Abstract
Glial fibrillary acidic protein expressing (GFAP+) glia modulate nociceptive neuronal activity in both the peripheral nervous system (PNS) and the central nervous system (CNS). Resident GFAP+ glia in dorsal root ganglia (DRG) known as satellite glial cells (SGCs) potentiate neuronal activity by releasing pro-inflammatory cytokines and neuroactive compounds. In this study, we tested the hypothesis that SGC Gq-coupled receptor (Gq-GPCR) signaling modulates pain sensitivity in vivo using Gfap-hM3Dq mice. Complete Freund’s adjuvant (CFA) was used to induce inflammatory pain, and mechanical sensitivity and thermal sensitivity were used to assess the neuromodulatory effect of glial Gq-GPCR activation in awake mice. Pharmacogenetic activation of Gq-GPCR signaling in sensory SGCs decreased heat-induced nociceptive responses and reversed inflammation-induced mechanical allodynia via peripheral adenosine A1 receptor activation. These data reveal a previously unexplored role of sensory SGCs in decreasing afferent excitability. The identified molecular mechanism underlying the analgesic role of SGCs offers new approaches for reversing peripheral nociceptive sensitization.
Similar content being viewed by others
Introduction
Chronic pain is closely associated with nociceptive sensitization and neuroinflammation1,2. In recent years, glial activation and glia-neuron interactions have emerged as key mechanisms underlying generation and maintenance of chronic pain3. Peripheral injury or inflammation induce long-lasting changes in GFAP+ glia including structural reorganization4,5, cell proliferation6,7, changes to neurotransmitter scavenging8,9,10,11, ion buffering capacities12, increases in gap junction coupling13,14,15, and release of pro-inflammatory cytokines, neurotrophins, and neuroactive compounds3,16,17,18,19. These changes in GFAP+ glia occur throughout the entire nociceptive pathway, including peripheral nerves20,21 and higher integrative brain regions22. Pharmacological inhibition of GFAP+ glial activation reduced manifestation of pain in animal models23,24. Therefore, activation of GFAP+ glia during inflammatory pain is considered to be pro-nociceptive and exacerbates symptoms of chronic pain.
Despite the growing body of work on glia-neuron interactions in nociceptive pathways, the hypothesis that GFAP+ glial Gq-GPCR activation modulates nociception in vivo has not been directly tested. This is largely due to limited means to selectively manipulate GFAP+ glial signaling in vivo. To test this hypothesis, we employed a transgenic mouse expressing the Gq-coupled DREADD (hM3Dq) under control of a GFAP minimal promoter (Gfap-hM3Dq mice), as previously described25. The hM3Dq-HA immunoreactivity was restricted to GFAP+ glia in both CNS and PNS25. Clozapine-N-oxide (CNO), the agonist for hM3Dq receptors, induces intracellular Ca2+ elevations comparable to those evoked by endogenous Gq-GPCR agonists in a majority of GFAP+ glia in the brain (CA1 hippocampal astrocytes25, visual cortical astrocytes26,27, medulla astrocytes27, and in PNS superior cervical ganglia satellite glial cells27 and enteric glia28). These data demonstrated the functional expression and integration of hM3Dq in GFAP+ glial signaling pathways in Gfap-hM3Dq mice. In addition, the hM3Dq exhibits no constitutive activity and can only be activated by the bio-inert small molecule, CNO29, providing a unique model for assessing the role of GFAP+ glia Gq-GPCR signaling in pain modulation in free-moving animals.
The present study sought to identify glial Gq-GPCR signaling as a viable therapeutic target for ameliorating chronic and acute pain. Using a CFA-induced inflammatory pain model, we demonstrated that the activation of Gq-GPCR signaling pathways in sensory ganglionic SGCs induced robust and long-lasting (~ 90 min) analgesia in the hind paws of Gfap-hM3Dq mice. The analgesic effects were observed not only in CFA-injected hind paws which suffered from inflammation-induced hypersensitivity, but also in saline-injected control (Von Frey tests) and intact (Hargreaves tests) hind paws. Pharmacological experiments and the usage of adenosine receptor knockout mice revealed that the analgesic effect of glial hM3Dq activation was due to the activation of Gq-GPCR signaling pathways in sensory SGCs, and was dependent on adenosine A1 receptor (A1R) activation in the PNS. These data revealed a novel role of sensory SGC Gq-GPCR signaling in pain control, suggesting a strong therapeutic potential of targeting the peripheral glial signaling for the treatment of acute and chronic pain. Future studies are warranted to develop selective manipulation of sensory SGC signaling as an alternative approach in pain management.
Results
Pharmacogenetic activation of Gq-GPCR signaling pathways in GFAP+ glia alleviated inflammation-induced mechanical allodynia in mice
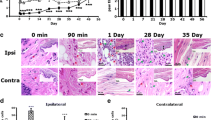
To test our hypothesis that Gq-GPCR signaling in GFAP+ glia modulates pain sensitivity, Gfap-hM3Dq mice25 were used to selectively activate GFAP+ glial Gq-GPCR signaling in vivo. We first tested our hypothesis in the CFA-induced inflammatory pain model. Gfap-hM3Dq mice and their WT littermate controls were subjected to unilateral injection of CFA in right hind paws (Fig. 1A). Mechanical pain sensitivity in CFA-injected hind paws was assessed prior to (baseline threshold) and five days after CFA injection (inflammation-induced threshold); normalized threshold was then calculated (Fig. 1B). CFA induced well-documented mechanical hyperalgesia and mechanical allodynia30 in CFA-injected paw in both the Gfap-hM3Dq mice and their littermate controls, as evidenced by a decreased mechanical pain threshold (~ 40% when compared to the baseline threshold measured from the same paw) (Fig. 1C). There was no significant difference in the reduction of mechanical pain thresholds between Gfap-hM3Dq mice and their littermate controls (N = 3 per group). A single administration of CNO (0.25 mg/kg, i. p.) reversed the normalized mechanical pain threshold in Gfap-hM3Dq mice but not in littermate controls (Fig. 2D). The CNO-induced reversal of inflammatory allodynia occurred within 15 min after drug administration and persisted for nearly 90 min. CNO injection resulted in significant main effects of time (F11,88 = 3.86, p < 0.001), genotype (F1,8 = 36.13, p < 0.001), as well as a significant time-by-genotype interaction (F11,88 = 3.22, p < 0.01). Conversely, saline exposure resulted in no significant main effects of time (F11,44 = 0.39), genotype (F1,4 = 1.36), and no significant time-by-genotype interaction (F11,44 = 0.54). These data suggested that Gq-GPCR activation in GFAP+ glia substantially alleviated inflammation-induced mechanical allodynia.
CNO-induced GFAP+ glial Gq-GPCR activation alleviated CFA-induced mechanical allodynia in vivo. (A) Schematic timeline of CFA-induced inflammatory pain animal model; (B) Von Frey apparatus for assessing mechanically induced pain thresholds. (C) CFA injection into hind paw induced comparable levels of mechanical allodynia in both Gfap-hM3Dq mice and WT littermate controls (N = 3 per genotype). (D) 0.25 mg/kg CNO i. p. administration largely reversed CFA-induced mechanical allodynia in CFA-injected paws in Gfap-hM3Dq mice, but not in WT littermate controls (N = 5 per genotype); **p < 0.01; ***p < 0.001 compared to pre-CNO. (B) was taken by Alison Xie; (C) and (D) were prepared using Graphpad Prism 7.04.
