Abstract
Background
Current treatment guidelines for male breast cancer are predominantly guided by female-only clinical trials. With scarce research, it is unclear whether breast-conserving therapy (BCT) is equivalent to mastectomy in men. We sought to compare overall survival (OS) among male breast cancer patients who underwent BCT versus mastectomy.
Methods
We performed a retrospective analysis of 8445 stage I–II (T1–2 N0–1 M0) male breast cancer patients from the National Cancer Database (2004–2014). Patients were grouped according to surgical and radiation therapy (RT). BCT was defined as partial mastectomy followed by RT. Multivariable and inverse probability of treatment-weighted (IPTW) Cox proportional hazards models were used to compare OS between treatment groups, controlling for demographic and clinicopathologic characteristics.
Results
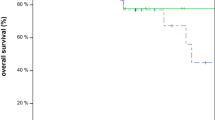
Most patients underwent total mastectomy (61.2%), whereas 18.2% underwent BCT, 12.4% underwent total mastectomy with RT, and 8.2% underwent partial mastectomy alone. In multivariable and IPTW models, partial mastectomy alone, total mastectomy alone, and total mastectomy with RT were associated with worse OS compared with BCT (p < 0.001 all). Ten-year OS was 73.8% for BCT and 56.3, 58.0 and 56.3% for other treatment approaches. Older age, higher T/N stage, histological grade, and triple-negative receptor status were associated with poorer OS (p < 0.05). Subgroup analysis by stage demonstrated similar results.
Conclusions
In this national sample of male breast cancer patients, BCT was associated with greater survival. The underlying mechanisms of this association warrant further study, because more routine adoption of BCT in male breast cancer appears to translate into clinically meaningful improvements in survival.



Similar content being viewed by others
References
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2017. CA Cancer J Clin. 2017;67(1):7–30.
Gradishar WJ, Anderson BO, Balassanian R, et al. National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology: Breast Cancer. Version 2.2017. https://www.nccn.org/professionals/physician_gls/pdf/breast.pdf.
Fisher B, Anderson S, Bryant J, et al. Twenty-year follow-up of a randomized trial comparing total mastectomy, lumpectomy, and lumpectomy plus irradiation for the treatment of invasive breast cancer. N Engl J Med. 2002;347(16):1233–41.
Aggarwal A, Liu ML, Krasnow SH. Breast cancer in male veteran population: an analysis from VA cancer registry. J Community Support Oncol. 2014;12(8):293–7.
O’Malley CD, Prehn AW, Shema SJ, Glaser SL. Racial/ethnic differences in survival rates in a population-based series of men with breast carcinoma. Cancer. 2002;94(11):2836–43.
Giordano SH, Cohen DS, Buzdar AU, Perkins G, Hortobagyi GN. Breast carcinoma in men: a population-based study. Cancer. 2004;101(1):51–7.
Stierer M, Rosen H, Weitensfelder W, et al. Male breast cancer: Austrian experience. World J Surg. 1995;19(5):687–92; discussion 692–3.
Schaub NP, Maloney N, Schneider H, Feliberti E, Perry R. Changes in male breast cancer over a 30-year period. Am Surg. 2008;74(8):707–11; discussion 711–2.
Ribeiro GG, Swindell R, Harris M, Banarjee SS, Cramer A. A review of the management of the male breast carcinoma based on an analysis of 420 treated cases. Breast. 1996;5:141–6.
Golshan M, Rusby J, Dominguez F, Smith BL. Breast conservation for male breast carcinoma. Breast. 2007;16(6):653–6.
Cloyd JM, Hernandez-Boussard T, Wapnir IL. Poor compliance with breast cancer treatment guidelines in men undergoing breast-conserving surgery. Breast Cancer Res Treat. 2013;139(1):177–82.
Cardoso F, Bartlett JMS, Slaets L, et al. Characterization of male breast cancer: results of the EORTC 10085/TBCRC/BIG/NABCG International Male Breast Cancer Program. Ann Oncol. 2018;29(2):405–17.
Cloyd JM, Hernandez-Boussard T, Wapnir IL. Outcomes of partial mastectomy in male breast cancer patients: analysis of SEER, 1983–2009. Ann Surg Oncol. 2013;20(5):1545–50.
Jagsi R, Abrahamse P, Hawley ST, Graff JJ, Hamilton AS, Katz SJ. Underascertainment of radiotherapy receipt in Surveillance, Epidemiology, and End Results registry data. Cancer. 2012;118(2):333–41.
Korde LA, Zujewski JA, Kamin L, et al. Multidisciplinary meeting on male breast cancer: summary and research recommendations. J Clin Oncol. 2010;28(12):2114–22.
Fentiman IS, Fourquet A, Hortobagyi GN. Male breast cancer. Lancet. 2006;367(9510):595–604.
Greif JM, Pezzi CM, Klimberg VS, Bailey L, Zuraek M. Gender differences in breast cancer: analysis of 13,000 breast cancers in men from the National Cancer Data Base. Ann Surg Oncol. Oct 2012;19(10):3199–204.
