Abstract
Quercetin (QC) is a dietary bioflavonoid that can be conjugated with nanoparticles to facilitate its brain bioavailability. We previously showed that quercetin-conjugated superparamagnetic iron oxide nanoparticles (QCSPIONs) reduced the level of blood glucose in diabetic rats. Glucose transporters (GLUTs), insulin-like growth factor-1 (IGF-1), and microRNA-29 (miR-29) play a critical role in brain glucose homeostasis. In the current study, we examined the effects of QCSPION on the expression of glucose metabolism-related genes, and the miR-29 family as a candidate regulator of glucose handling in the hippocampus of diabetic rats. Our in silico analyses introduce the miR-29 family as potential regulators of glucose transporters and IGF-1 genes. The expression level of the miR-29 family, IGF-1, GLUT1, GLUT2, GLUT3, and GLUT4 were measured by qPCR. Our results indicate that diabetes significantly results in upregulation of the miR-29 family and downregulation of the GLUT1, 2, 3, 4, and IGF-1 genes. Interestingly, QCSPIONs reduced miR-29 family expression and subsequently enhanced GLUT1, 2, 3, 4, and IGF-1expression. In conclusion, our findings suggest that QCSPION could regulate the expression of the miR-29 family, which in turn increases the expression of glucose transporters and IGF-1, thereby reducing diabetic complications.
Similar content being viewed by others
Introduction
Diabetes mellitus (DM) is the most prevalent disorder of the endocrine system which is recognized by hyperglycemia, resulting from defects in the secretion or/and function of insulin1. It has been shown that hyperglycemic conditions can strongly affect brain function. On the other hand, hypoglycemic shock induced by diabetes can lead to the central nervous system (CNS) dysfunction and brain cell death2. Glucose is the primary source of metabolic energy for the CNS and it goes across the plasma membrane of neurons with the help of glucose transporters (GLUTs)3,4. GLUT1, 2, 3, and 4 are widely distributed in the CNS, especially in the hippocampus, and play a vital role in brain glucose homeostasis5,6. GLUT1 is the main responsible for glucose transport from the blood–brain barrier (BBB) which is an insulin-independent and glucose insensitive GLUT. GLUT3 controls glucose absorption into the neuron7. Besides, the wide distribution of GLUT4, insulin and insulin-like growth factor-1 (IGF-1) receptors on the surface of neurons and glial cells showed that the brain is an insulin-sensitive organ8. A wide range of studies have shown that the expression, regulation, and activity of GLUTs can be disrupted during hyperglycemia4,9,10. These changes negatively affect glucose metabolism in the brain which results in impairing of synaptic plasticity, neurogenesis, and cognitive function11,12. Moreover, downregulation of neurotrophic factors such as IGF-1 was observed in the diabetic brain, which contributes to diabetic neurological disorders13,14. IGF-1 is a polypeptide hormone that is structurally and functionally homologous to insulin15,16. The biological activity of IGF-1 in the brain is done through its specific receptor (IGF-1R), which is expressed in different parts of the brain, including the hippocampus17. Like insulin, IGF-1 stimulates glucose absorption and metabolism in the brain. Interaction of IGF-1 with its receptor in different parts of the brain triggers the PI3K/Akt signaling pathway. PI3K/Akt signaling leads to translocation of GLUT4 to neuronal cell membranes, promoting glucose uptake into neurons18,19.
The role of microRNAs has been studied in diabetes and its complications20. Studies have highlighted the role of the microRNA-29 (miR-29) family in glucose homeostasis21. miR-29 family with three mature members of miR-29a, miR-29b, and miR-29c is a sensitive microRNA family to insulin deficiency and hyperglycemia22,23. The miR-29 family members with identical seed sequences target largely overlapping sets of genes24. Bioinformatics studies on the expression profile of miRNAs in diabetes show that GLUT1-4 and IGF-1 mRNAs are potential targets of the miR-29 family. Several studies have shown that GLUT1-4 and IGF-I genes are direct targets of the miR-29 family using different methods including in silico analyses, luciferase assay and qRT-PCR23,25,26,27,28,29. Studies in diabetic patients and animal models revealed that the expression of miR-29 family is increased in different tissues, including liver, pancreas, kidney, skeletal muscle, adipose tissue, and brain30,31,32,33,34,35,36,37. It is well known that miR-29 family negatively regulates the expression of GLUTs and IGF-1 in diabetic conditions23,29,38,39,40. Collectively, miR-29 family members can be considered as early markers of DM41.
Since the treatment of diabetes with chemical drugs have serious side effects, it is necessary to introduce exogenous antioxidants supplements, especially in the early stage of diabetes14. In this context, quercetin (QC) with the chemical formula C15H10O7 is identified as one of the most abundant flavonoid polyphenolic molecules in many fruits, vegetables, and seeds42. QC has beneficial effects on various diseases, such as cardiovascular disease, cancer, infection, diabetes, obesity, and neurological disorders43. There is strong evidence that QC improves hyperglycemia through a direct effect on gene expression at the transcriptional level and also by modulation of miRNAs as a part of the post-transcriptional gene regulation44. Although QC has multiple medicinal benefits, its low aqueous solubility, instability in the physiological environment, and poor bioavailability have restricted the use in clinical application45. Therefore, to overcome these limitations, it is necessary to develop a system that could protect QC against enzymatic degradation and provide an elevated pool of it in the body tissues, especially in the CNS42. Superparamagnetic iron oxide nanoparticles (SPIONs) are well accepted as an effective drug delivery system because of their unique size, colloidal stability, crossing the BBB, bio-distribution, and good safety profile46. Besides, SPIONs are magnetic targeted carriers (MTC) that can be localized in certain tissue under an external magnetic field. Currently, there are multiple FDA-approved magnetite-based nanoparticles, as well as numbers of applicable SPIONs are ongoing47. Application of the quercetin-conjugated superparamagnetic iron oxide nanoparticles (QCSPIONs) in animal models and cell culture has led to considerable results in our previous studies. In this regard, we reported that exposing PC12 cells to QCSPIONs (10 − 100 μg mL−1) caused a remarkable outgrowth of neurite and enhanced the neuronal branching complexity better than pure QC48. We reported that the antitoxic activity of SPIONs such as the catalase-like activity remained unchanged after conjugation in H2O2-induced toxicity condition of PC12 cells49. We also suggested that the concentration of QC in the brains of QCSPION-treated healthy rats was about 4.8 times for 50 mg kg−1 of QC and 8.6 times for 100 mg kg−1 of QC higher than rats treated with pure QC. Therefore, it can be concluded that SPIONs improve the bioavailability of QC and its passage through the BBB50. Besides, we showed that treatment with both QC and QCSPIONs (50 mg kg−1 and 100 mg kg−1) had no effect on hepatic GSH, TAC, MDA levels, and CAT activity of healthy rats51. In another study, we showed that treatment with QCSPIONs (50 and 100 mg kg−1) during 1 week improved memory performance in healthy rats better than pure QC via their interaction with proteins involved in Long-Term Potentiation (LTP)52. Because of the causal role of diabetes in CNS disorders especially cognitive dysfunction and dementia, we used QCSPIONs to reduce the effects of diabetes on learning and memory. We showed that oral delivery of QCSPIONs (25 mg kg-1) reduced blood glucose level and ameliorate learning and memory impairment of diabetic rats53. We focused on inflammation and oxidative stress as the underlying molecular mechanisms of these effects and reported that QCSPIONs could improve learning and memory impairment through targeting NF-κB/miR-146a and Nrf2/miR-27a pathways54,55. In the current study, we targeted GLUTs (GLUT1, GLUT2, GLUT3, and GLUT4), IGF-1, and miR-29 family as other classical targets of QCSPIONs in diabetic condition. Although several experimental studies have shown the role of GLUTs, IGF-1, and miR-29 family in the pathogenesis of diabetic complications, there is no enough knowledge about the effect of QC and QCSPIONs on the modulation of these genes. Thus, the purpose of the current study was to compare the effect of QC and QCSPIONs on the expression of GLUT1, GLUT2, GLUT3, GLUT4, and IGF-1 genes, as well as miR-29 family in the hippocampus of diabetic rats.