CNO-induced GFAP+ glial Gq-GPCR activation decreased heat sensitivity in the hind paws of naive mice. (A) Baseline heat sensitivity without any drug administration of animals used in (B). Gfap-hM3Dq mice exhibited similar heat sensitivity compared to their WT littermate controls in Hargreaves test (N = 9 control, N = 10 Gfap-hM3Dq). (B) 0.25 mg/kg CNO i. p. administration significantly increased paw withdrawal frequency at 30 min after CNO delivery (N = 9 control, N = 10 Gfap-hM3Dq). (C) Baseline heat sensitivity without any drug administration of animals used in (D). Gfap-hM3Dq mice exhibited similar heat sensitivity compared to their WT littermate controls (N = 10 control, N = 17 Gfap-hM3Dq). (D) Intrathecal administration (i. t.) of 0.5 mg/kg CNO significantly increased paw withdrawal latency up to 2 h (N = 10 control, N = 17 Gfap-hM3Dq). In both (B) and (D), *p < 0.05; **p < 0.01; ***p < 0.001 compared to pre-CNO. Figures were prepared using Graphpad Prism 7.04.
Gq-DREADD mediated Gq-GPCR activation in GFAP+ glia decreased hind paw heat sensitivity in naive mice
We next tested if CNO-induced reduction of pain sensitivity was restricted to mechanical nociception. We chose to examine effects of glial Gq-GPCR activation on heat-induced pain sensitivity, which is mechanistically distinct from mechanical nociception and predominately mediated by different nociceptive nerve fibers31. Hargreaves test was used to assess heat sensitivity in the hind paws of Gfap-hM3Dq mice and WT littermate controls. In all experiments, a fixed low intensity thermal beam was applied to a hind paw and the paw withdrawal latency to the beam was recorded. There was no significant difference in paw withdrawal latency between Gfap-hM3Dq mice and littermate controls (Fig. 2A). However, CNO (0.5 mg/kg, i. p.) significantly increased paw withdrawal latency of Gfap-hM3Dq mice, but not of littermate controls (Fig. 2B). Significant main effects of time (F8,136 = 3.73, p < 0.001) and genotype (F1,17 = 6.58, p < 0.05) were observed, but no significant time-by-genotype interaction (F8,136 = 1.70). These data demonstrated that Gq-GPCR activation in GFAP+ glia reduced hind paw heat sensitivity in addition to mechanical sensitivity, suggesting a general analgesic effect of glial Gq-GPCR activation.
Gq-GPCR activation in peripheral SGCs was responsible for CNO-induced decreases in afferent sensitivity
Systemic administration of CNO activates GFAP+ glial Gq-GPCR signaling in both CNS astrocytes and PNS glia27. To identify the site of the analgesic effect of glial Gq-GPCR activation, CNO (0.5 mg/kg) was delivered via i.t. injections in Gfap-hM3Dq mice and their WT littermate controls (control: N = 10, Gfap-hM3Dq: N = 17). A single i.t. injection of CNO mimicked the analgesic effect on hind paw heat sensitivity in Gfap-hM3Dq mice, suggesting that Gq-GPCR activation in spinal cord astrocytes and/or sensory satellite glial cells32 is sufficient to modulate pain sensitivity in vivo (Fig. 2D). There was no significant main effect of time (F4,100 = 0.87) but a significant main effect of genotype (F1,25 = 9.40, p < 0.01), and a significant time-by-genotype interaction (F4,100 = 4.66, p < 0.01) were observed. There was no significant difference in baseline paw withdrawal latency between Gfap-hM3Dq mice and the littermate controls (Fig. 2C).
To distinguish the possible analgesic effects of Gq-GPCR activation between spinal astrocytes and sensory satellite glial cells, trospium chloride, a peripheral muscarinic receptor blocker, was used to inhibit CNO-induced hM3Dq activation in PNS glia27. Using the CFA-induced inflammatory pain model (Fig. 3A), Gfap-hM3Dq mice were pretreated with either trospium chloride (20 mg/kg, i. p.) or saline 15 min prior to CNO administration (0.5 mg/kg, i. p.) followed by Von Frey testing (Fig. 3B; N = 11 saline pretreated; N = 10 trospium pretreated). Normalized paw withdrawal thresholds of both CFA- and saline-injected paws were calculated. Saline treatment did not alter CNO-induced reduction of mechanical allodynia in CFA-injected hind paws in Gfap-hM3Dq mice (Fig. 3C). In contrast, pretreatment with trospium chloride completely blocked CNO-induced analgesic effects in CFA-injected paws (Fig. 3C), suggesting that peripheral activation of hM3Dq was necessary for the CNO-induced analgesic effect in Gfap-hM3Dq mice. In the CFA-injected hind paws, we observed main effects of trospium (F1,19 = 25.31, p < 0.0001), time (F6,114 = 20.17, p < 0.0001), and a significant trospium-by-time interaction (F6,114 = 7.19, p < 0.0001).
CNO-induced analgesia in Gfap-hM3Dq mice was due to Gq-GPCR activation in peripheral GFAP+ glia and not due to CNO-induced decreases in motor activity. (A) Schematic timeline of peripheral hM3Dq blockade experiments Gfap-hM3Dq mice were subjected to CFA-induced inflammatory pain model as in Fig. 1. Von Frey tests were used to assess both baseline and inflammation induced mechanical pain threshold in both CFA-injected and saline-injected hind paws (N = 21 mice). (B) A summary of peripheral Gq-GPCR activation blockade in Gfap-hM3Dq mice with saline or Trospium pretreatment. (C,D) Trospium pretreatment prevented CNO-induced increases of pain threshold in both CFA-injected (C) and saline-injected (D) hind paws in Gfap-hM3Dq mice (N = 11 saline pretreated, N = 10 trospium pretreated). (E) 0.25 mg/kg CNO i. p. administration had no effect on rotarod performance (three trials, T1, T2, and T3) in WT littermate control mice, nor did pretreatment with trospium (N = 6 per group). (F) CNO led to decreased rotarod performance in Gfap-hM3Dq mice. Trospium pretreatment did not alter CNO-induced decreases in rotarod performance (N = 5 per group). +p < 0.01 compared to baseline in saline-treated mice; *p < 0.01, **p < 0.001 compared to saline-treated mice. (C–F) Were prepared using Graphpad Prism 7.04.