Massarweh SA, Sledge GW, Miller DP, McCullough D, Petkov VI, Shak S. Molecular characterization and mortality from breast cancer in men. J Clin Oncol. 2018;36(14):1396–404.
Boffa DJ, Rosen JE, Mallin K, et al. Using the National Cancer Database for outcomes research: a review. JAMA Oncol. 2017;3(12):1722–8.
Bilimoria KY, Bentrem DJ, Stewart AK, Winchester DP, Ko CY. Comparison of commission on cancer-approved and -nonapproved hospitals in the United States: implications for studies that use the National Cancer Data Base. J Clin Oncol. 2009;27(25):4177–81.
Schmocker RK, Caretta-Weyer H, Weiss JM, et al. Determining breast cancer axillary surgery within the surveillance epidemiology and end results-Medicare database. J Surg Oncol. 2014;109(8):756–9.
Lorimer PD, White RL, Walsh K, et al. Pediatric and adolescent melanoma: a National Cancer Data Base update. Ann Surg Oncol. Nov 2016;23(12):4058–66.
Yi M, Meric-Bernstam F, Ross MI, et al. How many sentinel lymph nodes are enough during sentinel lymph node dissection for breast cancer? Cancer. 2008;113(1):30–7.
Garrido MM, Kelley AS, Paris J, et al. Methods for constructing and assessing propensity scores. Health Serv Res. 2014;49(5):1701–20.
Austin PC. An introduction to propensity score methods for reducing the effects of confounding in observational studies. Multivar Behav Res. 2011;46(3):399–424.
Fisher B, Jeong JH, Anderson S, Bryant J, Fisher ER, Wolmark N. Twenty-five-year follow-up of a randomized trial comparing radical mastectomy, total mastectomy, and total mastectomy followed by irradiation. N Engl J Med. 2002;347(8):567–75.
Early Breast Cancer Trialists’ Collaborative Group (EBCTCG), McGale P, Taylor C, et al. Effect of radiotherapy after mastectomy and axillary surgery on 10-year recurrence and 20-year breast cancer mortality: meta-analysis of individual patient data for 8135 women in 22 randomised trials. Lancet. 2014;383(9935):2127–35.
Early Breast Cancer Trialists’ Collaborative G, Darby S, McGale P, et al. Effect of radiotherapy after breast-conserving surgery on 10-year recurrence and 15-year breast cancer death: meta-analysis of individual patient data for 10,801 women in 17 randomised trials. Lancet. 2011;378(9804):1707–16.
Yu E, Suzuki H, Younus J, et al. The impact of post-mastectomy radiation therapy on male breast cancer patients: a case series. Int J Radiat Oncol Biol Phys. 2012;82(2):696–700.
Jardel P, Vignot S, Cutuli B, et al. Should adjuvant radiation therapy be systematically proposed for male breast cancer? A systematic review. Anticancer Res. 2018;38(1):23–31.
Madden NA, Macdonald OK, Call JA, Schomas DA, Lee CM, Patel S. Radiotherapy and male breast cancer: a population-based registry analysis. Am J Clin Oncol. 2016;39(5):458–62.
Abrams MJ, Koffer PP, Wazer DE, Hepel JT. Postmastectomy radiation therapy is associated with improved survival in node-positive male breast cancer: a population analysis. Int J Radiat Oncol Biol Phys. 2017;98(2):384–91.
Jatoi I, Benson JR, Kunkler I. Hypothesis: can the abscopal effect explain the impact of adjuvant radiotherapy on breast cancer mortality? NPJ Breast Cancer. 2018;4:8.
Bagaria SP, Wasif N, Rawal B, McLaughlin SA, Giuliano AE. Is mastectomy undertreatment for low-risk breast cancers eligible for breast-conserving therapy? Cancer. 2015;121(16):2705–12.
Agarwal S, Pappas L, Neumayer L, Kokeny K, Agarwal J. Effect of breast conservation therapy vs mastectomy on disease-specific survival for early-stage breast cancer. JAMA Surg. 2014;149(3):267–74.
Christiansen P, Carstensen SL, Ejlertsen B, et al. Breast conserving surgery versus mastectomy: overall and relative survival-a population based study by the Danish Breast Cancer Cooperative Group (DBCG). Acta Oncol. 2018;57(1):19–25.
Maishman T, Cutress RI, Hernandez A, et al. Local recurrence and breast oncological surgery in young women with breast cancer: the POSH Observational Cohort Study. Ann Surg. 2017;266(1):165–72.
Ferzoco RM, Ruddy KJ. Optimal delivery of male breast cancer follow-up care: improving outcomes. Breast Cancer (Dove Med Press). 2015;7:371–9.
Funding
The National Center for Advancing Translational Sciences, NIH (UL1TR001860) and the Agency for Healthcare Research and Quality (T32HS022236).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
DISCLOSURE
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Bateni, S.B., Davidson, A.J., Arora, M. et al. Is Breast-Conserving Therapy Appropriate for Male Breast Cancer Patients? A National Cancer Database Analysis. Ann Surg Oncol 26, 2144–2153 (2019). https://doi.org/10.1245/s10434-019-07159-4
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-019-07159-4