Abstract
Background
A usual source of care (USC) has been conceptualized as having a health provider or place available for patients to consult when sick or in need of medical care. Having a USC is a means to achieve longitudinality of care with Primary Health Care (PHC) providers. Brazil has made enormous progress in PHC and thus provides an important opportunity to investigate USC in a middle-income country context.
Methods
This study uses data from a nationally representative household survey, the 2013 National Health Survey (n = 62,986), to describe the prevalence of having a USC in Brazil and to investigate to what extent the Family Health Strategy (FHS) has contributed to USC prevalence. Analyses include descriptive, bivariate and multivariable Poisson regression.
Results
Show very high rates of people reporting any type of USC (74.4 %) and more than one third reporting PHC as their USC. Household enrolment in the FHS was positively associated with having any USC (PR:1.09; 95 % CI: 1.07–1.12) and a stronger association with having PHC as the regular source of care (PR:1.63;95 % CI:1.54–1.73). FHS enrolment was negatively associated with reporting emergency/urgent care facilities as one’s USC (PR: 0.67; 95 % CI: 0.59–0.76). The association between the more consolidated FHS with having a USC was strongest in the poorest regions of the country (North, Northeast and Central-West). Having PHC as one’s USC showed a positive dose-response relationship with the FHS in all regions, especially in the Central-West.
Conclusions
Our results have important implications for the health care model in Brazil and in other countries, especially those seeking to base their national health systems more strongly on primary health care. The study suggests expanding primary health care can increase the establishment of a USC which can help assure better monitoring of chronic conditions and attention to patient needs.
Similar content being viewed by others
Background
A usual source of care (USC) has been conceptualized as having a specific health provider or place for patients to consult when sick or in need of medical care [1]. It is directly related with longitudinality, one of the core dimensions of primary health care [2], defined by patient follow-up over time by a general practitioner or PHC staff, characterizing an implicit therapeutic relationship based on professional responsibility and mutual confidence [3]. Furthermore, it has been shown to have beneficial effects on health care utilization and outcomes, and reduces unnecessary referrals to specialists [4–6].
Barbara Starfield argues that having a USC requires longitudinality of care with a PHC provider [6–9], despite other services that may substitute for a USC, such as specialist physicians or the emergency room. Lack of adequate access to PHC and/or acute exacerbation of a chronic condition may be explanations for reporting emergency services as a USC for some populations. Many studies have reported the increase in emergency services, even in high-level income countries [10–12]. A recent exploratory study in England shows that more than 25 % of non-planned accident and emergence services consultations are related to difficulties in obtaining a general practice appointment [13]. Furthermore, the use of emergency services as a USC is less likely to resolve the patient’s overall health needs and may lead to overcrowded emergency services, increased risk of nocosomial infections, and unnecessary expenses for the individual and the health system [14, 15].
Brazil provides an important location to investigate USC as a middle-income country that has made enormous progress in PHC and in overcoming inequities in the last decade, but remains with major inequalities between regions, communities and population groups [16–19]. Since the 1990s, Brazil’s health system has been aiming to achieve universality and comprehensiveness of care. One of the most important changes was the implementation of the Family Health Strategy (FHS) in 1994 with a large expansion from 2000, reaching almost 60 % coverage of the Brazilian population by 2013 [20]. It is now considered the world’s largest community-based PHC program. The beneficial impact of FHS is evidenced by positive evaluations by users, managers and health care professionals [6, 15, 21], improved availability, access to and use of health services [22] and improved health indicators, such as reduced infant mortality, avoidable hospitalization and heart and cerebrovascular disease mortality [23–27]. Despite these positive results, national inequalities and different models and/or insufficient FHS implementation remain [19, 28, 29].
The 2013 Brazilian National Health Household Survey collected indicators of utilization of health service from the user’s point of view, as well as individual data on FHS enrollment providing an opportunity to: describe the prevalence of reporting any type of USC in Brazil; examine prevalence and correlates of the different types of healthcare services reported as USCs; and investigate to what extent the FHS has contributed to the presence and type of USC reported and consequently to what extent FHS reduced inequities in access to health care.
