Abstract
There have been no new drugs for the treatment of schizophrenia in several decades and treatment resistance represents a major unmet clinical need. The drugs that exist are based on serendipitous clinical observations rather than an evidence-based understanding of disease pathophysiology. In the present review, we address these bottlenecks by integrating common, rare, and expression-related schizophrenia risk genes with knowledge of the druggability of the human genome as a whole. We highlight novel drug repurposing opportunities, clinical trial candidates which are supported by genetic evidence, and unexplored therapeutic opportunities in the lesser-known regions of the schizophrenia genome. By identifying translational gaps and opportunities across the schizophrenia disease space, we discuss a framework for translating increasingly well-powered genetic association studies into personalized treatments for schizophrenia and initiating the vital task of characterizing clinically relevant drug targets in underexplored regions of the human genome.
Similar content being viewed by others
Introduction
Schizophrenia is a complex and heterogeneous syndrome, affecting ~1% of the population and characterized by debilitating positive, negative, and cognitive symptoms in addition to severe comorbidities1,2,3. Despite the enormous burden on worldwide health including 1.9–2.8% of total years lived with disability4,5 and a 10–20 year reduction in life expectancy3,6, no drugs with novel mechanisms of action have emerged in the last three decades. Current antipsychotic medications only achieve full symptom remission in 15–25% of affected individuals7,8 and adverse side-effects such as weight gain, metabolic disturbances, over-sedation, extrapyramidal symptoms, and agranulocytosis9,10 are persistent problems. This is largely due to a lack of understanding of schizophrenia pathophysiology, incomplete characterization of the molecular targets of existing drugs, a scarcity of relevant preclinical models, and an inability to accurately predict treatment response as a result of disease heterogeneity11,12,13,14. In addition to these challenges, the increased rate of late-stage clinical trial failures and extended clinical development times for central nervous system (CNS) drug candidates15,16 has further dissuaded the pharmaceutical industry from pursuing novel drugs for schizophrenia.
In light of many of these difficulties, there has been renewed interest in recent years in drug repurposing, in other words, the identification of novel therapeutic indications for regulatory approved drugs17, in schizophrenia. The advantage of this strategy is that existing pharmacokinetic, dosing, toxicology and medicinal chemistry profiles of the drug candidates18 serve to expedite clinical trials in the new indication and reduce the costly attrition rate (~90%), associated with most novel drug entities19 particularly those aimed at neuropsychiatric indications. In many ways, this represents a return to the origins of schizophrenia drug discovery in the 1950s, when serendipitous clinical observation of the antipsychotic properties of drugs used in other indications, such as the pre-anesthetic chlorpromazine, laid the mechanistic foundation for the majority of monoaminergic drugs used today10,13,20. Although these monoaminergic compounds, which focus on differential dopamine and serotonin (5HT) receptor antagonism, have revolutionized the treatment of schizophrenia, many patient subgroups and symptom subdomains (e.g., negative symptoms and cognitive deficits) remain resistant to treatment21,22. A range of repurposing clinical trials3,6,21,22 have shown modest effect sizes in subgroups of patients. However low sample numbers, adjunctive administration protocols in chronically ill patients, and incomplete patient stratification have limited their applicability23.
The recent identification of genetic susceptibility loci for schizophrenia through large-scale genetic association studies suggests that each patient is likely to have a different combination of common but weak (weak effect on phenotype), or rare but penetrant (strong effect on phenotype), risk alleles24,25,26. These include over 138 schizophrenia risk loci identified in genome-wide association studies (GWAS) of common variation26,27, eight genome-wide significant loci affected by rare chromosomal copy number variants (CNV)28 and ultra-rare disruptive or de novo mutations which are enriched for gene sets involved in synaptic transmission29,30. Phenome-wide association studies (PheWAS)31,32, which correlate individual SNPs to multiple phenotypes, and transcriptome-wide association studies (TWAS)33, which integrate GWAS risk loci with genetic predictors of expression, have suggested further susceptibility genes. While these studies have provided support for existing schizophrenia drug targets, such as the dopamine 2 receptor (DRD2), they also offer an opportunity to identify drug targets which are not dependent on prior hypotheses of schizophrenia pathophysiology or the mechanisms of action of existing drugs. GWAS analyses in other disease indications have linked single-nucleotide polymorphisms (SNPs) in risk genes to widespread drug efficacy34. Examples include the interleukin-6 receptor gene, targeted by tocilizumab, in rheumatoid arthritis35 and the HMG-CoA reductase gene, targeted by statins, in conditions with elevated low-density lipoprotein cholesterol34.
One approach for prioritizing drug targets from disease association studies is to interpret the results in light of drug target annotation databases. The mechanism of action of many approved drugs is still subject to debate36,37 with comprehensive target lists more than doubling in recent times (266 in 200638 vs. 667 in 201737). This is due to improvements in drug–gene target mapping and the annotation of multi-target efficacies, complex subunits, and isoforms. Moreover, the fact that currently approved drugs only target a small fraction (3%) of the human proteome, relative to the estimated 15–35% of potentially druggable genes (i.e., genes which code for protein drug targets)39,40, has spurred efforts to characterize lesser studied human proteins and track their target development41. This has led to several market approvals in recent years including receptor deorphanization (i.e., identification of ligands for receptors which are predicted based on genetic or protein sequence information but for which endogenous ligands were previously unknown) for CNS targets HCRTR1/2 and S1PR1 genes to treat insomnia and multiple sclerosis respectively41. Nevertheless, recent analyses suggest that very little is known about ~40% of protein-coding genes in the human genome and that integration of diverse biomedical databases can provide a powerful tool for prioritizing underexplored drug targets41.
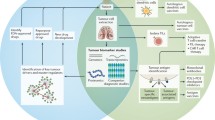
Here we bring together the results of major studies exploring genetic association to schizophrenia to provide a consolidated list of risk and protective genes (Fig. 1). These include sources of common variants identified using GWAS and PheWAS, rare variants identified through CNV analysis and sequencing of disruptive or de novo exon mutations, and genes with altered tissue-specific expression identified using RNA-sequencing and TWAS analysis. We cross-reference the schizophrenia-associated genes with a comprehensive list of FDA-approved drug targets and indications to provide an update on immediate repurposing opportunities for schizophrenia. Moreover, we compare the protein class distribution of these potential repurposing targets with that of drugs currently in clinical repurposing trials for schizophrenia to identify which clinical trial candidates are supported by genetic evidence and which risk genes are yet to be targeted using approved drugs. Finally, we use extended compound annotation resources developed by the illuminating the Druggable Genome (IDG) initiative to prioritize the repurposing drug targets and elucidate unexplored therapeutic opportunities within the schizophrenia genome.
Shows workflow described in Methods. Blue references are source studies of schizophrenia-associated genes. Red references represent cross-referencing resources used to annotate schizophrenia-associated genes and clinical trial drugs respectively. Uniprot refers to www.uniprot.org. Steps shown include the input of schizophrenia risk genes from source studies (a), identification of clinical repurposing targets suggested by genetic association studies (b, c), annotation of the targets of schizophrenia repurposing clinical trial drugs (d), comparison of the protein class distributions of targets suggested by genetic analyses and the schizophrenia clinical repurposing pipeline (e), annotation of genome-wide significant targets with IDG target development levels (f, g), prioritization of repurposing opportunities and unexplored therapeutic opportunities within the schizophrenia genome based on extended IDG target metadata (h). *Indicates studies reporting genome-wide significance, used for analyses focusing on genome-wide significance P values. + Indicates “T clinical” and “T clinical repurposing” target labels derived from steps (b–d).
