Abstract
Background
Obsessive–compulsive disorder (OCD) is the fourth most frequent diagnosis in psychiatry. Patients with OCD suffer from obsessive thinking and compulsive behavior, which impact their everyday life negatively.
Objective
Subjective quality of life (QoL) in patients with OCD was examined and compared to the general German population and to patients with schizophrenia.
Methods
Seventy-five patients, aged 21–72, with OCD (ICD 10 F42.0–F42.2) were recruited from the outpatient clinic for anxiety disorders at the Department of Psychiatry of the University of Leipzig. By means of the WHOQOL-BREF, QoL was assessed in patients with OCD in a representative sample of patients with schizophrenia and in a sample of the general population of Saxony/Germany.
Results
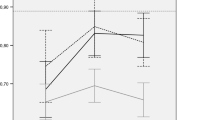
Compared with the general population, QoL in patients with OCDs was lower in all domains of the WHOQOL-BREF. Unexpectedly, QoL in patients with OCDs was lower in the domains “psychological well-being” and “social relationships” when compared with schizophrenia patients.
Conclusions
OCD has a substantial adverse effect on patients’ subjective QoL, which may be even greater than the adverse effect of schizophrenia. Therefore, it will be necessary to include interventions in the treatment of OCD aimed at improving residual deficits in psychosocial functioning and QoL.

Similar content being viewed by others
References
Aigner M, Forster-Streffleur S, Prause W, Freidl M, Weiss M, Bach M (2006) What does the WHOQOL-BREF measure? Measurement overlap between quality of life and depressive symptomatology in chronic somatoform pain disorder. Soc Psychiatry Psychiatr Epidemiol 41:81–86
Angermeyer MC, Kilian R, Matschinger H (2000) WHOQOL-100 und WHOQOL-BREF. Hogrefe, Göttingen
Angermeyer MC, Holzinger A, Stengler-Wenzke K (2002) Depression and quality of life: Results of a follow-up study. Int J Soc Psychiatry 48:189–199
Angermeyer MC, Kilian R (2005) Theoretical models of quality of life for mental disorders. In: Katschnig H, Freeman H, Sartorius N (eds) Quality of life in mental disorders. (2nd edn), Wiley, Newyork, pp 21–31
Bobes J, Gonzalez MP, Bascaran MT, Arango C, Saiz PA, Bousono M (2001) Quality of life and disability in patients with obsessive–compulsive disorder. Eur Psychiatry 16:239–245
Brieger P, Rottig S, Marneros A (2004) Lebensqualität bei unipolar depressiven und bipolar affektiven Patienten [Quality of life in unipolar depressive and bipolar affective patients]. Psychiatr Prax 31:304–309
Bystritsky A, Saxena S, Maidment K, Vapnik T, Tarlow G, Rosen R (1999) Quality-of-life changes among patients with obsessive–compulsive disorder in a partial hospitalization program. Psychiatr Serv 50:412–414
Bystritsky A, Liberman RP, Hwang S, Wallace CJ, Vapnik T, Maindment K, Saxena S (2001) Social functioning and quality of life comparisons between obsessive–compulsive and schizophrenic disorders. Depress Anxiety 14:214–218
Calvocoressi L, Libman D, Vegso SJ, McDougle CJ, Price LH (1998) Global functioning of inpatients with obsessive-compulsive disorder, schizophrenia, and major depression. Psychiatr Serv 49:379–381
Cook JA, Leff HS, Blyler CR, Gold PB, Goldberg RW, Mueser KT, Toprac MG, McFarlane WR, Shafer MS, Blankertz LE, Dudek K, Razzano LA, Grey DD, Burke-Miller (2005) Results of a multisite randomized trial of supported employment interventions for individuals with severe mental illness. Arch Gen Psychiatry 62:505–512
Deacon BJ, Abramowitz JS (2005) The Yale-Brown Obsessive Compulsive Scale: factor analysis, construct validity, and suggestions for refinement. J Anxiety Disord 19:573–585
Franz M, Meyer T, Reber T, Gallhofer B (2000) The importance of social comparisons for high levels of subjective quality of life in chronic schizophrenic patients. Qual Life Res 9:481–489
Goodman WK, Price LH, Rasmussen SA, Mazure C, Fleischmann RL, Hill CL, Heninger GR, Charney DS (1989a) The Yale-Brown Obsessive–Compulsive Scale. I. Development, use, and reliability. Arch Gen Psychiatry 46:1006–1011
Goodman WK, Price LH, Rasmussen SA, Mazure C, Delgado P, Heninger GR, Charney DS (1989b) The Yale-Brown Obsessive–Compulsive Scale. II. Validity. Arch Gen Psychiatry 46:1012–1016
Hansson L (1999) Advancing the concepts of quality of life. In: Priebe S, Oliver JPJ, Kaiser W (eds) Quality of life and mental health care. Wrightson, pp 19–47
Hollander E, Kwon JH, Stein DJ, Broatch J, Rowland CT, Himelein CA (1996) Obsessive–compulsive and spectrum disorders: overview and quality of life issues. J Clin Psychiatry 57:3–6
Jenike MA (2001) An update on obsessive-compulsive disorder. Bull Menninger Clin 65:4–25 (Review)
Katschnig H (2000) Schizophrenia and quality of life. Acta Psychiatr Scand 407:33–37
Katschnig H, Krautgartner M, Schrank B, Angermeyer MC (2006) Quality of life in depression. In: Katschnig H, Freeman H, Sartorius N (eds) Quality of life in mental disorders. (second edition), Wiley, Newyork, pp 129–140
