Abstract
Background
Although the National Comprehensive Cancer Network (NCCN) guidelines recommend use of lymph node dissection (LND) in patients with pancreatic neuroendocrine tumors (pNETs) > 2 cm, there is limited evidence to support the association between use of LND and overall survival (OS).
Methods
Patients with resected pNETs were identified in the National Cancer Database (2004–2014). The inverse probability of treatment weighting (IPTW) method was used to reduce the selection bias. IPTW-adjusted Kaplan–Meier curves and Cox proportional hazards models were used to compare OS of patients in different treatment groups.
Results
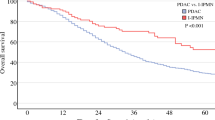
A total of 2664 patients diagnosed met the study entry criteria. Of these, 2132 patients (80.6%) received LND, with a median of nine nodes removed. Positive nodes were identified in 28.0% of patients who underwent LND. IPTW-adjusted Kaplan–Meier analysis showed that median OS was similar between the LND and LND-omitted groups (152.8 vs. 147.3 months; p = 0.61). In IPTW-adjusted Cox proportional hazards regression analysis, LND was not associated with an OS benefit (hazard ratio [HR] 1.15, 95% confidence interval [CI] 0.94–1.42; p = 0.18). The results were consistent across subgroups stratified by clinical T and N stages. Among patients with lymph node metastasis, the number of removed nodes (NRN) above the median was not associated with an improved OS (HR 0.82, 95% CI 0.60–1.13; p = 0.22).
Conclusions
LND had no additional therapeutic benefit among patients undergoing resection for pNETs. The present findings should be considered when managing patients with resectable pNETs.


Similar content being viewed by others
References
Milan SA, Yeo CJ. Neuroendocrine tumors of the pancreas. Curr Opin Oncol. 2012; 24:46–55.
Dasari A, Shen C, Halperin D, et al. Trends in the incidence, prevalence, and survival outcomes in patients with neuroendocrine tumors in the United States. JAMA Oncol. 2017;3(10):1335–42.
Hashim YM, Trinkaus KM, Linehan DC, et al. Regional lymph node dissection is indicated in the surgical treatment of pancreatic neuroendocrine tumors (PNETs). Ann Surg. 2014;259(2):197–203.
Tomassetti P, Campana D, Piscitelli L, et al. Endocrine pancreatic tumors: factors correlated with survival. Ann Oncol. 2005; 16:1806–10.
Bettini R, Boninsegna L, Mantovani W, et al. Prognostic factors at diagnosis and value of WHO classification in a mono-institutional series of 180 non-functioning pancreatic endocrine tumours. Ann Oncol. 2008; 19:903–8.
Krampitz GW, Norton JA, Poultsides GA, et al. Lymph Nodes and Survival in Pancreatic Neuroendocrine Tumors (pNET). Arch Surg. 2012;147(9):820-7.
Bilimoria KY, Talamonti MS, Tomlinson JS, et al. Prognostic score predicting survival after resection of pancreatic neuroendocrine tumors: analysis of 3851 patients. Ann Surg. 2008; 247:490–500.
Kazanjian KK, Reber HA, Hines OJ. Resection of pancreatic neuroendocrine tumors: results of 70 cases. Arch Surg. 2006; 141:765–69.
Ellison TA, Wolfgang CL, Shi C, et al. A single institution’s 26-year experience with nonfunctional pancreatic neuroendocrine tumors: a validation of current staging systems and a new prognostic nomogram. Ann Surg. 2014;259(2):204–12.
Rindi G, Klöppel G, Alhman H, et al. TNM staging of foregut (neuro)endocrine tumors: a consensus proposal including a grading system. 2007;451(4):757–62.
National Comprehensive Cancer Network (NCCN). NCCN Clinical Practice Guidelines in Oncology. Neuroendocrine Tumors. Version 3.2018.
Kunz PL, Reidy-Lagunes D, Anthony LB, et al. Consensus guidelines for the management and treatment of neuroendocrine tumors. Pancreas. 2013; 42(4):557–77.
MacFarlane JK, Ryall RD, Heald RJ. Mesorectal excision for rectal cancer. Lancet. 1993;341(8843):457–60.
Songun I, Putter H, Kranenbarg EM, et al. Surgical treatment of gastric cancer: 15-year follow-up results of the randomised nationwide Dutch D1D2 trial. Lancet Oncol. 2010;11:439–49.
Gratian L, Pura J, Dinan M, et al. Impact of extent of surgery on survival in patients with small nonfunctional pancreatic neuroendocrine tumors in the United States. Ann Surg Oncol. 2014;21(11):3515–21.
