Abstract
Objective
To examine for presence of subclinical neuropsychiatric lupus and cerebral atherosclerosis and their correlation with MRI/magnetic resonance angiography (MRA) findings and disease activity and to find if these radiological changes compared with laboratory parameters could be predictive of the early NP affection aiming for early management of these dysfunctions.
Patients and methods
Thirty adult female patients with systemic lupus erythematosus (SLE) were enrolled, with assessment of SLE disease activity using Systemic Lupus Erythematosus Disease Activity Index; psychometric evaluations using the Modified Mini-Mental State Examination to assess for cognitive dysfunction; Hamilton Depression Rating Scale and Hamilton Anxiety Scale to assess for depression and anxiety, respectively; and brain MRI/MRA to detect any changes in subclinical cases.
Results
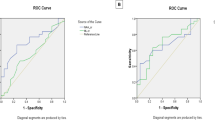
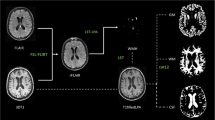
The mean age was 31.7 years. Twelve (40%) patients had positive antiphospholipid (aPL) antibodies with or without clinically evident antiphospholipid syndrome, 22 (73.33%) had different NP manifestations, 13 (43.3%) depression, 15 (50%) anxiety, and 16 (53.3%) cognitive dysfunction. All patients with depression and anxiety and 87.5% of patients with dementia showed abnormalities on MRI. All patients with positive aPL showed abnormalities on MRI, whereas abnormalities on MRI were found in only eight patients with SLE with negative aPL (100 vs. 44.4%). There was a significant correlation between SLE disease activity and both NP manifestations and abnormalities on MRI/MRA, and also between aPL antibodies and NP manifestations. Abnormalities on MRI included discrete white matter lesions, cortical atrophy, and gross infarctions.
Conclusion
Significant number of patients with SLE without overt NP manifestations had subclinical cerebrovascular and cognitive dysfunctions, depression, and anxiety by simple bedside questionnaires. SLE disease activity positively correlates with NP manifestations. The presence of aPL antibodies is a strong risk factor for developing NP SLE. Several distinct brain MRI patterns were observed in patients with active NP SLE, suggestive of different pathogenic mechanisms.
Article PDF
Similar content being viewed by others
References
Hahn B. Lupus eritematoso sistemico. In Fauci AS, Braunwald E, Kasper DL, editors. Harrison medicina interna. 17th ed. Rio de Janeiro: McGraw-Hill Interamericana do Brasil; 2008. pp. 2075–2083
Kozora E, Erkan D, West SG, Filley CM, Zhang L, Ramon G, et al. Site differences in mild cognitive dysfunction (MCD) among patients with systemic lupus erythematosus (SLE). Lupus 2013; 22:73–80
Pamfil C, Fanouriakis A, Damian L, Rinzis M, Sidiropoulos P, Tsivgoulis G, et al. EULAR recommendations for neuropsychiatric systemic lupus erythematosus vs. usual care: results from two European centres. Rheumatology (Oxford) 2015; 54:1270–1278
Anselm Mak A, Man Ho RC, Lau CS. Clinical implications of neuropsychiatric systemic lupus erythematosus. Adv Psychiatr Treat 2009; 15:451–458
Hanly JG. Diagnosis and management of neuropsychiatric SLE. Nat Rev Rheumatol 2014; 10:338–347
Magro-Checa C, Zirkzee EJ, Huizinga TM, Steup-Beekman GM. Management of neuropsychiatric systemic lupus erythematosus: current approaches and future perspectives. Drugs 2016; 76:459–483
Liang M, Corzillius M, Bae S, Lew RA, Fortin PR, Gordon C. The American College of Rheumatology nomenclature and case definitions for neuropsychiatric lupus syndromes. Arthritis Rheum 1999; 42:599–608
Hirohata S, Sakuma Y, Yanagida T, Yoshio T. Association of cerebrospinal fluid anti-Sm antibodies with acute confusional state in systemic lupus erythematosus. Arthritis Res Ther 2014; 16:450
Bertsias G, Ioannidis J, Aringer M, Bollen E, Bombardieri S, Bruce IN, et al. EULAR recommendations for the management of systemic lupus erythematosus with neuropsychiatric manifestations: report of a task force of the EULAR standing committee for clinical affairs. Ann Rheum Dis 2010; 69: 2074–2082
Petri M, Orbai A, Alarcón G, Gordon C, Merrill J, Fortin P, et al. Derivation and validation of the Systemic Lupus International Collaborating Clinics classification criteria for systemic lupus erythematosus. Arthritis Rheum 2012; 64:2677–2686
Bombardier C, Gladman D, Urowitz M, Caron D, Chang C, Austin A, et al. Derivation of the SLEDAI. A disease activity index for lupus patients. Arthritis Rheum 1992; 35:630–640
