Abstract
Background
Lichen sclerosus is a chronic, progressive, inflammatory skin disease that presents unique challenges, particularly in the pediatric population, where limited data exist regarding its manifestation and optimal management. This retrospective observational monocentric study aims to provide insights into the clinical characteristics and therapeutic strategies employed, in a cohort of children and adolescents with genital lichen sclerosus.
Methods
A comprehensive analysis was conducted involving a cohort of 60 pediatric patients ranging from 1 to 15 years old, all diagnosed with lichen sclerosus. These cases were referred to the Pediatric Dermatology Regional Center of the University of Padua, Italy, between January 2018 and January 2022. Moreover, we propose a treatment protocol that showed beneficial outcomes in all of our patients. Specifically, the initial use of mid-potency topical corticosteroids has proven effective in addressing severe acute flares. Following this acute phase, transitioning to long-term treatment with topical calcineurin inhibitors, such as tacrolimus or pimecrolimus, has demonstrated effectiveness in maintaining remission of the disease and also shown efficacy in treating mild cases. The therapeutic effectiveness was assessed by considering various clinical aspects, including erythema, paleness, skin erosions, and specific symptoms such as itching, burning, and pain.
Results
Erythema emerged as the predominant clinical sign, reported in 43 (78.3%) patients, followed by paleness, reported in 17 (28.3%) patients. Pruritus was observed in 25 girls (58.1% of females) and 2 boys (11.8% of males), while pain and burning sensations were predominantly reported in female children. Among females, we observed a higher prevalence of cutaneous comorbidities, such as atopic dermatitis, psoriasis, alopecia areata, and linear scleroderma, as opposed to autoimmune systemic diseases, that were more prevalent in males. Regarding therapeutic approaches, 21 (35.0%) patients applied topical corticosteroids, 28 (46,7%) applied topical tacrolimus and 21 (35,0%) applied topical pimecrolimus. All treated patients experienced notable benefits following the initiation of treatment proposed by our protocol.
Conclusions
This study provides further insights into the clinical presentation and management of lichen sclerosus in the pediatric population, shedding light on potential therapeutic pathways for optimizing patient outcomes in this specific demographic. The proposed protocol appears to be a promising strategy, especially when the onset of the disease occurs during childhood.
Similar content being viewed by others
Background
Lichen sclerosus (LS) is a chronic progressive inflammatory skin disease [1]. The exact prevalence of LS is unknown, but it seems to range between 0.1 and 3% with a higher predominance in females [2, 3].
LS commonly involves anogenital zones, but extragenital areas may also be affected [1, 4].
LS is characterized by ivory-white or porcelain-white plaques, patches, or spots with an atrophic aspect [2] and is often associated with symptoms such as itching, burning, dyspareunia, soreness, and dysuria, typically following a chronic course with phases of remissions and exacerbations [5]. The pathogenesis of LS remains unknown, although several studies suggest potential involvement of autoimmunity, genetics, hormonal factors, various infections, and local skin irritations [6, 7].
LS onset usually exhibits a bimodal age trend, occurring in pre-pubertal and post-menopausal stages [1]. Among patients with genital LS, 10–20% are children [8].
While high-potency corticosteroids are commonly used as initial treatment for genital LS in adults, effective maintenance therapeutic strategies and long-term safe approaches remain uncertain for both adults and children [9].
This study aims to describe the clinical characteristics and therapeutic approaches in a cohort of pediatric patients with genital LS.
