Abstract.
Aim/hypothesis:
We assessed whether dietary supplementation with coenzyme Q10 improves endothelial function of the brachial artery in patients with Type II (non-insulin-dependent) diabetes mellitus and dyslipidaemia.
Methods:
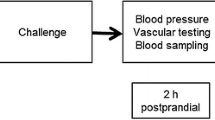
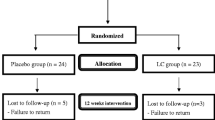
A total of 40 patients with Type II diabetes and dyslipidaemia were randomized to receive 200 mg of coenzyme Q10 or placebo orally for 12 weeks. Endothelium-dependent and independent function of the brachial artery was measured as flow-mediated dilatation and glyceryl-trinitrate-mediated dilatation, respectively. A computerized system was used to quantitate vessel diameter changes before and after intervention. Arterial function was compared with 18 non-diabetic subjects. Oxidative stress was assessed by measuring plasma F2-isoprostane concentrations, and plasma antioxidant status by oxygen radical absorbance capacity.
Results:
The diabetic patients had impaired flow-mediated dilation [3.8 % (SEM 0.5) vs 6.4 % (SEM 1.0), p = 0.016], but preserved glyceryl-trinitrate-mediated dilation, of the brachial artery compared with non-diabetic subjects. Flow-mediated dilation of the brachial artery increased by 1.6 % (SEM 0.3) with coenzyme Q10 and decreased by –0.4 % (SEM 0.5) with placebo (p = 0.005); there were no group differences in the changes in pre-stimulatory arterial diameter, post-ischaemic hyperaemia or glyceryl-trinitrate-mediated dilation response. Coenzyme Q10 treatment resulted in a threefold increase in plasma coenzyme Q10 (p < 0.001) but did not alter plasma F2-isoprostanes, oxygen radical absorbance capacity, lipid concentrations, glycaemic control or blood pressure.
Conclusion/interpretation:
Coenzyme Q10 supplementation improves endothelial function of conduit arteries of the peripheral circulation in dyslipidaemic patients with Type II diabetes. The mechanism could involve increased endothelial release and/or activity of nitric oxide due to improvement in vascular oxidative stress, an effect that might not be reflected by changes in plasma F2-isoprostane concentrations. [Diabetologia (2002) 45: 420–426]
Article PDF
Similar content being viewed by others
Author information
Authors and Affiliations
Additional information
Received: 14 August 2001 and in revised form: 15 November 2001
Rights and permissions
About this article
Cite this article
Watts, G., Playford, D., Croft, K. et al. Coenzyme Q10 improves endothelial dysfunction of the brachial artery in Type II diabetes mellitus. Diabetologia 45, 420–426 (2002). https://doi.org/10.1007/s00125-001-0760-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00125-001-0760-y