Results and discussion
Comparison of targets from genetic association studies and the clinical repurposing pipeline
A total of, 748 unique genes were associated with schizophrenia by analysis of common, rare, and gene expression variation (Fig. 1; Methods; and Supplementary Data 1)25,26,27,28,33,42,43,44,45,46. From these, 56 genes mapped to the known protein targets of 187 approved drugs (termed “druggable” genes, Supplementary Data 2) as defined by the Santos et al. list of comprehensive FDA-approved drug targets37. Overall, 24, 17 and seven genes were unique to studies of common, rare, and expression variation respectively, with the remaining eight genes (C4A, CACNA1C, CACNB2, CYP2D6, GRIN2A, GRIN2B, KCNB1, and NDUFA2) represented in at least two types of analysis. Of the druggable genes, 27 (48%) have not yet been targeted in clinical trials for schizophrenia23 representing novel repurposing opportunities. Conversely, the 89 drugs listed in clinical repurposing trials for schizophrenia23 mapped to 76 unique human targets, of which 23 (26%) were supported by genetic evidence (Supplementary Data 3), suggesting that a significant proportion of the clinical repurposing pipeline is supported by direct genetic target associations, with a potentially larger share implicated by indirect or downstream targets35. Comparison of the protein class distributions of drug targets implicated by genetic studies (Fig. 2a) relative to repurposing clinical trials (Fig. 2b) revealed a series of established (widely tested in clinical trials), emerging (scarcely tested in clinical trials), and novel (untested in clinical trials) repurposing targets. In broad terms, ion channels were enriched among genetic targets (40% of targets) relative to clinical trials (22%), G-protein-coupled receptors (GPCRs), or seven-pass-transmembrane domain receptors (7TMs), transporters and nuclear transcription factors were reduced in the genetic results (9, 2, and 4% respectively) relative to drugs in clinical trials (17, 16, and 6% respectively). The enzyme class showed similar representation (29–30%) although with notable differences in composition.
a Protein class distribution of 56 schizophrenia-associated genes (out of a total of 748)25,26,27,28,33,42,43,44,45,46 which are targeted by approved drugs (n = 187)37. Each segment concentrically shows the ChEMBL database protein target classification37, followed by the target gene (HUGO Gene Nomenclature Committee) and the source of genetic association in terms of analyses of common26,27,42,44 (C), rare25,28,43 (R), and gene expression33,45,46 (E) variation. Gene targets which match the targets of drugs in clinical repurposing trials for schizophrenia23 (n = 29) are shown in bold. b Protein class distribution of 76 human drug targets of approved drugs (n = 86) in clinical repurposing trials for schizophrenia. Each segment concentrically shows the ChEMBL protein target classification, followed by the ChEMBL drug target (individual proteins/protein complexes)37. The width of each drug target segment is proportional to the number of drugs associated with that target in clinical repurposing trials for schizophrenia. Some drugs have more than one target annotation (average 1.2). Drug targets which are supported by direct genetic evidence (n = 23) are shown in bold. Major protein target classes are colored as follows ion channel (green), membrane receptor (membrane R; turquoise), secreted (navy), structural (yellow), surface antigen (SA; red), transcription factor (TF; purple), transporter (pink), auxiliary transport protein (ATP; peach), enzyme (brown), enzyme modulator (EM; dark green), and epigenetic regulator (ER; orange). 7TM seven-pass-transmembrane domain receptors.
Established repurposing targets
Disease associations for subunits of nicotinic ACh receptor subtypes (e.g., CHRNA3 and CHRNB4) and Glu receptor subtypes (e.g., NMDA receptor—GRIN2A, GRIN2B, and GRIN1; AMPA receptor—GRIA1 and GRIA4; and kainite receptor—GRIK1) support the most extensive areas of repurposing activity, in terms of the number of clinical trials conducted, using glutamatergic (e.g., d-cycloserine and memantine) and cholinergic (e.g., galantamine, donepezil, and varenicline) cognitive enhancers23. Although clinical trials for these targets have met with mixed results23 the genetic data suggest that larger and well-controlled clinical trials employing key class derivatives might be warranted. In contrast, drugs related to monoaminergic, anti-inflammatory, metabolic, and hormonal mechanisms of action occupy a smaller target proportion in the genetic data relative to clinical trials. However, the clinical efficacy of subtypes of immune and metabolic compounds in subsets of patients, including the treatment of side-effects of medication, points to the fact that the genetically defined targets may not currently capture the full gamut of therapeutic possibilities.
Emerging repurposing targets
Several target classes were strongly suggested by genetic evidence yet are relatively under-represented as direct targets in clinical trials. Principal among these were the CaV channel subunit genes which, when considering primary and auxiliary subunits, accounted for 21% of the genetic target space yet only 3% of clinical trial targets. L-type (CACNA1C and CACNB2) and T-type (CACNA1I) CaV channel subunits were among the most significant findings to emerge from GWAS studies in terms of reproducibility, significance, sole occupation of respective risk loci, and the fact that the primary risk SNPs for each gene are within the gene itself26,27. These findings are supported by further L-type (CACNA1S and CACNB4), T-type (CACNA1H), N-type (CACNA1B), R-type (CACNA1E), and auxiliary (CACNA2D1–4) CaV channel subunit associations from rare disruptive43 and de novo mutation47 exome sequencing and gene expression analysis46. Although the pathophysiological mechanisms involving CaV channels are not well understood, the fundamental role of CaV channels in neuronal signaling, gene transcription, and neurotransmitter trafficking makes them plausible targets48,49. This is supported by evidence that carriers of the principal L-type CaV channel risk allele show alterations in CACNA1C expression and fMRI connectivity in key schizophrenia-associated brain regions50,51.
Despite this evidence, only five approved CaV channel blockers are currently being tested for schizophrenia23, representing under 3% of current clinical trials. Interestingly, L-type CaV channel blockers were tested in several clinical repurposing trials for schizophrenia prior to the publication of the human genome. However, these clinical trials showed heterogeneous outcomes35. For example, verapamil improved positive symptoms in acute patients but showed no effects in chronic patients, nilvadipine improved negative symptoms with no change in positive symptoms in chronic patients and nifedipine had no effect in chronic patients but improved cognitive symptoms in patients with tardive dyskinesia35. The heterogeneous results obtained from these clinical trials could in part be explained by small sample sizes, difficulties in controlling for clinical variables, the inclusion of chronic treatment-resistant patients, and low brain penetrance of some of the compounds (e.g., verapamil)35. Phenotypic screening in schizophrenia patient samples has subsequently highlighted that 1,4-dihydropyridine (DHP) L-type CaV channel blockers with extended ester substitutions at the third position of the pyridine ring might be more therapeutically relevant derivatives52. Taken together these findings suggest that CaV channels, particularly L-type channels, with a wealth of approved drugs available, warrant further investigation as potential repurposing targets.
Another genetically associated target class which is under-represented in the clinical trial pipeline are the mitochondrial complex 1 (NADH dehydrogenase) subunits accounting for 9% of the genetic targets (NDUFA13, NDUFA2, NDUFA4L2, NDUFA6, and NDUFAF2) and only 1% of the clinical repurposing targets (NADH dehydrogenase). Although this is largely due to the implication of multiple subunits within a single protein complex, the clustering of risk variants from different genetic loci within the same complex nevertheless makes this a plausible drug target. This finding is supported by evidence of mitochondrial dysfunction in postmortem brain tissue53 and a positive correlation between blood mRNA expression of mitochondrial complex 1 subunits and psychotic symptoms54 in schizophrenia. However, metformin, which is the only drug annotation associated with mitochondrial complex 1, has proved ineffective in clinical trials for schizophrenia55 suggesting that targeting this protein may require other ligands56.
Novel repurposing targets
Several drug targets which showed significant evidence of genetic association and were matched to approved drugs have not been tested in clinical trials, representing novel repurposing opportunities. Foremost among these were different subfamilies (B, G, KQT, V, and cGMP) of KV channels (KCNB1, KCNG2, KCNQ1, KCNQ5, KCNV1, and HCN1), further supported by mouse neurophenotypes and relative disease and pathway specificities (described below). KCNB1 was notable as it was supported by both common variation and expression while HCN1 had a higher level of ChEMBL activity and neurophenotype annotation. Limited evidence of KVs in schizophrenia includes increased KCNB1 expression in neocortical developmental stages associated with schizophrenia57 and behavioral abnormalities reminiscent of schizophrenia in KCNB1-AMIGO functional knockout mice58. HCN1 is strongly expressed in the dendrites of pyramidal cells in the cortex and hippocampus and is suggested to be involved in working memory and dendritic spine abnormalities in schizophrenia59,60. Importantly, KV channels work in concert with many of the aforementioned CaV channels to regulate neuronal excitability and neurotransmitter release59, representing a point of functional convergence between these genetic risk loci. They are also involved in physiological comorbidities of schizophrenia such as insulin resistance61. Approved drugs targeting KV risk genes include dalfampridine, ezogabine, guanidine, dronedarone, and ivabradine although the brain penetrance and side effect profiles of these compounds vary drastically. Additionally, drugs such as lamotrigine, gabapentin35, or the antiarrhythmic ibutilide, which was shown to ameliorate schizophrenia-associated cellular responses in phenotypic screens52, may serve to modulate KV function indirectly.
Other potentially novel repurposing opportunities supported by mouse neurophenotypes included cytochrome P450 enzymes, protein tyrosine kinases, mACh receptor, and B-cell surface marker. The cytochrome P450 enzymes are targeted by abiraterone and ketoconazole (CYP17A1) and quinidine (CYP2D6) respectively. CYP17A1 is notable as a key enzyme required for the production of glucocorticoids and sex hormones, such as estrogen, which are linked to schizophrenia62,63,64, while CYP2D6 is responsible for the dopamine synthesis in the brain65. Interestingly, CYP2D6 is also involved in the metabolism of antipsychotic medications, with direct implications for their pharmacokinetics and clinical efficacy66,67,68, suggesting that compounds targeting CYP2D6 may have potential as adjunctive medications. Protein tyrosine kinases (FGFR2, MET, PDGFR, FYN, and TEK) are notable as they indicate a highly druggable target class37 which has supported an increasing number drug approvals in recent years. However, toxicity and target characterization continue to represent significant hurdles. FGF2 is a key mediator of neurogenesis and cortical patterning relevant to neurodevelopmental models of schizophrenia69 and both FGFR2 and FYN interact with targets (PLC-γ1 and Src respectively) suggested by phenotypic screening52. Targeting the mACh receptor (CHRM4) is consistent with a renewed interest in selective mACh allosteric modulators for the treatment of schizophrenia70 and a significant increase in the grant funding behind CHRM4 in recent years23. Finally, B-cell surface antigen CD19 is notable with respect to functional abnormalities71,72 and genetic implications of B cells in schizophrenia26, although the targeting of this protein would require further elucidation given the importance of B cells in the immune response.
