Abstract
The β1 adrenergic receptor (β1AR) is recognized as a classical Gαs-coupled receptor. Agonist binding not only initiates G protein-mediated signaling but also signaling through the multifunctional adapter protein β-arrestin. Some βAR ligands, such as carvedilol, stimulate βAR signaling preferentially through β-arrestin, a concept known as β-arrestin-biased agonism. Here, we identify a signaling mechanism, unlike that previously known for any Gαs-coupled receptor, whereby carvedilol induces the transition of the β1AR from a classical Gαs-coupled receptor to a Gαi-coupled receptor stabilizing a distinct receptor conformation to initiate β-arrestin-mediated signaling. Recruitment of Gαi is not induced by any other βAR ligand screened, nor is it required for β-arrestin-bias activated by the β2AR subtype of the βAR family. Our findings demonstrate a previously unrecognized role for Gαi in β1AR signaling and suggest that the concept of β-arrestin-bias may need to be refined to incorporate the selective bias of receptors towards distinct G protein subtypes.
Similar content being viewed by others
Introduction
G protein-coupled receptors (GPCRs) represent the largest and the most versatile family of cell surface receptors1. Members of this receptor family translate diverse extracellular cues to intracellular responses, and are commonly targeted for medicinal therapeutics2, 3. One of the most commonly used therapeutic agents in medicine are ligands that target β adrenergic receptors (βARs) because they regulate many important physiological processes involved in the regulation of cardiovascular and pulmonary function4.
GPCRs selectively couple to different heterotrimeric G protein complexes (Gαβγ) that are classified into four families based on their α-subunits: Gαstimulatory (Gαs), Gαinhibitory/olfactory (Gαi/o), Gαq/11, and Gα12/13 5. Among the different G protein subtypes, βARs primarily transmit signals through Gαs 6. In the classical paradigm of βAR signaling, receptors exist in two distinct conformational states: active or inactive. Agonist binding stabilizes an active βAR conformation that promotes coupling with heterotrimeric G proteins, triggering guanine nucleotide exchange of Gαs and its dissociation from the Gβγ subunits, leading to the activation of adenylyl cyclase and triggering second messenger cyclic AMP signaling7, 8. Subsequent to agonist binding, activated βARs are phosphorylated by G protein-coupled receptor kinases (GRKs) leading to recruitment of the multifunctional β-arrestins (β-arrestin1 and β-arrestin2) and inhibition of further G protein coupling, a process termed desensitization8. It is now appreciated that β-arrestins also act as signal transducers in their own right7 to stimulate a distinct array of signaling and cellular responses, such as transactivation of the epidermal growth factor receptor (EGFR)9, 10, induction of extracellular signal-regulated kinase (ERK)10,11,12,13, and activation of Ca2+/calmodulin kinase II (CaMKII)14. Current data suggest a much greater complexity of GPCR signaling than the two-state (active or inactive) model whereby multiple receptor conformations can exist, each with a different affinity for its transducer, resulting in the activation of distinct cellular signaling pathways15,16,17. Whereas balanced ligands, such as isoproterenol, stabilize βAR conformations signal with equal efficacy through G proteins and β-arrestins, some ligands stabilize conformations that selectively recruit only one of the transducers to stimulate a specific subset of cellular signals, a process termed “biased agonism”18, 19. As biased ligands may be capable of selectively activating beneficial signaling while simultaneously blocking untoward receptor activated pathways20, understanding mechanisms of biased agonism can have important implications for drug discovery targeting GPCRs.
The β-blocker carvedilol is a β-arrestin-biased βAR ligand that preferentially activates β-arrestin-mediated pathways while having inverse agonism towards Gαs signaling7, 10, 19, 21. To date, the prevailing mechanistic concept of β-arrestin-bias for the Gαs-coupled β1AR is ligand-stimulated activation of β-arrestin in the absence of G protein coupling. However, recently it has been demonstrated for the angiotensin II type 1 receptor that the weak β-arrestin-biased agonist, [1Sar4Ile8Ile]-angiotensin II, is capable of activating both Gαq and Gαi 22, indicating a possible role of G proteins in β-arrestin-mediated signaling. Moreover, recent biophysical work suggests that both G protein and β-arrestin can simultaneously interact with an activated GPCR to form super complexes23, raising the possibility that association of β-arrestin with the receptor may not preclude interaction with a G protein. Here, we set out to test whether G protein coupling is a critical component of β-arrestin-biased βAR signaling. Our findings show that carvedilol, unique among other βAR agonists or antagonists tested, selectively promotes the recruitment of Gαi to β1ARs to initiate β-arrestin-biased signaling. These data underscore the complexity of β-arrestin-biased agonism and have important implications for identifying new therapeutic agents to selectively target β-arrestin-biased signaling.
Results
Gαi is required for carvedilol-induced β1AR-mediated ERK
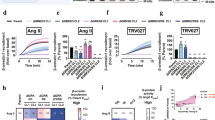
Previous studies have demonstrated that carvedilol induces βAR-mediated ERK phosphorylation in a Gαs-independent, β-arrestin-dependent manner10, 21. To determine whether Gαi is required for carvedilol-stimulated βAR signaling, we tested the effect of the Gαi inhibitor pertussis toxin (PTX) on carvedilol-stimulated ERK phosphorylation in HEK293 cells stably expressing FLAG-tagged β1AR or β2AR. PTX catalyzes the ADP-ribosylation of Gαi and prevents Gαi coupling to ligand bound receptors. In β1AR stable cells, carvedilol dose dependently increased ERK phosphorylation, which was significantly diminished by pretreatment with the Gαi inhibitor PTX (Fig. 1a, Supplementary Fig. 1a). In contrast, PTX had no effect on the carvedilol-induced β2AR-mediated ERK phosphorylation (Fig. 1a, Supplementary Fig. 1a). These observations suggest that Gαi is needed for carvedilol-induced β1AR, but not β2AR signaling.
