Abstract
Aims/hypothesis
The aim was to investigate whether an intensive lifestyle intervention, with high volumes of exercise, improves beta cell function and to explore the role of low-grade inflammation and body weight.
Methods
This was a randomised, assessor-blinded, controlled trial. Ninety-eight individuals with type 2 diabetes (duration <10 years), BMI of 25–40 kg/m2, no use of insulin and taking fewer than three glucose-lowering medications were randomised (2:1) to either the standard care plus intensive lifestyle group or the standard care alone group. Standard care consisted of individual guidance on disease management, lifestyle advice and blinded regulation of medication following a pre-specified algorithm. The intensive lifestyle intervention consisted of aerobic exercise sessions that took place 5–6 times per week, combined with resistance exercise sessions 2–3 times per week, with a concomitant dietary intervention aiming for a BMI of 25 kg/m2. In this secondary analysis beta cell function was assessed from the 2 h OGTT-derived disposition index, which is defined as the product of the Matsuda and the insulinogenic indices.
Results
At baseline, individuals were 54.8 years (SD 8.9), 47% women, type 2 diabetes duration 5 years (IQR 3–8) and HbA1c was 49.3 mmol/mol (SD 9.2); 6.7% (SD 0.8). The intensive lifestyle group showed 40% greater improvement in the disposition index compared with the standard care group (ratio of geometric mean change [RGM] 1.40 [95% CI 1.01, 1.94]) from baseline to 12 months’ follow-up. Plasma concentration of IL-1 receptor antagonist (IL-1ra) decreased 30% more in the intensive lifestyle group compared with the standard care group (RGM 0.70 [95% CI 0.58, 0.85]). Statistical single mediation analysis estimated that the intervention effect on the change in IL-1ra and the change in body weight explained to a similar extent (59%) the variance in the intervention effect on the disposition index.
Conclusions/interpretation
Our findings show that incorporating an intensive lifestyle intervention, with high volumes of exercise, in individuals with type 2 diabetes has the potential to improve beta cell function, associated with a decrease in low-grade inflammation and/or body weight.
Trial registration
ClinicalTrials.gov NCT02417012

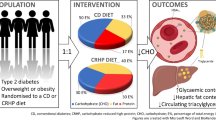
Graphical abstract
Similar content being viewed by others

Introduction
In healthy individuals, reductions in insulin sensitivity are accompanied by increased insulin secretion, whereby normoglycaemia is maintained. In type 2 diabetes, beta cells are unable to compensate for the increased insulin resistance, leading to hyperglycaemia [1]. While peripheral insulin resistance may be the earliest detectable abnormality [2], beta cell function is often markedly reduced by the time type 2 diabetes is diagnosed [3]. Lifestyle changes are part of first line treatment of type 2 diabetes [4] and lifestyle (i.e. exercise and/or diet) can improve glycaemic control measured by HbA1c [5,6,7,8,9]. Recently, it was reported that a diet-induced weight loss intervention, without increase in physical activity, led to remission of type 2 diabetes [7]. The mechanisms leading to remission were thought to depend on a reduction of ectopic fat in the liver and the pancreas, but were also dependent on improved beta cell function [10]. Exercise has been demonstrated to improve peripheral insulin sensitivity in individuals with type 2 diabetes [11], but it is less clear whether exercise can improve beta cell function [12, 13].
Effective lifestyle interventions often result in a concomitant weight loss and since weight loss may independently improve beta cell function [14, 15], this has to be taken into account. Although little is known about the effect of exercise on beta cell function, exercise has been suggested to improve beta cell function through a range of mechanisms [16], but the role of low-grade inflammation in lifestyle-induced improvements in beta cell function is largely unknown. Type 2 diabetes is considered an inflammatory disease with elevated levels of several cytokines including TNF-α, IL-6, IL-1 receptor antagonist (IL-1ra) and IL-1β [17]. Pharmacological inhibition of IL-1β with anakinra, an IL-1β receptor antagonist, resulted in improved beta cell function in individuals with type 2 diabetes [18]. This implies that IL-1β is a potential inflammatory mediator of pancreatic beta cell damage in type 2 diabetes. Since skeletal muscle is recognised as an endocrine organ that may be responsible for reducing low-grade inflammation in response to acute exercise and training [19, 20], this might provide a link between exercise and beta cell function.
We previously observed that a 12 month intensive lifestyle intervention, with high volumes of exercise, in individuals with type 2 diabetes led to discontinuation of glucose-lowering medication in more than 50% of the individuals compared with standard care and, in spite of the discontinuation of medication, a moderate reduction in HbA1c was observed [8]. The aim of this study was to investigate the mechanisms underlying the improved glycaemic control. We hypothesise that the intensive lifestyle intervention improves the disposition index, an OGTT-derived estimate of beta cell function, from baseline to 12 months’ follow-up. Moreover, we explore the role of low-grade inflammation as well as weight loss in relation to beta cell function.
