Abstract
Vasodilation in response to low oxygen (O2) tension (hypoxic vasodilation) is an essential homeostatic response of systemic arteries that facilitates O2 supply to tissues according to demand. However, how blood vessels react to O2 deficiency is not well understood. A common belief is that arterial myocytes are O2-sensitive. Supporting this concept, it has been shown that the activity of myocyte L-type Ca2+channels, the main ion channels responsible for vascular contractility, is reversibly inhibited by hypoxia, although the underlying molecular mechanisms have remained elusive. Here, we show that genetic or pharmacological disruption of mitochondrial electron transport selectively abolishes O2 modulation of Ca2+ channels and hypoxic vasodilation. Mitochondria function as O2 sensors and effectors that signal myocyte Ca2+ channels due to constitutive Hif1α-mediated expression of specific electron transport subunit isoforms. These findings reveal the acute O2-sensing mechanisms of vascular cells and may guide new developments in vascular pharmacology.
Similar content being viewed by others
Introduction
It has been known for over a century that oxygen (O2) is a major regulator of blood flow1,2,3,4,5,6; (see7,8 for reviews and references). O2 is a potent vasoconstrictor6,9,10,11,12 and in most systemic arterial territories, particularly in skeletal muscle, coronary, and cerebral vessels, a decrease in O2 tension (hypoxia) leads to rapid vasodilation8,13,14,15,16,17. In this manner, O2 supply to tissues (e.g., the working heart) is swiftly adapted to demand. This essential vasomotor response also contributes to neurovascular coupling, a dilation of small blood vessels whereby O2 availability is increased in the most active brain regions18,19,20. Details of the cellular mechanisms governing hypoxic vasodilation (HVD) remain controversial and the underlying molecular processes are largely unknown7,8,21.
The vascular endothelium and neighboring tissues can release relaxing factors that act on smooth muscle8,22,23,24,25,26,27,28,29. In addition, hemoglobin desaturation and release of vasodilators from red blood cells has been proposed to induce increases in blood flow in hypoxic capillaries30,31. However, numerous studies have suggested that myocytes are a primary site for vascular acute O2 sensing8,21,32. HVD has been recorded in arteries cleaned of surrounding tissue, denuded of endothelium, and bathed in cell-free external solutions equilibrated with low O2 tension (PO2)33,34,35. Moreover, hypoxic relaxation is observed in arteries depolarized and precontracted with high extracellular K+14,35,36,37, indicating that PO2 directly modulates transmembrane Ca2+ influx in vascular smooth muscle (VSM)36,38. In support of this concept, hypoxia, within physiological values, has been shown to elicit fast, and highly reversible inhibition of L-type voltage-gated Ca2+channels (the main ion channel type responsible for vascular contractility) in myocytes from several systemic rodent, porcine, and human arterial models9,35,37,39,40,41. However, the molecular mechanism underpinning Ca2+ channel regulation by PO2 has been elusive42. Here, we report that a constitutively expressed hypoxia inducible factor 1α (Hif1α)-dependent mitochondrial acute O2 sensing and signaling pathway, in systemic arterial myocytes, mediates the hypoxia-induced inhibition of Ca2+ channel activity and HVD.
Results
Disruption of mitochondrial complex I in arterial myocytes abolishes acute O2 modulation of Ca2+ channel activity and hypoxic vasodilation
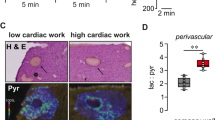
Inhibition of mitochondrial complex (MC) I activity in carotid body chemoreceptor glomus cells, the prototypical acute O2 sensors in mammals, suppresses responsiveness of these cells to hypoxia43,44,45. Hence, we investigated whether a similar phenomenon occurred in arterial myocytes. Disruption of MCI was achieved by targeting the gene encoding Ndufs2, a core subunit essential for ubiquinone (CoQ) binding and NADH dehydrogenase activity46. Cells lacking Ndufs2 show almost complete abolition of MCI function44,47. In the present study, mice (of both sexes) carrying Ndufs2 floxed and minus alleles45 were bred with mice carrying the tamoxifen (TMX)-activated Cre recombinase gene driven by the smooth muscle-specific SM22 promoter48,49. These adult mice, with conditional deficiency of MCI in VSM cells (MCI-SM mice), were studied in comparison with wild type (WT) mice. Two-month-old mice received a TMX diet for one month and were left to recover for at least one additional month on a normal diet (Fig. 1a). TMX-treated MCI-SM mice ( ≥ 4-months old) showed a strong and selective decrease in Ndufs2 mRNA obtained from the femoral artery and aorta (Fig. 1b, c). Ablation of Ndufs2 in VSM cells resulted in an ~80% decrease in MCI activity in the aorta (Fig. 1d). Except for an increase in spleen size, MCI-SM mice did not show any alteration in survival, body weight or anatomical features (Supplementary Figs. 1a–c). They had a normal hematocrit and arterial histology (Supplementary Figs. 1d–g), with normal heart rate and hypoxic ventilatory responses to hypoxia, a homeostatic reflex largely dependent on O2-sensing by carotid body glomus cells44,50, and hypercapnia (Supplementary Figs. 1h–j), However, in comparison with WT mice, MCI-SM mice showed a marked hyperlactatemia (Fig. 1e), probably as a consequence of the up-regulation of glycolysis in MCI-deficient myocytes45. They also showed a significant decrease in systolic and diastolic blood pressures (Fig. 1f), a phenomenon that could be due to the decreased vascular sensitivity to O2 tension and the blunted vasoconstrictor effect of O2 on aorta and peripheral arteries (see below). These changes indicated that even under basal physiological conditions the loss of MCI activity in VSM cells alters fundamental homeostatic mechanisms.
a MCI-SM mouse model and time course of tamoxifen (TMX) treatment. b, c Ndufs2 and Sdhd mRNA levels in femoral artery and aorta from WT mice (n = 5, blue dots) and MCI-SM mice (n = 5, orange dots). d Mitochondrial complex I (MCI) activity in aortas of WT and MCI-SM mice (n = 3). e Lactate plasma levels of WT (n = 8) and MCI-SM (n = 8) mice. f Systolic (n = 10) and diastolic (n = 11) blood pressure of WT and MCI-SM mice. g Femoral myocytes from WT (upper panel) and MCI-SM (lower panel) mice stained with antibodies against Ndufs2 (green) and alpha-smooth muscle actin (α-SMA, red). h Schematic drawing of a whole-cell patch-clamped myocyte dialyzed with 4 mM MgATP. i Reversible inhibition of Ca2+ currents recorded in acutely dispersed WT femoral myocytes upon exposure to hypoxia (O2 tension ~15 mmHg). Currents were generated by 20-ms depolarizing pulses to 10 mV. Time after switching from normoxia to hypoxia is indicated. j Time course of activation (time to reach the half maximal value; t1/2) of currents recorded at 10 mV, measured in WT femoral myocytes under normoxic (Nx, n = 13/5 cells/mice) or hypoxic (Hx, n = 11/5 cells/mice) conditions. k Time course of deactivation at −70 mV (tau of fast tail component) of currents recorded under normoxia (Nx, n = 13/5 cells/mice) or hypoxia (Hx, n = 11/5 cells/mice). l Loss of the hypoxic inhibition of Ca2+ currents in femoral myocytes from MCI-SM mice. m Effect of hypoxia expressed as percentage inhibition of the current elicited at −10, 0, 10 and 20 mV in femoral arterial myocytes from WT mice (n = 11/5 cells/mice) and MCI-SM mice (n = 15/5 cells/mice). Data are presented as mean ± SEM with statistically significant P values (<0.05) indicated in each panel. In b–f, j, k and m comparison of values was performed by two-tailed unpaired t tests. Source data are provided as a Source Data file.
Next, we studied acutely dispersed femoral myocytes, as a representative example of conduit systemic myocytes39,51, from MCI-SM mice which, despite having a selective absence of Ndufs2 immunoreactivity, appeared healthy and with the characteristic elongated shape of WT VSM cells (Fig. 1g). However, they showed an increase in mitochondrial number, similar to what we have previously seen in MCI-deficient carotid body glomus cells44, and aberrant ultrastructural changes that resemble those reported in skeletal muscle with mitochondrial myopathies52 (Supplementary Figs. 2a–i). Patch clamped MCI-deficient myocytes exhibited normal passive electrical parameters and density of voltage-gated Ca2+ and K+ channels (Fig. 1h; and Supplementary Figs. 3a–e), as well as responses to vasoactive agents (see below), indicating that as it occurs with O2-sensitive carotid body glomus cells44 arterial myocytes can survive mitochondrial dysfunction possibly due to compensatory up-regulation of glycolysis45 (see Fig. 1e). WT mouse femoral myocytes were exposed to hypoxia by switching from PO2 of 150 mmHg to ~15 mmHg in the solution bathing the cells39, covering in this manner the full range of O2 tensions existing in most tissues during normoxia and physiological hypoxia53. As observed previously in several types of systemic myocytes39,51, this treatment produced a fast, progressive, and reversible decrease in the amplitude of whole-cell L-type Ca2+ channel currents without altering their activation or deactivation kinetics (Fig. 1i–k and Supplementary Figs. 4a–d). However, in contrast to their normal histological appearance and basic electrophysiology, VSM cells from MCI-SM mice exhibited a practically abolished modulation of Ca2+ channel activity by PO2 (Fig. 1l, m). In these patch clamp experiments cells were dialyzed with intracellular MgATP to prevent activation of ATP-dependent K+ channels, despite the participation of these channels in VSM responses to physiological hypoxia is questioned21,32,35,41,54,55. Voltage-dependent K+ currents were unaffected by hypoxia (Supplementary Figs. 4e–g), suggesting that in femoral vascular myocytes voltage-gated K+ channels lack sites of interaction with the mitochondrial signals.
Femoral myocytes did not show any evidence of voltage-gated Na+ currents, despite we used a high-Na+ external solution in our patch clamp experiments. In addition, the size and time course of inward currents were unaffected by complete replacement of extracellular Na+ with the impermeant cation N-methyl-D-glucamine (Supplementary Figs. 5a, c). Modulation of the Ca2+ currents (recorded without Na+ in the internal solution) by hypoxia was also unaltered in the absence of extracellular Na+ (Supplementary Figs. 5b, c), thus making it unlikely any relevant role of Na+ control of mitochondrial signaling56 in the response to hypoxia of myocyte Ca2+ channels.