Methods
The Brazilian National Health Survey (Pesquisa Nacional de Saúde-PNS) is nationally-representative household survey developed by the Brazilian Institute of Geography and Statistics (IBGE) and Ministry of Health and conducted in 2013. Main objectives of PNS are: to describe the health situation and lifestyles of the Brazilian population, access and use of health services, and evaluation of the health care and prevention measures provided by the National Public Health System (Sistema Único de Saúde-SUS) [30]. The survey employs a complex sampling design. The primary sampling units are census tracts based on the 2010 census and randomly selected from the IBGE national master sampling plan. Within each census tract households were randomly selected from a national registry of addresses. Within selected households a randomly selected respondent aged 18 or over was invited to take part in the study. In order to account for losses the estimated sample size was of around 80,000 households based on a predicted non-response rate of 20 %. At the end of fieldwork, a total number of 81,167 households were visited, of which 69,994 were occupied, with 64,348 household interviews and 62,986 individual interviews with a selected household resident being conducted representing an overall response rate of 78 % [31]. Face to face interviews were conducted with properly trained interviewers and the assistance of handheld computers. No incentives were provided. Person-level survey weights take into account the probability of selection as well as non-response rates. Further detail of sample size calculations and weighting procedures can be found in Souza Jr et al, 2013 [32]. There are no missing data in the PNS as IBGE impute data for missing information. The PNS project was approved by the National Commission of Ethics in Research (CONEP) in June 2013, Regulation No. 328.159. The PNS data are publicly available on the IBGE and Fiocruz websites. The data do not have identification of the participant and the lowest level of available geographical breakdown is capital, metropolitan belt, rest of the state, which are too large to identify a participant.
The PNS data include general information on all residents of the household (given by one of the household residents who could inform about the socioeconomic situation and health of all of its residents) and from a randomly selected resident aged 18 or over. Further details about the PNS development have been reported in [31] and [32].
USC and its types were defined from two questions: “Do you usually go to the same place, the same doctor or health service when you need health care (yes or no) and “When you are sick or need health care where do you usually go”. Then, we constructed 6 outcomes: 1- Any USC- coded “no” for those who said no to the first question or go to pharmacies (no USC) and “yes” for those who go to public or private health centers, public or private home care, public or private hospitals and emergency care. 2- No USC (the opposite of having a USC); 3- Only PHC Provider-coded “no” if no USC or all sources except PHC and “yes” for PHC or home care provided by PHC; 4-Only Private Provider- coded “no” if no USC and all sources except private providers or “yes” for those who goes to outpatient private health centers or private home care; 5-Not an emergency care-coded “no” if no USC and other emergency room/urgent care or “yes” for all sources except emergency room/urgent care; 6-Only Emergency room/urgent care facility- coded “no” if no USC or all sources except emergency room/urgent and “yes” for all sources of emergency room/urgent care). The main “exposure” is whether the respondent’s household is registered as enrolled in the FHS. Of the total Brazilian population covered by the FHS (54 %), 86.6 % were registered over 1 year and 70 % had regular visits by community health workers (CHW) in the last year. In the construction of the FHS enrolment we consider 1- not enrolled; 2- incipient (those who were enrolled for less than 1 year or did not have regular visits by CHW in the last year) and 3-consolidated (those enrolled for 1 year or more and with regular visits by CHW in the last year). The adopted definition sought to address not only the time of implementation of the FHS, but a “proxy” (regular CHW visits) for systematic monitoring by the FHS team to the survey participant’s family. Other covariates (potential confounders) were used to adjust expected differences in prevalence rates of reporting a USC compared to not reporting a USC. And included: type of health care coverage- a combination of FHS and private insurance enrollment with four categories (1-none; 2- FHS enrolment only; 3- FHS enrolment and private insurance and 4- private insurance only; age; sex; self-reported skin color according to the official Brazilian census categories (white, black, pardo-someone from a mixture of skin color, that is, a person generated from some miscegenation- Asian, native Brazilian/Indigenous); educational attainment (none, less than high school completed, high school completed, more than high school); geographical area of residence (rural versus urban); state capital residence (versus elsewhere); country region (North, Northeast, South, Southeast, Central- West); self reported health status (excellent/very good/good versus fair/poor); self report of a chronic disease; and comorbidity (reporting of two or more chronic). We present descriptive statistics and bivariate analyses of USC and its different types by study covariates with Pearson chi square tests and respective p values to test for independency. We then present results of multivariable Poisson regression models for each USC outcome as the prevalence is over 10 % and adjusted prevalence ratios and 95 % confidence intervals (CI) for the association of enrollment in the FHS and USC and were estimated. Country region was used as “proxy” to the measurement of inequality in evaluating the association of FHS enrollment with USC. Historically, Brazil has marked geographical/regional inequalities such as social economical development, income distribution and distribution of public resources such as transportation, sanitation, health and educational services. Several studies demonstrate secular differences that divide the country into poorer (North and Northeast) and richer regions (South and Southeast) [19, 33, 34]. All analyses were performed using Stata version 12.1 and results incorporate appropriate weights and control for the complex sample design.