Interestingly, CNO also induced an analgesic effect in the saline-injected paws (Fig. 3D). In absence of inflammation, the mechanical pain thresholds in the saline-injected paws (left hind paws) remained unchanged at five days post-CFA injection into the right hind paws. CNO administration (0.25 mg/kg, i. p.) increased the mechanical pain threshold in saline-injected paws by approximately 50% during the first hour after CNO administration, similar to the observed effects on the CFA-injected paws. These data suggest that glial activation-induced analgesia was independent of CFA-induced inflammation. Pretreatment with trospium chloride also blocked CNO-induced analgesic effect in saline-injected paws in Gfap-hM3Dq mice (Fig. 3D; N = 11 saline pretreated, N = 10 trospium pretreated), further confirming that peripheral GFAP+ glial Gq-GPCR activation was responsible for CNO-induced decreases in pain sensitivity in Gfap-hM3Dq mice. For the saline-injected paw, a two-way ANOVA revealed significant main effects of trospium chloride (F1,19 = 9.05, p < 0.01 to saline pre-treatment), time (F6,114 = 11.03, p < 0.0001), and a significant trospium-by-time interaction (F6,114 = 4.52, p < 0.001).
CNO-induced activation of GFAP+ glial Gq-GPCR signaling produces mild sedative effects and decreases motor performance25. To determine if trospium blockade of CNO-induced analgesia was due to a reversal of locomotor deficits following CNO administration, Gfap-hM3Dq mice and their wild-type littermate controls were subjected to rotarod tests during which trospium and CNO were administered. Both Gfap-hM3Dq mice and their littermate controls received either saline or trospium (20 mg/kg, i. p.) pretreatment 15 min prior to CNO administration (0.25 mg/kg, i. p.). CNO administration slightly decreased rotarod performance in Gfap-hM3Dq mice (Fig. 3F) but not in littermate controls (Fig. 3E), consistent with our previous report25. Trospium had no additional effect on CNO-induced decreases in rotarod performance in Gfap-hM3Dq mice (Fig. 3F; N = 5 per group), suggesting that CNO-induced analgesia was not secondary to CNO-induced motoric deficits. There were no significant main effects of trospium (F1,8 = 1.00), trial (F2,16 = 0.75), nor a significant trospium-by-trial interaction (F2,16 = 0.20). Neither CNO nor trospium pretreatment produced any effect on rotarod performance in WT mice (Fig. 3E, N = 6 per group). There was no main effect of trospium (F1,10 = 1.40), a main effect of trial (F2,20 = 7.19, p < 0.01), and no significant trospium-by-trial interaction (F2,20 = 1.62).
Together, these data strongly suggest that Gq-GPCR activation in sensory ganglionic SGCs is responsible for CNO-induced decreases in pain sensitivity.
Sensory SGC Gq-GPCR activation underlies CNO-induced analgesia
Administration of CNO in Gfap-hM3Dq mice also induces Gq-GPCR activation in sympathetic ganglia, which increases sympathetic drive to the peripheral organs27. Sympathetic activation has been shown to exacerbate pain sensation via activation of adrenergic receptors on sensory nerves33,34,35. To test the extent to which CNO-induced sympathetic activation contributes to CNO-induced changes in pain sensitivity, Gfap-hM3Dq mice were subjected to 6-OHDA induced peripheral chemical sympathectomy (SymX)27,36 (Fig. 4A). When injected in the periphery, 6-OHDA enters noradrenergic terminals via norepinephrine reuptake transporters and destroys sympathetic terminals37, sparing cholinergic neurons, Schwann cells, non-myelinating glia including ganglionic SGCs, endothelial cells, and adrenal medulla37,38. In the CFA-injected hind paws, 6-OHDA-induced sympathectomy completely prevented the development of CFA-induced mechanical allodynia (Fig. 4B,C, N = 5 6-OHDA injection, N = 6 vehicle injection), but did not alter the baseline mechanical sensitivity in the saline-injected paws. There was a main effect of SymX (F1,9 = 24.85, p < 0.001), time (F6,54 = 43.18, p < 0.0001), but no SymX-by-time interaction (F6,54 = 0.3026). These data implied that sympathetic mechanisms are responsible for CFA-induced hypersensitivity in the used animal model. Peripheral sympathectomy did not result in changes in baseline pain threshold in saline-injected hind paws (Fig. 4C). There was no main effect of SymX (F1,9 = 0.18), a main effect of time (F6,54 = 20.78, p < 0.0001), and no significant SymX-by-time interaction (F6,54 = 0.8228). Application of CNO (i. p.) led to additional analgesic effects on both the CFA- and saline-injected paws in Gfap-hM3Dq mice. However, the CNO-induced analgesic effect was not altered by peripheral sympathectomy (Fig. 4B,C, N = 5 6-OHDA injection, N = 6 vehicle injection). These data provided evidence that while CFA-induced hind paw mechanical allodynia was dependent on sympathetic mechanisms, glial Gq-GPCR activation-evoked analgesia was not. Moreover, these data strongly suggested that sensory SGCs, but not sympathetic SGCs, were responsible for CNO-induced analgesia in Gfap-hM3Dq mice.
Peripheral chemical sympathectomy reversed inflammation induced mechanical allodynia in CFA-injected hind paws in Gfap-hM3Dq mice, while CNO induced additional analgesia effects in both CFA-injected and saline-injected hind paws. (A) Experimental timeline of 6-OHDA induced peripheral chemical sympathectomy and CFA-induced inflammatory pain in Gfap-hM3Dq mice (N = 6 vehicle injection, N = 5 6-OHDA injection). (B) Peripheral sympathectomy blocked CFA-induced mechanical allodynia in Gfap-hM3Dq mice. CNO-induced analgesia was observed in CFA-injected hind paws in both the vehicle- and 6-OHDA-injected groups. (C) Sympathectomy does not affect either the baseline pain threshold or CNO-induced analgesia in saline-injected hind paw. +p < 0.01 compared to baseline in vehicle treated mice; #p < 0.01 compared to baseline in sympathectomized mice. (B,C) Were prepared using Graphpad Prism 7.04.
Sensory SGC Gq-GPCR activation led to mechanical analgesia via peripheral A1R activation
Thus far, our data suggested that Gq-GPCR activation in SGCs in the peripheral sensory ganglia produced strong analgesia in both intact hind paws (Figs. 2, 3D, 4C, 5B,D, 6B,D) and hind paws with inflammation-induced hypersensitivity (Figs. 1, 3C, 4B, 5A,C, 6A,C). Previous reports indicated that sensory SGCs modulate peripheral neuronal activity via purinergic mechanisms in the context of neuropathic39 and inflammatory17 pain. To test if CNO-induced analgesia in Gfap-hM3Dq mice was dependent on glia-neuron adenosine signaling in sensory ganglia, pharmacological and genetic approaches were employed to dissect the potential molecular mechanism.
Pharmacological blockade of peripheral A1 Adenosine receptors prevented CNO-induced analgesia in Gfap-hM3Dq mice. Peripheral administration of SPT, a blood brain barrier impermeable inhibitor of adenosine receptors ablated CNO-induced analgesia in CFA-injected (A) and saline-injected (B) hind paws (N = 13 saline treated, N = 5 SPT treated). A1 adenosine receptor blocker CPX also prevented CNO-induced analgesia in CFA-injected (C) and saline-injected (D) hind paws (N = 13 saline treated, N = 12 CPX treated). +p < 0.01 compared to baseline in saline-treated animals; *p < 0.05, **p < 0.01, ***p < 0.001 compared to saline-treated animals. Figures were prepared using Graphpad Prism 7.04.
