Abstract
Background
We sought to determine whether the differences in short-term outcomes between patients undergoing robot-assisted radical prostatectomy (RARP) and those treated with open radical prostatectomy (ORP) differ by race and ethnicity.
Methods
This observational study used New York State Cancer Registry data linked to discharge records and included patients undergoing radical prostatectomy for localized prostate cancer during 2008–2018. We used logistic regression to examine the association between race and ethnicity (non-Hispanic White [NHW], non-Hispanic Black [NHB], Hispanic), surgical approach (RARP, ORP), and postoperative outcomes (major events, prolonged length of stay [pLOS], 30-day re-admission). We tested interaction between race and ethnicity and surgical approach on multiplicative and additive scales.
Results
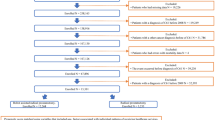
The analytical cohort included 18,926 patients (NHW 14,215 [75.1%], NHB 3195 [16.9%], Hispanic 1516 [8.0%]). The average age was 60.4 years (standard deviation 7.1). NHB and Hispanic patients had lower utilization of RARP and higher risks of postoperative adverse events than NHW patients. NHW, NHB, and Hispanic patients all had reduced risks of adverse events when undergoing RARP versus ORP. The absolute reductions in the risks of major events and pLOS following RARP versus ORP were larger among NHB {relative excess risk due to interaction (RERI): major events −0.32 [95% confidence interval (CI) −0.71 to −0.03]; pLOS −0.63 [95% CI −0.98 to −0.35]) and Hispanic (RERI major events −0.27 [95% CI −0.77 to 0.09]; pLOS −0.93 [95% CI −1.46 to −0.51]) patients than among NHW patients. The interaction was absent on the multiplicative scale.
Conclusions
RARP use has not penetrated and benefited all racial and ethnic groups equally. Increasing utilization of RARP among NHB and Hispanic patients may help reduce disparities in patient outcomes after radical prostatectomy.




Similar content being viewed by others
Data Availability
Data used in this study are subject to a data use agreement (DUA) between NYSDOH and Weill Cornell Medical College, and thus cannot be shared publicly. Investigators interested in the data should work with New York State to establish DUAs.
References
Braveman P. Health disparities and health equity: concepts and measurement. Annu Rev Public Health. 2006;27:167–94.
Phelan JC, Link BG, Tehranifar P. Social conditions as fundamental causes of health inequalities: theory, evidence, and policy implications. J Health Soc Behav. 2010;51(Suppl):S28-40.
Gandaglia G, Sammon JD, Chang SL, et al. Comparative effectiveness of robot-assisted and open radical prostatectomy in the postdissemination era. J Clin Oncol. 2014;32(14):1419–26.
Hu JC, O’Malley P, Chughtai B, et al. comparative effectiveness of cancer control and survival after robot-assisted versus open radical prostatectomy. J Urol. 2017;197(1):115–21.
Leow JJ, Chang SL, Meyer CP, et al. Robot-assisted versus open radical prostatectomy: a contemporary analysis of an all-payer discharge database. Eur Urol. 2016;70(5):837–45.
Trinh QD, Sammon J, Sun M, et al. Perioperative outcomes of robot-assisted radical prostatectomy compared with open radical prostatectomy: results from the nationwide inpatient sample. Eur Urol. 2012;61(4):679–85.
Tewari A, Sooriakumaran P, Bloch DA, Seshadri-Kreaden U, Hebert AE, Wiklund P. Positive surgical margin and perioperative complication rates of primary surgical treatments for prostate cancer: a systematic review and meta-analysis comparing retropubic, laparoscopic, and robotic prostatectomy. Eur Urol. 2012;62(1):1–15.
Trinh QD, Schmitges J, Sun M, et al. Improvement of racial disparities with respect to the utilization of minimally invasive radical prostatectomy in the United States. Cancer. 2012;118(7):1894–900.
Yanamadala S, Chung BI, Hernandez-Boussard TM. Robot-assisted versus open radical prostatectomy utilization in hospitals offering robotics. Can J Urol. 2016;23(3):8279–84.
Ulmer WD, Prasad SM, Kowalczyk KJ, et al. Factors associated with the adoption of minimally invasive radical prostatectomy in the United States. J Urol. 2012;188(3):775–80.
Barocas DA, Gray DT, Fowke JH, et al. Racial variation in the quality of surgical care for prostate cancer. J Urol. 2012;188(4):1279–85.
Schmid M, Meyer CP, Reznor G, et al. Racial differences in the surgical care of medicare beneficiaries with localized prostate cancer. JAMA Oncol. 2016;2(1):85–93.
Sukumar S, Ravi P, Sood A, et al. Racial disparities in operative outcomes after major cancer surgery in the United States. World J Surg. 2015;39(3):634–43.
Sathianathen NJ, Jarosek SL, Fan Y, Krishna SR, Konety BR. Racial disparities in surgical outcomes among males following major urologic cancer surgery. Am J Prev Med. 2018;55(5 Suppl 1):S14–21.
Ward JB, Gartner DR, Keyes KM, Fliss MD, McClure ES, Robinson WR. How do we assess a racial disparity in health? Distribution, interaction, and interpretation in epidemiological studies. Ann Epidemiol. 2019;29:1–7.
Lee J, Gerber D, Aphinyanaphongs Y, Curtin JP, Boyd LR. Laparoscopy decreases the disparity in postoperative complications between black and white women after hysterectomy for endometrial cancer. Gynecol Oncol. 2018;149(1):22–7.