Results
In silico analyses introduce the miR-29 family as a potential regulator of GLUTs and IGF-1
At the first step, we prepare a list of miRNAs that are involved in DM through a comprehensive literature review (Table 1)56,57,58,59. The miRNAs which were reported in different tissues relating to type 1 diabetes (T1D) at least in two studies were selected. Then, miRWalk 2.0 (http://zmf.umm.uni-heidelberg.de/apps/zmf/mirwalk2/custom.html), a target prediction resource that uses several miRNA target prediction tools and TargetScan 7.2 (http://www.targetscan.org/vert_72/) were used for prediction of miRNAs which target the 3′UTR region of GLUT1, 2, 3, 4 and IGF-1 genes. The analysis was limited to the target 3′UTR region of GLUT2, 3, 4, and IGF-1 genes of the rat because despite human GLUT1 data, no data is referring to rat GLUT1 gene in two databases. Our results indicate that GLUT 3, 4, and IGF-1 genes are targeted by miRNA-29a, miRNA-29b, and miRNA-29c. Furthermore, miRNA-29a can target the GLUT2 gene (Fig. 1). Finally, three miRNAs of the miR-29 family including, miRNA-29a, miRNA-29b, and miRNA-29c were filtered for further experimental investigations concerning their roles in diabetes and targeting four target genes.
Potential regulation of glucose transporters and IGF-1 by miR-29 family. Among all miRNAs which target the GLUT1, 2, 3, 4, and IGF-1 genes, three members of the miR-29 family can target commonly all GLUT3, 4, and IGF-1 genes. GLUT2 is also targeted by miRNA-29a. Cityscape 3.8.0 (https://cytoscape.org/release_notes_3_8_0.html) was used for network representation.
QC and QCSPIONs significantly reduce the expression of the miR-29 family in the hippocampus
The expression levels of the miR-29 family (miR-29a, miR-29b, miR-29c) in the hippocampus of the studied groups are shown in Fig. 2. One-way ANOVA analysis indicated that expression levels of miR-29a and miR-29c were increased more than threefold and miR-29b more than twofold in the diabetic group (p < 0.0001 for miR-29a, b, c). Treatment with pure and conjugated forms of QC significantly reduced the expression level of miR-29a (p < 0.001 for Q and p < 0.0001 for QCSPIONs), miR-29b (p < 0.001 for Q and QCSPIONs), and miR-29c (p < 0.0001 for Q and QCSPIONs) in the hippocampus of diabetic rats. What is interesting in this data is that the most significant effect was observed in the QCSPIONs treated group so that the expression levels of miR-29 family in QCSPIONs rats were significantly lower than those that received pure QC.
Effect of QC and QCSPIONs treatment on miR-29 family. (A) miR-29a, (B) miR-29b, (C) miR-29c in the hippocampus of diabetic rats. Data are mean with SEM (n = 5 per group). **P < 0.01, ***P < 0.001 and P < 0.0001 vs DC group (One-way ANOVA, Tukey’s multiple comparison tests). #P < 0.05, ##P < 0.01 vs QCSPION group. NDC non-diabetic control, DC diabetic control, DC + SPION diabetic treated with superparamagnetic iron oxide nanoparticle, DC + QC diabetic treated with quercetin, DC + QCSPION diabetic treated with quercetin-conjugated superparamagnetic iron oxide nanoparticle.
QC and QCSPIONs significantly increase the expression of GLUTs in the hippocampus
Real-time PCR results derived from mRNA expression levels of GLUT1, GLUT2, GLUT3, and GLUT4 in the hippocampus of diabetic rats are represented in Fig. 3. The expression levels of GLUT1, GLUT2, GLUT3, and GLUT4 in the hippocampus of diabetic rats were decreased significantly compared to the control group (P < 0.0001 for GLUT1-4). As shown in Fig. 3, after treatment with QC, expression levels of all studied GLUTs were increased significantly (P < 0.0001 for GLUT1, P < 0.01 for GLUT2, P < 0.01 for GLUT3, and P < 0.0001 for GLUT4). Moreover, we found that QCSPIONs were able to increase the expression of GLUT2, GLUT3, and GLUT4 up to a normal level more effectively than pure QC (P < 0.0001 for GLUT2, P < 0.001 for GLUT3, and P < 0.0001 for GLUT4). What is interesting in these results is that expression levels of all studied GLUTs in QCSPIONs rats were significantly higher than those that received pure QC.
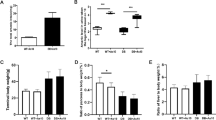
Effect of QC and QCSPIONs treatment on mRNA levels of glucose transporters. (A) GLUT1, (B) GLUT2, (C) GLUT 3, (D) GLUT4 in the hippocampus of diabetic rats. Data are mean with SEM (n = 5 per group). **P < 0.01, ***P < 0.001 and P < 0.0001 vs DC group (One-way ANOVA, Tukey’s multiple comparison tests). ##P < 0.01, ###P < 0.001 vs QCSPION group. NDC non-diabetic control, DC diabetic control, DC + SPION diabetic treated with superparamagnetic iron oxide nanoparticle, DC + QC diabetic treated with quercetin, DC + QCSPION diabetic treated with quercetin-conjugated superparamagnetic iron oxide nanoparticle, GLUT glucose transporter.
