Abstract
Background
Addressing sustainable development goals to reduce neonatal mortality remains a global challenge, and it is a concern in Ethiopia. As a result, the goal of this study was to assess the incidence and determinants of neonatal mortality in the first 3 days among babies delivered in the referral hospitals of the Amhara National Regional State.
Methods
A hospital-based prospective cohort study was conducted among 810 neonates in the first 3 days of delivery between March 1 and August 30, 2018. The neonates were followed up from the time of admission to 72 h. Interviewer-administered questionnaires and medical record reviews were conducted for data collection. Data were entered into Epi-data manager version 4.4 and analysed using STATA™ version 16.0. The neonate’s survival time was calculated using the Cox-Proportional hazards model.
Results
The overall incidence of neonatal mortality in this study was 151/1000 births. Neonatal mortality was significantly higher among neonates whose mothers came between 17 and 28 weeks of gestation for the first visit; among those whose mothers labour was not monitored with a partograph, mothers experienced postpartum haemorrhage and developed a fistula first 24 h, and experienced obstructed labour. However, 39% were less risky among neonates whose mothers were directly admitted and whose mothers had visited health facilities in less than 1-h, both.
Conclusions
This study revealed that approximately 1 in 7 neonates died within the first 3 days of life. The determinants were the timing of the first antenatal visit, quality of labour monitoring, maternal complications, and delay in seeking care. Thus, scaling up evidence-based interventions and harmonising efforts to improve antenatal care quality, promote institutional deliveries, provide optimal essential and emergency obstetric care, and ensure immediate postnatal care may improve neonatal survival.
Similar content being viewed by others
Background
The newborn period is critical in the miracle of life and death. In 2018, the global neonatal mortality rate was estimated to be 18 deaths per 1000 live births, with 28 deaths per 1000 live births in Sub-Saharan Africa, and in 2016, it was 30 deaths per 1000 live births in Ethiopia [1, 2]. According to a systematic review in developing countries, despite more than 99% of neonatal deaths in low and middle-income countries, these settings lack overall or cause-specific neonatal deaths [3]. The same systematic review also revealed that 57% of neonates died in the first 3 days of life, and two-thirds of these deaths occurred within the first 24 h. Furthermore, this review indicated that among 52% of under-five deaths in the Southeast Asia region, one-third of the neonatal mortality occurred within the first 3 days of life. Among 30% of the under-five deaths in the World Health Organization (WHO) African region, 17% of deaths occur within the first day of life [3]. The WHO also verifies that the danger of death is most significant in the first 24 h of life, with more than half of all neonatal deaths occurring within the first week of life [4]. In Ethiopia, a study conducted at a referral specialised teaching hospital revealed that the death of babies aged 1–3 days was riskier than 4–7 days [5].
In low and middle-income countries, it has been suggested that the scaling-up of evidence-based interventions that begin during the antenatal period, coordinated efforts aimed at improving the quality of antenatal care, promoting institutional deliveries, providing optimal essential and emergency obstetric care, and ensuring immediate postnatal care of neonates are essential [3, 6]. Consequently, some countries, including Ethiopia, have substantially improved targeted coverage for some interventions. However, these coverages have not resulted in the expected magnitude of reduction in neonatal mortality rate, specifically neonatal mortality within the first 3 days of life. The lack of a concurrent rise in the coverage of essential interventions in the continuum of care could be one of the possible reasons [3]. For example, a recent study in Ethiopia indicated that only 12.1% of women completed the continuum of maternal care services, and 25.1% did not receive any care during their recent births [7].
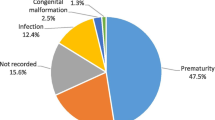
Although the perinatal mortality rate definition starts at 28 weeks of gestation in low and middle-income countries (LMICs), the mortality rate is higher than the developed countries that stated the definition from 20 weeks of gestation. The perinatal mortality rate includes all stillbirths and neonatal deaths in a given period over the total number of births multiplied by thousands [8]. In LMICs, there is a lower preterm newborns’ survival rate, and the numerator for perinatal mortality rate includes all fetal deaths with a gestational age of 28 weeks and above and all neonatal deaths within 7 days of life [8]. However, according to a global network study, in LMIC registries, most neonatal deaths occurred in babies > 37 weeks of gestation, weighing at least 2500 g shortly after birth [9]. Previous studies have also identified multiple risk factors for perinatal mortality rate in LMICs [10,11,12,13,14]. Poverty contributes to many newborn fatalities, either by increasing risk factors such as maternal infection or limiting access to sufficient care [15]. Studies have also revealed that the proportions of common causes of perinatal mortality rate include prematurity (17%); asphyxia (25%); infection (37%); tetanus (7%); diarrhoea (3%); congenital malformations (4%); and other causes (7%) [16,17,18,19]. Almost all the studies were conducted at the community level and within 28 days of life and recommended prevention through better medical care and hospitalisation in the intrapartum and early neonatal period [9].
