Abstract
Synovial sarcoma is a translocation-associated soft-tissue malignancy that frequently affects adolescents and young adults. It is driven by one of the fusion oncoproteins SS18-SSX1, SS18-SSX2, or rarely, SS18-SSX4. Prognosis of patients with recurrent or metastatic disease is generally poor, and newer therapeutic strategies are needed. In this review, we present recent discoveries in the pathogenesis, diagnosis, and treatment of synovial sarcoma. We discuss potential therapeutic strategies to improve clinical outcomes in this disease.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Synovial sarcoma is a soft-tissue malignancy that can arise at any age and anatomic area but tends to favor the distal extremities in young adults.1–4 It can be confused with other mesenchymal tumors.5 Small (<5 cm) tumors have a good prognosis, whereas larger ones are at greater risk for metastases and local recurrences.6,7 Recent developments in basic and translational research have provided fresh insights into the pathogenesis and treatment of this disease.
Pathology and Biology
SS18-SSX Fusion Genes
The majority of synovial sarcomas carry the pathognomonic t(X;18) translocation, resulting in fusion of the SS18 (formerly SYT) gene on chromosome 18 with an SSX gene on chromosome X (SSX1, SSX2, or rarely SSX4) (Fig. 1).5,8 This genetic trigger is the only consistent cytogenetic abnormality in the disease, which thus far has been found to have a relatively stable genome and few additional mutations.10–12 Although SS18-SSX exhibits both transcriptional activating and repressing properties, it is not a transcription factor and does not bind DNA directly.13–16 SS18 tends to facilitate transcriptional activation, whereas SSX tends to affect transcriptional repression.17,18
SS18-SSX1 is the most frequent translocation followed next by SS18-SSX2 and finally SS18-SSX4.16 SS18-SSX1 and SS18-SSX2 behave somewhat differently. It has been suggested that SS18-SSX1 acts more as a “proliferation oncogene,” conferring proliferative, migratory, and invasive advantages to cells, whereas SS18-SSX2 functions more as a “position oncogene,” with effects on architectural, adhesive, and cytoskeletal properties, but this concept is perhaps best regarded as a preliminary one at present.19
Cellular Origin and Differentiation
Synovial sarcoma is a misnomer, because it does not arise from synovium, and the cells do not express synovial markers.7 Instead, it exhibits mesenchymal and epithelial differentiation.4 No cellular origin has yet been proven, but current research suggests that it develops from primitive mesenchymal cells or myoblasts.10,20–22 Naka et al. found that silencing of SS18-SSX activated mesenchymal lineage genes in synovial sarcoma cells.23 Garcia et al. found that expression of SS18-SSX2 in myoblasts inhibited further myogenic differentiation.24 Early-stage MYF5-positive myoblasts expressing SS18-SSX2 develop sarcomas with 100% penetrance in mice.22 This study also showed that SS18-SSX2 expression in more mature muscle cells caused only myopathies.22
Epigenetic Modifications
SS18-SSX alters chromatin remodeling via epigenetic alterations through SWI/SNF- and histone deacetylase (HDAC)-associated mechanisms, thereby activating or abrogating DNA interactions with transcription factors.12,25–28 It competes with wild-type SS18 for assembly within SWI/SNF complexes, ejecting SNF5, a tumor suppressor.29
Oncogenic Pathways
Several cellular pathways seem to be important in synovial sarcoma.12 The expression of genes pertaining to the Notch and Hedgehog pathways is notably altered in some tumors.30–33 Genetic anomalies in the Wnt network also have been described.34–39 TLE1, a mediator of the Wnt pathway, is upregulated in certain cases.1,12,40,41 TLE1 may also affect HDAC activity and mediate gene silencing in this disease.42,43
Some tumors exhibit PTEN and/or PIK3CA mutations, which can lead to upregulation of the Akt-mTOR pathway.12,36,44–48 Akt stimulation can also occur via the activity of receptor tyrosine kinases (RTKs), including EGFR, IGF-1R, VEGFR, and PDGFR.49–55 SS18-SSX stimulates IGF-2 expression in tumor cell lines and thereby activates IGF-1R, Akt, and SRC.55,56 SS18-SSX also can induce IGF-2 in fibroblast cells.57 VEGF serum levels are increased in some patients.58 Several studies have shown overexpression of FGF and FGFR in tumor cells.59,60 Garcia et al. showed that SS18-SSX upregulates FGFR2, which was critical for proliferation.24 Ephrin RTKs may promote metastasis in synovial sarcoma. SS18-SSX2-positive tumors activate this pathway through upregulation of EphB2 receptor and ephrin B1 ligand, leading to cytoskeletal modifications and loss of cellular adhesion.19
Diagnosis
The pathologic diagnosis of synovial sarcoma remains a challenge, because there is histological overlap with other tumor types. Ideally, recognition of the disease should be based upon a combination of findings, including traditional morphology, identification of the chromosomal t(X;18) translocation, and a panel of immunohistochemical markers.
Histological Classification
Three distinct subtypes are recognized: (1) monophasic, which contains predominantly spindle cells; (2) biphasic, which contains spindle and epithelial-like cells, with areas recapitulating gland formation; and (3) poorly differentiated, which can be characterized by necrosis, bizarre mitoses, high cellularity, and nuclear atypia, but perhaps more often is seen as a proliferation of small, round cells (Fig. 2).13,61 Separation into subtypes is based upon somewhat subjective criteria, and there is a certain degree of overlap.