Methods
Study design, participants and randomisation
From April 2015 to August 2016 a total of 98 individuals were enrolled in this single-centre, assessor-blinded, randomised, clinical trial. Individuals, diagnosed with type 2 diabetes for less than 10 years, with a BMI of 25 to 40 kg/m2, taking fewer than three glucose-lowering medications and no insulin, with no severe diabetic complications, and no previous history of cardiovascular disease, were eligible for the study. Inclusion- and exclusion criteria have been described in detail earlier [21]. During the ≥6 weeks prior to baseline measurements and randomisation, glucose-, lipid- and blood-pressure-lowering pharmacological treatments were titrated and standardised following a pre-specified algorithm in order to minimise changes in medical treatment not directly linked to the intervention. Randomisation was generated by a computer and given to an external data manager with no involvement in the study. Individuals were randomised 2:1, stratified by sex, either to an intensive lifestyle and standard care group or a standard care group for 12 months, respectively. The full protocol is published [21]. All individuals provided informed written and oral consent. The study was conducted in accordance with the Helsinki Declaration, and the study protocol was approved by the national scientific ethical committee at the Capital Region of Denmark (H-1-2014-114). The clinical trial registration number is NCT02417012.
Interventions
All individuals, regardless of allocation, received standard care, controlled every third month by the study nurse. The standard care consisted of individual sessions with education in diabetes management, lifestyle advice and regulation of pharmacological treatment. Any change in glucose-, lipid- or blood-pressure-lowering medication was decided by an endocrinologist in a blinded fashion, following a pre-specified, treat-to-target algorithm and delivered to the individuals by the study nurse.
In addition to the standard care the intensive lifestyle group completed an intervention that consisted of high-volume, group-based exercise (4–8 individuals), with five to six aerobic exercise sessions per week, whereof two to three sessions per week were combined with resistance exercise. In the beginning all exercise sessions were supervised, but supervision gradually decreased over the 12 months [21]. During the entire year individuals wore a Polar V800 watch (Polar Electro, Finland), day and night, to objectively register exercise data, including duration. Furthermore, individuals were encouraged to be physically active corresponding to more than 10,000 steps per day, which was also tracked with Polar V800. On the dietary side individual guidance and meal plans were provided by clinical dietitians aiming at an intended energy deficit of 2092 kJ (500 kcal) per week, until a BMI of 25 kg/m2 was reached. Individuals were encouraged to sleep 7–8 h per night with the aim of adhering to regular bedtimes throughout the week. The final two components were self-monitoring and diabetes education/networking. More detailed information about the intervention is available [21].
Experimental day
An experimental day was completed at baseline and 12 months’ follow-up. Two days prior to each experimental day all individuals were instructed to refrain from moderate to vigorous intensity exercise, to minimise general physical activity and to pause all glucose-, lipid- and blood-pressure-lowering medication. Additionally, no alcohol was permitted, and individuals were encouraged to eat their habitual diet during the last 24 h. On the experimental day individuals arrived after a minimum of 8 h overnight fasting.
Anthropometrics, body composition and fitness
Body weight was measured with an electronic scale and height was measured with a Holtain stadiometer (Holtain, Crymych, UK) according to standard procedures. Individuals underwent a dual-energy x-ray absorptiometry scan (Lunar Prodigy Advance, GE Medical Systems Lunar, USA) with software (Prodigy, enCORE 2004, version 8.8, GE Lunar Corp, USA) for measurement of whole-body fat mass, fat-free mass and regional abdominal fat mass. BMI was calculated as weight in kg divided by the square of height in meters. Measurement of maximal oxygen uptake (\( \dot{V}{\mathrm{O}}_{2\max } \)) was performed using continuous indirect calorimetric measurements (Quark CPET, Cosmed, Italy) on a Monarch LC4 bicycle (Monark Exercise, Sweden). The test was performed with a 5 min warm-up followed by an increase of 20 watts/min until exhaustion.
OGTT
Individuals ingested 83 g of glucose dissolved in 300 ml of water for the OGTT (corresponding to 75 g anhydrous glucose). An antecubital vein catheter was inserted for blood sampling. Fasting blood samples were taken 10 min before the OGTT (−10) and 15, 30, 60, 90 and 120 min during the OGTT to measure glucose, insulin and C-peptide responses. All blood samples were centrifuged and stored at −80°C until further analysis. The Matsuda index, a measure of whole-body insulin sensitivity, was calculated as 10,000/√[fasting glucose × fasting insulin] × [mean glucose × mean insulin] [22] based on OGTT data. The insulinogenic index, the change in insulin secretion divided by the change in plasma glucose during the first 30 min of the OGTT, was used as an estimate of insulin secretion: ∆Insulin30-basal/∆Glucose30-basal [23, 24]. The disposition index was calculated as the product of the Matsuda index and the insulinogenic index. The disposition index describes the hyperbolic relationship between insulin-sensitive tissue and pancreatic beta cell secretion, i.e. beta cell function adjusted for insulin sensitivity [1]. HOMA-IR was calculated as: fasting insulin × fasting glucose/22.5 and HOMA-B as: (20 × fasting insulin)/(fasting glucose − 3.5) [25].
Blood analyses
Fasting plasma blood samples were analysed for TNF-α, IL-6, IL-10 and IL-1ra with immunoassay kits (Mesoscale, V-Plex human proinflammatory panel I and V-Plex human IL-1ra kit, Meso Scale Discovery, USA). Glucagon and glucagon-like peptide 1 (GLP-1) were assessed at 0 min, 30 min and 120 min during the OGTT and measured respectively with an RIA kit (EMD Millipore Corporation, USA) and with an in-house RIA specific for the amidated C-terminal (total GLP-1 assay, codename 89390). The assay is based on the COOH-terminus and results therefore reflect the secretion rates of GLP-1 (7-36NH2 and 9-36NH2) as described previously [26, 27]. All other blood sample measurements (C-reactive protein (CRP), HbA1c, glucose, insulin, total cholesterol, LDL- and HDL-cholesterol and triacylglycerol) were analysed at the Department of Clinical Biochemistry, Rigshospitalet, Denmark.