Neonatal mortality rates and determinants in the early neonatal period (the first 3 days of life in this case) are essential for arranging programs and identifying suitable interventions. Local and recent evidence about the spread of the problem could help implement programmatically relevant decision-making [10]. However, despite a high number of deaths in the first 3 days, data are scarce in the first 3days of life, particularly at the tertiary level of care. Moreover, since both biology and empirical data suggest that the cause of death distribution differs substantially between these periods, separate cause-of-death estimates are required for the first 3 days of life, within the first 7 days, and within 28 days of life [10]. Therefore, this study aimed to address the incidence and determinants of newborn death in the first 3 days of life among babies delivered in referral hospitals.
Methods
Study setting and period
This study was conducted at the maternity wards of referral hospitals in the Amhara Regional State between March 1 and August 30, 2018. The National Regional State is located between 9° 20′ and 14° 20′ North latitude and 36° 20′ and 40° 20′ East longitude in the Northwestern part of Ethiopia. According to the Central Statistics Agency, the projected total population estimate Amhara Region in 2020/21 is 22,536,999 (11,236,853 males and 11 300,146 females). Of these, 20.08% were urban residents [20]. According to the annual performance report published by the Federal Ministry of Health of Ethiopia in the 2009 Fiscal Year, the region had 68 hospitals, 841 health centres, and 3342 health posts [21]. Dessie, Felege-Hiwot, University of Gondar, Debre-Birhan, and Debre-Markos were referral hospitals at the time of data collection for this study. Each referral hospital was expected to serve a population of 5 million people. The University of Gondar Teaching Referral Hospital (UoGH), Felege Hiwot Referral Hospital (FHH), and Debre Markos Referral Hospital (DMH) were selected for this study.
The UoGH serves the residents of Gondar town and the neighbouring zones. The NICU was established 20 years ago and serves as the region’s tertiary referral unit, caring for high-risk newborns born at the hospital, referrals from other health facilities and home deliveries. Outpatient clinics, emergency departments, paediatrics and malnutrition wards, and neonatal intensive care units (NICUs) were among the services provided by paediatric and child health departments for rural and urban populations. Although neonatal hospitalisation varies seasonally, the annual average admission rate is 1140. There was no mechanical ventilators or continuous positive airway pressure (CPAP) equipment in this 32-bed NICU, including radiant heaters and nine incubators.
On the other hand, Bubble CPAP was locally developed for neonates with respiratory distress syndrome (RDS). There were also four incubators and three phototherapy machines for term babies. The babies were given oxygen via nasal prongs or a nasal catheter connected to oxygen cylinders or concentrators. Ampicillin and gentamicin were the most usually prescribed antibiotics for sepsis treatment. Medications were given through a peripheral vein, with the umbilical vein being used on a few occasions. The NICU has four rooms, which were helpful for preterm and term babies, infectious diseases, and maternity, where relatively stable neonates and newborns require kangaroo mother care. Seven medical interns, two pediatric residents, one paediatrician, and 17 nurses staff the NICU [22].
Felege Hiwot referral Hospital was a teaching hospital for Bahir Dar University and served the Bahir Dar special zone, west Gojjam zone, Awi zone, South Gondar Zone. More than 7 million people were living in these zones. The FHH was established in 1963 and has been in operation since then. Medical, surgical, gynaecological, orthopaedic, intensive care units, paediatrics, and ophthalmological wards with 375 beds and 561 employees currently provide health care services. Approximately 6300 neonates are diagnosed with various health issues each year. There were 60 beds, five paediatricians, and 20 nurses in the neonatal ward [23].
Furthermore, the DMH hospital served as a teaching hospital for Debre Markos University was the only referral hospital found in the East Gojjam Zone. This hospital serves a population of over 3.5 million individuals within its catchment area. For extremely ill neonates and those who require neonatal care, the hospital also offers neonatal intensive care. There were 27 nurses, one paediatrician, and two general practitioners working in the NICU. Ten NICU beds, four kangaroo mother care beds, 19 mother side beds, eight radiant warmers, and six incubators were available in the unit. The regular nursing procedures in the NICU were phototherapy, umbilical transfusion, oxygen administration, nasogastric tube insertion, intravenous infusion, urinary catheterisation, lumbar puncture, and CPAP. In 2017, this hospital provided neonatal intensive care services for 1419 neonates [24].
Study design and population
An institution-based prospective cohort study was conducted among a cohort of term pregnant mothers and newborns admitted to three systematically selected referral hospitals. All term pregnant mothers (≥37 weeks gestational age (GA)) were admitted to the selected referral hospitals included in this study. Additionally, neonates discharged with an appointment and normal status were followed using mothers’ phones and the nearby health extension workers till 3 days of life. Then, they followed up until they gave birth, and their neonates were followed up for a total of 72 h. Cohorts of newborns who were delivered from women aged 15–49 years were included. Those born to women with mental illnesses who could not hear or speak due to their disease and twins were excluded from the study.