Early studies suggested a relationship between tumor histology and fusion type.62 SS18-SSX1 tumors tended to be biphasic and had a higher proliferative Ki67 index, whereas SS18-SSX2 tumors were more likely to be monophasic with a lower Ki67 index.2,10,11,15,63–65 In an attempt to explain the presence of both epithelial and mesenchymal components, Saito et al. hypothesized that the cell of origin may have innate potential for undergoing epithelial differentiation, but loses the trait in certain cellular contexts and acquires mesenchymal features.62
Cytogenetic Diagnosis
Monophasic and poorly differentiated subtypes can sometimes be difficult to distinguish from other tumors. The translocation t(X;18) has been identified in synovial sarcoma only, and its sensitivity and specificity have been both established.5,8 In certain difficult cases, the detection of this fusion event (by RT-PCR or cytogenetic studies) has been instrumental to the correct diagnosis.1,42
Synovial sarcoma cannot be entirely excluded from the differential diagnosis if tumors have the morphological and clinical features of synovial sarcoma but do not bear an SS18-SSX fusion gene. In rare instances (estimated to be <5% of all cases), synovial sarcomas do not carry the characteristic SS18-SSX transcripts. These tumors may arise from alternative gene fusions (such as SS18L1/SSX1) or cryptic rearrangements.9,10,66 Apart from these exceptional cases, t(X;18) analysis remains an important tool for diagnosing synovial sarcoma.67
Immunohistochemical Markers
The diagnostic value of various markers has been limited by their lack of sensitivity and/or specificity. Immunomarkers with some utility include SMARCB1/INI1, cytokeratins, epithelial membrane antigen (EMA), carcinoembryonic antigen (CEA), vimentin, calponin, TLE1, Bcl2, CD34, CD99, and S100 protein (Fig. 2).1,42,68–75 Cytokeratins and EMA show a characteristic patchy pattern in the spindle cell component and a more uniform staining in the epithelial component. Strong, diffuse nuclear TLE1 reactivity may be a helpful finding in certain cases. Whereas Bcl2 and CD99 are usually reactive in synovial sarcoma, they are seen in many other tumors as well, thus limiting their specificity. Lai et al. found that NY-ESO-1, a cancer testis antigen, in synovial sarcoma, was highly expressed in 76% of tumors, which was greater than other spindle cell tumors.76 In contrast, however, Endo et al. showed that NY-ESO-1 is expressed in 49% of synovial sarcoma and that its distribution is not unique to this disease, because it is seen in myxoid liposarcomas, myxofibrosarcoma, and chondrosarcoma as well.77
Prognostic Factors
Many clinical factors have been studied to determine their potential prognostic value. Age has been reported to predict survival; young patients generally fare better than older ones.2,6,7,13,21,61,63,78–85 However, some authors found no effect of age.86–89 Most studies report no effect of gender on outcome with the exception of one study that found worse survival for males.13,81–83,87,88
Several tumor-related variables may be important. Tumor size has consistently predicted local recurrence and survival in many studies.2,6,13,63,84,90 Tumor location also seems to be significant with central locations having worse prognosis than extremities.13,82,86,90,91 Undifferentiated tumors, high histologic grade, high mitotic rate, and necrosis have been associated with worse outcome.2,6,7,13,84,90 Similarly, bone and neurovascular invasion are poor prognosticators.82,83,89 Local recurrence has been associated with greater risk of metastasis and shorter survival.13,79,81,87,90
Recent data suggest that fusion type does not have prognostic value, despite early studies suggesting that SS18-SSX1 produces more aggressive disease than SS18-SSX2.2,13,63,64,86 Similarly, biphasic histology is of questionable predictive value. In one study, monophasic tumors were to be indolent than biphasic tumors.82 However, in a different study, when FNCLCC grade was taken into account, biphasic histology was not an independent factor for outcome.13
Gene Expression Profiles
The various genes and pathways that exhibit perturbations in synovial sarcoma include Wnt (LEF1, TCF7, ZIC2, WNT5A, and FZD10), Hedgehog (PTCH1), NY-ESO-1 (CTAG1A), and Notch (JAG1, JAG2, and HES1), as well as RTKs (FGF2, FGF3, EGFR, PDGFR, and IGFBP3). Because these pathways are not consistently affected in all cases, efforts have been made to identify a genetic signature that predicts survival or tumor progression.6,12,14,54,60,92–95 The Complexity Index in Sarcoma (CINSARC) and the Genomic Index signatures are 67- and 97-gene panels, respectively, which have been found to have predictive value for metastasis in synovial sarcoma.95–97
Therapeutic Options
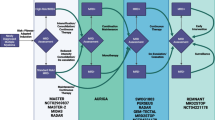
Therapeutic approaches vary according to stage and prognostic factors. The principles of surgical management are similar to those that apply to soft-tissue sarcomas in general. Patients with nonmetastatic, T1 (<5 cm), superficial tumors in favorable extremity sites may be treated with wide surgical excision alone. In one recent study of T1 tumors, it was found that microscopic disease was present in 43% of reexcised tumor beds, and reexcision of unplanned resections was strongly recommended.98 Larger tumors in deeper, more unfavorable locales may require radiation and surgery. For more advanced disease, multimodal treatment that entails surgery, radiotherapy, and systemic chemotherapy may be indicated.32,35 In this disease, however, the efficacy of current chemotherapy is less than optimal, and newer systemic therapies need to be developed (Fig. 3).
