Abstract
Background
Because duodenal adenocarcinoma (DA) is relatively rare, few studies have investigated the impact of resection type on long-term outcomes.
Methods
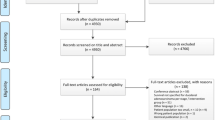
The Surveillance, Epidemiology, and End Results database was used to identify all patients between 1988 and 2010 with DA. Patients were divided into two groups based on the type of surgery received: simple resection (SR), defined as a simple removal of the primary site, and radical resection (RR), defined as removal of the primary site with a resection in continuity with other organs. Differences in disease-specific survival (DSS) and overall survival (OS) were compared.
Results
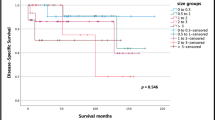
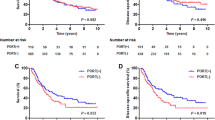
Of the 1,611 patients included, 746 (46.3 %) underwent SR and 865 (53.7 %) underwent RR. As expected, patients undergoing RR were more likely to present with poorly differentiated and large tumors, as well as advanced stage disease. Despite greater lymph node (LN) retrieval (11.0 vs. 6.8; p < 0.0001), RR was not associated with improved survival (5-year DSS and OS rates of 52.8 and 41.3 % for SR vs. 48.8 and 37.6 % for RR; p > 0.05). On univariate Cox proportional hazards regression analysis, the type of surgery was not associated with OS (odds ratio [OR] 0.98; 95 % confidence interval [CI] 0.87–1.11). Increasing TNM stages, tumor grade, fewer LNs removed, LN ratio, and absence of radiation were associated with worse survival. After controlling for confounding factors, type of surgery still did not influence OS (OR 1.11; 95 % CI 0.97–1.27).
Conclusions
Radical resection (e.g., in the form of pancreaticoduodenectomy) does not appear to impact survival compared with simple segmental resection for DA.



Similar content being viewed by others
References
Overman MJ, Hu C-Y, Wolff RA, Chang GJ. Prognostic value of lymph node evaluation in small bowel adenocarcinoma: analysis of the surveillance, epidemiology, and end results database. Cancer. 2010;116(23):5374–82. doi:10.1002/cncr.25324.
Overman MJ, Hu C-Y, Kopetz S, Abbruzzese JL, Wolff RA, Chang GJ. A population-based comparison of adenocarcinoma of the large and small intestine: insights into a rare disease. Ann Surg Oncol. 2012;19(5):1439–45. doi:10.1245/s10434-011-2173-6.
Moss WM, McCart PM, Juler G, Miller DR. Primary adenocarcinoma of the duodenum. Arch Surg. 1974;108(6):805–7.
Cortese AF, Cornell GN. Carcinoma of the duodenum. Cancer. 1972;29(4):1010–5.
Ouriel K, Adams JT. Adenocarcinoma of the small intestine. Am J Surg. 1984;147(1):66–71.
Sohn TA, Lillemoe KD, Cameron JL, et al. Adenocarcinoma of the duodenum: factors influencing long-term survival. J Gastrointest Surg Off J Soc Surg Aliment Tract. 1998;2(1):79–87.
Barnes G Jr, Romero L, Hess KR, Curley SA. Primary adenocarcinoma of the duodenum: management and survival in 67 patients. Ann Surg Oncol. 1994;1(1):73–8.
Joesting DR, Beart RW Jr, van Heerden JA, Weiland LH. Improving survival in adenocarcinoma of the duodenum. Am J Surg. 1981;141(2):228–31.
Lowell JA, Rossi RL, Munson JL, Braasch JW. Primary adenocarcinoma of third and fourth portions of duodenum. Favorable prognosis after resection. Arch Surg. 1992;127(5):557–60.
Kaklamanos IG, Bathe OF, Franceschi D, Camarda C, Levi J, Livingstone AS. Extent of resection in the management of duodenal adenocarcinoma. Am J Surg. 2000;179(1):37–41.
Bakaeen FG, Murr MM, Sarr MG, et al. What prognostic factors are important in duodenal adenocarcinoma? Arch Surg. 2000;135(6):635–41; discussion 641–42.
Brenner RL, Brown CH. Primary carcinoma of the duodenum; report of 15 cases. Gastroenterology. 1955;29(2):189–98.
