Abstract
Background
Plenty of evidence shows how social isolation and loneliness are associated with increased risk for numerous diseases and mortality. But findings about their interactive or combined effects on health outcomes and mortality remains inconclusive.
Objective
Analyze the longitudinal association of loneliness, social isolation and their interactions, with the all-cause mortality among older adults in Mexico.
Methods
A retrospective observational study was conducted. Mexican adults older than 50 years were included. Data from the Mexican Health and Aging Study (MHAS) in the 2015 and 2018 waves were used. The subjects were classified according to their level of loneliness and the presence of social isolation. Multivariate logistic regression analyzes were performed to determine the degree of association between loneliness and social isolation with all-cause mortality at a 3-year follow-up.
Results
From the total sample of 11,713 adults aged 50 years or over, 707 (6%) did not survive, 42% presented loneliness, and 53% were classified as socially isolated. After multivariate adjustment only social isolation (OR = 1.30, 95%CI:1.03–1.64) was associated with all-cause mortality, loneliness (Mild: OR = 0.83, 95%CI:0.59–1.16; Severe: OR = 1.03, 95%CI:0.71–1.64), and the interaction between loneliness and social isolation were not associated with all-cause mortality.
Conclusion
Social isolation, but not loneliness or their interaction, was associated with all-cause mortality in Mexican adults older than 50 years. This finding may help direct possible future interventions that help improve mental health in older adults from a highly collectivistic country.
Similar content being viewed by others
Background
Older persons are the fastest growing segment of the population worldwide. The World Health Organization (WHO) calculates that by 2050 one in every five people throughout the world will be 60 years of age or older. Among these, 80% will be living in low to middle income countries [1]. This demographic transition poses a burden to the individual and to his or her family, as well as to the society and represents a challenge for public health systems, especially in countries such as México [2], where 7.8% of its population is older than 65 years [3].
Loneliness has been defined as a feeling of isolation despite having a social network present [4] and can be considered as a subjective characteristic of the satisfaction that an individual feels about the quality of social relationships [5], while social isolation is defined as the presence of low quantity and quality of contact with other people [4] and is an objective characteristic on the count of social contacts of an individual [5]. Although social isolation could be related to loneliness [6], a low correlation and discrepancies between loneliness and social isolation have recently been observed [7].
Increasing age is considered a risk factor for loneliness and social isolation [4, 6]. The prevalence of loneliness in older adults is estimated between 10 and 50% [4], and chronic loneliness prevalence have been reported in 15–30% of older adults and occasional loneliness up to 60–80% [8]. And regarding social isolation of older adults, the prevalence is estimated at 6–43% [4]. In Mexico, the prevalence of loneliness is estimated at 13.2–34.9% [9, 10], and of social isolation at 34–43% [6, 11], both in older adults.
Plenty of evidence shows that social isolation and loneliness are associated with increased risk for numerous diseases, such as: cardio metabolic diseases in general population [12, 13], infectious diseases in patients aged 18 to 55 years [14], sleep alterations in general population [15], cognitive decline in older adults [16] and depression in older adults [17, 18]. Moreover, isolation and loneliness negatively impact the self-perception of health [19].
Conflicting results have been obtained through different studies for the role of loneliness or social isolation and mortality, some studies show an increased risk of mortality in older adults [20, 21], while others do not conclude that loneliness or social isolation are determining factors of fatal outcomes in the same population [22,23,24]. Although social isolation and loneliness often coexist, findings about their interactive or combined effects on health outcomes and mortality remains inconclusive [25]. Some studies have found a combined or synergic effect between social isolation and loneliness in middle-age and older adults [26, 27], other studies have found that the combination of loneliness and social isolation predict all-cause mortality in older adults [5], but the combined effect is not worse than experiencing either by itself [28, 29]. It remains unclear how these two aspects of human socialization interact with each other.
Currently, most previous studies come from high-income [20, 21, 24, 30], highly individualistic countries [31]. Given that there are cultural and socioeconomic factors that influence the effect of loneliness and social isolation on health and all-cause mortality risk [32], it is necessary to research highly collectivistic middle- and low-income countries, like Mexico, which can be used as a baseline for the study of the consequences of this phenomenon on wider spectrum of countries in Latin-American that share a similar family centered culture. Therefore, the aim for this study is to analyze the longitudinal association of loneliness, social isolation, and their interactions, with the all-cause mortality among older adults in Mexico.
Methods
Study design
An observational retrospective cohort study was carried out in which Mexican adults older than 50 years were included. The exclusion criteria were the lack of information on rates of loneliness and social isolation. Subjects with incomplete information were excluded from the study.