Gαi is required for the carvedilol-induced β1AR-mediated ERK phosphorylation both in vitro and in vivo. a Effect of PTX on carvedilol-induced βAR-mediated ERK phosphorylation in HEK293 cells. HEK293 cells stably expressing FLAG-tagged β1ARs or β2ARs were pretreated with vehicle or 200 ng per ml PTX for 16 h, then stimulated with indicated concentration of carvedilol for 5 min. Carvedilol induced ERK phosphorylation in both β1AR or β2AR stable cells in dose-dependent manner. The response in β1AR stable cells was blocked by PTX, whereas that in β2AR stable cells was PTX insensitive. b Effect of Gαi knockout on βAR-mediated ERK phosphorylation in HEK293 cells. The Gαi expression in β1AR or β2AR stable cells was depleted with CRISPR–Cas9 gene editing. Compared with wild-type β1AR stable cells, the carvedilol-induced ERK phosphorylation in Gαi knockout β1AR stable cells was diminished. In comparison, the response in β2AR stable cells was not affected. c Effect of PTX on carvedilol-stimulated ERK phosphorylation in Langendorff perfused hearts from β2AR knockout mice or β1AR knockout mice. Mice were pretreated with vehicle or 25 μg per kg PTX through intraperitoneal injection. 48 h after injection, mice hearts were excised and perfused with vehicle or 10 μM carvedilol for 10 min. PTX diminished the carvedilol-induced ERK phosphorylation in hearts from β2AR knockout mice, but not β1AR knockout mice. Data represent the mean ± SEM for n independent experiments (a, b) or n animals (c) as marked on the figure. Statistical significance vs. control was assessed using two-way ANOVA (a, b) or one-way ANOVA (c) with Bonferroni correction. NS no stimulation; Carv carvedilol; Iso isoproterenol; p-ERK phosphorylated ERK; t-ERK total ERK; WT wild type; KO knockout
To further delineate the role of Gαi in carvedilol-induced βAR signaling, we measured the level of ERK activation in β1AR or β2AR stable cells after removing Gαi using CRISPR/Cas9 gene editing. All three subtypes of Gαi (Gαi1, Gαi2, and Gαi3) were depleted with their specifically targeted guide RNAs (Supplementary Fig. 1b). Gαi depletion markedly blocked carvedilol-induced ERK phosphorylation in β1AR stable cells, while it had no effect in β2AR stable cells (Fig. 1b). The absence of Gαi was considerably more robust in abrogating carvedilol-stimulated ERK phosphorylation compared to that observed with PTX treatment (Fig. 1a).
We then determined if a similar signaling mechanism is involved in heart tissue by measuring ERK phosphorylation in Langendorff perfused mouse hearts following carvedilol stimulation. To study the specific effect of carvedilol on the β1AR, we used previously generated β2AR knockout mice24. Carvedilol perfusion robustly stimulated ERK phosphorylation in hearts of β2AR knockout mice, which was entirely abrogated in hearts of PTX-pretreated mice (Fig. 1c). In contrast, in β1AR knockout mice25 while carvedilol robustly induced ERK phosphorylation by activating the β2AR, PTX pretreatment was unable to block ERK activation (Fig. 1c). These data are consistent with our in vitro data and indicate a previously unrecognized, βAR subtype specific, requirement for Gαi in carvedilol-induced β1AR signaling.
Carvedilol-induced β1AR conformational change requires Gαi
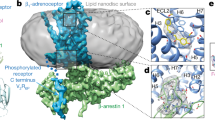
Different ligands for the same receptor stabilize unique conformational states promoting coupling to selective signal transducers and activation of distinct downstream signaling pathways7, 20. Since we showed that Gαi is required for carvedilol-induced β1AR signaling, we tested whether it allosterically stabilizes a unique carvedilol-bound β1AR conformation. We utilized a fluorescence resonance energy transfer (FRET)-based β1AR conformational sensor in which Cerulean (Cer) and YFP are inserted in the C-terminus and third intracellular loop of the receptor, respectively (Fig. 2a)26. Agonist-induced β1AR activation is represented by the loss of FRET, i.e., decrease of YFP/Cer ratio26. To test whether Gαi stabilizes a carvedilol-induced β1AR conformation, HEK293 cells stably expressing the β1AR FRET sensor were pretreated with vehicle or PTX, then stimulated with the balanced agonist isoproterenol or the β-arrestin-biased agonist carvedilol while monitoring the FRET ratio in real time. We found that compared to isoproterenol which caused a decrease in the FRET ratio, carvedilol induced a directional opposite response to the FRET signal, whereas the β1AR antagonist metoprolol showed no effect (Fig. 2b). Importantly, pretreatment with PTX significantly diminished the carvedilol-induced FRET ratio without any effect on the isoproterenol stimulated FRET-based receptor biosensor (Fig. 2c). Lastly, PTX alone did not affect the FRET ratio (Supplementary Fig. 2). These data demonstrate the β1AR adopts a distinct conformational state when bound to isoproterenol compared to carvedilol and that Gαi is needed to stabilize the carvedilol-bound β1AR conformation.