Novel therapeutic strategies in synovial sarcoma. Blunt arrows (⊥) indicate inhibition, sharp arrows (→) indicate stimulation, and straight lines (–) indicate interference. A Naïve T cells are cultured with NY-ESO-1 to expand T-cell populations and enhance their activity. Genetically engineered anti-NY-ESO-1 T cells elicit an immune response when reintroduced into the patient. B HDAC inhibitors downregulate HDAC, being responsible for the shift of DNA from transcriptionally active to inactive status. SS18-SSX interferes with SWI/SNF complex, leading to SNF5 ejection and degradation, mediating tumorigenesis. C Trabectedin inhibits synovial sarcoma by blocking transcription factors as well as depleting tumor macrophages. D Pazopanib represses many RTK pathways simultaneously or acts through a yet uncharacterized network in synovial sarcoma. E Dacarbazine alkylates DNA strands and inhibits cellular division. F Gemcitabine blocks DNA synthesis and docetaxel interferes with tubulin to repress mitosis. G By intercalation, doxorubicin inhibits DNA transcription and synthesis. Ifosfamide is an alkylating agent that blocks DNA transcription. H Injected SS18-SSX-loaded dendritic cells present SS18-SSX peptides to T cells to induce T-cell-mediated immunity
Doxorubicin (60–75 mg/m2) and ifosfamide (7.5–9 g/m2) comprise front-line therapy for synovial sarcoma.99–103 Together, the agents produce better outcomes in advanced disease than other chemotherapy regimens.7,82,103–107 Ferrari et al. reported 5-year, metastasis-free survival rates of 60 and 40% for patients treated with and without chemotherapy, respectively.82 Edmonson et al. showed partial tumor regression in 5 of 12 patients with residual, recurrent, or metastatic tumors, with a median overall survival of 11 months.103 Ifosfamide-based chemotherapy increased the 4-year, disease-specific survival rate from 67 to 88% in 101 patients with primary high-risk disease.106
High-dose ifosfamide (14 g/m2) alone has been used, but relatively few studies have been published to quantify its efficacy. Lee et al. reported that 2 of 7 patients experienced a complete response, and 4 of 11 patients had a partial response or disease stabilization.108 Median progression-free survival was 2.9 months, and median overall survival was 8.7 months.
An alternative treatment is the combination of gemcitabine and docetaxel, which may be considered in patients who cannot tolerate or are resistant to standard chemotherapy. Gemcitabine is an S-phase-specific nucleoside analog that blocks DNA synthesis. Docetaxel is a tubulin stabilizer and mitotic inhibitor. Early studies suggested that gemcitabine, despite its effectiveness in soft-tissue sarcomas, might not have much activity in synovial sarcoma.109,110 Similarly, in an early randomized study, patients receiving docetaxel exhibited no discernible responses.111 However a subsequent phase 2 trial showed objective but incomplete responses in 4 patients with synovial sarcoma treated with docetaxel.112 A recent, randomized, phase 2 trial compared gemcitabine plus docetaxel to gemcitabine alone in 122 patients with advanced soft-tissue sarcoma.113 For the combination treatment, the median progression-free and overall survivals were 6.2 and 17.9 months, respectively, whereas single agent gemcitabine resulted in 3 and 11.5 months survival, respectively. Two of the four synovial sarcoma patients treated with the combination of gemcitabine plus docetaxel exhibited stable disease. Similarly, two of four treated with gemcitabine alone had stable disease.
Multiple RTK networks are active in synovial sarcoma. Their co-inhibition may lead to synergistic antitumor effects.114,115 Clinical trials have been performed to analyze the benefit of RTK inhibitors (Table 1). Recent phase 2 and 3 studies suggest that pazopanib has activity in metastatic and refractory synovial sarcoma.116,117 In one phase 2 trial, the 3-month progression-free survival rate was 49% (18/37 patients), partial responses were noted in five patients, and the median overall survival duration was 310 days.116
Other trials have been designed to inhibit specific targets in synovial sarcoma. NCT00356031 is an ongoing phase 2 trial of a VEGFA antibody plus radiation on large (>5 cm) primary or recurrent synovial sarcoma. In a previous phase 2 study (NCT00831844), the IGF-1R antibody cixutumumab was found to have no benefit in 11 patients with recurrent refractory synovial sarcoma.118 An ongoing, phase 1 study (NCT00720174) examines the combination of cixutumumab and doxorubicin in advanced disease. It may be worth noting that in other soft-tissue sarcomas in which the IGF/IGF-1R axis is active, a shift from IGF-1R toward insulin receptor (IR) can occur. Hence, future efforts may need to target both IGF-1R and IR simultaneously.
Trabectedin is a promising agent, and partial regression of bilateral lung metastases was seen in one patient with advanced synovial sarcoma.119 In a recent retrospective study of 61 patients with advanced synovial sarcoma treated with trabectedin, 9 (15%) experienced partial responses and 19 (31%) had complete responses.120 The median progression-free survival was 3 months for the whole group and 7 months in the responding cohort. The mechanism of action is still being elucidated; it may affect transcription factors and tumor microenvironment through neoplastic macrophage depletion.121,122
HDAC- and SWI/SNF-mediated epigenetic modulation are potential therapeutic targets in synovial sarcoma. Radiotherapy induces DNA double strand breaks, stimulating DNA repair mechanisms, particularly those involving HDAC.123,124 In preclinical studies, HDAC inhibitors induced differentiation, apoptosis, and growth arrest of synovial sarcoma cells while increasing tumor cell sensitivity to radiation and chemotherapy.43,125,126 A phase 2 trial (NCT00112463) to study the efficacy of an HDAC inhibitor in synovial sarcoma has recently closed to accrual, and results of the trial are pending.
Wnt signaling inhibition via TCF/β-catenin complex inhibitors induces apoptosis and inhibits synovial sarcoma cell proliferation both in vitro and in vivo.34,127 A phase 1 clinical trial (NCT01469975) is being undertaken to evaluate the monoclonal antibody FZD10, which interrupts the Wnt pathway at the receptor-ligand level.
There have been some progress toward immunotherapeutic strategies. Particular mention should be made of NY-ESO-1, which is expressed in a substantial percentage of synovial sarcoma. Treatment of patients with NY-ESO-1-positive tumors with genetically engineered lymphocytes seems promising.76,128 Another immunotherapeutic approach involves SS18-SSX vaccine development, which may be employed with or without chemotherapeutic agents.6,90,129,130 Clinical studies exploring these therapeutic avenues are summarized in Table 2.
Conclusions
Synovial sarcoma is a malignant disease that frequently manifests in the extremities of young adults but can occur anywhere and in any age group. It has a tendency toward late recurrences and metastases, particularly in large tumors. Current multimodal treatment includes radiation, surgical resection, and chemotherapy. Multiple signaling networks and pathways have been identified in the disease. Understanding the molecular mechanisms of these phenomena may potentially lead to the development of newer and more effective therapies for patients with advanced and relapsed disease.