In agreement with the electrophysiological data, a strong inhibition of transmembrane Ca2+ influx triggered by either methyl 2,5-dimethyl-4-[2-(phenylmethyl)benzoyl]-1H-pyrrole-3-carboxylate (FPL), an L-type Ca2+ channel activator57,58, or depolarization with high extracellular K+15,36 was produced by hypoxia in intact Fura 2-loaded femoral myocytes. These effects of hypoxia were eliminated in MCI-SM myocytes (Fig. 2a–c and Supplementary Figs. 6a–d). Rotenone, a highly membrane-permeant MCI blocker, mimicked hypoxia and reversibly inhibited FPL-induced transmembrane Ca2+ influx, an effect that was markedly attenuated in femoral myocytes from MCI-SM mice (Fig. 2d, e). Preincubation of WT myocytes with rotenone not only produced a dose-dependent inhibition of the amplitude of FPL-induced Ca2+ signals but it occluded any further effect of hypoxia (Supplementary Figs. 7a–d). Caffeine-evoked Ca2+ release from the sarcoplasmic reticulum59 was unaltered in MCI-deficient myocytes (Supplementary Figs. 8a, b) and unaffected by rotenone (Supplementary Figs. 8c, d). Similar to hypoxia, blockers of the MCI (rotenone or piericidin A), MCIII (antimycin A) and MCIV (cyanide) decreased the amplitude of the Ca2+ currents and prevented any further effect of hypoxia (Fig. 2f left, g; and Supplementary Fig. 9a–f). Inhibition of the current with rotenone also occluded any further effect of cyanide (Fig. 2f, right, g).
a Changes in the FPL-evoked increase in cytosolic [Ca2+] elicited by hypoxia (O2 tension ~15 mmHg) in Fura-2-loaded femoral myocytes from WT and MCI-SM mice. b Box plot showing the increase in cytosolic [Ca2+] elicited by 1 μM FPL in dispersed cells from WT mice (n = 31/4 cells/mice, blue dots) and MCI-SM mice (n = 38/4 cells/mice, orange dots). c Effect of hypoxia on the FPL-evoked increase of cytosolic [Ca2+] in Fura-2-loaded dispersed myocytes from WT mice (n = 31/4 cells/mice) and MCI-SM mice (n = 38/4 cells/mice). d Changes in the FPL-evoked increase of cytosolic [Ca2+] induced by 1 μM rotenone (RTN) in WT and MCI-SM femoral myocytes. e Effect of rotenone on the FPL-evoked increase in cytosolic [Ca2+] in WT (n = 24/4 cells/mice) and MCI-SM (n = 17/3 cells/mice) femoral myocytes. f Inhibition of Ca2+ currents by 0.75 μM rotenone (RTN) in acutely dispersed femoral arterial myocytes from WT mice. Note that rotenone prevented any further effect of hypoxia (RTN+Hx, left) or 300 μM cyanide (RTN + CN, right). g Peak Ca2+ current density in WT myocytes at 10 mV under control conditions (n = 11/3 cells/mice) and in the presence of 0.75 μM rotenone (n = 11/3 cells/mice), 0.75 μM rotenone+hypoxia (n = 11/3 cells/mice), or 0.75 μM rotenone+300 μM cyanide (n = 9/3 cells/mice). In c, e and g data are presented as mean ± SEM with statistically significant P values (<0.05) indicated in each panel. The box plot in b represents median (middle line), 25th, 75th percentile (box), and largest and smallest values range (whiskers). In b P values were calculated with the two tailed Mann–Whitney test. In c and e comparison of values was done by two-tailed unpaired t tests. In g comparisons were performed by one-way ANOVA followed by Tukey’s multiple comparisons post hoc test. Source data are provided as a Source Data file.
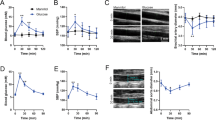
As responsiveness to hypoxia may change in different arterial segments and territories8,17, we also studied cerebral arterial VSM cells, as a representative example of resistance myocytes, which have a smaller size (Fig. 3a) and capacitance (Supplementary Figs. 3a and 10a) than femoral myocytes but similar O2-sensitive Ca2+ currents (Fig. 3b, c). Passive electrical parameters and Ca2+ current amplitudes of cerebral myocytes were unaffected by MCI deficiency (Supplementary Fig. 10a); however, the modulation of Ca2+ channel activity by hypoxia was abolished (Fig. 3b, c; Supplementary Fig. 10b, c). We also tested that modulation of FPL- or high extracellular K+-induced transmembrane Ca2+ influx by hypoxia was abolished in MCI-deficient myocytes from middle or posterior cerebral arteries (example of resistance VSM cells) (Fig. 3d–f) and from aorta (example of myocytes from conduit and more elastic artery) (Supplementary Figs. 11a–c). Consistent with the findings in single femoral and cerebral myocytes, endothelium-denuded femoral arteries resected from MCI-SM mice showed a normal passive diameter and contractile responses to FPL, high K+ and caffeine, although they had strongly inhibited hypoxia-induced vasodilation (Fig. 3g–j).
a Representative photomicrographs comparing acutely dispersed myocytes obtained from femoral (upper panel) and cerebral (lower panel) arteries. b Differential modulation of Ca2+ channels by hypoxia (O2 tension ~15 mmHg) in cerebral arterial myocytes from WT and MCI-SM mice. Current traces are superimposed to facilitate comparison. c Effect of hypoxia expressed as percentage inhibition of the current elicited at −10, 0, 10 and 20 mV in cerebral arterial myocytes from WT (blue dots) and MCI-SM (orange dots) mice (n = 10/3 cells/mice). d Changes in the FPL-evoked increase of cytosolic [Ca2+] by hypoxia, in Fura-2-loaded cerebral arterial myocytes from WT and MCI-SM mice. e Increase in cytosolic [Ca2+] elicited by 1 μM FPL in dispersed cells from WT mice (n = 21/3 cells/mice) and MCI-SM mice (n = 27/3 cells/mice). f Effect of hypoxia on the FPL-evoked increase in cytosolic [Ca2+], shown as percentage of the peak FPL-evoked signal in Fura-2 loaded dispersed cells from WT mice (n = 21/3 cells/mice) and MCI-SM mice (n = 27/3 cells/mice). g Changes in the FPL-evoked increase in arterial wall tension induced by hypoxia in femoral arterial rings from WT and MCI-SM mice. h Basal internal vessel circumference in WT and MCI-SM femoral rings (n = 14/4 rings/mice). i Box plot of isometric force generated in arterial rings from WT and MCI-SM mice in response to either 1 μM FPL (n = 21/7 rings/mice), 70 mM KCl (n = 18/7 and 19/7 rings/mice, respectively) or 5 mM caffeine (n = 13/4 rings/mice). j Effect of hypoxia on the FPL-induced contraction of WT and MCI-SM arterial rings (n = 14/4 rings/mice). In c, e, f, h and j data are presented as mean ± SEM with statistically significant P values (<0.05) indicated in each panel. P values were calculated with two-tailed unpaired t tests. In i the box plots represent median (middle line), 25th, 75th percentile (box), and largest and smallest values range (whiskers). P values were calculated with the Kruskal-Wallis test followed by Dunn’s multiple comparisons post hoc test. Source data are provided as a Source Data file.
Taken together, these data indicate that mice can survive MCI disruption in VSM, although they exhibit hyperlactatemia, decreased systemic blood pressure, and strong inhibition of HVD. Remarkably, MCI-deficient arterial myocytes have a normal morphology, electrical parameters, voltage-gated ionic currents, and response to caffeine but lack the hypoxic inhibition of transmembrane Ca2+ influx. These functional alterations appear to be due to the loss of L-type Ca2+ channel modulation by O2, a physiological process whose underlying mechanism has remained unknown and is now shown to be strictly dependent on MCI function.
Interaction of O2-dependent mitochondrial signals with Ca2+ channels
The production of intracellular reactive oxygen species (ROS) of mitochondrial origin has been reported in several VSM cell types exposed to hypoxia60,61,62. On the other hand, in O2 sensing carotid body glomus cells, hypoxia induces rapid and reversible increases in NADH and H2O2, which are abolished by MCI-deficiency44. It has recently been proposed that acute O2 sensing in glomus cells relies on a slowdown of the mitochondrial electron transport chain (ETC) in hypoxia and a subsequent backlog of electrons with the accumulation of NADH and ROS (H2O2) in the mitochondrial intermembrane space (IMS) (Fig. 4a). After equilibration with the cytosol, these mitochondrial signals, which are also produced by the rotenone-induced blockade of MCI, modulate membrane ion channels to induce glomus cell depolarization and transmitter release44,47. To test whether similar mitochondrial-to-membrane signaling mechanisms operate in VSM cells, we studied the effects of the intracellular application of NADH and H2O2, as well as the reducing agent N-acetylcysteine (NAC), on Ca2+ currents in dialyzed patch-clamped WT myocytes (Fig. 4b). We also assessed the effect of pharmacological modulation of the intracellular NADH/NAD+ ratio by extracellular application of highly membrane permeable α-hydroxybutyrate or α-ketobutyrate (αHB/αKB)47,63 (Fig. 4b). Both internal NADH and H2O2 at concentrations near estimated physiological levels produced a clear dose-dependent inhibition of Ca2+ currents, with the effects of the two agents found to be additive (Fig. 4c, d; and Supplementary Fig. 12a, b). Similar to hypoxia (see Figs. 1i–l), NADH and H2O2 consistently decreased Ca2+ current amplitude without affecting their activation or deactivation kinetics (Fig. 4e, f). Modulation of the Ca2+ current by hypoxia was blunted or even abolished in cells already loaded with relatively low doses of NADH plus H2O2 (Fig. 4c, g).
a Scheme of the mitochondrial electron transport chain and acute dynamic changes induced by hypoxia (Hx, red lines and symbols) in acute O2-sensing cells. IMS (mitochondrial intermembrane space), CoQH2 (reduced ubiquinone), RTN (rotenone), CN (cyanide). b Schematic drawing of a whole-cell patch-clamped myocyte dialyzed with 4 mM ATP plus variable concentrations of NADH, H2O2 or N-acetylcysteine (NAC). Membrane-permeable α-ketobutyrate (α-KB) and α-hydroxybutyrate (α-HB) were applied extracellularly. c Inhibition of femoral myocyte Ca2+ currents by hypoxia (O2 tension ~15 mmHg) and by intracellular dialysis with NADH (200 μM), H2O2 (25 μM), or both. d Peak current density at 10 mV under the experimental conditions indicated in (c). Number of cells/mice: Control (blue dots, 16/7); NADH (yellow dots, 9/3); H2O2 (orange dots, 8/3); NADH + H2O2 (brown dots, 10/4). e Box plot illustrating the time course of activation (time to reach half the maximal value; t1/2) of Ca2+ currents recorded from WT myocytes at 10 mV. C, control conditions (n = 10/4 cells/mice); NADH + H2O2, cells dialyzed with 200 μM NADH plus 25 μM H2O2 (n = 10/4 cells/mice). f Time course of deactivation (tau of fast component of tail current) of Ca2+ currents recorded from WT myocytes at −70 mV. C and NADH + H2O2 as indicated in (e). g Effect of hypoxia expressed as percentage inhibition of the current elicited at −10, 0, 10 and 20 mV in femoral myocytes from WT mice, under control conditions (n = 5/4 cells/mice) or dialyzed with 200 μM NADH + 25 μM H2O2 (n = 10/4 cells/mice). In d, f, and g data are presented as mean ± SEM with statistically significant P values (<0.05) indicated in each panel. In d comparisons were performed by one-way ANOVA followed by Tukey’s multiple comparisons post hoc test. In f and g comparisons were calculated using two-tailed unpaired t tests. In e the box plot represents median (middle line), 25th, 75th percentile (box), and largest and smallest values range (whiskers). P value was calculated with the two tailed Mann–Whitney test. Source data are provided as a Source Data file.
