Abstract
Background
Wilms’ tumor (WT) affects one in 10,000 children and accounts for 5% of all childhood cancers. Although the overall relapse rate for children with WT has decreased to less than 15 %, the overall survival for patients with recurrent disease remains poor at approximately 50 %. The aim of the study to evaluate the outcome of relapsed Wilms’ tumor pediatric patients treated at the National Cancer Institute (NCI), Egypt, between January 2008 and December 2015.
Results
One hundred thirty (130) patients diagnosed with WT during the study period, thirty (23%) patients had relapsed. The median follow up period was 22.3 months (range 3.6–140 months). The Overall Survival (OS) was 30.9% while the event-free survival (EFS) was 29.8% at a 5-year follow up period. Median time from diagnosis to relapse was 14.4 months. A second complete remission was attained in 18/30 patients (60%). The outcome of the 30 patients; 11 are alive and 19 had died. Three factors in our univariate analysis were prognostically significant for survival after relapse. The first was radiotherapy given after relapse (p = 0.012). The 5-year EFS and OS for the group that received radiotherapy were 41.9% versus 16.7% and 11.1% respectively for those that did not. The second was the state of lymph nodes among patients with local stage III (p = 0.004). Lastly, when risk stratification has been applied retrospectively on our study group, it proved to be statistically significant (p = 0.029).
Conclusion
Among relapsed pediatric WT, radiotherapy improved survival at the time of relapse and local stage III with positive lymph nodes had the worst survival among other stage III patients.
Similar content being viewed by others
Background
Wilms’ tumor affects one in 10,000 children and accounts for 5% of all childhood cancers. More than 80% of children are diagnosed with Wilms’ tumor below the age of five years, and the median age at diagnosis is 3.5 years [1]. The outlook for children with newly diagnosed Wilms’ tumors (WT) has improved dramatically with the advent of multimodal therapy, which includes surgery, chemotherapy, and for some, radiation therapy, with survival rates currently approaching 90 % [2]. Although the overall relapse rate for children with WT has decreased to less than 15 %, the overall survival for patients with recurrent disease remains poor at approximately 50% [3, 4].
Long-term follow-ups are mandatory, as approximately 15% of patients with favorable- histology WT and 50% of patients with anaplastic WT had recurrences. Most recurrences occur within two years of diagnosis, although the recurrences have been known to occur even after 25 years of initial treatment [5]. Before the 1990s, in many relapse WT patients, the same chemotherapy agents were generally used for the treatment of both primary and recurrent disease. The salvage rate for patients with recurrent favorable- histology WT used to be 25–40% [6]. Outcomes started improving up to 60% in the last 15–20 years when modern treatment combinations were tried [7].
Due to the small numbers of relapsed patients, advancements in the treatment of these patients have remained a challenge. Investigators from different cooperative groups have evaluated the role of different therapeutic strategies in an attempt to improve the outcomes of relapse WT. Therapy for these patients depends on the characteristics of their primary disease, the extent of previous therapy, and time from the initial diagnosis to relapse. The general principle of management shifted to include drugs that are not used during primary chemotherapy, using a risk-stratified approach. Patients with relapsed tumors are classified into three groups in the UMBRELLA protocol, group AA, group BB, and group CC, based on initial histology and the first line of treatment used [8].
Our study aimed at estimating the number of relapsed Wilms’ tumor patients between January 2008 and December 2015. Also, to correlate different factors in patients’ demographics, initial disease data, relapse data, post-relapse survival outcome, and defining factors related to the outcome.
Methods
This is a retrospective study on pediatric patients of relapse WT from January 2008 till December 2015. Patients’ medical records were reviewed for different data regarding the initial disease phase and at the relapse phase also for patients’ demographics. The initial disease stage was assigned the Children Oncology Group (COG) clinicopathologic staging of WT. Reference Pathology reports were reviewed for pathological subtype, local tumor stage, resection margins, renal capsule, and lymph node involvement. Information about first-line therapy and the response was collected. Operative details, lymph node dissection, tumor spillage, capsule rupture and/or perioperative complications. Histopathology for documentation of relapse was reviewed. Radiology reports were reviewed for the site of relapse. Post-relapse chemo-radiotherapy and surgery were analyzed in detail.