Berger L, Koppelman H. Primary carcinoma of the duodenum. Ann Surg. 1942;116(5):738–50.
Newton WT. Mortality and morbidity associated with resection of pancreaticoduodenal cancers. Am Surg. 1961;27:74–9.
Stewart HL, Lieber MM. Carcinoma of the suprapapillary portion of the duodenum. Arch Surg. 1937;35(1):99–129. doi:10.1001/archsurg.1937.01190130102005.
Rose DM, Hochwald SN, Klimstra DS, Brennan MF. Primary duodenal adenocarcinoma: a ten-year experience with 79 patients. J Am Coll Surg. 1996;183(2):89–96.
Van Ooijen B, Kalsbeek HL. Carcinoma of the duodenum. Surg Gynecol Obstet. 1988;166(4):343–7.
Tocchi A, Mazzoni G, Puma F, et al. Adenocarcinoma of the third and fourth portions of the duodenum: results of surgical treatment. Arch Surg. 2003;138(1):80–5.
Hu J-X, Miao X-Y, Zhong D-W, Dai W-D, Liu W, Hu W. Surgical treatment of primary duodenal adenocarcinoma. Hepatogastroenterology. 2006;53(72):858–62.
Sarela AI, Brennan MF, Karpeh MS, Klimstra D, Conlon KCP. Adenocarcinoma of the duodenum: importance of accurate lymph node staging and similarity in outcome to gastric cancer. Ann Surg Oncol. 2004;11(4):380–6. doi:10.1245/ASO.2004.05.021.
Gibbs JF. Duodenal adenocarcinoma: is total lymph node sampling predictive of outcome? Ann Surg Oncol. 2004;11(4):354–5. 10.1245/ASO.2004.02.914.
Lee HG, You DD, Paik KY, Heo JS, Choi SH, Choi DW. Prognostic factors for primary duodenal adenocarcinoma. World J Surg. 2008;32(10):2246–52. doi:10.1007/s00268-008-9678-6
Sexe RB, Wade TP, Virgo KS, Johnson FE. Incidence and treatment of periampullary duodenal cancer in the U.S. veteran patient population. Cancer. 1996;77(2):251–4. doi:10.1002/(SICI)1097-0142(19960115)77:2<251::AID-CNCR5>3.0.CO;2-P.
Poultsides GA, Huang LC, Cameron JL, et al. Duodenal adenocarcinoma: clinicopathologic analysis and implications for treatment. Ann Surg Oncol. 2012;19(6):1928–35. doi:10.1245/s10434-011-2168-3.
Liang T-J, Wang B-W, Liu S-I, et al. Number of involved lymph nodes is important in the prediction of prognosis for primary duodenal adenocarcinoma. J Chin Med Assoc JCMA. 2012;75(11):573–580. doi:10.1016/j.jcma.2012.08.002.
Delcore R, Thomas JH, Forster J, Hermreck AS. Improving resectability and survival in patients with primary duodenal carcinoma. Am J Surg. 1993;166(6):626–31. doi:10.1016/S0002-9610(05)80668-3.
Struck A, Howard T, Chiorean EG, Clarke JM, Riffenburgh R, Cardenes HR. Non-ampullary duodenal adenocarcinoma: factors important for relapse and survival. J Surg Oncol. 2009;100(2):144–8. doi:10.1002/jso.21319.
Kelsey CR, Nelson JW, Willett CG, et al. Duodenal adenocarcinoma: patterns of failure after resection and the role of chemoradiotherapy. Int J Radiat Oncol. 2007;69(5):1436–41. doi:10.1016/j.ijrobp.2007.05.006.
Swartz MJ, Hughes MA, Frassica DA, et al. ADjuvant concurrent chemoradiation for node-positive adenocarcinoma of the duodenum. Arch Surg. 2007;142(3):285–8. doi:10.1001/archsurg.142.3.285.
Disclosure
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cloyd, J.M., Norton, J.A., Visser, B.C. et al. Does the Extent of Resection Impact Survival for Duodenal Adenocarcinoma? Analysis of 1,611 Cases. Ann Surg Oncol 22, 573–580 (2015). https://doi.org/10.1245/s10434-014-4020-z
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-014-4020-z