Abstract
Background
Accurate measurement of healthcare costs is required to assess and improve the value of oncology care.
Objectives
We aimed to determine the cost of breast cancer care provision across collaborating health care organizations.
Methods
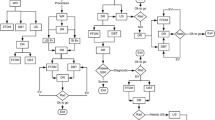
We used time-driven activity-based costing (TDABC) to calculate the complete cost of breast cancer care—initial treatment planning, chemotherapy, radiation therapy, surgical resection and reconstruction, and ancillary services (e.g., psychosocial oncology, physical therapy)—across multiple hospital sites. Data were collected between December 2019 and February 2020. TDABC steps involved (1) developing process maps for care delivery pathways; (2) determine capacity cost rates for staff, medical equipment, and hospital space; (3) measure the time required for each process step, both manually through clinic observation and using data from the Real-Time Location System (RTLS); and (4) calculate the total cost of care delivery.
Results
Surgical care costs ranged from $1431 for a lumpectomy to $12,129 for a mastectomy with prepectoral implant reconstruction. Radiation therapy was costed at $1224 for initial simulation and patient education, and $200 for each additional treatment. Base costs for chemotherapy delivery were $382 per visit, with additional costs driven by chemotherapy agent(s) administered. Personnel expenses were the greatest contributor to the cost of surgical care, except in mastectomy with implant reconstruction, where device costs equated to up to 60% of the cost of surgery.
Conclusion
The cost of complete breast cancer care depended on (1) treatment protocols; (2) patient choice of reconstruction; and (3) the need for ancillary services (e.g., physical therapy). Understanding the actual costs and cost drivers of breast cancer care delivery may better inform resource utilization to lower the cost and improve the quality of care.





Similar content being viewed by others
Change history
21 September 2021
A Correction to this paper has been published: https://doi.org/10.1245/s10434-021-10795-4
References
Akhavan S, Ward L, Bozic KJ. Time-driven activity-based costing more accurately reflects costs in arthroplasty surgery. ClinOrthop Relat Res. 2016;474(1):8–15. https://doi.org/10.1007/s11999-015-4214-0.
American College of Surgeons. ACS THRIVE (Transforming Health care Resources to Increase Value and Efficiency). Available at: https://www.facs.org/Quality-Programs/ACS-THRIVE. Accessed 16 Jan 2020.
American College of Surgeons. ACS risk calculator (National Surgical Quality Improvement Program, NSQIP). Available at: https://riskcalculator.facs.org/RiskCalculator/index.jsp. Accessed 25 Jan 2020.
Anderson SR, Kaplan RS. Time-driven activity-based costing. Harvard Business Review. 2004. Available at: https://hbr.org/2004/11/time-driven-activity-based-costing. Accessed 16 Jan 2020.
Blumen H, Fitch K, Polkus V. Comparison of treatment costs for breast cancer, by tumor stage and type of service. Am Health Drug Benefits. 2016;9(1):23–31.
Cafardi S, Centers for medicare and medicaid services. First Annual Report from the Evaluation of the Oncology Care Model: Baseline Period Final. 2018. Available at: https://downloads.cms.gov/files/cmmi/ocm-baselinereport.pdf. Accessed 25 Jan 2020.
Center for medicare & medicaid innovation. Oncology Care Model. 2015. Available at: https://innovation.cms.gov/initiatives/oncology-care/. Accessed 16 Jan 2020.
Center for Medicare & Medicaid Innovation. Radiation Oncology Model. 2019. Available at: https://innovation.cms.gov/initiatives/radiation-oncology-model/. Accessed 25 Jan 2020.
Centers for Medicare and Medicaid Services. Healthcare Cost Report Information System (HCRIS). 2020. Available at: https://www.cms.gov/Research-Statistics-Data-and-Systems/Downloadable-Public-Use-Files/Cost-Reports/. Accessed 29 Jan 2020.
Eappen S, Lane BH, Rosenberg B, et al. Relationship between occurrence of surgical complications and hospital finances. JAMA. 2013;309(15):1599–606. https://doi.org/10.1001/jama.2013.2773.
French KE, Albright HW, Frenzel JC, et al. Measuring the value of process improvement initiatives in a preoperative assessment center using time-driven activity-based costing. Healthcare. 2013;1(3–4):136–42. https://doi.org/10.1016/j.hjdsi.2013.07.007.
Gooch K. 34% of healthcare payments were tied to value-based care last year, report finds. 2018. Available at: https://www.beckershospitalreview.com/finance/34-of-healthcare-payments-were-tied-to-value-based-care-last-year-report-finds.html. Accessed 16 Jan 2020.
Haas DA, Brady M, Helmers RA, Rucci M, Kaplan RS. The Mayo Clinic Model for Running a Value-Improvement Program. Available at: https://hbr.org/2015/10/the-mayo-clinic-model-for-running-a-value-improvement-program. Accessed 21 Jan 2020.