Source of data
Data from the Mexican Health and Aging Study (MHAS) were used, which is a prospective cohort study initiated in 2001 with the aim of examining the aging process and its disease and disability burden; the study methodology has already been described previously [33, 34]. The MHAS has had several waves of data collection and evaluation as well as updating of the sample, in this study the data from the evaluation carried out in 2015 were used to obtain information on loneliness, social isolation and the rest of the sociodemographic, clinical, psychological and lifestyle characteristics. All-cause mortality information was obtained from the evaluation carried out in 2018. The MHAS was approved by the Institutional Review Boards and Ethics Committees of the University of Texas Medical Branch in the USA, the National Institute of Statistics and Geography (INEGI), and the National Institute of Public Health (INSP) in Mexico. The current study was approved by the National Institute of Geriatrics (DI-PI-007/2021).
Exposures
The exposure variables in this study were loneliness and social isolation, information from the 2015 wave was used.
Loneliness was assessed using the Revised UCLA Loneliness Scale (UCLA-LS) [35], which has been widely used in other studies [16, 27, 36], and its validity has also been evaluated elsewhere [37]. This scale has three items: 1) How often do you need company? 2) How often do you feel left out? 3) How often do you feel isolated? Each of the items admits answers from 1 “almost never” to 3 “often”. The total score of the three items results in an index with values from 3 to 9. Three categories are made: a score of 3 represents no loneliness (without); 4 to 5 mild loneliness; and, 6 to 9 severe loneliness, where 9, logically, indicates the most loneliness [38].
Social isolation was assessed by Berkman and Syme’s Social Network Index (SNI) [39]. The SNI is composed by four dichotomic items: housing, religious activity, groups, and closeness. 1) Housing: this item assigns a value of 1 to individuals with a couple and 0 to individuals without a couple. 2) Religious Activity: attending church at least once a month is given a value of 1, attending less than once a month or occasional attendance, receives a value of 0. 3) Groups: being an active member of any group, including religious ones, is given a value of 1, not being an active member of any group is given a value of 0. 4) Closeness: it assesses the number of relatives, kin, or close friends the person has. It produces a value from zero to three, where a value of 1 is given for being close with others and a value of 0 is given for not being close with others. The sum of the scores for these four individual items results in a final index. We used a reverse code to emphasize those who had higher scores as more isolated, where 0 represents a larger social network and 4 the absence of it. A value from 2 to 4 corresponds to an isolated individual, whereas a value of 0 or 1 speaks of an integrated individual. Cut-off points for evaluating social isolation were taken from Domènech-Abella J, 2019 [40].
Sociodemographic, clinical, psychological and lifestyle characteristics
For all Sociodemographic, clinical, psychological and lifestyle characteristics, the information from the 2015 wave was used.
The sociodemographic variables included in the study were age, weight and height (self reported), BMI, sex, socioeconomic level, years of schooling and the self-reported living alone status, for the living alone status, two categories were made. 1) Living alone: those without a couple or without anyone else living in the same household, and 2) Not living alone: those with a couple or other people living in the same household.
The self-reported clinical characteristics included in the study were comorbidities previously diagnosed by medical physicians (diabetes, hypertension, heart attack, lung chronic disease [asthma or emphysema], stroke and infectious diseases [including kidney infection, liver infection, tuberculosis, pneumonia and herpes or herpes zoster]), self-reported of activities of daily living affected or that need assistance (walking, bathing, eating, use of toilet, and getting into or out of bed) evaluated by the basic activities of daily living (ADL) questionnaire (categorized as one or more ADLs affected), [41]; self-reported of falls (defined as one or more falls in the las two years), hearing problems (defined as poor hearing or legally deaf), sight problems (defined as a poor sigh or legally blind), presence of limiting pain (defined as pain that limits the participant’s usual activities), unintentional weight loss (defined as unwanted weight loss of 5 Kg or more in the last two years), hospitalization (defined as frequency of hospitalizations in the previous year categorized as none hospitalization, one to five hospitalization and more than five hospitalizations.).
The psychological characteristics included in this study were depressive symptoms, cognition, emotional locus of control, and life satisfaction. Prescence depressive symptoms were assessed with the 9-item version of the Center of Epidemiological studies-Depression questionnaire (CESD-9) [42]. The cut- off point, validated for Mexican population, positive to depressive symptoms was a score of 5 or higher [43]. Cognition was measured with the Mexican version of the Cross-Cultural Cognitive Examination (CCCE) [44]. Emotional locus of control, defined as the individual’s beliefs regarding the extent which he or she is able to control or influence important life events including health outcomes [45], was measured with an adapted measure of Rotter’s scale [46], with values range from 4 to 16, where the higher the score the more he or she has a sense that he or she is in control of his or her own life. Satisfaction with life was measured using the response to the statement “I am satisfied with my life”, where she or he could agree, disagree, or remain neutral.
Lifestyle characteristics included were smoking and alcohol use. We classified the participants in three categories according to their smoking habits (has never smoked, former smoker, and current smoker) [47]; and according to daily alcohol intake considering the sex into: “Has never used” for people that have never consumed alcohol, “Currently doesn’t use or mild use”, “Moderate user” (1 alcoholic beverage for women per day and, 1 or 2 for men per day), and “Heavy user” (2 or more alcoholic beverage for women per day and, 3 or more for men per day) [48].
