Abstract
Purpose
Attention-deficit/hyperactivity disorder (ADHD), conduct disorder (CD), and oppositional defiant disorder (ODD) are common externalizing disorders of childhood. The common effects of these disorders on substance abuse need further investigation. The current study investigated the joint clusters of childhood/adolescence ADHD, CD, and ODD, and their influence on substance abuse/dependence in a population-based sample of adults.
Methods
The data were drawn from the PsyCoLaus study (n = 3,720) conducted in Lausanne, Switzerland. The population-based sample included 238 subjects meeting criteria for ADHD/ODD/CD diagnoses before the age of 15. Latent class analyses (LCA) were performed to derive comorbidity subtypes, which were subsequently characterized with respect to psychosocial correlates and substance use.
Results
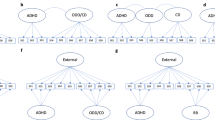
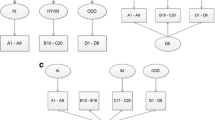
The best fit in LCAs was achieved with three latent classes: an ADHD subtype (35.7 %); an externalizing multimorbid subtype (33.6 %) involving ODD, ADHD, and CD; and a third subtype with CD (30.7 %). The CD subtype showed the highest association with substance use. Apart from this, the externalizing multimorbid subtype was also significantly linked to substance use. The ADHD subtype had only elevated frequencies for alcohol dependence in comparison with subjects that had no history of ADHD, ODD, and CD during childhood or adolescence. Finally, important interactions between subtypes and sex were observed with regard to substance use.
Conclusions
This study provides evidence showing that subtyping the externalizing disorders, ADHD, ODD and CD, along their comorbidity patterns leads to important differences regarding substance use. This could have implications for the etiology, prevention, and treatment of substance use disorders.

Similar content being viewed by others
References
Castellanos FX, Tannock R (2002) Neuroscience of attention-deficit/hyperactivity disorder: the search for endophenotypes. Nat Rev Neurosci 3(8):617–628. doi:10.1038/nrn896
Feldman HM, Reiff MI (2014) Clinical practice. Attention deficit-hyperactivity disorder in children and adolescents. N Engl J Med 370(9):838–846. doi:10.1056/NEJMcp1307215
Flory K, Lynam DR (2003) The relation between attention deficit hyperactivity disorder and substance abuse: what role does conduct disorder play? Clin Child Fam Psychol Rev 6(1):1–16
Charach A, Yeung E, Climans T, Lillie E (2011) Childhood attention-deficit/hyperactivity disorder and future substance use disorders: comparative meta-analyses. J Am Acad Child Adolesc Psychiatry 50(1):9–21. doi:10.1016/j.jaac.2010.09.019
Sihvola E, Rose RJ, Dick DM, Korhonen T, Pulkkinen L, Raevuori A, Marttunen M, Kaprio J (2011) Prospective relationships of ADHD symptoms with developing substance use in a population-derived sample. Psychol Med 41(12):2615–2623. doi:10.1017/S0033291711000791
De Sanctis VA, Trampush JW, Harty SC, Marks DJ, Newcorn JH, Miller CJ, Halperin JM (2008) Childhood maltreatment and conduct disorder: independent predictors of adolescent substance use disorders in youth with attention deficit/hyperactivity disorder. J Clin Child Adolesc Psychol 37(4):785–793. doi:10.1080/15374410802359650
Kollins SH, McClernon FJ, Fuemmeler BF (2005) Association between smoking and attention-deficit/hyperactivity disorder symptoms in a population-based sample of young adults. Arch Gen Psychiatry 62(10):1142–1147. doi:10.1001/archpsyc.62.10.1142
Elkins IJ, McGue M, Iacono WG (2007) Prospective effects of attention-deficit/hyperactivity disorder, conduct disorder, and sex on adolescent substance use and abuse. Arch Gen Psychiatry 64(10):1145–1152. doi:10.1001/archpsyc.64.10.1145