Prioritization of repurposing opportunities in schizophrenia
We sought to prioritize genetically supported repurposing opportunities in terms of practicality and novelty by cross-referencing a subset of druggable37 schizophrenia risk genes, from GWAS26,27 (n = 22), TWAS33 (n = 4), and CNV28 (n = 2) reference studies reporting genome-wide significance, with extended target annotation resources of the human genome curated by the IDG initiative (Fig. 1; Methods; and Supplementary Data 1)41. Comparison of the number of approved drugs available relative to the genome-wide association significance for each target per study (Fig. 3a) revealed that several of the most significant target genes with multiple drugs available (e.g., CaV channel subunits- CACNA1C, CACNB2, and CACNA1I, nicotinic acetylcholine (nACh) receptor subunits—CHRNA3 and CHRNB4, and GluR subunits GRIN2A and GRIA1) are already being targeted in clinical repurposing trials for schizophrenia. The gene with the highest number of approved drugs was DRD2 reflecting existing approvals for antipsychotic drugs in schizophrenia.
Shows genome-wide significant schizophrenia risk genes, from GWAS26,27 (n = 22, square), TWAS33 (n = 4, triangle), and CNV28 (n = 2, circle) reference studies, which are targeted by approved drugs37. Genes which have been targeted in clinical repurposing trials for schizophrenia23 are shown in red and novel repurposing opportunities are shown in blue. Axes comprise genome-wide significant P values from the respective studies cross-referenced with extended molecular drug target annotations for each gene37,41. Plots highlight gene ‘druggability’ in terms of a the number of FDA-approved drugs available and b abundance of chemical-target interaction data in the ChEMBL database, in addition to c CNS relevance in terms of the number of synaptic pathway annotations (Pathway Commons, KEGG, Reactome databases) and neurophenotypes resulting from orthologous gene mutations in mice (Mouse Genome Informatics database; NA—no phenotype data available, 0—non-neurophenotypes, 1—either MP:0003631 “nervous system phenotype” or MP:0005386 “behavior/neurological phenotype”, 2—both MP:0003631 “nervous system phenotype” or MP:0005386 “behavior/neurological phenotype”), d specificity in terms of total cellular pathway annotations (Pathway Commons, KEGG, Reactome databases) and disease associations and e commercial viability in terms of associated National Institutes of Health (NIH) grant expenditures (2000–2015) and total European Bioinformatics Institute (EMBL-EBI) patent counts. P values from different TWAS expression reference panels are represented as discrete points. Genes are labeled using standardized nomenclature (HUGO Gene Nomenclature Committee).
Of the genes which are not currently direct clinical trial targets, CYP17A1 was the most significant among the GWAS data and the muscarinic ACh receptor (CHRM4) had the largest number of available drugs. Other genes, which are not currently targeted in clinical trials, with intermediate significance and drug availability included KV channel subunits (KCNV1, KCNG2, KCNB1, and HCN1) and tyrosine kinases (FYN and TEK). To further prioritize the druggable genes, we assessed the amount of chemical-target interaction data in the ChEMBL database for each gene (Fig. 3b). This revealed several as yet untargeted genes which had greater functional target annotation than those which are already targeted in clinical trials for schizophrenia, including CYP17A1, TEK, CHRM4, CA14, and FYN.
Comparison of the relative implication of the druggable genes in synaptic pathways and orthologous nervous system or behavioral/neurological phenotypes (“neurophenotypes”) in transgenic mice (Fig. 3c), revealed that the majority of genes which are already targeted in schizophrenia have a high number of synaptic pathway annotations and mouse neurophenotypes. However, several of the untargeted risk genes such as HCN1, FYN, CHRM4, and CD19 and to a lesser extent CYP17A1, TEK, KCNB1, and KCNV1 were associated with mouse neurophenotypes, despite a low level of synaptic annotation, suggesting that these genes may be linked to pathophysiological mechanisms in the CNS which are either not fully characterized or fall beyond the scope of synaptic abnormalities. Exploration of genetic disease pleiotropy (i.e., the effect of single genes on multiple diseases) vs. pathway promiscuity (i.e., the involvement of single genes across multiple pathways) (Fig. 3d) suggested that while untargeted genes such as CYP17A1, CYP2D6, and CD19 are relatively promiscuous in terms of their cellular pathway and physiological disease effects, other genes such as KCNB1, KCNV1, KCNG2, and HCN1 are relatively specific to a subset of known pathways and schizophrenia. Finally, assessment of the drug development opportunities for currently untargeted druggable schizophrenia genes, by comparing grant expenditure with EBI patent counts (Fig. 3e), suggested that while patent numbers for the majority of the genes correlate with research expenditure, some genes such as CYP17A1, CYP2D6, and CD19 have resulted in relatively few patents, despite large investment, whereas genes like CHRM4 and CACNB2 might be more patentable for the investment made.
Unexplored therapeutic opportunities within the schizophrenia genome
To prioritize genes associated with schizophrenia in terms of their potential druggability beyond immediate drug repurposing opportunities, we annotated all genome-wide significant schizophrenia risk genes (n = 573 unique), from GWAS26,27 (n = 414), TWAS33 (n = 152), and CNV28 (n = 112) reference studies (Fig. 4a), with target development categories from a recent comprehensive summary of unexplored therapeutic opportunities in the human genome curated by the IDG initiative (Fig. 1; Methods; and Supplementary Data 1)41. The IDG initiative categorizes protein-coding genes as four target types: T clinical (Tclin)—targets linked to approved drug mechanisms of action (3%), T chemical (Tchem)—targets which bind small molecules with high potency (6%), T biology (Tbio)—targets with evidence of bioactivity (53%), and T dark genome (Tdark)—unexplored targets (38%)41. Schizophrenia risk genes revealed an enrichment of potentially druggable targets associated with either preliminary chemical (Tchem 8%) or biological (Tbio 63%) evidence, in addition to the targets associated with approved drugs (Tclin and Tclin_RP 5%; described earlier) (Fig. 4b). This suggests that there is a host of potentially innovative drug targets for schizophrenia beyond those which currently match known drugs and is consistent with the concept that human disease mutations are more prevalent in core functional genes73.
a Shows overlap between genome-wide significant schizophrenia risk genes (n = 573 unique), from GWAS26,27 (n = 414, orange), TWAS33 (n = 152, purple), and CNV28 (n = 112, green) reference studies. Genes shared between sources of schizophrenia-associated genetic variation data (n = 6) are labeled. Genes are labeled using standardized nomenclature (HUGO Gene Nomenclature Committee). b Schematic representation of the distribution of genome-wide significant schizophrenia risk genes across target development levels in terms of the number of genes and the % of total schizophrenia risk genes. Target development levels reflect the degree to which a gene target is characterized for therapeutic purposes in human disease indications and include T clinical (Tclin; green)—targets linked to approved drug mechanisms of action, T chemical (Tchem; yellow)—targets which bind small molecules with high potency, T biology (Tbio; red)—targets with evidence of bioactivity and T dark genome (Tdark; purple)—unexplored targets41. T clinical repurposing (Tclin_RP; blue) reflects a subset of Tclin targets which additionally map to drugs which have been tested in clinical repurposing trials for schizophrenia23. Total druggable genes in the human genome, corresponding to human molecular targets of approved drugs across disease indications (Tdruggable; gray; n = 667)37, and the total number of genes in the human genome (Ttotal; white; n = 20,120)41 are shown as background for comparison.
