Abstract
Purpose
To determine the feasibility and acceptability of using a patient decision aid (DA) for women with elevated breast cancer risk who are considering MRI screening.
Methods
This pilot study employed a mixed methods design to develop, modify, and test an interactive DA. The DA was administered among a consecutive patient sample with an estimated Tyrer-Cuzick v.8 lifetime breast cancer risk of 20% or greater and without a pathologic genetic mutation. The decisional conflict scale was used to measure decisional conflict. Post-intervention provider and patient feedback evaluated shared decision-making, feasibility, and acceptability.
Results
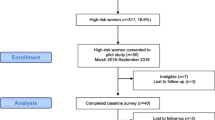
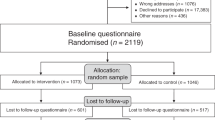
Twenty-four patients participated, with a median age of 44 years. Prior to DA use, sixteen patients (67%) were unsure whether to add MRI to their screening, six patients elected MRI (25%), and two patients declined MRI (8%). Following DA use, thirteen of sixteen of the initially undecided participants (81%) established a preference, with eleven electing to add MRI screening. Of participants with an initial preference, all maintained the same decision following use of the DA. Prior to the DA, the median decisional conflict score among participants was 25% (range 0–60%) compared with 0% (range 0–25%) after the DA. Healthcare providers reported that the DA was useful and easily incorporated into clinical workflow.
Conclusions
This pilot study shows that there may be a benefit to DA utilization in the high-risk breast cancer clinic to guide shared decision-making in establishing a screening preference. The findings warrant further research to test the use of the DA in a larger, multi-site trial.


Similar content being viewed by others
References
Saslow D, Boetes C, Burke W, et al. American Cancer Society Guidelines for breast screening with MRI as an adjunct to mammography. CA Cancer J Clin. 2007;57(2):75–89.
National Comprehensive Cancer Network. NCCN Guidelines for breast cancer screening and diagnosis. 2023. https://www.nccn.org. Accessed 18 Apr 2023.
Jiang X, McGuinness JE, Sin M, Silverman T, Kukafka R, Crew KD. Identifying women at high risk for breast cancer using data from the electronic health record compared with self-report. JCO Clin Cancer Inform. 2019;3:1–8.
Freedman A, Graubard B, Rao S, McCaskill-Stevens W, Ballard-Barbash R, Gail M. Estimates of the number of U.S. women who could benefit from tamoxifen for breast cancer chemoprevention. J Natl Cancer Inst. 2003;95(7):526–32.
Breast Cancer Surveillance Consortium. 2023. http://www.bcsc-research.org/. Accessed 18 Apr 2023.
Prummel MV, Done SJ, Muradali D, et al. Digital compared to screen-film mammography: breast cancer prognostic features in an organized screening program. Breast Cancer Res Treat. 2014;147(2):389–99.
Othman E, Wang J, Sprague BL, et al. Comparison of false positive rates for screening breast magnetic resonance imaging (MRI) in high risk women performed on stacked versus alternating schedules. SpringerPlus. 2015;4(1):77. https://doi.org/10.1186/s40064-015-0793-1.
Brewer NT, Salz T, Lillie SE. Systematic review: the long-term effects of false-positive mammograms. Ann Intern Med. 2007;146(7):502–10.
Dabbous FM, Dolecek TA, Berbaum ML, et al. Impact of a false-positive screening mammogram on subsequent screening behavior and stage at breast cancer diagnosis. Cancer Epidemiol Biomark Prev. 2017;26(3):397–403.
Nelson HD, Pappas M, Cantor A, Griffin J, Daeges M, Humphrey L. Harms of breast cancer screening: systematic review to update the 2009 U.S. preventive services task force recommendation. Ann Intern Med. 2016;164(4):256–67.
Partnering with patients to drive shared decisions, better value, and care improvement: Workshop Proceedings. National Academies Press; 2014.
Breast Screening Decisions. 2023. https://bsd.weill.cornell.edu/#/. Accessed 18 Apr 2023.