Dialysis of myocytes with NAC (0.5 mM) did not appreciably change the Ca2+ current amplitude (Fig. 5a, b), but did strongly inhibit the hypoxic modulation of these channels (Fig. 5a, c). Moreover, the application of cell-permeant αHB, which increases intracellular NADH levels, decreased, as seen with hypoxia, the amplitude of the Ca2+ current (Fig. 5d, e). In contrast, αKB, which reduces intracellular NADH47,63, had little effect by itself but decreased the hypoxic modulation of the current (Fig. 5d, f). These data indicate that the increase in intracellular NADH and H2O2 levels produces a robust inhibition of myocyte Ca2+ currents similar to that elicited by hypoxia or rotenone, and that lowering PO2 does not have any further effect on the current once NADH and H2O2 are interacting with the Ca2+ channels. Loading the cells with NAC can prevent the action of hypoxia-generated H2O2, while the increase in NADH alone (application of extracellular αHB) partially mimics hypoxia. These findings strongly suggest that the fast, reversible, and MCI-dependent hypoxic modulation of myocyte L-type Ca2+ channel activity is mediated by mitochondrial NADH and H2O2.
a Ca2+ current traces recorded at 10 mV from dispersed femoral arterial myocytes. Left, Superimposed traces obtained in control conditions and in cells dialyzed with N-acetylcysteine (NAC). Right, Superimposed traces obtained in cells dialyzed with NAC before and after exposure to hypoxia. b Current density at 10 mV in control conditions (n = 5/4 cells/mice) and in the presence of 500 μM NAC (n = 11/4 cells/mice). c Effect of hypoxia, expressed as percentage inhibition of the current elicited at −10, 0, 10 and 20 mV on myocyte Ca2+ currents recorded in control conditions (n = 9/6 cell/mice) or in cells dialyzed with 500 μM NAC (n = 11/4 cells/mice). d Inset. Scheme representing the reversible conversion of αKB into αHB in cells with parallel consumption or generation of NADH. LDH (lactate dehydrogenase), HBDB (β-hydroxybutyrate dehydrogenase). Modulation of Ca2+ channels by extracellular application of 2.5 mM αHB or 2.5 mM αKB in femoral myocytes (see Fig. 4b). The effects of hypoxia are also shown. e Ca2+ current density at 10 mV recorded in myocytes under control conditions and in the presence of 2.5 mM αHB or 2.5 mM αHB+hypoxia (n = 14/4 cells/mice). f Ca2+ current density at 10 mV recorded in femoral myocytes in control conditions and in the presence of 2.5 mM αKB or 2.5 mM αKB+hypoxia (n = 15/3 cells/mice). Data in b, c, e and f are presented as mean ± SEM with statistically significant P values (<0.05) indicated in each panel. Comparisons were calculated using two-tailed unpaired t tests. Source data are provided as a Source Data file.
Transgenic expression of yeast NADH dehydrogenase in MCI-deficient arterial myocytes restores O2 modulation of Ca2+ channels
Given the essential role played by MCI in acute hypoxia signaling in arterial myocytes, we tested whether transgenic expression of Ndi1, a single-molecule yeast NADH dehydrogenase, can rescue Ca2+ channel sensitivity to hypoxia in MCI-deficient VSM cells. Ndi1 is attached to the inner mitochondrial membrane and transfers electrons from NADH to CoQ, but unlike MCI this activity is not coupled to a proton pump45 (Fig. 6a). In this way, Ndi1 expression allowed us to assess if the recovery of NADH dehydrogenase activity by itself, without the electrochemical gradient generated by MCI, is sufficient to induce functional recovery in MCI-null myocytes. To this end, we generated two new conditional adult mouse models (named WT/NDI1-SM and MCI/NDI1-SM) in which TMX treatment induced Ndi1 expression in WT and MCI-SM mice, respectively (Fig. 6b). We showed immunocytochemical evidence of Ndi1 expression in VSM cells (Fig. 6c) and the appropriate selective down-/up-regulation of Ndufs2 and Ndi1 mRNAs, respectively, in arteries of the various mouse strains (Fig. 6d, e). Ndi1 expression did not induce any major alteration in survival, body weight or organ size in WT mice; however, the presence of Ndi1 rescued practically all the systemic structural and functional alterations observed in MCI-SM mice (Supplementary Figs. 13a–d). Notably, increased lactatemia and low systolic and diastolic blood pressures, which were characteristic features of MCI-SM mice (see Fig. 1e, f), showed full recovery in MCI/NDI1-SM mice (Fig. 6f, g).
a Scheme illustrating the replacement of mitochondrial complex I (MCI) with Ndi1 in the MCI/NDI1-SM mouse model. b Experimental MCI/MDI1-SM mouse model and time course of tamoxifen (TMX) treatment. c Immunostaining illustrating α-smooth muscle actin (α-SMA, red) and Ndi1 expression (green fluorescent protein, GFP) in freshly dispersed femoral arterial myocytes from WT (upper panel) and WT/NDI1-SM (lower panel) mice. d, e Ndufs2 and Ndi1 mRNA levels in aortas from WT (blue dots), MCI-SM (orange dots), MCI/NDI1-SM (green dots) and WT/NDI1-SM (black dots) mice (n = 5 replicates per group, with each replicate consisting of one mouse of the corresponding genotype). f Basal plasma lactate levels in WT mice (n = 8), MCI-SM mice (n = 8) MCI/NDI1-SM mice (n = 11) and WT/NDI1-SM mice (n = 9). g Systolic and diastolic blood pressure in WT mice (n = 11, 10 respectively), MCI-SM mice (n = 11, 10 respectively) MCI/NDI1-SM mice (n = 12, 12 respectively) and WT/NDI1-SM mice (n = 10, 10 respectively). h Macroscopic current traces illustrating the reversible inhibition of L-type Ca2+ channel currents by hypoxia in femoral arterial myocytes from WT/NDI1-SM and MCI/NDI1-SM mice. i Effect of hypoxia expressed as percentage inhibition of the Ca2+ current elicited at −10, 0, 10 and 20 mV in femoral arterial myocytes from WT/NDI1-SM mice (n = 12/4 cells/mice) and MCI/NDI1-SM mice (n = 11/4 cells/mice). In d–g, and i, data are presented as mean ± SEM with statistically significant P values (<0.05) indicated in each panel. In d–g comparisons were performed by one-way ANOVA followed by Tukey’s multiple comparisons post hoc test. In i comparison of values were performed by two-tailed unpaired t tests. Source data are provided as a Source Data file.
While Ndi1 expression in WT myocytes did not produce any change in Ca2+ current amplitude or modulation by O2 (Supplementary Fig. 13e), Ndi1 did induce an almost complete recovery of the inhibition of Ca2+ current by hypoxia in MCI/NDI1-SM myocytes (Fig. 6h, i, and Supplementary Fig. 13f), which was abolished in MCI-null VSM cells (see Figs. 1i, m). In agreement with these data, inhibition of FPL-induced transmembrane Ca2+ influx by hypoxia, which was blunted by Ndufs2 deficiency (see Fig. 2a–c), was also rescued in Ndi1-expressing myocytes (Fig. 7a, left, b, c). In contrast, the responsiveness of FPL-induced transmembrane Ca2+ influx to rotenone (see Fig. 2d, e) was not recovered in MCI/NDI1-SM myocytes, where it is well known that Ndi1 is insensitive to this drug45 (Fig. 7a right, d).
a Changes in the FPL-evoked increase of cytosolic [Ca2+] by hypoxia (left) and 1 μM rotenone (right), in intact Fura-2-loaded femoral arterial myocytes from MCI/NDI1-SM mice. b Box plot of increases in cytosolic [Ca2+] elicited by 1 μM FPL in dispersed myocytes from WT (n = 31/3 cells/mice), MCI-SM (n = 38/4 cells/mice) and MCI/NDI1-SM (n = 21/3 cells/mice) mice. c Box plot representing the effect of hypoxia on the FPL-evoked increase of cytosolic [Ca2+], shown as percentage decrease of the peak FPL-induced signal in Fura-2-loaded dispersed myocytes from WT (blue dots, n = 31/3 cells/mice), MCI-SM (orange dots, n = 38/4 cells/mice) and MCI/NDI1-SM (green dots, n = 21/3 cells/mice) mice. d Quantification of the effect of rotenone on the FPL-evoked increase of cytosolic [Ca2+] in dispersed myocytes from WT (n = 24/4 cells/mice), MCI-SM (n = 17/3 cells/mice) and MCI/NDI1-SM (n = 16/3 cells/mice) mice. e Hypoxia and αKB-induced changes in NADH autofluorescence (AF in arbitrary units, arb. units) recorded in arterial myocytes from WT, MCI-SM and MCI/NDI1-SM mice. f Box plot showing the maximal increase in NADH autofluorescence (arb. units) in response to hypoxia, in arterial myocytes from WT (n = 19/7 cells/mice), MCI-SM (n = 22/9 cells/mice) and MCI/NDI1-SM (n = 23/9 cells/mice) mice. In d data are presented as mean ± SEM with statistically significant P values (<0.05) indicated. Comparisons were performed by one-way ANOVA followed by Dunnett’s multiple comparisons post hoc test. Box plots in b, c and f represent median (middle line), 25th, 75th percentile (box), and largest and smallest values range (whiskers). P values were calculated with the Kruskal-Wallis test followed by Dunn’s multiple comparisons post hoc test. Source data are provided as a Source Data file.
To further demonstrate the recovery of hypoxia signaling in Ndi1 expressing MCI-deficient myocytes, we recorded reversible changes in NADH autofluorescence induced by hypoxia in single dispersed myocytes using two photon microfluorimetry. As shown previously in O2-sensitive glomus cells47, hypoxia induced rapid and reversible increases in NADH levels in WT myocytes. This signal was practically abolished in cells from MCI-SM mice and was fully recovered in MCI/NDI1-SM myocytes (Fig. 7e, f). In all these genetically different cell types, a clear decrease in NADH levels was observed after addition of αKB (1 mM) (Fig. 7e), which permeates to the cell interior and consumes NADH during its conversion to αHb (see Fig. 5d). These data further support the view that the essential role played by MCI during hypoxia is to generate the signaling molecules (NADH and H2O2) that regulate Ca2+ channels. In this regard, Ndufs2 deficiency can be fully rescued by the transgenic expression of yeast NADH dehydrogenase.