References
Jagdis A, Rubin BP, Tubbs RR, Pacheco M, Nielsen TO. Prospective evaluation of TLE1 as a diagnostic immunohistochemical marker in synovial sarcoma. Am J Surg Pathol. 2009;33(12):1743-51.
Ren T, Lu Q, Guo W, et al. The clinical implication of SS18-SSX fusion gene in synovial sarcoma. Br J Cancer. 2013;109(8):2279-85.
van de Rijn M, Barr FG, Xiong QB, Hedges M, Shipley J, Fisher C. Poorly differentiated synovial sarcoma: an analysis of clinical, pathologic, and molecular genetic features. Am J Surg Pathol. 1999;23(1):106-12.
Machen SK, Easley KA, Goldblum JR. Synovial sarcoma of the extremities: a clinicopathologic study of 34 cases, including semi-quantitative analysis of spindled, epithelial, and poorly differentiated areas. Am J Surg Pathol. 1999;23(3):268-75.
Guillou L, Coindre J, Gallagher G, et al. Detection of the synovial sarcoma translocation t(X;18) (SYT;SSX) in paraffin-embedded tissues using reverse transcriptase-polymerase chain reaction: a reliable and powerful diagnostic tool for pathologists. A molecular analysis of 221 mesenchymal tumors fixed in different fixatives. Hum Pathol. 2001;32(1):105-12.
Przybyl J, Sciot R, Wozniak A, et al. Metastatic potential is determined early in synovial sarcoma development and reflected by tumor molecular features. Int J Biochem Cell Biol. 2014;53:505-13.
Spurrell EL, Fisher C, Thomas JM, Judson IR. Prognostic factors in advanced synovial sarcoma: an analysis of 104 patients treated at the Royal Marsden Hospital. Ann Oncol. 2005;16(3):437-44.
Ladanyi M. Fusions of the SYT and SSX genes in synovial sarcoma. Oncogene. 2001;20(40):5755-62.
Storlazzi CT, Mertens F, Mandahl N, et al. A novel fusion gene, SS18L1/SSX1, in synovial sarcoma. Genes Chromosomes Cancer. 2003;37(2):195-200.
Sandberg AA, Bridge JA. Updates on the cytogenetics and molecular genetics of bone and soft-tissue tumors. Synovial sarcoma. Cancer Gen Cytogen. 2002;133(1):1-23.
Ladanyi M, Antonescu CR, Leung DH, et al. Impact of SYT-SSX fusion type on the clinical behavior of synovial sarcoma: a multi-institutional retrospective study of 243 patients. Cancer Res. 2002;62(1):135-40.
Nielsen TO, Poulin NM, Ladanyi M. Synovial sarcoma: recent discoveries as a roadmap to new avenues for therapy. Cancer Discovery. 2015;5(2):124-34.
Guillou L, Benhattar J, Bonichon F, et al. Histologic grade, but not SYT-SSX fusion type, is an important prognostic factor in patients with synovial sarcoma: a multicenter, retrospective analysis. J Clin Oncol. 2004;22(20):4040-50.
Fernebro J, Francis P, Eden P, et al. Gene expression profiles relate to SS18/SSX fusion type in synovial sarcoma. Int J Cancer. 2006;118(5):1165-72.
Nilsson G, Skytting B, Xie Y, et al. The SYT-SSX1 variant of synovial sarcoma is associated with a high rate of tumor cell proliferation and poor clinical outcome. Cancer Res. 1999;59(13):3180-4.
Dimitriadis E, Rontogianni D, Kyriazoglou A, et al. Novel SYT-SSX fusion transcript variants in synovial sarcoma. Cancer Gen Cytogen. 2009;195(1):54-8.
Brett D, Whitehouse S, Antonson P, Shipley J, Cooper C, Goodwin G. The SYT protein involved in the t(X;18) synovial sarcoma translocation is a transcriptional activator localised in nuclear bodies. Hum Mol Gen. 1997;6(9):1559-64.
Perani M, Antonson P, Hamoudi R, et al. The proto-oncoprotein SYT interacts with SYT-interacting protein/co-activator activator (SIP/CoAA), a human nuclear receptor co-activator with similarity to EWS and TLS/FUS family of proteins. J Biol Chem. 2005;280(52):42863-76.
Barco R, Hunt LB, Frump AL, et al. The synovial sarcoma SYT-SSX2 oncogene remodels the cytoskeleton through activation of the ephrin pathway. Mol Biol Cell. 2007;18(10):4003-12.
Saito T, Nagai M, Ladanyi M. SYT-SSX1 and SYT-SSX2 interfere with repression of E-cadherin by snail and slug: a potential mechanism for aberrant mesenchymal to epithelial transition in human synovial sarcoma. Cancer Res. 2006;66(14):6919-27.
Kerouanton A, Jimenez I, Cellier C, et al. Synovial sarcoma in children and adolescents. J Pediatric Hematol Oncol. 2014;36(4):257-62.
Haldar M, Hancock JD, Coffin CM, Lessnick SL, Capecchi MR. A conditional mouse model of synovial sarcoma: insights into a myogenic origin. Cancer Cell. 2007;11(4):375-88.
Naka N, Takenaka S, Araki N, et al. Synovial sarcoma is a stem cell malignancy. Stem Cells. 2010;28(7):1119-31.
Garcia CB, Shaffer CM, Alfaro MP, et al. Reprogramming of mesenchymal stem cells by the synovial sarcoma-associated oncogene SYT-SSX2. Oncogene. 2012;31(18):2323-34.
Middeljans E, Wan X, Jansen PW, Sharma V, Stunnenberg HG, Logie C. SS18 together with animal-specific factors defines human BAF-type SWI/SNF complexes. PloS One. 2012;7(3):e33834.
Soulez M, Saurin AJ, Freemont PS, Knight JC. SSX and the synovial-sarcoma-specific chimaeric protein SYT-SSX co-localize with the human Polycomb group complex. Oncogene. 1999;18(17):2739-46.
van der Vlag J, Otte AP. Transcriptional repression mediated by the human polycomb-group protein EED involves histone deacetylation. Nature Gen. 1999;23(4):474-8.
