Abstract
Background
While benefit-risk (B-R) assessment in the real-world setting is an important challenge for pharmacovigilance, few studies have explored this approach. To investigate the utility and limitations of B-R assessment using a health care database by applying the Benefit Risk Action Team (BRAT) framework, we have conducted a case study with erythropoietin agents.
Methods
Postmarketing data from the Medical Data Vision health care database were used in a B-R comparison between methoxy polyethylene glycol-epoetin beta (continuous erythropoietin receptor activator; C.E.R.A.) and other erythropoiesis-stimulating agents (ESAs). Data were from patients with chronic kidney disease (CKD) treated with C.E.R.A. (n = 131: nondialysis, 109; hemodialysis, 22) or other ESAs (n = 542: nondialysis, 327; hemodialysis, 215) between July 2011 and March 2014.
Results
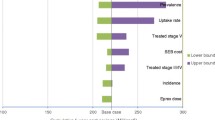
The B-R profile for C.E.R.A. appeared to be similar to that for other ESAs in both nondialysis and hemodialysis patients with CKD, when benefits and risks were mainly assessed in terms of odds ratios. Despite various point estimates and confidence intervals for each outcome, the results of subgroup analyses showed no notable differences from the overall analysis in B-R assessment.
Conclusions
B-R assessment can be performed using the BRAT framework with a health care database, but limitations exist when using a single data source. Care should be taken when selecting data for extraction and defining outcomes of interest. Further research is necessary to facilitate practical application of this approach.
Similar content being viewed by others
References
The CIRS-BRAT Framework. CIRS; http://www.cirs-brat.org/. Published 2014. Accessed March 16, 2016.
Coplan PM, Noel RA, Levitan BS, et al. Development of a framework for enhancing the transparency, reproducibility and communication of the benefit-risk balance of medicines. Clin Pharmacol Ther. 2011;89(2):312–315.
Levitan BS, Andrews EB, Gilsenan A, et al. Application of the BRAT framework to case studies: observations and insights. Clin Pharmacol Ther. 2011;89(2):217–224.
Noel R, Hermann R, Levitan B, et al. Application of the Benefit-Risk Action Team (BRAT) framework in pharmaceutical R&D results from a pilot program. Drug Inform J. 2012;46(6):736–743.
European Medicines Agency. Benefit-Risk Methodology Project. Work package 4 report: benefit-risk tools and processes. http://www.ema.europa.eu/docs/en_GB/document_library/Report/2012/03/WC500123819.pdf. Published May 9, 2012. Accessed March 16, 2016.
Liberti L, McAuslane N, Walker SR, et al. Progress on the development of a benefit/risk framework for evaluating medicines. Regulatory Focus. March 2010.
Sarac SB, Rasmussen CH, Rasmussen MA, et al. A comprehensive approach to benefit-risk assessment in drug development. Basic Clin Pharmacol Toxicol. 2012;111(1):65–72.
Felli JC, Noel RA, Cavazzoni PA. A multiattribute model for evaluating the benefit-risk profiles of treatment alternatives. Med Decis Making. 2009;29(1):104–115.
Christine EH, Hendrika AH, Shahrul MI, et al. Benefit-risk assessment in a post-market setting: a case study integrating real-life experience into benefit-risk methodology. Pharmacoepidemiol Drug Saf. 2014;23:974–983.
Müllerová H, Lu C, Li H, et al. Prevalence and burden of breathlessness in patients with chronic obstructive pulmonary disease managed in primary care. PLoS One. 2014;9(1):e85540.
Dregan A, van Staa TP, McDermott L, et al. Point-of-care cluster randomized trial in stroke secondary prevention using electronic health records. Stroke. 2014;45(7):2066–2071.
Petherick ES, Cullum NA, Pickett KE, Investigation of the effect of deprivation on the burden and management of venous leg ulcers: a cohort study using the THIN database. PLoS One. 2013;8(3):e58948.
Ueyama H, Hinotsu S, Tanaka S, et al. Application of a self-controlled case series study to a database study in children. Drug Saf. 2014;37(4):259–268.
Olesen JB, Lip GY, Lindhardsen J, et al. Risks of thromboembolism and bleeding with thromboprophylaxis in patients with atrial fibrillation: a net clinical benefit analysis using a “real world” nationwide cohort study. Thromb Haemost. 2011;106(4):739–749.
Friberg L, Rosenqvist M, Lip GY. Net clinical benefit of warfarin in patients with atrial fibrillation a report from the Swedish atrial fibrillation cohort study. Circulation. 2012;125(19):2298–2307.
Jarsch M, Brandt M, Lanzendorfer M, et al. Comparative erythropoietin receptor binding kinetics of C.E.R.A. and epoetin-beta determined by surface plasmon resonance and competition binding assay. Pharmacology. 2008;81(1):63–69.
Nakai S, Hanafusa N, Masakane I, et al. An overview of regular dialysis treatment in Japan (as of 31 December 2012). Ther Apher Dial. 2014;18(6):535–602.
Tsubakihara Y, Nishi S, Akiba T, et al. 2008 Japanese Society for Dialysis Therapy: guidelines for renal anemia in chronic kidney disease. Ther Apher Dial. 2010;14(3):240–275.
Akizawa T, Saito A, Gejyo F, et al. Impact of recombinant human erythropoietin treatment during predialysis periods on the progression of chronic kidney disease in a large-scale cohort study (Co-JET study). Ther Apher Dial. 2014;18(2):140–148.
European Medicines Agency. The European Union risk management plan for C.E.R.A. http://www.ema.europa.eu/docs/en_GB/document_library/EPAR_-_Scientific_Discussion/human/000739/WC500033669.pdf. Published 2007. Accessed March 16, 2016.
Marc P, Emmanuel B, Chao-Yin C, et al. A trial of darbepoetin alfa in type 2 diabetes and chronic kidney disease. N Engl J Med. 2009;361:2019–2032.
Japanese Society for Pharmacoepidemiology. The results of a survey of databases applicable to clinical epidemiology and pharmacoepidemiology in Japan. http://www.jspe.jp/mt-static/FileUpload/files/JSPE_DB_TF_E.pdf. Published October 2015. Accessed November 10, 2015.
Carol KR, Theodore C. Biostatistics in Clinical Trials. New York: Wiley; 2001.
Pagno M, Gauvreau K. Principles of Biostatistics. 2nd ed. Pacific Grove, CA: Duxbury Press; 2000.
Akizawa T, Saito A, Gejyo F, et al. Low hemoglobin levels and hypo-responsiveness to erythropoiesis-stimulating agent associated with poor survival in incident Japanese hemodialysis patients. Ther Apher Dial. 2014;18(5):404–413.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sugitani, Y., Udagawa, Y., Matsuda, S. et al. Postmarketing Benefit-Risk Assessment for Erythropoiesis-Stimulating Agents Using a Health Care Database. Ther Innov Regul Sci 50, 823–832 (2016). https://doi.org/10.1177/2168479016656029
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1177/2168479016656029