Acute O2 sensitivity of arterial myocytes relies on the constitutive activity of Hif1α and expression of atypical cytochrome c oxidase subunits
The hypoxia inducible transcription factors Hif1α and Hif2α are key mediators of cellular transcriptional responses to hypoxia64. We have shown that Hif2α, which is expressed at constitutively high levels in the carotid body65,66,67, is required for induction of a transcriptional program that determines the expression of atypical MCIV subunit isoforms conferring acute responsiveness of chemoreceptor glomus cells to physiological hypoxia68,69,70. Given that Hif2α is expressed in systemic arteries, although at lower levels than in the lung (Supplementary Fig. 14a), we investigated whether conditional deletion of the Hif2α gene (Epas1) also alters myocyte acute O2 sensing. To this end, we analyzed the EPAS1-ESR mouse model with a TMX-induced loss of Epas1 alleles in adulthood68 (Supplementary Fig. 14b). We found a marked selective decrease of Epas1 mRNA in the aortas of EPAS1-ESR mice, however no changes in mRNA levels of relevant MCIV subunit isoforms were observed (Supplementary Fig. 14c). Modulation of Ca2+ channel activity (Supplementary Figs. 15a–d) and FPL-mediated Ca2+ influx (Supplementary Figs. 15e–g) during hypoxia were also unaltered in Hif2α-deficient myocytes. These findings indicated that Hif2α is not responsible for the acute O2 sensitivity of systemic VSM cells. They also led us to hypothesize that the expression of MCIV subunit isoforms presumably involved in acute O2 sensing could be under the transcriptional control of Hif1α, which is expressed in arterial smooth muscle at higher levels than those seen for Hif2α (Supplementary Fig. 16a).
To address this question, we generated adult HIF1α-SM mice with a conditional loss of Hif1α alleles in VSM cells (Fig. 8a) following the same breeding protocol and TMX treatment described for MCI-SM mice (see Fig. 1a). We confirmed a marked selective decrease in Hif1α mRNA levels in aortic tissue (with unchanged Epas1 mRNA levels) paralleled by a manifest mRNA down-regulation of relevant atypical MCIV subunit isoforms, such as Cox4i2 or Cox8b68, as well as Pgk1, a well-known Hif1α-dependent gene encoding a glycolytic enzyme71,72. Other mRNA species encoding MCIV subunits (Ndufa4l2, Ndufa4), enzymes (Pcx), or transcription factors suggested to regulate the expression of MCIV subunits (Rbpj, Chchd2, Cxxc5)73 were either less affected or unaltered (Fig. 8b, c). Remarkably, HIF1α-SM mice did not show any major alteration in body weight or gross modification of organ size, hematocrit or heart rate (Supplementary Figs. 16b–e). However, similar to MCI-SM mice (see Fig. 1f), HIF1α-SM mice showed a clear decrease in systolic and diastolic blood pressures (Fig. 8d). Hif1α-deficient femoral artery myocytes appeared normal, with an unchanged density of L-type Ca2+ channels (Supplementary Figs. 16f, g). However, in these myocytes, modulation of Ca2+ channel activity by hypoxia, as evidenced both by direct measurements of whole-cell currents and by FPL-induced transmembrane Ca2+ influx in Fura-2-loaded isolated cells, were practically abolished (Fig. 8e–i, Supplementary Figs. 16f, g). In contrast, the rise in cytosolic [Ca2+] induced by either caffeine or phenylephrine (an α1 receptor agonist)74, was unaffected (Fig. 8j). These data indicated that O2 modulation of Ca2+ channel activity in arterial myocytes depends on Hif1α, possibly due to the expression of Hif1α-dependent mitochondrial MCIV subunit isoforms.
a Experimental HIF1α-SM mouse model and time course of tamoxifen (TMX) treatment. b, c Box plot (b) and scatter diagram (c) of mRNA levels of Hif1α and other genes potentially involved in acute O2 sensing and mitochondrial function in aortas of WT and HIF1α-SM mice. N values in WT and HIF1α-SM mice, respectively, were: Hif1α (18, 20), Cox4i2 (20, 20); Epas1 (22, 22); Cox4i1 (12, 12); Cox8b (10, 11); Cox8a (12, 12); Ndufa4l2 (11, 10); Ndufa4 (12, 12); Pgk1 (7, 7); Pcx (11, 9); Rbpj (4, 5); Chchd2 (4, 5) and Cxxc5 (4, 5). d Systolic and diastolic blood pressure in WT (n = 6) and HIF1α-SM (n = 6) mice. e Macroscopic current traces illustrating the differential modulation of Ca2+ channels by hypoxia in acutely dispersed femoral arterial myocytes from WT and HIF1α-SM mice. f Effect of hypoxia expressed as percentage inhibition of the current elicited at −10, 0, 10 and 20 mV in femoral arterial myocytes from WT mice (n = 9/5 cells/mice) and HIF1α-SM mice (n = 11/5 cells/mice). g Changes of the FPL-evoked increase in cytosolic [Ca2+] by hypoxia in intact Fura-2-loaded femoral arterial myocytes from WT and HIF1α-SM mice. h Increase in cytosolic [Ca2+] elicited by 1 μM FPL in dispersed cells from WT mice (n = 20/3 cells/mice) and HIF1α-SM mice (n = 20/3 cells/mice). i Box plot showing the effect of hypoxia on the FPL-evoked increase of cytosolic [Ca2+], expressed as percentage decrease in the peak FPL signal, in Fura-2-loaded dispersed cells from WT mice (n = 20/3 cells/mice) and HIF1α-SM mice (n = 23/3 cells/mice). j Increase in cytosolic [Ca2+] elicited by 5 mM caffeine (CAF) and 300 μM phenylephrine (PE) in dispersed cells from WT mice (n = 32/3 and 19/3 cells/mice, respectively) and HIF1α-SM mice (n = 49/3 and 21/3 cells/mice, respectively). In c, d, f, h and j data are presented as mean ± SEM with statistically significant P values (<0.05) indicated in each panel. Box plots in b and i represent median (middle line), 25th, 75th percentile (box), and largest and smallest values range (whiskers). P values were calculated with two tailed Mann–Whitney tests. In c, d, f, h, and j comparisons were performed by two-tailed unpaired t tests. Source data are provided as a Source Data file.
Among the MCIV subunits whose mRNA expression was modulated by Hif1α in arterial myocytes (see Fig. 8b, c), we focused on Cox4i2, a tissue-specific Cox4 isoform that is highly expressed in the lung75 and the carotid body66,67, and which is induced by hypoxia in several cell classes in a Hif1α-dependent manner76. Expression of Cox4i2 instead of Cox4i, the most common subunit isoform, alters cytochrome c oxidase (CCO) activity75,76,77 and is essential for ROS production and depolarization of cultured pulmonary VSM cells in response to hypoxia78. Mice lacking Cox4i2 show abolition of the acute phase of hypoxic pulmonary vasoconstriction78 and strong inhibition of the acute O2-sensing properties of CB glomus cells68. To analyze the participation of Cox4i2 in the acute O2-modulation of Ca2+ channel activity in systemic arterial myocytes, we generated adult conditional Cox4i2-deficient mouse models using either TMX-activatable generalized Ubiquitin (UBC)-Cre or smooth muscle-specific SM-Cre (COX4I2-UBC and COX4I2-SM mice, respectively) (Fig. 9a). In the two mouse models, we observed a clear selective decrease in Cox4i2 mRNA in aortic myocytes (Fig. 9b, c). In addition, we showed a decrease in Cox4i2 immunostaining in Cox4i2-deficient femoral myocytes (Fig. 9d). COX4I2-SM mice showed normal body weight, organ size and hematocrit (Supplementary Figs. 17a–c). However, we observed a strong inhibition of the hypoxic modulation of Ca2+ currents measured in dispersed Cox4i2-deficient femoral VSM cells (Fig. 9e, f; Supplementary Figs. 17d, e). Moreover, endothelium-denuded femoral arteries removed from these mice had normal passive diameters and contractile responses to FPL and high K+, but were, nevertheless, practically insensitive to hypoxia (Fig. 9g–j). These observations suggest that the Hif1α-dependent expression of Cox4i2 in vascular myocytes plays a fundamental role in the acute modulation of Ca2+ channel activity by PO2 and in HVD.
a Experimental COX4I2-deficient mouse models and time course of tamoxifen (TMX) treatment. b Cox4i2 (n = 4, 4) and Cox4i1 (n = 5, 4) mRNA levels in aortas from WT (blue dots) and COX4I2-SM (orange dots) mice, respectively (n replicates, with each replicate consisting of one mouse of the corresponding genotype). c Cox4i2 and Cox4i1 mRNA levels in aortas from WT and COX4I2-UBC mice (n = 5 replicates per group, with each replicate consisting of one mouse of the corresponding genotype). d Representative immunostaining of Cox4i2 (green) and alpha-smooth muscle actin (α-SMA, red) in acutely dispersed femoral arterial myocytes from WT (upper panel) and COX4I2-SM (lower panel) mice. e Macroscopic current traces demonstrating the differential modulation of Ca2+ channels by hypoxia in acutely dispersed femoral arterial myocytes from WT and COX4I2-UBC mice. f Effect of hypoxia expressed as percentage inhibition of the current elicited at −10, 0, 10 and 20 mV in femoral arterial myocytes from WT mice (n = 11/4 cells/mice) and COX4I2-UBC (n = 10/4 cells/mice) mice. g Changes in the FPL-evoked increase in arterial wall tension induced by hypoxia in femoral arterial rings from WT and COX4I2-SM mice. h Quantification of the internal vessel circumference under passive conditions in femoral arterial rings from WT mice (n = 12/4 cells/mice) and COX4I2-SM (12/4 cells/mice) mice. i Quantitative analysis of isometric force generated in arterial rings from WT and COX4I2-SM mice in response to either 1 μM FPL (n = 12/4 rings/mice) or 70 mM KCl (n = 12/4 rings/mice). j Quantification of the effect of hypoxia on the FPL-induced contraction, shown as percentage of the peak FPL-induced force, in arterial femoral rings from WT mice (n = 12/4 rings/mice) and COX4I2-SM (n = 12/4 rings/mice) mice. Data are presented as mean ± SEM with statistically significant P values (<0.05) indicated in each panel. In b, c, f, h, i, and j comparisons were performed using two-tailed unpaired t tests. Source data are provided as a Source Data file.
Discussion
Two main conclusions can be drawn from the studies presented in this paper. The first is that acute modulation of L-type Ca2+ channels by PO2 in systemic arterial myocytes depends on the integrated functions of mitochondria working as O2 sensors and effectors. The O2 modulation of Ca2+ channels is abolished in MCI-deficient cells, but can be rescued by the transgenic expression of a yeast NADH dehydrogenase, and mimicked by the intracellular application of NADH and H2O2. Remarkably, modulation of Ca2+ channels by O2 depends on dynamic changes in the mitochondrial ETC, and requires a permanent, constitutive activation of Hif1α, which in turn determines the expression of at least one atypical MCIV subunit isoform. It must be also stressed that our electrophysiological studies, done on VMS cells dialyzed with 4 mM MgATP, strongly suggest that changes in intracellular ATP levels21,32,35,41,54,55 are not involved in inhibition of Ca2+ channel activity and depolarization-induced Ca2+ influx during hypoxia. These findings support a mitochondrial-to-membrane signaling (MMS) model of acute O2 sensing44,68 in which the decrease in MCIV activity under hypoxia leads to a backlog of electrons along the ETC and an increase in the reduced ubiquinone (CoQH2) pool. This results in a slowdown of MCI activity and the accumulation of NADH and H2O2 which interact with Ca2+ channels (Fig. 10). This model provides a mechanistic explanation for the rapid and reversible inhibition of Ca2+ currents by hypoxia, a phenomenon observed in myocytes from several mammalian systemic conduit and resistance arteries whose underlying mechanisms have remained unknown9,35,37,39,40,41.