QC and QCSPIONs significantly increase the expression of IGF-1 in the hippocampus
As shown in Fig. 4, the expression level of IGF-1 was decreased significantly in the hippocampus of diabetic rats compared to the control group (P < 0.001). The comparison between groups showed that treatment with QC and QCSPIONs led to a significant increase in IGF-1 mRNA expression level compared to the diabetic group (P < 0.05 for Q and QCSPIONs).
Effect of QC and QCSPIONs treatment on mRNA level of IGF-1 in the hippocampus of diabetic rats. Data are mean with SEM (n = 5 per group). *P < 0.05, ***P < 0.001 vs DC group (One-way ANOVA, Tukey’s multiple comparison tests). NDC non-diabetic control, DC diabetic control, DC + SPION diabetic treated with superparamagnetic iron oxide nanoparticle, DC + QC diabetic treated with quercetin, DC + QCSPION diabetic treated with quercetin-conjugated superparamagnetic iron oxide nanoparticle.
Discussion
Diabetes causes secondary pathophysiological changes in the brain and diabetic patients are significantly more likely to develop cognitive impairment. QC has the potential to treat glucose metabolism disorders in DM and has been considered as a promising drug combination to reduce diabetes complications43. In a previous report, we showed that dextran-coated superparamagnetic iron oxide nanoparticles with minimal toxicity improve learning and memory impairment in diabetic rats better pure QC even at concentrations below pure QC53. The goal of the current study is assessment of glucose metabolism-related genes and the miR-29 family as one of the classical targets of QCSPIONs in diabetic conditions (Fig. 5).
First, miRNA-mRNA interaction of glucose transporters genes,IGF1 gene and miR-29 family was predicted. Then, the anti-diabetic and neuroprotection effects of QC and QCSPION on the expression of miR-29 family in the hippocampus of diabetic rats were detected. Real-time PCR results show that the expression levels of miR-29a and miR-29c in the hippocampus of diabetic rats were increased more than threefold and miR-29b more than twofold in comparison to the control group. Several studies have shown that the expression of miR-29 family is increased by hyperglycemia and proinflammatory cytokines, which are two main hallmarks of diabetes41. Upregulation of miR-29 is a key factor in the loss of pancreatic beta cells and development of the first stage of T1D41. As we reported in our previous study, induction of diabetes for fifty days destroyed pancreatic beta cells and significantly increased blood glucose level in rats. Besides, we showed that levels of inflammatory cytokines such as TNF-α increased in the hippocampus of diabetic rats54. Therefore, it can be concluded that increased expression of miR-29 can be due to hyperglycemia and the presence of inflammatory markers. These findings are in agreement with studies conducted on cell cultures and diabetic models that indicated upregulation of miRNA-29a-c in different tissues. In this regard, a study by Li et al. in 2017 showed that inhibition of IGF-1 expression by the miR-29 family led to myocardial apoptosis and cardiovascular complications in diabetic rats27. Massart et al. in 2017 reported that overexpression of miR-29a and miR-29c in cultured human skeletal muscle primary cells impaired glucose metabolism by decreasing GLUT1 expression38. Hirata et al. in 2017 showed that increased expression of miR-29a and miR-29b led to downregulation of GLUT2 expression in the pancreas of NONcNZO10/LtJ mice29. The result of a study conducted by Esteves et al. in 2018 showed that upregulation of miR-29b-3p and miR-29c-3p led to reduction of GLUT4 expression by 50 to 77% in the skeletal muscle of diabetic rat23.
Our results indicate that treatment with QC in both pure and conjugated forms normalized the upregulation of miR-29 family. Despite several studies regarding the modulation effect of QC on miRNA expression in different pathological conditions60, no study has been investigated the effect of this flavonoid on miR-29 family expression. However, it can be proposed that the reduced expression of miR-29 family is the result of modulation effect of QC on miRNAs expression as a part of the post-transcriptional gene regulation and direct effect of QC on the reduction of hyperglycemia and proinflammatory cytokines, and regeneration of islets of Langerhans61,62. Anti-diabetic effects of QC in pure and it's compound with other agents have been reported through the regeneration of the pancreatic islets, increasing insulin secretion, inhibition of Glucose-6-phosphatase, augmenting liver glycogen content, and stimulation of GLUT expression and translocation43,63.
In the current study, GLUTs mRNA levels were decreased in the hippocampus of diabetic rats. It is well studied that majority of glucose absorption in the hippocampus is mediated through GLUT1 which is expressed in microvessels, as well as GLUT2 and GLUT3 that are highly expressed in pyramidal cells located in the CA3 and dentate gyrus5,64,65. In addition, GLUT4 is an insulin-sensitive glucose transporter and exhibits overlapping distributions with the insulin receptor and IGF-1 receptor in the hippocampus of the rodent brain9,66. Here, we observed a significant reduction in expression levels of GLUTs 1, 2, 3, and especially GLUT4 in the hippocampus of diabetic rats compared to untreated diabetic rats. Among various GLUT levels evaluated, GLUT4 were significantly decreased in the brain of diabetic rats. Since the production of insulin in diabetic rats is less, the insulin-dependent GLUT4 is reduced more than other GLUTs in this condition. Among various GLUT levels evaluated, GLUT2 expression showed the lowest decrease in hyperglycemic condition, which could be due to the high sensitivity of this glucose transporter to glucose concentration and a compensatory mechanism for severe depletion of other GLUTs. These results are in line with previous reports. In this regard, Bakirtzi et al. in 2009 showed that GlUT4 in the brain is sensitive to insulin level and neuronal insulin resistance stimulates GLUT4 translocation to the plasma membrane to promote glucose uptake67. Sun et al. in 2018 revealed that the expression levels of GLUT3 decreased in adult hippocampal stem cells affected by STZ, which reduced their differentiation potential68. Moreover, Choi et al. in 2019 reported that GLUT1 expression level in the hippocampus of mice administered with STZ and fed with a high-fat diet was decreased, while they showed that hippocampal expression of GLUT2 was increased in diabetic rats69.