Results
Descriptive and bivariate statistics for the sample are shown in Table 1. Slightly more than half of our sample was female, approximately one-fifth was 25–34 years of age and 12.3 % was 65 and older. About half of respondents self-classified as white and 41.9 % as pardo. Up to 50 % completed primary school. Most (86.2 %) resided in urban areas, a quarter lived in one of the 26 state capitals or federal district and 43.8 % were from the Southeast Region. The majority (74.4 %) of the sample reported having any type of USC but differed according to demographics. Compared to those without a USC, having a USC predominated among women, the elderly (≥65 years), those who self-identify as white, among extremes of educational attainment (less than primary school or completed college), more likely to reside in urban areas, other cities than the capital and in the South and Southeast Regions. Regarding types of USC separately: 61.9 % reported a source other than emergency/urgent care services, 35.5 % only PHC, 17.5 % only private physician and 12.6 % only emergency care. Having PHC as an USC was slightly higher among women; among those 44 and older; those self-classified as pardo or indigenous; those with none or educational less than primary school; rural residence; cities other than the capital and in the South Region. Other types of USC and demographics are in Table 1.
Table 2 presents descriptive and bivariate statistics for the respondents’ reported health variables. Most reported good self-rated health, slightly more than one third reported a chronic disease, few reported comorbidities (12.7 %), approximately one-fourth reported enrollment in private insurance, more than half reported enrollment in the FHS (20.4 % incipient and 34.2 % consolidated FHS coverage). Regarding type of health care, the majority of respondents were enrolled in the FHS by itself. Compared to those without a USC, having a USC was more common among those with chronic conditions, with comorbidities, enrolled in private insurance, enrolled in the FHS (even higher with consolidated FHS coverage), and among those with FHS by itself or in combination with private insurance. Having PHC as one’s USC was higher among those reporting poor health, chronic disease, comorbidity, not enrolled in private insurance, and enrolled in the FHS.
Tables 1 and 2 shows similar comparisons but in the opposite direction for those who did not report a USC as this variable is the complement of having a USC.
Table 3 presents results of the multivariable Poisson regression models for any USC and each USC type. Levels of FHS consolidation showed an overall positive association with having any USC, but of a small magnitude. FHS was more strongly associated with having PHC as one’s USC with a dose response relationship: consolidated FHS had a higher likelihood of having PHC as one’s USC, less so for incipient FHS coverage. Levels of FHS consolidation showed a negative association with having a private physician as one’s USC. Levels of FHS consolidation showed a positive dose-response association with having any service except emergency/urgent care service as one’s USC. And levels of FHS consolidation showed a negative association with reporting emergency/urgent care services as one’s USC with a strong dose response relationship.
Table 3 also shows results of the multivariable Poisson regression models for any USC and each USC type by region. The association between levels of FHS consolidation and having a USC was positive and stronger in the poorest regions of the country (the North, Northeast and Central West). Having PHC as one’s USC showed a positive dose response relationship in all Regions especially in the Central-West. Having a private physician as one’s USC was negatively associated with levels of FHS consolidation and was stronger in the South Region. Reporting any service except emergency/urgent care as one’s USC was positively associated with levels of FHS consolidation and stronger in the Central West region. In addition, having emergency/urgent care services as one’s USC was negatively associated (in a dose response manner) in the Southeast but did not reach levels of statistical significance in the other regions.