Comparison of the sources of genetic evidence suggested that the majority of target space continues to be driven by common (GWAS) risk variants reflecting the larger statistical power and sample numbers in these studies. Overlap is greatest between GWAS and TWAS results (n = 89 genes) as GWAS risk loci are used to index TWAS SNP associations and the studies use overlapping sample sets. The data clearly highlights six genes (PPP4C, DOC2A, INO80E, MAPK3, TAOK2, and YPEL3) common to all datasets, as follow-up candidates. Interestingly, none of these genes mapped to approved drug targets, suggesting vital opportunities for clinical development. Tchem targets MAPK3 and TAOK2 are both serine/threonine-protein kinases which interact with the MAPK signaling cascade and are involved in the stability of the postsynaptic density (PSD), strongly implicated in schizophrenia25,30,74,75. MAPK3 is further reported to be a regulatory trigger for the functional cassette involving KCTD13 and MVP which regulates brain development and neuronal proliferation phenotypes33. Tbio genes PPP4C and YPEL3 are involved in the regulation of histone acetylation76 and cellular senescence77, while Tdark genes DOC2A and INO80E are involved in spontaneous calcium-dependent neurotransmitter release78 and chromatin remodeling79, respectively. In addition to elucidating the role of these six genes in schizophrenia, the absence of highly specific ligands targeting these genes suggests that a greater toolbox of ligands to explore their therapeutic target validity in live cellular systems is required. In this respect, the ChEMBL activity annotations and knockout model organisms33 available for MAPK3 and TAOK2 are an amenable starting point for translational follow-up. Interestingly, while TWAS associations for most of these genes were linked to altered gene expression in the brain (PPP4C, DOC2A, MAPK3, and TAOK2), some risk alleles were associated with altered expression in the blood (PPP4C and INO80E) or adipose tissue (PPP4C and YPLE3). This highlights the fact that some schizophrenia risk genes show systemic expression alterations and raises questions about the genetic predisposition to side-effects of antipsychotic medication such as neutropenia and weight gain.
Further dissection of genome-wide significant schizophrenia risk genes to reveal untapped potentially translatable drug targets showed a total of 60 genes with chemical-target interaction data in the ChEMBL database (Fig. 5a), 266 genes with associated mouse neurophenotypes (Fig. 5b), and 29 genes with synaptic pathway annotations (Fig. 5c and Supplementary Fig. 1). While, targets of clinical drugs (Tclin), including those which are already in clinical repurposing trials for schizophrenia (Tclin_RP), were well represented as a benchmark across these parameters, there were notable genes in the Tchem and Tbio categories which were significantly associated to the disease and had similar or even greater levels of annotation than the Tclin/Tclin_RP targets, representing a second and third tier of potentially translatable targets respectively. These included Tchem genes (e.g., MCHR1, MAPT, EPHX2, NOS1, CHRFAM7A, NEK1, MGLL, PRKD1, and AKT3) with a wealth of ChEMBL chemical-target interaction data (including 14 genes with target-specific chemical ligands- Supplementary Data 1 ChEMBL selective compounds) and Tchem (e.g., PTPRF, GRM3, GRM8, and AKT3) and Tbio (e.g., PLCB2, CHRNA5, DLG1, SLC32A1, RIMS1, and RRAS) genes which had both mouse neurophenotype and synaptic pathway associations. Interestingly, while Tchem genes were abundant at the highest level of mouse neurophenotype association, Tbio genes (e.g., PLCB2, CHRNA5, and DLG1) dominated the synaptic pathway associations, indicating a paucity of ligands for synaptic proteins aside from neurotransmitter receptors.
Figure shows all genome-wide significant schizophrenia risk genes (n = 573 unique), from GWAS26,27 (n = 414, square), TWAS33 (n = 152, triangle), and CNV28 (n = 112, circle) reference studies. For each gene negatively transformed P values (−log P values) for genome-wide association to schizophrenia from the respective studies are cross-referenced with extended molecular drug target annotations41 to highlight therapeutic opportunities in terms of a “druggability” defined by abundance of chemical-target interaction data in the ChEMBL database, b CNS relevance defined by number of neurophenotypes resulting from orthologous gene mutations in mice (Mouse Genome Informatics database; NA—no phenotype data available, 0—non-neurophenotypes, 1—either MP:0003631 “nervous system phenotype” or MP:0005386 “behavior/neurological phenotype”, 2—both MP:0003631 “nervous system phenotype” and MP:0005386 “behavior/neurological phenotype”), c CNS relevance defined by number of synaptic pathway annotations (Pathway Commons, KEGG, Reactome databases), and d novelty in terms of the Harmonizome data availability score which integrates the cumulative probability of each gene (or protein product) occurring across 70 major publically available online resources and is an indicator of experimental information density90. P values from different TWAS expression reference panels are represented as discrete points. Target development levels reflect the degree to which a gene target is characterized for therapeutic purposes in human disease indications and include T clinical (Tclin; green)—targets linked to approved drug mechanisms of action, T chemical (Tchem; yellow)—targets which bind small molecules with high potency, T biology (Tbio; red)—targets with evidence of bioactivity and T dark genome (Tdark; purple)—unexplored targets41. T clinical repurposing (Tclin_RP; blue) reflects a subset of Tclin targets which additionally map to drugs which have been tested in clinical repurposing trials for schizophrenia23. Genes are labeled using standardized nomenclature (HUGO Gene Nomenclature Committee). For representation only genes with ChEMBL activity >10 (a), at least one synaptic pathway annotation (b, c), or Harmonizome score <10 (d) are labeled.
Risk genes with high ChEMBL activity annotations represent more immediately translatable targets in the sense that they have a wealth of chemical ligand-binding and activity information which can be used to guide target development. For example, the risk gene MCHR1, which has not been targeted in schizophrenia, has a ChEMBL activity count comparable to that of the established schizophrenia target DRD2, including 4029 compounds and 5897 bioactivity registries. Moreover, MCHR1 signaling has been shown to modulate dopamine-related responses in mesocorticolimbic, but not nigrostriatal, dopaminergic pathways in animal models of schizophrenia80, suggesting that it may be a novel therapeutic target which avoids the extrapyramidal toxicity inherent to subclasses of antipsychotic drugs.
Risk genes with both synaptic pathway and neurophenotype annotations are more likely to be involved in pathophysiological mechanisms in the CNS and are practical in terms of the availability of animal models for behavioral testing and target validation. Among these, Tchem genes such as GRM3 and GRM8 are consistent with preliminary evidence of preclinical and clinical effects of metabotropic GluR modulation on symptoms of schizophrenia81, while genes such as AKT3 are supported by altered expression of Akt isoforms in the brain and immune cells of schizophrenia patients82. Another Tchem candidate, receptor-type tyrosine-protein phosphatase F (PTPRF), is interesting in terms of its association with insulin resistance83, a feature which has recently been shown to correlate with the polygenic risk of schizophrenia and diminished treatment response in subgroups of first-episode patients84. Conversely, Tbio targets PLCB2, PLCH2, PLCL1, and PLCL2 are notable in that related PLC isotypes have been linked to altered expression in the brain of schizophrenia patients postmortem85, schizophrenia-like behavioral abnormalities in knockout animal models85,86 and altered calcium flux responses in peripheral blood cells of drug-naïve schizophrenia patients52. Moreover, DLG1 and NRXN1 are hub proteins in synaptic and ARC-complex networks strongly associated with schizophrenia87, while RIMS1 and SLC32A1 are involved in synaptic vesicle exocytosis88 and vesicular GABA reuptake, respectively89. Taken together these findings suggest that the cross-examination of Tchem and Tbio targets with metadata such as ChEMBL activity scores or synapse and neurophenotype annotations can highlight translatable gene targets which might be mechanistically plausible and practical despite lower levels of clinical development in the context of schizophrenia.
To assess how the targets were distributed in terms of novelty we mapped the risk genes against an independent composite score (Harmonizome data availability (HDA) score) which integrates the cumulative probability of each protein occurring across 70 publically available online resources and is an indicator of the experimental information density associated with the protein (Fig. 5d)90. These resources include experimental data such as biomolecular interactions, expression in cell lines and tissues, genetic associations with the knockout mouse or human phenotypes, and changes in expression after drug treatment derived from large “-omics” repositories and publications. As expected, HDA scores were greatest for Tclin and Tclin_RP genes followed by Tchem, Tbio, and Tdark genes respectively, reflecting a gradient of novelty which is inversely related to the HDA score. Interestingly, schizophrenia risk genes were distributed in a bimodal manner across this target space. Well-documented risk genes such as CACNA1 and GRIN2A led the first wave with high HDA scores followed by a range of Tchem and Tbio targets.
However, towards the other end of the scale, the results revealed a subgroup of genes (n = 27; Supplementary Fig. 1), comprised primarily of Tdark annotations, which had low HDA scores and about which relatively little is known. Notably, several of these genes (e.g., ZSCAN23, ZSCAN31, ZKSCAN3, and BORCS7) were more significantly associated with schizophrenia than those under clinical development suggesting that they might represent drug targets which require further functional characterization. Recent data suggest that lysosomal trafficking protein BORCS7, in conjunction with Tbio target AS3MT, might alter early neuronal differentiation in subgroups of schizophrenia patients91. Conversely, DNA-binding zinc-finger proteins ZSCAN23 and ZSCAN31 are representative of a larger group of significantly associated transcription factors (n = 37) which are scarcely characterized in the context of schizophrenia. Although transcription factors have previously been less druggable than other protein families41, recent zebrafish phenotypic screens have underlined the importance of specific Tdark transcription factors (e.g., ZNF536) in functional phenotypes relevant to schizophrenia, such as the development of forebrain neurons implicated in social behavior and stress92. Moreover, the present data suggest up to 15 underexplored schizophrenia-associated transcription factors with orthologous mouse neurophenotypes (Supplementary Data 1). This suggests that systematic efforts to characterize and target lesser-known transcription factors or their druggable downstream targets are warranted.
