Abstract
Background
The American Joint Committee on Cancer includes extranodal tumor deposits in the tumor–node–metastasis classification of colon cancer. However, it is unclear how tumor deposits compare with lymph node metastases in prognostic significance. This study evaluated the survival impact of tumor deposits relative to lymph node metastases in stage III colon cancer.
Methods
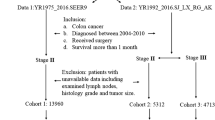
The US National Cancer Database (2010–2012) was reviewed for resectable stage III adenocarcinoma of the colon, and stratified by presence of tumor deposits and lymph node metastases. Univariate and multivariate survival analyses were performed.
Results
Of 6424, 10.1% had both tumor deposits and lymph node metastases [5-year survival (5YS) 40.2%], 2.5% had tumor deposits alone (5YS 68.1%), and 87.4% had lymph node metastases alone (5YS 55.4%). Patients with lymph node metastases alone tended to have a greater number of lymph nodes retrieved (20.9 versus 18.8, p = 0.0126) and were more likely to receive adjuvant therapy (66.9 vs 58.0%, p = 0.003) than those with only tumor deposits. Patients with both had significantly worse survival at all T stages (p < 0.05, all). There was no significant difference in survival between tumor deposits alone and lymph node metastases alone at any T stage (p > 0.8, all). After controlling for patient, disease, and treatment characteristics, patients with tumor deposits alone [hazard ratio (HR) 0.56, p = 0.001] or only lymph node metastases (HR 0.64, p < 0.001) were associated with improved survival relative to patients with both.
Conclusions
Concomitant presence of tumor deposits and lymph node invasion carries poor prognostic significance. Tumor deposits alone appear to have prognostic implications similar to lymph node invasion alone.


Similar content being viewed by others
References
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2017. CA: Cancer J Clin. 2017;67(1):7–30.
Cancer AJCo. Cancer staging system 2017. https://cancerstaging.org/references-tools/Pages/What-is-Cancer-Staging.aspx. Accessed 6 June 2017.
Network NCC. Colon cancer. Clinical Practice Guielines in Oncology (NCCN Guidelines). 2015; version 2.2016.
Goldstein NS, Turner JR. Pericolonic tumor deposits in patients with T3 N + MO colon adenocarcinomas: markers of reduced disease free survival and intra-abdominal metastases and their implications for TNM classification. Cancer. 2000;88(10):2228–2238.
Lo DS, Pollett A, Siu LL, Gallinger S, Burkes RL. Prognostic significance of mesenteric tumor nodules in patients with stage III colorectal cancer. Cancer. 2008;112(1):50–54.
Puppa G, Maisonneuve P, Sonzogni A, et al. Pathological assessment of pericolonic tumor deposits in advanced colonic carcinoma: relevance to prognosis and tumor staging. Mod Pathol. 2007;20(8):843–855.
Belt EJ, van Stijn MF, Bril H, et al. Lymph node negative colorectal cancers with isolated tumor deposits should be classified and treated as stage III. Ann Surg Oncol. 2010;17(12):3203–3211.
Cuccurullo V, Mansi L. AJCC Cancer Staging Handbook: from the AJCC Cancer Staging Manual (7th edition). Eur J Nucl Med Mol Imaging. 2011;38(2):408-408.
Ueno H, Mochizuki H, Shirouzu K, et al. Actual status of distribution and prognostic impact of extramural discontinuous cancer spread in colorectal cancer. J Clin Oncol. 2011;29(18):2550–2556.
Song YX, Gao P, Wang ZN, et al. Can the tumor deposits be counted as metastatic lymph nodes in the UICC TNM staging system for colorectal cancer? PloS ONE. 2012;7(3):e34087.
Al Sahaf O, Myers E, Jawad M, Browne TJ, Winter DC, Redmond HP. The prognostic significance of extramural deposits and extracapsular lymph node invasion in colon cancer. Dis Colon Rectum. 2011;54(8):982–988.
Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40(5):373–383.
Deyo RA, Cherkin DC, Ciol MA. Adapting a clinical comorbidity index for use with ICD-9-CM administrative databases. J Clin Epidemiol. 1992;45(6):613–619.
Nagtegaal ID, Knijn N, Hugen N, et al. Tumor deposits in colorectal cancer: improving the value of modern staging-a systematic review and meta-analysis. J Clin Oncol. 2017;35(10):1119–1127.
Nagayoshi K, Ueki T, Nishioka Y, et al. Tumor deposit is a poor prognostic indicator for patients who have stage II and III colorectal cancer with fewer than 4 lymph node metastases but not for those with 4 or more. Dis Colon Rectum. 2014;57(4):467–474.
Jin M, Roth R, Rock JB, Washington MK, Lehman A, Frankel WL. The impact of tumor deposits on colonic adenocarcinoma AJCC TNM staging and outcome. Am J Surg Pathol. 2015;39(1):109–115.
Li J, Yang S, Hu J, et al. Tumor deposits counted as positive lymph nodes in TNM staging for advanced colorectal cancer: a retrospective multicenter study. Oncotarget. 2016;7(14):18269–18279.
J. Milburn Jessup RMG, Asare EA, Benson AB III, Brierley JD, George J, Chang VC, Compton CC, De Nardi P, Goodman KA, Donna Gress, Justin, Guinney LLG, Hamilton SR, Hanna NN, Kakar S, Kosinski LA, Serban Negoita SO, Overman MJ, Quirke P, Rohren E, Sargent DJ, Lynne T, Schumacher-Penberthy DS, Sinicrope FA, Steele SR, Stojadinovic A, Sabine Tejpar MRW, Welton ML, Washington MK. Colon and rectum. AJCC Cancer Staging Manual, 8th Edn. Chicago: American Joint Committee on Cancer; 2017.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Disclaimer
The National Cancer Data Base (NCDB) is a joint project of the Commission on Cancer (CoC) of the American College of Surgeons and the American Cancer Society. The CoC’s NCDB and the hospitals participating in the CoC NCDB are the source of the de-identified data used herein; they have not verified and are not responsible for the statistical validity of the data analysis or the conclusions derived by the authors.
Rights and permissions
About this article
Cite this article
Mirkin, K.A., Kulaylat, A.S., Hollenbeak, C.S. et al. Prognostic Significance of Tumor Deposits in Stage III Colon Cancer. Ann Surg Oncol 25, 3179–3184 (2018). https://doi.org/10.1245/s10434-018-6661-9
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-018-6661-9