Abstract
Background
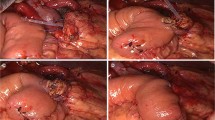
Postoperative pancreatic fistulas (POPFs) are considered inevitable in some patients after pancreaticoduodenectomy (PD), and measures to minimize their clinical impact are needed. Postpancreatectomy hemorrhage (PPH) and intra-abdominal abscess (IAA) are the most severe POPF-related complications, and concomitant leakage of contaminated intestinal content is considered the main cause. An innovative method, modified non-duct-to-mucosa pancreaticojejunostomy (TPJ), was created to prevent concomitant leakage of intestinal content, and its effectiveness was compared between two periods.
Methods
All PD patients undergoing pancreaticojejunostomy from 2012 to 2021 were included. The TPJ group consisted of 529 patients recruited from January 2018 to December 2021. A total of 535 patients receiving the conventional method (CPJ) from January 2012 to June 2017 were used as a control group. PPH and POPF were defined according to the International Study Group of Pancreatic Surgery definition, but only PPH grade C was included for analysis. An IAA was defined as a collection of postoperative fluid managed by CT-guided drainage with documental culture.
Results
There were no significant differences in the rate of POPF between the two groups (46.0% vs. 44.8%; p = 0.700). Furthermore, the percentages of bile in the drainage fluid in the TPJ and CPJ groups were 2.3% and 9.2%, respectively (p < 0.001). Lower proportions of PPH (0.9% vs. 6.5%; p < 0.001) and IAA (5.7% vs. 10.8%; p < 0.001) were observed for TPJ than for CPJ. On adjusted models, TPJ was significantly associated with a lower rate of PPH (odds ratio [OR] 0.132, 95% confidence interval [CI] 0.051–0.343; p < 0.001) and IAA (OR 0.514, 95% CI 0.349–0.758; p = 0.001) than CPJ.
Conclusions
TPJ is feasible to be performed and is associated with a similar rate of POPF but a lower percentage of concomitant bile in the drainage fluid and subsequent rates of PPH and IAA than CPJ.

Similar content being viewed by others
References
Fernandez-del Castillo C, Morales-Oyarvide V, McGrath D, et al. Evolution of the Whipple procedure at the Massachusetts General Hospital. Surgery. 2012;152(3 Suppl 1):S56-63.
Cameron JL, Riall TS, Coleman J, Belcher KA. One thousand consecutive pancreaticoduodenectomies. Ann Surg. 2006;244(1):10–5.
O’Mahoney PRA, Yeo HL, Sedrakyan A, et al. Centralization of pancreatoduodenectomy a decade later: impact of the volume-outcome relationship. Surgery. 2016;159(6):1528–38.
Grobmyer SR, Kooby D, Blumgart LH, Hochwald SN. Novel pancreaticojejunostomy with a low rate of anastomotic failure-related complications. J Am Coll Surg. 2010;210(1):54–9.
Olakowski M, Grudzinska E, Mrowiec S. Pancreaticojejunostomy-a review of modern techniques. Langenbecks Arch Surg. 2020;405(1):13–22.
Schuh F, Mihaljevic AL, Probst P, et al. A simple classification of pancreatic duct size and texture predicts postoperative pancreatic fistula: a classification of the International Study Group of Pancreatic Surgery (ISGPS). Ann Surg. 2021. https://doi.org/10.1097/SLA.000000000000485.
Honda G, Kurata M, Okuda Y, et al. Novel device for pancreaticojejunostomy via a pure laparoscopic approach. J Am Coll Surg. 2013;216(6):e73-76.
Cheng Q, Zhang B, Zhang Y, et al. Predictive factors for complications after pancreaticoduodenectomy. J Surg Res. 2007;139(1):22–9.
Wente MN, Veit JA, Bassi C, et al. Postpancreatectomy hemorrhage (PPH): an International Study Group of Pancreatic Surgery (ISGPS) definition. Surgery. 2007;142(1):20–5.
Tien YW, Wu YM, Liu KL, Ho CM, Lee PH. Angiography is indicated for every sentinel bleed after pancreaticoduodenectomy. Ann Surg Oncol. 2008;15(7):1855–61.
Tien YW, Lee PH, Yang CY, Ho MC, Chiu YF. Risk factors of massive bleeding related to pancreatic leak after pancreaticoduodenectomy. J Am Coll Surg. 2005;201(4):554–9.
Andrianello S, Marchegiani G, Malleo G, et al. Pancreaticojejunostomy with externalized stent vs pancreaticogastrostomy with externalized stent for patients with high-risk pancreatic anastomosis: a single-center, phase 3, randomized clinical trial. JAMA Surg. 2020;155(4):313–21.
Floortje van Oosten A, Smits FJ, van den Heuvel DAF, van Santvoort HC, Molenaar IQ. Diagnosis and management of postpancreatectomy hemorrhage: a systematic review and meta-analysis. HPB (Oxford). 2019;21(8):953–61.
Lin YJ, Ho TW, Wu CH, et al. Specific bile microorganisms caused by intra-abdominal abscess on pancreaticoduodenectomy patients: a retrospective cohort study. Curr Oncol. 2021;29(1):111–21.
Clavien PA, Barkun J, de Oliveira ML, et al. The Clavien–Dindo classification of surgical complications: five-year experience. Ann Surg. 2009;250(2):187–96.
Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240(2):205–13.
Bassi C, Marchegiani G, Dervenis C, et al. The 2016 update of the International Study Group (ISGPS) definition and grading of postoperative pancreatic fistula: 11 years after. Surgery. 2017;161(3):584–91.