Initial treatment protocol of the entire study group
Most studied patients were treated initially according to a modified, COG-based protocol (i.e., no LOH of 1p and 16q as a risk factor and without an upfront surgical approach in all cases). Stage I and II FH tumors received 18 weeks EE4A [vincristine (VCR) and dactinomycin (AMD)] without radiotherapy (RTH). Stage III received 24 weeks of DD4A [VCR, AMD, and DOX (doxorubicin)] together with local radiotherapy. Stage IV patients were treated locally with surgery and RTH as either stage I/II or III FH WT. Regimen M (cyclophosphamide and etoposide alternating with vincristine, doxorubicin, and dactinomycin for a total of 33 weeks) with radiotherapy for stage 4 patients with pulmonary metastasis with a slow response after 6w DD4A regimen or extrapulmonary metastatic disease. For the unfavorable histology (UH) group, stage I, II, and III, focal anaplasia, together with stage I diffuse anaplasia, received DD-4A regimen. Stage IV, focal anaplastic were treated with the UH regimen (cyclophosphamide, carboplatin, and etoposide alternating with vincristine, doxorubicin, and cyclophosphamide for 30 weeks) and RT to the metastatic sites. Patients with stages II, III, and IV diffuse anaplastic received regimen UH and RT (Additional file 1).
Risk stratification of relapse WT
Retrospectively, we applied the umbrella protocol risk stratification i.e. groups AA, BB, and CC [8]. Standard Risk: defined as patients with favorable histology WT with relapse after therapy with only vincristine and/or actinomycin D. Those were found. High Risk: defined as patients with favorable histology WT with relapse after therapy with three or more agents (at least including doxorubicin). Very High Risk: defined as patients with recurrent anaplastic—regardless of adoption of primary chemotherapy or primary surgery- or post-chemotherapy blastemal-type WT.
Relapsing Wilms’ tumor regimen treatment protocols
All patients received chemotherapy for their first relapse. The most commonly used regimens were ICE and CCE for six cycles on average. The relapsing protocol has also been used for 2 cases in our study; this regimen consists of alternating two courses of the carboplatin–etoposide and one course of cyclophosphamide every 3 weeks for 25 weeks. Patients were evaluated for response assessment after every two cycles (Additional file 1: Table S1).
Radiotherapy for relapsed patients was given for most of relapsed Wilms’ tumor patients, Radiation delivery mainly using 3D conformal radiotherapy (3DCRT), Treatment modality using photon beam with energy ranging from 6 to 10 MV according to patient’s separation (i.e. thickness) but in most cases 6 MV was sufficient, Children with abdominal recurrence received 1980 cGy, the dose for lung irradiation, using 150 cGy daily fractions, generally reaches 1200 cGy. Patients with non-respectable liver nodules usually received up to 1980 cGy if the entire liver was diffusely involved. Patients who achieved a complete remission following chemotherapy and/or hepatic resection did not receive radiation therapy to the liver.
Statistical analysis
Survival analysis was done using the Kaplan-Meier method and a comparison between two survival curves was done using a log-rank test. All tests were two-tailed. Overall survival (OS) was calculated as the period between the date of the first relapse and the date of death from any cause or the date of the last follow up. Event-free survival (EFS) was calculated as the period between the time of the first relapse and the date of disease progression or second relapse, date of last follow up or date of death. p value of ≤ 0.05 was considered statistically significant.
Results
Among the 130 patients diagnosed with Wilms’ tumor between 2008 and 2015, 39 patients (30%) had relapsed. Nine patients were excluded for incomplete data or due to receiving treatment outside. In the remaining 30, 18 were males (60 %) 12 females (40%). The median age at diagnosis was four years. No congenital anomalies were documented. Tumors located in the right kidney were found in 12 patients (40%) and those in the left kidney were in 16 patients (53%). One patient had bilateral with pulmonary metastasis and another one had an extrarenal (retroperitoneal) WT.