Study endpoints
The primary outcome in this secondary analysis was the change in the disposition index from baseline to 12 months’ follow-up. Secondary outcomes were the change in the Matsuda and the insulinogenic indices from baseline to 12 months’ follow-up. Furthermore, we investigated the change in CRP, TNF-α, IL-6, IL-10 and IL-1ra from baseline to 12 months’ follow-up. We applied statistical single mediation analysis to investigate the association between the change in the disposition index from baseline to 12 months’ follow-up and the change in one of the following mediators: IL-1ra, body weight or \( \dot{V}{\mathrm{O}}_{2\max } \). Additional single mediation analyses were performed to assess the association between the change in IL-1ra and the change in one of the following mediators: \( \dot{V}{\mathrm{O}}_{2\max } \), relative fitness (mlO2 kg−1 min−1), body weight, fat mass or regional abdominal fat mass. Some of the included outcome measures have previously been reported; 2 h glucose, HbA1c, fasting glucose, fasting insulin, lipids, blood pressure, fitness and body composition from baseline to 12 months’ follow-up [8, 28, 29], but are included in this sub-study to facilitate the interpretation.
Statistics
The analyses were performed according to the intention-to-treat principle. Some outcomes were collected at baseline and 12 months’ follow-up, while other outcomes were collected at baseline, 3-, 6-, 9- and 12-months’ follow-up. Outcomes were analysed using linear mixed models and repeated measures linear mixed models. An ANOVA was carried out that included group (two levels), time (four levels), sex (two levels) and the possible interaction between group and time as fixed effects, and with baseline value as a covariate and the unique patient identifier as a random effect. Data are presented as mean difference in change with 95% CI, unless stated otherwise. The natural logarithmic transformation was applied to obtain normality when appropriate. The differences in mean change from log-transformed data were exponentiated and data are expressed as the ratio of the geometric mean change (RGM) within and between groups, allowing us to present data as the per cent change. Incremental AUC (iAUC) and total AUC (tAUC) were calculated using the trapezoidal method [30]. tAUC was defined as the area above concentrations of zero and iAUC was defined as the area above fasting concentration. Model assumptions were investigated through the predicted values and the standardised residuals. Single mediation analysis was performed according to Baron and Kenny [31], which is a series of regression models fitted to the changes of an independent variable (group with two levels), a dependent variable and a mediator. One model regressed the dependent variable with the independent variable (path c, total effect) and another regressed the mediator on the independent variable (path a). Finally, a model regressed the dependent variable on both the independent variable (direct effect, path c´) and mediator (path b). A bootstrapping approach (5000 bootstrap resamples) was used to obtain bias-corrected 95% CIs. The proportion of mediation was quantified by dividing the mediation effect (path a × b) with the total effect (path c). Analyses of average (mean) exercise volume (aerobic and strength, min/week) across 12 months and the indices (Matsuda, insulinogenic and disposition) were based on linear regression. The significance level was set to p < 0.05 (two-tailed). All statistical calculations were performed using Stata IC/SE 13.1 (StataCorp, USA).
Results
We enrolled 98 individuals in the study. The flow chart has been published previously [8]. Ninety-five individuals, who completed the 2 h OGTT at baseline, were included in the intention-to-treat analysis with 33 individuals in the standard care group and 62 individuals in the intensive lifestyle group. At baseline, individuals were 54.8 years (SD 8.9), 47% women, the duration of type 2 diabetes was 5 years (IQR 3–8) and HbA1c 49.3 mmol/mol (SD 9.2); 6.7% (SD 0.8) (Table 1). From baseline to 12 months’ follow-up the intensive lifestyle group lost more weight than the standard care group (between-group difference −4.14 kg [95% CI −6.79, −1.48]; p = 0.002) and \( \dot{V}{\mathrm{O}}_{2\max } \) (mlO2/min) increased by 427.3 mlO2/min [95% CI 255.0, 599.5] (p < 0.001) more in the intensive lifestyle group compared with the standard care group (Table 2).
Beta cell function, insulin sensitivity and insulin secretion
From baseline to 12 months’ follow-up the disposition index increased 40% more in the intensive lifestyle group compared with the standard care group (RGM 1.40, [95% CI 1.01, 1.94]; p = 0.042) (Table 2, Fig. 1). The Matsuda index increased 23% more in the intensive lifestyle group compared with the standard care group from baseline to 12 months’ follow-up (RGM 1.23 [95% CI 1.01, 1.49]; p = 0.039) (Table 2, Fig. 1) and there was no between-group difference in the insulinogenic index from baseline to 12 months’ follow-up (Table 2, Fig. 1). Per protocol analysis supported the observed findings, where the intensive lifestyle group improved the disposition index by 62% (RGM 1.62 [95% CI 1.13, 2.31]; p = 0.08) more than the standard care group from baseline to 12 months’ follow-up (Table 3). A positive association was observed between average exercise volume (aerobic and strength, min/week) and the disposition index (r = 0.18 and p < 0.001) and the Matsuda index (r = 0.18 and p < 0.001), whereas no association was found in relation to the insulinogenic index (r = 0.002 and p = 0.42) (Fig. 2).