Folstein M, Folstein S, McHugh P. Mini-mental state. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 1975; 12:189–198
Hamilton M. A rating scale for depression. J Neurol Neurosurg Psychiatry 1960; 23:56–62
Hamilton M. Diagnosis and rating of anxiety. Br J Psychiatry Special Pub 1969; 3:76–79
Popescu A, Kao A. Neuropsychiatric systemic lupus erythematosus. Curr Neuropharmacol 2011; 9:449
Jönsen A, Bengtsson A, Nived O, Ryberg B, Sturfelt G. Outcome of neuropsychiatric systemic lupus erythematosus within a defined Swedish population: increased morbidity but low mortality. Rheumatology 2002; 41:1308–1312
Shehata G, Abdel-Kareem M, Yassin A, El Adl A. Sub-clinical cerebro-vascular cognitive function and mood changes in patients with systemic lupus erythematosus. Open Access Rheumatol 2010; 2:17–25
Nery F, Borba E, Viana V, Hatch J, Soares J, Bonfá E, et al. Prevalence of depressive and anxiety disorders in systemic lupus erythematosus and their association with anti-ribosomal P antibodies. Prog Neuropsychopharmacology Biol Psychiatry 2008; 32:695–700
Unterman A, Nolte J, Boaz M, Abady M, Shoenfeld Y, Zandman-Goddard G. Neuropsychiatric syndromes in systemic lupus erythematosus: a meta-analysis. Semin Arthritis Rheum 2011; 41:1–11
Ainiala H, Dastidar P, Loukkola J, Lehtimäki T, Korpela M, Peltola J, et al. Cerebral MRI abnormalities and their association with neuro-psychiatric manifestations in SLE: a population-based study. Scand J Rheumatol 2005; 34:376–382
Kheirandish M, Faezi ST, Paragomi P, Akhlaghi M, Gharibdoost F, Shahali A, et al. Prevalence and severity of depression and anxiety in patients with systemic lupus erythematosus: an epidemiologic study in Iranian patients. Mod Rheumatol 2014; 25:405–409
Cavaco S, Martins da Silva A, Santos E, Coutinho E, Marinho A, Moreira I, et al. Are cognitive and olfactory dysfunctions in neuropsychiatric lupus erythematosus dependent on anxiety or depression? J Rheumatol 2012; 39:770–776
Arinuma Y, Kikuchi H, Wada T, Nagai T, Tanaka S, Oba H, Hirohata S. Brain MRI in patients with diffuse psychiatric/neuropsychological syndromes in systemic lupus erythematosus. Lupus Sci Med 2014; 1: e000050. doi: 10.1136/lupus-2014-000050s
Jennings J, Sundgren P, Attwood J, McCune J, Maly P. Value of MRI of the brain in patients with systemic lupus erythematosus and neurologic disturbance. Neuroradiology 2004; 46:15–21
Toubi E, Khamashta M, Panarra A, Hughes G. Association of antiphospholipid antibodies with central nervous system disease in systemic lupus erythematosus. Am J Med 1995; 99:397–401
Shehata G, Elserogy Y, Ahmad H, Abdel-KareemM, Al-kabeer A, Rayan M, et al. Multimodal neurophysiological and psychometric evaluation among patients with systemic lupus erythematosus. Int J Gen Med 2011; 4:325
Syuto T, Shimizu A, Takeuchi Y, Tanaka S, Hasegawa M, Nagai Y, et al. Association of antiphosphatidylserine/prothrombin antibodies with neuropsychiatric systemic lupus erythematosus. Clin Rheumatol 2009; 28:841–845
Karassa F, loannidis J, Boki K. Risk factors for central nervous system involvement in systemic lupus erythematosus. J Rheumatol 2000; 93: 169–174
Sanna G, Bertolaccini M, Cuadrado M. Neuro-psychiatric manifestations in systemic lupus erythematosus: prevalence and association with antiphospholipid antibodies. J Rheumatol 2003; 30:985–992
Nery F, Borba E, Hatch J, Soares J, Bonfá E, Neto F. Major depressive disorder and disease activity in systemic lupus erythematosus. Compr Psychiatry 2007; 48:14–19
Toledano P, Sarbu N, Espinosa G, Bargalló N, Cervera R. Neuropsychiatric systemic lupus erythematosus: magnetic resonance imaging findings and correlation with clinical and immunological features. Autoimmunity Rev 2013; 12:1166–1170
Author information
Authors and Affiliations
Corresponding author
Additional information
This is an open access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 3.0 License, which allows others to remix, tweak, and build upon the work non-commercially, as long as the author is credited and the new creations are licensed under the identical terms.
Rights and permissions
This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Morad, C.S., Mansour, H.E., Ibrahim, S.E. et al. Subclinical neuropsychiatric dysfunctions in female patients with systemic lupus erythematosus. Egypt Rheumatol Rehabil 45, 49–56 (2018). https://doi.org/10.4103/err.err_46_17
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.4103/err.err_46_17