Sample size and sampling technique
The sample size of 832 was calculated using Epi-info version 7 stat calc software. The following assumptions of the incidence ratio of early neonatal death of 369 per 2142 deliveries [25], 95% confidence level, the margin of error 2.75, and 15% lost follow-up.
Systematic random sampling was used to identify 832 admitted term pregnant women enrolled in the follow-up study. First, a simple random sampling (i.e., lottery method) technique selected the three hospitals. The study subjects were then allocated the proportion of the expected admitted number of term pregnant women per referral hospital, 300 each for UoGH and FHH, and 210 for DMH. The computed sample was then chosen in order from each referral hospital.
Variables
Times-to-event, the event of interest was early neonatal death and dichotomised as (alive =1 and died = 0). The determinant variables included socio-demographic and economic factors: ethnicity, religion, place of residence, marital status, education status of the mother, and occupational status of the mother, age of mother, maternal and neonatal related factors: ANC follow up, parity gravidity, mode of delivery gestational age, birth weight, age of neonate at discharge, and sex of neonate. Neonatal illnesses include respiratory distress, perinatal asphyxia, sepsis, congenital malformation, hyaline membrane disease, and meconium aspiration syndrome—care/ service-related factors: Partograph follow-up, length of stay, and obstetric complications.
Data quality assurance and questionnaire
First, we prepared the English questionnaire, translated it to Amharic’s local language, and back to English by different individuals to check its consistency. The survey was pretested on 42 mothers (14 exposed and 28 unexposed cohorts) in Debre Tabor Hospital, which differs from the study hospitals. The questionnaire (Additional file 1) was then assessed for its clarity and completeness. Some skip patterns were corrected, and questions difficult to ask were rephrased. The questionnaire had three parts. The first part was socio-demographic factors (i.e., maternal age, body mass index, age at first marriage, age at early pregnancy, age at first delivery, ethnicity, residence, marital status, educational status, husband educational status, occupation, an estimated distance of home from health institution, determining range from primary health institute to referral hospital, religion, and income). The reproductive factors constitute the second part, like gravidity, parity, gestational age, referral status, birth attendant, previous cesarean section, mode of final delivery, antenatal care attendance, number of ANC visits, duration of labour before the presentation, prior history of abortion, and obstetric complications. The third part was that programmatic factors included infrastructure and transportations. The completed questionnaires were checked day-to-day for inclusiveness, correctness, clarity, and consistency by the supervisors and the principal investigators, and necessary corrections and changes were made. During data entry and analysis, complete and consistent variables were checked using frequency distributions, cross-tabulations, sorting in ascending, and descending order.
Data collection process
Because of the day and night allocation of data collectors in each hospital, six bachelor (two per hospital) holders experienced midwives collected data interchangeably (by shift), and three general practitioners (1 per each hospital) were supervised the process. Three days of training were given based on the study’s objective and the value of collecting the actual data. The structured questionnaire was discussed in detail, going through every question, and clarification was provided. A field manual was prepared for the supervisors and data collectors for use during data collection. The six data collectors were present in the respective hospitals during the complete 24 h.
The data collectors collected the data daily. Medical record review and an interviewer-administered questionnaire were used to collect data on the intended variables of interest until the time of discharge from the hospital or 72 h. We retained only the previously collected data were retained for analysis in cases of readmission. We assessed the neonates for the entire period of hospital stay (both in the maternity ward and neonatal intensive care unit). There was no follow-up after hospital discharge.
Data management and analysis
Early neonatal mortality was the event of interest, coded as “1” for failure and “0” for censored. Time-to-event was considered by subtracting the date of admission from the time of the event. Data entered into Epi-Data manager version 4.4 and analysed using STATA™ version 16.0. for the follow-up time and age of the cohort, we calculated the mean and standard deviation. The cox-Proportional hazard model was used to determine risk factors for newborns’ survival time delivered at the hospitals. A tolerance level with a cut point of 0.2 was used to omit multicollinearity.
The Kaplan Meier curves were used to estimate survival time. The log-rank test was used to look at statistical variances between the groups of variables. Statistical significance was declared at p-value < 0.05. A summary statistic of proportions, including hazard ratio and 95% confidence intervals, was used. Screening of risk factors for the newborn’s death employed bivariate Cox regression for each variable one at a period. Those variables with p < 0.25 throughout the bivariate Cox regression analysis were taken as an entrant variable to control possible confounders for the multivariate Cox regression model.
Operational definitions
Early neonatal mortality: This refers to a neonate’s death within the first 72 h of life.
Neonatal survival: is referred to as being alive until the end of the follow-up period (72 h).
Term pregnancy: It is defined as a pregnancy lasting between 37 and 42 weeks of gestation.
Maternal First Delay refers to the delay after the onset of actual labour to reach a health facility.