Irene Papanicolas, Liana R. Woskie and AJ. Health Care Spending in US, Other High-Income Countries. Commonwealth Fund 2018. Available at: https://www.commonwealthfund.org/publications/journal-article/2018/mar/health-care-spending-united-states-and-other-high-income. Accessed 16 Jan 2020.
Kaplan RS, Porter ME. How to solve the cost crisis in health care. Harvard Business Review. 2011;89(9).
Kaplan RS, Witkowski M, Abbott M, et al. Using time-driven activity-based costing to identify value improvement opportunities in healthcare. J Healthc Manag. 2014;59(6):399–412. https://doi.org/10.1097/00115514-201411000-00006.
Keel G, Savage C, Rafiq M, Mazzocato P. Time-driven activity-based costing in health care: A systematic review of the literature. Health Policy (New York). 2017;121(7):755–63. https://doi.org/10.1016/j.healthpol.2017.04.013.
Klassen AF, Pusic AL, Scott A, Klok J, Cano SJ. Satisfaction and quality of life in women who undergo breast surgery: a qualitative study. BMC Womens Health. 2009;9:11. https://doi.org/10.1186/1472-6874-9-11.
Lagendijk M, Mittendorf E, King TA, Gibbons C, Pusic A, Dominici LS. Incorporating patient-reported outcome measures into breast surgical oncology: advancing toward value-based care. Oncologist. 2020;25(5):384–90. https://doi.org/10.1634/theoncologist.2019-0355.
Laviana AA, Ilg AM, Veruttipong D, et al. Utilizing time-driven activity-based costing to understand the short- and long-term costs of treating localized, low-risk prostate cancer. Cancer. 2016;122(3):447–55. https://doi.org/10.1002/cncr.29743.
Lievens Y, Obyn C, Mertens AS, Van Halewyck D, Hulstaert F. Stereotactic body radiotherapy for lung cancer: How much does it really cost? J Thorac Oncol. 2015;10(3):454–61. https://doi.org/10.1097/JTO.0000000000000421.
Najjar PA, Strickland M, Kaplan RS. Time-driven activity-based costing for surgical episodes. JAMA Surg. 2017;152(1):96–7. https://doi.org/10.1001/jamasurg.2016.3356.
Ong WL, Schouwenburg MG, van Bommel ACM, et al. A standard set of value-based patient-centered outcomes for breast cancer. JAMA Oncol. 2017;3(5):677. https://doi.org/10.1001/jamaoncol.2016.4851.
Porter ME. What is value in health care? N Engl J Med. 2010;363(26):2477–81. https://doi.org/10.1056/NEJMp1011024.
Porter ME, Teisberg EO. Redefining competition in health care. Harvard Bus Rev 2004;82(6).
Schutzer ME, Arthur DW, Anscher MS. Time-driven activity-based costing: a comparative cost analysis of whole-breast radiotherapy versus balloon-based brachytherapy in the management of early-stage breast cancer. J Oncol Pract. 2016;12(5):e584–93. https://doi.org/10.1200/jop.2015.008441.
Spinks T, Guzman A, Beadle BM, et al. Development and feasibility of bundled payments for the multidisciplinary treatment of head and neck cancer: a pilot program. J Oncol Pract. 2018;14(2):e103–12. https://doi.org/10.1200/jop.2017.027029.
Waks AG, Winer EP. Breast cancer treatment: a review. JAMA. 2019;321(3):288–300. https://doi.org/10.1001/jama.2018.19323.
Acknowledgments
The authors acknowledge Eileen Joyce, Cari Ryding, and Michelle Physic for assistance in preparing the process maps, and Kaitlyn Riffenburg and Ryan Leib for support in extracting data from the RTLS system.
Funding
Dr. Navraj S. Nagra was supported by the US-UK Fulbright Commission, and the study was supported by the Patient-Reported Outcomes, Value and Experience (PROVE) Center, Department of Surgery, Brigham and Women’s Hospital, Boston, MA, USA.
Author information
Authors and Affiliations
Contributions
NSN, TWF, and ALP conceived and designed the study; NSN, ET, and JM conducted the study methodology; and MJH, LSD, JRB, RSK, and ALP provided oversight to the methodology. All authors reviewed the manuscript and approved the final version for submission.
Corresponding author
Ethics declarations
DISCLOSURE
Robert Kaplan is a compensated advisor, with cash and stock options, for Avant-garde Health. Navraj S. Nagra, Elena Tsangaris, Jessica Means, Michael J. Hassett, Laura S. Dominici, Jennifer R. Bellon, Justin Broyles, Thomas W. Feeley, and Andrea L. Pusic have no conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: Figure 2 was updated.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Nagra, N.S., Tsangaris, E., Means, J. et al. Time-Driven Activity-Based Costing in Breast Cancer Care Delivery. Ann Surg Oncol 29, 510–521 (2022). https://doi.org/10.1245/s10434-021-10465-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-021-10465-5