Abstract
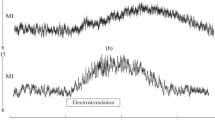
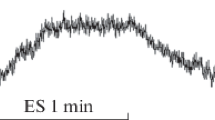
Changes in the blood flow in the skin of the plantar surface of the hallux were investigated by laser Doppler flowmetry in eight healthy subjects during transcutaneous electrical spinal cord stimulation (tESCS) with the pulse parameters used to activate locomotion. Continuous tESCS in the area of C5–C6 vertebrae did not cause significant changes in the blood flow, while electrical stimulation at T 12–T 1 and L 1–L 2 levels resulted in an increase in skin perfusion by 22–27%. Wavelet analysis of microcirculatory fluctuations showed that tESCS induced flaxomotions in the range of sensory peptidergic fibers and enhanced the amplitude of fluctuations of microcirculation in the endothelium-dependent range. These results suggest that tESCS stimulates microcirculation in the skin mainly due to antidromic stimulation of sensory peptidergic nerve fibers, which promotes activity of microvascular endothelium, vasodilator secretion, a decrease in vascular resistance, and an increase in microcirculation.
Similar content being viewed by others
References
Gerasimenko, Y., Gorodnichev, R., Moshonkina, T., et al., Transcutaneous electrical spinal-cord stimulation in humans, Ann. Phys. Rehabil. Med., 2015, vol. 58, no. 4, p. 225.
Shah, P., Sureddi, S., Alam, M., et al., Unique spatiotemporal neuromodulation of the lumbosacral circuitry shapes locomotor success after spinal cord injury, J. Neurotrauma, 2016, vol. 33, no. 18, p. 1709.
Gerasimenko, Y., Gorodnichev, R., Puhov, A., et al., Initiation and modulation of locomotor circuitry output with multisite transcutaneous electrical stimulation of the spinal cord in noninjured humans, J. Neurophysiol., 2015, vol. 113, no. 3, p. 834.
Dimitrijevic, M.R., Danner, S.M., and Mayr, W., Neurocontrol of movement in humans with spinal cord injury, Artif. Organs, 2015, vol. 39, no. 10, p. 823.
Cameron, T., Safety and efficacy of spinal cord stimulation for the treatment of chronic pain: A 20-year literature review, J. Neurosurg., 2004, vol. 100, p. 254.
Johnson, J.M., Minson, C.T., and Kellogg, D.L., Cutaneous vasodilator and vasoconstrictor mechanisms in temperature regulation, Compr. Physiol., 2014, vol. 4, no. 1, p. 33.
Grishin, A.A., Moshonkina, T.R., Solopova, I.A., et al., A five-channel noninvasive electrical stimulator of the spinal cord for rehabilitation of patients with severe motor disorders, Biomed. Eng., 2017, vol. 50, no. 5, p. 300.
Bogacheva, I.N., Moshonkina, T.R., Bobrova, E.V., et al., Effect of transcutaneous electrical spinal cord stimulation and mechanotherapy in the muscle activity regulation, Vestn. Tver. Gos. Univ., Ser. Biol. Ekol., 2015, no. 2, p. 7.
Krupatkin, A.I. and Sidorov, V.V., Funktsional’naya diagnostika sostoyaniya mikrotsirkulyatorno-tkanevykh sistem (Rukovodstvo dlya vrachei) (Functional Diagnostics of Microcirculatory Tissue System State (Handbook for Doctors)), Moscow: Librokom, 2013.
Bagno, A. and Martini, R., Wavelet analysis of the Laser Doppler signal to assess skin perfusion, Conf. Proc. IEEE Eng. Med. Biol. Soc., 2015, p. 7374.
Holowatz, L.A., Thompson-Torgerson, C.S., Kenney, W.L., et al., The human cutaneous circulation as a model of generalized microvascular function, J. Appl. Physiol., 2008, vol. 105, no. 1, p. 370.
Johnson, J.M., Pérgola, P.E., Liao, F.K., et al., Skin of the dorsal aspect of human hands and fingers possesses an active vasodilator system, J. Appl. Physiol., 1995, vol. 78, no. 3, p. 948.
Wu, M., Linderoth, B., and Foreman, R.D., Putative mechanisms behind effects of spinal cord stimulation on vascular diseases: A review of experimental studies, Auton. Neurosci., 2008, vol. 138, nos. 1–2, p. 9.
Foreman, R.D. and Linderoth, B., Neural mechanisms of spinal cord stimulation, Int. Rev. Neurobiol., 2012, vol. 107, p. 879.
Tanaka, S., Barron, K.W., Chandler, M.J., et al., Low intensity spinal cord stimulation may induce cutaneous vasodilation via CGRP release, Brain Res., 2001, vol. 896, nos. 1–2, p. 183.
Lobov, G.I. and Gurkov, A.S., Modulation of blood flow in the microvasculature of fingers after the formation a radiocephalic arteriovenous fistula, Nefrol. Dial., 2014, vol. 16, no. 3, p. 364.
Bayliss, W.M., On the origin from the spinal cord of the vasodilator fibers of the hind-limb and on the nature of these fibers, J. Physiol., 1901, vol. 26, nos. 3–4, p. 173.
Croom, J.E., Foreman, R.D., Chandler, M.J., and Barron, K.W., Cutaneous vasodilation during dorsal column stimulation is mediated by dorsal roots and CGRP, Am. J. Physiol., 1997, vol. 272, p. 950.
Darré, L. and Domene, C., Binding of capsaicin to the TRPV1 ion channel, Mol. Pharmaceutics, 2015, vol. 12, no. 12, p. 4454.
Walsh, D.A., Mapp, P.I., and Kelly, S., Calcitonin gene-related peptide in the joint: Contributions to pain and inflammation, Br. J. Clin. Pharmacol., 2015, vol. 80, no. 5, p. 965.
Wu, M., Komori, N., Qin, C., et al., Roles of peripheral terminals of transient receptor potential vanilloid-1 containing sensory fibers in spinal cord stimulationinduced peripheral vasodilation, Brain Res., 2007, vol. 1156, p. 80.
Author information
Authors and Affiliations
Corresponding author
Additional information
Original Russian Text © G.I. Lobov, N.A. Shcherbakova, R.M. Gorodnichev, A.A. Grishin, Y.P. Gerasimenko, T.R. Moshonkina, 2017, published in Fiziologiya Cheloveka, 2017, Vol. 43, No. 5, pp. 36–42.
Rights and permissions
About this article
Cite this article
Lobov, G.I., Shcherbakova, N.A., Gorodnichev, R.M. et al. Effect of transcutaneous electrical spinal cord stimulation on the blood flow in the skin of lower limbs. Hum Physiol 43, 518–523 (2017). https://doi.org/10.1134/S0362119717050103
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1134/S0362119717050103