Intervention effect on the indices. (a) ∆ Matsuda index; (b) ∆ Insulinogenic index; and (c) ∆ Disposition index. Data are represented as median (IQR) from baseline to 12 months’ follow-up with individual points. *p < 0.05 and ***p < 0.001 within-group difference in mean change from baseline to 12 months’ follow-up. †p < 0.05 between-group difference in mean change from baseline to 12 months’ follow-up
Glucose, insulin, GLP-1 and glucagon
Plasma glucose and insulin levels during the OGTT at baseline and 12 months’ follow-up are depicted in Fig. 3. From baseline to 12 months’ follow-up, blood glucose, expressed as the tAUC0–120min of the glucose curve during the OGTT was reduced in the intensive lifestyle group compared with the standard care group (between-group difference −154.1 mmol/l × min [95% CI −291.5, −16.7]; p = 0.028) more (Table 2). The between-group difference in the iAUC0–120min of the glucose curve was −135.0 mmol/l × min [95% CI −197.5, −72.5] (p < 0.001) in favour of the intensive lifestyle group (Table 2). Plasma insulin, GLP-1 and glucagon (tAUC0–120min and iAUC0–120min) during the OGTT showed no difference in change between groups (Table 2). Other clinical markers of glycaemic control are presented in Table 2.
Glucose and insulin data. (a, b) Plasma glucose levels and tAUC from the 2 h OGTT at baseline and 12 months’ follow-up, respectively. (c, d) Plasma insulin levels and tAUC from the 2 h OGTT at baseline and 12 months’ follow-up, respectively. Data are represented as least square means ± SE and bar charts are represented as median (IQR) with individual points. StC, standard care; IL, intensive lifestyle
Low-grade inflammation
The plasma concentration of IL-1ra decreased 30% more in the intensive lifestyle group compared with the standard care group from baseline to 12 months’ follow-up (RGM 0.70 [95% CI 0.58, 0.85]; p < 0.001) (Table 2). No between-group difference in CRP TNF-α, IL-6 or IL-10 was observed from baseline to 12 months’ follow-up (Table 2).
Beta cell function: low-grade inflammation and body weight
Single mediation analysis suggested that IL-1ra levels accounted for 59% of the total intervention effect on the disposition index (Table 4). While the intervention effect on \( \dot{V}{\mathrm{O}}_{2\max } \) (mlO2/min) was not associated with the intervention effect on IL-1ra (p = 0.221) the intervention effect on body weight (p = 0.010), fat mass (p < 0.001), regional abdominal fat mass (p = 0.001) and relative fitness (mlO2 kg−1 min−1) (p = 0.003) was (Table 4). In another single mediation analysis, we found that the change in body weight also accounted for 59% of the total intervention effect on the disposition index (Table 4).
Discussion
The primary finding of this study was that the intensive lifestyle intervention, with high volumes of exercise, improved the disposition index, owing to an improvement in whole-body insulin sensitivity rather that an improvement in the insulin secretion per se. Moreover, we observed that the increment in the disposition index was associated with the intervention effect on low-grade inflammation and/or body weight.
Similar to our findings, Karstoft et al observed that an exercise-induced improvement in the disposition index was primarily due to enhanced insulin sensitivity [32]. In addition, we observed a lowering of glucose tAUC0–120min and iAUC0–120min during the OGTT in the intensive lifestyle group compared with standard care, which confirms that the beta cells were less exposed to glucotoxicity. Since the intensive lifestyle intervention consisted of high volumes of exercise, we explored the isolated role of exercise and found that the average exercise volume (aerobic and strength, min/week) was associated with both the Matsuda index and the disposition index, but also low-grade inflammation and body weight, which is in line with the primary finding. No association was observed between the average exercise volume (aerobic and strength, min/week) and the insulinogenic index, suggesting that exercise does not modify insulin secretion per se, which is in line with other findings [32, 33]. In contrast, Dela and colleagues found that aerobic exercise improved insulin secretion [12]; however, the difference in insulin secretion was only observed at glucose concentrations of 25 mmol/l during the hyperglycaemic clamp, in contrast to the more physiological range in our study. The insulinogenic index was assessed during the initial 30 min of the OGTT and only a total of three individuals from the intensive lifestyle group had glucose levels above 24 mmol/l in that period. Thus, it remains unclear whether we would have observed an association between average exercise volume (aerobic and strength, min/week) and the insulinogenic index, if we had exposed the included individuals to a higher glucose stress. It remains unknown why the disposition index improved by 35% in the standard care group, but the individuals in the standard care group may also have increased their physical activity level and decreased their energy intake. Although speculative, the improved disposition index in the standard care group may be due to a larger proportion receiving GLP-1 receptor agonist at 12 months’ follow-up (42% vs 12%), which is associated with weight loss [34]. Altogether, this may explain the small numerical improvement in both the Matsuda index and the insulinogenic index and thus the disposition index. We observed no between-group difference in GLP-1 or glucagon (tAUC0–120 min and iAUC0–120 min) and it is widely debatable whether lifestyle changes affect GLP-1 and glucagon, probably due to inadequate study designs in this area of research.