Discussion
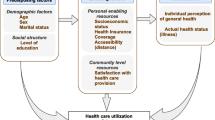
This study reports very high rates of having a USC - only one quarter of the Brazilian population did not report a USC. Most Brazilians do not rely on emergency/urgent care services as their USC. More than one third report PHC as their USC and a small proportion report their USC as private physicians or emergency/urgent care facilities. It is well documented that health services utilization depends on individual needs determined by demographic and social characteristics in addition to health status [35], and on the accessibility, acceptability, and appropriateness of health services as determined by the health system’s means of healthcare organization, financing, and delivery.
Despite FHS consolidation as the main PHC organization model in Brazil, its implementation is heterogeneous and could explain why only one third reported PHC as their usual source of care. Qualitative and quantitative studies have demonstrated differences in FHS performance between states, municipalities and even within a single municipality geographical area [36, 37]. This heterogeneity reflects geographical inequalities and differences in the implementation across the country. Another possible explanation is that the implementation of the universal public health system in Brazil is relatively recent compared to other developed countries. And weaknesses in primary health care remains as an important challenge for managers and researchers [21].
In Brazil, the national public health system (the SUS)--especially the consolidation of primary health care through the FHS--has been associated with beneficial effects on equity of access to healthcare [19] and has been shown to provide a strong link between users and FHS health care teams. This link has been carefully constructed through a process of territorialization and other mechanisms such as the presence of CHW in the teams to strengthen links between the population and the health system. Territorialization means each multi-professional health team (composed of a physician, a nurse, a nurse assistant and 4–6 CHWs) is assigned a specific territory and has a list of which families it serves. Teams are organized by local geographic areas to provide primary care to about 1000 families (or approximately 3500 people). Furthermore, one of the CHW tasks is to visit the households in the catchment area regularly especially in homes where there is someone with a chronic condition, a woman who recently gave birth, or a young child.
Having PHC as one’s USC was more pronounced in sub-groups of the population such as women and those 44 and older, as expected, but also among those who often face barriers (inequities) to health care including pardos and indigenous people, those with lower levels of educational attainment, those residing in rural areas and those residing in non-capital cities. Most likely, this is the result of FHS consolidation in certain areas. As one would also expect, having any type of USC was more frequent among those with higher health needs, those enrolled in private insurance or those enrolled in the FHS. However, having PHC as one’s USC was more frequent among those not enrolled in private insurance, and among those with higher health needs and those enrolled in the FHS.
The consolidation of the FHS was associated with having PHC as a USC and the more consolidated the FHS the higher the rate of reporting PHC as one’s USC in comparison to those not enrolled in the FHS and after controlling for a set of potential confounders. This result is consistent with a previous study showing that families enrolled in the FHS were more likely to have a usual source of medical care [35]. This previous study conduct in 2008 based on National Household Survey found that adults living in households enrolled in FHS were more likely engaged with a usual source of care as compared to those in families with neither FHS enrollment nor private health plans.
The observed trend was present in all five Brazilian regions. However, it was more pronounced in the Northeast, one of the poorest Regions of the country and in the Central West. In Brazil, inequalities among the population are still very much present and Viacava (2010) analyzing data from 10 years on access and use of health services indicates that access increased significantly in Brazil mainly for those living in the poorest regions of the country [38].
Emergency/urgent care services in most cases do not provide either informational or clinical continuity of care. Patients may seek this type of service due to acute episodes of chronic conditions and/or because of fewer perceived barriers to accessing higher level medical technologies [39]. This study has shown that FHS consolidation was negatively associated with reporting emergency/urgent care services as one’s USC. Further, the more consolidated the FHS coverage, the lower the rate of reporting emergency/urgent care services as one’s USC, even after controlling for a set of potential confounders. This trend was most pronounced in the Southeast and South (the richest regions of the country) and in the Central-West.
It is well known that a positive patient/provider relationship is essential for successful treatment. This applies to improving patient adherence to treatment plans for chronic conditions as well as dealing with stigmatized health problems such as mental health or tuberculosis, all of which require trust as a fundamental ingredient in the therapeutic process. However, trust between patients and health providers needs time to develop. A study conducted in the United Kingdom demonstrates that the length of time of a patient/physician relationship was significantly and independently associated with trust [9]. In our study, consolidated FHS (household enrolled 1 year or more with 2 or more visits from a community health worker in the past year) was associated with having PHC as one’s USC and reporting less use of emergency services as a USC. This finding emphasizes not only the importance of PHC vis-a-vis FHS in Brazil but the consolidation of the Program throughout the country.