Furuyama T, Banerjee R, Breen TR, Harte PJ. SIR2 is required for polycomb silencing and is associated with an E(Z) histone methyltransferase complex. Current Biol. 2004;14(20):1812-21.
Kadoch C, Crabtree GR. Reversible disruption of mSWI/SNF (BAF) complexes by the SS18-SSX oncogenic fusion in synovial sarcoma. Cell. 2013;153(1):71-85.
Artavanis-Tsakonas S, Rand MD, Lake RJ. Notch signaling: cell fate control and signal integration in development. Science. 1999;284(5415):770-6.
Greenwald I. LIN-12/Notch signaling: lessons from worms and flies. Genes Develop. 1998;12(12):1751-62.
Radaelli S, Stacchiotti S, Casali PG, Gronchi A. Emerging therapies for adult soft-tissue sarcoma. Expert Rev Anticancer Ther. 2014;14(6):689-704.
Ingham PW. Hedgehog signaling: a tale of two lipids. Science. 2001;294(5548):1879-81.
Trautmann M, Sievers E, Aretz S, et al. SS18-SSX fusion protein-induced Wnt/beta-catenin signaling is a therapeutic target in synovial sarcoma. Oncogene. Oct 16 2014;33(42):5006-16.
Linch M, Miah AB, Thway K, Judson IR, Benson C. Systemic treatment of soft-tissue sarcoma-gold standard and novel therapies. Nat Rev Clin Oncol. 2014;11(4):187-202.
Saito T, Oda Y, Kawaguchi K, et al. PTEN and other tumor suppressor gene mutations as secondary genetic alterations in synovial sarcoma. Oncology Rep. 2004;11(5):1011-5.
Subramaniam MM, Calabuig-Farinas S, Pellin A, Llombart-Bosch A. Mutational analysis of E-cadherin, beta-catenin and APC genes in synovial sarcomas. Histopathology. 2010;57(3):482-6.
Saito T, Oda Y, Sakamoto A, et al. APC mutations in synovial sarcoma. J Pathol. 2002;196(4):445-9.
Kelleher F, O’Donnell CP, Rafee S. WNT Signaling and synovial sarcoma. Sarcoma Res Int. 2014;1(1):5.
Baird K, Davis S, Antonescu CR, et al. Gene expression profiling of human sarcomas: insights into sarcoma biology. Cancer Res. 2005;65(20):9226-35.
Nakayama R, Mitani S, Nakagawa T, et al. Gene expression profiling of synovial sarcoma: distinct signature of poorly differentiated type. Am J Surg Pathol. 2010;34(11):1599-607.
Chuang HC, Hsu SC, Huang CG, Hsueh S, Ng KF, Chen TC. Reappraisal of TLE-1 immunohistochemical staining and molecular detection of SS18-SSX fusion transcripts for synovial sarcoma. Pathol Int. 2013;63(12):573-80.
Su L, Sampaio AV, Jones KB, et al. Deconstruction of the SS18-SSX fusion oncoprotein complex: insights into disease etiology and therapeutics. Cancer Cell. 2012;21(3):333-47.
Jiang BH, Liu LZ. Role of mTOR in anticancer drug resistance: perspectives for improved drug treatment. Drug resistance updates: reviews and commentaries in antimicrobial and anticancer chemotherapy. 2008;11(3):63-76.
Wan X, Helman LJ. The biology behind mTOR inhibition in sarcoma. Oncologist. 2007;12(8):1007-18.
Barretina J, Taylor BS, Banerji S, et al. Subtype-specific genomic alterations define new targets for soft-tissue sarcoma therapy. Nat Gen. 2010;42(8):715-21.
Teng HW, Wang HW, Chen WM, et al. Prevalence and prognostic influence of genomic changes of EGFR pathway markers in synovial sarcoma. J Surg Oncol. 2011;103(8):773-81.
Chang Q, Li Y, White MF, Fletcher JA, Xiao S. Constitutive activation of insulin receptor substrate 1 is a frequent event in human tumors: therapeutic implications. Cancer Res. 2002;62(21):6035-8.
Friedrichs N, Trautmann M, Endl E, et al. Phosphatidylinositol-3’-kinase/AKT signaling is essential in synovial sarcoma. Int J Cancer. 2011;129(7):1564-75.
Bozzi F, Ferrari A, Negri T, et al. Molecular characterization of synovial sarcoma in children and adolescents: evidence of akt activation. Trans Oncol. 2008;1(2):95-101.
Setsu N, Kohashi K, Fushimi F, et al. Prognostic impact of the activation status of the Akt/mTOR pathway in synovial sarcoma. Cancer. 2013;119(19):3504-13.
Thomas DG, Giordano TJ, Sanders D, et al. Expression of receptor tyrosine kinases epidermal growth factor receptor and HER-2/neu in synovial sarcoma. Cancer. 2005;103(4):830-8.
Xie Y, Skytting B, Nilsson G, Brodin B, Larsson O. Expression of insulin-like growth factor-1 receptor in synovial sarcoma: association with an aggressive phenotype. Cancer Res. 1999;59(15):3588-91.
Ho AL, Vasudeva SD, Lae M, et al. PDGF receptor alpha is an alternative mediator of rapamycin-induced Akt activation: implications for combination targeted therapy of synovial sarcoma. Cancer Res. 2012;72(17):4515-25.
Michels S, Trautmann M, Sievers E, et al. SRC signaling is crucial in the growth of synovial sarcoma cells. Cancer Res. 2013;73(8):2518-28.
de Bruijn DR, Allander SV, van Dijk AH, et al. The synovial-sarcoma-associated SS18-SSX2 fusion protein induces epigenetic gene (de)regulation. Cancer Res. 2006;66(19):9474-82.