In line with others, we observed a decrease in low-grade inflammation [35]. We moreover observed that the intensive lifestyle intervention effect on IL-1ra was associated with the improvement in the disposition index. IL-1β is considered a key mediator of beta cell failure [36, 37] and plasma levels of the anti-inflammatory cytokine IL-1ra reflect plasma levels of IL-1β [37]. Although this is speculative, the observed decrease in IL-1ra may reflect a decrease in IL-1β and thus explain the association between the disposition index and IL-1ra. We also observed a decrease in TNF-α, IL-6 and IL-10 in the intensive lifestyle group, but with no between-group difference. It can be speculated that cytokines such as TNF-α exert their action locally, while IL-1ra to a larger extent is considered a circulating cytokine [38]. As IL-1ra is downstream from IL-1β in the inflammatory cascade, but also downstream of TNF-α and IL-6, a lowering of IL-1ra may reflect a decrease in the cumulative inflammatory load from upstream cytokines. Since TNF-α may cause insulin resistance [19], the previously described within-group effect on TNF-α may explain why the intensive lifestyle intervention, with high volumes of exercise, enhanced insulin sensitivity. It is well described that insulin sensitivity improves with exercise through a range of mechanisms [39], which means that TNF-α is probably partially responsible for the observed change in insulin sensitivity. Importantly, while acute exercise increases the cytokine level, we here observed a decrease. However, an increase in IL-6 with acute exercise without a preceding increase in TNF-α and a following increase in IL-1ra and IL-10 is considered an anti-inflammatory response [40]. In contrast, regular exercise is associated with a training-induced reduction in basal levels of IL-6 [19], as observed here.
Weight loss is often a consequence of a lifestyle intervention with a dietary approach [7], an exercise-based intervention [5] or when exercise and diet are combined [9], the latter being relevant to our study. Thus, it can be complicated to interpret the effects of a lifestyle intervention with an associated weight loss [32, 41]. However, not all exercise-based interventions that improve beta cell function in type 2 diabetes are accompanied by weight loss [42, 43], suggesting that beta cell function may improve despite individuals being weight stable. To explore the role of weight loss in relation to beta cell function we performed single mediation analysis and found that the observed change in body weight was associated with 59% of the intensive lifestyle intervention effect on the disposition index. In the Diabetes Remission Clinical Trial (DiRECT) study the diet-induced remission was due to a reduction in ectopic fat, but dependent upon improved beta cell function [10]. We did not measure ectopic fat, but we observed a moderate decrease in fat mass and a large reduction in regional abdominal fat mass in the intensive lifestyle group compared with the standard care group. Since low-grade inflammation is known to be associated with both abdominal fat mass and fitness [19, 44] we performed single mediation analyses and found that the intensive lifestyle intervention effect on IL-1ra was consistently associated with the change in body weight, fat mass and regional abdominal fat mass, while no association was observed with the change in \( \dot{V}{\mathrm{O}}_{2\max } \). Our findings suggest that an intensive lifestyle intervention may improve the disposition index, primarily driven by enhanced insulin sensitivity, and the possible underlying regulatory mechanism seems to be related to changes in low-grade inflammation and body weight. However, our study design and methodology does not allow us to present a hierarchical order of the suggested mechanisms nor to draw any causative conclusions. While weight loss may be the natural first choice, suggesting that this change appeared prior to the reduction in low-grade inflammation, it has been found that exercise-induced IL-6 is implicated in the reduction of visceral fat [45]. This finding suggests that regular exercise may elicit an anti-inflammatory response that is necessary to obtain a reduction in visceral fat, which suggests that the improvement of the disposition index appeared through changes in low-grade inflammation and/or body weight.
Limitations
Our study had some limitations. The derivation of beta cell function from a meal-stimulated test is based on the assumption of a hyperbolic relationship between insulin sensitivity and insulin secretion [1]. While subject to debate [46, 47], it is widely accepted to incorporate a measure of insulin sensitivity when assessing beta cell function to obtain insight of the interaction between insulin secretion and insulin sensitivity [48] and the hyperbolic relationship from OGTT-derived data has been validated across the entire glucose continuum [49, 50]. The use of indirect measures of beta cell function (Disposition index), insulin sensitivity (Matsuda index) and insulin secretion (Insulinogenic index), are not as accurate as various clamping methods. However, the indices are calculated based on data acquired under physiological conditions, in contrast to the supraphysiological conditions of the clamp methods, which make our findings physiologically relevant. Another aspect that needs to be considered is the use of average exercise volume (aerobic and strength, min/week). To understand the interactions between exercise, body weight and low-grade inflammation, time course changes in these variables could have facilitated our findings. However, we were unable to perform these analyses as we did not collect meal-stimulated (OGTT) or fasting blood samples in the intermediate time period from baseline to 12 months’ follow-up. While statistical single mediation analyses were applied to generate hypotheses regarding the underlying mechanisms, no causative conclusions can be drawn. Finally, we observed substantial interindividual variance regarding indices in both groups, which can be explained by group heterogeneity, a reflection of the intention-to-treat study design and/or diabetes duration. The included individuals were screened prior to baseline measurement. However, diabetes duration was self-reported, which is subject to information bias and it is very likely that a time gap exists between the debut of disease and the time of diagnosis. This could potentially contribute to some of the observed interindividual variance of the indices.
In summary a 12 month intensive lifestyle intervention has the potential to improve beta cell function, as reflected by the disposition index, more than standard care. The observed change in the disposition index was mainly driven by an increase in insulin sensitivity. Furthermore, the intensive lifestyle intervention was associated with a decrease in low-grade inflammation and a moderate weight loss, but their individual importance for the improvement of the disposition index needs further elaboration.
Data availability
Data are available upon request to the guarantors of the work MYJ and MR-L.