Limitations of the study include: 1- the definition of the outcome variable – USC – refers to a provider or place a patient consult when sick or in need of medical advice and is considered one of the hallmarks of primary health care [5]. Furthermore, USC is used in many self-reported surveys and is operationalized through questions such as “Is there one particular place that you go if you are sick or need advice about your health?” and “Is there a regular doctor you usually see at this place?” [8, 9]. In our study USC was defined as in health services studies. While it is true that “see the same doctor” and “go to same place” have different implications regarding longitudinality and continuity of care, Mainous et al., for example, find that trust in one’s physician has more beneficial consequences in effectiveness of medical care than seeing the same provider [7]. In our study, it was impossible to differentiate between having same doctor or the same place since the questionnaire did not make this distinction. However, in Brazil, different from other countries most primary care is provided by only one physician (in the Family Health Strategy, teams are composed by one physician, one nurse and 6 community health agents). There are also PHC teams composed by more than one physician, especially in big cities, related to other types of PHC organization besides FHS. But the consolidation of PHC in Brazil is mainly due for the implementation of FHS. Therefore, the limitation of the questionnaire most likely does not strongly affect longitudinality as a criterion for USC. 2- Results are based on self-report and may represent overestimates of true values of individual reports of a usual source of care. Nevertheless, evidence has shown high levels of USC in other studies and we provide estimates of different types of USC here to provide more valid information in the country as a whole and in different regions. 3- Because the data are cross-sectional we are unable to determine causal relationships of the observed associations between level of FHS enrollment and USC. Nevertheless the observed associations were consistent and in the same positive direction as in other regions of the country.
Conclusions
The results of this study have important implications for the health care model in Brazil and in other countries, especially those seeking to base their national health systems more strongly on primary health care. The study suggests that expanding and consolidating primary health care can increase access to a USC with PHC providers, as emphasized by Starfield [6] and others, assuring patients better follow-up, monitoring of chronic conditions, and attending to patient overall health needs.
Abbreviations
- CHW:
-
community health workers
- CONEP:
-
National Commission of Ethics in Research
- FHP:
-
Family Health Program
- IBGE:
-
The Brazilian Institute of Geography and Statistics
- PHC:
-
Primary health care
- PNS:
-
Pesquisa Nacional de Saúde
- SUS:
-
Sistema Único de Saúde
- USC:
-
Usual Source of Care
References
Starfield B. Is primary care essential? Lancet. 1994;344(8930):1129–33.
Kringos DS, Boerma WG, Hutchinson A, van der Zee J, Groenewegen PP. The breadth of primary care: a systematic literature review of its core dimensions. BMC Health Serv Res. 2010;10(1):65.
Christakis DA. Continuity of care: process or outcome? Ann Fam Med. 2003;1(3):131–3.
Cunha EM, Giovanella L. Longitudinalidade/continuidade do cuidado: identificando dimensões e variáveis para a avaliação da Atenção Primária no contexto do sistema público de saúde brasileiro. Ciênc Saúde Coletiva. 2011;16(supl. 1):1029–42.
Du Z, Liao Y, Chen C-C, Hao Y, Hu R. Usual source of care and the quality of primary care: a survey of patients in Guangdong province, China. Int J Equity Health. 2015;14(1):60.
Starfield B. Atenção primária: equilíbrio entre necessidades de saúde, serviços e tecnologia: Unesco; Ministério da Saúde; 2004.
Mainous III A, Gill JM. The importance of continuity of care in the likelihood of future hospitalization: is site of care equivalent to a primary clinician? Am J Public Health. 1998;88(10):1539–41.
O’Malley AS, Mandelblatt J, Gold K, Cagney KA, Kerner J. Continuity of care and the use of breast and cervical cancer screening services in a multiethnic community. Arch Intern Med. 1997;157(13):1462–70.