Gαi is required for carvedilol-induced β1AR conformation change. a In the FRET-based β1AR conformation sensor, YFP and Cerulean (Cer) are inserted in the third intracellular loop and the C-tail of β1AR respectively. b Ligand-induced changes of the FRET ratio in HEK293 cells stably expressing β1AR FRET sensor. The stable cells were stimulated with 100 μM carvedilol, 10 μM isoproterenol, 10 μM or 100 μM β1AR antagonist metoprolol, while FRET was monitored in real-time as the emission ratio of YFP to Cer. Carvedilol stimulation increased the FRET ratio, while isoproterenol decreased it, demonstrating the distinct β1AR conformations induced by these two ligands. Metoprolol had no effect on the FRET ratio. c Effect of PTX on ligand-induced FRET ratio change. Cells were pretreated with vehicle or 200 ng per ml PTX for 16 h before ligand stimulation. PTX blocked carvedilol-induced change, while having no effect on the isoproterenol response, suggesting that Gαi is required to stabilize the carvedilol-induced β1AR conformation. Data represent the mean ± SEM for n independent experiments as marked on the figure. Statistical significance vs. unstimulated cells was assessed using one-way ANOVA with Bonferroni correction (b); statistical significance between PTX-pretreated and non-pretreated cells was assessed using two-way ANOVA with Bonferroni correction (c, left panel), or two-tailed paired Student’s t-test (c, right panel)
Carvedilol selectively promotes Gαi recruitment to β1ARs
To determine the mechanism of how Gαi is involved in carvedilol-induced β1AR signaling, we measured ligand-promoted Gαi recruitment to βARs with an in situ proximity ligation assay (PLA), a confocal-microscopy based assay that allows direct visualization and quantification of protein–protein interactions. Using HEK293 cells stably expressing β1ARs, we show an over twofold increase in the PLA signal after carvedilol treatment, indicating recruitment of Gαi to the β1AR (Fig. 3a). In contrast, carvedilol had no effect on the recruitment of Gαi to β2ARs, but Gαi was robustly recruited by isoproterenol consistent with the known process of G protein switching for β2ARs27 (Fig. 3a). Importantly, pretreatment with the βAR antagonist propranolol blocked the carvedilol-induced Gαi recruitment to β1ARs (Fig. 3b), indicating the recruitment is dependent on ligand interaction with the β1AR orthosteric binding pocket. To further demonstrate recruitment of Gαi to carvedilol-stimulated β1AR, we also performed co-immunoprecipitation experiments. Carvedilol stimulation increased the amount of Gαi bound to β1ARs in a dose-dependent manner, whereas it resulted in a decrease of Gαi that could be co-immunoprecipitated with β2ARs (Fig. 3c, Supplementary Fig. 3a). As a control for the effect of detergent on protein interaction during the co-immunoprecipitation, experiments were also performed with 1% n-Dodecyl β-D-maltoside (DDM) lysis buffer and showed similar results (Supplementary Fig. 3b). The amount of Gαi bound to β2ARs was increased by the balanced agonist isoproterenol (Fig. 3c), as we observed with the PLA experiments and again consistent with the previously identified process of Gαs/Gαi switching27.
Carvedilol promotes Gαi recruitment and activation in β1AR stable cells, but not in β2AR stable cells. HEK293 cells stably expressing FLAG-tagged β1ARs or β2ARs were stimulated with 10 μM carvedilol or 10 μM isoproterenol for 5 min. a In proximity ligation assay (PLA), cells were immuno-stained with Gαi antibody raised in mouse and β1AR (or β2AR) antibody raised in rabbit. The red PLA signal represents the protein interactions of Gαi and β1AR (or β2AR). The area in yellow squares are enlarged for better view. Carvedilol promoted Gαi recruitment to β1ARs, but not to β2ARs. Scale bar = 20 μm. b β1AR stable cells were pretreated with vehicle or 10 μM propranolol for 30 min. The βAR antagonist propranolol blocked the carvedilol response, suggesting that β1AR–Gαi coupling is induced by the binding of carvedilol to the β1AR orthosteric binding pocket. Scale bar = 20 μm. c The effect of carvedilol and isoproterenol on Gαi recruitment was confirmed with co-immunoprecipitation assays. FLAG-tagged β1ARs or β2ARs were immunoprecipitated with anti-FLAG M2 beads, and Gαi3 was detected with its specific antibody by western blot. d Carvedilol specifically activated Gαi in β1AR stable cells. Cells were transfected with Gαi2. 48 h after transfection, cells were treated with 10 μM carvedilol for 5 min or 30 min, or 10 μM isoproterenol for 5 min. Activated Gαi was immunoprecipitated with an antibody specifically recognizing the active form of Gαi, and immunoblotted with an Gαi antibody. In the middle lane marked as actGαi, cells were transfected with constitutively active Gαi2, serving as positive control. Carvedilol stimulation activated Gαi in β1AR stable cells, but not in β2AR stable cells. Data represent the mean ± SEM for n independent experiments as marked on the figure. Statistical significance vs. unstimulated cells (NS) was assessed using one-way ANOVA with Bonferroni correction
We next determined whether carvedilol could induce Gαi protein activation using an antibody that specifically recognizes the active GTP-bound Gαi. Carvedilol stimulation promoted the activation of Gαi in β1AR stable cells, but not in β2AR stable cells (Fig. 3d), which was blocked by PTX (Supplementary Fig. 3c).
To determine whether Gαi recruitment is specifically stimulated by carvedilol, we tested a number of βAR agonists and antagonists with PLA (Fig. 4a) and co-immunoprecipitation (Fig. 4b, Supplementary Fig. 4). Remarkably, no other ligand tested induced Gαi recruitment to β1ARs, suggesting that this process may be a unique property of the β-arrestin-biased ligand carvedilol.
A number of βAR agonists or antagonists tested do not have significant effect on Gαi recruitment. a β1AR stable cells were stimulated with vehicle or 10 μM indicated ligands for 5 min. Interaction of β1AR and Gαi were detected by PLA. Scale bar = 20 μm. b β1AR or β2AR stable cells were stimulated with ligands at indicated concentration for 5 min. Gαi recruitment was detected by co-immunoprecipitation. Both assays suggested that none of the ligands tested had similar effect of carvedilol on Gαi recruitment. Data represent the mean ± SEM for n independent experiments as marked on the figure. Statistical significance vs. unstimulated cells was assessed using one-way ANOVA with Bonferroni correction
Collectively, these data support a concept that carvedilol selectively promotes the recruitment and activation of Gαi to the β1AR subtype triggering β-arrestin-mediated signaling.
