Abstract
Introduction
Sarcopenia is linked to poor outcomes after abdominal surgery. We hypothesized that radiographic sarcopenia metrics enhance prediction of complications after pancreaticoduodenectomy (PD) when combined with clinical and frailty data.
Methods
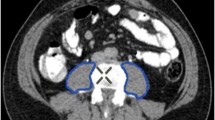
Preoperative geriatric assessments and CT scans of patients undergoing PD were reviewed. Sarcopenia was assessed at L3 using total psoas area index (TPAI) and weighted average Hounsfield units (HU), i.e., estimates of psoas muscle volume and density. Outcomes included 30-day American College of Surgeons National Surgical Quality Improvement Program (NSQIP) serious complications, Clavien–Dindo complications, unplanned intensive care unit (ICU) admission, hospital length of stay (LOS), non-home facility (NHF) discharge, and readmission rates.
Results
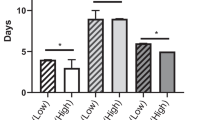
Low HU score correlated with NSQIP serious complications (r = −0.31, p = 0.0098), Clavien–Dindo complication grade (r = −0.29, p = 0.0183), unplanned ICU admission (r = −0.28, p = 0.0239), and NHF discharge (r = −0.25, p = 0.0426). Controlling for a “base model” of age, body mass index, American Society of Anesthesiologists score, and comorbidity burden, Fried’s exhaustion (odds ratio [OR] 4.72 [1.23–17.71], p = 0.021), and HU (OR 0.88 [0.79–0.98], p = 0.024) predicted NSQIP serious complications. Area under the receiver-operator characteristic (AUC) curves demonstrated that the combination of the base model, exhaustion, and HU trended towards improving the prediction of NSQIP serious complications compared with the base model alone (AUC = 0.81 vs. 0.70; p = 0.09). Additionally, when controlling for the base model, TPAI (β-coefficient = 0.55 [0.10–1.01], p = 0.018) and exhaustion (β-coefficient = 2.47 [0.75–4.20], p = 0.005) predicted LOS and exhaustion (OR 4.14 [1.48–11.6], p = 0.007) predicted readmissions.
Conclusions
When combined with clinical and frailty assessments, radiographic sarcopenia metrics enhance prediction of post-PD outcomes.


Similar content being viewed by others
References
Rahib L, Smith BD, Aizenberg R, Rosenzweig AB, Fleshman JM, Matrisian LM. Projecting cancer incidence and deaths to 2030: the unexpected burden of thyroid, liver, and pancreas cancers in the United States. Cancer Res. 2014;74(11):2913–21.
Mohammed S, Fisher WE. Quality metrics in pancreatic surgery. Surg Clin North Am. 2013;93(3):693–709.
Haigh PI, Bilimoria KY, DiFronzo LA. Early postoperative outcomes after pancreaticoduodenectomy in the elderly. Arch Surg. 2011;146(6):715–23.
Sohn TA, Yeo CJ, Cameron JL, et al. Should pancreaticoduodenectomy be performed in octogenarians? J Gastrointest Surg. 1998;2(3):207–16.
Ito Y, Kenmochi T, Irino T, et al. The impact of surgical outcome after pancreaticoduodenectomy in elderly patients. World J Surg Oncol. 2011;9:102.
Scurtu R, Bachellier P, Oussoultzoglou E, Rosso E, Maroni R, Jaeck D. Outcome after pancreaticoduodenectomy for cancer in elderly patients. J Gastrointest Surg. 2006;10(6):813–22.
Walston J, Hadley EC, Ferrucci L, et al. Research agenda for frailty in older adults: toward a better understanding of physiology and etiology: summary from the American Geriatrics Society/National Institute on Aging Research Conference on Frailty in Older Adults. J Am Geriatr Soc. 2006;54(6):991–1001.