Mainous AG, Baker R, Love MM, Gray DP, Gill JM. Continuity of care and trust in one’s physician: evidence from primary care in the United States and the United Kingdom. Fam Med. 2001;33(1):22–7.
Cowling TE, Harris M, Watt H, Soljak M, Richards E, Gunning E, et al. Access to primary care and the route of emergency admission to hospital: retrospective analysis of national hospital administrative data. BMJ Qual Saf. 2016;25:(6):432-40.
Tang N, Stein J, Hsia RY, Maselli JH, Gonzales R. Trends and characteristics of US emergency department visits, 1997-2007. JAMA. 2010;304(6):664–70.
Skinner H, Blanchard J, Elixhauser A. Trends in emergency department visits, 2006–2011: Statistical Brief# 179. 2006.
Cowling TE, Harris MJ, Watt HC, Gibbons DC, Majeed A. Access to general practice and visits to accident and emergency departments in England: cross-sectional analysis of a national patient survey. Br J Gen Pract. 2014;64(624):e434–e9.
Cowling TE, Cecil EV, Soljak MA, Lee JT, Millett C, Majeed A, et al. Access to primary care and visits to emergency departments in England: a cross-sectional, population-based study. PLoS One. 2013;8(6):e66699.
Acosta AM, da Silva Lima MAD. Características de usuários frequentes de serviços de urgência: revisão integrativa. Revista Eletrônica de Enfermagem. 2013;15(2):564–73.
Carvalho RAdS, Santos VS, Melo CMd, Gurgel RQ, Oliveira CCdC. Inequalities in health: living conditions and infant mortality in Northeastern Brazil. Revista de Saúde Pública. 2015;49. http://dx.doi.org/10.1590/S0034-8910.2015049004794
Duncan P, Bertolozzi MR, Cowley S, Egry EY, Chiesa AM, de Siqueira França FO. “Health for All” in England and Brazil? Int J Health Serv. 2015;45(3):545–63.
Guimarães JMN, Werneck GL, Faerstein E, Lopes CS, Chor D. Early socioeconomic position and self-rated health among civil servants in Brazil: a cross-sectional analysis from the Pró-Saúde cohort study. BMJ Open. 2014;4(11):e005321.
Rasella D, Machado DB, Castellanos MEP, Paim J, Szwarcwald CL, Lima D, et al. Assessing the relevance of indicators in tracking social determinants and progress toward equitable population health in Brazil. Glob Health Action. 2016;9. http://dx.doi.org/10.3402/gha.v9.29042
Carvalho Malta D, Siqueira Santos MA, Rizzato Stopa S, Barroso Vieira JE, Alves Melo E, dos Reis C, et al. A Cobertura da Estratégia de Saúde da Família (ESF) no Brasil, segundo a Pesquisa Nacional de Saúde, 2013. Revista Ciência & Saúde Coletiva. 2016;21(2):327-38.
Pinto HA, Sousa ANAd, Ferla AA. O Programa Nacional de Melhoria do Acesso e da Qualidade da Atenção Básica: várias faces de uma política inovadora. Saúde em debate Londrina Vol 38, n esp(out 2014), p 358–72. 2014.
Nedel FB, Facchini LA, Martín-Mateo M, Vieira LAS, Thumé E. Family Health Program and ambulatory care-sensitive conditions in Southern Brazil. Rev Saude Publica. 2008;42(6):1041–52.
Aquino R, de Oliveira NF, Barreto ML. Impact of the family health program on infant mortality in Brazilian municipalities. Am J Public Health. 2009;99(1):87–93.
Macinko J, de Souza MFM, Guanais FC, da Silva Simoes CC. Going to scale with community-based primary care: an analysis of the family health program and infant mortality in Brazil, 1999–2004. Soc Sci Med. 2007;65(10):2070–80.
Dourado I, Oliveira VB, Aquino R, Bonolo P, Lima-Costa MF, Medina MG, et al. Trends in primary health care-sensitive conditions in Brazil: the role of the Family Health Program (Project ICSAP-Brazil). Med Care. 2011;49(6):577–84.
Rasella D, Aquino R, Barreto ML. Reducing childhood mortality from diarrhea and lower respiratory tract infections in Brazil. Pediatrics. 2010;126(3):e534–e40.