Sun Y, Gao D, Liu Y, Huang J, Lessnick S, Tanaka S. IGF2 is critical for tumorigenesis by synovial sarcoma oncoprotein SYT-SSX1. Oncogene. 2006;25(7):1042-52.
Wakamatsu T, Naka N, Sasagawa S, et al. Deflection of vascular endothelial growth factor action by SS18-SSX and composite vascular endothelial growth factor- and chemokine (C-X-C motif) receptor 4-targeted therapy in synovial sarcoma. Cancer Sci. 2014;105(9):1124-34.
Nielsen TO, West RB, Linn SC, et al. Molecular characterisation of soft-tissue tumours: a gene expression study. Lancet. 2002;359(9314):1301-7.
Ishibe T, Nakayama T, Okamoto T, et al. Disruption of fibroblast growth factor signal pathway inhibits the growth of synovial sarcomas: potential application of signal inhibitors to molecular target therapy. Clin Cancer Res. 2005;11(7):2702-12.
Palmerini E, Benassi MS, Quattrini I, et al. Prognostic and predictive role of CXCR4, IGF-1R and Ezrin expression in localized synovial sarcoma: is chemotaxis important to tumor response? Orphanet J Rare Dis. 2015;10:6.
Saito T. The SYT-SSX fusion protein and histological epithelial differentiation in synovial sarcoma: relationship with extracellular matrix remodeling. Int J Clin Exp Pathol. 2013;6(11):2272-9.
Haldar M, Randall RL, Capecchi MR. Synovial sarcoma: from genetics to genetic-based animal modeling. Clin Orthop Rel Res. 2008;466(9):2156-67.
Inagaki H, Nagasaka T, Otsuka T, Sugiura E, Nakashima N, Eimoto T. Association of SYT-SSX fusion types with proliferative activity and prognosis in synovial sarcoma. Mod Pathol. 2000;13(5):482-8.
Antonescu CR, Kawai A, Leung DH, et al. Strong association of SYT-SSX fusion type and morphologic epithelial differentiation in synovial sarcoma. Diagn Mol Pathol.2000;9(1):1-8.
Przybyl J, Sciot R, Rutkowski P, et al. Recurrent and novel SS18-SSX fusion transcripts in synovial sarcoma: description of three new cases. Tumour Biol. 2012;33(6):2245-53.
Keith JL, Bilbao J, Croul S, et al. Clinical Neuropathology practice guide 6-2013: morphology and an appropriate immunohistochemical screening panel aid in the identification of synovial sarcoma by neuropathologists. Clin Neuropathol. 2013;32(6):461-70.
Kohashi K, Oda Y, Yamamoto H, et al. Reduced expression of SMARCB1/INI1 protein in synovial sarcoma. Mod Pathol. 2010;23(7):981-90.
Ordonez NG, Mahfouz SM, Mackay B. Synovial sarcoma: an immunohistochemical and ultrastructural study. Hum Pathol. 1990;21(7):733-49.
Jorgensen LJ, Lyon H, Myhre-Jensen O, Nordentoft A, Sneppen O. Synovial sarcoma. An immunohistochemical study of the epithelial component. APMIS Acta Pathol Microbiol Immunol Scand. 1994;102(3):191-6.
Fisher C, Montgomery E, Healy V. Calponin and h-caldesmon expression in synovial sarcoma; the use of calponin in diagnosis. Histopathology. 2003;42(6):588-93.
Terry J, Saito T, Subramanian S, et al. TLE1 as a diagnostic immunohistochemical marker for synovial sarcoma emerging from gene expression profiling studies. Am J Surg Pathol. 2007;31(2):240-6.
Valente AL, Tull J, Zhang S. Specificity of TLE1 expression in unclassified high-grade sarcomas for the diagnosis of synovial sarcoma. Appl Immunohistochem Mol Morphol. 2013;21(5):408-13.
Foo WC, Cruise MW, Wick MR, Hornick JL. Immunohistochemical staining for TLE1 distinguishes synovial sarcoma from histologic mimics. Am J Clin Pathol. 2011;135(6):839-44.
Kosemehmetoglu K, Vrana JA, Folpe AL. TLE1 expression is not specific for synovial sarcoma: a whole section study of 163 soft-tissue and bone neoplasms. Mod Pathol. 2009;22(7):872-8.
Lai JP, Robbins PF, Raffeld M, et al. NY-ESO-1 expression in synovial sarcoma and other mesenchymal tumors: significance for NY-ESO-1-based targeted therapy and differential diagnosis. Mod Pathol. 2012;25(6):854-8.
Endo M, de Graaff MA, Ingram DR, et al. NY-ESO-1 (CTAG1B) expression in mesenchymal tumors. Mod Pathol. 2015;28(4):587-95.
Shi W, Indelicato DJ, Morris CG, Scarborough MT, Gibbs CP, Zlotecki RA. Long-term treatment outcomes for patients with synovial sarcoma: a 40-year experience at the University of Florida. Am J Clin Oncol. 2013;36(1):83-8.
Guadagnolo BA, Zagars GK, Ballo MT, et al. Long-term outcomes for synovial sarcoma treated with conservation surgery and radiotherapy. Int J Radiat Oncol Biol Phys. 2007;69(4):1173-80.
Chan JA, McMenamin ME, Fletcher CD. Synovial sarcoma in older patients: clinicopathological analysis of 32 cases with emphasis on unusual histological features. Histopathology. 2003;43(1):72-83.
Spillane AJ, A’Hern R, Judson IR, Fisher C, Thomas JM. Synovial sarcoma: a clinicopathologic, staging, and prognostic assessment. J Clin Oncol. 2000;18(22):3794-803.
Ferrari A, Gronchi A, Casanova M, et al. Synovial sarcoma: a retrospective analysis of 271 patients of all ages treated at a single institution. Cancer. 2004;101(3):627-34.