The mitochondrial-based O2-sensing system in arterial myocytes resembles in many aspects the MMS pathway supporting the acute O2-dependent control of membrane excitability in carotid body glomus cells that is responsible for the ventilatory response to hypoxia45,50,68. Although studied in less detail, similar mechanisms appear to mediate acute O2 sensing and responsiveness to hypoxia in other peripheral chemoreceptors, such as cells in the embryonic/neonatal adrenal medulla and the abdominal paraganglia44,79. Moreover, the mitochondria production of H2O2 in myocytes of resistance arteries has been suggested to mediate acute pulmonary artery vasoconstriction60,61,62. It seems, therefore, that the MMS model described here for HVD could be a general mechanism that operates in organs of the homeostatic acute O2 sensing system80. To function as O2 sensors within physiological ranges of PO2, mitochondria require the expression of atypical MCIV subunit isoforms (Cox4i2 and others) that may alter the catalytic activity (affinity for O2 and/or accessibility of substrates to the active site) of CCO68,77. Remarkably, whereas in carotid body glomus cells and catecholaminergic peripheral chemoreceptors the expression of Cox4i2 depends on the constitutive high expression of Hif2α,68,79 in systemic arterial myocytes the same process relies on the constitutive activity of Hif1α, which further indicates that the two transcription factors are not redundant but that they have tissue-specific specializations81,82.
Our results strongly suggest that NADH and H2O2 are the mitochondrial hypoxic signals that inhibit Ca2+ channel activity in arterial myocytes. This observation fits well with previous data indicating that recombinant as well as native L-type Ca2+ channels are modulated by H2O242,83,84,85. Nicotine dinucleotides have been shown to bind and modulate several subtypes of K+ channels; however, their effect on other ion channel types is less known86. Although in our studies HVD seemed to depend mainly on the inhibition of Ca2+ channel activity, it is conceivable that modulation of other channel types by PO2 contributes to vasodilation in specific arterial segments, given the functional heterogeneity existing in vascular territories8,17. The activation of voltage-gated K+ channels has been suggested to participate in HVD87, with a recent study in myocytes from small-diameter mouse mesenteric arteries showing that intracellular NADH stimulates K+ channel activity and enhances the sensitivity of the channel to H2O288. NADH and H2O2 are promiscuous molecules whose actions probably depend on the ion channel subunits expressed in the various VSM cells and the existence of O2 sensing microdomains formed by mitochondria placed near clusters of specific ion channel classes (e.g., L-type Ca2+ channels) in the plasma membrane89. In addition to NADH and H2O2, it has been suggested that oxidation of the constitutively produced redox reagent hydrogen sulfide (H2S) by the enzyme sulfide-quinone oxidoreductase (SQR) in VSM cells contributes to the CoQH2 pool. In this way, accumulation of CoQH2 during hypoxia leads to an increase in H2S90. We did not consider H2S to be a relevant hypoxic signal in our studies because rotenone and piericidin A, selective inhibitors of MCI, completely inhibited the effect of hypoxia on Ca2+ channels.
The second far-reaching conclusion from our work is that the modulation of Ca2+ channels by PO2 in arterial myocytes is a process of functional relevance. Circulatory blood flow is regulated by a complex ensemble of signaling pathways that show redundancy and compensation7,8,91. However, we found that both modulation of Ca2+ channel activity by PO2 in single myocytes and HVD of whole arteries ex vivo are selectively abolished in adult Ndufs2-, Cox4i2-, or Hif1α-deficient mice, despite the vessels and myocytes having a normal structure, electrophysiology, and responses to other vasoactive agents (FPL, high K+, caffeine, or phenylephrine). Moreover, adult MCI-SM or HIF1α-SM mice, which did not show O2 modulation of myocyte Ca2+ channels, presented with a decrease in basal systemic blood pressure. These alterations in the control of tissue blood perfusion at rest could have severe consequences for the maintenance of homeostasis under challenging conditions (e.g., physical exercise or sojourn at high altitude) or for long-term adaptive brain and cardiac functions. In addition to their pathophysiological significance, our findings provide new scenarios (NADH mimetics, mitochondrial metabolism, and HIF inhibitors among others) of potential interest in cardiovascular pharmacology.
Methods
Genetically modified mouse models
MCI-SM mice
Mice carrying Ndufs2 floxed allele44 were bred with those carrying tamoxifen-induced CRE recombinase under the control of smooth muscle cell-specific SM22α promoter48 to generate NDUFS2 adult conditional knockout mice (Ndufs2 flox/-;SM22-Cre, named as MCI-SM in the text and figures).
MCI/NDI1-SM and WT/NDI1-SM mice
MCI-SM mice were bred with mice carrying a lox-STOP-lox site preceding yeast Ndi1 sequence targeted to the Rosa26 locus45. The resulting mice (MCI/NDI1-SM mice) expressed NDI1 in NDUFS2-deficient VSM cells. Mice carrying yeast NADH dehydrogenase (NDI1) and green fluorescent protein (GFP) sequences were also bred with those carrying tamoxifen-induced CRE recombinase under the control of SM22α promoter to express NDI1 in VSM cells (named as WT/NDI1-SM).
HIF1α-SM mice
Mice carrying Hif1α floxed allele (The Jackson laboratory, Stock No: 007561)92 were bred with those carrying tamoxifen-induced CRE recombinase under the control of smooth muscle cell-specific SM22α promoter to generate HIF1α adult conditional knockout mice (HIF1α flox/-;SM22-Cre, named as HIF1α-SM in the text and figures).
EPAS1-ESR mice
Mice carrying Epas1 floxed allele (The Jackson laboratory, Stock No: 008407)68,82 were bred with those carrying tamoxifen-inducible Cre recombinase transgene93 to generate HIF2α adult conditional knockout mice (Epas1 flox/-;ESR-Cre, named as EPAS1-ESR in the text and figures).
COX4I2-SM and COX4I2-UBC mice
Mice carrying Cox4i2 floxed allele68,78 were bred with those carrying tamoxifen-induced CRE recombinase under the control of either smooth muscle cell-specific SM22α promoter or human ubiquitin C (UBC) promoter94 to generate COX4I2 adult conditional knockout mice (Cox4i2 flox/-;SM22-Cre and Cox4i2 flox/-;UBC-Cre mice which are named, respectively, as COX4I2-SM and COX4I2-UBC in the text and figures).
Animal maintenance and treatments
Mice were housed at regulated temperature (22 ± 1 °C) in a 12 h light/dark cycle with ad libitum access to food and drink. Both male and female mice were used in the current study. Mice strains were in mixed genetic background (129 Sv:C57BL/6 or 129 Sv:C57BL/6/Balb/c). To induce Cre-mediated recombination, two-months old wild type and knockout mice were treated with tamoxifen-containing diet (TAM400/CreER, 400 mg tamoxifen citrate/kg, Envigo) for a month followed by 1 to 1.5 months of normal diet before experiments. For in vitro studies, animals were sacrificed with intraperitoneal administration of a lethal dose of sodium thiopental (120-150 mg/Kg) before tissue dissection. Dissected tissues were used for either functional, biochemical or histological analyzes. For RNA isolation and measurement of mitochondrial complex I activity, tissues were flash-frozen in liquid N2 and stored at −80 °C until use. All procedures were approved by the Institutional Committee for animal care and use at the University of Seville (PN2019 07/04/2020/051). Handling of the animals was conducted in accordance with the European Community Council directive of 22 September 2010 (Directive 2010/63/EU) and the implementations of 5 June 2019 (Regulation 2019/2010) for the Care and Use of Laboratory Animals. Mice used in the in vivo measurements were subsequently sacrificed for the in vitro experiments in order to minimize the number of animals used in the study.
Plethysmography
Plethysmography used to monitor ventilation in conscious unrestricted rodents has been previously described45,50. Mice were placed inside plethysmographic chambers (EMKA Technologies) and continuously exposed at a constant flow rate (1 L/min) with a gas mixture containing 21% O2, 0.04% CO2 and 78.96% N2 (normoxia); 10% O2, 0.04% CO2 and 89.96% N2 (hypoxia); or 21% O2, 5% CO2 and 74% N2 (hypercapnia). Data acquisition was performed using the software Iox2 (EMKA Technologies). The hermetic chambers were provided with O2 and CO2 sensors to monitor the gas composition in parallel with changes in respiratory frequency recorded by a pressure sensor during the experiment. Each animal was exposed to two cycles of hypoxia (5 min) followed by a final exposure to hypercapnia (2 min).
Measurement of arterial pressure and heart rate
Systolic and diastolic pressures and heart rate were determined by using a non-invasive tail-cuff transmission photoplethysmography (BP-2000) Blood Pressure Analysis System for mice and rats, (Bioseb, in vivo research instruments, RRID:SCR_02 2985). Conscious mice were placed in a restrained cage with automatic temperature control that gently warms the animals. Before taking the real pressure values, mice were recorded for 3 previous days to allow them to get used to the system and to avoid pressure increases due to stress produced by the technique. Values recorded during the 4th and 5th days were used to average systolic and diastolic pressures and heart rate in each mouse.
Measurement of hematocrit and blood lactate
Lactate Plus Meter was used to determine lactate plasma concentration (Nova Biomedical). Control solutions with 1–1.6 mM and 4–5.4 mM lactate, provided by the supplier, were used to calibrate the device. For measurements, a small drop of blood obtained from the mouse tail after a lancet puncture, was placed on the specific strip for lactate quantification. Hematocrit was measured by collecting blood from an incision of the carotid artery using a hematocrit tube allowing blood to flow by capillarity action into tube. The ends of the tube were sealed with bone wax and the tubes were placed in a microhematocrit centrifuge and span for 5 minutes at 2.500 g. The hematocrit is expressed as the percentage of blood volume occupied by erythrocytes.
Measurement of contractility in arterial rings
Femoral arteries were isolated, cleaned of connective and endothelial tissue, cut in rings ( ~ 2 mm in diameter) and mounted on a small vessel myograph (Danish Myo Technology) connected to a digital recorder (AcqKnowledge 3.8.1, BIOPAC System) to measure isometric tension. Endothelium-denuded rings were placed in a chamber with Kreb’s solution and bubbled with 95 % O2 and 5 % CO2 at pH = 7.4. The “hypoxic” solution was bubbled with 5% CO2, and 95% N2. Before the experiments, the segments were subjected to an optimal tension test (90 % tension was equivalent to an intramural pressure of 100 mmHg) and stabilized for at least 1 h, when basal tone was determined in unstimulated arteries. The drugs were added directly to the chamber while vessel tension was monitored. Experiments were performed at ~30 °C.
Histology
Complete femoral arteries (with endothelial and connective tissue) were fixed with 4% paraformaldehyde. Arteries were then cleared and embedded in paraffin. Paraffin sections (6 μm) were dewaxed, rehydrated, and stained with hematoxilin–eosin following standard procedures. Measures were done with ImageJ software (version 1.51 S) and each value was obtained from triplicate determinations of femoral artery from at least four mice in each condition.