Gfap-hM3Dq mice lacking A1R, but not those lacking A2AR failed to exhibit CNO-induced analgesia. CNO-induced analgesia was observed in A1 heterozygous (Het) but not in A1 knockout (KO) mice in both CFA-injected (A) and saline-injected (B) hind paws (N = 9 A1 Het mice, and N = 13 A1 KO mice). CNO-induced analgesia remained intact in both A2A heterozygous and in A2A knockout mice in both the CFA-injected (C) and saline-injected (D) hind paws (N = 7 per group). +p < 0.01 compared to baseline in heterozygous mice; #p < 0.01 compared to baseline in knockout mice. Figures were prepared using Graphpad Prism 7.04.
Gfap-hM3Dq mice were subjected to CFA-induced inflammatory pain, as described in Fig. 1A. Von Frey tests were performed prior to and 5 days after CFA-injections on both CFA-injected and saline-injected hind paws to assess the mechanical pain threshold. Two adenosine receptor blockers were used in separate experiments to evaluate the potential role of adenosine receptors in CNO-induced analgesia. In one set of experiments, 8-(p-Sulfophenyl) theophylline hydrate (SPT), a non-selective adenosine receptor antagonist that does not readily cross the blood–brain barrier40 was injected (10 mg/kg, i.p.) in Gfap-hM3Dq mice 15 min prior to CNO administration. In both CFA-injected and saline-injected hind paws, pretreatment with SPT completely blocked CNO-induced analgesia in Gfap-hM3Dq mice (Fig. 5A,B, N = 13 saline treated, N = 5 SPT treated). For the CFA-treated paw, a two-way ANOVA with time as a repeated measure and SPT as a between subjects factor revealed main effects of SPT (F1,16 = 23.59, p < 0.001), time (F6,96 = 16.32, p < 0.0001), and a significant SPT-by-time interaction (F6,96 = 7.78, p < 0.0001). For the saline-injected paw, main effects were found for SPT (F1,16 = 12.81, p < 0.01), time (F6,96 = 5.42, p < 0.0001), and a significant SPT-by-time interaction (F6,96 = 5.11, p < 0.001). These data suggested that activation of peripheral adenosine receptors was necessary for CNO-induced analgesia in Gfap-hM3Dq mice.
In the second set of experiments, 8-Cyclopentyl-1,3-dipropylxanthin (CPX), a selective A1R antagonist was administered (1 mg/kg, i. p.) 15 min prior to CNO administration (Fig. 5C,D). Pretreatment with CPX also blocked CNO-induced analgesia in both CFA-injected and saline-injected hind paws of Gfap-hM3Dq mice (Fig. 5C,D, N = 13 saline treated, N = 12 CPX treated). In the CFA-treated paw, we found main effects of CPX (F1,23 = 45.34, p < 0.0001), time (F6,138 = 21.47, p < 0.0001), and a significant CPX-by-time interaction (F6,138 = 6.87, p < 0.0001). For the saline-injected paw, we observed significant main effects of CPX (F1,23 = 28.92, p < 0.0001), time (F6,138 = 9.71, p < 0.0001), and a significant CPX-by-time interaction (F6,138 = 15.07, p < 0.0001). Taken together, these data suggested that activation of peripheral A1Rs was necessary for peripheral glial activation-induced analgesia.
We next tested the role of A1R activation in CNO-induced analgesia by genetically deleting A1Rs or A2ARs in Gfap-hM3Dq mice. Genetic deletion of A1R prevented CNO-induced analgesia (Fig. 6A,B). For the CFA treated paw, a two-way genotype-by-time ANOVA revealed main effects of genotype (F1,120 = 32.88, p < 0.0001), time (F6,120 = 26.44, p < 0.0001) and a genotype-by-time interaction (F6,120 = 21.48, p < 0.0001). For the saline-injected paw, we observed no main effect of genotype (F1,120 = 1.48), a main effect of time (F6,120 = 3.82, p < 0.01), and a significant genotype-by-time interaction (F6,120 = 3.23, p < 0.01).
In contrast, genetic deletion of A2A receptors had no effect on CNO-induced analgesia in Gfap-hM3Dq mice (Fig. 6C,D). For the CFA-injected paw, there was only a main effect of time (F6,72 = 30.50, p < 0.0001), but no main effect of genotype (F1,72 = 0.01), and no significant genotype-by-time interaction (F6,72 = 1.07). Further, for the saline-injected paw, only a main effect of time was observed (F6,72 = 17.61, p < 0.0001), with no main effect of genotype (F1,72 = 0.07) nor a significant genotype-by-time interaction (F6,72 = 0.40). Collectively, these data suggest that sensory SGC Gq-GPCR-mediated analgesia was dependent on peripheral A1R activation.
Discussion
Our findings demonstrate that sensory SGCs are capable of reducing heat sensitivity and reversing the symptoms of inflammation-induced mechanical allodynia following Gq-GPCR activation in vivo, thus, suggesting an analgesic role of these cells (Fig. 7). SGCs are the main type of glia in peripheral ganglia41,42. In the dorsal root ganglia (DRGs), SGCs form envelopes around individual neurons41, creating distinct functional units consisting of a single sensory neuron and several surrounding SGCs. Sensory SGCs express receptors and transporters of neurotransmitters, ion channels and gap junctions41, suggesting their physiological roles in regulating sensory neuronal excitability. Sensory SGCs also express the machinery necessary for releasing neuromodulatory peptides, cytokines, and neurotrophins41, indicating their active roles in modulating sensory neuronal activity in both health and disease. However, the ability of sensory SGC signaling to modulate nociception has never been tested in intact and free-moving animals. This is due to the difficulties with selective activation of SGC signaling pathways in vivo. In the current study, we took advantage of the Gfap-hM3Dq transgenic mouse line25 in which GFAP+ glial Gq-GPCR signaling pathways could be selectively activated in vivo by an otherwise bio-inert ligand, CNO29. The Gfap-hM3Dq mice and Cre-dependent hM3Dq mice have been used in recent studies to assess the physiological roles of peripheral GFAP+ glia in vivo25,27,28,43. In combination with the pharmacological manipulations, Gfap-hM3Dq mice served as a powerful model to study GFAP+ glial Gq-GPCR signaling in nociception.
Summary of experimental strategies and approaches. Gfap-hM3Dq mice express hM3Dq, a Gq-coupled engineered GPCR in GFAP+ glial cells throughout the nervous system. The ligand of hM3Dq, CNO effectively induces hind paw mechanical analgesia (Fig. 1) and decreases thermal sensitivity (Fig. 2) in GFAP-hM3Dq mice. To distinguish the potential analgesic effect of CNS astrocytes vs PNS GFAP+ glia following their Gq-GPCR activation, a peripheral acting blocker of muscarinic receptors, Trospium chloride, was administrated to block CNO-induced and hM3Dq-mediated Gq-GPCR activation in peripheral glia. Astrocytic Gq-GPCR activation alone did not lead to significant changes in hind paw mechanical sensitivity (Fig. 3), which suggested that peripheral GFAP+ glial Gq-GPCR activation is responsible for CNO-induced hind paw analgesia. The glial-induced analgesic effect was independent from inflammation and not affected by peripheral sympathectomy (Fig. 4), suggesting that peripheral glial Gq-GPCR activation directly modulate sensory neuronal activity and/or afferent excitability. To further test this hypothesis, peripheral acting and selective adenosine receptor A1 adenosine receptor antagonists were administrated prior to CNO in GFAP-hM3Dq mice. Blockade of peripheral A1R activation completely abolished peripheral GFAP+ glial activation induced mechanical analgesia (Fig. 5); similar results were repeated using A1R KO mice that also express hM3Dq in GFAP+ glia (Fig. 6). These experiments strongly suggested that peripheral glial Gq-GPCR activation decreases hind paw mechanical sensitivity via peripheral activation of A1R.