Signaling dependence on both Gαi and β-arrestins
Previous studies have shown that carvedilol stimulation of β1ARs promotes the internalization and activation of EGFRs, which in turn activates downstream signaling such as ERK phosphorylation10. To dissect the mechanism of carvedilol-induced Gαi-dependent signaling, we tested the effect of PTX on β1AR-mediated EGFR internalization. We transfected HEK293 cells stably expressing β1ARs with GFP-tagged EGFR, and monitored internalization by confocal microscopy. When stimulated with isoproterenol or carvedilol, GFP-EGFR redistributed from the plasma membrane into endosomes, similar to that observed after EGF treatment (Fig. 5a). Pretreatment with PTX significantly blocked the carvedilol-induced EGFR internalization, while without any effect on the isoproterenol response, indicating a requirement for Gαi for carvedilol-induced response (Fig. 5a).
Both Gαi and β-arrestins are required for carvedilol-induced β1AR-mediated EGFR internalization. a The effect of PTX on ligand-stimulated EGFR internalization. β1AR stable cells with transient transfection of GFP-EGFR were pretreated with vehicle or 200 ng per ml PTX for 16 h. Then the cells were stimulated with 10 μM carvedilol, 10 μM isoproterenol or 10 ng per ml EGF for 5 min. Both carvedilol and isoproterenol promoted EGFR internalization, but only the carvedilol-induced response was PTX sensitive. Scale bar = 10 μm. b Either PTX pretreatment or β-arrestins knockdown blocked carvedilol-induced EGFR internalization. β1AR stable cells were transfected with GFP-EGFR together with scrambled control siRNA or β-arrestin1/2 siRNA. 48 h after transfection, cells were pretreated with vehicle or 200 ng per ml PTX for 16 h before stimulation. Scale bar = 10 μm. c Carvedilol-induced EGFR internalization was abrogated in β-arrestins or Gαi knockout cells. Wild type, β-arrestin1/2 knockout or Gαi knockout cells were transfected with CFP-tagged β1ARs. Cells were stimulated with 10 μM carvedilol, 10 μM isoproterenol or 10 ng per ml EGF for 5 min. The EGFR level on cell surface was assessed by flow cytometry. Both carvedilol- and isoproterenol-induced EGFR internalization were impaired in the β-arrestin knockout cells, whereas only the carvedilol-induced response was blocked in the Gαi knockout cells. Data represent the mean ± SEM for n independent experiments as marked on the figure. Statistical significance was assessed using two-tailed paired Student’s t-test (a) or one-way ANOVA with Bonferroni correction (b, c)
Consistent with previous study showing that carvedilol-induced β1AR-mediated EGFR transactivation is β-arrestin-dependent10, siRNA knockdown of β-arrestin1 and β-arrestin2 abrogated both isoproterenol- and carvedilol-induced EGFR internalization (Fig. 5b, Supplementary Fig. 5a). While transactivation triggered EGFR internalization induced by both ligands are β-arrestin dependent, the precise molecular mechanism appears to have distinct features. Whereas the carvedilol-induced response requires both Gαi and β-arrestin, the isoproterenol-induced response is PTX insensitive.
To more robustly determine the role of Gαi and β-arrestin in carvedilol-stimulated EGFR transactivation, we generated β-arrestin or Gαi deficient cells using CRISPR–Cas9 gene editing (Supplementary Fig. 5b). The wild type, Gαi knockout or β-arrestin1/2 knockout cells were transfected with CFP-tagged β1AR. After ligand stimulation, the level of cell surface EGFRs was analyzed by flow cytometry (Fig. 5c). In wild-type cells, EGFRs were internalized following the treatment with EGF, isoproterenol or carvedilol. The depletion of Gαi blocked carvedilol-induced EGFR internalization, whereas absence of Gαi had no effect on EGF- or isoproterenol-induced responses. In contrast, β-arrestin1/2 knockout cells showed impaired EGFR internalization in response to both isoproterenol and carvedilol. Taken together, these results suggest that the carvedilol-induced EGFR internalization are dependent on both Gαi and β-arrestins.
Consistent with our observation for EGFR internalization, carvedilol-induced ERK phosphorylation required both Gαi and β-arrestins (Fig. 6a, b). Either Gαi inhibition by PTX or β-arrestin knockdown with siRNA diminished carvedilol-induced ERK phosphorylation (Fig. 6a). Moreover, in HEK293 cells transfected with FLAG-β1ARs but depleted of either Gαi or β-arrestin, carvedilol stimulated ERK activation was completely abrogated (Fig. 6b). Interestingly, removing either β-arrestin1 or β-arrestin2 prevented carvedilol-stimulated ERK phosphorylation, suggesting that both isoforms are required for carvedilol-stimulated signaling (Fig. 6b).