Kuo EJ, Salem RR. Population-level analysis of pancreatic neuroendocrine tumors 2 cm or less in size. Ann Surg Oncol. 2013;9:2815–2821.
Tsutsumi K, Ohtsuka T, Mori Y, et al. Analysis of lymph node metastasis in pancreatic neuroendocrine tumors (PNETs) based on the tumor size and hormonal production. J Gastroenterol. 2012;47(6):678–85.
Rindi G, Falconi M, Klersy C, et al. TNM staging of neoplasms of the endocrine pancreas: results from a large international cohort study. J Natl Cancer Inst. 2012;104(10):764–77.
Chu QD, Hill HC, Douglass HO Jr, et al. Predictive factors associated with long-term survival in patients with neuroendocrine tumors of the pancreas. Ann Surg Oncol. 2002;9(9):855–62.
Ferrone CR, Tang LH, Tomlinson J, et al. Determining prognosis in patients with pancreatic endocrine neoplasms: can the WHO classification system be simplified? J Clin Oncol. 2007; 25(35):5609–15.
Ito H, Abramson M, Ito K, et al. Surgery and staging of pancreatic neuroendocrine tumors: a 14-year experience. J Gastrointest Surg. 2010;14(5):891–8.
Parekh JR, Wang SC, Bergsland EK, et al. Lymph node sampling rates and predictors of nodal metastasis in pancreatic neuroendocrine tumor resections: the UCSF experience with 149 patients. Pancreas. 2012;41(6):840–4.
Sallinen VJ, Le Large TTY, Tieftrunk E, et al. Prognosis of sporadic resected small (≤ 2 cm) nonfunctional pancreatic neuroendocrine tumors: a multi-institutional study. HPB (Oxford). 2018;20(3):251–59.
Luo G, Javed A, Strosberg JR, et al. Modified staging classification for pancreatic neuroendocrine tumors on the basis of the American Joint Committee on Cancer and European Neuroendocrine Tumor Society Systems. J Clin Oncol. 2017;35(3):274–80.
Mise Y, Vauthey JN, Zimmitti G, et al. Ninety-day postoperative mortality is a legitimate measure of hepatopancreatobiliary surgical quality. Ann Surg. 2015;262(6):1071–8.
Amin M, Edge S, Greene F, et al. AJCC cancer staging manual, 8th ed. New York, NY: Springer; 2017.
Rubin DB. Multiple imputation for nonresponse in surveys. New York, NY: Wiley; 2004.
Edge SB, Byrd DR, Compton CC, et al. AJCC cancer staging manual (7th ed). New York, NY: Springer; 2010.
Mizumoto T, Toyama H, Terai S, et al. Prediction of lymph node metastasis in pancreatic neuroendocrine tumors by contrast enhancement characteristics. Pancreatology. 2017;17(6): 956–61.
Choi SH, Kim HJ, Kim SY, et al. Computed tomography features predictive of lymph node involvement in patients with a nonfunctioning pancreatic neuroendocrine tumor. Pancreas. 2017; 46(8):1056–63.
Sadowski SM, Neychev V, Millo C, et al. Prospective study of 68 Ga-DOTATATE positron emission tomography/computed tomography for detecting gastro-entero-pancreatic neuroendocrine tumors and unknown primary sites. J Clin Oncol. 2016;34(6):588–96.
Angelousi A, Kaltsas G, Koumarianou A, et al. Chemotherapy in NETs: when and how. Rev Endocr Metab Disord. 2017;18(4):485–97.
Acknowledgment
This work was supported by the National Natural Science Foundation of China (81672461); Chinese Academy of Medical Sciences Innovation Fund for Medical Sciences (CIFMS; Grant No. 2017-12M-4-002); and the Capital Health Research and Development of Special (2018-1-4021). Sheng Luo’s research was partly supported by Grant R01NS091307 from the National Institute of Neurological Disorders and Stroke (NINDS) and Grant R56AG062302 from the National Institute on Aging (NIA).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Rui Mao, Hong Zhao, Kan Li, Sheng Luo, Megan Turner, Jian-Qiang Cai, and Dan Blazer III report no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Mao, R., Zhao, H., Li, K. et al. Outcomes of Lymph Node Dissection for Non-metastatic Pancreatic Neuroendocrine Tumors: A Propensity Score-Weighted Analysis of the National Cancer Database. Ann Surg Oncol 26, 2722–2729 (2019). https://doi.org/10.1245/s10434-019-07506-5
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-019-07506-5