Mitochondrial complex I activity dipstick assay
MCI activity in aorta was determined using complex I enzyme activity dipstick assay kit (Abcam) following the manufacturer’s instruction with minor modifications. Aorta arteries pooled from 2 mice were homogenized in 100 µl extraction buffer followed by incubation on ice for 20 minutes. The homogenate was then centrifuged at 16000 g for 30 minutes and the supernatant was collected for the enzymatic assay. 8 µg of protein extract, which was determined using the BioRad protein assay (BioRad), were applied to measure the MCI activity. The signal on the dipstick was scanned with an image analyzer (ImageQuant LAS 4000mini, GE Healthcare) and the signal intensity was quantified using the ImageQuant TL software (GE Healthcare).
Real-time quantitative PCR
Total RNA was isolated from adult mice ( ~ 4 months old) 1–1.5 months after the completion of tamoxifen treatment. Total RNA was isolated from aorta and femoral arteries using RNeasy Micro kit (Qiagen). Due to the small tissue size, each femoral artery replicate was pooled from 2 mice to obtain enough amount of RNA. The RNA quality was determined using an Agilent 2100 Bioanalyzer (Agilent). cRNA was then amplified from VSM total RNA using GeneChip WT PLUS Reagent Kit (Affymetrix). Total RNA from brain and lungs were isolated using Trizol (Ambion, Life Technologies). 500 ng of total RNA (or amplified cRNA in the case of aorta and femoral arteries) was copied to cDNA using QuantiTect Reverse Transcription Kit (Qiagen) in a final volume of 20 μl. Real-time quantitative PCR reactions were performed in a 7500 Fast Real Time PCR System (Life Technologies). PCR reactions were performed in duplicates in a total volume of 20 μl containing 1–4 μl of cDNA solution and 1 μl of Taqman probe of the specific gene (ThermoFisher Scientific) (Supplementary Table 1. Oligonucleotides). Gapdh was also estimated in each sample to normalize the amount of total RNA (or cRNA) input in order to perform relative quantifications.
Preparation of acutely dispersed arterial myocytes
Vascular smooth muscle (VSM) cells from femoral, middle and posterior cerebral arteries, and aorta were obtained after carefully dissection and cleaning of connective and endothelial tissues. Afterwards, small segments of endothelium-free arteries artery were placed in smooth muscle dissociation solution (SMDS, Ca2+ free) containing 1 mg/ml papain (Worthington), 1 mg/ml BSA (Sigma) and 1 mg/ml dithiothreitol (DTT; Sigma) and incubated at 37 °C for 15 min (femoral arteries) or 12 min (cerebral arteries) in a shaking water bath. After two washings in SMDS (with 10 μM Ca2+) a second 15 min (femoral arteries) or 12 min (cerebral arteries) incubation was performed with SMDS (10 μM Ca2+) in a 0.7 mg/ml collagenase F, 0.3 mg/ml collagenase H (Sigma) and 1 mg/ml BSA solution. Single cells were obtained by gentle trituration with a wide-bore glass pipette, plated on glass cover slips treated with poly-L-lysine, stored at 4◦C, and used within the same day. Ionic composition of SMDS was (in mM): NaCl 145; KCl 4.2; KH2PO4 0.6; MgCl2 1.2; Hepes 10; glucose 11, pH adjusted to 7.4 with NaOH.
Immunohistochemistry of isolated arterial myocytes
Freshly isolated VSM cells were plated onto glass cover slips and let to sit for 20 min at room temperature before the immunofluorescence assay. Cells were fixed with 4% paraformaldehyde (PF) in phosphate buffer, pH 7.5, for 15 min at 20 °C, washed in PBTx (PBS, 0.1% Triton X-100), and blocked with PBTx-10 mg/ml BSA-2% normal goat serum for 10 min, Primary antibodies were diluted in blocking solution and incubated with the cells for 60 min at room temperature: COX4I2 (1:100 dilution, 11463-1-1AP, Proteintech); NDUFS2 (1:200 dilution, ab192022, Abcam); α-SMA (1:100 dilution, A2547, Sigma); GFP (1:200 dilution, A11122, Invitrogen). After washes in PBTx, cells were incubated with secondary antibodies for 60 min. The fluorescently labeled secondary antibodies: Alexa 568 or Alexa 488 (1:1000 dilution, A11011, A11015, Invitrogen). Nuclei were labeled with 4’, 6’-diamidino-2-phenylindole (DAPI) staining. Immunofluorescent images were obtained using Leica Stellaris 8 confocal microscopy (Leica) and Leica Application Suite X software (Leica Microsystems).
Electron microscopy
For Transmission Electronic Microscope (TEM) analysis, femoral arteries were fixed for 2 h at 4 °C in 2.5% glutaraldehyde prepared in 0.1 M sodium cacodylated buffer, pH 7.4. After three washing steps (5 min each one), samples were post fixed for 1 hour at 4 °C in 1% osmium tetroxide in the same buffer. After three washing steps (20 min each one), the samples were immersed in 2% uranyl acetate, dehydrated through a gradient acetone series (50%, 70%, 90% and 100%), and embedded in Spurr resin (Tedpella). Blocs were obtained by polymerization at 70 °C for 8 h. Thin sections were cut with a diamond knife in an ultramicrotome (Leica UC7) and examined with a transmission electron microscope (Zeiss Libra 120) operating at 80 kV. The electron microscopy images were taken at different magnifications with an EMCCD camera (TRS 2k × 2k).
Microfluorimetric measurements
For cytosolic Ca2+ measurements, dispersed myocytes from femoral and cerebral arteries, and aorta were incubated in SMDS containing 4 μM Fura 2-AM (F-1221, Molecular Probes) for 30 minutes at room temperature and subsequently incubated for 15 min in SMDS to remove excess Fura2-AM. After loading the cells, the coverslip was transferred to the recording chamber and continuously perfused with external solution. The set up consists of an inverted microscope (Nikon eclipse Ti) equipped with a 40x/0.60 NA objective, a monochromator (Polychrome V, Till Photonics), and a CCD camera, controlled by Aquacosmos software (version 2.6, Hamamatsu Photonics). Alternating excitation wavelengths of 340 and 380 nm were used, and background fluorescence was subtracted before obtaining the F340/F380 ratio. A dichroic FF409-Di03 (Semrock) and a band pass filter FF01-510/84 (Semrock) were used. Cytosolic [Ca2+] signals were digitized at a sampling interval of 500 ms. Experiments were performed at ~35 °C.
NAD(P)H microfluorimetric measurements in dispersed myocytes from femoral artery were performed using two-photon laser scanning microscope (2PLSM) containing a multiphoton galvanometer scanning system (Scientifica Ltd) with an Olympus Å~60/1.0 NA water-dipping objective lens. A Chameleon Ultra II (680–1080 nm), 3.5 W Ti: sapphire laser system (Coherent laser group) provided the 2 P excitation source. Laser power attenuation was achieved using two Pockels cell electro-optic modulators (S-MP-4700 and S-MP-6000-INT/UK) in series controlled by Labview. Labview software was written by Scientifica (version 12.0). Non-descanned emission photons were detected with GaAsP photomultiplier tube (PMT), S-MDU-PMT-50, green, 490 nm to 560 nm. To measure changes in NADH autofluorescence, cells were excited with 720 nm light using a non-ratiometric protocol. Green channel (490–560 nm) fluorescent emission signals were detected using a non-descanned Scientifica S-MDU-PMT-50-50 select GaAsP PMT. Continuous acquisition mode (rate of 0.76 f.p.s., 146 n pixels) was used for the selected wavelength. Time series analysis was conducted offline using ImageJ (version 1.51 S). Multiple cytosolic ROIs and a background ROI were measured, the background was subtracted for each ROI at each time point. As recording control, 1 mM αKB was added to the external solution (showing a clear decrease in the basal NADH autofluorescence level) at the end of each experiment.
Patch clamp recordings in dispersed myocytes
Macroscopic ionic currents were recorded from dispersed mouse arterial myocytes using the whole cell configuration. Patch clamp pipettes (2–3 MΩ) were pulled from capillary glass tubes (Kimax, Kimble Products) with a horizontal pipette puller (Sutter instruments model P-1000) and fire-polished with a microforge MF-830 (Narishige). Voltage-clamp recordings were obtained with an EPC-7 amplifier (HEKA Electronik). The signal was filtered (3–10 kHz), subsequently digitized with an analog/digital converter (ITC-16 Instrutech Corporation) and finally sent to the computer. Data acquisition and storage was performed using the PULSE/PULSEFIT software (HEKA, Electronics) at a sampling interval of 20 μs. Experiments were performed at room temperature.
Recording solutions
For microflourimetric measurements, dispersed myocytes were transferred to a recording chamber and continuously superfused with a control solution containing (in mM): 125 NaCl, 4.5 KCl, 23 NaHCO3, 1 MgCl2, 2.5 CaCl2, 5 glucose and 5 sucrose, at ~35 °C. In 70 mM K+ solution, NaCl was replaced equimolarly with KCl. The “normoxic” solution was bubbled with a gas mixture of 20% O2, 5% CO2, and 75% N2 (O2 tension ~145–150 mmHg). Hypoxia in the chamber was obtained by switching to a “hypoxic” solution bubbled with 5% CO2, and 95% N2 to reach an O2 tension of ~15 mmHg in the chamber.
Macroscopic inward Ca2+ (Ba2+), and outward K+ currents were recorded in dialyzed arterial myocytes. Solutions used to record whole-cell Ca2+ (Ba2+) currents contained (in mM): external solution: 140 NaCl, 10 BaCl2, 4.7 KCl, 10 HEPES, and 10 glucose, pH 7.4 and osmolality 300 mOsm/Kg; and internal solution: 130 CsCl, 10 EGTA, 10 HEPES, and 4 ATP-Mg, pH 7.2 and osmolality 285 mOsm/Kg. In Na+-free solutions extracellular Na+ was completely equimolarly replaced with impermeant cation N-methy-D-glucamine (NMDG). Solutions used to record whole-cell K+ currents contained (in mM): external solution: 140 NaCl, 2.5 KCl, 4 MgCl2, 2.5 CaCl2, 10 HEPES, and 10 glucose, pH 7.4; and internal solution: 80 K+ glutamate, 50 KCl, 1 MgCl2, 10 HEPES, 4 MgATP, and 5 EGTA, pH 7.2. The external solutions were bubbled and equilibrated with air or mixtures of N2 and air to achieve the desired O2 tension.
For wire myography all measurements were performed in a final volume of 5 mL of Krebs solution, whose composition was (in mM): 119 NaCl, 4.7 KCl, 1.17 KH2HPO4, 24 NaHCO3, 2.5 CaCl2, 1.17 MgSO4, 5.5 glucose, constantly bubbled with 95% O2 and 5% CO2 at pH 7.4. In 70 mM K+ solution, NaCl was replaced equimolarly with KCl. The “hypoxic” solution was bubbled with 5% CO2, and 95% N2.
All reagents used were added to the external (e.g., FPL or caffeine) or internal (e.g., MgATP) solutions at the indicated concentrations.