Carvedilol-induced β1AR-mediated ERK phosphorylation is dependent on both Gαi and β-arrestins. a The effect of PTX and β-arrestin knockdown on carvedilol-stimulated ERK phosphorylation. β1AR stable cells with transfection of control siRNA or β-arrestin1/2 siRNA were pretreated with vehicle or PTX, then simulated with 10 μM carvedilol for 5 min or 30 min. Carvedilol-stimulated ERK phosphorylation was diminished by either PTX pretreatment or β-arrestins siRNA, suggesting the requirement of Gαi and β-arrestins for this signaling. b The β1AR-mediated ERK phosphorylation in β-arrestin or Gαi knockout cells. Wild type, β-arrestin knockout or Gαi knockout HEK293 cells were transfected with FLAG-tagged β1ARs. Cells were stimulated with 10 μM carvedilol for 5 or 30 min, 10 μM isoproterenol or 10 ng per ml EGF for 5 min. The depletion of either β-arrestins or Gαi impaired carvedilol-induced ERK phosphorylation. Data represent the mean ± SEM for n independent experiments as marked on the figure. Statistical significance vs. unstimulated cells was assessed using one-way ANOVA with Bonferroni correction
When βARs are stimulated by the balanced agonist isoproterenol, protein kinase A (PKA) activated by Gαs-dependent cyclic AMP phosphorylates the receptor leading to a switch of β2AR G protein coupling from Gαs to Gαi. The now Gαi coupled β2AR acts as a negative regulator of Gαs signaling and activates ERK signaling via dissociated Gβγ subunits from heterotrimeric Gαi 27,28,29. Here, we sought to determine if Gβγ subunits are required for carvedilol-stimulated Gαi-dependent ERK phosphorylation. Gβγ inhibition was achieved by transfection of T8-βARKct, a chimeric molecule consisting of two components: the C-terminus of the β adrenergic receptor kinase (βARKct) that competitively binds Gβγ, therefore acting as an inhibitor of Gβγ30; and the extracellular and transmembrane domain of CD8 receptor, which anchors the chimeric protein to the plasma membrane and potentiates its inhibitory effect31. The Gβγ blockade efficiency of T8-βARKct was confirmed by testing its effect on lysophosphatidic acid (LPA)-induced phosphorylation of cyclic AMP-responsive element-binding protein (CREB) (Fig. 7a). We show that the inhibition of Gβγ by T8-βARKct did not affect the carvedilol-induced ERK activation (Fig. 7b). This suggests that unlike isoproterenol stimulated Gαi-signaling achieved by G protein switching, carvedilol-induced Gαi-dependent β1AR signaling does not require Gβγ.
Gβγ subunits are not required for carvedilol-induced β1AR-mediated ERK phosphorylation. a Validation of the Gβγ inhibition by T8-βARKct. HEK293 cells with or without transient transfection of T8-βARKct were stimulated with 10 μM LPA for 5 min. T8-βARKct diminished the LPA-induced CREB phosphorylation, a known Gβγ-dependent process, confirming the inhibition of Gβγ subunits by T8-βARKct. b The Gβγ subunits are not required for carvedilol-induced β1AR-mediated ERK phosphorylation. β1AR stable cells with or without T8-βARKct transfection was pretreated with vehicle or 200 ng per ml PTX for 16 h. The cells were then stimulated with 10 μM carvedilol or 10 μM isoproterenol for 5 min. T8-βARKct did not have significant effect on ERK phosphorylation, suggesting that Gβγ subunits were not required. Data represent the mean ± SEM for n independent experiments as marked on the figure. Statistical significance vs. unstimulated cells was assessed using one-way ANOVA with Bonferroni correction
Collectively, these data demonstrate that both Gαi and β-arrestins are required for carvedilol-induced β1AR signaling. Notably, either PTX pretreatment or β-arrestin knockdown was able to significantly block the carvedilol-induced β1AR-mediated EGFR internalization and ERK phosphorylation, and these responses were completely abrogated when either Gαi or β-arrestin was depleted by gene editing. Taken together these data suggest that Gαi and β-arrestins are likely involved in the same signaling cascade, rather than acting in parallel pathways downstream of β1AR.
Phosphorylation of β1AR is not required for Gαi recruitment
GRK-mediated receptor phosphorylation plays a critical role in β-arrestin-dependent signaling of βARs32. When β1ARs are stimulated by balanced agonists, such as isoproterenol or dobutamine, GRK-mediated β1AR phosphorylation of the carboxyl-terminal tail occurs and is required for agonist mediated β-arrestin recruitment9, 33. For the β2AR, a similar process has been show to occur whereby stimulation with the β-arrestin-biased agonist carvedilol promotes β2AR phosphorylation at specific GRK sensitive amino acid residues 355 and 356 of the c-terminal tail21, 32. Here, we sought to determine whether GRK-mediated phosphorylation of the β1AR is a necessary step in the carvedilol-induced Gαi recruitment to the receptor. To address this question, we used a mutant β1AR that lacks the putative GRK phosphorylation sites within the receptor carboxyl-terminal tail (GRK-β1AR) and therefore unable to be phosphorylated by GRKs9, 33. We show that carvedilol stimulation increased Gαi recruitment to a similar extent between wild type and GRK-β1ARs, as assessed by co-immunoprecipitation (Fig. 8a) and suggests that GRK-mediated β1AR phosphorylation is not required for carvedilol-induced Gαi recruitment to the β1AR.