Closer examination of schizophrenia-linked Tdark proteins as a whole revealed nine genes with associated mouse neurophenotypes of which three (DOC2A, INO80E, and HIRIP3) were supported by more than one analysis method (GWAS, TWAS, and CNV; Supplementary Fig. 2a) and relatively specific for neurophenotypes compared to other mouse phenotypes (Supplementary Fig. 2b). Underexplored genes such as DOC2A and INO80E, involved in spontaneous calcium-dependent neurotransmitter release and chromatin remodeling respectively, are clear candidates for follow-up. Likewise, genes, such as C22orf39, specific for neurophenotypes and about which scarcely anything is known to indicate a potentially relevant knowledge gap.
Translational challenges and perspective
The gene-target associations discussed represent an initial shortlist of known susceptibility genes across the existing target annotation space, with an emphasis on identifying potential low-hanging fruits. However, the translation of genetic variants into drug discovery opportunities poses several challenges with relevance to future work.
First, the translational of gene-target associations into clinical compounds depends on whether the gene has a disease-modifying effect, whether the compound implicated evokes a change in the activity of the target in the desired direction and, vitally, the pharmacokinetics and safety of any resulting drug candidate in humans. While these steps fall beyond the scope of the current review, which focuses on target hypothesis generation, they form a crucial framework for follow-up studies.
Second, the majority of genetic risk loci for schizophrenia are yet to be defined. Polygenic risk profile scores based on GWAS risk loci, currently account for 3–8% of disease liability for schizophrenia and individual risk loci often have relatively small effect sizes26,27. While theoretical projections suggest that RPS might be able to explain up to 25–33% of disease liability, this remains considerably less than the 65–80% heritability observed in family and monozygotic twin studies3,93. Moreover, it is becoming apparent that large increases in sample size are required to achieve modest increases in the number of common risk loci identified94, with many of these likely to be of low odds ratio or low frequency within the population. Although susceptibility loci with modest odds ratios, for example, DRD2 (odds ratio 1.08) which is targeted by current antipsychotics, can represent valid drug targets it is likely that many of the risk alleles already identified will continue to represent the most robust genetic risk factors.
Moreover, it is difficult to isolate the causative genomic variants and genes within putative susceptibility loci. Several of the implicated loci are too broad to distinguish genes which are genuine drug target candidates from genes which are simply in linkage disequilibrium with the true causative variants. For example, the extended major histocompatibility complex (MHC) which is the most significant PGC-SCZ GWAS locus, encompassing hundreds of genes, is excluded from most GWAS drug target analyses due to inconclusive identification of causative variants, with the exception of genes coding for C4A95. The exclusion of a large number of immune-related genes in this region may contribute to the lack of genetic evidence for immune-targeted repurposing candidates. Conversely, it is currently unknown whether many of the genes included in this study are causative and corrections for gene size, effect size, and multiple testing are restricted to the studies of origin. In this respect, the current study represents a parallel framework for evaluating whether a gene is druggable and consequently a relevant lead to follow-up in terms of fine mapping. High-resolution mapping, using deep-coverage and long-read whole-genome sequencing, may improve identification of causative genomic variants, especially rare variants within non-coding regions, and help to answer more complex questions such as structural variation, variants in repetitive DNA, and phasing96.
Third, the most poignant challenge is understanding the functional implications of putative risk genes and how they interact to elicit the altered cellular and organismal phenotypes associated with the disease. The majority of risk SNPs reside in intergenic regions, introns, or correspond to synonymous mutations. Therefore it is hard to ascertain how a given risk polymorphism affects gene expression or protein function and whether an agonist or antagonist is required to target the disease phenotype. While TWAS and brain RNA-seq studies have shed light on this, expression profiles can vary depending on the reference tissue type used50,51. Conversely, expression quantitative trait loci (eQTL) catalogs require greater curation to accurately ascertain tissue specificity for a given genomic variant97. Projects such as PsychENCODE98 and Genotype-Tissue Expression (GTEx)99 aim to address this by exploring the pathophysiological relationship between non-coding regulatory elements and gene expression patterns in different brain regions from patients and controls. Moreover, the most relevant drug targets for schizophrenia might not be directly implicated risk loci (each of which likely has a relatively small or nonspecific impact on the phenotype), but instead hub proteins with disease-modifying effects on multiple risk genes within a cellular network. Although protein–protein interaction maps of schizophrenia susceptibility loci have begun to address this there remain challenges in terms of reconstruction and prioritization of hub proteins, as seen from the high number of FDA-approved candidate compounds implicated by some studies100.
Fourth, in terms of drug repurposing, the matching of risk genes to known drug targets is only as complete as the drug target annotation on which it is based. The Santos et al. molecular drug target list37 used to annotate schizophrenia risk genes, is based largely on the mechanism of action annotations from FDA-approved drug labels and primary literature. It is therefore robust in identifying low-hanging fruit for repurposing found at the intersection between well-characterized clinical targets and genetic risk loci. However, in many ways, the list is conservative in terms of defining the full repurposing opportunities related to genetic variation in schizophrenia. For example, analyses using the Drug–Gene Interaction Database (DGIdb)40 and the Psychoactive Drug Screening Database (Ki DB)101, which look more broadly at drug–gene interactions beyond FDA mechanisms of action, suggest further interactions with potassium channels (KCNN3 and KCNJ13), cytochrome P450 enzymes (CYP26B1 and CYP21A2), and ACh receptor subunits (CHRNA5), in addition to other novel targets. However, the therapeutic and pharmacokinetic implications of many of these interactions are less well documented and in some cases may represent adverse reactions. In either case, the matching of risk genes to approved drug targets represents a heuristic means of shortlisting repurposing drug candidates, which subsequently require closer examination in terms of the direction of pharmacological effect, dosing, contraindications, and therapeutic intent. In this respect, there is also an urgent need to develop a standardized ontology of drug activity for computational mining102 and to account for direct or indirect targets which are not associated with FDA-approved mechanisms of action. Although FDA-approved drug targets annotations have increased drastically in recent years37,38, this still reflects a small portion (3%) of the human proteome and falls considerably short of the 15–35% of genes which are theoretically druggable39,40. It is therefore vital to track the development level of protein targets beyond approved drug matches to identify both imminent potential repurposing opportunities, such as Tchem proteins which are targeted in clinical trials for novel drugs.
Finally, although the study of lesser-known genes, such as the Tdark proteins associated with schizophrenia, continues to face challenges, such as confirmation bias and risk aversion, several initiatives are underway to address this knowledge deficit. These include the Monarch Initiative103, which integrates clinical data with model organisms to identify phenotypically relevant cross-species disease models, or the International Mouse Phenotyping Consortium (IMPC)73, which aims to phenotype knockout mouse lines for up to 20,000 human orthologue genes. Recent data from the IMPC shows that approximately one-third of single-gene knockout models so far have at least one significant neurophenotype observation, many of which overlap with Online Mendelian Inheritance in Man (OMIM)104, GWAS Catalog105, and DISEASES106 databases. Functional phenotypic screening in schizophrenia patient-derived cellular models107, such as primary peripheral blood cells ex vivo52,72 or iPSC-derived neurons108, or risk-gene knockout model organisms92 have also been used to functionally characterize lesser-known genes. Importantly these approaches support the screening of novel compound or drug repurposing libraries, such as the Repurposing Hub109 or National Centre for Advancing Translational Sciences (NCATS)110 libraries, so that gene sets which are strongly associated with the disease yet have a paucity of ligand-binding information, such as PSD proteins or subsets of transcription factors, might be targeted. These efforts are further supported by improvements in the diversity of molecular probes as represented by the NIH Molecular Libraries Initiative111 or signature matching between drug and disease transcriptome profiles112.
The boundaries of the druggable genome are constantly evolving in terms of the number of target proteins and the depth of target annotation, suggesting that many more therapeutic targets are possible across the human disease space. Integration of genetic data with systematic evidence-based protein target annotation is a powerful tool for prioritizing hypotheses of drug targets in schizophrenia, ranging from new potential repurposing opportunities such as those represented by members of the voltage-gated potassium channel or cytochrome P450 families to relatively unexplored genes with orthologous neurological and behavioral phenotypes, such as INO80E and DOC2A, found at the intersection between common, rare and expression genetic risk variants. This approach provides a valuable means to evaluate the results of previous clinical trials in addition to providing a framework for addressing genetic heterogeneity in future drug discovery efforts. Together with new experimental techniques which address the daunting, yet essential, the task of illuminating lesser studied proteins in the human genome, this approach serves to drive the identification of mechanistically diverse potential drug candidates and support much-needed personalized therapeutic improvements in treatment-resistant patient populations or symptom domains of schizophrenia.