Abbreviations
- CRP:
-
C-reactive protein
- GLP-1:
-
Glucagon-like peptide 1
- iAUC:
-
Incremental AUC
- IL-1ra:
-
IL-1 receptor antagonist
- RGM:
-
Ratio of geometric mean change
- tAUC:
-
Total AUC
References
Kahn SE, Prigeon RL, McCulloch DK et al (1993) Quantification of the relationship between insulin sensitivity and beta-cell function in human subjects. Evidence for a hyperbolic function. Diabetes 42(11):1663–1672. https://doi.org/10.2337/diab.42.11.1663
Taylor R (2012) Insulin resistance and type 2 diabetes. Diabetes 61(4):778–779. https://doi.org/10.2337/db12-0073
Rudenski AS, Hadden DR, Atkinson AB et al (1988) Natural history of pancreatic islet B-cell function in type 2 diabetes mellitus studied over six years by homeostasis model assessment. Diabet Med 5(1):36–41. https://doi.org/10.1111/j.1464-5491.1988.tb00938.x
American Diabetes Association (2018) 7. Obesity management for the treatment of type 2 diabetes: standards of medical care in diabetes—2018. Diabetes Care 41(Suppl. 1):S65–S72. https://doi.org/10.2337/dc18-S007
Balducci S, Zanuso S, Nicolucci A et al (2010) Effect of an intensive exercise intervention strategy on modifiable cardiovascular risk factors in subjects with type 2 diabetes mellitus: a randomized controlled trial: the Italian Diabetes and Exercise Study (IDES). Arch Intern Med 170(20):1794–1803. https://doi.org/10.1001/archinternmed.2010.380
Umpierre D, Ribeiro PA, Kramer CK et al (2011) Physical activity advice only or structured exercise training and association with HbA1c levels in type 2 diabetes: a systematic review and meta-analysis. JAMA 305(17):1790–1799. https://doi.org/10.1001/jama.2011.576
Lean ME, Leslie WS, Barnes AC et al (2018) Primary care-led weight management for remission of type 2 diabetes (DiRECT): an open-label, cluster-randomised trial. Lancet 391(10120):541–551. https://doi.org/10.1016/S0140-6736(17)33102-1
Johansen MY, MacDonald CS, Hansen KB et al (2017) Effect of an intensive lifestyle intervention on glycemic control in patients with type 2 diabetes: a randomized clinical trial. JAMA 318(7):637–646. https://doi.org/10.1001/jama.2017.10169
Look Ahead Research Group, Wing RR, Bolin P et al (2013) Cardiovascular effects of intensive lifestyle intervention in type 2 diabetes. N Engl J Med 369(2):145–154. https://doi.org/10.1056/NEJMoa1212914
Taylor R, Al-Mrabeh A, Zhyzhneuskaya S et al (2018) Remission of human type 2 diabetes requires decrease in liver and pancreas fat content but is dependent upon capacity for beta cell recovery. Cell Metab 28(4):547–556. https://doi.org/10.1016/j.cmet.2018.07.003
Way KL, Hackett DA, Baker MK, Johnson NA (2016) The effect of regular exercise on insulin sensitivity in type 2 diabetes mellitus: a systematic review and meta-analysis. Diabetes Metab J 40(4):253–271. https://doi.org/10.4093/dmj.2016.40.4.253
Dela F, von Linstow ME, Mikines KJ, Galbo H (2004) Physical training may enhance beta-cell function in type 2 diabetes. Am J Physiol Endocrinol Metab 287(5):E1024–E1031. https://doi.org/10.1152/ajpendo.00056.2004
Hordern MD, Cooney LM, Beller EM, Prins JB, Marwick TH, Coombes JS (2008) Determinants of changes in blood glucose response to short-term exercise training in patients with type 2 diabetes. Clin Sci (Lond) 115(9):273–281. https://doi.org/10.1042/CS20070422
Hofso D, Jenssen T, Bollerslev J et al (2011) Beta cell function after weight loss: a clinical trial comparing gastric bypass surgery and intensive lifestyle intervention. Eur J Endocrinol 164(2):231–238. https://doi.org/10.1530/EJE-10-0804
Ferrannini E, Mingrone G (2009) Impact of different bariatric surgical procedures on insulin action and β-cell function in type 2 diabetes. Diabetes Care 32(3):514–520. https://doi.org/10.2337/dc08-1762
Curran M, Drayson MT, Andrews RC et al (2020) The benefits of physical exercise for the health of the pancreatic beta-cell: a review of the evidence. Exp Physiol 105(4):579–589. https://doi.org/10.1113/EP088220
Knudsen SH, Pedersen BK (2015) Targeting inflammation through a physical active lifestyle and pharmaceuticals for the treatment of type 2 diabetes. Curr Diab Rep 15(10):82. https://doi.org/10.1007/s11892-015-0642-1
Larsen CM, Faulenbach M, Vaag A et al (2007) Interleukin-1-receptor antagonist in type 2 diabetes mellitus. N Engl J Med 356(15):1517–1526. https://doi.org/10.1056/NEJMoa065213
Pedersen BK (2017) Anti-inflammatory effects of exercise: role in diabetes and cardiovascular disease. Eur J Clin Investig 47(8):600–611. https://doi.org/10.1111/eci.12781
Pedersen BK, Febbraio MA (2008) Muscle as an endocrine organ: focus on muscle-derived interleukin-6. Physiol Rev 88(4):1379–1406. https://doi.org/10.1152/physrev.90100.2007
Ried-Larsen M, Christensen R, Hansen KB et al (2015) Head-to-head comparison of intensive lifestyle intervention (U-TURN) versus conventional multifactorial care in patients with type 2 diabetes: protocol and rationale for an assessor-blinded, parallel group and randomised trial. BMJ Open 5(12):e009764. https://doi.org/10.1136/bmjopen-2015-009764