All-cause mortality
A face-to-face interview was conducted in all the homes of the participants during the year 2018, the interview was carried out with the relatives of the participant, and all-cause mortality during the 3-year follow-up period were registered, no loss to follow-up was recorded in the participants.
Statistical analysis
Descriptive data is presented as mean and standard deviation (SD) together with its standardized mean (Z score) for quantitative data, and as frequency and percentage for qualitative data. Comparisons of quantitative variables between groups of exposition were made by t-test and one-way Welch’s ANOVA, poshoc comparison were made by the Dunnett’s t test. Comparison of qualitative variables between groups of exposition were made by chi-square test. Comparison of all-cause mortality incidences between levels of loneliness and between socially integrated and socially isolated subjects were made by the chi-square test. Kendall, gamma and Spearman correlation analyzes were applied to determine the correlation between loneliness and social isolation scores, similarly, Cramer’s test was applied to determine the degree of association between the categories of loneliness and social isolation, and the variable living alone with loneliness and social isolation.
Univariate logistic regression analyzes were applied to determine the association of various social, clinical, and psychological characteristics with all-cause mortality; variables associated with all-cause mortality with a p value ≤0.05 were included for adjustment of a logistic regression model in which included the levels of loneliness, social isolation, and their interactions as all-cause mortality predictors. The model was adjusted for coviables that have previously shown an association with mortality in older adults: age, sex, schooling, more than one activity of daily living affected, presence of depressive symptoms, satisfaction with life, internal locus of control, multimorbidity (defined as 2 or more comorbidities present in the same participant), infectious diseases, falls, sight problems, hearing problems, limiting pain, smoking, alcohol consumption, unintended weight loss, hospitalization and living alone. A sensitivity analyses were conducted considering the loneliness as a binary variable (Without loneliness vs Mild and severe loneliness).
The assumptions of the multivariates models were verified by collinearity tests, residual analysis, and calculation of the goodness of fit. The results are summarized as Odds Ratio (OR) and 95% confidence intervals (95%CI).
A value of p < 0.05 was considered as statistical significance. No data imputations were performed. All analyzes were performed with Stata and SPSS v.21 statistical software.
Results
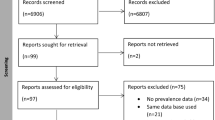
A total of 14,203 subjects were included in the study, of which 2490 were excluded. The final sample was 11,713 subjects. Figure 1 shows the flow chart for obtaining the final sample. The mean age was 66.6 (SD: 9.37) years. 58.2% (n = 6817) of the subjects were women. 86.7% of subjects had no prior hospitalizations, 9.5% of subjects had 1 to 5 prior hospitalizations, and only 3.9% of subjects had more than 5 prior hospitalizations. The incidence of all-cause mortality in the 3 years of follow-up was 6.0% (95%CI: 5.6–6.5) (n = 707).
The mean loneliness score was 4.03 (SD: 1.54, Z score: − 0.0035, Z score SD: 0.80), and the social isolation score was 1.65 (SD: 0.80, Z score: − 0.01, Z score SD: 0.99). Of the 11,713 participants, 42.05% presented some degree of loneliness, and 53.34% were classified as socially isolated.
Table 1 shows the sociodemographic, clinical, psychological and lifestyle characteristics in the total sample and according to the classification of loneliness and social isolation. As the level of loneliness increases, the financial situation is worse, similar in the presence of depressive symptoms, and satisfaction with life. The frequency of falls is also higher in subjects with some degree of loneliness. The situation is similar with participants with social isolation, a higher proportion of a poor financial situation is observed in isolated subjects, but not in the rest of the categories. The presence of depressive symptoms is higher in subjects with social isolation, but satisfaction with life is similar, as is the frequency of falls. The presence of multimorbidity increases with the level of loneliness, but it is not higher among subjects with social isolation. Unintentional weight loss is greater in subjects with greater loneliness, but only 3% greater in subjects with isolation than those who are socially integrated. Of the 5466 subjects with social isolation, only 17% live alone, like the 14 and 16% of subjects with mild or severe loneliness who live alone.
The incidence of all-cause mortality in participants without loneliness was 5.1% (95%CI: 4.6–5.6), in subjects with mild loneliness it was 6.1% (95%CI: 5.3–7.0), and in those with severe loneliness it was 9.2% (95%CI: 7.9–10.5) (p < 0.0001); and in the case of socially integrated subjects the incidence of all-cause mortality was 4.6% (95%CI: 4.0–5.1) and in subjects with social isolation it was 7.3% (95%CI: 6.7–7.9) (p < 0.0001). The incidence of all-cause mortality in subjects without loneliness and social integration was 4.1% (95%CI: 3.5–4.8), in participants without loneliness and social isolation was 6.1% (95%CI:5.3–6.9) in participants with mild loneliness and social isolation it was 7.4% (95%CI: 6.1–8.6) while in the participants with mild loneliness and social integrated it was 4.4% (95%CI:3.2–5.5), and in those with severe loneliness and social isolation it was 10.5% (95%CI: 8.8–12.2) while in the participants with severe loneliness and social integrated it was 7.0% (95%CI:5.1–8.8).