Methods
Comparison of targets from genetic association studies and the clinical repurposing pipeline
Schizophrenia risk genes which matched HUGO Gene Nomenclature Committee (HGNC) references (n = 1019) were compiled from the largest and most recent reference analyses exploring sources of common (n = 435)26,27,42,44, rare (n = 246)25,28,43, and gene expression (n = 338)33,45,46, genetic variation associated with schizophrenia (Supplementary Data 1 and Fig. 1a). Gene IDs and corresponding metadata (e.g., reference SNPs, analysis methods) from the source studies were matched to unique UniProt accession numbers (n = 748; Fig. 1b) to provide a list of schizophrenia-associated protein targets. UniProt accessions (protein targets) were annotated with drug target efficacy information for approved drugs (e.g., drug name, molecule type, FDA mechanism of action (MOA), ChEMBL target ID, ChEMBL protein target classification, FDA approval date, and anatomical therapeutic chemical classification (ATC) codes)37, and therapeutic disease indications109 to determine protein targets which are targeted by approved drugs and the respective therapeutic indications of these drugs (Fig. 1c). In parallel, the same drug target efficacy information37 was used to map the protein targets of drugs in the clinical repurposing pipeline for schizophrenia (described in detail below; Fig. 1d). The ChEMBL protein target classifications of repurposing targets suggested by genetic analyses and targets in the schizophrenia clinical repurposing pipeline were compared (Fig. 1e) to identify areas of overlap (i.e., targets which are, “T clinical_repurposing” (n = 29), or are not, “T clinical” (n = 27), under development in the schizophrenia repurposing pipeline. The later “T clinical” represents novel repurposing opportunities).
Annotation of schizophrenia repurposing clinical trial drugs
Drugs explored in clinical repurposing trials for schizophrenia (n = 89 including ketamine, ClinicalTrials.gov)23 were annotated with drug target efficacy information for approved drugs (e.g., molecule type, mechanism of action, UniProt accession, ChEMBL target ID, ChEMBL protein target classification, FDA approval date, and anatomical therapeutic chemical classification code)37 and therapeutic disease indications109 (Fig. 1d). Drugs (n = 7) listed as having primary microbial targets were cross-referenced with the mechanism of action annotations in Drug Bank and corresponding human Uniprot accessions and ChEMBL IDs were added to the drug profile where relevant (minocycline, pyrimethamine, amantadine, and ceftriaxone). Anti-microbial drugs without human annotations in Santos et al.37 or Drug Bank (artemisinin, cysteine, and cycloserine) were excluded. Uniprot accessions were used to assess overlap between targets for drugs in schizophrenia clinical repurposing trials and schizophrenia risk genes. For drugs with multiple target annotations (n = 20), up to two protein target classification entries were selected for each drug, based on matching to schizophrenia risk genes (if applicable), primary therapeutic relevance (Drug Bank mechanism of action), and mechanistic diversity across the drug set. Drugs with multiple subunit annotations within the same target protein complex were consolidated to reflect a single protein target classification.
Prioritization of repurposing opportunities and unexplored therapeutic opportunities within the schizophrenia genome
A subset of studies, reporting genome-wide significant P values26,27,28,33(Fig. 1a*), were used for prioritization of repurposing opportunities in schizophrenia and exploring therapeutic opportunities within the schizophrenia genome. These comprised 769 schizophrenia-associated genes, derived from common (GWAS; n = 416), rare (CNV; n = 112), and gene expression (TWAS; n = 241) genetic variation studies (Supplementary Data 1), which matched to 573 unique UniProt accession numbers (Fig. 1f). UniProt accessions were annotated with protein target development levels (TDLs) from genomic, proteomic, chemical, and disease-related human genome data repositories curated by the Illuminating the Druggable Genome (IDG) Knowledge Management Center41 (Fig. 1g). These included: “T clinical”—targets linked to approved drug mechanisms of action, “T chemical”—targets which bind small molecules with high potency, “T biology”—targets with evidence of bioactivity, and “T dark genome”—unexplored targets. An additional category was created for proteins targeted in clinical repurposing trials for schizophrenia, “T clinical_repurposing”. TDLs for targets previously matched to FDA mechanisms of action in the repurposing analysis (described above) were labeled accordingly as “T clinical_repurposing” and “T clinical” (Fig. 1g+). Uniprot accessions for each target were also annotated with extended metadata curated by the IDG Knowledge Management Center (e.g., HUGO Gene Nomenclature gene name, protein family, publication metrics, antibody count, HarmonizomeDAS score, Gene Ontology count, OMIM phenotypes, grant funding, pathway count, disease count, murine orthologue phenotype count, ChEMBL activity count, and PANTHER classification)41. Neurophenotypes resulting from orthologous gene mutations in mice were defined using IDG data based on the Mouse Genome Informatics database using search terms MP:0003631 “nervous system phenotype” and MP:0005386 “behavior/neurological phenotype”. The distribution of genome-wide significant schizophrenia targets was then examined across the TDL space and cross-referenced with the IDG extended metadata to prioritize both potential repurposing targets and unexplored therapeutic opportunities (Fig. 1h). For cross-referencing, genome-wide significance P values for schizophrenia-associated genes are reported as in the study of origin. Therefore P values are only comparable within targets from the same analysis type (i.e., common, rare, and expression variation).
Reporting Summary
Further information on research design is available in the Nature Research Reporting Summary linked to this article.
Data availability
All data generated or analysed during this study, including aggregate data, are included in this published article (and its supplementary information files). Source data is available as UniProt accession codes (www.uniprot.org) with references in Supplementary Data 1 and descriptions in the Methods.
Code availability
Code is available from the corresponding author on reasonable request.
References
Malan-Müller, S. et al. A systematic review of genetic variants associated with metabolic syndrome in patients with schizophrenia. Schizophr. Res. 170, 1–17 (2016).
Mitchell, A. J. et al. Prevalence of metabolic syndrome and metabolic abnormalities in schizophrenia and related disorders-A systematic review and meta-analysis. Schizophr. Bull. 39, 1–13 (2011).
Kahn, R. S. et al. Schizophrenia. Nat. Rev. Dis. Prim. 1, 15067 (2015).
Vos, T. et al. Years lived with disability (YLDs) for 1160 sequelae of 289 diseases and injuries 1990-2010: a systematic analysis for the Global Burden of Disease Study 2010. Lancet 380, 2163–2196 (2012).
Rössler, W., Joachim Salize, H., Van Os, J. & Riecher-Rössler, A. Size of burden of schizophrenia and psychotic disorders. Eur. Neuropsychopharmacol. 15, 399–409 (2005).
Owen, M. J., Sawa, A. & Mortensen, P. B. Schizophrenia. Lancet 388, 86–97 (2016).
Pangalos, M. N., Schechter, L. E. & Hurko, O. Drug development for CNS disorders: strategies for balancing risk and reducing attrition. Nat. Rev. Drug Discov. 6, 521–532 (2007).
Schennach, R., Riedel, M., Musil, R. & Möller, H.-J. Treatment response in first-episode schizophrenia. Clin. Psychopharmacol. Neurosci. 10, 78–87 (2012).
Berton, O. & Nestler, E. J. New approaches to antidepressant drug discovery: beyond monoamines. Nat. Rev. Neurosci. 7, 137–151 (2006).
Wong, M.-L. & Licinio, J. From monoamines to genomic targets: a paradigm shift for drug discovery in depression. Nat. Rev. Drug Discov. 3, 136–151 (2004).
Schwarz, E., Guest, P. C., Steiner, J., Bogerts, B. & Bahn, S. Identification of blood-based molecular signatures for prediction of response and relapse in schizophrenia patients. Transl. Psychiatry 2, e82 (2012).
Tomasik, J. et al. Pretreatment levels of the fatty acid handling proteins H-FABP and CD36 predict response to olanzapine in recent-onset schizophrenia patients. Brain. Behav. Immun. 52, 178–186 (2016).
Conn, P. J. & Roth, B. L. Opportunities and challenges of psychiatric drug discovery: roles for scientists in academic, industry, and government settings. Neuropsychopharmacology 33, 2048–2060 (2008).
Agid, Y. et al. How can drug discovery for psychiatric disorders be improved? Nat. Rev. Drug Discov. 6, 189–201 (2007).
Scannell, J. W., Blanckley, A., Boldon, H. & Warrington, B. Diagnosing the decline in pharmaceutical R&D efficiency. Nat. Rev. Drug Discov. 11, 191–200 (2012).