Molina BS, Pelham WE Jr (2003) Childhood predictors of adolescent substance use in a longitudinal study of children with ADHD. J Abnorm Psychol 112(3):497–507
Szobot CM, Rohde LA, Bukstein O, Molina BS, Martins C, Ruaro P, Pechansky F (2007) Is attention-deficit/hyperactivity disorder associated with illicit substance use disorders in male adolescents? A community-based case-control study. Addiction 102(7):1122–1130. doi:10.1111/j.1360-0443.2007.01850.x
Serra-Pinheiro MA, Coutinho ES, Souza IS, Pinna C, Fortes D, Araujo C, Szobot CM, Rohde LA, Mattos P (2012) Is ADHD a risk factor independent of conduct disorder for illicit substance use? A meta-analysis and metaregression investigation. J Atten Disord 17(6):459–469. doi:10.1177/1087054711435362
Disney ER, Elkins IJ, McGue M, Iacono WG (1999) Effects of ADHD, conduct disorder, and gender on substance use and abuse in adolescence. Am J Psychiatry 156(10):1515–1521
Acosta MT, Castellanos FX, Bolton KL, Balog JZ, Eagen P, Nee L, Jones J, Palacio L, Sarampote C, Russell HF, Berg K, Arcos-Burgos M, Muenke M (2008) Latent class subtyping of attention-deficit/hyperactivity disorder and comorbid conditions. J Am Acad Child Adolesc Psychiatry 47(7):797–807. doi:10.1097/CHI.0b013e318173f70b
Hicks BM, Krueger RF, Iacono WG, McGue M, Patrick CJ (2004) Family transmission and heritability of externalizing disorders: a twin-family study. Arch Gen Psychiatry 61(9):922–928. doi:10.1001/archpsyc.61.9.922
Coolidge FL, Thede LL, Young SE (2000) Heritability and the comorbidity of attention deficit hyperactivity disorder with behavioral disorders and executive function deficits: a preliminary investigation. Dev Neuropsychol 17(3):273–287. doi:10.1207/S15326942DN1703_1
Jain M, Palacio LG, Castellanos FX, Palacio JD, Pineda D, Restrepo MI, Munoz JF, Lopera F, Wallis D, Berg K, Bailey-Wilson JE, Arcos-Burgos M, Muenke M (2007) Attention-deficit/hyperactivity disorder and comorbid disruptive behavior disorders: evidence of pleiotropy and new susceptibility loci. Biol Psychiatry 61(12):1329–1339. doi:10.1016/j.biopsych.2006.06.026
Vidal SI, Vandeleur C, Rothen S, Gholam-Rezaee M, Castelao E, Halfon O, Aubry JM, Ferrero F, Preisig M (2012) Risk of mental disorders in children of parents with alcohol or heroin dependence: a controlled high-risk study. Eur Addict Res 18(5):253–264. doi:10.1159/000337328
Preisig M, Waeber G, Vollenweider P, Bovet P, Rothen S, Vandeleur C, Guex P, Middleton L, Waterworth D, Mooser V, Tozzi F, Muglia P (2009) The PsyCoLaus study: methodology and characteristics of the sample of a population-based survey on psychiatric disorders and their association with genetic and cardiovascular risk factors. BMC Psychiatry 9:9. doi:10.1186/1471-244X-9-9
Firmann M, Mayor V, Vidal PM, Bochud M, Pecoud A, Hayoz D, Paccaud F, Preisig M, Song KS, Yuan X, Danoff TM, Stirnadel HA, Waterworth D, Mooser V, Waeber G, Vollenweider P (2008) The CoLaus study: a population-based study to investigate the epidemiology and genetic determinants of cardiovascular risk factors and metabolic syndrome. BMC Cardiovasc Disord 8:6. doi:10.1186/1471-2261-8-6
Preisig M, Fenton BT, Matthey ML, Berney A, Ferrero F (1999) Diagnostic interview for genetic studies (DIGS): inter-rater and test–retest reliability of the French version. Eur Arch Psychiatry Clin Neurosci 249(4):174–179
Nurnberger JI Jr, Blehar MC, Kaufmann CA, York-Cooler C, Simpson SG, Harkavy-Friedman J, Severe JB, Malaspina D, Reich T (1994) Diagnostic interview for genetic studies. Rationale, unique features, and training. NIMH genetics initiative. Arch Gen Psychiatry 51(11):849–859 (discussion 863–844)