Kay SR, Fiszbein A, Opler LA (1987) The Positive and Negative Syndrome Scale (PANSS) for schizophrenia. Schizophr Bull 13:261–276
Kilian R, Dietrich S, Toumi M, Angermeyer MC (2004) Quality of life in persons with schizophrenia in out-patient treatment with first- or second-generation antipsychotics. Acta Psychiatr Scand 110:108–118
Koran LM, Thienemann ML, Davenport R (1996) Quality of life for patients with obsessive–compulsive disorder. Am J Psychiatry 153:783–788
Koran LM (2000) Quality of life in obsessive-compulsive disorder. Psychiatr Clin North Am 23:509–517
Kuehner C (2002) Subjective quality of life: validity issues with depressed patients. Acta Psychiatr Scand 106:62–70
Lochner C, Stein DJ (2003) Heterogeneity of obsessive–compulsive disorder: a literature review. Harv Rev Psychiatry 11:113–32
Lochner C, Mogotsi M, du Toit PL, Kaminer D, Niehaus DJ, Stein DJ (2003) Quality of life in anxiety disorders: a comparison of obsessive–compulsive disorder, social anxiety disorder, and panic disorder. Psychopathology 36:255–262
Masellis M, Rector NA, Richter MA (2003) Quality of life in OCD: differential impact of obsessions, compulsions, and depression comorbidity. Can J Psychiatry 48:72–77
Mendlowicz MV, Stein MB (2000) Quality of life in individuals with anxiety disorders. Am J Psychiatry 157:669–682
Mendlowicz MV, Braga RJ, Marrocos RP, Figueira I (2005) Comorbidity and disability in outpatients with schizophrenia. Am J Psychiatry 162:400
Moritz S, Rufer M, Fricke S, Karow A, Morfeld M, Jelinek L, Jacobsen D (2005) Quality of life in obsessive–compulsive disorder before and after treatment. Compr Psychiatry 46:453–459
Millet B, Kochman F, Gallarda T, Krebs MO, Demonfaucon F, Barrot I, Bourdel MC, Olie JP, Loo H, Hantouche EG (2004) Phenomenological and co-morbid features associated in obsessive–compulsive disorder: influence of age of onset. J Affect Dis 79:241–246
Rapaport MH, Clary C, Fayyad R, Endicott J (2005) Quality-of-life impairment in depressive and anxiety disorders. Am J Psychiatry 162:1171–1178
Rössler W, Salize HJ, van Os J, Riecher-Rössler A (2005) Size of burden of schizophrenia and psychotic disorders. Eur Neuropsychopharmacol 15:399–409
Rüesch P, Graf J, Meyer PC, Rössler W, Hell D (2004) Occupation, social support and quality of life in persons with schizophrenic or affective disorders. Soc Psychiatry Psychiatr Epidemiol 39:686–694
Skantze K, Malm U, Dencker SJ, May PR, Corrigan P (1992) Comparison of quality of life with standard of living in schizophrenic out-patients. Br J Psychiatry 161:797–801
Stein DJ, Allen A, Bobes J (2000) Quality of life in obsessive–compulsive disorder. CNS Spectr 5:37–39
Stein DJ (2002) Obsessive–compulsive disorder. Lancet 360:397–405
Steketee G (1997) Disability and family burden in obsessive-compulsive disorder. Can J Psychiatry 42:919–928
Stengler-Wenzke K, Angermeyer MC (2002) Ambulante Gruppentherapie für Patienten mit Zwangserkrankungen und deren Angehörige [Behavioral group therapy for patients with OCD and family members]. Psychiatr Prax 29:136–141
Stengler-Wenzke K, Angermeyer MC (2005) Inanspruchnahme von professioneller Hilfe von Patienten mit Zwangserkrankungen [Employment of professional help by patients with obsessive-compulsive disorders]. Psychiat Prax 32:195–201
Stengler-Wenzke K, Beck M, Holzinger A, Angermeyer MC (2004) Stigmaerfahrungen von Patienten mit Zwangserkrankungen [Stigma experiences of patients with obsessive compulsive disorders]. Fortschr Neurol Psychiatr 72:7–13
The WHO World Health Report: New understanding, new hope. WHO, Geneva, 2001
THE WHOQOL GROUP (1998) Development of the World Health Organization WHOQOL-BREF quality of life assessment. Soc Sci Med 28:551–558
Ware JE, Sherbourne CD (1992) The MOS 36-Item Short-Form Health Survey (SF-36). I. Conceptual framework and item selection. Med Care 30:473–483
Weissman MM, Bland RC, Canino GJ, Greenwald S, Hwu HG, Lee CK, Newman SC, Oakley-Browne MA, Rubio-Stipec M, Wickramaratne PJ, et al. (1994) The cross- national epidemiology of obsessive compulsive disorder. The Cross National Collaborative Group. J Clin Psychiatry 55:5–10
Wills TA (1981) Downward comparison principles in social psychology. Psychol Bull 90:245–271
World Health Organization (1993) The 10th revision of the International Classification of Diseases. Chapter V (F): Mental and behavioral disorders. Huber, Göttingen
World Health Organization (1999) The “newly defined” burden of mental problems. Fact Sheets no217. WHO, Geneva
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Stengler-Wenzke, K., Kroll, M., Matschinger, H. et al. Subjective quality of life of patients with obsessive–compulsive disorder. Soc Psychiat Epidemiol 41, 662–668 (2006). https://doi.org/10.1007/s00127-006-0077-8
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00127-006-0077-8