Pankevich, D. E., Altevogt, B. M., Dunlop, J., Gage, F. H. & Hyman, S. E. Improving and accelerating drug development for nervous system disorders. Neuron 84, 546–553 (2014).
Langedijk, J., Mantel-Teeuwisse, A. K., Slijkerman, D. S. & Schutjens, M. H. D. B. Drug repositioning and repurposing: terminology and definitions in literature. Drug Discov. Today 20, 1027–1034 (2015).
O’Connor, K. A. & Roth, B. L. Finding new tricks for old drugs: an efficient route for public-sector drug discovery. Nat. Rev. Drug Discov. 4, 1005–1014 (2005).
Gleeson, M. P., Hersey, A., Montanari, D. & Overington, J. Probing the links between in vitro potency, ADMET and physicochemical parameters. Nat. Rev. Drug Discov. 10, 197–208 (2011).
Carpenter, W. T. & Davis, J. M. Another view of the history of antipsychotic drug discovery and development. Mol. Psychiatry 17, 1168–1173 (2012).
Schooler, N. R. et al. Defining therapeutic benefit for people with schizophrenia: focus on negative symptoms. Schizophr. Res. 162, 169–174 (2015).
Millan, M. J. et al. Cognitive dysfunction in psychiatric disorders: characteristics, causes and the quest for improved therapy. Nat. Rev. Drug Discov. 11, 141–168 (2012).
Lago, S. & Bahn, S. Clinical trials and therapeutic rationale for drug repurposing in schizophrenia. ACS Chem. Neurosci. 10, 58–78 (2018).
Purcell, S. M. et al. A polygenic burden of rare disruptive mutations in schizophrenia. Nature 506, 185–190 (2014).
Fromer, M. et al. De novo mutations in schizophrenia implicate synaptic networks. Nature 506, 179–184 (2014).
Ripke, S. et al. Biological insights from 108 schizophrenia-associated genetic loci. Nature 511, 421–427 (2014).
Li, Z. et al. Genome-wide association analysis identifies 30 new susceptibility loci for schizophrenia. Nat. Genet. 49, 1576–1583 (2017).
Marshall, C. R. et al. Contribution of copy number variants to schizophrenia from a genome-wide study of 41,321 subjects. Nat. Genet. 49, 27–35 (2017).
Fromer, M. et al. De novo mutations in schizophrenia implicate synaptic networks. Nature 506, 179–184 (2014).
Purcell, S. M. et al. A polygenic burden of rare disruptive mutations in schizophrenia. Nature 506, 185–190 (2014).
Denny, J. C. et al. Systematic comparison of phenome-wide association study of electronic medical record data and genome-wide association study data. Nat. Biotechnol. 31, 1102–1111 (2013).
Rastegar-Mojarad, M., Ye, Z., Kolesar, J. M., Hebbring, S. J. & Lin, S. M. Opportunities for drug repositioning from phenome-wide association studies. Nat. Biotechnol. 33, 342–345 (2015).
Gusev, A. et al. Transcriptome-wide association study of schizophrenia and chromatin activity yields mechanistic disease insights. Nat. Genet. 50, 538–548 (2018).
Sanseau, P. et al. Use of genome-wide association studies for drug repositioning. Nat. Biotechnol. 30, 317–320 (2012).
Lencz, T. & Malhotra, A. K. Targeting the schizophrenia genome: a fast track strategy from GWAS to clinic. Mol. Psychiatry 20, 820–826 (2015).
Rask-Andersen, M., Masuram, S. & Schiöth, H. B. The druggable genome: evaluation of drug targets in clinical trials suggests major shifts in molecular class and indication. Annu. Rev. Pharmacol. Toxicol. 54, 9–26 (2014).
Santos, R. et al. A comprehensive map of molecular drug targets. Nat. Rev. Drug Discov. 16, 19–34 (2016).
Harris et al. How many drug targets are there? Nat. Rev. Drug Discov. 5, 993–996 (2006).
Hopkins, A. L. & Groom, C. R. The druggable genome. Nat. Rev. Drug Discov. 1, 727–730 (2002).
Griffith, M. et al. DGIdb: Mining the druggable genome. Nat. Methods 10, 1209–1210 (2013).
Oprea, T. I. et al. Unexplored therapeutic opportunities in the human genome. Nat. Rev. Drug Discov. 17, 317–332 (2018).
Sekar, A. et al. Schizophrenia risk from complex variation of complement component 4. Nature 530, 177–183 (2016).
Purcell, S. M. et al. A polygenic burden of rare disruptive mutations in schizophrenia. Nature 506, 185–190 (2014).
Moosavinasab, S. et al. ‘RE:fine drugs’: an interactive dashboard to access drug repurposing opportunities. Database 2016, 1–5 (2016).
Jaffe, A. E. et al. Developmental and genetic regulation of the human cortex transcriptome illuminate schizophrenia pathogenesis. Nat. Neurosci. 21, 1117–1125 (2018).
Fromer, M. et al. Gene expression elucidates functional impact of polygenic risk for schizophrenia. Nat. Neurosci. 19, 1442–1453 (2016).
Fromer, M. et al. De novo mutations in schizophrenia implicate synaptic networks. Nature 506, 179–184 (2014).
Berridge, M. J. Calcium signalling and psychiatric disease: bipolar disorder and schizophrenia. Cell Tissue Res. 357, 477–492 (2014).
Zamponi, G. W. Targeting voltage-gated calcium channels in neurological and psychiatric diseases. Nat. Publ. Gr. 15, 19–34 (2015).
Heyes, S. et al. Genetic disruption of voltage-gated calcium channels in psychiatric and neurological disorders. Prog. Neurobiol. 134, 36–54 (2015).
Bhat, S. et al. CACNA1C (Cav1.2) in the pathophysiology of psychiatric disease. Prog. Neurobiol. 99, 1–14 (2012).
Lago, S. G. et al. Drug discovery in neuropsychiatric disorders using high-content single-cell screening of signaling network responses ex vivo. Sci. Adv. 5, eaau9093 (2019).
Prabakaran, S. et al. Mitochondrial dysfunction in schizophrenia: evidence for compromised brain metabolism and oxidative stress. Mol. Psychiatry 9, 684–697 (2004). 643.
Akarsu, S. et al. Mitochondrial complex I and III gene mRNA levels in schizophrenia, and their relationship with clinical features. J. Mol. Psychiatry 2, 6 (2014).
Choi, Y.-J. Efficacy of adjunctive treatments added to olanzapine or clozapine for weight control in patients with schizophrenia: a systematic review and meta-analysis. ScientificWorldJournal 2015, 970730 (2015).
Manji, H. et al. Impaired mitochondrial function in psychiatric disorders. Nat. Rev. Neurosci. 13, 293–307 (2012).
Ohi, K. et al. Specific gene expression patterns of 108 schizophrenia-associated loci in cortex. Schizophr. Res. 174, 35–38 (2016).
Peltola, M. A. et al. AMIGO-Kv2.1 potassium channel complex is associated with schizophrenia-related phenotypes. Schizophr. Bull. 42, sbv105 (2015).
Tsay, D., Dudman, J. T. & Siegelbaum, S. A. HCN1 channels constrain synaptically evoked Ca2+ spikes in distal dendrites of CA1 pyramidal neurons. Neuron 56, 1076–1089 (2007).
Arnsten, A. F. T. Prefrontal cortical network connections: key site of vulnerability in stress and schizophrenia. Int. J. Dev. Neurosci. 29, 215–223 (2011).
Waxman, S. G. & Zamponi, G. W. Regulating excitability of peripheral afferents: emerging ion channel targets. Nat. Neurosci. 17, 153–163 (2014).
Heringa, S. M., Begemann, M. J. H., Goverde, A. J. & Sommer, I. E. C. Sex hormones and oxytocin augmentation strategies in schizophrenia: a quantitative review. Schizophr. Res. 168, 603–613 (2015).
de Boer, J., Prikken, M., Lei, W. U., Begemann, M. & Sommer, I. The effect of raloxifene augmentation in men and women with a schizophrenia spectrum disorder: a systematic review and meta-analysis. npj Schizophr. 4, 1 (2018).
Chiappelli, J. et al. Disrupted glucocorticoid-Immune interactions during stress response in schizophrenia. Psychoneuroendocrinology 63, 86–93 (2016).
Haduch, A. & Daniel, W. A. The engagement of brain cytochrome P450 in the metabolism of endogenous neuroactive substrates: a possible role in mental disorders. Drug Metab. Rev. 50, 415–429 (2018).
Dean, L. Aripiprazole therapy and CYP2D6 genotype. Medical Genetics Summaries (2012).
Dean, L. Clozapine therapy and CYP2D6, CYP1A2, and CYP3A4 genotypes. Medical Genetics Summaries (2012).
Dean, L. Risperidone therapy and CYP2D6 genotype. Medical Genetics Summaries (2012).