Statistical analysis
Statistical analyzes were carried out using Prism Version 8.2.1 (279) for MacOS. Normality of the data sets was tested with the Shapiro-Wilk test, D’Agostino and Pearson test, or Kolmogorov-Smirnov test. In cases, a log transformation was performed to normalize the distribution prior to parametric analysis. Data with normal distribution were described as mean ± standard error of the mean (SEM) with the number (n) of experiments indicated. For graphical representation of the data with normal distribution we used bar diagrams, with indication of the mean ± SEM, and a scatter plot of the data points superimposed. For graphical representation of non-parametric data, we used box plots with indication of median, quartiles, and whiskers (highest and lowest values). Comparison between two groups was performed as follows: For parametric data we used paired or unpaired t tests. For non-parametric data we used Mann Whitney unpaired test. All tests, parametric and non-parametric, were two-tailed. Comparison of several groups was done as follows: For parametric data we used one-way ANOVA followed by either Tukey’s, Sidak’s or Dunnett’s multiple comparisons test. For non-parametric data, we used Kruskal-Wallis test followed by Dunn’s multiple comparisons test to compare every group with each other. Statistical tests used are indicated in the figure legends. A P < 0.05 was considered statistically significant with the values indicated in the figures.
Reporting summary
Further information on research design is available in the Nature Portfolio Reporting Summary linked to this article.
Data availability
The data supporting the findings from this study are available within the manuscript and its supplementary information. Any remaining raw data will be available from the corresponding author upon reasonable request. Source data are provided with this paper.
References
Carrier, O., Walker, J. R. & Guyton, A. C. Role of oxygen in autoregulation of blood flow in isolated vessels. Am. J. Physiol. 206, 951–954 (1964).
Coburn, R. F. Oxygen tension sensors in vascular smooth muscle. Adv. Exp. Med. Biol. 78, 101–115 (1977).
Sparks, H. V. Effect Of Local Metabolic Factors On Vascular Smooth Muscle in Handbook of Physiology: The Cardiovascular System II (eds. Bohr, D. F., Somlyo, A. P. & Sparks, H. V.) 181–309 (American Physiological Society, 1980).
Renkin, E. M. Control Of Microcirculation And Blood-tissue Exchange in Handbook of Physiology: The Cardiovascular System VI (eds. Renkin, E. M. & Michel, C. C.) 627–687 (American Physiological Society, 1984).
Kontos, H. A. & Wei, E. P. Oxygen-dependent mechanisms in cerebral autoregulation. Ann. Biomed. Eng. 13, 329–334 (1985).
Jackson, W. F. Arteriolar oxygen reactivity: where is the sensor? Am. J. Physiol. 253, H1120–H1126 (1987).
Gupte, S. A. & Wolin, M. S. Oxidant and redox signaling in vascular oxygen sensing: implications for systemic and pulmonary hypertension. Antioxid. Redox Signal. 10, 1137–1152 (2008).
Jackson, W. F. Arteriolar oxygen reactivity: where is the sensor and what is the mechanism of action? J. Physiol. 594, 5055–5077 (2016).
Welsch, D. G., Jackson, W. F. & Segal, S. S. Oxygen induces electromechanical coupling in arteriolar smooth muscle cells: a role for L-type Ca2+ channels. Am. J. Physiol. 274, H2018–H2024 (1998).
Lombard, J. H., Frisbee, J. C. & Falck, R. J. Evaluation Of Cytochrome P450-4a ω-Hydroxylase And 20-hydroxyeicosatetraenoic Acid As An O2 Sensing Mechanism In The Microcirculation in Methods in Enzymology (eds. Chandan K. S. & Gregg L. S.) 140–165 (Academic Press, 2004).
Justesen, B. L. et al. Retinal arterioles have impaired reactivity to hyperoxia in type 1 diabetes. Acta Ophthalmol. 88, 453–457 (2010).
Ngo, A. T., Riemann, M., Holstein-Rathlou, N. H., Torp-Pedersen, C. & Jensen, L. J. Significance of KATP channels, L-type Ca2+ channels and CYP450-4A enzymes in oxygen sensing in mouse cremaster muscle arterioles in vivo. BMC Physiol. 13, 8 (2013).
Detar, R. Mechanism of physiological hypoxia-induced depression of vascular smooth muscle contraction. Am. J. Physiol. 238, H761–H769 (1980).
Marriott, J. F. & Marshall, J. M. Differential effects of hypoxia upon contractions evoked by potassium and noradrenaline in rabbit arteries in vitro. J. Physiol. 422, 1–13 (1990).
Frisbee, J. C., Maier, K. G., Falck, J. R. & Roman, R. J. Integration of hypoxic dilation signalling pathways for skeletal muscle resistance arteries. Am. J. Physiol. Regul. Integr. Comp. Physiol. 283, R309–R319 (2002).
Marshall, M. J. & Ray, C. J. Contribution of non-endothelium-dependent substances to exercise hyperaemia: are they O2 dependent? J. Physiol. 590, 6307–6320 (2012).
Westhoff, J. et al. Vasomotion of mice mesenteric arteries during low oxygen levels. Eur. J. Med. Res. 23, 38 (2018).
Kontos, H. A. et al. Local mechanism of CO2 action of cat pial arterioles. Stroke 9, 104–108 (1978).
Hoiland, R. L., Bain, A. R., Rieger, M. G., Bailey, D. M. & Ainsli, P. N. Hypoxemia, oxygen content, and the regulation of cerebral blood flow. Am. J. Physiol. Regul. Integr. Comp. Physiol. 310, 398–413 (2016).
Shaw, K., Bell, L. & Boyd, K. Neurovascular coupling and oxygenation are decreased in hippocampus compared to neocortex because of microvascular differences. Nat. Commun. 12, 4497 (2021).
Gauthier, K. M. Hypoxia-induced vascular smooth muscle relaxation: increased ATP-sensitive K+ efflux or decreased voltage-sensitive Ca2+ influx? Am. J. Physiol. Heart Circ. Physiol. 291, H24–H25 (2006).
Busse, R., Pohl, U., Kellner, C. & Klemm, U. Endothelial cells are involved in the vasodilatory response to hypoxia. Pflug. Arch. 397, 78–80 (1983).
Messina, E. J., Sun, D., Koller, A., Wolin, M. S. & Kaley, G. Role of endothelium-derived prostaglandins in hypoxia-elicited arteriolar dilation in rat skeletal muscle. Circ. Res. 71, 790–796 (1992).
Fredricks, K. T., Liu, Y. & Lombard, J. H. Response of extraparenchymal resistance arteries of rat skeletal muscle to reduced PO2. Am. J. Physiol. 267, H706–H715 (1994).
Longden, T. A. et al. Capillary K+-sensing initiates retrograde hyperpolarization to increase local cerebral blood flow. Nat. Neurosci. 20, 717–726 (2017).
Donovan, J. et al. Coronary artery hypoxic vasorelaxation is augmented by perivascular adipose tissue through a mechanism involving hydrogen sulphide and cystathionine-β-synthase. Acta Physiol. (Oxf.). 224, e13126 (2018).
Kellawan, J. M. et al. Differential contribution of cyclooxygenase to basal cerebral blood flow and hypoxic cerebral vasodilation. Am. J. Physiol. Regul. Integr. Comp. Physiol. 318, R468–R479 (2020).
Paganelli, F., Gaudry, M., Ruf, J. & Guieu, R. Recent advances in the role of the adenosinergic system in coronary artery disease. Cardiovasc. Res. 117, 1284–1294 (2021).
Keller, T. C. S. et al. Endothelial alpha globin is a nitrite reductase. Nat. Commun. 13, 6405 (2022).
Ellsworth, M. L. et al. Erythrocytes: oxygen sensors and modulators of vascular tone. Physiology 24, 107–116 (2009).
Premont, R. T., Singel, D. J. & Stamler, J. S. The enzymatic function of the honorary enzyme: S-nitrosylation of hemoglobin in physiology and medicine. Mol. Asp. Med. 84, 101056 (2022).
Daut, J. et al. Hypoxic dilation of coronary arteries is mediated by ATP-sensitive potassium channels. Science 247, 1341–1344 (1990).
Yuan, X. J., Tod, M. L. & Rubin, L. J. Contrasting effects of hypoxia on tension in rat pulmonary and mesenteric arteries. Am. J. Physiol. 259, H281–H289 (1990).
Leach, R. M., Robertson, T. P., Twort, C. H. & Ward, J. P.Hypoxic vasoconstriction in rat pulmonary and mesenteric arteries. Am. J. Physiol. 266, L223–L2231 (1994).
Smani, T. et al. Reduction of Ca2+ channel activity by hypoxia in human and porcine coronary myocytes. Cardiovasc. Res. 53, 97–104 (2002).
Ebeigbe, A. B. & Pickard, J. D. Responses of systemic vascular smooth muscle to hypoxia. Q. J. Exp. Physiol. Cogn. Med. Sci. 65, 273–292 (1980).
Herrera, G. M. & Walker, B. R. Involvement of L-type calcium channels in hypoxic relaxation of vascular smooth muscle. J. Vasc. Res. 35, 265–273 (1998).
Pearce, W. J., Ashwal, S., Long, D. M. & Cuevas, J. Hypoxia inhibits calcium influx in rabbit basilar and carotid arteries. Am. J. Physiol. 262, H106–H113 (1992).
Franco-Obregon, A., Ureña, J. & Lopez-Barneo, J. Oxygen-sensitive calcium channels in vascular smooth muscle cells and their possible role in hypoxic arterial relaxation. Proc. Natl Acad. Sci. USA 92, 4715–4719 (1995).
Franco-Obregon, A. & Lopez-Barneo, J. Differential oxygen sensitivity of calcium channels in rabbit smooth muscle cells of conduit and resistance pulmonary arteries. J. Physiol. 491, 511–518 (1996).
Quayle, J. M., Turner, M. R., Burrell, H. E. & Kamishima, T. Effects of hypoxia, anoxia, and metabolic inhibitors on KATP channels in rat femoral artery myocytes. Am. J. Physiol. Heart Circ. Physiol. 291, H71–H80 (2006).
Moreno-Domínguez, A., Colinas, O., Smani, T., Ureña, J. & López-Barneo, J. Acute oxygen sensing by vascular smooth muscle cells. Front. Physiol. 14, 1142354 (2023).
Ortega-Sáenz, P., Pardal, R., García-Fernández, M. & López-Barneo, J. Rotenone selectively occludes sensitivity to hypoxia in rat carotid body glomus cells. J. Physiol. 548, 789–800 (2003).
Fernández-Aguera, M. C. et al. Oxygen sensing by arterial chemoreceptors depends on mitochondrial complex I signaling. Cell. Metab. 22, 825–837 (2015).
Jiménez-Gómez, B. et al. Transgenic NADH dehydrogenase restores oxygen regulation of breathing in mitochondrial complex I-deficient mice. Nat. Commun. 14, 1172 (2023).
Kashani-Poor, N., Zwicker, K., Kerscher, S. & Brandt, U. A central functional role for the 49-kDa subunit within the catalytic core of mitochondrial complex I. J. Biol. Chem. 276, 24082–24087 (2001).