Methods
This data was acquired through a retrospective observational study conducted at the Pediatric Dermatology Regional Center of the University of Padua, Italy. The diagnosis of LS was clinically established by dermatologists with specialized expertise in this pathology, specifically dedicated to managing rare diseases of this nature. The inclusion criteria encompassed children under 18 years of age who were diagnosed clinically or histologically with genital and/or extragenital LS and were referred to our center for care, undergoing our therapeutic protocol, from January 2018 to January 2022. Clinical diagnosis, based on an inclusion protocol, was established, reserving histological diagnosis for doubtful cases or in male children undergoing phimosis surgery. Exclusion criteria included children taking any form of systemic drugs. For each patient, a consistent team of dermatologists, specializing in pediatric dermatology, collected the following data: age, sex, accompanying skin disease, age at onset of LS, clinical characteristics, involved anatomical areas, associated symptoms, and family history of both skin and systemic diseases. Additionally, we documented therapeutic approaches utilized for these patients. The first-line treatment was selected based on severity. For cases with mild pruritus and erythema, treatment involved the use of topical calcineurin inhibitors: once daily for the first month, followed by 2–3 times per week. Patients with skin erosions, hyperkeratosis, and severe itch received topical steroids initially, with a switch to calcineurin inhibitors after 3 months, without overlapping. Given the lack of well-defined pediatric severity scales in the literature, severity assessment was made through clinical observation of characteristic signs and symptoms, considering lesion extent, associated symptoms, and impact on the patient’s quality of life. Remission was described as being free from disease from 3 months after the start of the protocol until the end of the retrospectively analyzed period. Where applicable, the Itch Numeric Rating Scale (Itch NRS) was assessed in children aged 7 years and older, while the Children’s Dermatology Life Quality Index (CDLQI) was evaluated in children aged 4 years and older. All data were recorded and stored using Excel software for Windows 11.
Results
The mean age of our patients was 8.4 ± 3.4 years, and the mean age at onset of LS was 7 ± 2.8 years. Our patient population comprised 43 (71.7%) females and 17 (28.3%) males, with a median age of 9 years. Demographic, clinical features and therapeutic approaches in each patient are summarized in Table 1.
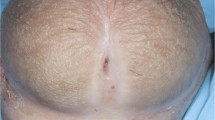
Within our cohort, 48 (80.0%) patients applied moisturizers and emollients and 23 (38.3%) utilized topical vitamin E-based cream. Additionally, 21 (35.0%) patients applied topical corticosteroids, 28 (46.7%) used topical tacrolimus 0.1%, and 21 (35.0%) used topical pimecrolimus 1.0%, all of which yielded favorable clinical results with Itch NRS and CDLQI scores. Notably, we observed a marked improvement in clinical erythema and skin erosions across all patients. No patients required topical steroids due to the inefficacy of the calcineurin inhibitors. Moreover, there were no adverse reactions or instances of flaring observed during the application of our protocol (Fig. 1). Patients maintained therapy with 2 applications per week of topical calcineurin inhibitors, without experiencing flares. Finally, our analysis did not reveal any discernible differences in treatment response based on gender, age, or severity.
Discussion
It is widely acknowledged that LS exhibits a higher incidence in girls than boys [10], with a ratio of approximately 2.5/1 in our study. This gender disproportion might be attributed to a detection bias, as male children are often admitted for LS-related phimosis (14 out of 17 boys of our cohort—82.4% of boys underwent surgery for phimosis), whereas girls may remain asymptomatic initially, later developing typical lesions.
The mean age of our patients and the mean age at LS onset align with existing literature, where typically places the onset of LS in children between 3 and 14 years [11]. In our study, the mean age at LS onset was 7.4 ± 2.9 years in girls and 5.5 ± 2.5 years in boys, compared to a reported mean age of 8.6 years in males in the literature [12].
While previous studies reported a 10–17% ratio of family history in LS patients [10, 11], our findings differ, with only 8.3% of our patients reporting a family history of LS (1 boy—5.9% of males and 4 girls—9.3% of females).
Recent studies suggest that 15–34% of LS cases in adult women and 14% in girls coincide with allergies or autoimmune diseases.
In our population, we observed 1 patient with Hashimoto’s disease and 1 had celiac disease, and 4 (6.7%) had atopic dermatitis. Cutaneous comorbidities, such as atopic dermatitis, psoriasis, alopecia areata, and linear scleroderma, were more prevalent in females, while autoimmune systemic diseases, specifically Hashimoto’s thyroiditis and celiac disease, showed a higher prevalence among males. These findings underline the need for ongoing clinical monitoring in LS patients to assess treatment response, advise on long-term control [12, 13], and detect potential onset of other autoimmune and/or skin diseases.