In this study, QC and QCSPIONs were able to increase the expression of GLUT2, GLUT3, and GLUT4 up to normal levels. Due to the direct effect of QC on the regeneration of pancreatic beta cells and subsequent insulin production, the expression of GLUT4 increased more than other GLUTs under QC treatment. Our results are in agreement with reports that have indicated that QC supplementation and other flavonoids can greatly regulate the expression level of GLUTs in the brain. In this regard, Eid et al. in 2015 showed that QC treatment in culturing L6 skeletal muscle cells resulted in the transfer of GLUT4 to the cell surface and increase glucose uptake by activation of AMPK70. Mehta et al. in 2017 showed that chronic stress decreased the expression of insulin receptor and GLUT4 in the hippocampus of mice. QC improved the disruption of the insulin signaling pathway and increased GLUT4 expression and insulin receptors of the hippocampus71. In the same year, Sandeep et al. showed that expression levels of GLUT1, GLUT2, GLUT3, and GLUT4 were reduced in the brain of diabetic rats. QC supplement was able to greatly increase the level of GLUTs and the main components involved in the insulin signaling pathway72. Besides, Eldamarawi et al. in 2020 showed that cotreatment of QC with metformin reduced hyperglycemia and insulin resistance by increasing the expression of GLUT-4 through neutralizing oxidative stress and inflammatory states in skeletal muscles and adipose tissue of diabetic rats73.
Moreover, the results of our study indicate that the expression of hippocampal IGF-1 in the diabetic group is significantly lower than the control group. These results are in accordance with a study by Ola et al. that reported the downregulation of IGF-1 in the brains of diabetic rats14. Furthermore, Zebrowska et al. reported that serum concentration of IGF-1 significantly reduced in patients with T1D74. A number of studies suggest that insulin has a regulatory role in the synthesis of IGF-1. Through an upregulation of hepatic growth hormone (GH) receptor expression, insulin increases the hepatic sensitivity for GH stimulation in the production of IGF-1. Insulin also increases IGF-I mRNA concentrations directly by increasing transcript stability75,76. Therefore, decreased expression of IGF-1 can be attributed to insulin deficiency in diabetes. IGF-1 induces growth, proliferation, differentiation, survival, and stability of neurons, as well as stimulates neuronal glucose uptake77,78. The IGF-1 signaling pathway is also responsible for controlling the phosphorylation of tau protein. The decrease in IGF-1 and disruption of the signaling pathway lead to tau hyperphosphorylation and neuronal death79. On the other hand, reducing the expression of IGF-1 under hyperglycemic conditions led to a decrease in the glucose uptake through GLUT4 in neurons by affecting on translocation of this glucose transporter78.
Here, IGF-1 mRNA level was increased in diabetic rats after oral administration of QC and QCSPIONs. Our results are in agreement with reports which have indicated that flavonoids can greatly regulate the expression level, synthesis, and secretion of neurotrophic factors in the brain. In this regard, Ola et al. demonstrated that treatment with morin increases the expression level of IGF-1 in the brain of diabetic rats14. Isik et al. also showed that level of IGF-1 increased after treatment with curcumin in diabetic rats80. To the best of our knowledge, there is no report evaluating QC on IGF-1 expression level.
Conclusion
In general, our results showed that hyperglycemia can dysregulate the miR-29 family that may be the reason for the downregulation of the genes involved in glucose transport. Because in silico analysis in this study and experimental results in other studies have shown that IGF-1 and GLUTs are the direct targets of the miR-29 family, it can be concluded that miR-29 family dysregulation may be a reason for the downregulation of these genes. QC in pure and particularly conjugated with SPIONs leads to normalization level of these microRNAs and consequently the target genes. Based on the results, we propose that oral treatment of QCSPIONs can improve glucose homeostasis disorder via regulation of miR-29 family expression and increasing GLUTs and IGF-1 gene expression levels. Overall, conjugation of flavonoids such as QC with superparamagnetic nanoparticles can be a promising clinical path against CNS complications caused by diabetes in the future.
Methods
Animals
Male Wistar rats weighing 200–230 g (40 animals) were bought from the Royan Institute (Isfahan, Iran) and housed for 2 months at 25 °C ± 2 °C with 40–50% humidity under a 12 h light/dark cycle with free access to food and water. All maintenance, handling, experiments, and tissue collection were performed following the guidelines for the care and use of laboratory animals (USA National Institute of Health Publication No 80–23, revised 1996) and in compliance with the ARRIVE guidelines (http://www.nc3rs.org.uk/page.asp?id=1357) and were approved by the animal ethics committee of the University of Isfahan.
Induction of diabetes and experimental design
Diabetes induction and experimental design were elaborated by our colleagues in a previous study53. Briefly, T1D was induced by intraperitoneal injections of 20 mg kg−1 STZ on 5 consecutive days. In order to confirm the incidence of T1D in the rats, blood samples were taken from the tail vein after the last injection of STZ and glucose levels measured by a glucometer. All STZ-treated rats revealed fasting glycemia over 250 mg dL−1 and are used in our study.
All rats were randomly divided into five groups (8 animals each):
Control group: Rats in the control group receive deionized water (DI) for 35 days.
Diabetes group: Rats in the diabetic group receive deionized water (DI) for 35 days.
QC group: Rats in the diabetic group treated with 25 mg kg-1 of free QC solution for 35 days.
SPIONs group: Rats in the diabetic group were treated with 25 mg kg-1 Fe3O4 NPs for 35 days.
QSPIONs group: Rats in the diabetic group were treated with 25 mg kg-1 QCFe3O4 NPs for 35 days.
All of the treatments were dissolved in deionized water (DI) immediately before administration and gavaged in separate groups of rats 5 days after the last injection of STZ. The dose and duration of quercetin were selected based on previous studies that revealing beneficial effects of quercetin on diabetic complication81,82,83,84. In order to evaluate the effect of treatments on the blood glucose levels, the blood glucose levels were measured seven times: two times before the onset of treatment, the onset of treatment, and four times after the treatment at intervals of ten days. At the end of the experiment, all animals were sacrificed by ketamine-xylazine anesthesia (100 mg/kg ketamine,10 mg/kg xylazine). The hippocampus was removed from the hemispheres and kept at − 70 °C until use.