Hubbard RE, Story DA. Patient frailty: the elephant in the operating room. Anaesthesia. 2014;69(Suppl 1):26–34.
Kim SW, Han HS, Jung HW, et al. Multidimensional frailty score for the prediction of postoperative mortality risk. JAMA Surg. 2014;149(7):633–40.
Hewitt J, Moug SJ, Middleton M, et al. Prevalence of frailty and its association with mortality in general surgery. Am J Surg. 2014;209:254–9.
Arya S, Kim SI, Duwayri Y, et al. Frailty increases the risk of 30-day mortality, morbidity, and failure to rescue after elective abdominal aortic aneurysm repair independent of age and comorbidities. J Vasc Surg. 2014;61:324–31.
McAdams-DeMarco MA, Law A, King E, et al. Frailty and mortality in kidney transplant recipients. Am J Transplant. 2015;15(1):149–54.
Makary MA, Segev DL, Pronovost PJ, et al. Frailty as a predictor of surgical outcomes in older patients. J Am Coll Surg. 2010;210(6):901–8.
Dale W, Hemmerich J, Kamm A, et al. Geriatric assessment improves prediction of surgical outcomes in older adults undergoing pancreaticoduodenectomy: a prospective cohort study. Ann Surg. 2014;259(5):960–5.
Korc-Grodzicki B, Sun SW, Zhou Q, et al. Geriatric assessment as a predictor of delirium and other outcomes in elderly patients with cancer. Ann Surg. 2015;261(6):1085–90.
Lee JS, He K, Harbaugh CM, et al; Michigan Analytic Morphomics Group (MAMG). Frailty, core muscle size, and mortality in patients undergoing open abdominal aortic aneurysm repair. J Vasc Surg. 2011;53(4):912–7.
Hasselager R, Gögenur I. Core muscle size assessed by perioperative abdominal CT scan is related to mortality, postoperative complications, and hospitalization after major abdominal surgery: a systematic review. Langenbecks Arch Surg. 2014;399(3):287–95.
Reisinger KW, van Vugt JL, Tegels JJ, et al. Functional compromise reflected by sarcopenia, frailty, and nutritional depletion predicts adverse postoperative outcome after colorectal cancer surgery. Ann Surg. 2015;261(2):345–52.
Voron T, Tselikas L, Pietrasz D, et al. Sarcopenia impacts on short- and long-term results of hepatectomy for hepatocellular carcinoma. Ann Surg. 2015;261(6):1173–83.
Peng P, Hyder O, Firoozmand A, et al. Impact of sarcopenia on outcomes following resection of pancreatic adenocarcinoma. J Gastrointest Surg. 2012;16(8):1478–86.
Age adjusted Charlson Comorbidity Index. http://farmacologiaclinica.info/scales/Charlson_Comorbidity. Accessed 1 Nov 2014.
Fried LP, Tangen CM, Walston J, et al; Cardiovascular Health Study Collaborative Research Group. Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci. 2001;56(3):M146–56.
Guralnik JM, Simonsick EM, Ferrucci L, et al. A short physical performance battery assessing lower extremity function: association with self-reported disability and prediction of mortality and nursing home admission. J Gerontol. 1994;49(2):M85–94.
Prado CM, Lieffers JR, McCargar LJ, et al. Prevalence and clinical implications of sarcopenic obesity in patients with solid tumours of the respiratory and gastrointestinal tracts: a population-based study. Lancet Oncol. 2008;9(7):629–35.
Goodpaster BH, Thaete FL, Kelley DE. Composition of skeletal muscle evaluated with computed tomography. Ann N Y Acad Sci. 2000;904:18–24.
Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240:205–13.
ACS NSQIP Surgical Risk Calculator. About the ACS Risk Calculator. http://www.riskcalculator.facs.org/Home/About/ Accessed 1 Nov 2014.
Bilimoria KY, Liu Y, Paruch JL, et al. Development and evaluation of the universal ACS NSQIP surgical risk calculator: a decision aid and informed consent tool for patients and surgeons. J Am Coll Surg. 2013;217(5):833–42; e1–3.
