Abstract
Background
The prognostic impact of renal cell carcinoma (RCC) morphotype remains unclear in patients who undergo partial nephrectomy (PN). Our objective was to determine the risk factors for recurrence after PN, including RCC morphotype.
Methods
Patients with RCC who had undergone PN were extracted from the prospective, national French database, UroCCR. Patients with genetic predisposition, bilateral or multiple tumours, and those who had undergone secondary totalization were excluded. Primary endpoint was 5-year, recurrence-free survival (RFS), and secondary endpoint was overall survival (OS). Risk factors for recurrence were assessed by multivariable Cox regression analysis.
Results
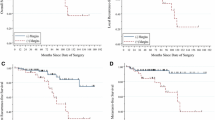
Overall, 2,767 patients were included (70% male; median age: 61 years [interquartile range (IQR) 51-69]). Most (71.5%) of the PN procedures were robot-assisted. Overall, 2,573 (93.0%) patients were recurrence free, and 74 died (2.7%). Five-year RFS was 84.9% (IQR 82.4-87.4). A significant difference in RFS was observed between RCC morphotypes (p < 0.001). Surgical margins (hazard ratio [HR] = 2.0 [95% confidence interval (CI): 1.3-3.2], p < 0.01), pT stage >1 (HR = 2.6 [95% CI: 1.8-3.7], p < 0.01]) and Fuhrmann grade >2 (HR = 1.9 [95% CI: 1.4-2.6], p < 0.001) were risk factors for recurrence, whereas chromophobe subtype was a protective factor (HR = 0.08 [95% CI: 0.01-0.6], p = 0.02). Five-year OS was 94.0% [92.4-95.7], and there were no significant differences between RCC subgroups (p = 0.06). The main study limitation was its design (multicentre national database), which may be responsible for declarative bias.
Conclusions
Chromophobe morphotype was significantly associated with better RFS in RCC patients who underwent PN. Conversely, pT stage, Fuhrman group and positive surgical margins were risk factors for recurrence.


Similar content being viewed by others
References
Moch H, Cubilla AL, Humphrey PA, Reuter VE, Ulbright TM. The 2016 WHO classification of Tumours of the urinary system and male genital organs-part A: renal, penile, and testicular Tumours. Eur Urol. 2016;70(1):93–105. https://doi.org/10.1016/j.eururo.2016.02.029.
Ljungberg B, Albiges L, Abu-Ghanem Y, et al. European association of urology guidelines on renal cell carcinoma: The 2019 update. Eur Urol. 2019;75(5):799–810. https://doi.org/10.1016/j.eururo.2019.02.011.
Muglia VF, Prando A. Renal cell carcinoma: histological classification and correlation with imaging findings. Radiol Bras. 2015;48(3):166–74. https://doi.org/10.1590/0100-3984.2013.1927.
Ficarra V, Brunelli M, Cheng L, et al. Prognostic and therapeutic impact of the histopathologic definition of parenchymal epithelial renal tumors. Eur Urol. 2010;58(5):655–68. https://doi.org/10.1016/j.eururo.2010.08.001.
Abdel-Rahman O. Impact of tumor size on the outcome of patients with small renal cell carcinoma. Expert Rev Anticancer Ther. 2017;17(8):769–73. https://doi.org/10.1080/14737140.2017.1340838.
Leibovich BC, Lohse CM, Crispen PL, et al. Histological subtype is an independent predictor of outcome for patients with renal cell carcinoma. J Urol. 2010;183(4):1309–15. https://doi.org/10.1016/j.juro.2009.12.035.
Kuthi L, Jenei A, Hajdu A, et al. Prognostic factors for renal cell carcinoma subtypes diagnosed according to the 2016 WHO renal tumor classification: a study involving 928 patients. Pathol Oncol Res POR. 2017;23(3):689–98. https://doi.org/10.1007/s12253-016-0179-x.
Touijer K, Jacqmin D, Kavoussi LR, et al. The expanding role of partial nephrectomy: a critical analysis of indications, results, and complications. Eur Urol. 2010;57(2):214–22. https://doi.org/10.1016/j.eururo.2009.10.019.
Nguyen DP, Vertosick EA, Corradi RB, et al. Histological subtype of renal cell carcinoma significantly affects survival in the era of partial nephrectomy. Urol Oncol. 2016;34(6):259.e1-8. https://doi.org/10.1016/j.urolonc.2016.01.005.
Bigot P, Bernhard J-C, Gill IS, et al. The subclassification of papillary renal cell carcinoma does not affect oncological outcomes after nephron sparing surgery. World J Urol. 2016;34(3):347–52. https://doi.org/10.1007/s00345-015-1634-0.
Kutikov A, Egleston BL, Wong Y-N, Uzzo RG. Evaluating overall survival and competing risks of death in patients with localized renal cell carcinoma using a comprehensive nomogram. J Clin Oncol. 2010;28(2):311–7. https://doi.org/10.1200/JCO.2009.22.4816.
Bensalah K, Bigot P, Albiges L, et al. French ccAFU guidelines - update 2020–2022: management of kidney cancer. Progres En Urol J Assoc Francaise Urol Soc Francaise Urol. 2020;30(12S):S2-51. https://doi.org/10.1016/S1166-7087(20)30749-1.
Cheville JC, Lohse CM, Zincke H, Weaver AL, Blute ML. Comparisons of outcome and prognostic features among histologic subtypes of renal cell carcinoma. Am J Surg Pathol. 2003;27(5):612–24. https://doi.org/10.1097/00000478-200305000-00005.