Bergh P, Meis-Kindblom JM, Gherlinzoni F, et al. Synovial sarcoma: identification of low and high risk groups. Cancer. 1999;85(12):2596-607.
ten Heuvel SE, Hoekstra HJ, Bastiaannet E, Suurmeijer AJ. The classic prognostic factors tumor stage, tumor size, and tumor grade are the strongest predictors of outcome in synovial sarcoma: no role for SSX fusion type or ezrin expression. Appl Immunohistochem Molec Morphol. 2009;17(3):189-95.
Vlenterie M, Ho VK, Kaal SE, Vlenterie R, Haas R, van der Graaf WT. Age as an independent prognostic factor for survival of localised synovial sarcoma patients. Br J Cancer. 2015;113(11):1602-6.
Speth BM, Krieg AH, Kaelin A, et al. Synovial sarcoma in patients under 20 years of age: a multicenter study with a minimum follow-up of 10 years. J Child Orthop. 2011;5(5):335-42.
Takenaka S, Ueda T, Naka N, et al. Prognostic implication of SYT-SSX fusion type in synovial sarcoma: a multi-institutional retrospective analysis in Japan. Oncol Rep. 2008;19(2):467-76.
Golouh R, Stanta G, Bracko M, Bonin S. Correlation of MTS1/p16 and nm23 mRNA expression with survival in patients with peripheral synovial sarcoma. J Surg Oncol. 2001;76(2):83-8.
Lewis JJ, Antonescu CR, Leung DH, et al. Synovial sarcoma: a multivariate analysis of prognostic factors in 112 patients with primary localized tumors of the extremity. J Clin Oncol. 2000;18(10):2087-94.
Thway K, Fisher C. Synovial sarcoma: defining features and diagnostic evolution. Ann Diagn Pathol. 2014;18(6):369-80.
Canter RJ, Qin LX, Maki RG, Brennan MF, Ladanyi M, Singer S. A synovial sarcoma-specific preoperative nomogram supports a survival benefit to ifosfamide-based chemotherapy and improves risk stratification for patients. Clin Cancer Res. 2008;14(24):8191-7.
Nagayama S, Fukukawa C, Katagiri T, et al. Therapeutic potential of antibodies against FZD 10, a cell-surface protein, for synovial sarcomas. Oncogene. 2005;24(41):6201-12.
Ishibe T, Nakayama T, Aoyama T, Nakamura T, Toguchida J. Neuronal differentiation of synovial sarcoma and its therapeutic application. Clin Ortho Res. 2008;466(9):2147-55.
Nielsen TO, Hsu FD, O’Connell JX, et al. Tissue microarray validation of epidermal growth factor receptor and SALL2 in synovial sarcoma with comparison to tumors of similar histology. Am J Pathol. 2003;163(4):1449-56.
Lagarde P, Przybyl J, Brulard C, et al. Chromosome instability accounts for reverse metastatic outcomes of pediatric and adult synovial sarcomas. J Clin Oncol. 2013;31(5):608-15.
Metzger-Filho O, Catteau A, Michiels S, et al. Genomic Grade Index (GGI): feasibility in routine practice and impact on treatment decisions in early breast cancer. PloS One. 2013;8(8):e66848.
Chibon F, Lagarde P, Salas S, et al. Validated prediction of clinical outcome in sarcomas and multiple types of cancer on the basis of a gene expression signature related to genome complexity. Nat Med. 2010;16(7):781-7.
El Beaino M, Araujo DM, Gopalakrishnan V, Lazar AJ, Lin PP. Prognosis of T1 synovial sarcoma depends upon surgery by oncologic surgeons. J Surg Oncol. 2016;114(4):490-4.
Ryan CW, Desai J. The past, present, and future of cytotoxic chemotherapy and pathway-directed targeted agents for soft-tissue sarcoma. American Society of Clinical Oncology educational book / ASCO. American Society of Clinical Oncology meeting. 2013.
Bramwell VH, Anderson D, Charette ML. Doxorubicin-based chemotherapy for the palliative treatment of adult patients with locally advanced or metastatic soft-tissue sarcoma: a meta-analysis and clinical practice guideline. Sarcoma. 2000;4(3):103-12.
Volkova M, Russell R, 3rd. Anthracycline cardiotoxicity: prevalence, pathogenesis and treatment. Curr Cardiol Rev. 2011;7(4):214-20.
Tascilar M, Loos WJ, Seynaeve C, Verweij J, Sleijfer S. The pharmacologic basis of ifosfamide use in adult patients with advanced soft-tissue sarcomas. Oncologist. 2007;12(11):1351-60.
Edmonson JH, Ryan LM, Falkson CI, Hicks DG, Blum RH. Phase II study of ifosfamide+doxorubicin in patients with advanced synovial sarcomas (E1793): A Trial of the Eastern Cooperative Oncology Group. Sarcoma. 2003;7(1):9-11.
Siehl JM, Thiel E, Schmittel A, et al. Ifosfamide/liposomal daunorubicin is a well tolerated and active first-line chemotherapy regimen in advanced soft-tissue sarcoma: results of a phase II study. Cancer. 2005;104(3):611-7.
Eilber FC, Dry SM. Diagnosis and management of synovial sarcoma. J Surg Oncol. 2008;97(4):314-20.
Eilber FC, Brennan MF, Eilber FR, et al. Chemotherapy is associated with improved survival in adult patients with primary extremity synovial sarcoma. Ann Surg. 2007;246(1):105-13.
Ferrari A, De Salvo GL, Dall’Igna P, et al. Salvage rates and prognostic factors after relapse in children and adolescents with initially localised synovial sarcoma. Eur J Cancer. 2012;48(18):3448-55.
Lee SH, Chang MH, Baek KK, et al. High-dose ifosfamide as second- or third-line chemotherapy in refractory bone and soft-tissue sarcoma patients. Oncology. 2011;80(3-4):257-61.
Svancarova L, Blay JY, Judson IR, et al. Gemcitabine in advanced adult soft-tissue sarcomas. A phase II study of the EORTC Soft Tissue and Bone Sarcoma Group. Eur J Cancer. 2002;38(4):556-9.