Ikonopedia IBIS: online Tyrer-Cuzick model breast cancer risk evaluation tool. 2023. https://ibis.ikonopedia.com/. Accessed 12 Apr 2023.
Hollen PJ, Gralla RJ, Jones RA, et al. A theory-based decision aid for patients with cancer: results of feasibility and acceptability testing of DecisionKEYS for cancer. Support Care Cancer. 2013;21(3):889–99.
Janis IL, Mann L. A theoretical framework for decision counseling. Yale University Press; 1982.
Janis IL, Mann L. Decision making: a psychological analysis of conflict, choice, and commitment. 8th edn. Free Press; 1979.
Chu C, Yoder J, Smolkin M, Hollen PJ, Dengel LT. A decision aid for patients with minimally suspicious screening mammograms: a pilot study. Oncol Nurs Forum. 2022;49(5):471–9.
O’Connor AM, Rostom A, Fiset V, et al. Decision aids for patients facing health treatment or screening decisions: systematic review. BMJ. 1999;319(7212):731–4.
O’Connor AM, Jacobsen MJ, Stacey D. An evidence-based approach to managing women’s decisional conflict. J Obstet Gynecol Neonatal Nurs. 2002;31(5):570–81.
O’Connor A. Decisional conflict scale. 2003. https://decisionaid.ohri.ca/docs/develop/User_Manuals/UM_decisional_conflict.pdf.
RStudio Team (2020). RStudio: integrated development for R. RStudio, PBC, Boston, MA. http://www.rstudio.com/.
Stacey D, Légaré F, Lewis K, et al. Decision aids for people facing health treatment or screening decisions. Cochrane Database Syst Rev. 2017. https://doi.org/10.1002/14651858.CD001431.pub5.
Fowler FJ, Gallagher PM, Drake KM, Sepucha KR. Decision dissonance: evaluating an approach to measuring the quality of surgical decision making. Jt Comm J Qual Patient Saf. 2013;39(3):136–44.
Frongillo M, Feibelmann S, Belkora J, Lee C, Sepucha K. Is there shared decision making when the provider makes a recommendation? Patient Educ Couns. 2013;90(1):69–73.
Rosenberg SM, Tracy MS, Meyer ME, et al. Perceptions, knowledge, and satisfaction with contralateral prophylactic mastectomy among young women with breast cancer: a cross-sectional survey. Ann Intern Med. 2013;159(6):373–81.
Sepucha K, Feibelmann S, Chang Y, et al. Factors associated with the quality of patients’ surgical decisions for treatment of hip and knee osteoarthritis. J Am Coll Surg. 2013;217(4):694–701.
Sepucha KR, Borkhoff CM, Lally J, et al. Establishing the effectiveness of patient decision aids: key constructs and measurement instruments. BMC Med Inform Decis Mak. 2013;13(2):1–11. https://doi.org/10.1186/1472-6947-13-S2-S12.
Joseph-Williams N, Edwards A, Elwyn G. Power imbalance prevents shared decision making. BMJ. 2014;348:g3178. https://doi.org/10.1136/bmj.g3178.
Légaré F, Ratté S, Gravel K, Graham ID. Barriers and facilitators to implementing shared decision-making in clinical practice: update of a systematic review of health professionals’ perceptions. Patient Educ Couns. 2008;73(3):526–35.
Acknowledgment
Financial support for this study was provided entirely by a Grant from the University of Virginia, Internal Department of Surgery Grant.
Funding
Research supported by a Pilot Project Grant from the University of Virginia, Internal Department of Surgery Grant. The funding agreement ensured the authors’ independence in designing the study, interpreting the data, writing, and publishing the report.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chu, C., Smith, C.E., Gorski, J. et al. Implementation of a Novel Patient Decision Aid for Women with Elevated Breast Cancer Risk Who Are Considering MRI Screening: A Pilot Study. Ann Surg Oncol 30, 6152–6158 (2023). https://doi.org/10.1245/s10434-023-13901-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-023-13901-w