Moons KGM, Royston P, Vergouwe Y, et al. Prognosis and prognostic research: what, why, and how? BMJ. 2009;338:b375.
Cohen J CP, West SG, Aiken LS. Applied multiple regression/correlation analysis for the behavioral sciences. 3rd edn. Mahwah, NJ: Lawrence Earlbaum Associates; 2003.
House MG, Fong Y, Arnaoutakis DJ, et al. Preoperative predictors for complications after pancreaticoduodenectomy: impact of BMI and body fat distribution. J Gastrointest Surg. 2008;12(2):270–8.
Williams TK, Rosato EL, Kennedy EP, et al. Impact of obesity on perioperative morbidity and mortality after pancreaticoduodenectomy. J Am Coll Surg. 2009;208(2):210–7.
Tsai S, Choti MA, Assumpcao L, et al. Impact of obesity on perioperative outcomes and survival following pancreaticoduodenectomy for pancreatic cancer: a large single-institution study. J Gastrointest Surg. 2010;14(7):1143–50.
Wolters U, Wolf T, Stützer H, et al. ASA classification and perioperative variables as predictors of postoperative outcome. Br J Anaesth. 1996;77:217–22.
Finlayson E, Fan Z, Birkmeyer JD. Outcomes in octogenarians undergoing high-risk cancer operation: a national study. J Am Coll Surg. 2007;205:729–34.
Riall TS, Reddy DM, Nealon WH, et al. The effect of age on short-term outcomes after pancreatic resection: a population-based study. Ann Surg. 2008;248:459–67.
Englesbe MJ, Terjimanian MN, Lee JS, et al. Morphometric age and surgical risk. J Am Coll Surg. 2013;216(5):976–85.
Levi B, Zhang P, Lisiecki J, et al. Use of morphometric assessment of body composition to quantify risk of surgical-site infection in patients undergoing component separation ventral hernia repair. Plast Reconstr Surg. 2014;133(4):559e–66e.
Waits SA, Kim EK, Terjimanian MN, et al. Morphometric age and mortality after liver transplant. JAMA Surg. 2014;149(4):335–40.
Cooper AB, Slack R, Fogelman D, et al. Characterization of anthropometric changes that occur during neoadjuvant therapy for potentially resectable pancreatic cancer. Ann Surg Oncol. 2014;22:2416–23.
Acknowledgment
The authors gratefully acknowledge Mitchell C. Posner, M.D., Jeffrey B. Matthews, M.D., Eugene A. Choi, M.D., and Alaine Kamm, N.P., who recruited and cared for study patients and collected data; Aparna Palakodeti, Ph.D., who participated in study design and CT analysis; Teresa G. Barry and Randi Rothman, who performed GA and collected data; and Nneka Chukwueke, who collected data. Finally, we dedicate this work to the memory of our beloved friend and colleague, Joshua A. Hemmerich, Ph.D.
Disclosure
This study was funded by Carole and Gordon Segal, the Michael Rolfe Pancreatic Cancer Foundation, and the Ben D. Kissel Fund for Pancreatic Cancer Research. The authors maintained full independence in the conduct of this research and have no commercial interests in the subject of this study.
Author information
Authors and Affiliations
Corresponding author
Additional information
Joshua A. Hemmerich was Deceased on March 25, 2015.
Kevin K. Roggin and William Dale have contributed equally to this work.
Rights and permissions
About this article
Cite this article
Sur, M.D., Namm, J.P., Hemmerich, J.A. et al. Radiographic Sarcopenia and Self-reported Exhaustion Independently Predict NSQIP Serious Complications After Pancreaticoduodenectomy in Older Adults. Ann Surg Oncol 22, 3897–3904 (2015). https://doi.org/10.1245/s10434-015-4763-1
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-015-4763-1