Correlation analyzes showed a significant correlation between loneliness and social isolation scores (gamma: 0.2, tau: 0.13, rho: 0.15; all p < 0.0001) indicating that when social isolation decreases, the feeling of loneliness decreases too. Loneliness and social isolation categories are weakly associated (Cramer’s V: 0.13, p < 0.0001), while living alone is moderately associated with loneliness (Cramer’s V: 0.15, p < 0.0001) and social isolation (Cramer’s V: 0.26, p < 0.0001).
Table 2 shows the results of the univariate logistic regression analyzes to determine the association of various sociodemographic, clinical, psychological, and lifestyle characteristics with all-cause mortality. All characteristics except financial status were associated in some way with all-cause mortality.
Table 3 shows the results of the logistic regression models to determine the effect of loneliness and social isolation, as well as their interactions with all-cause mortality, it was observed in the unadjusted model that severe loneliness (OR = 1.73, 95% CI: 1.24–2.40, p = 0.001) and social isolation (OR = 1.50, 95%CI: 1.21–1.87, p < 0.0001) were associated with a higher probability of death, however, no interaction was observed between loneliness and social isolation that was associated with increased all-cause mortality. After multivariate adjustment for the sociodemographic, clinical, psychological and lifestyle characteristics associated with all-cause mortality, it was observed that only social isolation (OR = 1.30, 95%CI: 1.03–1.64, p = 0.03) was the factor associated with a higher probability of all-cause mortality, and the interaction between loneliness and social isolation continued to have no effect on all-cause mortality. The sensitivity shows in the table 4, similar results were found, showing that the effect size of social isolation is not due to data segregation into 3 loneliness categories.
Discussion
In this retrospective observational study, we aimed to analyze the association of loneliness and isolation and their interaction with all-cause mortality in older adults, after multivariate adjustment for various covariates associated with all-cause mortality, we found that only social isolation was associated with an increased risk of all-cause mortality at a three-year follow-up, neither loneliness nor the interaction between loneliness and social isolation were associated with all-cause mortality.
Subjects with any degree of loneliness, as well as those with social isolation, presented higher proportions of alterations in mental health and physical health, other studies have also identified the risk of mental health problems such as depression, dementia, dissatisfaction with life, attempted suicide and abuse [49, 50], as well as greater alterations in physical health, since it has been found that participants with loneliness or isolation required more visits to the emergency room, hospital readmissions, risk of falls, and risk of malnutrition [4].
The cause of loneliness has been described in the theory of cognitive discrepancy, which indicates that loneliness is the cause of the mismatch between the actual quality and quantity of social interactions and those that the subject expects, this discrepancy can be caused by various social situations among them the same social isolation [51], this is the reason why loneliness and social isolation have been studied together, because they can be a synergistic or combined effect of isolation and loneliness, in our study we observed a relationship between both variables and we also have higher incidences of all-cause mortality when some level of loneliness was present in conjunction with social isolation, but when the risk of death is evaluated, through univariate logistic regression considering each variable together with its interaction, the association of loneliness and isolation with all-cause mortality was shown, but the interaction had no significant effect, the above is consistent with a lack of interdependence between these two aspects of socialization and support the idea that each one (loneliness and social isolation) has their own independent pathway to all-cause mortality. After multivariate adjustment, neither interaction nor loneliness had a significant effect on all-cause mortality, only social isolation was associated with increased mortality odds, these findings speak to those where the combined effect is not worse than experiencing either by itself [28, 29] and those of Gilmore and Ramage [52] who did not find a significant interaction between isolation and loneliness; and recently Ward et al. in 2021 showed that subjects with social isolation but not loneliness (HR = 1.37, 95%CI: 1.04–1.81) had the same mortality risk as subjects with loneliness and social isolation present at the same time (HR = 1.43, 95%CI:1.09–1.87) [5]; in the same line of thought, Stokes et al. in 2021, observed in a 10-year follow-up that only social isolation (HR = 1.13, 95%CI: 1.04–1.23) but not loneliness (HR = 1.05, 95%CI: 0.93–1.18) had a significant association with all-cause mortality [29]. Therefore, although social isolation and loneliness can coexist, and there is evidence showing that they may be correlated [53], it can be suggested that social isolation may be the cause of the increased risk of all-cause mortality.
The reasoning for which it has been considered that loneliness can predict mortality has been mainly mentioned the risk of physical inactivity, depression and defective immune functioning [54, 55] which are associated with worse outcomes or the development of diseases in older adults, on the other hand, a decrease in social interaction can affect the search for appropriate medical treatment, establish non-adherence to medications and, thus, developing unhealthy behaviors [56]. Also, socially isolated, or lonely older adults, have an increased perception of threats and vulnerability, this hypervigilance alters the psychological self-regulatory processes that influence physiologic functions, undermining sleep quality; the aforementioned, combined with unhealthy behaviors observed in socially isolated elderly such as smoking, drinking, obesity and physical inactivity [5], would increase the risk of morbidity and mortality [5, 26]. Studies showing a greater affinity of isolation with mortality than loneliness suggest that behaviors related to health care such as less use or access to medical care may be the cause of increased mortality [5], consistent with this, in our study we observed fewer hospitalizations of isolated participants than those with severe loneliness, which could suggest a relationship between this lack of medical care and the results we observed.