In our study, erythema was the most common clinical sign (observed in 43 patients—78.3%), followed by paleness (17 patients—28.3%). Phimosis was the predominant clinical sign in boys, while skin erosions and purpura were rare (detected in 2 patients—3.3%). These data are in accordance with data reported in literature [12, 13].
Among females, the perianal region was involved in 18 patients (41.9%), without causing constipation. Small and large genital lips, vulvar vestibule, and clitoris were frequently affected. In males, the inner and outer leaflet of the foreskin, as well as the penis were the most commonly affected areas. LS affected the urethra in 1 male patient, and no extra-genital lesions were detected.
Symptom percentages mirrored literature findings [12], with pruritus observed in 25 girls (58.1% of females) and 2 boys (11.8% of males) while pain and burning sensations were reported only by females. LS commonly affects the anogenital region in girls, whereas boys often experience involvement of the glans, foreskin, and the urethra [14].
According to the guidelines from the “British Association of Dermatologists” (2018) [13], high-potency topical corticosteroids, particularly clobetasol propionate (CP) 0.05% ointment, are recommended as the first-line treatment for LS. The advised regimen is once daily for 3 months. Furthermore, the guidelines suggest that adults should continue using CP 0.05% for ongoing active LS disease, and there is insufficient evidence to recommend topical calcineurin inhibitors for LS patients [13].
In our study population, tacrolimus 0.1% ointment was well-tolerated by all patients, with 28 patients (46.7%) successfully using it once daily. Only 11 patients (18.3%) used mometasone furoate 0.05% cream as a topical steroid, and none required high-potency steroids like CP 0.05% Male children required chronic application of calcineurin inhibitors, but firstly they needed to use topical corticosteroids likely because phimosis typically responds better to this treatment [15]. Female children with LS usually required chronic use of a calcineurin inhibitor to settle inflammation, and less commonly, they needed to use topical corticosteroids.
The primary advantages of topical calcineurin inhibitors in a long-term treatment compared to conventional topical corticosteroids lie in their more selective mechanism of action, without the potential side effects associated with corticosteroids, such as skin atrophy [16, 17]. Given that LS is a chronic disease requiring prolonged treatment and that affected skin areas are often atrophic, a topical drug that induces skin atrophy may not be the optimal therapeutic choice.
Regarding safety, topical calcineurin inhibitors are generally well tolerated in our experience. Although they may be associated with mild-to-moderate and transient application-site reactions, such as pruritus and skin burning, these symptoms typically resolve with continued treatment, as reported in literature [18].
Based on our experience, we propose a flow-chart for the management of LS in pediatric patients, suggesting the use of mild-potency topical corticosteroids (TCS) for acute flares, especially in cases with skin erosions and severe itching, followed by the introduction of topical calcineurin inhibitors for long-term treatment (Fig. 1). In cases presenting with itching (NRS > 6), hyperkeratosis, and erosions, especially when a higher severity was observed, we elected to use topical corticosteroids, given the robust support for their efficacy in the existing literature [12]. Conversely, for milder cases characterized by erythema, paleness, or an Itch NRS score < 6, we adopted topical calcineurin inhibitors (TCI) as the primary treatment, noting beneficial effects.
A potential limitation of our study is the relatively small number of patients; further research is undoubtedly warranted to elucidate the efficacy of our protocol and the use of topical calcineurin inhibitors.
Conclusion
To the best of our knowledge, this represents the first observational study focusing on children with LS under the care of dermatologists specializing in pediatric dermatology. Given the rarity of lichen sclerosus, especially in pediatric age, the clinical results of this study aim to share our experience, contributing to the understanding and management of this rare and challenging skin disease in children. In our clinical practice, we have observed that topical calcineurin inhibitors are employed more frequently than topical steroids, yielding positive clinical signs and symptoms of LS, and proving well-tolerated. Consequently, based on our experience, adopting a therapeutic strategy involving mid-potency topical corticosteroids for managing acute flares, followed by the application of topical calcineurin inhibitors for long-term treatment, appears to be a promising approach for LS patients, especially when the onset of the disease occurs in childhood. Further studies and data are undoubtedly necessary to enhance the robustness of our recommendations. Collecting consistent data in the field of rare skin diseases, particularly in pediatric age, remains challenging but is crucial for advancing our understanding and improving patient care.