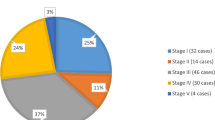
Initial stages I, II, III, and IV was documented in 7(23.3%), 3(10%),12(40%), and 7 cases (23.3%) retrospectively. Only one patient had bilateral WT (3.3%). Initial metastasis was documented in 8/30 patients (26.6%). Lung metastases were found in all metastatic cases and combined liver and lung metastases were only found in 2/8 cases. All stage IV cases had local stage III, which made a total of 19 cases (63.3%). Favorable histology (FH) was documented in 24 patients (80%) and unfavorable histology (UH) in 6 patients (20%). Initial staging and treatment regimen are summarized in (Table 1)
Median time from diagnosis to relapse was 14.4 months; early relapse (less than 12 months) in 43.3 % (n = 13) while 56.7% (n = 17) relapsed after 12 months. Local relapse was found in 11/30 cases (36.3%). Distant relapse was in 10/30 patients (33.3%), all 10 patients had lung relapse and two of which were associated with liver or bone. Combined relapse was in 9/30 patients (30%).
Diagnosis of relapse was mainly based on radiological confirmation of recurrence; however pathological confirmation of relapse was confirmed in 9/30 (30%) patients. Anaplasia was documented in 2 cases only. Blastemal predominance was present in two patients. None of the pathology documented at the time of relapse was similar to the pathology at initial disease presentation except for one patient that had diffuse anaplasia initially and at relapse. The other patient with anaplastic Wilms’ tumor at relapse showed initially favorable histology. Despite the role of molecular genetics at diagnosis and at relapse like tumor-specific loss of heterozygosity (LOH) for chromosomes 1p and 16q but not done as unavailability in our center.
During the first-line treatment: Upfront nephrectomy was performed in 21/30 patients (70%). Intraoperative capsule rupture was documented in 2/30 cases (6.6%), whereas tumor spillage in 1/30 cases (3.3%). Lymph node sampling proved pathological involvement in 5/30 cases (16.7%). Neoadjuvant chemotherapy was given to 9/30 patients (30%); radiotherapy was given to 17/30 patients (56.7%), while anthracycline in 18/30 patients (60%).
After relapse, surgical excision of the relapsed tumor was feasible in 17 patients (56.7%). Radiotherapy was a major part in the treatment of relapsed cases, eighteen (18) patients (60%) had received radiation to sites of relapse. Flank irradiation 1080 cGy was given to six patients with local recurrence and whole abdominal radiotherapy 1980 cGy was given to six patients with a boost to para-aortic lymph nodes in two patients. Five patients received lung irradiation 1200 cGy. Two patients with non-respectable liver nodules received up to 1980 cGy and one patient received radiotherapy 3060 cGy to metastatic D12–L1 vertebrae.
All patients received chemotherapy for their first relapse. The most commonly used regimens were ICE and CCE for six cycles on average. The relapsing protocol has also been used for 2 cases in our study; this regimen consists of alternating two courses of the carboplatin–etoposide and one course of cyclophosphamide every 3 weeks for 25 weeks. Patients were evaluated for response assessment after every two cycles.
A second complete remission (CR) was attained in 18 patients (60%) and partial remission (PR) in 3 patients (10%). One patient (3.3%) showed a stationary response (SD) and 7 patients (23.3%) had progressive disease (PD). Out of the 18 patients that achieved a second CR, 8 continued to follow up in CR, while 8 had a second relapse, one patient lost follow-up, and one patient died on treatment. In the patients with the second relapse, only 3 received a third treatment line. One is alive under therapy while the remaining had died. The final outcome of the 30 patients: 11 are alive and 19 dead (Table 2).
Several adverse prognostic factors were recorded in our study; unfavorable histology at diagnosis, initial local stage III, recurrence < 12 months, abdominal and lung relapse, previous anthracycline therapy, and time from nephrectomy < 12 months. The patients having just one bad prognostic factor were 23.3% (n = 7), similarly were the patients having 2 or 3 adverse prognostic factors 23.3% each. Those with more than 3 formed collectively 26.7% (n = 8). One patient had none of the previously mentioned bad prognostic factors.
