Abstract
Background
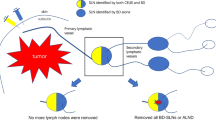
In breast cancer patients, sentinel lymph nodes (SLN) can be identified in the breast clinic using contrast-enhanced ultrasound (CEUS). This study aimed to characterize and compare the extent of axillary metastases in patients with either a benign or malignant SLN core biopsy at the end of surgical treatment.
Methods
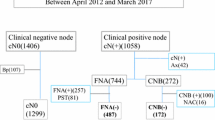
Between 2009 and 2014, prospective data were collected on consecutive patients who underwent targeted core biopsy of SLN identified using CEUS in the breast clinic. Patients with abnormal lymph nodes (LN) detected on grey-scale ultrasound were not included. Patients whose initial SLN core biopsy was benign were compared with those who had a malignant SLN core biopsy.
Results
555 patients with invasive breast cancer had SLN successfully identified and core biopsied. 487 had a benign SLN core biopsy and 427 (88 %) did not have metastases found in surgically excised SLN. Only 2 % of patients with an initial benign SLN core biopsy were found to have 2 or more LN macrometastases. 68 patients had a malignant SLN core biopsy and 52 % had 2 or more LN macrometastases. The total volume of LN metastases was higher in the group of patients who had an initial malignant SLN core biopsy (P < 0.001).
Conclusions
Patients with a normal grey-scale ultrasound and benign SLN core biopsy are unlikely to have extensive axillary disease and may be ideally suited for axillary conservation. The decision to omit axillary LN dissection for patients with a malignant SLN core biopsy must be carefully considered because many will have undetected high-volume metastases.


Similar content being viewed by others
References
Schijven MP, Vingerhoets AJ, Rutten HJ, Nieuwenhuijzen GA, Roumen RM, van Bussel ME, Voogd AC. Comparison of morbidity between axillary lymph node dissection and sentinel node biopsy. Eur J Surg Oncol. 2003;29:341–50.
Veronesi U, Paganelli G, Viale G, et al. A randomised comparison of sentinel-node biopsy with routine axillary dissection in breast cancer. N Engl J Med. 2003;349:546–53.
CG80 Early and locally advanced breast cancer: full guideline. United Kingdom, National Institute for Health and Clinical Excellence. February 2009. http://www.nice.org.uk/guidance/cg80/resources/guidance-early-and-locally-advanced-breast-cancer-pdf. Accessed July 2014
Gur AS, Unal B, Johnson R, Ahrendt G, Bonaventura M, Gordon P, Sonan A. Predictive probability of four different breast cancer nomograms for nonsentinel axillary lymph node metastasis in positive sentinel node biopsy. J Am Coll Surg. 2009;208:229–35.
Giuliano AE, Hunt KK, Ballman KV, Beitsch PD, Whitworth PW, Blumencranz PW, et al. Axillary dissection vs no axillary dissection in women with invasive breast cancer and sentinel node metastasis. JAMA. 2011;305:569–75.
Grill IS, Kestin LL, Goldstein N, Mitchell C, Martinez A, Ingold J, Vicini FA. Risk factors for regional nodal failure after breast-conserving therapy: regional nodal irradiation reduces rate of axillary failure in patients with four or more positive lymph nodes. Int J Radiat Oncol Biol Phys. 2003;56:658–70.
Alvarez S, Anorbe E, Alcorta P, Lopez F, Alonso I, Cortes J. Role of sonography in the diagnosis of axillary lymph node metastases in breast cancer: a systematic review. AJR Am J Roentgenol. 2006;186:1342–8.
Caudle AS, Kuerer HM, Le-Petross HT, Yang W, Yi M, Bedrosian I, Krishnamurthy S, Fornage BD, Hunt KK, Mittendorf EA. Predicting the extent of nodal disease in early-stage breast cancer. Ann Surg Oncol. 2014;21:3440–7.
Yang WT, Metreweli C, Lam PK, Chang J. Benign and malignant breast masses and axillary nodes: evaluation with echo enhanced color power Doppler ultrasound. Radiology. 2001;220:795–802.
Sever A, Jones S, Cox K, Weeks J, Mills P, Jones P. Preoperative localization of sentinel lymph nodes using intradermal microbubbles and contrast-enhanced ultrasonography in patients with breast cancer. Br J Surg. 2009;96:1295–9
Goldberg BB, Merton DA, Liu JB, et al. Sentinel lymph nodes in a swine model with melanoma: contrast-enhanced lymphatic US. Radiology. 2004;230:324–30.
Cox K, Sever A, Jones S, Weeks J, Mills P, Devalia H, et al. Validation of a technique using microbubbles and contrast-enhanced ultrasound (CEUS) to biopsy sentinel lymph nodes (SLN) in preoperative breast cancer patients with a normal grey-scale axillary ultrasound. Eur J Surg Oncol. 2013;39:760–5.
Kilbride KE, Lee MC, Nees AV, Cimmino VM, Diehl KM, Sabel MS, Hayes DF, Schott AF, Kleer CG, Chang AE, Newman LA. Axillary staging prior to neoadjuvant chemotherapy for breast cancer: predictors of recurrence. Ann Surg Oncol. 2008;15:3252–8.
Su YL, Li SH, Chen YY, Chen HC, Tay Y, Huang CH, Chou FF, Wu SC, Rau KM. Postmastectomy radiotherapy benefits subgroups of breast cancer patients with T1–2 tumor and 1–3 axillary lymph node(s) metastasis. Radiol Oncol. 2014;48:314–22.
Mills P, Sever AR, Weeks J, Fish D, Jones S, Jones P. Axillary ultrasound assessment in primary breast cancer: an audit of 653 cases. Breast J. 2010;16:460–3.
NHS breast screening programme and association of breast surgery: an audit of screen-detected breast cancers for the year of screening April 2012 to March 2013. May 2014. Public Health England, Wellington House, London, UK. www.gov.uk/phe.
Acknowledgment
This work was presented as a poster at the 2014 San Antonio Breast Cancer Symposium, San Antonio, TX, USA.
Disclosure
The authors have no conflicts of interest to report.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cox, K., Weeks, J., Mills, P. et al. Contrast-Enhanced Ultrasound Biopsy of Sentinel Lymph Nodes in Patients with Breast Cancer: Implications for Axillary Metastases and Conservation. Ann Surg Oncol 23, 58–64 (2016). https://doi.org/10.1245/s10434-015-4606-0
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-015-4606-0