There are important cultural and socioeconomic moderators of the relationship between social isolation and loneliness, and health and mortality. On the one hand, evidence suggests cultural individualism or collectivism moderates the effect of loneliness on health and mortality. Individualism refers to valuing and striving for autonomy and placing one’s personal goals above those of others. Collectivism refers to seeing the interests of one’s group, such as one’s family or community, as more important than those of oneself [57]. Studies have found the effect of loneliness on health could be stronger in more collectivistic countries [58] like Latin American countries, current evidence shows that in Latin America loneliness has a small significant effect on mortality (HR = 1.13, 95%CI:1.01–1.26, I2 = 10.1%) [10], but without considering social isolation, that is why research in Latin America is urgent in order to have a complete vision of the effects of loneliness and social isolation on all-cause mortality.
In Mexico, the study of loneliness in older adults is relatively recent, the main findings are its association with chronic-degenerative diseases such as renal failure, diabetes, and hypertension [13], and regarding social isolation it was found, in a recent study, an association with all-cause mortality after a 12-year follow-up [59].
Our findings emphasize how important it is for social and health-care policy makers to develop effective intervention programs to reduce social isolation among older adults, especially considering the current context of the COVID-19 pandemic. Thus, it is critical to increase awareness about the impact that social isolation has on health to design interventions that can help older adults regain or maintain social activities and to develop strategies to remain socially connected [60].
The main limitation of this study was the lack of all-cause mortality follow-up dates and dates of the beginig of the exposition, which limited the performance of a Cox proportional hazards model, other limitations are the self-report of clinical characteristics such as diagnoses of comorbidities, activities of the daily life affected, history of fall, weight loss and previous hospitalizations, and there was also no medical information available at the time of the survey. In addition, the MHAS is a representative sample, but it is only representative of the Mexican population, therefore, more studies must be carried out in Latin American countries with which the findings of this study can be contrasted.
The strengths of this study is the large representative study sample from Mexico that allows a better estimation of the effect sizes controlling for various covariates, likewise, this study is one of the first and largest in a highly collectivistic as well middle-low-income country, implying that our findings may help resolve conflicts about the effect of loneliness and social isolation globally.
Conclusion
Social isolation, but not loneliness or their interaction, was associated with all-cause mortality in Mexican adults older than 50 years. This finding may help direct possible future interventions that help improve mental health in older adults from a highly collectivistic country.
Availability of data and materials
The datasets analyzed for this study are of public use and can be found in the Mexican Health an Aging Study (MHAS) website http://www.mhasweb.org/.
References
World Health Organization. World report on ageing and health [Internet]. 2015 [cited 2021 Sep 21]. Available from: https://www.apps.who.int/iris/handle/10665/186463.
Ceonsejo Nacional de Población. Proyecciones de la Población 2010-2050 [Internet]. México; 2012. Available from: http://www.conapo.gob.mx/work/models/CONAPO/Resource/1529/2/images/DocumentoMetodologicoProyecciones2010_2050.pdf.
CONEVAL. 2018. “Informe de Evaluación de la Política de Desarrollo social.” Recovered October 20th, from https://www.coneval.org.mx/Evaluacion/IEPSM/IEPSM/Documents/IEPDS_2018.pdf.
Freedman A, Nicolle J. Social isolation and loneliness: the new geriatric giants: approach for primary care. Can Fam Physician. 2020;66(3):176–82.
Ward M, May P, Normand C, Kenny RA, Nolan A. Mortality risk associated with combinations of loneliness and social isolation. Findings from the Irish longitudinal study on ageing (TILDA). Age Ageing. 2021;50(4):1329–35. https://doi.org/10.1093/ageing/afab004.
Moreno-Tamayo K, Manrique-Espinoza B, Ramírez-García E, Sánchez-García S. Social isolation undermines quality of life in older adults. Int Psychogeriatr. 2020;32(11):1283–92. https://doi.org/10.1017/S1041610219000310.
McHugh JE, Kenny RA, Lawlor BA, Steptoe A, Kee F. The discrepancy between social isolation and loneliness as a clinically meaningful metric: findings from the Irish and English longitudinal studies of ageing (TILDA and ELSA). Int J Geriatr Psychiatry. 2017;32(6):664–74. https://doi.org/10.1002/gps.4509.
Hawkley LC, Thisted RA, Masi CM, Cacioppo JT. Loneliness predicts increased blood pressure: 5-year cross-lagged analyses in middle-aged and older adults. Psychol Aging. 2010;25(1):132–41. https://doi.org/10.1037/a0017805.