Matsuda M, DeFronzo RA (1999) Insulin sensitivity indices obtained from oral glucose tolerance testing: comparison with the euglycemic insulin clamp. Diabetes Care 22(9):1462–1470. https://doi.org/10.2337/diacare.22.9.1462
Wareham NJ, Phillips DI, Byrne CD, Hales CN (1995) The 30 minute insulin incremental response in an oral glucose tolerance test as a measure of insulin secretion. Diabet Med 12(10):931. https://doi.org/10.1111/j.1464-5491.1995.tb00399.x
Phillips DI, Clark PM, Hales CN, Osmond C (1994) Understanding oral glucose tolerance: comparison of glucose or insulin measurements during the oral glucose tolerance test with specific measurements of insulin resistance and insulin secretion. Diabet Med 11(3):286–292. https://doi.org/10.1111/j.1464-5491.1994.tb00273.x
Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC (1985) Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 28(7):412–419. https://doi.org/10.1007/bf00280883
Wewer Albrechtsen NJ, Bak MJ, Hartmann B et al (2015) Stability of glucagon-like peptide 1 and glucagon in human plasma. Endocr Connect 4(1):50–57. https://doi.org/10.1530/EC-14-0126
Orskov C, Rabenhoj L, Wettergren A, Kofod H, Holst JJ (1994) Tissue and plasma concentrations of amidated and glycine-extended glucagon-like peptide I in humans. Diabetes 43(4):535–539. https://doi.org/10.2337/diab.43.4.535
Ried-Larsen M, Johansen MY, MacDonald CS et al (2019) Type 2 diabetes remission 1 year after an intensive lifestyle intervention: a secondary analysis of a randomized clinical trial. Diabetes Obes Metab 21(10):2257–2266. https://doi.org/10.1111/dom.13802
MacDonald CS, Johansen MY, Nielsen SM et al (2020) Dose–response effects of exercise on glucose-lowering medications for type 2 diabetes: a secondary analysis of a randomized clinical trial. Mayo Clin Proc 95(3):488–503. https://doi.org/10.1016/j.mayocp.2019.09.005
Yeh KC, Kwan KC (1978) A comparison of numerical integrating algorithms by trapezoidal, Lagrange, and spline approximation. J Pharmacokinet Biopharm 6(1):79–98. https://doi.org/10.1007/BF01066064
Baron RM, Kenny DA (1986) The moderator–mediator variable distinction in social psychological research: conceptual, strategic, and statistical considerations. J Pers Soc Psychol 51(6):1173–1182. https://doi.org/10.1037//0022-3514.51.6.1173
Karstoft K, Winding K, Knudsen SH et al (2014) Mechanisms behind the superior effects of interval vs continuous training on glycaemic control in individuals with type 2 diabetes: a randomised controlled trial. Diabetologia 57(10):2081–2093. https://doi.org/10.1007/s00125-014-3334-5
Temple KA, Tjaden AH, Atkinson KM et al (2019) Association of habitual daily physical activity with glucose tolerance and β-cell function in adults with impaired glucose tolerance or recently diagnosed type 2 diabetes from the Restoring Insulin Secretion (RISE) Study. Diabetes Care 42(8):1521–1529. https://doi.org/10.2337/dc19-0538
Davies MJ, Bergenstal R, Bode B et al (2015) Efficacy of liraglutide for weight loss among patients with type 2 diabetes: The SCALE diabetes randomized clinical trial. JAMA 314(7):687–699. https://doi.org/10.1001/jama.2015.9676
Petersen AM, Pedersen BK (2005) The anti-inflammatory effect of exercise. J Appl Physiol (1985) 98(4):1154–1162. https://doi.org/10.1152/japplphysiol.00164.2004
Eguchi K, Manabe I (2013) Macrophages and islet inflammation in type 2 diabetes. Diabetes Obes Metab 15(Suppl 3):152–158. https://doi.org/10.1111/dom.12168
Donath MY, Shoelson SE (2011) Type 2 diabetes as an inflammatory disease. Nat Rev Immunol 11(2):98–107. https://doi.org/10.1038/nri2925
Benatti FB, Pedersen BK (2015) Exercise as an anti-inflammatory therapy for rheumatic diseases-myokine regulation. Nat Rev Rheumatol 11(2):86–97. https://doi.org/10.1038/nrrheum.2014.193
Maarbjerg SJ, Sylow L, Richter EA (2011) Current understanding of increased insulin sensitivity after exercise - emerging candidates. Acta Physiol (Oxf) 202(3):323–335. https://doi.org/10.1111/j.1748-1716.2011.02267.x
Pedersen BK, Steensberg A, Keller P et al (2003) Muscle-derived interleukin-6: lipolytic, anti-inflammatory and immune regulatory effects. Pflugers Arch 446(1):9–16. https://doi.org/10.1007/s00424-002-0981-z
Slentz CA, Tanner CJ, Bateman LA et al (2009) Effects of exercise training intensity on pancreatic β-cell function. Diabetes Care 32(10):1807–1811. https://doi.org/10.2337/dc09-0032
Nieuwoudt S, Fealy CE, Foucher JA et al (2017) Functional high-intensity training improves pancreatic beta-cell function in adults with type 2 diabetes. Am J Physiol Endocrinol Metab 313(3):E314–E320. https://doi.org/10.1152/ajpendo.00407.2016
Heiskanen MA, Motiani KK, Mari A et al (2018) Exercise training decreases pancreatic fat content and improves beta cell function regardless of baseline glucose tolerance: a randomised controlled trial. Diabetologia 61(8):1817–1828. https://doi.org/10.1007/s00125-018-4627-x