Synthesis of QCSPIONs
QCSPIONs were synthesized by our colleagues in a previous study. In summary, the synthesis of dextran-coated superparamagnetic iron oxide nanoparticles was performed by using the chemical co-participation (CPT) method. For this purpose, 1.135 gr of anhydrous FeCl3 with 0.695 gr of FeCl2 was dissolved in 200 mL DI water. After complete mixing, some ammonia solution was added to the mixture at 70 °C and stirred for 1 h until the pH of the solution reached nine. In the next step, 0.45 gr of dextran was dissolved in 50 mL water and then added to the above mixture. The mixture was stirred continuously for two hours at 90 °C and then by an external magnet, the resultant dextran-coated superparamagnetic iron oxide nanoparticles were collected. After washing with DI water and ethanol, the nanoparticles were dehydrated in an oven at 70 ºC overnight. To prepare QCSPIONs, QC was added to dextran-coated superparamagnetic iron oxide nanoparticles and EDC/NHS was used as a linker. Then, synthesized QCSPIONs were sequestered from suspension by a magnet. After washing with DI water, and acetone and QCSPIONs were dehydrated using a freeze drier.
RNA extraction
To extract RNA, 50–100 mg of hippocampus tissue was used for each sample. Tissue samples were squashed in a sterile petri dish, and then total RNA (including messenger RNA and microRNA) was extracted using TRIzol (Invitrogen, Life Technologies, Grand Island, NY, USA) according to the manufacturer’s protocol. The destructed tissue in TRIzol solution was completely homogenized by repetitive pipetting using a syringe 2.5 cc with a needle 21 g. The quantity and quality of extracted RNA were assessed using a nanodrop spectrophotometer (Thermo Fisher Scientific, USA). The integrity of the extracted RNA was checked by 18 s and 28 s ribosomal bands on 1% agarose gel, stained with GelRed, without the presence of extra bands. Before the formation of cDNA, 1 μg of the extracted RNA was treated with 1 U RNase-free DNase I (Thermo Fisher Scientific Inc, USA) to remove the contamination of DNA in RNA samples. All steps of the experiment were performed under a laminar hood and by using RNase-free gloves, tubes, and strips to prevent RNA degradation.
cDNA synthesis
500 ng treated RNA with DNase I, was used for cDNA synthesis using a cDNA synthesis kit (Takara, Japan). The reaction in a final volume of 10 μL containing 500 ng RNA, 2 μL 5 × prime script buffer, 0.5 μL RT enzyme, 0.5 μL oligo dT primer, 0.5 μL random 6mer was incubated at 37 °C for 15 min, and at 85 °C for 5 s.
Moreover, cDNA synthesis for microRNA was performed using BON-miR miRNA 1st-strand kit (Bonyakhteh, Tehran, Iran, Cat No # BON209001) through polyadenylation. Briefly, elongation of microRNAs was performed in a polyadenylation reaction, with a final volume of 20 μL at 37 °C for 30 min. Then the reaction to make cDNA was performed immediately after polyadenylation reaction and using the existing compounds in BON-miR miRNA 1st-Strand cDNA Synthesis Kit, for each sample of polyadenylated RNA.
Real-time PCR
Gene transcripts were measured in Real-time PCR, using 2 × Master Mix Green (Ampliqon Odense, Denmark). In order to normalize levels of mRNA and microRNA expression, β-actin and Snord-47 genes were selected as reference genes respectively. As the expression level of these genes is stable relative to changes in glucose and stable in different tissues, they are good choices for analysis of mRNA and microRNA expression. Primer genes of this study were designed using the online software of OligoArchitect (www.oligoarchitect.com/LoginServlet), and then their specificity was examined on the NCBI website (www.NCBI. nlm.nih.gov/blast). The best primers were selected and purchased from Bioneer Company (City, Korea). Sequences of the primers used in this study are listed in Table 2. qPCR reaction to measure the expression level of mRNA was performed in a final volume of 10 μL, containing 5 μL SYBR Green 1 μL cDNA, 0.5 μM of 10 pM forward, 0.5 μM of 10 pM reverse primers. The reaction performed under the condition of 15 s at 95 °C as the first denaturation step, followed by 39 cycles at 95 °C for 15 s and 57 °C for 30 s, and 72 °C for 15 s.
Forward and reverse primers for microRNA were designed and synthesized by Bonyackteh Company (Bonyakhteh, Tehran, Iran). qPCR reaction was carried out in a final volume of 13 μL, containing 1 μL cDNA, 0.5 μL miRNA specific forward primer, 0.5 μL universal reverse primer, 6.5 μL qPCR master mix. After the initial denaturation step at 95 °C for 2 min, the reaction was performed as 40 cycles at 95 °C for 5 s and 60 °C for 30 s. The development of PCR steps was specified by measuring the intensity of light emitted from SYBER Green at the end of the elongation phase. At the end of the reaction, the specificity of products for PCR reaction was confirmed by analyzing the melting curves. The concentration of primers, cDNAs, the efficiency of primers, and conditions of PCR was optimized. Gene expression was calculated using the 2−ΔΔCT method.
Statistical analyses
The results were reported as mean ± SEM and analyzed by using the GraphPad Prism software package (GraphPad Software Inc., San Diego, CA, USA). Groups were compared by one-way ANOVA followed by Tukey’s multiple comparison tests or Student’s t-test. Value of p < 0.05 was considered to be statistically significant.
References
Rom, S. et al. Hyperglycemia-driven neuroinflammation compromises BBB leading to memory loss in both diabetes mellitus (DM) type 1 and type 2 mouse models. Mol. Neurobiol. 56, 1883–1896 (2019).
Cryer, P. E. Hypoglycemia, functional brain failure, and brain death. J. Clin. Investig. 117, 868–870 (2007).
Bronisz, A., Ozorowski, M. & Hagner-Derengowska, M. Pregnancy ketonemia and development of the fetal central nervous system. Int. J. Endocrinol. https://doi.org/10.1155/2018/1242901 (2018).
Leão, L. L. et al. Does hyperglycemia downregulate glucose transporters in the brain?. Med. Hypotheses 139, 109614 (2020).
Reznikov, G. P. C. G. L. & Reagan, L. 19 Expression and Functional Activities of Glucose Transporters in the Central Nervous System (Neural Membranes and Transport, 2007).
Sayem, A. S. M. et al. Action of phytochemicals on insulin signaling pathways accelerating glucose transporter (GLUT4) protein translocation. Molecules 23, 258 (2018).
Simmons, R. A. Fetal and Neonatal Physiology 428–435 (Elsevier, Amsterdam, 2017).
Arrieta-Cruz, I. & Gutiérrez-Juárez, R. The role of insulin resistance and glucose metabolism dysregulation in the development of Alzheimer s disease. Rev. Invest. Clin. 68, 53–58 (2016).
Reagan, L. P. Neuronal insulin signal transduction mechanisms in diabetes phenotypes. Neurobiol. Aging 26, 56–59 (2005).