Herrera-Badilla A, Navarrete-Reyes AP, Amieva H, Avila-Funes JA. Loneliness is associated with frailty in community-dwelling elderly adults. J Am Geriatr Soc. 2015;63(3):607–9. https://doi.org/10.1111/jgs.13308.
Gao Q, Prina AM, Prince M, Acosta D, Luisa Sosa A, Guerra M, et al. Loneliness among older adults in Latin America, China, and India: prevalence, correlates and association with mortality. Int J Public Health. 2021;66:604449. https://doi.org/10.3389/ijph.2021.604449.
INEGI. 2018. “Estadísticas a propósito del día internacional de las personas de edad (adultos mayores)” https://www.inegi.org.mx/contenidos/saladeprensa/aproposito/2018/edad2018_nal.pdf.
Montero-López M, Sánchez-Sosa JJ. La soledad como fenómeno psicológico: un análisis conceptual. Salud Mental. 2001;24(1):19–27.
Rivera-Ledesma A, Montero-López M, Sandoval R. Desajuste Psicológico, Calidad de Vida y Afrontamiento en Pacientes Diabéticos con Insuficiencia Renal Crónica en Diálisis Peritoneal. Salud Mental. 2012;35(4):329–37.
Cohen S, Doyle WJ, Skoner DP, Rabin BS, Gwaltney JMJ. Social ties and susceptibility to the common cold. JAMA. 1997;277(24):1940–4.
Ben Simon E, Walker MP. Sleep loss causes social withdrawal and loneliness. Nat Commun. 2018;9(1):3146. https://doi.org/10.1038/s41467-018-05377-0.
Lara E, Martín-María N, De la Torre-Luque A, Koyanagi A, Vancampfort D, Izquierdo A, et al. Does loneliness contribute to mild cognitive impairment and dementia? A systematic review and meta-analysis of longitudinal studies. Ageing Res Rev. 2019;52:7–16. https://doi.org/10.1016/j.arr.2019.03.002.
Erzen E, Çikrikci Ö. The effect of loneliness on depression: a meta-analysis. Int J Soc Psychiatry. 2018;64(5):427–35. https://doi.org/10.1177/0020764018776349.
VanderWeele TJ, Hawkley LC, Thisted RA, Cacioppo JT. A marginal structural model analysis for loneliness: implications for intervention trials and clinical practice. J Consult Clin Psychol. 2011;79(2):225–35. https://doi.org/10.1037/a0022610.
Stickley A, Koyanagi A, Roberts B, Richardson E, Abbott P, Tumanov S, et al. Loneliness: its correlates and association with health behaviours and outcomes in nine countries of the former Soviet Union. PLoS One. 2013;8(7):e67978. https://doi.org/10.1371/journal.pone.0067978.
Holt-Lunstad J, Smith TB, Baker M, Harris T, Stephenson D. Loneliness and social isolation as risk factors for mortality: a meta-analytic review. Perspect Psychol Sci. 2015;10(2):227–37. https://doi.org/10.1177/1745691614568352.
Valtorta NK, Kanaan M, Gilbody S, Ronzi S, Hanratty B. Loneliness and social isolation as risk factors for coronary heart disease and stroke: systematic review and meta-analysis of longitudinal observational studies. Heart. 2016;102(13):1009–16. https://doi.org/10.1136/heartjnl-2015-308790.
Steptoe A, Shankar A, Demakakos P, Wardle J. Social isolation, loneliness, and all-cause mortality in older men and women. Proc Natl Acad Sci U S A. 2013;110(15):5797–801. https://doi.org/10.1073/pnas.1219686110.
Julsing JE, Kromhout D, Geleijnse JM, Giltay EJ. Loneliness and all-cause, cardiovascular, and noncardiovascular mortality in older men: the Zutphen elderly study. Am J Geriatr psychiatry Am J Geriatr Psychiatry. 2016;24:475–84.
Mehrabi F, Béland F. Effects of social isolation, loneliness and frailty on health outcomes and their possible mediators and moderators in community-dwelling older adults: a scoping review. Arch Gerontol Geriatr. 2020;90:104119. https://doi.org/10.1016/j.archger.2020.104119.
Donovan NJ, Blazer D. Social isolation and loneliness in older adults: review and commentary of a National Academies Report. Am J Geriatr Psychiatry. 2020;28(12):1233–44. https://doi.org/10.1016/j.jagp.2020.08.005.
Beller J, Wagner A. Loneliness, social isolation, their synergistic interaction, and mortality. Health Psychol. 2018;37(9):808–13. https://doi.org/10.1037/hea0000605.
Yildirim Y, Kocabiyik S. The relationship between social support and loneliness in Turkish patients with cancer. J Clin Nurs. 2010;19(5–6):832–9. https://doi.org/10.1111/j.1365-2702.2009.03066.x.
Lennartsson C, Rehnberg J, Dahlberg L. The association between loneliness, social isolation and all-cause mortality in a nationally representative sample of older women and men. Aging Ment Health. 2021:1–8. https://doi.org/10.1080/13607863.2021.1976723.
