfeld D, Wiedemann HP, deBoisblanc B, Connors AF Jr, Hite RD, Harabin AL (2006) Pulmonary-artery versus central venous catheter to guide treatment of acute lung injury. N Eng J Med 354:2213–2224
Shah MR, Hasselblad V, Stevenson LW, Binanay C, O’Connor CM, Sopko G, Califf RM (2005) Impact of the pulmonary artery catheter in critically ill patients: meta-analysis of randomized clinical trials. JAMA 294:1664–1670
Sakka SG, Reinhart K, Meier-Hellmann A (1999) Comparison of pulmonary artery and arterial thermodilution cardiac output in critically ill patients. Intensive Care Med 25:843–846
Godje O, Friedl R, Hannekum A (2001) Accuracy of beat-to-beat cardiac output monitoring by pulse contour analysis in hemodynamical unstable patients. Med Sci Monit 7:1344–1350
Hamzaoui O, Monnet X, Richard C, Osman D, Chemla D, Teboul JL (2008) Effects of changes in vascular tone on the agreement between pulse contour and transpulmonary thermodilution cardiac output measurements within an up to 6-hour calibration-free period. Crit Care Med 36:434–440
Linton RA, Band DM, Haire KM (1993) A new method of measuring cardiac output in man using lithium dilution. Br J Anaesth 71:262–266
Cecconi M, Fawcett J, Grounds RM, Rhodes A (2008) A prospective study to evaluate the accuracy of pulse power analysis to monitor cardiac output in critically ill patients. BMC Anesthesiol 8:3
Cecconi M, Dawson D, Grounds RM, Rhodes A (2009) Lithium dilution cardiac output measurement in the critically ill patient: determination of precision of the technique. Intensive Care Med 35:498–504
De Backer D, Marx G, Tan A, Junker C, Van Nuffelen M, Huter L, Ching W, Michard F, Vincent JL (2011) Arterial pressure-based cardiac output monitoring: a multicenter validation of the third-generation software in septic patients. Intensive Care Med 37:233–240
Monnet X, Anguel N, Jozwiak M, Richard C, Teboul JL (2012) Third-generation FloTrac/Vigileo does not reliably track changes in cardiac output induced by norepinephrine in critically ill patients. Br J Anaesth 108:615–622
Marque S, Gros A, Chimot L, Gacouin A, Lavoue S, Camus C, Le Tulzo Y (2013) Cardiac output monitoring in septic shock: evaluation of the third-generation Flotrac-Vigileo. J Clin Monit Comput 27:273–279
Monnet X, Picard F, Lidzborski E, Mesnil M, Duranteau J, Richard C, Teboul JL (2012) The estimation of cardiac output by the Nexfin device is of poor reliability for tracking the effects of a fluid challenge. Crit Care 16:R212
Taton O, Fagnoul D, De Backer D, Vincent JL (2013) Evaluation of cardiac output in intensive care using a non-invasive arterial pulse contour technique (Nexfin((R))) compared with echocardiography. Anaesthesia 68:917–923
Monnet X, Chemla D, Osman D, Anguel N, Richard C, Pinsky MR, Teboul JL (2007) Measuring aortic diameter improves accuracy of esophageal Doppler in assessing fluid responsiveness. Crit Care Med 35:477–482
Fagnoul D, Vincent JL, Backer DD (2012) Cardiac output measurements using the bioreactance technique in critically ill patients. Crit Care 16:460
Kupersztych-Hagege E, Teboul JL, Artigas A, Talbot A, Sabatier C, Richard C, Monnet X (2013) Bioreactance is not reliable for estimating cardiac output and the effects of passive leg raising in critically ill patients. Br J Anaesth 111:961–966
Edul VS, Enrico C, Laviolle B, Vazquez AR, Ince C, Dubin A (2012) Quantitative assessment of the microcirculation in healthy volunteers and in patients with septic shock. Crit Care Med 40:1443–1448
Creteur J, De Backer D, Sakr Y, Koch M, Vincent JL (2006) Sublingual capnometry tracks microcirculatory changes in septic patients. Intensive Care Med 32:516–523
Mesquida J, Espinal C, Gruartmoner G, Masip J, Sabatier C, Baigorri F, Pinsky MR, Artigas A (2012) Prognostic implications of tissue oxygen saturation in human septic shock. Intensive Care Med 38:592–597
Ekbal NJ, Dyson A, Black C, Singer M (2013) Monitoring tissue perfusion, oxygenation, and metabolism in critically ill patients. Chest 143:1799–1808
De Backer D, Hollenberg S, Boerma C, Goedhart P, Buchele G, Ospina-Tascon G, Dobbe I, Ince C (2007) How to evaluate the microcirculation: report of a round table conference. Crit Care 11:R101
De Backer D, Creteur J, Preiser JC, Dubois MJ, Vincent JL (2002) Microvascular blood flow is altered in patients with sepsis. Am J Respir Crit Care Med 166:98–104
De Backer D, Creteur J, Dubois MJ, Sakr Y, Vincent JL (2004) Microvascular alterations in patients with acute severe heart failure and cardiogenic shock. Am Heart J 147:91–99
Tachon G, Harrois A, Tanaka S, Kato H, Huet O, Pottecher J, Vicaut E, Duranteau J (2014) Microcirculatory alterations in traumatic hemorrhagic shock. Crit Care Med 42:1433–1441
Trzeciak S, McCoy JV, Dellinger RP, Arnold RC, Rizzuto M, Abate NL, Shapiro NI, Parrillo JE, Hollenberg SM (2008) Early increases in microcirculatory perfusion during protocol-directed resuscitation are associated with reduced multi-organ failure at 24 h in patients with sepsis. Intensive Care Med 34:2210–2217
Hernandez G, Bruhn A, Luengo C, Regueira T, Kattan E, Fuentealba A, Florez J, Castro R, Aquevedo A, Pairumani R, McNab P, Ince C (2013) Effects of dobutamine on systemic, regional and microcirculatory perfusion parameters in septic shock: a randomized, placebo-controlled, double-blind, crossover study. Intensive Care Med 39:1435–1443
Acknowledgments
Prof Alexandre Mebazaa acknowledges the contribution of Anais Caillard for the literature search. Prof Roman Jaeschke acknowledges Bram Rochwerg and Waleed Alhazzani for their help in reviewing the statements in view of the literature and the GRADE system.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and the source are credited.
About this article
Cite this article
Cecconi, M., De Backer, D., Antonelli, M. et al. Consensus on circulatory shock and hemodynamic monitoring. Task force of the European Society of Intensive Care Medicine. Intensive Care Med 40, 1795–1815 (2014). https://doi.org/10.1007/s00134-014-3525-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00134-014-3525-z