Wedell-Neergaard AS, Eriksen L, Gronbaek M, Pedersen BK, Krogh-Madsen R, Tolstrup J (2018) Low fitness is associated with abdominal adiposity and low-grade inflammation independent of BMI. PLoS One 13(1):e0190645. https://doi.org/10.1371/journal.pone.0190645
Wedell-Neergaard AS, Lang Lehrskov L, Christensen RH et al (2019) Exercise-induced changes in visceral adipose tissue mass are regulated by il-6 signaling: a randomized controlled trial. Cell Metab 29(4):844–855 e843. https://doi.org/10.1016/j.cmet.2018.12.007
Pacini G, Mari A (2003) Methods for clinical assessment of insulin sensitivity and beta-cell function. Best Pract Res Clin Endocrinol Metab 17(3):305–322. https://doi.org/10.1016/s1521-690x(03)00042-3
Cersosimo E, Solis-Herrera C, Trautmann ME, Malloy J, Triplitt CL (2014) Assessment of pancreatic beta-cell function: review of methods and clinical applications. Curr Diabetes Rev 10(1):2–42. https://doi.org/10.2174/1573399810666140214093600
Hannon TS, Kahn SE, Utzschneider KM et al (2018) Review of methods for measuring beta-cell function: Design considerations from the Restoring Insulin Secretion (RISE) Consortium. Diabetes Obes Metab 20(1):14–24. https://doi.org/10.1111/dom.13005
Solomon TP, Malin SK, Karstoft K et al (2014) Determining pancreatic beta-cell compensation for changing insulin sensitivity using an oral glucose tolerance test. Am J Physiol Endocrinol Metab 307(9):E822–E829. https://doi.org/10.1152/ajpendo.00269.2014
Utzschneider KM, Prigeon RL, Faulenbach MV et al (2009) Oral disposition index predicts the development of future diabetes above and beyond fasting and 2-h glucose levels. Diabetes Care 32(2):335–341. https://doi.org/10.2337/dc08-1478
Acknowledgements
The authors would like to thank all the included study participants and L. S. Hansen, K. Kofoed, K. Thomsen and A. Blom (The Centre of Inflammation and Metabolism and the Centre for Physical Activity Research, Rigshospitalet, University of Copenhagen), who helped collect data; R. Ø. Nielsen (Institute for Public Health, Aarhus University) for assisting with randomisation and allocation procedures; M. S. Jensen (The Centre of Inflammation and Metabolism and the Centre for Physical Activity Research, Rigshospitalet, University of Copenhagen), who conducted the standard care provided to all participants. Additionally, A.-K. Lundby, L. Foged (The Centre of Inflammation and Metabolism and the Centre for Physical Activity Research, Rigshospitalet, University of Copenhagen) and L. Albæk (Department of Biomedical Sciences, Faculty of Health and Medical Sciences, University of Copenhagen) are acknowledged for the technical assistance with laboratory analyses. Some of the data were submitted as an abstract and presented at the 23rd Annual Congress of the European College of Sport Science in 2018 by M. Ried-Larsen.
Authors’ relationships and activities
AAV was appointed vice president for AstraZeneca’s Translational Research and Early Clinical Development during the study period but remained in the scientific steering committee of this study. MR-L received speakers fee from Novo Nordisk A/S. The remaining authors declare that there are no relationships or activities that might bias, or be perceived to bias, their work.
Contribution statement
MYJ, KK, CSM, KBH, AAV, BKP and MR-L contributed to the study concept and design. MYJ, KK, CSM, KBH and MR-L contributed to acquisition of the data. All authors interpreted the data. MYJ and MR-L performed the statistical analysis. MYJ drafted the manuscript. All authors contributed with critical revision of the manuscript and approved the final version for submission. MYJ and MR-L are the guarantors of this work and, as such, had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis.
Funding
The Centre for Physical Activity Research (CFAS) is supported by grants from TrygFonden (grants ID 101390 and ID 20045). During the study period, the Centre of Inflammation and Metabolism (CIM) was supported by a grant from the Danish National Research Foundation (DNRF55). The project is supported by funding from TrygFonden and additional analyses were supported by funding from Aase and Ejnar Danielsens Fond. This work was also supported by a grant from Rigshospitalet (MYJ). The Contour Next glucose monitors were provided by Bayer A/S, Copenhagen, Denmark. The funders of the study had no role in the study design, data collection, data analysis, data interpretation, or the writing of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Johansen, M.Y., Karstoft, K., MacDonald, C.S. et al. Effects of an intensive lifestyle intervention on the underlying mechanisms of improved glycaemic control in individuals with type 2 diabetes: a secondary analysis of a randomised clinical trial. Diabetologia 63, 2410–2422 (2020). https://doi.org/10.1007/s00125-020-05249-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-020-05249-7