How does SGC Gq-GPCR activation produce analgesic effect on hind paw heat and mechanical sensitivity? Our data suggest that it is likely due to a SGC-mediated inhibitory effect on excitability of DRG neurons via A1 adenosine receptor activation. Although our approach did not restrict the genetic deletion or the pharmacological inhibition of A1Rs in DRG neurons, purinergic signaling has been reported to mediate SGC-neuron interaction in the DRGs44. We established that blocking peripheral adenosine receptors with SPT, or A1Rs with CPX, completely reverses CNO-induced analgesia in Gfap-hM3Dq mice, suggesting that glial Gq-GPCR activation likely activates neuronal A1Rs in the sensory ganglia. These data are in line with the previous results which showed that astrocyte-released adenosine triphosphate (ATP) activates A1Rs in hippocampal neurons, leading to heterosynaptic suppression of glutamatergic synaptic responses45. We also found that CNO-induced analgesia was completely abolished in A1R knockout mice, further confirming that A1R activation is responsible for the neuromodulatory effect of SGC Gq-GPCR activation. Interestingly, CNO-induced analgesia remained intact in A2AR knockout mice in the context of CFA-induced inflammatory pain. It has been reported that A2AR knockout mice exhibit a significant decrease of mechanical allodynia in animal models of neuropathic pain, as well as a suppression of thermal hyperalgesia and allodynia39. Taken together, our data suggest that SGC Gq-GPCR signaling modulates sensory neuronal activity exclusively via activation of A1R but not of A2AR, in inflammation-induced chronic pain models.
The analgesic effect of SGC activation was only suggested once in the previous studies46. Chen et al. reported that the P2X7R activation in sensory SGCs tonically suppressed neuronal P2X3R expression and decreased the excitability of DRG neurons46. P2X7R is abundantly expressed in sensory SGCs46,47,48, and can trigger exocytosis of ATP via increases in Ca2+46, suggesting potential inhibitory feedback via bi-directional purinergic signaling between DRG neurons and SGCs. CNO-induced hM3Dq activation also elevates intracellular Ca2+ in SGCs. It is possible that hM3Dq activation in sensory SGCs induces ATP release via similar mechanisms as those triggered by P2X7R activation. However, hM3Dq activation also leads to the activation of many Gq-GPCR signaling cascades in GFAP+ glia49 in addition to elevating intracellular Ca2+. Additional studies are needed to identify the molecular mechanism underlying potential CNO-induced ATP release from sensory SGCs.
Pharmacogenetic activation of central GFAP+ glia produces a mild sedative effect25 and impaired motor function (Fig. 3E,F), which might influence the perception of pain or the motor function in nociceptive behavior. In this study, trospium chloride, a peripheral hM3Dq blocker, was used to distinguish the effects of central vs peripheral glial activation following CNO administration. The trospium chloride blockade of peripheral hM3Dq activation completely abolished CNO-induced analgesia, suggesting that peripheral GFAP+ glial activation is responsible for the observed analgesic effect on inflammation-induced mechanical hypersensitivity.
It was important to compare the effect of CNO-induced analgesia to the sympathectomy-produced reversal of mechanical hypersensitivity, as reports indicate that sympathetic sprouting into DRGs contributes to chronic pain following peripheral injury33,35,50. However, sympathetic blockade51 and chemical sympathectomy52 resulted in poor clinical outcomes in patients suffering from chronic pain53. Therefore, it was unexpected to observe that 6-OHDA-induced peripheral sympathectomy completely prevented CFA-induced mechanical allodynia in Gfap-hM3Dq mice (Fig. 4). CNO administration in Gfap-hM3Dq mice led to an additional analgesic effect on mechanical sensitivity in both CFA-injected and saline-injected hind paws (Fig. 4). These data suggest that SGC Gq-GPCR signaling modulates nociception independently of inflammation-induced sympathetic pain mechanisms.
We previously reported that CNO-induced sympathetic ganglionic SGC activation in Gfap-hM3Dq mice increased sympathetically-driven cardiac function27,43, and blood pressure25 in vivo. Our findings suggest that sympathetic SGCs directly increase post-ganglionic neuronal activity following CNO-induced Gq-GPCR activation27. However, in the same animal, sensory SGC activation produces a robust analgesic effect that is likely due to direct inhibition of sensory neuronal activity. It is unclear how the same Gq-GPCR activation in sympathetic and sensory SGCs produce opposite neuromodulatory effects. Future studies on the molecular mechanisms underlying ganglionic SGC-neuron interaction in both sympathetic and sensory ganglia are needed.
As reflected in Fig. 7, the current study points towards the SGC Gq-GPCR signaling as a potential target for reversing inflammatory pain. Unpublished data from our laboratory indicate that in sciatic nerve injury-induced neuropathic pain model, CNO i. p. administration also significantly decreases mechanical allodynia in ipsilateral hind paw in Gfap-hM3Dq mice. In the current report, we provided data that CNO-induced analgesia occurred in saline-injected and intact hind paws in Gfap-hM3Dq mice. Taken together, our findings strongly suggest that SGC Gq-GPCR activation-induced analgesia applies to physiological and pathological conditions, including both nerve-injury-induced and inflammation-induced chronic pain models.
Therapeutic strategies targeting glial activation have been previously considered for pain control23. However, the glial inhibitors currently utilized in pain models are usually selected for their anti-inflammatory properties or inhibitory effects on glial metabolism. The choice of glial inhibitors is mostly based on the assumption that glial activation is pro-nociceptive23. Our data in Gfap-hM3Dq mice demonstrate a strong anti-nociceptive property of Gq-GPCR signaling pathways in sensory SGCs. For several reasons, we believe that sensory SGC Gq-GPCR signaling pathway could be a strong candidate for potential pharmacological therapies for the treatment of acute and chronic pain. First, glial-mediated inhibition of sensory neurons can reduce the ongoing peripheral nociceptive input into the CNS, which is required for the maintenance of chronic pain54,55. Second, sensory SGCs are positioned near the spinal cord, therefore, pharmacological activation of SGC signaling would not require drugs to cross the blood–brain barrier. Third, modulation of sensory neuronal activity via glial signaling may reduce the potential side effects of direct activation of the receptors on neuronal cell bodies. Finally, the pharmacological effects of glial Gq-GPCR activation in vivo are fast-acting and long-lasting25,27, despite the rapid clearance of the ligand56. The combination of the above-mentioned factors makes SGC an ideal candidate for developing glia-focused therapeutic approaches. Future efforts aimed at screening for glial-specific Gq-GPCRs or chemical compounds to activate glial Gq-GPCRs would provide additional resources for the development of novel and effective treatments for chronic pain conditions.