Mahdi H, Lockhart D, Moslemi-Kebria M, Rose PG. Racial disparity in the 30-day morbidity and mortality after surgery for endometrial cancer. Gynecol Oncol. 2014;134(3):510–5.
Damle RN, Flahive JM, Davids JS, Maykel JA, Sturrock PR, Alavi K. Examination of racial disparities in the receipt of minimally invasive surgery among a national cohort of adult patients undergoing colorectal surgery. Dis Colon Rectum. 2016;59(11):1055–62.
New York State Department of Health. New York State Cancer Registry (NYSCR). 2021. Available at: https://www.health.ny.gov/health_care/medicaid/redesign/ehr/registry/nyscr.htm. Accessed 17 Nov 2021.
New York State Department of Health. Statewide Planning and Research Cooperative System (SPARCS). 2021. Available at: https://www.health.ny.gov/statistics/sparcs/. Accessed 17 Nov 2021.
Sanda MG, Cadeddu JA, Kirkby E, et al. Clinically localized prostate cancer: AUA/ASTRO/SUO guideline. Part I: risk stratification, shared decision making, and care options. J Urol. 2018;199(3):683–90.
New York State Department of Health. Race and Ethnicity Codes (Source: CDC Race and Ethnicity Code Set -Version 1.0). 2014. Available at: https://www.health.ny.gov/statistics/sparcs/sysdoc/apprr.htm. Accessed 4 May 2023.
Tameze Y, Low YH. Outpatient robotic surgery: considerations for the anesthesiologist. Adv Anesth. 2022;40(1):15–32.
VanderWeele TJ, Knol MJ. A Tutorial on Interaction. Epidemiol Methods. 2014;3(1):33.
Knol MJ, VanderWeele TJ. Recommendations for presenting analyses of effect modification and interaction. Int J Epidemiol. 2012;41(2):514–20.
McWilliams JM, Meara E, Zaslavsky AM, Ayanian JZ. Differences in control of cardiovascular disease and diabetes by race, ethnicity, and education: U.S. trends from 1999 to 2006 and effects of medicare coverage. Ann Intern Med. 2009;150(8):505–15.
Egan BM, Li J, Sutherland SE, Rakotz MK, Wozniak GD. Hypertension control in the United States 2009–2018: factors underlying falling control rates during 2015 to 2018 across age- and race-ethnicity groups. Hypertension. 2021;78(3):578–87.
Alibhai SM, Leach M, Tomlinson G, et al. 30-day mortality and major complications after radical prostatectomy: influence of age and comorbidity. J Natl Cancer Inst. 2005;97(20):1525–32.
Walz J, Montorsi F, Jeldres C, et al. The effect of surgical volume, age and comorbidities on 30-day mortality after radical prostatectomy: a population-based analysis of 9208 consecutive cases. BJU Int. 2008;101(7):826–32.
Miller J, Smith A, Kouba E, Wallen E, Pruthi RS. Prospective evaluation of short-term impact and recovery of health related quality of life in men undergoing robotic assisted laparoscopic radical prostatectomy versus open radical prostatectomy. J Urol. 2007;178(3 Pt 1):854–8 (Discussion 859).
Pompe RS, Beyer B, Haese A, et al. Postoperative complications of contemporary open and robot-assisted laparoscopic radical prostatectomy using standardised reporting systems. BJU Int. 2018;122(5):801–7.
Jarrin OF, Nyandege AN, Grafova IB, Dong X, Lin H. Validity of race and ethnicity codes in medicare administrative data compared with gold-standard self-reported race collected during routine home health care visits. Med Care. 2020;58(1):e1–8.
New York State Department of Health Statewide Planning and Research Cooperative System (SPARCS). Facility Race/Ethnicity Concordance Reports. 2014. Available at: https://www.health.ny.gov/statistics/sparcs/reports/race_eth/. Accessed 9 May 2023.
Funding
This study was partially supported by the Dean’s Diversity and Healthcare Disparity Research Awards of Weill Cornell Medicine (Principal Investigator: Jialin Mao).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Jason D. Wright has received research funding from Merck and honoraria from UpToDate. Jim C. Hu declares he was a consultant for Intuitive Surgical and Pfizer. Health Research, Inc., where Maria J. Schymura is an employee, received a standard fee for conducting a linkage between discharge records and cancer registry records, however this does not constitute a relevant conflict of interest. Jialin Mao, Jeanine M. Genkinger, Andrew G. Rundle, Tabassum Z. Insaf, and Parisa Tehranifar have no conflicts of interest to declare
Human or Animal Participant
This study was determined as exempt by the Weill Cornell Medicine Institutional Review Board.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Disclaimer The data used to produce this publication were provided by the NYSDOH. However, the conclusions derived and views expressed herein are those of the authors and do not reflect the conclusions or views of NYSDOH. NYSDOH, its employees, officers, and agents make no representation, warranty or guarantee as to the accuracy, completeness, currency, or suitability of the information provided here.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mao, J., Genkinger, J.M., Rundle, A.G. et al. Robot-Assisted Surgery and Racial and Ethnic Disparities in Post-Prostatectomy Outcomes Among Prostate Cancer Patients. Ann Surg Oncol 31, 1373–1383 (2024). https://doi.org/10.1245/s10434-023-14447-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-023-14447-7