Neither PKA-mediated nor GRK-mediated β1AR phosphorylation is required for carvedilol-induced Gαi recruitment. C-tail of β1AR is required but not sufficient for Gαi recruitment. a HEK293 cells were transfected with FLAG-tagged wild-type, PKA- or GRK- β1ARs. Carvedilol promoted Gαi recruitment to mutant β1ARs lacking the putative PKA- or GRK-mediated phosphorylation sites, to a similar extent as to the wild-type β1ARs. b HEK293 cells stably expressing FLAG-tagged β1ARs were pretreated with vehicle or 10 μM H89 for 30 min. The PKA inhibitor H89 did not have a significant effect on carvedilol-induced β1AR–Gαi coupling. c HEK293 cells were transfected with FLAG-tagged β1AR, β2AR or chimeric βAR constructs in which the receptor C-tails were exchanged between the two receptor subtypes. Carvedilol did not promote Gαi recruitment to the β1AR with C-tail from β2AR. On the other hand, the β1AR C-tail did not make β2AR capable of recruiting Gαi with carvedilol stimulation. Data represent the mean ± SEM for n independent experiments as marked on the figure. Statistical significance vs. unstimulated cells was assessed using one-way ANOVA with Bonferroni correction
βARs can switch coupling from Gαs to Gαi when stimulated with a balanced agonist27, 29. In the Gαs-Gαi switching model, agonist stimulated β2AR–Gαi coupling is dependent on PKA-mediated receptor phosphorylation27, 29. To determine whether a similar mechanism is involved in the carvedilol-induced Gαi recruitment to β1ARs, we used a β1AR mutant lacking the putative PKA phosphorylation sites (PKA-β1AR) or the PKA inhibitor H89. In our experiments, carvedilol stimulation promotes the Gαi recruitment to PKA-β1ARs, similar as to wild-type receptors (Fig. 8a), whereas PKA inhibition with H89 did not have a significant effect (Fig. 8b).
Taken together, these data suggest that neither GRK- nor PKA-mediated receptor phosphorylation is required for carvedilol-induced Gαi recruitment to β1ARs.
β1AR C-tail is required but not sufficient for Gαi coupling
Since the C-terminus of the βARs play vital roles in recruiting signal effectors and regulating downstream signaling34, we postulated that specific amino acid residues within the β1AR C-tail are critical for receptor subtype specificity of Gαi recruitment. To test this hypothesis, we transfected HEK293 cells with βAR chimera mutants in which the C-tail of β1ARs was exchanged with that of β2ARs14, and assessed Gαi recruitment to chimera βARs with co-immunoprecipitation. Carvedilol stimulation promoted the recruitment of Gαi to the wild-type β1ARs, but was abrogated when the β1AR contained the C-tail from the β2AR (β1/2AR) (Fig. 8c). In contrast, the effect of carvedilol on Gαi recruitment to the β2AR with the β1AR C-tail (β2/1AR) was similar to that of wild-type β2ARs. These data suggest that the C-tail of the β1AR is required for Gαi recruitment, but alone is insufficient for this process to occur and is consistent with the crystal structure of the β2AR and G protein complex showing multiple receptor-G protein contact points35.
Discussion
In this study, we provide new insight into the molecular mechanism of biased agonism at the β1AR. Carvedilol, a ligand classically known as a βAR antagonist, activates β-arrestin signaling by switching the uniquely Gαs-coupled β1AR to a Gαi-coupled receptor. We show that carvedilol is unique among a number of agonists and antagonists tested to promote the recruitment and activation of Gαi to β1ARs. The recruited Gαi in turn stabilizes a carvedilol-bound β1AR conformation that is required for β-arrestin-biased β1AR signaling as measured by EGFR internalization and ERK phosphorylation. These results indicate that the previously defined G protein bias vs. β-arrestin-bias may be attributed to ligand-induced selective coupling of receptors to specific G protein subtypes, i.e., G protein subtype bias. In our conceptual model for β1AR biased signaling, we speculate that binding of carvedilol to the β1AR stabilizes a unique receptor conformation that recruits and activates Gαi to promote β-arrestin-mediated signaling (Fig. 9). While carvedilol is also known to stimulate β2AR signaling, Gαi recruitment was not required for β2AR-mediated β-arrestin-biased signaling and suggests that different mechanisms for bias may be operative between βAR subtypes.
Schematic model of the carvedilol-induced Gαi-β-arrestin-biased signaling of β1ARs. Binding of carvedilol to the orthosteric site of the β1AR stablizes a distinct intermediate conformation that then promotes the recruitment of Gαi. The carvedilol- and Gαi-bound receptor in turn stabilizes a unique β1AR conformation that mediates β-arrestin-biased signaling
In the classical view of GPCR signaling, agonist stabilization of specific active conformational states promotes coupling of heterotrimeric G proteins and stimulation of downstream signaling36. Receptor signaling is then terminated by a process involving receptor phosphorylation, β-arrestin recruitment and receptor internalization. However, recent studies suggest that the classical “on–off” (active and inactive) model is oversimplified20, as GPCRs transmit signaling through multiple transducers to regulate diverse arrays of pathways. First, some GPCRs can couple to multiple G proteins. For example, the isoproterenol-activated β2AR switches coupling from Gαs to Gαi 27. In this study, we show that carvedilol switches the classical Gαs-coupled receptor β1AR to a Gαi-coupled receptor. However, in contrast to the Gαs-Gαi switching of the β2AR, the carvedilol-induced β1AR–Gαi coupling does not involve Gαs activation and PKA-mediated receptor phosphorylation. The carvedilol-induced β1AR–Gαi signaling is also different from the actions of classical Gαi-coupled receptors such as the muscarinic M2 receptor and the α2 adrenergic receptor37, as its activation of ERK is not mediated through Gβγ subunits. Second, in addition to their role as signal terminators for G protein signaling, β-arrestins can act as signal transducers in their own right. Current conceptual models support the idea that ligands may differentially stabilize distinct receptor conformations that recruit divergent portfolio of signaling transducers and effector proteins to active a select suite of cellular signaling pathways, a concept termed functional selectivity or biased agonism15.