Materials and methods
Animals
All transgenic and knockout mice were generated and maintained in the C57BL/6J background. Males were used in all experiments. Mice were maintained in a temperature-controlled environment at the University of North Carolina at Chapel Hill (UNC-CH) on a 12-h light/12-h dark cycle, with ad libitum access to food and water. Experiments took place during the light cycle. All experimental procedures on animals were performed according to the protocols approved by the IACUC of the UNC-CH (protocol 13-276.0).
Gfap-hM3Dq mice were generated, bred, and genotyped as previously described25. Briefly, the mice expressed HA-hM3Dq driven by a 2.2kB human GFAP promoter. Gfap-hM3Dq+/− mice were bred to C57Bl6/J wild type (WT) mice (Jackson Labs, Bar Harbor, ME) to generate hemizygous and WT progeny. All experiments were performed in Gfap-hM3Dq+/− mice (hM3Dq mice) from N11 to N15 generational backcross. In all experiments, hM3Dq-negative, WT littermates were used as controls.
Mice lacking A1R (A1−/− mice)57 and A2AR (A2A−/− mice)58 were gifted by Dr. Stephen Tilley (UNC-CH). These mouse lines were crossed separately with Gfap-hM3Dq+/− mice, resulting in hemizygous hM3Dq expression in GFAP+ cells in either A1−/− mice (Gfap-hM3Dq+/−::A1−/−) or A2A−/− mice (Gfap-hM3Dq+/−::A2A−/−). In all presented experiments, Gfap-hM3Dq+/− mice with heterozygous expression of A1R (Gfap-hM3Dq+/−::A1+/− mice) or A2AR (Gfap-hM3Dq+/−::A2A+/− mice) were used as controls, respectively.
Complete Freund’s adjuvant (CFA) induced inflammatory pain
To induce acute inflammation and subsequent chronic pain, 20 µL CFA (Sigma-Aldrich, MO, USA) was injected into the right hind paw of each mouse. Saline (20 µL) was injected into the left hind paw as an internal experimental control. CFA-injected mice were placed on soft bedding for 7 days during the rest of the experimental period. The mechanical sensitivity of the CFA-injected and saline-injected paws was assessed before CFA injections and 5 or 7 days after CFA injections depending on the experiments (Figs. 1A, 3A, 4A).
Von Frey test for assessing mechanical pain threshold
The Von Frey test was used to determine the mechanical pain threshold of the hind paws of hM3Dq mice and their WT littermate controls, as previously described59. The apparatus consisted of a clear plastic isolation chamber (7.5 cm wide × 7.5 cm long × 15 cm tall) on top of a wire mesh floor (0.5 cm2 grid) to allow access to the hind paws. Mechanical threshold was measured as the minimum filament weight that induced 5 paw responses (withdrawal or licking/biting) out of 10 applications. For each mouse, a baseline threshold was established just prior to CFA injection. Five days after CFA injection, pharmacological intervention of pain threshold was tested before and after pharmacogenetic (CNO administration) or pharmacological manipulation in 15-min increments.
Hargreaves test for assessing thermal pain threshold
Gfap-hM3Dq mice and their WT littermate controls were individually placed in a plastic isolation container (7.5 cm wide × 7.5 cm long × 15 cm tall) on an elevated glass plate. After 60 min of habituation, a low intensity thermal beam was applied to the footpad of each hind paw intermittently in time increments, as indicated in Fig. 2. The latency time from the application of the light beam to the paw flick response was recorded. The beam was cut off after a maximum of 20 s to prevent tissue damage. CNO was administered by either intraperitoneal injection (i. p., 0.25 mg/kg) or intrathecal injection (i. t., 0.50 mg/kg) using the direct lumbar puncture method, as previously described60.
Rotarod test for assessing motor function and learning
The balance and motor coordination of Gfap-hM3Dq mice and their WT littermate controls were tested on an accelerating rotarod, as previously described25. Speed (RPM) was set at an initial value of 3, with a progressive increase to a maximum of 30 RPM during a 5-min trial. CNO (0.25 mg/kg) was given 15 min prior to the first trial. Mice were pretreated with saline or 20 mg/kg trospium27 15 min prior to injection of CNO. Each mouse underwent a training session consisting of three trials, with 45 s between each trial. The latency time to fall, or to rotate fully around the turning barrel, was recorded.
Chemical sympathectomy
Chemical sympathectomy was performed by two 6-hyadroxydopamine (6-OHDA; 150 mg/kg in 0.1% ascorbic acid, i. p.) injections three days apart36 to trigger sympathetic denervation in peripheral organs including sensory ganglia. The α-adrenergic receptor blocker phentolamine (150 µg/kg, i. p.) was injected with the first 6-OHDA injection to protect animals from massive release of catecholamines associated with 6-OHDA administration36. Saline-injected Gfap-hM3Dq animals received two 0.1% ascorbic acid injections, and a phentolamine injection with the first ascorbic acid injection. This treatment regimen has been proven effective in eliminating sympathetic nerve-released catecholamines27,36,38. Von Frey tests were performed 3 days after the second 6-OHDA injection27.
Pharmacogenetic and pharmacological manipulations
Clozapine-N-Oxide (CNO, powder form, provided by the NIH through B.L. Roth) was dissolved in DMSO at 1 mg/mL, and then diluted in physiological saline to applicable concentration. CNO was administered i. p. at 0.25 mg/kg25,27 (0.125% final DMSO concentration), unless otherwise indicated. Trospium Chloride (Toronto Research Chemicals) was diluted in physiological saline and administered i. p. at 20 mg/kg27. 8-(p-Sulfophenyl) theophylline hydrate (SPT) and 8-Cyclopentyl-1,3-dipropylxanthin (CPX) were purchased from Sigma Aldrich (Milwaukee, WI). Each drug was initially dissolved in DMSO (10 mg/mL), and then diluted to working concentration with physiological saline. The non-selective, blood–brain-barrier impermeable adenosine receptor antagonist SPT was delivered at 10 mg/kg61. The selective A1R antagonist CPX was delivered at 1 mg/kg61.
Statistics
The basal sensitivity between genotypes in the Hargreave’s test was analyzed using two-tailed independent samples t-test. All other experiments were analyzed using two-way ANOVA with genotype or drug as between subjects factors, and time as a repeated measure, with Fisher’s Least Significant Difference (LSD) post-hoc analysis, as needed. Statistics were performed using Statistica 12 (Dell, Tulsa, OK), and the figures were generated using Graphpad Prism 7.04 (La Jolla, CA; https://www.graphpad.com/scientific-software/prism/).
Statement of ethical approval
The study was approved by the Institutional Animal Care and Use Committee (IACUC) of the UNC-CH (protocol 13-276.0). All experiments were performed exclusively in UNC-CH and in accordance with the relevant guidelines and regulations.