Results
During the 72 h’ observation, 810 newborns (97.4% of the sample) followed for 37,454 new-borns-hours at the three hospitals. The mean (+SD) length of stay at the four hospitals was 46.23(+ 29.31) hours. Of the 810 newborns, 10.4% were stillbirths, 17.1% were alive but complicated, and 72.5% were alive without complications.
Maternal and neonatal clinical characteristics
Out of the 84 stillbirths, 25 were from primiparous women, 15 deaths in the first 72 h out of the 38 deaths observed among women who gave 2 to 4 births. As Table 1 shows, 81.9% of the newborns who survived were mothers who received antenatal care. Out of 84 stillbirths, 58 of them were diagnosed with intrauterine fetal death before starting actual labour, whereas the rest 26 were fresh stillbirths during delivery (Table 1).
Neonatal illness
The leading cause of disease in Amhara regional state referral hospitals was neonatal jaundice 52(42.4%), followed by other complications 30(24.6%) like birth trauma, congenital anomalies, and asphyxia 22(17.7%) (Fig. 1).
Of the 688 neonates discharged, 56.7% were discharged alive, 2.5% were discharged with treatment, and 17.3% were referred to the NICU. In contrast, the rest of the 23.5% were discharged with an appointment.
Neonatal survival
During the study period, a total of 15.1% (n = 122) of neonates deaths were observed, making an overall newborn mortality rate of 151 per thousand births. Of the 122 newborn deaths, 84(68.9%) were stillbirths, 38(31.1%) died in the first 72 h (Table 2). The overall incidence of neonates mortality was 1.012 per thousand early neonate hours.
Kaplan-Mair survival analysis
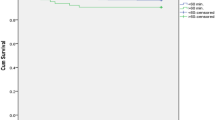
There was a higher mortality level in the first 24 h compared to after 24 to 72 h. This finding indicates a substantial reduction in death after the neonates survive the early 24 h of life in the observation period (Fig. 2). Similarly, the curve indicates that neonatal mortality shows substantial decrement among those whose labour was monitored with Partograph (Fig. 3).
Determinants of neonatal mortality
We included the variables with a p-value of less than 0.25 in the Cox proportional hazards regression model’s crude model. Then, after controlling for potential confounders using multivariate Cox proportional hazard regression, the timing of first antenatal care visit, monitoring with partograph, type of admission of the women, and maternal complications within the first 24 h (postpartum haemorrhage, fistula, and obstructed labour) were the variables that determine neonatal survival within the first 72 h of life.
Gestational age at the first antenatal care visit was found to be a risk factor for neonatal mortality. Women who came between 17 and 28 weeks of gestation for the first visit were 1.67 times more likely to lose their child [AHR = 1.67: 95% CI: 1.02, 2.73] than those who started the initial antenatal care visit before 16 weeks of gestation. Mothers not monitored with a partograph during labour were 2.66 times the risk of neonatal mortality [AHR = 2.66:95% CI: 1.70, 4.15] compared to their counterparts. Direct admission was 39% less risk of neonatal death than [AHR = 0.61:95% CI: 0.38, 0.97] those admitted from referral to another health facility.
Maternal complications within 24 h were also a significant risk factor for newborn mortality. Mothers experiencing postpartum haemorrhage were about three times risky for new-borns death [AHR = 2.88; 95% CI:1.69, 4.89], and those who developed fistula in the first 24 h were also about four times risky for new-borns death [AHR = 3.75; 95% CI: 1.23, 11.43]. Obstructed labour was more than twice risky [AHR = 2.14; 95% CI: 1.35, 3.38] for neonatal mortality and less than 1-h maternal first delay in visiting health facility was 39% less risk of neonatal death [AHR =0.61; 95% CI: 0.37, 0.98] (Table 3).
Discussion
Losing a newborn within the first 3 days of life, during which high neonatal mortality occurred, was shocking for the family and community and is devastating globally. Especially in developing countries, addressing this issue was a complex task for several factors. The study aimed to determine the incidence and determinants in the first 3 days among babies delivered in referral hospitals. In this study, 810 neonates born at the referral hospitals were included during the study period, and male predominance was noted in 53.5% of the study participants. Our study finding is in line with studies carried out in Pakistan (63%) [26], South Africa (57.8%) [27], in India (63.3%), in St Paul’s Hospital Millennium Medical College (61.1%) [28] and University of Gondar hospital (58.3) [22], Ethiopia. Natural selection response to differential survival prospects [29] and cultural and social factors [22] discrepancy between female and male babies. Our study’s causes of neonatal deaths were neonatal jaundice, complications such as birth trauma and congenital anomaly, asphyxia, umbilical sepsis, and neonatal sepsis, which are in line with the causes found in Ghana [30, 31], and Uganda [32].