The β-arrestin-biased ligand carvedilol has three unique features at the β1AR: (1) it has inverse efficacy for Gαs-dependent adenylyl cyclase activity; (2) it promotes the recruitment of Gαi, not Gαs, to the β1AR; (3) it activates the classical β-arrestin signaling using a Gαi paradigm. These unique signaling properties of carvedilol may be attributed to its ability to stabilize a distinct receptor active conformation15. For the β2AR, carvedilol uniquely induces significant conformational rearrangement around residue Lys263 and Cys265 in the third intracellular loop of the receptor, which may expose the loop toward intracellular surface and facilitate the receptor interaction with β-arrestins15. Though a previous study suggests the crystal structure of carvedilol-bound β1AR is similar to that of the cyanopindolol-bound inactive state structure38, additional conformations stabilized by carvedilol may require the binding of transducers such as Gαi or β-arrestin. This requirement of transducer binding for receptor conformational stability is supported by the structural study of the β2AR showing that the interaction of a G protein, or a G protein-like-protein nanobody, is required to stabilize the agonist-induced receptor active conformation39. In our study, using a FRET-based β1AR conformation sensor, we show that carvedilol induces a change of FRET ratio, representing a receptor conformational change. Notably, the β1AR conformation induced by carvedilol is distinct from the one induced by the balanced agonist isoproterenol, as carvedilol increased the FRET ratio while isoproterenol decreased it. This further supports a concept that receptors can adopt distinct conformations when stimulated by different ligands. As our results show that carvedilol promotes the recruitment of Gαi to β1ARs, while a wide range of other βAR ligands tested do not, it is possible that carvedilol induces a β1AR conformational change that exposes allosteric binding sites on the receptor to allow for receptor–Gαi interaction. In turn, the bound Gαi stabilizes the carvedilol-induced active receptor conformation and is consistent with our data where pretreatment with the Gαi inhibitor PTX impairs the carvedilol activated β1AR conformation. Together these data support the concept that carvedilol-induced Gαi is a positive allosteric modulator of the β-arrestin-biased β1AR active conformation.
While we have not determined the precise mechanism of how Gαi binding to the carvedilol-occupied β1AR triggers β-arrestin signaling, we postulate that it may involve subsequent receptor phosphorylation in a process known as the “barcode” hypothesis19. Upon ligands stimulation, GPCRs can be phosphorylated by distinct GRK subtypes at specific sites. Previous study identified β2AR sites that are specifically phosphorylated by GRK2 and GRK632. While the balanced agonist isoproterenol stimulates β2AR phosphorylation at both GRK2- and GRK6-specific sites, carvedilol only stimulates receptor phosphorylation at the GRK6-specific sites. This “barcode” phosphorylation pattern of receptors plays essential roles in regulating the recruitment and functionality of signaling transducers19. For instance, β2AR phosphorylation mediated by GRK2 and GRK6 induces distinct β-arrestin conformations, and differentially regulates receptor internalization and ERK activation32. Similarly for the β1AR, GRK2-mediated and GRK5/6-mediated receptor phosphorylation leads to distinct cellular responses9, 40, suggesting that a phosphorylation barcode for the β1AR may also direct β-arrestin signaling. To dissect the mechanism of how Gαi regulates β1AR signaling, future studies will need to compare the isoproterenol- or carvedilol-induced barcode phosphorylation patterns of the β1AR, as well as the effect of Gαi inhibitor PTX on it.
While our data show that both Gαi and β-arrestins are required for carvedilol-induced biased signaling of the β1AR, whether β-arrestin is recruited to the carvedilol occupied β1AR remains to be determined. Using a number of methodologies, such as co-immunoprecipitation, confocal- or bioluminescence resonance energy transfer-based assays, we were unable to detect carvedilol-induced β-arrestin recruitment to the β1AR. This may be due to a number of reasons: (1) ligand-induced β-arrestin recruitment and activation is rapid, within 2 s after stimulation, and reversible41; (2) the affinity of the β1AR–β-arrestin interaction is low. Both the β1AR and the β2AR are known as class A receptors, since they are characterized by transient and weak interaction with β-arrestins along with a rapid recycling to the plasma membrane after internalization. To demonstrate carvedilol triggered β-arrestin recruitment to the β2AR, previous studies used a chimeric receptor consisting of the β2AR fused to vasopressin V2 receptor cytoplasmic tail (β2AR-V2R) to increase the affinity of β-arrestin to the ligand occupied receptor21. However, as we have shown (Fig. 8c), the C-tail of the β1AR is required for Gαi recruitment. Therefore substituting the β1AR C-tail with the V2R tail would not provide a chimeric receptor suitable to study the role of Gαi in carvedilol stimulated β-arrestin recruitment. Importantly, we cannot exclude that the carvedilol-stimulated β1AR signaling is mediated by β-arrestin by an indirect mechanism that does not require direct binding of β-arrestin to the β1AR. A recent study identified unique features for the β1AR with respect to β-arrestin interaction and activation42, where a brief interaction with the activated β1AR is sufficient to target β-arrestin2 to clathrin-coated structures and trigger ERK signaling even in the absence of receptor association42. This β-arrestin “activation at a distance” mechanism suggests that a β1AR–β-arrestin complex may not be essential for the activation of β-arrestin-dependent signaling and could explain our findings for a role of β-arrestin in carvedilol-induced signaling without a direct β1AR–β-arrestin interaction. Lastly, it is also possible that instead of directly engagement with the β1AR, β-arrestins could associate with other components of the signaling cascade such as the transactivated EGFR. This has recently been shown for the vasopressin V2 receptor signaling, where β-arrestins are recruited to, and act downstream of, the transactivated insulin-like growth factor receptor43.
Carvedilol is a βAR antagonist (β-blocker), a family of drugs that are widely used in the therapeutic treatment of cardiovascular diseases such as hypertension and heart failure, as β1ARs and β2ARs are predominant GPCR subtypes expressed in mammalian heart and play vital roles in the regulation of cardiac function4. In heart failure, treatment with β-blockers improves left ventricle function, reverses the pathological cardiac remodeling, and reduces mortality and morbidity44, 45. However, β-blockers have different clinical efficacies. Some evidence suggests that carvedilol has a superior effect on cardiovascular survival to other β-blockers46. The molecular basis for this remains to be elucidated, but has been attributed to the additional properties of carvedilol other than β-blockers, such as the antioxidant, antiproliferative effects and α1 adrenergic receptor blockade47. Interestingly, carvedilol appears to be unique among βAR blockers in that it can activate β-arrestin-dependent signaling that confers cardioprotection10, 21. Given the possible cardioprotective role of Gαi during cardiac stress48 and the ability of carvedilol to promote β1AR–Gαi coupling, it is possible that this unique property of carvedilol is also important for its therapeutic efficacy.