Stokes AC, Xie W, Lundberg DJ, Glei DA, Weinstein MA. Loneliness, social isolation, and all-cause mortality in the United States. SSM - Ment Heal. 2021;1:100014. https://doi.org/10.1016/j.ssmmh.2021.100014.
Leigh-Hunt N, Bagguley D, Bash K, Turner V, Turnbull S, Valtorta N, et al. An overview of systematic reviews on the public health consequences of social isolation and loneliness. Public Health. 2017;152:157–71. https://doi.org/10.1016/j.puhe.2017.07.035.
Patterson AC. Does the mortality risk of social isolation depend upon socioeconomic factors? J Health Psychol. 2016;21(10):2420–33. https://doi.org/10.1177/1359105315578302.
Napier AD, Depledge M, Knipper M, Lovell R, Ponarin E, Sanabria E, et al. Cultural Contexts of Health and Well-being. Europe: World Health Organization; 2017.
Mexican Health and Aging Study (MHAS). Data Files and Documentation (public use): Mexican Health and Aging Study [Internet]. Available from: www.MHASweb.org.
Wong R, Michaels-Obregon A, Palloni A. Cohort profile: the Mexican health and aging study (MHAS). Int J Epidemiol. 2017;46(2):e2.
Russell D, Peplau LA, Cutrona CE. The revised UCLA loneliness scale: concurrent and discriminant validity evidence. J Pers Soc Psychol. 1980;39(3):472–80. https://doi.org/10.1037//0022-3514.39.3.472.
Rico-Uribe LA, Caballero FF, Olaya B, Tobiasz-Adamczyk B, Koskinen S, Leonardi M, et al. Loneliness, social networks, and health: a cross-sectional study in three countries. PLoS One. 2016;11(1):e0145264. https://doi.org/10.1371/journal.pone.0145264.
Trucharte A, Calderón L, Cerezo E, Contreras A, Peinado V, Valiente C. Three-item loneliness scale: psychometric properties and normative data of the Spanish version. Curr Psychol. 2021:1–9. https://doi.org/10.1007/s12144-021-02110-x.
Musich S, Wang SS, Hawkins K, Yeh CS. The impact of loneliness on quality of life and patient satisfaction among older. Sicker Adults. Gerontol Geriatr Med. 2015;1:2333721415582119. https://doi.org/10.1177/2333721415582119.
Musich S, Wang SS, Hawkins K, Yeh CS. The impact of loneliness on quality of life and patient satisfaction among older. Sicker Adults Gerontol Geriatr Med. 2015;1:2333721415582119.
Domènech-Abella J, Mundó J, Haro JM, Rubio-Valera M. Anxiety, depression, loneliness and social network in the elderly: longitudinal associations from the Irish longitudinal study on ageing (TILDA). J Affect Disord. 2019;246:82–8. https://doi.org/10.1016/j.jad.2018.12.043.
Newall NEG, Menec VH. Loneliness and social isolation of older adults: why it is important to examine these social aspects together. J Soc Pers Relat. 2019;36(3):925–39. https://doi.org/10.1177/0265407517749045.
Radloff LS. The CES-D scale: a self-report depression scale for research in the general population. Appl Psychol Meas. 1977;1(3):385–401. https://doi.org/10.1177/014662167700100306.
Aguilar-Navarro SG, Fuentes-Cantú A, Avila-Funes JA, García-Mayo EJ. Validity and reliability of the screening questionnaire for geriatric depression used in the Mexican health and age study. Salud Publica Mex. 2007;49(4):256–62. https://doi.org/10.1590/s0036-36342007000400005.
Glosser G, Wolfe N, Albert ML, Lavine L, Steele JC, Calne DB, et al. Cross-cultural cognitive examination: validation of a dementia screening instrument for neuroepidemiological research. J Am Geriatr Soc. 1993;41(9):931–9. https://doi.org/10.1111/j.1532-5415.1993.tb06758.x.
Angel RJ, Angel JL, Hill TD. Subjective control and health among Mexican-origin elders in Mexico and the United States: structural considerations in comparative research. J Gerontol B Psychol Sci Soc Sci. 2009;64(3):390–401. https://doi.org/10.1093/geronb/gbn029.
Rotter JB. Generalized expectancies for internal versus external control of reinforcement. Psychol Monogr. 1966;80(1):1–28.
Lazcano-Ponce E, Reynales-Shigematsu LM, Guerrero-López CM, Vallejo-Mateos A, Muños-Hernández JA, Barrientos-Gutiérrez T, et al. Encuesta Nacional de Adicciones 2011: tabaco. México: Cuernavaca; 2013.
Carrillo-Vega MF, Albavera-Hernández C, Ramírez-Aldana R, García-Peña C. Impact of social disadvantages in the presence of diabetes at old age. BMC Public Health. 2019;19(1):1013. https://doi.org/10.1186/s12889-019-7348-2.