Okuno S, Edmonson J, Mahoney M, Buckner JC, Frytak S, Galanis E. Phase II trial of gemcitabine in advanced sarcomas. Cancer. 2002;94(12):3225-9.
Verweij J, Lee SM, Ruka W, et al. Randomized phase II study of docetaxel versus doxorubicin in first- and second-line chemotherapy for locally advanced or metastatic soft-tissue sarcomas in adults: a study of the european organization for research and treatment of cancer soft tissue and bone sarcoma group. J Clin Oncol. 2000;18(10):2081-6.
Kostler WJ, Brodowicz T, Attems Y, et al. Docetaxel as rescue medication in anthracycline- and ifosfamide-resistant locally advanced or metastatic soft-tissue sarcoma: results of a phase II trial. Ann Oncol. 2001;12(9):1281-8.
Maki RG, Wathen JK, Patel SR, et al. Randomized phase II study of gemcitabine and docetaxel compared with gemcitabine alone in patients with metastatic soft-tissue sarcomas: results of sarcoma alliance for research through collaboration study 002 [corrected]. J Clin Oncol. 2007;25(19):2755-63.
Erber R, Thurnher A, Katsen AD, et al. Combined inhibition of VEGF and PDGF signaling enforces tumor vessel regression by interfering with pericyte-mediated endothelial cell survival mechanisms. FASEB J. 2004;18(2):338-40.
Timke C, Zieher H, Roth A, et al. Combination of vascular endothelial growth factor receptor/platelet-derived growth factor receptor inhibition markedly improves radiation tumor therapy. Clin Cancer Res. 2008;14(7):2210-9.
Sleijfer S, Ray-Coquard I, Papai Z, et al. Pazopanib, a multikinase angiogenesis inhibitor, in patients with relapsed or refractory advanced soft-tissue sarcoma: a phase II study from the European organisation for research and treatment of cancer-soft-tissue and bone sarcoma group (EORTC study 62043). J Clin Oncol. 2009;27(19):3126-32.
Kasper B, Sleijfer S, Litiere S, et al. Long-term responders and survivors on pazopanib for advanced soft-tissue sarcomas: subanalysis of two European Organisation for Research and Treatment of Cancer (EORTC) clinical trials 62043 and 62072. Ann Oncol. 2014;25(3):719-24.
Weigel B, Malempati S, Reid JM, et al. Phase 2 trial of cixutumumab in children, adolescents, and young adults with refractory solid tumors: a report from the Children’s Oncology Group. Pediatr Blood Cancer. 2014;61(3):452-6.
Zanardi E, Maruzzo M, Montesco MC, Roma A, Rastrelli M, Basso U. Response to trabectedin in a patient with advanced synovial sarcoma with lung metastases. Anti-cancer Drugs. 2014;25(10):1227-30.
Sanfilippo R, Dileo P, Blay JY, et al. Trabectedin in advanced synovial sarcomas: a multicenter retrospective study from four European institutions and the Italian Rare Cancer Network. Anti-cancer Drugs. 2015;26(6):678-81.
Di Giandomenico S, Frapolli R, Bello E, et al. Mode of action of trabectedin in myxoid liposarcomas. Oncogene. 2014;33(44):5201-10.
Germano G, Frapolli R, Belgiovine C, et al. Role of macrophage targeting in the antitumor activity of trabectedin. Cancer Cell. 2013;23(2):249-62.
Shiloh Y. The ATM-mediated DNA-damage response: taking shape. Trends Biochem Sci. 2006;31(7):402-10.
Bakkenist CJ, Kastan MB. DNA damage activates ATM through intermolecular autophosphorylation and dimer dissociation. Nature. 2003;421(6922):499-506.
Ito T, Ouchida M, Morimoto Y, et al. Significant growth suppression of synovial sarcomas by the histone deacetylase inhibitor FK228 in vitro and in vivo. Cancer Lett. 2005;224(2):311-9.
Watanabe R, Ui A, Kanno S, et al. SWI/SNF factors required for cellular resistance to DNA damage include ARID1A and ARID1B and show interdependent protein stability. Cancer Res. 2014;74(9):2465-75.
Barham W, Frump AL, Sherrill TP, et al. Targeting the Wnt pathway in synovial sarcoma models. Cancer Discov. 2013;3(11):1286-301.
Robbins PF, Morgan RA, Feldman SA, et al. Tumor regression in patients with metastatic synovial cell sarcoma and melanoma using genetically engineered lymphocytes reactive with NY-ESO-1. J Clin Oncol. 2011;29(7):917-24.
Gure AO, Wei IJ, Old LJ, Chen YT. The SSX gene family: characterization of 9 complete genes. Int J Cancer. 2002;101(5):448-53.
Bloom JE, McNeel DG, Olson BM. Vaccination using peptides spanning the SYT-SSX tumor-specific translocation. Expert Rev Vaccines. 2012;11(12):1401-4.
Chugh R, Wathen JK, Maki RG, et al. Phase II multicenter trial of imatinib in 10 histologic subtypes of sarcoma using a bayesian hierarchical statistical model. J Clin Oncol. 2009;27(19):3148-53.
Bond M, Bernstein ML, Pappo A, et al. A phase II study of imatinib mesylate in children with refractory or relapsed solid tumors: a Children’s Oncology Group study. Pediatr Blood Cancer. 2008;50(2):254-8.
Acknowledgment
We acknowledge Kim-Anh Vu for graphic art assistance and the Amschwand Sarcoma Cancer Foundation for support.
Disclosures
Each author has declared that he or she has no commercial associations or has received any financial or material support that might pose a conflict of interest with the submitted article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
El Beaino, M., Araujo, D.M., Lazar, A.J. et al. Synovial Sarcoma: Advances in Diagnosis and Treatment Identification of New Biologic Targets to Improve Multimodal Therapy. Ann Surg Oncol 24, 2145–2154 (2017). https://doi.org/10.1245/s10434-017-5855-x
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-017-5855-x