In our study, 122 neonates were lost within the first 3 days of life, giving an overall neonatal mortality rate of 151/1000 total deaths and a stillbirth rate of 103.7/1000 total births. This figure shows a significant decline from a study conducted in the Tikur Anbesa specialised hospital (225/1000 live births) [33] and (302/1000 live births) [22]. This decline might be due to the impacts of different interventions for the last 6 years. However, it was much higher than the global neonatal mortality rate in 2016 [34], and in studies conducted in Southern Ethiopia [35, 36], Eastern Ethiopia [37], Southwest Ethiopia [38], Sudan [39], Uganda [25], Zambia [40] and Ghana [30].. Our study finding was also much higher than a finding of a systematic review of perinatal mortality rate in Ethiopia that indicated 75/1000 live births at the institutional level, 43/1000 total births with follow up studies, 59.1/1000 total births in the Amhara region, and 29.5/1000 total births among early newborns (up to 7 days) [41]. The variances might be attributed to study designs, health service coverage, socioeconomic factors, and PMR’s definition in other studies. In addition, the higher PMR in this study might be because of the admission of complicated mothers and the consideration of perinatal mortality rate up to 3 days in referral hospitals. This finding implies that the situation of neonatal mortality is still not progressing as anticipated in referral hospitals and strengthen the argument made by the study conducted in Jimma Zone [38] and a previous systematic review [6], which concluded that “health facility delivery had no significant effect on neonatal mortality.” However, this study’s findings should be interpreted vigilantly because of the stillbirth rate reports among admitted term pregnant women in referral hospitals. Possible misclassification of pregnancy outcomes (e.g., severe asphyxia of neonates) might overestimate the actual burden of stillbirth in the study area. Though there might be differences based on some factors, this implies that there is a need to plan tailored and targeted interventions by all stakeholders at different levels.
Regarding the determinants of neonatal mortality within the first 72 h, gestational age at the first antenatal care visit was a risk factor. Women who came between 17 and 28 weeks of gestation for the first visit were 1.67 times more likely to lose their child than those who started the initial antenatal care visit before 16 weeks of pregnancy. This finding is consistent with studies conducted in Tigray regional state [42], Felege Hiwot referral hospital [43], and Gaza-Strip [44]. This result infers that the earlier the start of prenatal care visits, the more the mothers will have time to complete four follow-ups, which will help us a new method of obstetric problems, which suggests the recent WHO recommendation of positive pregnancy experiences [45]. Thus, this study implies that the early start of the antenatal visit and possible consideration of the new WHO recommendation for antenatal care visits in Ethiopian referral hospitals could play vital roles in reducing early newborn deaths.
Maternal complications within 24 h were also a significant risk factor for neonatal mortality. Of these, the experience, postpartum haemorrhage, fistula development within the first 24 h, and obstructed labour were found to be three times, four times, and more than twice risky for neonatal death within the first 72 h of life. Our study’s findings regarding fistula and postpartum haemorrhage as risks for neonatal mortality were unique in this finding. The possible reason for neonatal mortality among mothers facing postpartum haemorrhage and fistula might be intrapartum asphyxia. In cases of maternal complications, the attention of health care providers diverts to saving the mother, and in some cases, neonates would not get adequate care, which leads them to intrapartum asphyxia. However, future research should be conducted to get the exact cause of neonatal mortality in such complications. However, this study’s results, which identified obstructed labour as a risk of neonatal mortality, were similar to studies conducted in Hawassa University hospital, Ethiopia [46], and tertiary hospitals in Tanzania [47]. These findings might be due to asphyxia and prolonged labour-related consequences leading to premature neonatal death.
Moreover, mothers who were not monitored with partograph during labour were nearly three times the risk of neonatal mortality than their counterparts. This result was supported by a study in Addis Ababa [48] and Tigray regional state [42]. This outcome entails that feto-maternal health should be monitored with the start of the active first stage of labour for timely management of prolonged labour, and its consequences will be early identified as prevention and control of early neonatal death.
Furthermore, direct admission was 39% less risk of newborn mortality than those admitted from referral to another health facility. In other words, mothers who require a referral were either suffer from severe obstetric problems or transfer time. We extend the time to receive skilled care. Besides, less than 1 h of maternal first delay to visit health was 39% less risk of neonatal death. This result was similar to a study in Tigray Northern Ethiopia, showing that seeking skilled care at the start of labour was protective for perinatal mortality [42], Uganda [32], and India [49]. This result indicates that the first delay in maternal death also contributes to early neonatal death. We suggest that healthcare providers pay attention to newborns’ care with significant intrapartum asphyxia, including respiratory, temperature, and nutritional support.