Terwisscha van Scheltinga, A. F., Bakker, S. C., Kahn, R. S. & Kas, M. J. H. Fibroblast growth factors in neurodevelopment and psychopathology. Neuroscientist 19, 479–494 (2013).
Foster, D. J. & Conn, P. J. Allosteric modulation of GPCRs: new insights and potential utility for treatment of schizophrenia and other CNS disorders. Neuron 94, 431–446 (2017).
Steiner, J. et al. Acute schizophrenia is accompanied by reduced T cell and increased B cell immunity. Eur. Arch. Psychiatry Clin. Neurosci. 260, 509–518 (2010).
Lago, S. G. et al. Exploring the neuropsychiatric spectrum using high-content functional analysis of single-cell signaling networks. Mol. Psychiatry 25, 2355–2372 (2018).
Dickinson, M. E. et al. High-throughput discovery of novel developmental phenotypes. Nature 537, 508–514 (2016).
Föcking, M. et al. Proteomic and genomic evidence implicates the postsynaptic density in schizophrenia. Mol. Psychiatry 20, 424–432 (2015).
Yadav, S. et al. TAOK2 kinase mediates PSD95 stability and dendritic spine maturation through septin7 phosphorylation. Neuron 93, 379–393 (2017).
Zhang, X. et al. Histone deacetylase 3 (HDAC3) activity is regulated by interaction with protein serine/threonine phosphatase 4. Genes Dev. 19, 827–839 (2005).
Kelley, K. D. et al. YPEL3, a p53-regulated gene that induces cellular senescence. Cancer Res. 70, 3566–3575 (2010).
Mochida, S., Orita, S., Sakaguchi, G., Sasaki, T. & Takai, Y. Role of the Doc2 alpha-Munc13-1 interaction in the neurotransmitter release process. Proc. Natl Acad. Sci. USA 95, 11418–11422 (1998).
Poli, J., Gasser, S. M. & Papamichos-Chronakis, M. The INO80 remodeller in transcription, replication and repair. Philos. Trans. R. Soc. B Biol. Sci. 372, 20160290 (2017).
Chung, S. et al. The melanin-concentrating hormone (MCH) system modulates behaviors associated with psychiatric disorders. PLoS ONE 6, e19286 (2011).
Stansley, B. J. & Conn, P. J. The therapeutic potential of metabotropic glutamate receptor modulation for schizophrenia. Curr. Opin. Pharmacol. 38, 31–36 (2018).
Emamian, E. S., Hall, D., Birnbaum, M. J., Karayiorgou, M. & Gogos, J. a. Convergent evidence for impaired AKT1-GSK3beta signaling in schizophrenia. Nat. Genet. 36, 131–137 (2004).
Ahmad, F. & Goldstein, B. J. Functional association between the insulin receptor and the transmembrane protein-tyrosine phosphatase LAR in intact cells. J. Biol. Chem. 272, 448–457 (1997).
Tomasik, J. et al. Association of insulin resistance with schizophrenia polygenic risk score and response to antipsychotic treatment. JAMA Psychiatry 76, 864–867 (2019).
Yang, Y. R. et al. Primary phospholipase C and brain disorders. Adv. Biol. Regul. 61, 80–85 (2015).
Yang, Y. R. et al. Forebrain-speci fi c ablation of phospholipase C γ 1 causes manic-like behavior. Mol. Psychiatry 22, 1473–1482 (2017).
Cardno, A. G. et al. Heritability estimates for psychotic disorders; the Maudsly twin psychosis series. Arch. Gen. Psychiatry 56, 162–168 (1999).
Deng, L., Kaeser, P. S., Xu, W. & Südhof, T. C. RIM proteins activate vesicle priming by reversing autoinhibitory homodimerization of Munc13. Neuron 69, 317–331 (2011).
Juge, N., Muroyama, A., Hiasa, M., Omote, H. & Moriyama, Y. Vesicular inhibitory amino acid transporter is a Cl-/gamma-aminobutyrate Co-transporter. J. Biol. Chem. 284, 35073–35078 (2009).
Rouillard, A. D. et al. The harmonizome: a collection of processed datasets gathered to serve and mine knowledge about genes and proteins. Database 2016, baw100 (2016).
Li, M. et al. A human-specific AS3MT isoform and BORCS7 are molecular risk factors in the 10q24.32 schizophrenia-associated locus. Nat. Med. 22, 649–656 (2016).
Thyme, S. B. et al. Phenotypic landscape of schizophrenia-associated genes defines candidates and their shared functions. Cell 177, 478–491.e20 (2019).
Harrison, P. J. Recent genetic findings in schizophrenia and their therapeutic relevance. J. Psychopharmacol. 29, 85–96 (2015).
Hyman, S. E. The daunting polygenicity of mental illness: making a new map. Philos. Trans. R. Soc. Lond. B. Biol. Sci. 373, 1–8 (2018).
Sekar, A. et al. Schizophrenia risk from complex variation of complement component 4. Nature 530, 177–183 (2016).
Sanders, S. J. et al. Whole genome sequencing in psychiatric disorders: the WGSPD consortium whole genome sequencing for psychiatric disorders (WGSPD). Nat. Neurosci. 20, 1–17 (2017).
Hertzberg, L., Katsel, P., Roussos, P., Haroutunian, V. & Domany, E. Integration of gene expression and GWAS results supports involvement of calcium signaling in Schizophrenia. Schizophr. Res. 164, 92–99 (2015).
Akbarian, S. et al. The PsychENCODE project. Nat. Neurosci. 18, 1707–1712 (2015).
MacArthur, D. G. et al. Genetic effects on gene expression across human tissues. Nature 550, 204–213 (2017).
Ganapathiraju, M. K. et al. Schizophrenia interactome with 504 novel protein–protein interactions. npj Schizophr. 2, 16012 (2016).
Roth, B. L., Lopez, E., Beischel, S., Westkaemper, R. B. & Evans, J. M. Screening the receptorome to discover the molecular targets for plant-derived psychoactive compounds: a novel approach for CNS drug discovery. Pharmacol. Ther. 102, 99–110 (2004).
Nelson, S. J. et al. Formalizing drug indications on the road to therapeutic intent. J. Am. Med. Inform. Assoc. 24, 1169–1172 (2017).
Mungall, C. J. et al. The Monarch initiative: an integrative data and analytic platform connecting phenotypes to genotypes across species. Nucleic Acids Res. 45, D712–D722 (2017).
Amberger, J., Bocchini, C. A., Scott, A. F. & Hamosh, A. McKusick’s online Mendelian inheritance in man (OMIM(R). Nucleic Acids Res. 37, D793–D796 (2009). .
MacArthur, J. et al. The new NHGRI-EBI Catalog of published genome-wide association studies (GWAS Catalog). Nucleic Acids Res. 45, D896–D901 (2017).
Pletscher-Frankild, S., Pallejà, A., Tsafou, K., Binder, J. X. & Jensen, L. J. DISEASES: text mining and data integration of disease–gene associations. Methods 74, 83–89 (2015).
Lago, S. G., Tomasik, J. & Bahn, S. Functional patient-derived cellular models for neuropsychiatric drug discovery. Transl. Psychiatry 11, 128 (2021).
Brennand, K. et al. Modelling schizophrenia using human induced pluripotent stem cells. Nature 473, 221–225 (2011).
Corsello, S. M. et al. The drug repurposing hub: a next-generation drug library and information resource. Nat. Med. 23, 405–408 (2017).
Huang, R. et al. The NCGC pharmaceutical collection: a comprehensive resource of clinically approved drugs enabling repurposing and chemical genomics. Sci. Transl. Med. 3, 80ps16 (2011).
Austin, C. P., Brady, L. S., Insel, T. R. & Collins, F. S. NIH molecular libraries initiative. Science 306, 1138–1139 (2004).
Pushpakom, S. et al. Drug repurposing: progress, challenges and recommendations. Nat. Rev. Drug Discov. 18, 41–58 (2018).
Acknowledgements
We would like to thank Dr. Jakub Tomasik for his bioinformatics assistance with database and figure preparation and comments on the manuscript and Dr. Jason Cooper for help consolidating gene lists. We are also grateful to Prof. Tudor I. Oprea for advice on drug target annotation. This work was supported by grants to S.B. from the Stanley Medical Research Institute (SMRI).
Author information
Authors and Affiliations
Contributions
S.G.L. conducted the literature review, compiled the source data, and curated the drug target annotations. S.G.L. and S.B. prepared the manuscript.
Corresponding authors
Ethics declarations
Competing interests
S.B. is a director of Psynova Neurotech Ltd. and Psyomics Ltd. The remaining authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Lago, S.G., Bahn, S. The druggable schizophrenia genome: from repurposing opportunities to unexplored drug targets. npj Genom. Med. 7, 25 (2022). https://doi.org/10.1038/s41525-022-00290-4
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41525-022-00290-4
- Springer Nature Limited