Rasella D, Harhay MO, Pamponet ML, Aquino R, Barreto ML. Impact of primary health care on mortality from heart and cerebrovascular diseases in Brazil: a nationwide analysis of longitudinal data. 2014.
Editorial. For the universal right to health: health is a right and not a business Saúde debate. 2014;38(101):194–6.
Almeida P. Mapeamento e análise dos modelos de atenção primária à saúde nos países da América do Sul. Atenção Primária à Saúde no Brasil. Rio de Janeiro: Isags; 2014.
Szwarcwald CL, Malta DC, Pereira CA, Vieira MLFP, Conde WL, Souza Junior PRB, et al. National Health Survey in Brazil: design and methodology of application. Ciência & Saúde Coletiva. 2014;19(2):333–42.
Damacena GN, Szwarcwald CL, Malta DC, Souza Júnior PRB, Vieira MLFP, Pereira CA, et al. O processo de desenvolvimento da Pesquisa Nacional de Saúde no Brasil, 2013. Epidemiologia e Serviços de Saúde. 2015;24(2):197–206.
Souza-Júnior PRB, Freitas MPS, Antonaci GA, Szwarcwald CL. Desenho da amostra da Pesquisa Nacional de Saúde 2013. Epidemiologia e Serviços de Saúde. 2015;24(2):207–16.
Reis E. Spatial income inequality in Brazil, 1872–2000. EconomiA. 2014;15(2):119–40.
Viana SM, Nunes A, Santos J, Barata R. Medindo as desigualdades em saúde no Brasil: uma proposta de monitoramento. Brasília: Organização Pan-Americana da Saúde, Instituto de Pesquisa Econômica Aplicada; 2001.
Macinko J, Lima Costa MF. Access to, use of and satisfaction with health services among adults enrolled in Brazil’s Family Health Strategy: evidence from the 2008 National Household Survey. Tropical Med Int Health. 2012;17(1):36–42.
Medina MG, Hartz ZMA. The role of the Family Health Program in the organization of primary care in municipal health systems. Cadernos de Saúde Pública. 2009;25(5):1153–67.
Fausto MCR, Giovanella L, Mendonça MHM, Seidl H, Gagno J. A posição da Estratégia Saúde da Família na rede de atenção à saúde na perspectiva das equipes e usuários participantes do PMAQ-AB. Saúde debate. 2014;38(spe):13–33.
Viacava F. Ten years of information on health services access and use. Cadernos de Saúde Pública. 2010;26(12):2210–1.
Acosta AM, da Silva Lima MAD. Usuários frequentes de serviço de emergência: fatores associados e motivos de busca por atendimento. Revista Latino-Americana de Enfermagem. 2015;23(2):337–44.
Acknowledgments
The authors would like to express their gratitude to Drs. Celia Landmann Szwarcwald and James Macinko who inspired us to write the article, and to Paulo Roberto Borges de Souza Júnior for the database organization.
Funding
This work was supported by the Brazilian Ministry of Health. No funding bodies had any role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Authors’ contributions
This manuscript has not been submitted or accepted for publication elsewhere. All authors contributed to the concept of the paper and data analysis. ID, MGM and RA were responsible for the writing of the final version of the manuscript. All authors have read and approved the paper, have met the criteria for authorship as established by the International Committee of Medical Journal Editors, believe that the paper represents honest work, and are able to verify the validity of the results reported. None of the authors have any conflicts of interest (including financial and other relationships) to report.
Competing interests
The authors declare that they have no competing interests.
Ethics approval and consent to participate
The study was approved by the Brazilian National Commission of Ethics in Research (CONEP) in June 2013, Regulation No. 328.159. And followed the National Health Council (CNS) assuring the subjects’ voluntariness, anonymity and possibility of withdrawal at any moment in the study, through the signing of a Consent Form.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated.
About this article
Cite this article
Dourado, I., Medina, M.G. & Aquino, R. The effect of the Family Health Strategy on usual source of care in Brazil: data from the 2013 National Health Survey (PNS 2013). Int J Equity Health 15, 151 (2016). https://doi.org/10.1186/s12939-016-0440-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12939-016-0440-7