Sato, K., Nishijima, T., Yokokawa, T. & Fujita, S. Acute bout of exercise induced prolonged muscle glucose transporter-4 translocation and delayed counter-regulatory hormone response in type 1 diabetes. PLoS ONE 12, e0178505 (2017).
Litmanovitch, E., Geva, R. & Rachmiel, M. Short and long term neuro-behavioral alterations in type 1 diabetes mellitus pediatric population. World J. Diabetes 6, 259 (2015).
Roriz-Filho, J. S. et al. (Pre) diabetes, brain aging, and cognition. Biochim. Biophys. Acta 1792, 432–443 (2009).
Lupien, S. B., Bluhm, E. J. & Ishii, D. N. Systemic insulin-like growth factor-I administration prevents cognitive impairment in diabetic rats, and brain IGF regulates learning/memory in normal adult rats. J. Neurosci. Res. 74, 512–523 (2003).
Ola, M. S. et al. Flavonoid, morin inhibits oxidative stress, inflammation and enhances neurotrophic support in the brain of streptozotocin-induced diabetic rats. Neurol. Sci. 35, 1003–1008 (2014).
Cai, W. et al. Domain-dependent effects of insulin and IGF-1 receptors on signalling and gene expression. Nat. Commun. 8, 1–14 (2017).
LeRoith, D. & Yakar, S. Mechanisms of disease: metabolic effects of growth hormone and insulin-like growth factor 1. Nat. Clin. Pract. Endocrinol. Metab. 3, 302–310 (2007).
Fernandez, A. M. & Torres-Alemán, I. The many faces of insulin-like peptide signalling in the brain. Nat. Rev. Neurosci. 13, 225–239 (2012).
Pennuto, M., Pandey, U. B. & Polanco, M. J. Insulin-like growth factor 1 signaling in motor neuron and polyglutamine diseases: From molecular pathogenesis to therapeutic perspectives. Front. Neuroendocrinol. 57, 100821 (2020).
Wrigley, S., Arafa, D. & Tropea, D. Insulin-like growth factor 1: at the crossroads of brain development and aging. Front. Cell. Neurosci. 11, 14 (2017).
Simeoli, R. & Fierabracci, A. Insights into the Role of MicroRNAs in the Onset and Development of Diabetic Neuropathy. Int. J. Mol. Sci. 20, 4627 (2019).
Tang, X., Tang, G. & Özcan, S. Role of microRNAs in diabetes. Biochim. Biophys. Acta 1779, 697–701 (2008).
Welch, C., Chen, Y. & Stallings, R. MicroRNA-34a functions as a potential tumor suppressor by inducing apoptosis in neuroblastoma cells. Oncogene 26, 5017–5022 (2007).
Esteves, J. V. et al. Diabetes modulates MicroRNAs 29b–3p, 29c–3p, 199a–5p and 532–3p expression in muscle: possible role in GLUT4 and HK2 repression. Front. Endocrinol. 9, 536 (2018).
Dooley, J. et al. The microRNA-29 family dictates the balance between homeostatic and pathological glucose handling in diabetes and obesity. Diabetes 65, 53–61 (2016).
Fenn, A. M. et al. Increased micro-RNA 29b in the aged brain correlates with the reduction of insulin-like growth factor-1 and fractalkine ligand. Neurobiol. Aging 34, 2748–2758 (2013).
Hu, Y. et al. Evaluation of miR-29c inhibits endotheliocyte migration and angiogenesis of human endothelial cells by suppressing the insulin like growth factor 1. Am. J. Transl. Res. 7, 866 (2015).
Li, Z., Jiang, R., Yue, Q. & Peng, H. MicroRNA-29 regulates myocardial microvascular endothelial cells proliferation and migration in association with IGF1 in type 2 diabetes. Biochem. Biophys. Res. Commun. 487, 15–21 (2017).
Li, J. et al. Up-regulated miR-29c inhibits cell proliferation and glycolysis by inhibiting SLC2A3 expression in prostate cancer. Gene 665, 26–34 (2018).
Hirata, T. et al. Pathological and gene expression analysis of a polygenic diabetes model, NONcNZO10/LtJ mice. Gene 629, 52–58 (2017).
Bagge, A. et al. MicroRNA-29a is up-regulated in beta-cells by glucose and decreases glucose-stimulated insulin secretion. Biochem. Biophys. Res. Commun. 426, 266–272 (2012).
Roggli, E. et al. Changes in microRNA expression contribute to pancreatic β-cell dysfunction in prediabetic NOD mice. Diabetes 61, 1742–1751 (2012).
Pandey, A. K. et al. miR-29a levels are elevated in the db/db mice liver and its overexpression leads to attenuation of insulin action on PEPCK gene expression in HepG2 cells. Mol. Cell. Endocrinol. 332, 125–133 (2011).
Liang, J. et al. MicroRNA-29a-c decrease fasting blood glucose levels by negatively regulating hepatic gluconeogenesis. J. Hepatol. 58, 535–542 (2013).
Long, J., Wang, Y., Wang, W., Chang, B. H. & Danesh, F. R. MicroRNA-29c is a signature microRNA under high glucose conditions that targets Sprouty homolog 1, and its in vivo knockdown prevents progression of diabetic nephropathy. J. Biol. Chem. 286, 11837–11848 (2011).
Nielsen, L. B. et al. Circulating levels of microRNA from children with newly diagnosed type 1 diabetes and healthy controls: Evidence that miR-25 associates to residual beta-cell function and glycaemic control during disease progression. Exp. Diabetes Res. https://doi.org/10.1155/2012/896362 (2012).
Volpicelli, F. et al. The microRNA-29a modulates serotonin 5-HT7 receptor expression and its effects on hippocampal neuronal morphology. Mol. Neurobiol. 56, 8617–8627 (2019).
Podolska, A. et al. MicroRNA expression profiling of the porcine developing brain. PLoS ONE 6, e14494 (2011).
Massart, J. et al. Altered miR-29 expression in type 2 diabetes influences glucose and lipid metabolism in skeletal muscle. Diabetes 66, 1807–1818 (2017).
Han, C. et al. miR-29a promotes myocardial cell apoptosis induced by high glucose through down-regulating IGF-1. Int. J. Clin. Exp. Med. 8, 14352 (2015).
Li, J. et al. miR-29b contributes to multiple types of muscle atrophy. Nat. Commun. 8, 1–15 (2017).
Slusarz, A. & Pulakat, L. The two faces of miR-29. J. Cardiovasc. Med. 16, 480 (2015).
