Abstract
Background
The administration of fluid irradiated with non-equilibrium atmospheric pressure plasma (NEAPP) has attracted much interest as a novel therapeutic method for cancer. The authors previously reported on the efficacy of plasma-activated medium (PAM) for treating cancer cell lines through the induction of apoptosis. In this study, the therapeutic effect of PAM was evaluated in vivo using a peritoneal metastasis mouse model.
Methods
Two gastric cancer cell lines were used in proliferation assays performed to optimize the production of PAM by changing the distance between the plasma source and the medium surface and by altering the volume of irradiated medium. Wound-healing and adhesion assays were conducted to determine the effect of PAM therapy on cell migration and adhesion capacity in vitro. Finally, a mouse model established by the intraperitoneal injection of enhanced green fluorescent protein-tagged gastric cancer cells was used to explore the efficacy of PAM administered intraperitoneally in inhibiting peritoneal metastasis formation.
Results
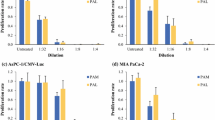
Shorter distances between the plasma source and the medium surface and smaller volumes of treated medium increased the anti-tumor effect of PAM. The PAM treatment attenuated gastric cancer cell migration and adhesion in vitro. The intraperitoneal administration of PAM decreased the formation of peritoneal metastatic nodules by 60% in the mouse model, and no adverse events were observed.
Conclusions
Plasma-activated liquids may represent a novel therapeutic method for the treatment of peritoneal metastases in gastric cancer.





Similar content being viewed by others
References
Jung KW, Won YJ, Kong HJ, Oh CM, Lee DH, Lee JS. Cancer statistics in Korea: incidence, mortality, survival, and prevalence in 2011. Cancer Res Treat. 2014;46:109–23.
Siegel R, Ma J, Zou Z, Jemal A. Cancer statistics, 2014. CA Cancer J Clin. 2014;64:9–29.
Shiozaki H, Elimova E, Slack RS, et al. Prognosis of gastric adenocarcinoma patients with various burdens of peritoneal metastases. J Surg Oncol. 2015;113:29–35.
Brun P, Brun P, Vono M, et al. Disinfection of ocular cells and tissues by atmospheric-pressure cold plasma. PLoS One. 2012;7:e33245.
Fridman G, Friedman G, Gutsol A, Shekhter AB, Vasilets VN, Fridman A. Applied plasma medicine. Plasma Process Polym. 2008;5:503–33.
Fridman G, Peddinghaus M, Balasubramanian M, Ayan H, Fridman A, Gutsol A, et al. Blood coagulation and living tissue sterilization by floating-electrode dielectric barrier discharge in air. Plasma Chem Plasma Proc. 2006;26:425–42.
Ahn HJ, Kim KI, Kim G, Moon E, Yang SS, Lee JS. Atmospheric-pressure plasma jet induces apoptosis involving mitochondria via generation of free radicals. PLoS One. 2011;6:e28154.
Gesbert F, Larue L. Non-thermal plasmas: novel preventive and curative therapy against melanomas? Exp Dermatol. 2014;23:716–7.
Hou J, Ma J, Yu KN, Li W, Cheng C, Bao L, Han W. Nonthermal plasma treatment altered gene expression profiling in non-small cell lung cancer A549 cells. BMC Genomics. 2015;16:435.
Ma Y, Ha CS, Hwang SW, Lee HJ, Kim GC, Lee KW, Song K. Nonthermal atmospheric pressure plasma preferentially induces apoptosis in p53-mutated cancer cells by activating ROS stress-response pathways. PLoS One. 2014;9:e91947.
Thiyagarajan M, Sarani A, Gonzales XF. Characterization of an atmospheric pressure plasma jet and its applications for disinfection and cancer treatment. Stud Health Technol Inform. 2013;184:443–9.
Tanaka H, Mizuno M, Ishikawa K, et al. Plasma with high electron density and plasma-activated medium for cancer treatment. Clin Plasma Med. 2015;3:72–6.
Tanaka H, Mizuno M, Toyokuni S, et al. Cancer therapy using nonthermal atmospheric pressure plasma with ultra-high electron density. Phys Plasmas. 2015;22:122004.
Tanaka H, Mizuno M, Ishikawa K, et al. Plasma-activated medium selectively kills glioblastoma brain tumor cells by downregulating a survival signaling molecule, AKT kinase. Plasma Med. 2011;1:265–77.
Hattori N, Yamada S, Torii K, et al. Effectiveness of plasma treatment on pancreatic cancer cells. Int J Oncol. 2015;47:1655–62.
Torii K, Yamada S, Nakamura K, et al. Effectiveness of plasma treatment on gastric cancer cells. Gastric Cancer. 2014;18:635–43.
Utsumi F, Kajiyama H, Nakamura K, Tanaka H, Hori M, Kikkawa F. Selective cytotoxicity of indirect nonequilibrium atmospheric pressure plasma against ovarian clear-cell carcinoma. Springerplus. 2014;3:398.