Despite the indications of the Ghanian study [30], this study has some inherent limitations. First, though this study was unique in addressing the first 3 days of life with a follow-up study design to determine the risk factors of early neonatal mortality, being only at the tertiary level of care may elevate the actual incidence estimate of premature neonatal death in the region. Second, the study was based on tertiary hospitals and may not show the picture of secondary and primary hospitals, and data were only collected up to 72 h of the life of the newborns. Therefore, cases occurring after 72 h were missed. Third, a mixed-method study design should have been used to identify the issues related to mothers and health care providers’ perceptions of the quality of services provided in the referral hospitals. Further longitudinal studies focusing on early neonatal death should explore health system, maternal, and obstetric factors, especially in the first 3 days.
Conclusions
We hypothesised high neonatal mortality in tertiary care centres in the first 3 days of life and found that about 1 in 7 newborns died in the first 3 days of life in the tertiary level of care in Northwestern Ethiopia. The leading causes of newborn death were neonatal jaundice, followed by complications like birth trauma, congenital anomalies, and asphyxia.
Moreover, the determinants of neonatal mortality were delay for the first ANC visit, more than 1-h maternal first delay to visit a health facility, and health system-related determinants such as not monitoring labour with, admission by referral were the significant factors. Furthermore, obstetric determinants were mothers’ experience of postpartum haemorrhage, fistula development within the first 24 h, and obstructed labour. Therefore, each hospital in the region must start implementing the WHO recommendation on positive pregnancy experience for addressing the health system and obstetric risk factors of newborn mortality. Additionally, awareness creation and adherence to the recommended level of care are essential.
Availability of data and materials
On reasonable request, the corresponding author will provide the datasets generated during the current work.
Abbreviations
- AHR:
-
Adjusted Hazard Ratio
- ANC:
-
Antenatal Care
- CHR:
-
Crude Hazard Ratio
- CI:
-
Confidence Interval
- DMH:
-
Debre Markos Hospital
- CPAP:
-
continuous positive airway pressure machines
- ETB:
-
Ethiopian Birr
- FHH:
-
Felege Hiwot Hospital
- GA:
-
Gestational Age
- SD:
-
Standard Deviation
- LMICs:
-
Low- and middle-income countries
- NICU:
-
neonatal intensive care unit
- RDS:
-
respiratory distress syndrome
- UoGH:
-
university of Gondar hospital
- WHO:
-
World Health Organization
References
Hug L, Sharrow D, You D: Levels & trends in child mortality: report 2017. Estimates developed by the UN Inter-agency Group for Child Mortality Estimation 2019.
Demographic IE. Health survey 2016: key indicators report. Addis Ababa Ethiopia, and Rockville: CSA and ICF; 2016.
Sankar M, Natarajan C, Das R, Agarwal R, Chandrasekaran A, Paul V. When do newborns die? A systematic review of the timing of overall and cause-specific neonatal deaths in developing countries. J Perinatol. 2016;36(1):S1–S11.
Organisation WH: Children: reducing mortality. Weekly Epidemiological Record 2014, 89(38):418–420.
Worku B, Kassie A, Mekasha A, Tilahun B, Worku A. Predictors of early neonatal mortality at a neonatal intensive care unit of a specialised referral teaching hospital in Ethiopia. Ethiop J Health Dev. 2012;26(3):200–7.
Tura G, Fantahun M, Worku A. The effect of health facility delivery on neonatal mortality: systematic review and meta-analysis. BMC Pregnancy Childbirth. 2013;13(1):1–9.
Emiru AA, Alene GD, Debelew GT. Women’s retention on the continuum of the maternal care pathway in west Gojjam zone, Ethiopia: a multilevel analysis. BMC Pregnancy Childbirth. 2020;20:1–14.
Organization WH: Neonatal and perinatal mortality: country, regional and global estimates: World Health Organization; 2006.
Belizán JM, McClure EM, Goudar SS, Pasha O, Esamai F, Patel A, et al. Neonatal death in low-middle income countries: a global network study. Am J Perinatol. 2012;29(8):649.
Oza S, Lawn JE, Hogan DR, Mathers C, Cousens SN. Neonatal cause-of-death estimates for the early and late neonatal periods for 194 countries: 2000–2013. Bull World Health Organ. 2014;93:19–28.
Bayou G, Berhan Y: Perinatal mortality and associated risk factors: a case-control study. Ethiop J Health Sci 2012, 22(3).
Orsido TT, Asseffa NA, Berheto TM. Predictors of neonatal mortality in neonatal intensive care unit at referral Hospital in Southern Ethiopia: a retrospective cohort study. BMC Pregnancy Childbirth. 2019;19(1):83.
Wakgari N, Wencheko E. Risk factors of neonatal mortality in Ethiopia. Ethiop J Health Dev. 2013;27(3):192–9.
Alam N. Teenage motherhood and infant mortality in Bangladesh: maternal age-dependent effect of parity one. J Biosoc Sci. 2000;32(2):229–36.
Vogel JP, Souza JP, Mori R, Morisaki N, Lumbiganon P, Laopaiboon M, et al. Maternal complications and perinatal mortality: findings of the World Health Organization multicountry survey on maternal and newborn health. BJOG. 2014;121(Suppl 1):76–88.
