Abstract
Background
The aim of this study was to develop a nomogram to predict the risk of developing clinically relevant postoperative pancreatic fistula (CR-POPF) after pancreaticoduodenectomy (PD) using preoperative clinical and imaging data.
Methods
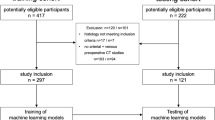
The data of 205 patients were retrospectively analyzed, randomly divided into training (n = 125) and testing groups (n = 80). The patients’ preoperative laboratory indicators, preoperative clinical baseline data, and preoperative imaging data [enhanced computed tomography (CT), enhanced magnetic resonance imaging (MRI)] were collected. Univariate analyses combined with multivariate logistic regression were used to identify the independent risk factors for CR-POPF. These factors were used to train and validate the model and to develop the risk nomogram. The area under the curve (AUC) was used to measure the predictive ability of the models. The integrated discrimination improvement index (IDI) and decision curve analysis (DCA) were used to assess the clinical feasibility of the nomogram in relation to five other models established in literature.
Results
CT visceral fat area (P = 0.014), the pancreatic spleen signal ratio on T1 fat-suppressed MRI sequences (P < 0.001), and CT main pancreatic duct diameter (P = 0.001) were identified as independent prognostic factors and used to develop the model. The final nomogram achieved an AUC of 0.903. The IDI and DCA showed that the nomogram outperformed the other five CR-POPF models in the training and testing cohorts.
Conclusion
The nomogram achieved a superior predictive ability for CR-POPF following PD than other models described in literature. Clinicians can use this simple model to optimize perioperative planning according to the patient’s risk of developing CR-POPF.

Similar content being viewed by others
References
Menahem B, Guittet L, Mulliri A, et al. Pancreaticogastrostomy is superior to pancreaticojejunostomy for prevention of pancreatic fistula after pancreaticoduodenectomy: an updated meta-analysis of randomized controlled trials. Ann Surg. 2015;261:882–7.
Bassi C, Marchegiani G, Dervenis C, et al. The 2016 update of the International Study Group (ISGPS) definition and grading of postoperative pancreatic fistula: 11 years after. Surgery. 2017;161:584–91.
Wente MN, Bassi C, Dervenis C, et al. Delayed gastric emptying (DGE) after pancreatic surgery: a suggested definition by the International Study Group of Pancreatic Surgery (ISGPS). Surgery. 2007;142:761–8.
Callery MP, Pratt WB, Kent TS, et al. A prospectively validated clinical risk score accurately predicts pancreatic fistula after pancreatoduodenectomy. J Am Coll Surg. 2013;216:1–14.
Gaujoux S, Cortes A, Couvelard A, et al. Fatty pancreas and increased body mass index are risk factors of pancreatic fistula after pancreaticoduodenectomy. Surgery. 2010;148:15–23.
Wellner UF, Kayser G, Lapshyn H, et al. A simple scoring system based on clinical factors related to pancreatic texture predicts postoperative pancreatic fistula preoperatively. HPB (Oxford). 2010;12:696–702.
Graham JA, Kayser R, Smirniotopoulos J, et al. Probability prediction of a postoperative pancreatic fistula after a pancreaticoduodenectomy allows for more transparency with patients and can facilitate management of expectations. J Surg Oncol. 2013;108:137–8.
Roberts KJ, Hodson J, Mehrzad H, et al. A preoperative predictive score of pancreatic fistula following pancreatoduodenectomy. HPB (Oxford). 2014;16:620–8.
Lin Z, Tang B, Cai J, et al. Preoperative prediction of clinically relevant postoperative pancreatic fistula after pancreaticoduodenectomy. Eur J Radiol. 2021;139:109693.
Satoi S, Takai S, Matsui Y, et al. Less morbidity after pancreaticoduodenectomy of patients with pancreatic cancer. Pancreas. 2006;33:45–52.
El Nakeeb A, ElGawalby A, Ali MA, et al. Efficacy of octreotide in the prevention of complications after pancreaticoduodenectomy in patients with soft pancreas and non-dilated pancreatic duct: a prospective randomized trial. Hepatobiliary Pancreat Dis Int. 2018;17:59–63.
Vickers AJ, Elkin EB. Decision curve analysis: a novel method for evaluating prediction models. Med Decis Mak. 2006;26:565–74.
Rousson V, Zumbrunn T. Decision curve analysis revisited: overall net benefit, relationships to ROC curve analysis, and application to case-control studies. BMC Med Inform Decis Mak. 2011;11:45.
Kerr KF, Brown MD, Zhu K, Janes H. Assessing the clinical impact of risk prediction models with decision curves: guidance for correct interpretation and appropriate use. J Clin Oncol. 2016;34:2534–40.