Berney A, Preisig M, Matthey ML, Ferrero F, Fenton BT (2002) Diagnostic interview for genetic studies (DIGS): inter-rater and test–retest reliability of alcohol and drug diagnoses. Drug Alcohol Depend 65(2):149–158
Endicott J, Spitzer RL (1978) A diagnostic interview: the schedule for affective disorders and schizophrenia. Arch Gen Psychiatry 35(7):837–844
Orvaschel H, Puig-Antich J, Chambers W, Tabrizi MA, Johnson R (1982) Retrospective assessment of prepubertal major depression with the Kiddie-SADS-e. J Am Acad Child Psychiatry 21(4):392–397
Lubke GH, Muthén B (2005) Investigating population heterogeneity with factor mixture models. Psychol Methods 10(1):21–39. doi:10.1037/1082-989X.10.1.21
Akaike H (1987) Factor analysis and AIC. Psychometrika 52(3):317–332
Schwarz G (1978) Estimating the dimension of a model. Ann Stat 6:461–464
Sclove SL (1987) Application of model-selection criteria to some problems in multivariate analysis. Psychometrika 52:333–343
Vuong QH (1989) Likelihood ratio tests for model selection and non-nested hypotheses. Econometrica 57:307–333
Lo Y, Mendell NR, Rubin DB (2001) Testing the number of components in a normal mixture. Biometrika 88(3):767–778
Nylund KL, Asparouhov T, Muthén BO (2007) Deciding on the number of classes in latent class analysis and growth mixture modeling: a monte carlo simulation study. Struct Equ Model 14(4):535–569
Muthén B (2004) Latent variable analysis: growth mixture modeling and related techniques for longitudinal data. In: Kaplan D (ed) Handbook of quantitative methodology for the social sciences. Sage Publications, Newbury Park, pp 345–368
Muthén LK, Muthén BO (1998–2012) Mplus user’s guide. 7th edn. Muthén&Muthén, Los Angeles
Biederman J, Wilens TE, Mick E, Faraone SV, Spencer T (1998) Does attention-deficit hyperactivity disorder impact the developmental course of drug and alcohol abuse and dependence? Biol Psychiatry 44(4):269–273
Ohlmeier MD, Peters K, Te Wildt BT, Zedler M, Ziegenbein M, Wiese B, Emrich HM, Schneider U (2008) Comorbidity of alcohol and substance dependence with attention-deficit/hyperactivity disorder (ADHD). Alcohol Alcohol 43(3):300–304. doi:10.1093/alcalc/agn014
Maxwell A (2013) Are some individuals diagnosed with ADHD prone to alcohol abuse? Consideration of two possible mediating factors for this susceptibility. J Atten Disord 17(2):98–101. doi:10.1177/1087054711427400
Molina BS, Pelham WE, Cheong J, Marshal MP, Gnagy EM, Curran PJ (2012) Childhood attention-deficit/hyperactivity disorder (ADHD) and growth in adolescent alcohol use: the roles of functional impairments, ADHD symptom persistence, and parental knowledge. J Abnorm Psychol 121(4):922–935. doi:10.1037/a0028260
Knop J, Penick EC, Nickel EJ, Mortensen EL, Sullivan MA, Murtaza S, Jensen P, Manzardo AM, Gabrielli WF Jr (2009) Childhood ADHD and conduct disorder as independent predictors of male alcohol dependence at age 40. J Stud Alcohol Drugs 70(2):169–177
Cumyn L, French L, Hechtman L (2009) Comorbidity in adults with attention-deficit hyperactivity disorder. Can J Psychiatry 54(10):673–683
Mannuzza S, Klein RG, Bonagura N, Malloy P, Giampino TL, Addalli KA (1991) Hyperactive boys almost grown up. V. Replication of psychiatric status. Arch Gen Psychiatry 48(1):77–83
Barkley RA, Fischer M, Smallish L, Fletcher K (2004) Young adult follow-up of hyperactive children: antisocial activities and drug use. J Child Psychol Psychiatry 45(2):195–211
Arcos-Burgos M, Velez JI, Solomon BD, Muenke M (2012) A common genetic network underlies substance use disorders and disruptive or externalizing disorders. Hum Genet 131(6):917–929. doi:10.1007/s00439-012-1164-4
Burke JD, Loeber R, Lahey BB (2001) Which aspects of ADHD are associated with tobacco use in early adolescence? J Child Psychol Psychiatry 42(4):493–502