Tekelab T, Akibu M, Tagesse N, Tilhaun T, Yohanes Y, Nepal S. Neonatal mortality in Ethiopia: a protocol for systematic review and meta-analysis. Syst Rev. 2019;8(1):103.
Tafere TE, Afework MF, Yalew AW. Does antenatal care service quality influence essential newborn care (ENC) practices? In Bahir Dar City Administration, north West Ethiopia: a prospective follow up study. Italian J Paediatrics. 2018;44(1):105.
Liu L, Oza S, Hogan D, Chu Y, Perin J, Zhu J, et al. Global, regional, and national causes of under-5 mortality in 2000–15: an updated systematic analysis with implications for the sustainable development goals. Lancet. 2016;388(10063):3027–35.
Mengesha HG, Sahle BW. Cause of neonatal deaths in northern Ethiopia: a prospective cohort study. BMC Public Health. 2017;17(1):62.
Commission CSAoEaAP: Population Projection of Ethiopia for All Regions at WeredaLevel from 2014–2020. Central Statistical Agency of Ethiopia 2020.
Federal Ministry of Health E. Health Sector TransformationPlan 1 Version 1 Annual Performance Report EFY 2008 (2015/16). In: Federal Negarit Gazette. Addis Ababa: Federal Ministry of Health, Ethiopia; 2015.
Demisse AG, Alemu F, Gizaw MA, Tigabu Z. Patterns of admission and factors associated with neonatal mortality among neonates admitted to the neonatal intensive care unit of University of Gondar Hospital, Northwest Ethiopia. Pediatric Health med Therapeutics. 2017;8:57.
Tewabe T, Mehariw Y, Negatie E, Yibeltal B. Neonatal mortality in the case of Felege Hiwot referral hospital, Bahir Dar, Amhara regional state, north West Ethiopia 2016: a one-year retrospective chart review. Italian J Paediatrics. 2018;44(1):1–5.
Alebel A, Wagnew F, Petrucka P, Tesema C, Moges NA, Ketema DB, et al. Neonatal mortality in the neonatal intensive care unit of Debre Markos referral hospital, Northwest Ethiopia: a prospective cohort study. BMC Pediatr. 2020;20(1):1–11.
Nakimuli A, Mbalinda SN, Nabirye RC, Kakaire O, Nakubulwa S, Osinde MO, et al. Stillbirths, neonatal deaths and neonatal near-miss cases attributable to severe obstetric complications: a prospective cohort study in two referral hospitals in Uganda. BMC Pediatr. 2015;15(1):44.
Ali SR, Ahmed S, Lohana H. Disease patterns and outcomes of neonatal admissions at a secondary care hospital in Pakistan. Sultan Qaboos Univ Med J. 2013;13(3):424.
Hoque M, Haaq S, Islam R. Causes of neonatal admissions and deaths at a rural hospital in KwaZulu-Natal, South Africa. Southern Afr J Epidemiol Infection. 2011;26(1):26–9.
Rakholia R, Rawat V, Bano M, Singh G. Neonatal morbidity and mortality of sick newborns admitted in a teaching hospital of Uttarakhand. CHRISMED J Health Res. 2014;1(4):228.
Crawford M, Doyle W, Meadows N. Gender differences at birth and differences in fetal growth. Hum Reprod. 1987;2(6):517–20.
Welaga P, Moyer CA, Aborigo R, Adongo P, Williams J, Hodgson A, et al. Why are babies dying in the first month after birth? A 7-year study of neonatal mortality in northern Ghana. PLoS One. 2013;8(3):e58924.
Edmond KM, Quigley MA, Zandoh C, Danso S, Hurt C, Agyei SO, et al. Aetiology of stillbirths and neonatal deaths in rural Ghana: implications for health programming in developing countries. Paediatr Perinat Epidemiol. 2008;22(5):430–7.
Waiswa P, Kallander K, Peterson S, Tomson G, Pariyo GW. Using the three delays model to understand why newborn babies die in eastern Uganda. Trop Med Int Health. 2010;15(8):964–72.
Bogale Worku AK. Amha Mekasha, Birkneh Tilahun, Alemayehu Worku: predictors of early neonatal mortality at a neonatal intensive care unit of a specialised referral teaching hospital in Ethiopia. Ethiop J Health Dev. 2012;26(3):200–7.
IGME U: Levels & Trends in Child Mortality: Report 2017, Estimates developed by the UN inter-Agency Group for Child Mortality Estimation. United Nations Children’s Fund N Y 2017.
Limaso AA, Dangisso MH, Hibstu DT. Neonatal survival and determinants of mortality in Aroresa district, southern Ethiopia: a prospective cohort study. BMC Pediatr. 2020;20(1):33.
Shifa GT, Ahmed AA, Yalew AW. Early days of life are crucial for child survival in Gamo Gofa zone, southern Ethiopia: a community-based study. BMC Pediatr. 2016;16(1):30.