References
Ji, R., Andrea, N., Huh, Y., Terrando, N. & Maixner, W. Neuroinflammation and central sensitization in chronic and generalized pain. Anestesiología 19, 343–366 (2018).
Gold, M. S. & Gebhart, G. F. Nociceptor sensitization in pain pathogenesis Michael. Mater. Med. 16, 1248–1257 (2010).
Ji, R., Berta, T. & Nedergaard, M. Glia and pain: Is chronic pain a gliopathy?. Pain 154, S10–S28 (2013).
Gosselin, R., Suter, M. R. & Ji, R. Glial cells and chronic pain. Neuroscientist 16, 519–531 (2011).
Honore, P. et al. Murine models of inflammatory, neuropathic and cancer pain each generates a unique set of neurochemical changes in the spinal cord and sensory neurons. Neuroscience 98, 585–598 (2000).
Echeverry, S., Shi, X. Q. & Zhang, J. Characterization of cell proliferation in rat spinal cord following peripheral nerve injury and the relationship with neuropathic pain. Pain 135, 37–47 (2008).
Donegan, M., Kernisant, M., Cua, C., Jasmin, L. & Ohara, P. T. Satellite glial cell proliferation in the trigeminal ganglia after chronic constriction injury of the infraorbital nerve. Glia 61, 2000–2008 (2013).
Vera-Portocarrero, L. P. et al. Rapid changes in expression of glutamate transporters after spinal cord injury. Brain Res. 927, 104–110 (2002).
Lepore, A. C. et al. Spatial and temporal changes in promoter activity of the astrocyte glutamate transporter GLT1 following traumatic spinal cord injury. J. Neurosci. Res. 89, 1001–1017 (2011).
Putatunda, R., Hala, T. J., Chin, J. & Lepore, A. C. Chronic at-level thermal hyperalgesia following rat cervical contusion spinal cord injury is accompanied by neuronal and astrocyte activation and loss of the astrocyte glutamate transporter, GLT1, in superficial dorsal horn. Brain Res. 1581, 64–79 (2014).
Watson, J. L., Hala, T. J., Putatunda, R., Sannie, D. & Lepore, A. C. Persistent at-level thermal hyperalgesia and tactile allodynia accompany chronic neuronal and astrocyte activation in superficial dorsal horn following mouse cervical contusion spinal cord injury. PLoS ONE 9, e109099 (2014).
Olsen, M. L., Campbell, S. C., McFerrin, M. B., Floyd, C. L. & Sontheimer, H. Spinal cord injury causes a wide-spread, persistent loss of Kir4.1 and glutamate transporter 1: Benefit of 17β-oestradiol treatment. Brain 133, 1013–1025 (2010).
Chen, G. et al. Connexin-43 induces chemokine release from spinal cord astrocytes to maintain late-phase neuropathic pain in mice. Brain 137, 2193–2209 (2014).
Hanani, M. Intercellular communication in sensory ganglia by purinergic receptors and gap junctions: Implications for chronic pain. Brain Res. 1487, 183–191 (2012).
Ohara, P. T., Vit, J.-P., Bhargava, A. & Jasmin, L. Evidence for a role of connexin 43 in trigeminal pain using RNA interference in vivo. J. Neurophysiol. 100, 3064–3073 (2008).
Ji, R., Chamessian, A. & Zhang, Y. Pain regulation by non-neuronal cells and inflammation. Pain Res. 354, 572–577 (2016).
Zhang, X., Chen, Y., Wang, C. & Huang, L.-Y.M. Neuronal somatic ATP release triggers neuron-satellite glial cell communication in dorsal root ganglia. Proc. Natl. Acad. Sci. U. S. A. 104, 9864–9869 (2007).
Kim, D. et al. Thrombospondin-4 contributes to spinal sensitization and neuropathic pain states. J. Neurosci. 32, 8977–8987 (2012).
Jiang, B. et al. CXCL13 drives spinal astrocyte activation and neuropathic pain via CXCR5. J. Clin. Investig. 126, 745–761 (2016).
Ohtori, S., Takahashi, K., Moriya, H. & Myers, R. R. TNF-alpha and TNF-alpha receptor type 1 upregulation in glia and neurons after peripheral nerve injury: Studies in murine DRG and spinal cord. Spine (Phila. Pa. 1976). 29, 1082–1088 (2004).
Peters, C. M., Jimenez-Andrade, J. M., Kuskowski, M. A., Ghilardi, J. R. & Mantyh, P. W. An evolving cellular pathology occurs in dorsal root ganglia, peripheral nerve and spinal cord following intravenous administration of paclitaxel in the rat. Brain Res. 1168, 46–59 (2007).
Kim, S. K. et al. Cortical astrocytes rewire somatosensory cortical circuits for peripheral neuropathic pain. J. Clin. Investig. 126, 1983–1997 (2016).
Watkins, L. R. & Maier, S. F. Glia: A novel drug discovery target for clinical pain. Nat. Rev. Drug Discov. 2, 973–985 (2003).
Takeda, M., Takahashi, M. & Matsumoto, S. Contribution of activated interleukin receptors in trigeminal ganglion neurons to hyperalgesia via satellite glial interleukin-1β paracrine mechanism. Brain Behev. Immun. 22, 1016–1023 (2008).
Agulhon, C. et al. Modulation of the autonomic nervous system and behaviour by acute glial cell Gq protein-coupled receptor activation in vivo. J. Physiol. 591, 5599–5609 (2013).
Bonder, D. E. & McCarthy, K. D. Astrocytic Gq-GPCR-linked IP3R-dependent Ca2+ signaling does not mediate neurovascular coupling in mouse visual cortex in vivo. J. Neurosci. 34, 13139–13150 (2014).
Xie, A. X., Lee, J. J. & McCarthy, K. D. Ganglionic GFAP+ glial Gq-GPCR signaling enhances heart functions in vivo. JCI Insight 2, 1–20 (2017).
McClain, J. L., Fried, D. E. & Gulbransen, B. D. Agonist-evoked Ca2+ signaling in enteric glia drives neural programs that regulate intestinal motility in mice. C. Cell. Mol. Gastroenterol. Hepatol. 1, 631–645 (2015).
Armbruster, B. N., Li, X., Pausch, M. H., Herlitze, S. & Roth, B. L. Evolving the lock to fit the key to create a family of G protein-coupled receptors potently activated by an inert ligand. Proc. Natl. Acad. Sci. U. S. A. 104, 5163–5168 (2007).
Ren, K. & Dubner, R. Inflammatory models of pain and hyperalgesia. ILAR J. 40, 111–118 (1999).
Dubin, A. E. D. & Patapoutian, A. Nociceptors: The sensors of the pain pathway. J. Clin. Investig. 120, 3760–3772 (2010).
Wang, X. et al. Gene transfer to dorsal root ganglia by intrathecal injection: Effects on regeneration of peripheral nerves. Mol. Ther. 12, 314–320 (2005).
Zhou, X. et al. Satellite-cell-derived nerve growth factor and neurotrophin-3 are involved in noradrenergic sprouting in the dorsal root ganglia following peripheral nerve injury in the rat. Eur. J. Neurosci. 11, 1711–1722 (1999).