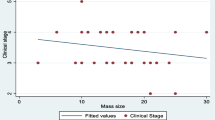
The median follow up period was 22.3 months (ranged from 3.6 to 140.7 months). The 5-year (OS) was 30.9% while the 5-year (EFS) was 29.8% (Fig. 1). Median time from diagnosis to relapse was 14.4 months. The 5 year OS for relapse < 12 months from diagnosis was 44.8% while that for relapses > 12 months was 18.4% and that was not statistically significant (p value = 0.478). Favorable histology had better survival rates than those with unfavorable histology but it was also statistically insignificant. The local stage did affect OS but was not statistically significant. The 5 year OS for stages I, II, and III was 47.6%, 25%, and 24.2% respectively.
The prognostically significant factors for survival were radiotherapy given after relapse with The 5 year OS for the group that received radiotherapy was 41.9% versus 11.1% for those who did not (p value = 0.012) (Fig. 2). The state of lymph nodes in locally stage III was statistically significant, the 5 year EFS for patients with initially negative lymph nodes was 35%, while those with positive lymph nodes (n = 15) all died before the end of the first year of follow up, p value (0.004) (Fig. 3). Risk stratification has been applied retrospectively in our study group. Standard risk (SR) Group AA, High risk (HR) BB, and Very high risk (VHR) CC formed 33.3%, 46.7%, and 20% of patients respectively. On the correlating risk category with survival, it proved statistically significant (p = 0.029).
The 5 year OS for local relapse was 12.5% while that of distant relapse was 40.0%, combined relapse came with the best survival at 44.4%. The affection of survival by the number of adverse prognostic factors was not statistically significant (Table 3).
Discussion
WT is the most common renal tumor of infancy and childhood. Its incidence is one per 10,000 children under the age of 15 years worldwide [1]. Multimodality treatment has resulted in a significant improvement in the 4-year survival, from approximately 30% in the 1930s to more than 85% in the modern era. The overall prognosis in WT remains poor in developing countries [9]. Acquiring information about the cure rate after treatment of relapsed WT is difficult because numbers of patients are small due to the high cure rate after primary treatment. Moreover, interpretation of the published studies is complicated by differences in initial therapy and patient selection [10].
In our study, the relapse rate was high accounting for 30%. The relapse rate reported by other Egyptian studies varied between 17.9% and 24.2% [11].These are all higher than those demonstrated by the 4th NWTS and the 9th SIOP which were 11% and 10% respectively [12]. The median age at initial diagnosis was four years. This was comparable to the study of all relapses in patients registered in the German SIOP/GPOH trials where the median age was 4.5 years [13].
In our study, stage III tumors were the most common (40%), followed by stages I and IV (23.3%) each. Then came stage II (10%) and lastly stage V (3.3%). The stage distribution came slightly different to that in a Swedish study on 13 relapsed cases where stage I formed 38% of cases (n = 5), stage II 15% (n = 2), stage III 23% (n = 3), stage IV 8% (n = 1) and stage V 15% (n = 2) [14].
In our study, the 5-year post-relapse survival was 30.9% this was approximate to another study in the University of Iowa on 21 patients, where it was reported to be 33% [15]. Likewise, the United Kingdom Children’s Cancer Study Group analyzed 71 children with a 24% post-relapse survival at a median follow-up of 3 years [10]. At the St. Jude Children’s Research Hospital, Williams and colleagues reported a 25% post-relapse survival in 32 patients with a median follow-up of 6.5 years [15]. However, our results were less than those reported by the Koreans where a study conducted in Seoul national university children’s hospital calculated survival to be 40.9% [16]. The outcome of relapses of nephroblastoma in patients registered in the SIOP/GPOH trials and studies, the overall survival after relapse was 48% (median follow-up 5 years) [13].