Desta BN, Assefa N, Damte TD, Hordofa LO. Neonatal mortality and its risk factors in eastern Ethiopia: a prospective cohort study in Kersa health and demographic surveillance system (Kersa HDSS). Mortality. 2016;13(18):19.
Debelew GT, Afework MF, Yalew AW. Determinants and causes of neonatal mortality in Jimma zone, Southwest Ethiopia: a multilevel analysis of prospective follow-up study. PLoS One. 2014;9(9):e107184.
Bashir AO, Ibrahim GH, Bashier IA, Adam I. Neonatal mortality in Sudan: analysis of the Sudan household survey, 2010. BMC Public Health. 2013;13(1):287.
Lukonga E, Michelo C. Factors associated with neonatal mortality in the general population: evidence from the 2007 Zambia Demographic and health survey (DHS); a cross-sectional study. Pan Afr Med J. 2015;20(1):64.
Jena BH, Biks GA, Gelaye KA, Gete YK. Magnitude and trend of perinatal mortality and its relationship with the inter-pregnancy interval in Ethiopia: a systematic review and meta-analysis. BMC Pregnancy Childbirth. 2020;20(1):1–13.
Goba GK, Tsegay H, Gebregergs GB, Mitiku M, Kim KA, Alemayehu M. A facility-based study of factors associated with perinatal mortality in Tigray, northern Ethiopia. Int J Gynaecol Obstet. 2018;141(1):113–9.
Tewabe T, Mehariw Y, Negatie E, Yibeltal B. Neonatal mortality in the case of Felege Hiwot referral hospital, Bahir Dar, Amhara regional state, north West Ethiopia 2016: a one-year retrospective chart review. Ital J Pediatr. 2018;44(1):57.
Imad El Awour YA, Ashour M. Determinants and risk factors of neonatal mortality in the Gaza strip, occupied Palestinian territory: a case-control study; 2012.
WHO: WHO recommendations on Positive pregnancy experience; 2016.
Getachew Bayou YB. perinatal mortality and associated risk factors: a case-control study. Ethiop J Health Sci. 2012;22(3):153.
Mmbaga BT, Lie RT, Olomi R, Mahande MJ, Olola O, Daltveit AK. Causes of perinatal death at a tertiary care hospital in Northern Tanzania 2000–2010: a registry-based study. BMC Pregnancy Childbirth. 2012;12(139):1-9.
Getiye Y, Fantahun M. Factors associated with perinatal mortality among public health deliveries in Addis Ababa, Ethiopia, an unmatched case-control study. BMC Pregnancy Childbirth. 2017;17(1):245.
Bapat U, Alcock G, More NS, Das S, Joshi W, Osrin D. Stillbirths and newborn deaths in slum settlements in Mumbai, India: a prospective verbal autopsy study. BMC Pregnancy Childbirth. 2012;12(1):39.
Acknowledgements
We want to forward our deepest gratitude to Debre Tabor University. We are also grateful to Amhara National regional state health bureau and respective referral hospitals. Finally, we also need to forward our gratitude to the data collectors and study participants.
Funding
Debre Tabor University supplied the remuneration for data collectors and supervisors. On the other hand, the university played no part in the study design, data collecting, analyses, publication decision, or manuscript preparation.
Author information
Authors and Affiliations
Contributions
All authors contributed to the work reported, whether in the conceptualisation, research design, execution, data gathering, analysis, interpretation, or all of these areas. All authors contributed to the manuscript’s drafting, revision, and critical evaluation. Authors given final consent to the version that will be published, have agreed on the journal to which the manuscript will be submitted and agreed to be responsible for all elements of the work.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Ethical confirmation was granted from the Institution ethical Review Committee of Debre Tabor University, and all methods were performed following the relevant guidelines and regulations. A letter of formal permission and support was written to the respective administrator office. The aim of the research was undoubtedly clarified to concerned bodies. Mothers were told that they have the right to be involved or not to be involved in the study before they signed written informed consent. The research aims undoubtedly clarified, written informed consent was obtained from all study subjects and their legal guardian(s), confidentiality was ensured, and the study’s process was explained to the neonates’ mothers. Data collectors read the respondents’ consent and mark if they agree for mothers who could not read and write. The study participants knew that data collectors were skilled only to gather evidence, and the data was not being passed to anybody. The confidentiality of the information (personal identification and idea were not used in a way that might threaten the respondent) was maintained, and the study participants’ privacy was respected. There was no payment/incentive for participating in this interview.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Worke, M.D., Mekonnen, A.T. & Limenh, S.K. Incidence and determinants of neonatal mortality in the first three days of delivery in northwestern Ethiopia: a prospective cohort study. BMC Pregnancy Childbirth 21, 647 (2021). https://doi.org/10.1186/s12884-021-04122-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12884-021-04122-8