Wang, W. et al. The biological activities, chemical stability, metabolism and delivery systems of quercetin: A review. Trends Food Sci. Technol. 56, 21–38 (2016).
Ebrahimpour, S., Zakeri, M. & Esmaeili, A. Crosstalk between Obesity, Diabetes, and Alzheimer’s Disease: Introducing quercetin as an effective triple herbal medicine. Ageing Res. Rev. 2020, 101095 (2020).
Wang, D., Sun-Waterhouse, D., Li, F., Xin, L. & Li, D. MicroRNAs as molecular targets of quercetin and its derivatives underlying their biological effects: A preclinical strategy. Crit. Rev. Food Sci. Nutr. 59, 2189–2201 (2019).
Ghosh, A., Sarkar, S., Mandal, A. K. & Das, N. Neuroprotective role of nanoencapsulated quercetin in combating ischemia-reperfusion induced neuronal damage in young and aged rats. PLoS ONE 8, e57735 (2013).
Kumar, S. R. et al. Quercetin conjugated superparamagnetic magnetite nanoparticles for in-vitro analysis of breast cancer cell lines for chemotherapy applications. J. Colloid Interface Sci. 436, 234–242 (2014).
Vakili-Ghartavol, R. et al. Toxicity assessment of superparamagnetic iron oxide nanoparticles in different tissues. Artif. Cells Nanomed. Biotechnol. 48, 443–451 (2020).
Katebi, S., Esmaeili, A., Ghaedi, K. & Zarrabi, A. Superparamagnetic iron oxide nanoparticles combined with NGF and quercetin promote neuronal branching morphogenesis of PC12 cells. Int. J. Nanomed. 14, 2157 (2019).
Yarjanli, Z., Ghaedi, K., Esmaeili, A., Zarrabi, A. & Rahgozar, S. The antitoxic effects of quercetin and quercetin-conjugated iron oxide nanoparticles (QNPs) against H2O2-induced toxicity in PC12 cells. Int. J. Nanomed. 14, 6813 (2019).
Najafabadi, R. E., Kazemipour, N., Esmaeili, A., Beheshti, S. & Nazifi, S. Using superparamagnetic iron oxide nanoparticles to enhance bioavailability of quercetin in the intact rat brain. BMC Pharmacol. Toxicol. 19, 59 (2018).
Kazemipour, N. et al. Hepatotoxicity and nephrotoxicity of quercetin, iron oxide nanoparticles, and quercetin conjugated with nanoparticles in rats. Comp. Clin. Pathol. 27, 1621–1628 (2018).
Amanzadeh, E. et al. Quercetin conjugated with superparamagnetic iron oxide nanoparticles improves learning and memory better than free quercetin via interacting with proteins involved in LTP. Sci. Rep. 9, 1–19 (2019).
Ebrahimpour, S., Esmaeili, A. & Beheshti, S. Effect of quercetin-conjugated superparamagnetic iron oxide nanoparticles on diabetes-induced learning and memory impairment in rats. Int. J. Nanomed. 13, 6311 (2018).
Ebrahimpour, S., Esmaeili, A., Dehghanian, F. & Beheshti, S. Effects of quercetin-conjugated with superparamagnetic iron oxide nanoparticles on learning and memory improvement through targeting microRNAs/NF-κB pathway. Sci. Rep. 10, 1–14 (2020).
Ebrahimpour, S., Shahidi, S. B., Abbasi, M., Tavakoli, Z. & Esmaeili, A. Quercetin-conjugated superparamagnetic iron oxide nanoparticles (QCSPIONs) increases Nrf2 expression via miR-27a mediation to prevent memory dysfunction in diabetic rats. Sci. Rep. 10, 1–12 (2020).
Lorenzen, J., Kumarswamy, R., Dangwal, S. & Thum, T. MicroRNAs in diabetes and diabetes-associated complications. RNA Biol. 9, 820–827 (2012).
Feng, J., Xing, W. & Xie, L. Regulatory roles of microRNAs in diabetes. Int. J. Mol. Sci. 17, 1729 (2016).
Guay, C. & Regazzi, R. Circulating microRNAs as novel biomarkers for diabetes mellitus. Nat. Rev. Endocrinol. 9, 513 (2013).
Kumar, M., Nath, S., Prasad, H. K., Sharma, G. & Li, Y. MicroRNAs: A new ray of hope for diabetes mellitus. Protein Cell 3, 726–738 (2012).
Dostal, Z. & Modriansky, M. The effect of quercetin on microRNA expression: A critical review. Biomed. Pap. Med. Faculty Palacky Univ. Olomouc 163 (2019).
Eitah, H. E. et al. Modulating impacts of quercetin/sitagliptin combination on streptozotocin-induced diabetes mellitus in rats. Toxicol. Appl. Pharmacol. 365, 30–40 (2019).
Yang, D. K. & Kang, H.-S. Anti-diabetic effect of cotreatment with quercetin and resveratrol in streptozotocin-induced diabetic rats. Biomol. Ther. 26, 130 (2018).
Vessal, M., Hemmati, M. & Vasei, M. Antidiabetic effects of quercetin in streptozocin-induced diabetic rats. Comp. Biochem. Physiol. C 135, 357–364 (2003).
Grillo, C., Piroli, G., Hendry, R. & Reagan, L. Insulin-stimulated translocation of GLUT4 to the plasma membrane in rat hippocampus is PI3-kinase dependent. Brain Res. 1296, 35–45 (2009).
Lv, H. et al. Intranasal insulin administration may be highly effective in improving cognitive function in mice with cognitive dysfunction by reversing brain insulin resistance. Cogn. Neurodyn. 1–16 (2020).
Zhao, F.-Q. & Keating, A. F. Functional properties and genomics of glucose transporters. Curr. Genomics 8, 113–128 (2007).
Bakirtzi, K. et al. Cerebellar neurons possess a vesicular compartment structurally and functionally similar to Glut4-storage vesicles from peripheral insulin-sensitive tissues. J. Neurosci. 29, 5193–5201 (2009).
Sun, P. et al. Streptozotocin impairs proliferation and differentiation of adult hippocampal neural stem cells in vitro-correlation with alterations in the expression of proteins associated with the insulin system. Front. Aging Neurosci. 10, 145 (2018).
Choi, Y.-S. et al. Hyperpolarized [1-13C] lactate flux increased in the hippocampal region in diabetic mice. Mol. Brain 12, 1–10 (2019).
Eid, H. M., Nachar, A., Thong, F., Sweeney, G. & Haddad, P. S. The molecular basis of the antidiabetic action of quercetin in cultured skeletal muscle cells and hepatocytes. Pharmacogn. Mag. 11, 74 (2015).
