Abstract
Purpose
Sexual dysfunction is assumed to be common, but understudied, in breast cancer patients. Herein, we use the validated female sexual functioning index (FSFI) to evaluate changes in female sexual function after breast cancer surgery.
Methods
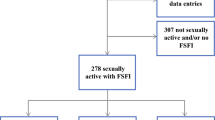
The FSFI assesses sexual function in six domains (desire, arousal, lubrication, orgasm, satisfaction, pain) on a 36-point scale, with scores >26.6 indicating better sexual function. We identified 226 women with unilateral breast cancer undergoing surgery at our institution from June 2010–January 2015. All completed the FSFI preoperatively and at a median of 13 months postoperatively. We quantified declines in FSFI scores and considered p-values <0.05 statistically significant.
Results
Overall, 119 women had breast-conserving surgery (BCS), 40 had unilateral mastectomy (UM), and 67 had UM plus contralateral prophylactic mastectomy (CPM). All women had similar baseline FSFI scores (medians: BCS, 26.3; UM, 25.2; UM+CPM, 23.7; p = 0.23). At follow-up, sexual function had declined significantly in BCS (23.5; p < 0.001) and UM (17.4; p = 0.010), but was unchanged in UM+CPM (22.8; p = 0.74) women. Interestingly, all women maintained their desire for sex (p = 0.17). BCS and UM women demonstrated significant declines in all other subscale domains (all p < 0.045). UM+CPM women demonstrated no decline in any subscale domain, yet did not exhibit superior sexual function to those having UM or BCS (medians: BCS, 23.5; UM, 17.4; UM+CPM, 22.8; p = 0.21).
Conclusions
Baseline sexual dysfunction exists in women diagnosed with breast cancer. Surgery negatively impacts sexual function. Patients who choose mastectomy do not exhibit superior sexual function over those having BCS at 13 months following surgery.
Similar content being viewed by others
References
Fallowfield L, Jenkins V. Psychosocial/survivorship issues in breast cancer: are we doing better? J Natl Cancer Inst. 2015; 107:335.
DeSantis CE, Lin CC, Mariotto AB, et al. Cancer treatment and survivorship statistics, 2014. CA Cancer J Clin. 2014; 64:252–71.
Dizon DS. Quality of life after breast cancer: survivorship and sexuality. Breast J. 2009; 15:500–4.
Thors CL, Broeckel JA, Jacobsen PB. Sexual functioning in breast cancer survivors. Cancer Control. 2001; 8:442–8.
Ussher JM, Perz J, Gilbert E, et al. Talking about sex after cancer: a discourse analytic study of health care professional accounts of sexual communication with patients. Psychol Health. 2013; 28:1370–90.
Dow J, Kennedy Sheldon L. Breast cancer survivors and sexuality: a review of the literature concerning sexual functioning, assessment tools, and evidence-based interventions. Clin J Oncol Nurs. 2015; 19:456–61.
Bredart A, Dolbeault S, Savignoni A, et al. Prevalence and associated factors of sexual problems after early-stage breast cancer treatment: results of a French exploratory survey. Psychooncology. 2011; 20:841–50.
Stead ML. Sexual dysfunction after treatment for gynaecologic and breast malignancies. Curr Opin Obstet Gynecol. 2003; 15:57–61.
Kiebert GM, de Haes JC, van de Velde CJ. The impact of breast-conserving treatment and mastectomy on the quality of life of early-stage breast cancer patients: a review. J Clin Oncol. 1991; 9:1059–70.
Ohsumi S, Shimozuma K, Kuroi K, Ono M, Imai H. Quality of life of breast cancer patients and types of surgery for breast cancer: current status and unresolved issues. Breast Cancer. 2007; 14:66–73.
Janz NK, Mujahid M, Lantz PM, et al. Population-based study of the relationship of treatment and sociodemographics on quality of life for early stage breast cancer. Qual Life Res. 2005; 14:1467–9.