Lee SS, Hinshaw SP (2006) Predictors of adolescent functioning in girls with attention deficit hyperactivity disorder (ADHD): the role of childhood ADHD, conduct problems, and peer status. J Clin Child Adolesc Psychol 35(3):356–368. doi:10.1207/s15374424jccp3503_2
Vonmoos M, Hulka LM, Preller KH, Jenni D, Schulz C, Baumgartner MR, Quednow BB (2013) Differences in self-reported and behavioral measures of impulsivity in recreational and dependent cocaine users. Drug Alcohol Depend 133(1):61–70. doi:10.1016/j.drugalcdep.2013.05.032
Germano E, Gagliano A, Curatolo P (2010) Comorbidity of ADHD and dyslexia. Dev Neuropsychol 35(5):475–493. doi:10.1080/87565641.2010.494748
Bellak L, Black RB (1992) Attention-deficit hyperactivity disorder in adults. Clin Ther 14(2):138–147
Ganelin-Cohen E, Ashkenasi A (2013) Disordered sleep in pediatric patients with attention deficit hyperactivity disorder: an overview. Isr Med Assoc J 15(11):705–709
Couwenbergh C, van den Brink W, Zwart K, Vreugdenhil C, van Wijngaarden-Cremers P, van der Gaag RJ (2006) Comorbid psychopathology in adolescents and young adults treated for substance use disorders: a review. Eur Child Adolesc Psychiatry 15(6):319–328. doi:10.1007/s00787-006-0535-6
Carpentier PJ, Knapen LJ, van Gogh MT, Buitelaar JK, De Jong CA (2012) Addiction in developmental perspective: influence of conduct disorder severity, subtype, and attention-deficit hyperactivity disorder on problem severity and comorbidity in adults with opioid dependence. J Addict Dis 31(1):45–59. doi:10.1080/10550887.2011.642756
Button TM, Rhee SH, Hewitt JK, Young SE, Corley RP, Stallings MC (2007) The role of conduct disorder in explaining the comorbidity between alcohol and illicit drug dependence in adolescence. Drug Alcohol Depend 87(1):46–53. doi:10.1016/j.drugalcdep.2006.07.012
Olsson M (2009) DSM diagnosis of conduct disorder (CD)––a review. Nord J Psychiatry 63(2):102–112. doi:10.1080/08039480802626939
Witkiewitz K, King K, McMahon RJ, Wu J, Luk J, Bierman KL, Coie JD, Dodge KA, Greenberg MT, Lochman JE, Pinderhughes EE (2013) Evidence for a multi-dimensional latent structural model of externalizing disorders. J Abnorm Child Psychol 41(2):223–237. doi:10.1007/s10802-012-9674-z
Khalifa N, Duggan C, Howard R, Lumsden J (2012) The relationship between childhood conduct disorder and adult antisocial behavior is partially mediated by early-onset alcohol abuse. Personal Disord 3(4):423–432. doi:10.1037/a0027017
Loeber R, Green SM, Keenan K, Lahey BB (1995) Which boys will fare worse? Early predictors of the onset of conduct disorder in a six-year longitudinal study. J Am Acad Child Adolesc Psychiatry 34(4):499–509
Burke JD, Loeber R, Birmaher B (2002) Oppositional defiant disorder and conduct disorder: a review of the past 10 years, part II. J Am Acad Child Adolesc Psychiatry 41(11):1275–1293. doi:10.1097/00004583-200211000-00009
Whitmore EA, Mikulich SK, Thompson LL, Riggs PD, Aarons GA, Crowley TJ (1997) Influences on adolescent substance dependence: conduct disorder, depression, attention deficit hyperactivity disorder, and gender. Drug Alcohol Depend 47(2):87–97
Acknowledgments
The CoLaus/PsyCoLaus study was supported by grants from the Swiss National Science Foundation (105993, 118308, 122661 and 139468) and two grants from GlaxoSmithKline Clinical Genetics.
Conflict of interest
All authors declare that they have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Rodgers, S., Müller, M., Rössler, W. et al. Externalizing disorders and substance use: empirically derived subtypes in a population-based sample of adults. Soc Psychiatry Psychiatr Epidemiol 50, 7–17 (2015). https://doi.org/10.1007/s00127-014-0898-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-014-0898-9