Arias-Mayenco, I. et al. Acute O2 sensing: Role of coenzyme QH2/Q ratio and mitochondrial ROS compartmentalization. Cell. Metab. 28, 145–158 (2018).
Solway, J. et al. Structure and expression of a smooth muscle cell-specific gene, SM2. 2 alpha J. Biol. Chem. 270, 13460–13469 (1995).
Li, L., Miano, J. M., Mercer, B. & Olson, E. N. (1996). Expression of the SM22 alpha promoter in transgenic mice provides evidence for distinct transcriptional regulatory programs in vascular and visceral smooth muscle cells. J. Cell. Biol. 132, 849–859 (1996).
Cabello-Rivera, D. et al. Oxygen regulation of breathing is abolished in mitochondrial complex III-deficient arterial chemoreceptors. Proc. Natl Acad. Sci. USA 119, e2202178119 (2022).
Franco-Obregón, A. & López-Barneo, J. Low PO2 inhibits Ca2+ channel activity in arterial smooth muscle cells. Am. J. Physiol. 271, H2290–H2299 (1996).
Vincent, A. E. et al. The spectrum of mitochondrial ultrastructure defects in mitochondrial myopathy. Sci. Rep. 6, 30610 (2016).
Li, L., Shen, S., Bickler, P. & Jacobson, M. P. Searching for molecular hypoxia sensors among oxygen-dependent enzymes. Elife 12, e87705 (2023).
Dart, C. & Standen, N. B. Activation of ATP-dependent K+ channels by hypoxia in smooth muscle cells isolated from the pig coronary artery. J. Physiol. 483, 29–39 (1995).
Jackson, W. F. Hypoxia does not activate ATP-sensitive K+ channels in arteriolar muscle cells. Microcirculation 7, 137–145 (2000).
Hernansanz-Agustín, P. et al. Na+ controls hypoxic signaling by the mitochondrial respiratory chain. Nature 586, 287–291 (2020).
Zheng, W., Rampe, D. & Triggle, D. J. Pharmacological, radioligand binding, and electrophysiological characteristics of FPL 64176, a novel nondihydropyridine Ca2+ channel activator, in cardiac and vascular preparations. Mol. Pharmacol. 40, 734–741 (1991).
Rampe, D. & Dage, R. C. Functional interactions between two Ca2+ channel activators, (S)-Bay K 8644 and FPL 64176, in smooth muscle. Mol. Pharmacol. 41, 599–602 (1992).
Watanabe, C., Yamamoto, H., Hirano, K., Kobayashi, S. & Kanaide, H. Mechanisms of caffeine-induced contraction and relaxation of rat aortic smooth muscle. J. Physiol. 456, 193–213 (1992).
Michelakis, E. D., Thebaud, B., Weir, E. K. & Archer, S. L. Hypoxic pulmonary vasoconstriction: redox regulation of O2-sensitive K+ channels by a mitochondrial O2-sensor in resistance artery smooth muscle cells. J. Mol. Cell. Cardiol. 37, 1119–1136 (2004).
Sommer, N. et al. Mitochondrial cytochrome redox states and respiration in acute pulmonary oxygen sensing. Eur. Respir. 36, 1056–1066 (2010).
Waypa, G. B. et al. Hypoxia triggers subcellular compartmental redox signaling in vascular smooth muscle cells. Circ. Res. 106, 526–535 (2010).
Sullivan, L. B. et al. Supporting aspartate biosynthesis is an essential function of respiration in proliferating cells. Cell 162, 552–563 (2015).
López-Barneo, J. & Simon, M. C. Cellular adaptation to oxygen deficiency beyond the nobel award. Nat. Commun. 11, 607 (2020).
Tian, H., Hammer, R. E., Matsumoto, A. M., Russell, D. W. & McKnight, S. L. The hypoxia-responsive transcription factor EPAS1 is essential for catecholamine homeostasis and protection against heart failure during embryonic development. Genes Dev. 12, 3320–3324 (1998).
Zhou, T., Chien, M. S., Kaleem, S. & Matsunami, H. Single cell transcriptome analysis of mouse carotid body glomus cells. J. Physiol. 594, 4225–4251 (2016).
Gao, L. et al. Gene expression analyses reveal metabolic specifications in acute O2-sensing chemoreceptor cells. J. Physiol. 595, 6091–6120 (2017).
Moreno-Dominguez, A. et al. Acute O2 sensing through HIF2α-dependent expression of atypical cytochrome oxidase subunits in arterial chemoreceptors. Sci. Signal. 13, eaay9452 (2020).
Colinas, O., Moreno-Domínguez, A., Ortega-Sáenz, P. & López-Barneo, J. Constitutive expression of Hif2α confers acute O2 sensitivity to carotid body glomus cells. Adv. Exp. Med. Biol. 1427, 153–162 (2023).
Bishop, T. & Ratcliffe, P. J. Genetic basis of oxygen sensing in the carotid body: HIF2α and an isoform switch in cytochrome c oxidase subunit 4. Sci. Signal. 13, eaba1302 (2020).
Semenza, G. L., Roth, P. H., Fang, H. M. & Wang, G. L. Transcriptional regulation of genes encoding glycolytic enzymes by hypoxia-inducible factor 1. J. Biol. Chem. 269, 23757–23763 (1994).
Rankin, E. B. et al. Hypoxia-inducible factor-2 (HIF-2) regulates hepatic erythropoietin in vivo. J. Clin. Invest 117, 1068–1077 (2007).
Aras, S. et al. Oxygen-dependent expression of cytochrome c oxidase subunit 4-2 gene expression is mediated by transcription factors RBPJ, CXXC5 and CHCHD2. Nucleic Acids Res. 41, 2255–2266 (2013).
Lee, C. H. et al. (2001). The mechanism of phenylephrine-mediated Ca2+ oscillations underlying tonic contraction in the rabbit inferior vena cava. J. Physiol. 534, 641–650 (2001).
Hüttemann, M. et al. Cytochrome c oxidase subunit 4 isoform 2-knockout mice show reduced enzyme activity, airway hyporeactivity, and lung pathology. FASEB J. 26, 3916–3930 (2012).
Fukuda, R. et al. HIF-1 regulates cytochrome oxidase subunits to optimize efficiency of respiration in hypoxic cells. Cell 129, 111–122 (2007).
Pajuelo-Reguera, D. et al. Cytochrome c oxidase subunit 4 isoform exchange results in modulation of oxygen affinity. Cells 9, 4432020 (2020).
Sommer, N. et al. Mitochondrial complex IV subunit 4 isoform 2 is essential for acute pulmonary oxygen sensing. Circ. Res. 121, 424–438 (2017).
Prange-Barczynska, M. et al. Hif-2α programmes oxygen chemosensitivity in chromaffin cells. Preprint at bioRxiv, https://doi.org/10.1101/2023.07.14.548982 (2023).
Weir, E. K., Lopez-Barneo, J., Buckler, K. J. & Archer, S. L. (2005). Acute oxygen-sensing mechanisms. N. Engl. J. Med. 353, 2042–2055 (2005).
Scortegagna, M. et al. Multiple organ pathology, metabolic abnormalities and impaired homeostasis of reactive oxygen species in Epas1−/− mice. Nat. Gen. 35, 331–340 (2003).
Gruber, M. et al. Acute postnatal ablation of Hif-2α results in anemia. Proc. Natl Acad. Sci. USA 104, 2301–2306 (2007).
Chiamvimonvat, N. et al. Functional consequences of sulfhydryl modification in the pore-forming subunits of cardiovascular Ca2+ and Na+ channels. Circ. Res. 76, 325–334 (1995).
Fearon, I. M. et al. Modulation of recombinant human cardiac L-type Ca2+ channels α1C subunits by redox reagents and hypoxia. J. Physiol. 514, 629–637 (1999).
Muralidharan, P., Szappanos, H. C., Ingley, E. & Hool, L. Evidence for redox sensing by a human cardiac calcium channel. Sci. Rep. 6, 19067 (2016).
Kilfoil, P. J., Tipparaju, S. M., Barski, O. A. & Bhatnagar, A. Regulation of ion channels by pyridine nucleotides. Circ. Res. 112, 721–741 (2013).
Jackson, W. F. Kv channels and the regulation of vascular smooth muscle tone. Microcirculation 25, https://doi.org/10.1111/micc.12421 (2018).
Raph, S. M., Dwenger, M. M., Hu, X. & Nystoriak, M. A. Basal NAD(H) redox state permits hydrogen peroxide-induced mesenteric artery dilatation. J. Physiol. 601, 2621–2634 (2023).
Yang, Q. et al. Clustering of L-type calcium channels by Shank3. J. Neurochem. 167, 16–37 (2023).
Olson, K. R. A case for hydrogen sulfide metabolism as an oxygen sensing mechanism. Antioxid. (Basel) 10, 1650 (2021).
Segal, S. S. Regulation of blood flow in the microcirculation. Microcirculation 12, 33–45 (2005).
Ryan, H. E. et al. Hypoxia-inducible factor-1α is a positive factor in solid tumor growth. Cancer Res. 60, 4010–4015 (2000).
Hayashi, S. & McMahon, A. P. Efficient recombination in diverse tissues by a tamoxifen-inducible form of Cre: A tool for temporally regulated gene activation/inactivation in the mouse. Dev. Biol. 244, 305–318 (2002).
Ruzankina, Y. et al. Deletion of the developmentally essential gene ATR in adult mice leads to age-related phenotypes and stem cell loss. Cell Stem Cell 1, 113–126 (2007).
Acknowledgements
This research was supported by the Spanish Ministries of Science and Innovation and Health (Grants SAF2016-74990-R, JL-B. and PID2019-106410RB-I00, J.L.-B. funded by MCIN/AEI/10.13039/501100011033, and the European Research Council (ERC Advanced Grant PRJ201502629, J.L.-B.). We thank Dr. Juan Luis Ribas (CITIUS, University of Seville) for help with electron microscopy. We also thank the staff of IBiS and “Centro de Producción y Experimentación Animal Oscar Pintado” for technical assistance.
Author information
Authors and Affiliations
Contributions
A.M.-D., O.C., I.A.-M., J.M.C. J.L.L.-O., A.P. and J.L.-B. performed the experiments and/or analyzed the data. N.C., N.W. and N.S. provided essential material for the experiments. All authors contributed to the design of the study and to the discussion of the data. A.M.-D. and J.L.-B generated the draft of the paper. J.L.-B. coordinated the project and the writing of the paper.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval
This study was performed following the recommendations set out in the Global Code of Conduct for Research in Resource-Poor Settings.
Peer review
Peer review information
Nature Communications thanks the anonymous reviewers for their contribution to the peer review of this work. A peer review file is available.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Source data
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/.
About this article
Cite this article
Moreno-Domínguez, A., Colinas, O., Arias-Mayenco, I. et al. Hif1α-dependent mitochondrial acute O2 sensing and signaling to myocyte Ca2+ channels mediate arterial hypoxic vasodilation. Nat Commun 15, 6649 (2024). https://doi.org/10.1038/s41467-024-51023-3
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41467-024-51023-3
- Springer Nature Limited