Mungroop TH, van Rijssen LB, van Klaveren D, et al. Alternative fistula risk score for pancreatoduodenectomy (a-FRS): design and international external validation. Ann Surg. 2019;269:937–43.
Zhang JY, Huang J, Zhao SY, et al. Risk factors and a new prediction model for pancreatic fistula after pancreaticoduodenectomy. Risk Manag Healthc Policy. 2021;14:1897–906.
Lapshyn H, Petruch N, Thomaschewski M, et al. A simple preoperative stratification tool predicting the risk of postoperative pancreatic fistula after pancreatoduodenectomy. Pancreatology. 2021;21:957–64.
Li Y, Zhou F, Zhu DM, et al. Novel risk scoring system for prediction of pancreatic fistula after pancreaticoduodenectomy. World J Gastroenterol. 2019;25:2650–64.
Gateva AT, Velikova TV, Kamenov ZA. Peroxiredoxin 4 levels in patients with PCOS and/or obesity. J Gynecol Obstet Hum Reprod. 2019;48:739–43.
Di J, Cheng Y, Chang D, Liu Y. A Meta-Analysis of the impact of obesity, metabolic syndrome, insulin resistance, and microbiome on the diagnosis of Barrett’s esophagus. Dig Dis. 2020;38:165–77.
Kountouras J, Doulberis M, Polyzos SA, Katsinelos P. Metabolic syndrome components including high abdominal obesity and sarcopenia in patients with inflammatory bowel disease. Ann Gastroenterol. 2019;32:214.
Spencer M, Yao-Borengasser A, Unal R, et al. Adipose tissue macrophages in insulin-resistant subjects are associated with collagen VI and fibrosis and demonstrate alternative activation. Am J Physiol Endocrinol Metab. 2010;299:E1016-1027.
Tranchart H, Gaujoux S, Rebours V, et al. Preoperative CT scan helps to predict the occurrence of severe pancreatic fistula after pancreaticoduodenectomy. Ann Surg. 2012;256:139–45.
Park CM, Park JS, Cho ES, et al. The effect of visceral fat mass on pancreatic fistula after pancreaticoduodenectomy. J Investig Surg. 2012;25:169–73.
Mitchell DG, Vinitski S, Saponaro S, et al. Liver and pancreas: improved spin-echo T1 contrast by shorter echo time and fat suppression at 1.5 T. Radiology. 1991;178:67–71.
Winston CB, Mitchell DG, Outwater EK, Ehrlich SM. Pancreatic signal intensity on T1-weighted fat saturation MR images: clinical correlation. J Magn Reson Imaging. 1995;5:267–71.
Liang X, Shi LG, Hao J, et al. Risk factors and managements of hemorrhage associated with pancreatic fistula after pancreaticoduodenectomy. Hepatobiliary Pancreat Dis Int. 2017;16:537–44.
Eshmuminov D, Karpovich I, Kapp J, et al. Pancreatic fistulas following distal pancreatectomy are unrelated to the texture quality of the pancreas. Langenbecks Arch Surg. 2021;406:729–34.
Chong E, Ratnayake B, Lee S, et al. Systematic review and meta-analysis of risk factors of postoperative pancreatic fistula after distal pancreatectomy in the era of 2016 International Study Group pancreatic fistula definition. HPB (Oxford). 2021;23:1139–51.
Nathan H, Cameron JL, Goodwin CR, et al. Risk factors for pancreatic leak after distal pancreatectomy. Ann Surg. 2009;250:277–81.
Hashimoto Y, Sclabas GM, Takahashi N, et al. Dual-phase computed tomography for assessment of pancreatic fibrosis and anastomotic failure risk following pancreatoduodenectomy. J Gastrointest Surg. 2011;15:2193–204.
Mathur A, Pitt HA, Marine M, et al. Fatty pancreas: a factor in postoperative pancreatic fistula. Ann Surg. 2007;246:1058–64.
Chu CK, Mazo AE, Sarmiento JM, et al. Impact of diabetes mellitus on perioperative outcomes after resection for pancreatic adenocarcinoma. J Am Coll Surg. 2010;210:463–73.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Disclosure
The authors certify that there are no conflict of interest related to the manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zou, J., Xue, X. & Qin, L. Development of a Nomogram to Predict Clinically Relevant Postoperative Pancreatic Fistula After Pancreaticoduodenectomy on the Basis of Visceral Fat Area and Magnetic Resonance Imaging. Ann Surg Oncol 30, 7712–7719 (2023). https://doi.org/10.1245/s10434-023-13943-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-023-13943-0