Deyo RA, Cherkin DC, Ciol MA. Adapting a clinical comorbidity index for use with ICD-9-CM administrative databases. J Clin Epidemiol. 1992;45(6):613–9.
Wu JM, Ho TW, Yen HH, et al. Endoscopic retrograde biliary drainage causes intra-abdominal abscess in pancreaticoduodenectomy patients: an important but neglected risk factor. Ann Surg Oncol. 2019;26(4):1086–92.
Callery MP, Pratt WB, Kent TS, Chaikof EL, Vollmer CM Jr. A prospectively validated clinical risk score accurately predicts pancreatic fistula after pancreatoduodenectomy. J Am Coll Surg. 2013;216(1):1–14.
Bassi C, Falconi M, Molinari E, et al. Duct-to-mucosa versus end-to-side pancreaticojejunostomy reconstruction after pancreaticoduodenectomy: results of a prospective randomized trial. Surgery. 2003;134(5):766–71.
Kanda M, Fujii T, Kodera Y, Nagai S, Takeda S, Nakao A. Nutritional predictors of postoperative outcome in pancreatic cancer. Br J Surg. 2011;98(2):268–74.
Pedrazzoli S, Liessi G, Pasquali C, Ragazzi R, Berselli M, Sperti C. Postoperative pancreatic fistulas: preventing severe complications and reducing reoperation and mortality rate. Ann Surg. 2009;249(1):97–104.
Kwon HJ, Ha HT, Choi YY, Kim SG. The effects of the end-to-side inverted mattress pancreaticojejunostomy on postoperative pancreatic fistula: a single surgeon’s experience. Ann Surg Treat Res. 2015;89(2):61–7.
Yao GL, An MJ, Fan YG. Invaginated duct to mucosa pancreaticojejunostomy reduce postoperative pancreatic leakage: a matched case-controlled study. Medicine (Baltimore). 2021;100(49):e27834.
Kelemen D, Papp R, Kaszás B, Bíró Z, Vereczkei A. Pancreatojejunostomy with modified purse-string suture technique. Langenbecks Arch Surg. 2016;401(3):403–7.
Kusnierz K, Mrowiec S, Lampe P. A comparison of two invagination techniques for pancreatojejunostomy after pancreatoduodenectomy. Gastroenterol Res Pract. 2015;2015:894292.
Buc E, Flamein R, Golffier C, et al. Peng’s binding pancreaticojejunostomy after pancreaticoduodenectomy: a French prospective study. J Gastrointest Surg. 2010;14(4):705–10.
Morelli L, Di Franco G, Guadagni S, et al. Technical details and results of a modified end-to-side technique of pancreatojejunostomy: a personal series of 100 patients. J Gastrointest Surg. 2017;21(12):2090–9.
Fujii T, Sugimoto H, Yamada S, et al. Modified Blumgart anastomosis for pancreaticojejunostomy: technical improvement in matched historical control study. J Gastrointest Surg. 2014;18(6):1108–15.
Wang M, Xu S, Zhang H, Peng S, Zhu F, Qin R. Imbedding pancreaticojejunostomy used in pure laparoscopic pancreaticoduodenectomy for nondilated pancreatic duct. Surg Endosc. 2017;31(4):1986–92.
Isselbacher KJ, Senior JR. The intestinal absorption of carbohydrate and fat. Gastroenterology. 1964;46:287–98.
Elmslie R. The effect of bile on the activation of trypsinogen and the activity of trypsin in pancreatic juice. Br J Surg. 1965;52:465–70.
Sarkany RP, Moreland BH. Enhancement of the autocatalytic activation of trypsinogen to trypsin by bile and bile acids. Biochim Biophys Acta. 1985;839(3):262–7.
Kitamoto Y, Yuan X, Wu Q, McCourt DW, Sadler JE. Enterokinase, the initiator of intestinal digestion, is a mosaic protease composed of a distinctive assortment of domains. Proc Natl Acad Sci USA. 1994;91(16):7588–92.
Muili KA, Wang D, Orabi AI, et al. Bile acids induce pancreatic acinar cell injury and pancreatitis by activating calcineurin. J Biol Chem. 2013;288(1):570–80.
Luthen RE, Niederau C, Grendell JH. Effects of bile and pancreatic digestive enzymes on permeability of the pancreatic duct system in rabbits. Pancreas. 1993;8(6):671–81.
Mussle B, Hempel S, Kahlert C, Distler M, Weitz J, Welsch T. Prognostic impact of bacterobilia on morbidity and postoperative management after pancreatoduodenectomy: a systematic review and meta-analysis. World J Surg. 2018;42(9):2951–62.
Mintziras I, Maurer E, Kanngiesser V, Lohoff M, Bartsch DK. Preoperative bacterobilia is an independent risk factor of SSIs after partial PD. Dig Surg. 2020;37(5):428–35.
Acknowledgment
This study was supported by grant number 110-2221-E-002 -014 -MY3 from the Ministry of Science and Technology, Taiwan, which had no role in the study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wu, JM., Lin, YJ., Wu, CH. et al. Novel Non-duct-to-Mucosa Pancreaticojejunostomy Reconstruction After Pancreaticoduodenectomy: Focus on the Occurrence of Post-pancreatectomy Hemorrhage and Intra-abdominal Abscess. Ann Surg Oncol 30, 5063–5070 (2023). https://doi.org/10.1245/s10434-023-13114-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-023-13114-1