Radiotherapy given after relapse was a prognostically significant factor for survival (p value 0.012). The 5 year EFS and OS for the group that received radiotherapy were 41.9% versus 16.7% and 11.1% respectively for those that didn’t (Table 2). A total of 18 patients have received radiotherapy and 9 are alive from which 7 in second CR. There is limited information available on the role of RTH in the management of relapse WT. In the NWTS report, 30 patients developed solitary pulmonary relapse and they underwent bilateral lung irradiation, and chemotherapy with or without surgical resection; the 4-year post-relapse survivals were 76% and 77%, respectively. Whereas 55 patients had multiple pulmonary nodules at relapse, their 4-year survival after whole-lung RTH and chemotherapy was 44% [17]. NWTS-5 protocol recommends surgical resection of persistent pulmonary nodules after induction chemotherapy, patients with pulmonary relapse who achieve a complete remission after surgical resection receive whole-lung RTH if there is no history of prior pulmonary irradiation [18].
In our study, univariate analysis of proposed risk factors indicated that EFS and OS were significantly associated with individual stage III criteria among patients with local stage III. Of prognostic relevance in this subgroup was the initial state of lymph nodes with a p value 0.004. The patients with initially negative lymph nodes had a 5 year EFS of 35%, while those with positive lymph nodes (n = 15) all have died before the end of the first year of follow up. This was comparable to another study where each criterion designating stage III was assessed in terms of affecting survival. The EFS and OS were better for patients with negative lymph nodes. The multivariate analysis showed the joined effect of lymph nodes involvement and microscopic residual disease was most predictive of outcome [19]. In another retrospective study of 95 cases over 20 years, 28 cases had a relapse; on multivariate analysis, lymph nodes positivity and anaplasia were independently correlated with disease-specific survival [20].
Reinhard et al. provided an analysis of prognostic factors for post-relapse survival [13]. In their study of 170 relapses of all 1392 children registered in SIOP/GPOH trials from the year 1989 till 2003; it was found that lower disease stage at diagnosis had a better outcome. Stage I and II had a better outcome than stage III (p = 0.008). They also found that early relapse within 6 months from diagnosis was a strong predictor of poor survival after relapse (p = 0.0001). Furthermore, patients with isolated distant metastasis had a significantly better outcome (OS = 59%) than those with isolated local (OS = 50%) and combined relapses (OS = 12%) (p = 0.001). Finally, high-risk histology was one of the adverse prognostic factors for poor post-relapse outcomes [13]. A number of factors were analyzed in our study in relevance to post-relapse survival. Not all factors were of prognostic relevance; however, the small number of our study’s cohort requires further analysis of the proposed factors.
Risk stratification based on umbrella protocol [8] has been applied retrospectively in our study group. Group AA formed 33.3% of patients, Group BB 46.7%, and Group CC formed 20% of cases. On the correlating risk category with survival, it proved statistically significant (p = 0.029).
Before the mid-1980s, the OS for relapse WT was 30%. During this era, salvage therapy consisted of vincristine, dactinomycin, doxorubicin, radiation therapy, or surgery. In recent years (Table 4), cyclophosphamide, ifosfamide, cisplatin, carboplatin, and etoposide were shown to be active against relapse WT and multiagent regimens containing these drugs, mostly ICE (ifosfamide, carboplatin, and etoposide) have significantly improved post-relapse survival rates to the 50-60% range [21]. However, the role of high-dose chemotherapy and stem cell rescue (ASCR) in patients with high-risk recurrent WT is not fully defined [24]. A study performed at the Memorial Children hospital in Chicago proved a good outcome after treatment of relapsed Wilms’ tumor with high-dose chemotherapy (HDT) followed by ASCR. Seven of 13 patients are alive in CR with a median follow-up of 30 months [22]. In our study, there was no uniform approach for chemotherapy post relapse. 40% of patients received ICE as second-line therapy for relapse while 36.7% received CCE. CR was reached in 66% of patients that received ICE while 36.3 % achieved CR in the patients that received CCE.
Our study had limitations, considering the small number of the study group as well as the absence of the risk-oriented approach for the treatment of relapse from the start.