Ganz PA, Schag AC, Lee JJ, Polinsky ML, Tan SJ. Breast conservation versus mastectomy. Is there a difference in psychological adjustment or quality of life in the year after surgery? Cancer. 1992; 69:1729–38.
Howlader NNA, Krapcho M, Garshell J, Miller D, Altekruse SF, Kosary CL, Yu M, et al. SEER cancer statistics review, 1975-2012, National Cancer Institute; 2015. http://seer.cancer.gov/csr/1975_2012/. Accessed 1 Dec 2015.
Panjari M, Bell RJ, Davis SR. Sexual function after breast cancer. J Sex Med. 2011; 8:294–302.
Bartula I, Sherman KA. The Female Sexual Functioning Index (FSFI): evaluation of acceptability, reliability, and validity in women with breast cancer. Support Care Cancer. 2015; 23:2633–41.
Rosen R, Brown C, Heiman J, et al. The Female Sexual Function Index (FSFI): a multidimensional self-report instrument for the assessment of female sexual function. J Sex Marital Ther. 2000; 26:191–208.
Meston CM. Validation of the Female Sexual Function Index (FSFI) in women with female orgasmic disorder and in women with hypoactive sexual desire disorder. J Sex Marital Ther. 2003; 29:39–46.
Wiegel M, Meston C, Rosen R. The female sexual function index (FSFI): cross-validation and development of clinical cutoff scores. J Sex Marital Ther. 2005; 31:1–20.
Revicki DA, Margolis MK, Bush EN, DeRogatis LR, Hanes V. Content validity of the Female Sexual Function Index (FSFI) in pre- and postmenopausal women with hypoactive sexual desire disorder. J Sex Med. 2011; 8:2237–45.
Flynn KE, Reese JB, Jeffery DD, et al. Patient experiences with communication about sex during and after treatment for cancer. Psychooncology. 2012; 21:594–601.
Hill EK, Sandbo S, Abramsohn E, et al. Assessing gynecologic and breast cancer survivors’ sexual health care needs. Cancer. 2011; 117:2643–51.
Kennedy V, Abramsohn E, Makelarski J, et al. Can you ask? We just did! Assessing sexual function and concerns in patients presenting for initial gynecologic oncology consultation. Gynecol Oncol. 2015; 137:119–24.
Mayer DK, Nekhlyudov L, Snyder CF, Merrill JK, Wollins DS, Shulman LN. American Society of Clinical Oncology clinical expert statement on cancer survivorship care planning. J Oncol Pract. 2014; 10:345–51.
Gradishar WJ, Anderson BO, Balassanian R, et al. Invasive breast cancer version 1.2016. NCCN clinical practice guidelines in oncology. J Natl Compr Canc Netw. 2016; 14:324–54.
Nash R, Goodman M, Lin CC, et al. State variation in the receipt of a contralateral prophylactic mastectomy among women who received a diagnosis of invasive unilateral early-stage breast cancer in the United States, 2004-2012. JAMA Surg. Epub 29 Mar 2017.
Hwang ES, Locklear TD, Rushing CN, et al. Patient-reported outcomes after choice for contralateral prophylactic mastectomy. J Clin Oncol. 2016; 34:1518–27.
Funding
No sources of funding were used to assist in the preparation of this study.
Disclosure
Lauren F. Cornell, Dawn M. Mussallem, Tammeza C. Gibson, Nancy N. Diehl, Sanjay P. Bagaria, and Sarah A. McLaughlin have no conflicts of interest to declare.
Author information
Authors and Affiliations
Corresponding author
Appendix
Appendix





Rights and permissions
About this article
Cite this article
Cornell, L.F., Mussallem, D.M., Gibson, T.C. et al. Trends in Sexual Function After Breast Cancer Surgery. Ann Surg Oncol 24, 2526–2538 (2017). https://doi.org/10.1245/s10434-017-5894-3
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-017-5894-3