Mehta, V., Singh, T. R. & Udayabanu, M. Quercetin ameliorates chronic unpredicted stress-induced behavioral dysfunction in male Swiss albino mice by modulating hippocampal insulin signaling pathway. Physiol. Behav. 182, 10–16 (2017).
Sandeep, M. & Nandini, C. Influence of quercetin, naringenin and berberine on glucose transporters and insulin signalling molecules in brain of streptozotocin-induced diabetic rats. Biomed. Pharmacother. 94, 605–611 (2017).
Eldamarawi, M. & Abdelazeem, M. Effect of quercetin and metformin on glucose transporter-4 expression, oxidative stress, inflammation markers and insulin resistance in type 2 diabetes mellitus. Bull. Egypt. Soc. Physiol. Sci. 40, 70–85 (2020).
Żebrowska, A., Hall, B., Maszczyk, A., Banaś, R. & Urban, J. Brain-derived neurotrophic factor, insulin like growth factor-1 and inflammatory cytokine responses to continuous and intermittent exercise in patients with type 1 diabetes. Diabetes Res. Clin. Pract. 144, 126–136 (2018).
Holt, R., Simpson, H. & Sönksen, P. The role of the growth hormone–insulin-like growth factor axis in glucose homeostasis. Diabet. Med. 20, 3–15 (2003).
van Dijk, P. R. et al. Different effects of intraperitoneal and subcutaneous insulin administration on the GH-IGF-1 axis in type 1 diabetes. J. Clin. Endocrinol. Metab. 101, 2493–2501 (2016).
Bondy, C. A. & Cheng, C. M. Signaling by insulin-like growth factor 1 in brain. Eur. J. Pharmacol. 490, 25–31 (2004).
Cheng, C. M. et al. Insulin-like growth factor 1 regulates developing brain glucose metabolism. Proc. Natl. Acad. Sci. USA 97, 10236–10241 (2000).
Schubert, M. et al. Insulin receptor substrate-2 deficiency impairs brain growth and promotes tau phosphorylation. J. Neurosci. 23, 7084–7092 (2003).
Isik, A. T. et al. Curcumin ameliorates impaired insulin/IGF signalling and memory deficit in a streptozotocin-treated rat model. Age 31, 39–49 (2009).
Bhutada, P. et al. Ameliorative effect of quercetin on memory dysfunction in streptozotocin-induced diabetic rats. Neurobiol. Learn. Mem. 94, 293–302 (2010).
Pattanashetti, L. A., Taranalli, A. D., Parvatrao, V., Malabade, R. H. & Kumar, D. Evaluation of neuroprotective effect of quercetin with donepezil in scopolamine-induced amnesia in rats. Indian J. Pharmacol. 49, 60 (2017).
Denny Joseph, K. Combined oral supplementation of fish oil and quercetin enhances neuroprotection in a chronic rotenone rat model: Relevance to Parkinson’s disease. Neurochem. Res. 40, 984–905 (2015).
Maciel, R. M. et al. Neuroprotective effects of quercetin on memory and anxiogenic-like behavior in diabetic rats: Role of ectonucleotidases and acetylcholinesterase activities. Biomed. Pharmacother. 84, 559–568 (2016).
Berry, G. J., Budgeon, L. R., Cooper, T. K., Christensen, N. D. & Waldner, H. The type 1 diabetes resistance locus B10 Idd9. 3 mediates impaired B-cell lymphopoiesis and implicates microRNA-34a in diabetes protection. Eur. J. Immunol. 44, 1716–1727 (2014).
Zheng, Y. et al. miR-101a and miR-30b contribute to inflammatory cytokine-mediated β-cell dysfunction. Lab. Invest. 95, 1387–1397 (2015).
Sims, E. K. et al. MicroRNA 21 targets BCL2 mRNA to increase apoptosis in rat and human beta cells. Diabetologia 60, 1057–1065 (2017).
Sebastiani, G. et al. Increased expression of microRNA miR-326 in type 1 diabetic patients with ongoing islet autoimmunity. Diabetes Metab. Res. Rev. 27, 862–866 (2011).
Baseler, W. A. et al. miR-141 as a regulator of the mitochondrial phosphate carrier (Slc25a3) in the type 1 diabetic heart. Am. J. Physiol. Cell Physiol. 303, C1244–C1251 (2012).
Cui, C. et al. miR-145 regulates diabetes-bone marrow stromal cell-induced neurorestorative effects in diabetes stroke rats. Stem Cells Transl. Med. 5, 1656–1667 (2016).
Yu, M. et al. Inhibiting microRNA-144 abates oxidative stress and reduces apoptosis in hearts of streptozotocin-induced diabetic mice. Cardiovasc. Pathol. 24, 375–381 (2015).
Yang, M. et al. Decreased mi R-146 expression in peripheral blood mononuclear cells is correlated with ongoing islet autoimmunity in type 1 diabetes patients 1 型糖尿病患者外周血单个核细胞 miR-146 表达下调与胰岛持续免疫失衡相关. J. Diabetes 7, 158–165 (2015).
Grieco, F. A. et al. MicroRNAs miR-23a-3p, miR-23b-3p, and miR-149-5p regulate the expression of proapoptotic BH3-only proteins DP5 and PUMA in human pancreatic β-cells. Diabetes 66, 100–112 (2017).
Acknowledgments
This work was supported by a grant from the University of Isfahan.
Author information
Authors and Affiliations
Contributions
A.E. conceived and designed the experiments. S.D. and M.Z. performed experiments and data analysis. SH.E. offered technical assistance. F.D. performed in silico analysis. S.D., M.Z., SH.E. wrote the manuscript. A.E. contributed to the analysis and manuscript critique.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Dini, S., Zakeri, M., Ebrahimpour, S. et al. Quercetin‑conjugated superparamagnetic iron oxide nanoparticles modulate glucose metabolism-related genes and miR-29 family in the hippocampus of diabetic rats. Sci Rep 11, 8618 (2021). https://doi.org/10.1038/s41598-021-87687-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-021-87687-w
- Springer Nature Limited
This article is cited by
-
In diabetic male Wistar rats, quercetin-conjugated superparamagnetic iron oxide nanoparticles have an effect on the SIRT1/p66Shc-mediated pathway related to cognitive impairment
BMC Pharmacology and Toxicology (2023)
-
Quercetin attenuates neurotoxicity induced by iron oxide nanoparticles
Journal of Nanobiotechnology (2021)