Conclusions
Radiotherapy post-relapse played a major role in improving the outcome of relapse. The state of lymph node positivity should be taken into consideration when treating relapsed local stage III cases as they proved to have a worse outcome than other relapsed stage III patients. Risk tailored therapy is recommended for a standardized therapeutic approach at our institution that is stratified according to individualized risk factors.
Availability of data and materials
The datasets used and analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- COG:
-
Children Oncology Group
- CR:
-
complete remission
- FH:
-
favorable histology
- HDC:
-
high-dose chemotherapy
- LOH:
-
loss of heterozygosity
- NWTS:
-
National Wilms Tumor Study Group
- PD:
-
progressive disease
- RTH:
-
radiotherapy
- SIOP:
-
International Society of Pediatric Oncology
- WT:
-
Wilms’ tumor
References
Szychot E, Apps J, Pritchard-Jones K, et al. Wilms’ tumor: biology, diagnosis and treatment. Transl Pediatr. 2014.
D’Angio GJ, Evans A, Breslow N, Beckwith B, Bishop H, Farewell V, Goodwin W, Leape L, Palmer N, Sinks L, Sutow W, Tefft M, Wolff J. The treatment of Wilms’ tumor: results of the second national Wilms’ tumor study. Cancer. 1981.
Grundy P, Breslow N, Green DM, Sharples K, Evans A, D’Angio GJ. Prognostic factors for children with recurrent Wilms’ tumor: results from the second and third national Wilms’ tumor study. J Clin Oncol. 1989.
Pinkerton CR, Groot-Loonen JJ, Morris-Jones PH, Pritchard J. Response rates in relapsed wilms’ tumor. A need for new effective agents. Cancer. 1991.
Sarin YK, Graf N. Management of recurrent Wilms’ tumor. J Int Med Sci Acad. 2014.
Dome JS, Liu T, Krasin M, Lott L, Shearer P, Daw NC, Billups CA, Wilimas JA. Improved survival for patients with recurrent Wilms tumor: the experience at St. Jude Children’s Research Hospital. J Pediatr Hematol Oncol. 2002.
Kalapurakal JA, Dome JS, Perlman EJ, Malogolowkin M, Haase GM, Grundy P, Coppes MJ. Management of Wilms’ tumour: current practice and future goals. Lancet Oncol. 2004.
Van Den Heuvel-Eibrink MM, Hol JA, Pritchard-Jones K, Van Tinteren H, Furtwängler R, Verschuur AC, Vujanic GM, Leuschner I, Brok J, Rübe C, Smets AM, Janssens GO, Godzinski J, Ramírez-Villar GL, De Camargo B, Segers H, Collini P, Gessler M, Bergeron C, Spreafico F, Graf N. Position paper: rationale for the treatment of Wilms tumour in the UMBRELLA SIOP-RTSG 2016 protocol. Nat Rev Urol. 2017;14:743–52.
Parimkayala D, Md R, Sinha S. Outcome of Wilm’s tumour in a tertiary care centre: Our experience. IOSR J Dent Med Sci. 2017;16:2279–861 Available from: www.iosrjournals.org.
Groot-Loonen JJ, Pinkerton CR, Morris-Jones PH, Pritchard J. How curable is relapsed Wilm’s tumour? Arch Dis Child. 1990.
Abd E-AHH, Habib EE, Mishrif MM. Wilms’ tumor: the experience of the pediatric unit of Kasr El-Aini center of radiation oncology and nuclear medicine (NEMROCK). J Egypt Natl Canc Inst. 2005;17:308–14.
Tournade MF, Com-Nougué C, De Kraker J, Ludwig R, Rey A, Burgers JMB, Sandstedt B, Godzinski J, Carli M, Potter R, Zucker JM. Optimal duration of preoperative therapy in unilateral and nonmetastatic Wilms’ tumor in children older than 6 months: results of the Ninth International Society of Pediatric Oncology Wilms’ Tumor Trial and Study. J Clin Oncol. 2001.
Reinhard H. Outcome of relapses of nephroblastoma in patients registered in the SIOP/GPOH trials and studies. Oncol Rep. 2008;31:4163–8.