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- LS:
-
Lichen sclerosus
- CP:
-
Clobetasol propionate
References
Nair P (2017) Vulvar lichen sclerosus et atrophicus. J Mid-life Health 8:55
Corazza M, Schettini N, Zedde P et al (2021) Vulvar lichen sclerosus from pathophysiology to therapeutic approaches: evidence and prospects. Biomedicines 9:950
Fistarol SK, Itin PH (2013) Diagnosis and treatment of lichen sclerosus: an update. Am J Clin Dermatol 14:27–47
Morrel B, van Eersel R, Burger CW et al (2020) The long-term clinical consequences of juvenile vulvar lichen sclerosus: a systematic review. J Am Acad Dermatol 82:469–477
Kirtschig G, Becker K, Günthert A et al (2015) Evidence-based (S3) guideline on (anogenital) lichen sclerosus. J Eur Acad Dermatol Venereol 29:e1–e43
Kirtschig G. Lichen sclerosus—presentation, diagnosis and management. Deutsches Ärzteblatt international. Epub ahead of print 13 May 2016.https://doi.org/10.3238/arztebl.2016.0337.
Dinh H, Purcell SM, Chung C et al (2016) Pediatric lichen sclerosus: a review of the literature and management recommendations. J Clin Aesthet Dermatol 9:49–54
Winfrey OK, Fei YF, Dendrinos ML et al (2022) Lichen sclerosus throughout childhood and adolescence: not only a premenarchal disease. J Pediatr Adolesc Gynecol 35:624–628
Orszulak D, Dulska A, Niziński K et al (2021) Pediatric vulvar lichen sclerosus—a review of the literature. IJERPH 18:7153
Tran DA, Tan X, Macri CJ et al (2019) Lichen sclerosus: an autoimmunopathogenic and genomic enigma with emerging genetic and immune targets. Int J Biol Sci 15:1429–1439
Akbaş A, Kılınç F (2021) Clinic and demographic characteristics of pediatric patients with lichen sclerosus. TurkJPediatr 63:126
Balakirski G, Grothaus J, Altengarten J, Ott H (2020) Paediatric lichen sclerosus: a systematic review of 4516 cases. Br J Dermatol 182(1):231–233. https://doi.org/10.1111/bjd.18267
Lewis FM, Tatnall FM, Velangi SS et al (2018) British Association of Dermatologists guidelines for the management of lichen sclerosus, 2018. Br J Dermatol 178:839–853
Tong LX, Sun GS, Teng JMC (2015) Pediatric lichen sclerosus: a review of the epidemiology and treatment options. Pediatr Dermatol 32:593–599
Liu J, Yang J, Chen Y et al (2016) Is steroids therapy effective in treating phimosis? A meta-analysis Int Urol Nephrol 48:335–342
Luger T, Paller AS, Irvine AD et al (2021) Topical therapy of atopic dermatitis with a focus on pimecrolimus. Acad Dermatol Venereol 35:1505–1518
Stacey SK, McEleney M (2021) Topical corticosteroids: choice and application. Am Fam Physician 103:337–343
Wollenberg A, Christen-Zäch S, Taieb A et al (2020) ETFAD/EADV Eczema task force 2020 position paper on diagnosis and treatment of atopic dermatitis in adults and children. Acad Dermatol Venereol 34:2717–2744
Acknowledgements
None.
Funding
No funding sources.
Author information
Authors and Affiliations
Contributions
RM, writing—original draft and editing; FC, writing, review, and supervising; and ABF, supervision.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable (retrospective study).
Consent for publication
Specific verbal and written consent to participate was obtained by participants.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Caroppo, F., Mazzetto, R. & Fortina, A.B. Clinical features and therapeutic approaches of genital lichen sclerosus in children: results of an observational monocentric study. Egypt Pediatric Association Gaz 71, 89 (2023). https://doi.org/10.1186/s43054-023-00238-y
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s43054-023-00238-y