Chang JW, Kang SU, Shin YS, et al. Non-thermal atmospheric pressure plasma inhibits thyroid papillary cancer cell invasion via cytoskeletal modulation, altered MMP-2/-9/uPA activity. PLoS One. 2014;9:e92198.
Kim CH, Kwon S, Bahn JH, Lee K, Jun SI, Rack PD, Baek SJ. Effects of atmospheric nonthermal plasma on invasion of colorectal cancer cells. Appl Phys Lett. 2010;96:243701.
Utsumi F, Kajiyama H, Nakamura K, et al. Effect of indirect nonequilibrium atmospheric pressure plasma on anti-proliferative activity against chronic chemo-resistant ovarian cancer cells in vitro and in vivo. PLoS One. 2013;8:e81576.
Ohashi N, Kodera Y, Nakanishi H, et al. Efficacy of intraperitoneal chemotherapy with paclitaxel targeting peritoneal micrometastasis as revealed by GFP-tagged human gastric cancer cell lines in nude mice. Int J Oncol. 2005;27:637–44.
Kieft IE, Broers JLV, Caubet-Hilloutou V, Slaaf DW, Ramaekers FCS, Stoffels E. Electric discharge plasmas influence attachment of cultured CHO K1 cells. Bioelectromagnetics. 2004;25:362–8.
Keidar M, Walk R, Shashurin A, et al. Cold plasma selectivity and the possibility of a paradigm shift in cancer therapy. Br J Cancer. 2011;105:1295–301.
Vandamme M, Robert E, Dozias S, Sobilo J, Lerondel S, Le Pape A, et al. Response of human glioma U87 xenografted on mice to nonthermal plasma treatment. Plasma Med. 2011;1:27–43.
Brulle L, Vandamme M, Ries D, et al. Effects of a nonthermal plasma treatment alone or in combination with gemcitabine in a MIA PaCa2-luc orthotopic pancreatic carcinoma model. PLoS One. 2012;7:e52653.
Vandamme M, Robert E, Lerondel S, et al. ROS implication in a new antitumor strategy based on nonthermal plasma. Int J Cancer. 2012;130:2185–94.
Walk RM, Snyder JA, Srinivasan P, et al. Cold atmospheric plasma for the ablative treatment of neuroblastoma. J Pediatr Surg. 2013;48:67–73.
Utsumi F, Kajiyama H, Nakamura KAE, et al. Variable susceptibility of ovarian cancer cells to nonthermal plasma-activated medium. Oncol Rep. 2016;35:3169–77.
Joh HM, Choi JY, Kim SJ, Chung TH, Kang TH. Effect of additive oxygen gas on cellular response of lung cancer cells induced by atmospheric-pressure helium plasma jet. Sci Rep. 2014;4:6638.
Winter J, Wende K, Masur K, et al. Feed gas humidity: a vital parameter affecting a cold atmospheric-pressure plasma jet and plasma-treated human skin cells. J Phys D Appl Phys. 2013;46:295401.
Rice BW, Cable MD, Nelson MB. In vivo imaging of light-emitting probes. J Biomed Opt. 2001;6:432–40.
Kishimoto H, Zhao M, Hayashi K, et al. In vivo internal tumor illumination by telomerase-dependent adenoviral GFP for precise surgical navigation. Proc Natl Acad Sci USA. 2009;106:14514–7.
Kishimoto H, Aki R, Urata Y, et al. Tumor-selective, adenoviral-mediated GFP genetic labeling of human cancer in the live mouse reports future recurrence after resection. Cell Cycle. 2011;10:2737–41.
Weissleder R. A clearer vision for in vivo imaging. Nat Biotechnol. 2001;19:316–7.
Disclosures
There are no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
10434_2016_5759_MOESM1_ESM.ppt
Supplementary material 1 (PPT 845 kb) Experimental system for producing PAM. (a) Photograph of our device. (b) Schematics of PAM production.
10434_2016_5759_MOESM2_ESM.pptx
Supplementary material 2 (PPTX 73 kb)Effect of repeated PAM exposure. A total of 3×103 cells were seeded into a 96-well plate, and the medium was replaced as follows. Untreated: The medium was replaced every 24 h with RPMI-1640. 1: At 24 h after seeding, the medium was replaced with PAM, and after another 24 h and 48 h, the medium was replaced with RPMI-1640. 2: At 24 h and 48 h after seeding, the medium was replaced with PAM, and after another 24 h, the medium was replaced with RPMI-1640. 3: At 24 h, 48 h and 72 h after seeding, the medium was replaced with PAM. Finally, at 96 h after seeding, an MTS assay was performed, and the proliferation rates were calculated. Each column represents the mean of three replicates, and the error bars represent standard deviation.
Rights and permissions
About this article
Cite this article
Takeda, S., Yamada, S., Hattori, N. et al. Intraperitoneal Administration of Plasma-Activated Medium: Proposal of a Novel Treatment Option for Peritoneal Metastasis From Gastric Cancer. Ann Surg Oncol 24, 1188–1194 (2017). https://doi.org/10.1245/s10434-016-5759-1
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-016-5759-1