Kullendorff CM. Relapses in Wilms tumour. Pediatr Surg Int. 2003;19:635–8.
Wilimas JA, Douglass EC, Hammond E. Relapsed Wilms’ tumor. Factors affecting survival and cure. Am J Clin Oncol Cancer Clin Trials. 1985.
Park ES, Kang HJ, Shin HY, Ahn HS. Improved survival in patients with recurrent Wilms tumor: the experience of the Seoul National University Children’s Hospital. J Korean Med Sci. 2006.
Macklis RM, Oltikar A, Sallan SE. Wilms’ tumor patients with pulmonary metastases. Int J Radiat Oncol Biol Phys. 1991.
Paulino AC. Relapsed Wilms tumor: is there a role for radiation therapy? Am J Clin Oncol Cancer Clin Trials. 2001.
Ehrlich PF, Anderson JR, Ritchey ML, Dome JS, Green DM, Grundy PE, Perlman EJ, Kalapurakal JA, Breslow NE, Shamberger RC. Clinicopathologic findings predictive of relapse in children with stage III favorable-histology wilms tumor. J Clin Oncol. 2013.
Honeyman JN, Rich BS, McEvoy MP, Knowles MA, Heller G, Riachy E, Kobos R, Shukla N, Wolden SL, Steinherz PG, La Quaglia MP. Factors associated with relapse and survival in Wilms tumor: a multivariate analysis. J Pediatric Surg. 2012.
Abu-Ghosh AM, Krailo MD, Goldman SC, Slack RS, Davenport V, Morris E, Laver JH, Reaman GH, Cairo MS. Ifosfamide, carboplatin and etoposide in children with poor-risk relapsed Wilm’s tumor: a Children’s Cancer Group report. Ann Oncol. 2002.
Campbell AD, Cohn SL, Reynolds M, Seshadri R, Morgan E, Geissler G, Rademaker A, Marymount M, Kalapurakal J, Haut PR, Duerst R, Kletzel M. Treatment of relapsed Wilms’ tumor with high-dose therapy and autologous hematopoietic stem-cell rescue: the experience at children’s memorial hospital. J Clin Oncol. 2004.
Malogolowkin M, Cotton CA, Green DM, et al. Treatment of Wilms tumor relapsing after initial treatment with vincristine, actinomycin D, and doxorubicin. A report from the National Wilms Tumor Study Group. Ped Blood Cancer. 2008;50:236–41.
Spreafico F, Jones KP, Malogolowkin MH, Bergeron C, Hale J, De Kraker J, Dallorso S, Acha T, De Camargo B, Dome JS, Graf N. Treatment of relapsed Wilms tumors: lessons learned. Expert Rev Anticancer Ther. 2009;9:1807–15.
Hale J, Hobson R, Moroz V, Sartori P. Results of UK Children’s Cancer and Leukemia Group (CCLG) protocol for relapsed Wilms tumor (UKWR): united relapse strategy improves outcome. Proc Meet Int Soc Paediatr Oncol. 2008;62 (Abstract O154).
Acknowledgements
Not applicable.
Funding
There was no funding for this study by any means.
Author information
Authors and Affiliations
Contributions
Study concept: WZ. Study design: WZ, DM. Data acquisition: DM, AI. Data analysis and interpretation: DM, WZ, AI. Manuscript preparation: DM, WZ. Manuscript editing: WZ, DM, YM. Manuscript review: WZ, YM. All authors have read and approved the manuscript
Authors’ information
Not applicable.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The Institutional Review Board (IRB) at the National Cancer Institute, Cairo University, has approved the waiver of patient consent form because of the retrospective nature of the study which used archived data and did not affect patient well-being in any way. The reference number is not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Additional file 1: Table S1.
Relapsing Wilms Tumor Regimens Treatment Protocols.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Zekri, W., Yacoub, D.M., Ibrahim, A. et al. Relapsed Wilms’ tumor in pediatric patients: challenges in low- to middle-income countries—a single-center experience. J Egypt Natl Canc Inst 32, 21 (2020). https://doi.org/10.1186/s43046-020-00032-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s43046-020-00032-6