Kuiper JS, Zuidersma M, Oude Voshaar RC, Zuidema SU, van den Heuvel ER, Stolk RP, et al. Social relationships and risk of dementia: a systematic review and meta-analysis of longitudinal cohort studies. Ageing Res Rev. 2015;22:39–57. https://doi.org/10.1016/j.arr.2015.04.006.
Wright-St Clair VA, Neville S, Forsyth V, White L, Napier S. Integrative review of older adult loneliness and social isolation in Aotearoa/New Zealand. Australas J Ageing. 2017;36(2):114–23. https://doi.org/10.1111/ajag.12379.
Burholt V, Scharf T. Poor health and loneliness in later life: the role of depressive symptoms, social resources, and rural environments. J Gerontol B Psychol Sci Soc Sci. 2014;69(2):311–24. https://doi.org/10.1093/geronb/gbt121.
Gilmour H, Ramage-Morin PL. Social isolation and mortality among Canadian seniors. Health Rep. 2020;31(3):27–38. https://doi.org/10.25318/82-003-x202000300003-eng.
Tomaka J, Thompson S, Palacios R. The relation of social isolation, loneliness, and social support to disease outcomes among the elderly. J Aging Health. 2006;18(3):359–84. https://doi.org/10.1177/0898264305280993.
Valtorta NK, Kanaan M, Gilbody S, Ronzi S, Hanratty B. Loneliness and social isolation as risk factors for coronary heart disease and stroke: systematic review and meta-analysis of longitudinal observational studies. Heart. 2016;102(13):1009–16. https://doi.org/10.1136/heartjnl-2015-308790.
Hakulinen C, Pulkki-Råback L, Virtanen M, Jokela M, Kivimäki M, Elovainio M. Social isolation and loneliness as risk factors for myocardial infarction, stroke and mortality: UK biobank cohort study of 479 054 men and women. Heart. 2018;104(18):1536–42. https://doi.org/10.1136/heartjnl-2017-312663.
Coyle CE, Dugan E. Social isolation, loneliness and health among older adults. J Aging Health. 2012;24(8):1346–63. https://doi.org/10.1177/0898264312460275.
Rokach A. The effect of gender and culture on loneliness: a Mini review. Emerg Sci J. 2018;2(2):59–64. https://doi.org/10.28991/esj-2018-01128.
Lykes VA, Kemmelmeier M. What predicts loneliness? Cultural difference between individualistic and collectivistic societies in Europe. J Cross-Cult Psychol. 2014;45(3):468–90. https://doi.org/10.1177/0022022113509881.
Moreno-Tamayo K, Juárez F, Manrique-Espinoza B, Mejía-Pailles G. The relationship between social isolation and mortality among adults aged 50 and older in a 12-year follow-up analysis in Mexico. Res Aging. 2022;44(9-10):758. https://doi.org/10.1177/01640275221078972.
Fakoya OA, McCorry NK, Donnelly M. Loneliness and social isolation interventions for older adults: a scoping review of reviews. BMC Public Health. 2020;20(1):129. https://doi.org/10.1186/s12889-020-8251-6.
Acknowledgements
Not applicable.
Funding
The MHAS (Mexican Health and Aging Study) is partly sponsored by the National Institute of Health/National Institute on Aging (grant number NIH R01AG018016) in the United States and the Instituto Nacional de Estadística y Geografía (INEGI) in Mexico. Publication of this article was supported by a grant from the Secretaría de Ciencia, Ciudad de México CM-SECTEI/200/2020 “Red colaborativa de Investigación Traslacional para el Envejecimiento Saludable de la Ciudad de México (RECITES).
Author information
Authors and Affiliations
Contributions
All authors gave final approval of the version to be published and agreed to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work were appropriately investigated and resolved. Conceptualization: CGP. Methodology: RRA, PRR, AKG and CGP Validation: PRR, LRLJ, SSG, PTV and CGP. Formal Analysis: AKG, RRA and CGP. Data Curation: AKG, RRA and CGP. Writing – Original Draft Preparation: AKG, PRR, SSG and CGP. Writing – Review & Editing: AKG, RRA, LRLJ, SSG, PTV and CGP. Supervision: CGP.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
The MHAS was approved by the Institutional Review Boards and Ethics Committees of the University of Texas Medical Branch in the USA, the Instituto Nacional de Estadística y Geografía (INEGI), and the Instituto Nacional de Salud Pública (INSP) in Mexico. This research have been performed in accordance with the Declaration of Helsinki and all the subjects provided written informed consent. The current analysis obtained research ethics approval from the Institutional Ethical Committee of the Instituto Nacional de Geriatría (DI-PI- 007/2021).
Consent for publication
Not applicable.
Competing interests
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/. The Creative Commons Public Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
About this article
Cite this article
Kammar-García, A., Ramírez-Aldana, R., Roa-Rojas, P. et al. Association of loneliness and social isolation with all-cause mortality among older Mexican adults in the Mexican health and aging study: a retrospective observational study. BMC Geriatr 23, 45 (2023). https://doi.org/10.1186/s12877-023-03750-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1186/s12877-023-03750-3