Abdel-Rahman O. Impact of histological subtype on outcomes of renal cell carcinoma patients. J Drug Assess. 2018;7(1):14–20. https://doi.org/10.1080/21556660.2018.1439831.
Keegan KA, Schupp CW, Chamie K, Hellenthal NJ, Evans CP, Koppie TM. Histopathology of surgically treated renal cell carcinoma: survival differences by subtype and stage. J Urol. 2012;188(2):391–7. https://doi.org/10.1016/j.juro.2012.04.006.
Volpe A, Novara G, Antonelli A, et al. Chromophobe renal cell carcinoma (RCC): oncological outcomes and prognostic factors in a large multicentre series. BJU Int. 2012;110(1):76–83. https://doi.org/10.1111/j.1464-410X.2011.10690.x.
Teloken PE, Thompson RH, Tickoo SK, et al. Prognostic impact of histological subtype on surgically treated localized renal cell carcinoma. J Urol. 2009;182(5):2132–6. https://doi.org/10.1016/j.juro.2009.07.019.
Przybycin CG, Cronin AM, Darvishian F, et al. Chromophobe renal cell carcinoma: a clinicopathologic study of 203 tumors in 200 patients with primary resection at a single institution. Am J Surg Pathol. 2011;35(7):962–70. https://doi.org/10.1097/PAS.0b013e31821a455d.
Huang WC, Levey AS, Serio AM, et al. Chronic kidney disease after nephrectomy in patients with renal cortical tumours: a retrospective cohort study. Lancet Oncol. 2006;7(9):735–40. https://doi.org/10.1016/S1470-2045(06)70803-8.
Bensalah K, Pantuck AJ, Rioux-Leclercq N, et al. Positive surgical margin appears to have negligible impact on survival of renal cell carcinomas treated by nephron-sparing surgery. Eur Urol. 2010;57(3):466–73. https://doi.org/10.1016/j.eururo.2009.03.048.
Hakam N, Heidar NA, Khabsa J, Hneiny L, Akl EA, Khauli R. Does a positive surgical margin after nephron sparing surgery affect oncological outcome in renal cell carcinoma? A systematic review and meta-analysis Urology. 2021;S0090–4295(21):00562–8. https://doi.org/10.1016/j.urology.2021.04.058.
Richard PO, Lavallée LT, Pouliot F, et al. Is routine renal tumor biopsy associated with lower rates of benign histology following nephrectomy for small renal masses? J Urol. 2018;200(4):731–6. https://doi.org/10.1016/j.juro.2018.04.015.
Van Poppel H, Da Pozzo L, Albrecht W, et al. A prospective, randomised EORTC intergroup phase 3 study comparing the oncologic outcome of elective nephron-sparing surgery and radical nephrectomy for low-stage renal cell carcinoma. Eur Urol. 2011;59(4):543–52. https://doi.org/10.1016/j.eururo.2010.12.013.
Sun M, Trinh Q-D, Bianchi M, et al. A non-cancer-related survival benefit is associated with partial nephrectomy. Eur Urol. 2012;61(4):725–31. https://doi.org/10.1016/j.eururo.2011.11.047.
Mejean A, Hopirtean V, Bazin JP, et al. Prognostic factors for the survival of patients with papillary renal cell carcinoma: meaning of histological typing and multifocality. J Urol. 2003;170(3):764–7. https://doi.org/10.1097/01.ju.0000081122.57148.ec.
Yoo S, You D, Jeong IG, et al. Histologic subtype needs to be considered after partial nephrectomy in patients with pathologic T1a renal cell carcinoma: papillary vs. clear cell renal cell carcinoma. J Cancer Res Clin Oncol. 2017;143(9):1845–51. https://doi.org/10.1007/s00432-017-2430-6.
Wallis CJD, Garbens A, Chopra S, Gill IS, Satkunasivam R. Robotic Partial Nephrectomy: Expanding Utilization. Advancing Innovation J Endourol. 2017;31(4):348–54. https://doi.org/10.1089/end.2016.0639.
Cacciamani GE, Medina LG, Gill T, et al. Impact of surgical factors on robotic partial nephrectomy outcomes: comprehensive systematic review and meta-analysis. J Urol. 2018;200(2):258–74. https://doi.org/10.1016/j.juro.2017.12.086.
Zhang X, Shen Z, Zhong S, Zhu Z, Wang X, Xu T. Comparison of peri-operative outcomes of robot-assisted vs laparoscopic partial nephrectomy: a meta-analysis. BJU Int. 2013;112(8):1133–42. https://doi.org/10.1111/bju.12255.
Vartolomei MD, Matei DV, Renne G, et al. Robot-assisted partial nephrectomy: 5-yr oncological outcomes at a single European tertiary cancer center. Eur Urol Focus. 2019;5(4):636–41. https://doi.org/10.1016/j.euf.2017.10.005.
Funding
The authors declare no funding for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
The authors have no potential conflicts of interest to report.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tabourin, T., Pinar, U., Parra, J. et al. Impact of Renal Cell Carcinoma Histological Variants on Recurrence After Partial Nephrectomy: A Multi-Institutional, Prospective Study (UROCCR Study 82). Ann Surg Oncol 29, 7218–7228 (2022). https://doi.org/10.1245/s10434-022-12052-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-022-12052-8