McLachlan, E. M. Diversity of sympathetic vasoconstrictor pathways and their plasticity after spinal cord injury. Clin. Auton. Res. 17, 6–12 (2007).
Hu, P. & McLachlan, E. M. Distinct sprouting responses of sympathetic and peptidergic sensory axons proximal to a sciatic nerve transection in guinea pigs and rats. Neurosci. Lett. 295, 59–63 (2000).
Ferrari, A. U., Daffonchio, A., Franzelli, C. & Mancia, G. Potentiation of the baroreceptor-heart rate reflex by sympathectomy in conscious rats. Hypertension 18, 230–235 (1991).
Kostrzewa, R. M. & Jacobowitz, D. M. Pharmacological actions of 6-hydroxydopamine. Pharmacol. Rev. 26, 199–288 (1974).
Marano, G., Ramirez, A., Mori, I. & Ferrari, A. U. Sympathectomy inhibits the vasoactive effects of nicotine in conscious rats. Cardiovasc. Res. 42, 201–205 (1999).
Bura, S. A., Nadal, X., Ledent, C., Maldonado, R. & Valverde, O. A2A adenosine receptor regulates glia proliferation and pain after peripheral nerve injury. Pain 140, 95–103 (2008).
Pekny, M. et al. Mice lacking glial fabrillary acidic protein display astrocytes devoid of intermediate filaments buu develop and reproduce normally. EMBO J. 14, 1590–1598 (1995).
Hanani, M. Satellite glial cells in sensory ganglia: From form to function. Brain Res. Brain Res. Rev. 48, 457–476 (2005).
Hanani, M. Satellite glial cells in sympathetic and parasympathetic ganglia: In search of function. Brain Res. Rev. 64, 304–327 (2010).
Xie, A. X., Chaia, A. I. & McCarthy, K. D. Targeting sympathetic glia for treating cardiovascular diseases. Recept. Clin. Investig. 4, e1572 (2017).
Gu, Y. et al. Neuronal soma-satellite glial cell interactions in sensory ganglia and the participation of purinergic receptors. Neuron Glia Biol. 6, 53–62 (2010).
Zhang, J. M. et al. ATP released by astrocytes mediates glutamatergic activity-dependent heterosynaptic suppression. Neuron 40, 971–982 (2003).
Chen, Y. et al. Activation of P2X7 receptors in glial satellite cells reduces pain through downregulation of P2X3 receptors in nociceptive neurons. Proc. Natl. Acad. Sci. U. S. A. 105, 16773–16778 (2008).
Kobayashi, K. et al. Differential expression patterns of mRNAs for P2X receptor subunits in neurochemically characterized dorsal root ganglion neurons in the rat. J. Comp. Neurol. 481, 377–390 (2005).
Zhang, X. F., Han, P., Faltynek, C. R., Jarvis, M. F. & Shieh, C. C. Functional expression of P2X7 receptors in non-neuronal cells of rat dorsal root ganglia. Brain Res. 1052, 63–70 (2005).
Xie, A. X., Petravicz, J. & McCarthy, K. D. Molecular approaches for manipulating astrocytic signaling in vivo. Front. Cell. Neurosci. 9, 144 (2015).
McLachlan, E. M. & Hu, P. Inflammation in dorsal root ganglia after peripheral nerve injury: Effects of the sympathetic innervation. Auton. Neurosci. 182, 108–117 (2014).
O’Connell, N. E. et al. Local anaesthetic sympathetic blockade for complex regional pain syndrome. Cochrane Database Syst. Rev. 2016, 1–57 (2016).
Straube, S., Derry, S., Ra, M. & Cole, P. Cervico-thoracic or lumbar sympathectomy for neuropathic pain and complex regional pain syndrome. Cochrane Libr. https://doi.org/10.1002/14651858.CD002918.pub3.www.cochranelibrary.com (2014).
Chang, C., McDonnell, P. & Eric Gershwin, M. Complex regional pain syndrome—False hopes and miscommunications. Autoimmun. Rev. https://doi.org/10.1016/j.autrev.2018.10.003 (2019).
Staud, R., Koo, E., Robinson, M. E. & Price, D. D. Enhanced central pain processing of fibromyalgia patients is maintained by muscle afferent input: A randomized, double- blind, placebo controlled study. Pain 130, 177–187 (2008).
Nelson, E. E. & Guyer, A. E. Widespread hyperalgesia in irritable bowel syndrome is dynamically maintained by tonic visceral impulse input and placebo/nocebo factors: Evidence from human psychophysics, animal models, and neuroimaging. Neuroimage 1, 233–245 (2012).
Bender, D., Holschbach, M. & Stöcklin, G. Synthesis of n.c.a. carbon-11 labelled clozapine and its major metabolite clozapine-N-oxide and comparison of their biodistribution in mice. Nucl. Med. Biol. 21, 921–925 (1994).
Gimenez-Llort, L. et al. Mice lacking the adenosine A1 receptor are anxious and aggressive, but are normal learners with reduced muscle strength and survival rate. Eur. J. Neurosci. 16, 547–550 (2002).
Ledent, C., Vaugeois, J., Schiffmann, S., Pedrazzini, T. & Yacoubi, M. Aggressiveness, hypoalgesia and high blood pressure in mice lacking the adenosine A2a receptor. Nature 388, 674–678 (1997).
Cobos, E. J. et al. Inflammation-induced decrease in voluntary wheel running in mice, a nonreflexive test for evaluating inflammatory pain and analgesia. Pain 153, 876–884 (2012).
Fairbanks, C. A. Spinal delivery of analgesics in experimental models of pain and analgesia. Adv. Drug Deliv. Rev. 55, 1007–1041 (2003).
Anderson, R., Sheehan, M. J. & Strong, P. Characterization of the adenosine receptors mediating hypothermia in the conscious mouse. Br. J. Pharmacol. 113, 1386–1390 (1994).
Acknowledgements
We thank Dr. Stephen Tilley (UNC-CH) for providing the adenosine receptor knock out mice; Kristen M. Boyt (Kash laboratory, UNC-CH) for generating and characterizing Gfap-hM3Dq mice; Dr. Sarah Taves for initiating this project and helpful discussions; two talented undergraduate research assistants, Robert Ladd (UNC-CH) and Jakovin J. Lee (University of South Carolina) for performing some of the Von Frey experiments. This work was supported by the CCTSI Pilot Award CO‐M‐19‐7 (to A.X.X.), NIH/NINDS grant NS058904 (to K.D.M.), and NIH/NIDDK grant DK121506 (to A.P.M.).
Author information
Authors and Affiliations
Contributions
A.X.X., A.M., S.K.M., and K.D.M. designed and conducted the experiments, A.M. analyzed data, A.X.X. and A.P.M. drafted the manuscript. All authors have read and approved this manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Xie, A.X., Madayag, A., Minton, S.K. et al. Sensory satellite glial Gq-GPCR activation alleviates inflammatory pain via peripheral adenosine 1 receptor activation. Sci Rep 10, 14181 (2020). https://doi.org/10.1038/s41598-020-71073-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-020-71073-z
- Springer Nature Limited