Abstract
Background
Oral propranolol accelerates the involution of infantile haemangiomas (IHs). However, it is not clear whether IHs treated with oral propranolol are associated with fewer sequelae than when left untreated.
Objectives
To quantify and describe sequelae associated with IHs treated with oral propranolol, and to explore whether treated IHs are associated with fewer sequelae than untreated IHs.
Materials & Methods
This multicentre, retrospective, cohort study included patients with IH treated with oral propranolol ≥2 mg/kg for at least six months, with photographic images available at baseline and at age 4–5 years. A historical comparison cohort comprised 185 patients with untreated IHs. Main outcomes/measures were: IH features, treatment characteristics and type/degree of sequelae.
Results
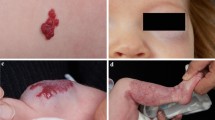
Oral propranolol, most commonly at 2 mg/kg/day (mean duration: nine months), was initiated in 171 patients (mean age: 6.02 months). After treatment, 125 of 171 (73.1%) IHs were associated with no/minimal sequelae. The most common sequelae were telangiectasia (78%), fibrofatty tissue (37%) and anetodermic skin (28%). Deep IHs were associated with significantly fewer sequelae than other subtypes. Ulceration appeared to increase the likelihood of severe sequelae. IHs with a stepped border was associated with more severe sequelae than those with a progressive border (44% versus 27%, p < 0.05). Treated IHs resolved without sequelae or were associated with a sequela that did not need correction in 27.7% more cases than untreated IHs (RR: 1.61; p < 0.001).
Conclusion
Among IHs treated with oral propranolol, 73% resolved without, or were associated with minimal sequelae. Deep IHs were associated fewer sequelae than other sub-types. Oral propranolol decreased the likelihood of IH sequelae requiring correction
Similar content being viewed by others
References
Munden A, Butschek R, Tom WL, et al. Prospective study of infantile haemangiomas: incidence, clinical characteristics and association with placental anomalies. Br J Dermatol 2014; 170: 907–13.
Bauland CG, Lüning TH, Smit JM, Zeebregts CJ, Spauwen PH. Untreated hemangiomas: growth pattern and residual lesions. Plast Reconstr Surg 2011; 127: 1643–8.
Couto RA, Maclellan RA, Zurakowski D, Greene AK. Infantile hemangioma: clinical assessment of the involuting phase and implications for management. Plast Reconstr Surg 2012; 130: 619–24.
Baselga E, Roe E, Coulie J, et al. Risk factors for degree and type of sequelae after involution of untreated hemangiomas of infancy. JAMA Dermatol 2016; 152: 1239–43.
Léauté-Labrèze C, Harper JI, Hoeger PH. Infantile haemangioma. Lancet 2017; 390: 85–94.
Luu M, Frieden IJ. Haemangioma: clinical course, complications and management. Br J Dermatol 2013; 169: 20–30.
Hoeger PH, Harper JI, Baselga E, et al. Treatment of infantile haemangiomas: recommendations of a European expert group. Eur J Pediatr 2015; 174: 855–65.
Baselga Torres E, Bernabéu Wittel J, van Esso Arbolave DL, et al. Spanish consensus on infantile haemangioma. An Pediatr (Barc) 2016; 85: 256–65.
Darrow DH, Greene AK, Mancini AJ, Nopper AJ. Section on dermatology, section on otolaryngology-head & neck surgery, and section on plastic surgery. Diagnosis and management of infantile hemangioma: executive summary. Pediatrics 2015; 136: 786–91.
Cheng CE, Friedlander SF. Infantile hemangiomas, complications and treatments. Semin Cutan Med Surg 2016; 35: 108–16.
Krowchuk DP, Frieden IJ, Mancini AJ, et al. Clinical practice guideline for the management of infantile hemangiomas. Pediatrics 2019; 143: e20183475.
Léauté-Labrèze C, Hoeger P, Mazereeuw-Hautier J, et al. A randomized, controlled trial of oral propranolol in infantile hemangioma. N Engl J Med 2015; 372: 735–46.
Baselga E, Dembowska-Baginska B, Przewratil P, et al. Efficacy of propranolol between 6 and 12 months of age in high-risk infantile hemangioma. Pediatrics 2018; 142: e20173866.
Yu Z, Cai R, Chang L, et al. Clinical and radiological outcomes of infantile hemangioma treated with oral propranolol: a long-term follow-up study. J Dermatol 2019; 46: 376–82.
Coulie J, Coyette M, Moniotte S, Bataille AC, Boon LM. Has propranolol eradicated the need for surgery in the management of infantile hemangioma?. Plast Reconstr Surg 2015; 136: 154.
Chamlin SL, Haggstrom AN, Drolet BA, et al. Multicenter prospective study of ulcerated hemangiomas. J Pediatr 2007; 151: 684–689e1.
Funding
This investigator initiated study was sponsored by Dr Eulalia Baselga. The study received the support of Pierre Fabre Dermatologie.
Author information
Authors and Affiliations
Corresponding author
Additional information
Disclosures
Conflicts of interest: E. Baselga, M. El Hachem, and A. Torrelo received fees from Pierre Fabre Dermatologie. All other authors have no conflicts of interest to disclose.
Additional Contributions
The authors thank David P. Figgitt PhD, ISMPP CMPP™, and Kathy Croom, Content Ed Net, for providing editorial assistance with the manuscript, which was funded by Pierre Fabre Dermatologie, Lavaur, France. The authors thank the patients and their parents/legal guardians for granting permission to publish information and photographs associated with this study.
About this article
Cite this article
Baselga, E., El Hachem, M., Diociaiuti, A. et al. Sequelae following infantile haemangiomas treated with propranolol. Eur J Dermatol 31, 785–790 (2021). https://doi.org/10.1684/ejd.2021.4172
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1684/ejd.2021.4172