In conclusion, we identify a new signaling mechanism of GPCR biased agonism. To date, the β1AR was considered to be predominantly coupled to Gαs, and β-arrestin-dependent β1AR signaling to be independent of G proteins. However, our data supports a concept where carvedilol has three unique properties at the β1AR: (1) it is inert with respect to Gαs; (2) it recruits Gαi and converts the β1AR from a Gαs-coupled receptor to one that couples to Gαi; and (3) it activates classical β-arrestin-dependent signaling in a Gαi paradigm. These data suggest a greater complexity for receptor signaling bias than previously appreciated in that coupling of distinct G protein subtypes to the activated receptor are needed for β-arrestin-biased agonism. These data also have important implications when considering the development of new therapeutic ligands designed to selectively target β-arrestin-biased signaling pathways.
Methods
Cell culture
HEK293 cells (American Type Culture Collection) stably expressing FLAG-tagged β1AR or β2AR are maintained and transfected as previously described33, 49. Cells were periodically treated with BMCyclin (Roche) to avoid mycoplasma contamination. Cells were incubated overnight in serum-free medium supplemented with 0.1% BSA, 10 mM HEPES and 1% penicillin–streptomycin and pretreated with pertussis toxin (200 ng per ml, overnight), H89 (10 μM, 30 min) or propranolol (10 μM, 30 min) before ligand stimulation. HEK293 cells stably expressing β1AR-FRET sensor were used for the FRET experiments.
Generation of β-arrestin or Gαi knockout cell line
Plasmids carrying S. pyogenes Cas9 (SpCas9) next to a cloning site for guide RNA (gRNA) with EGFP (pSpCas9 (BB)-2A-GFP, Addgene 48138) or puromycin resistant gene (pSpCas9(BB)-2A-Puro, Addgene 48139) were obtained from Addgene (deposited by the laboratory of Dr. F. Zhang50). Designing of the guide RNAs for Gαi or β-arrestins and cloning the guide RNAs into the Cas9 plasmids were performed as previously described50.
For β-arrestin knockout cells, β-arrestin1 was targeted using guide sequence oligos (top: CACCGCATCGACCTCGTGGACCCTG; bottom: AACCAGGGTCCACGAGGTCGATGC). β-arrestin2 was targeted using guide sequence oligos (top: CACCGCGTAGATCACCTGGACAAAG; bottom: AAACCTTTGTCCAGGTGATCTACGC). The guide sequence oligos were cloned into pSpCas9(BB)-2A-Puro. After confirming the cloning by sequencing, plasmids were transfected into HEK293 cells using Fugene 6 transfection reagent (Promega). 72 h after transfection, cells were harvested to check INDEL (insertion deletion) in the genome by surveyor’s assay. Puromycin (2.5 μg per ml) was added into the medium of surveyor positive cells to select cells with the plasmid containing puromycin resistant gene along with guide RNA and Cas9. The knockout of β-arrestins were confirmed by western blot.
For Gαi knockout cells, Gαi1 was targeted using guide sequence oligos (top: CACCGCGCCGTCCTCACGGAGGTTG; bottom: AAACCAACCTCCGTGAGGACGGCGC), Gαi2 was targeted using guide sequence oligos (top: CACCGAGACAACCGCCCGGTACTGC, bottom: AAACGCAGTACCGGGCGGTTGTCTC), and Gαi3 was targeted using guide sequence oligos (top: CACCGGGACGGCTAAAGATTGACTT; bottom: AAACAAGTCAATCTTTAGCCGTCCC). The guide sequence oligos were cloned into pSpCas9 (BB)-2A-GFP. Plasmids targeting the three Gαi subtypes were co-transfected into HEK293 cells. GFP positive cells were selected by fluorescence-activated cell sorting, diluted for growth and single cell colonies were obtained. The Gαi knockout were confirmed by western blot.
Immunoblotting and immunoprecipitation
Following stimulation, cells were scraped in 1% NP-40 lysis buffer (20 mM Tris, pH 7.4, 137 mM NaCl, 20% glycerol, 1% Nonidet P-40, 2 mM sodium orthovanadate, 1 mM PMSF, 10 mM sodium fluoride, 10 μg per ml aprotinin, 5 μg per ml leupeptin and phosphatase inhibitors) or 1% DDM lysis buffer (20 mM HEPES, 150 mM NaCl, 1% n-Dodecyl β-d-maltoside, protease inhibitors and phosphatase inhibitors). For immunoprecipitation of FLAG-tagged β1AR or β2AR, 1–2 mg of protein was incubated overnight with 30 μl of anti-FLAG M2 magnetic beads (Sigma). For immunoprecipitation of active Gαi, protein was incubated for 2 h with anti-active Gαi antibody (New East Biosciences) and Protein A/G beads (EMD Millipore). Immunoprecipitates or cell lysate samples were separated by SDS-PAGE, transferred to PVDF membrane (Bio-Rad) and subjected to immunoblotting with various primary antibodies. Immunoblots were detected using enhanced chemiluminescence (Thermo Fisher Scientific) and analyzed with ImageJ software. Uncropped blots are shown in Supplementary Fig. 6.
Antibodies
Please refer the information of antibodies to Supplementary Table 1.
ERK phosphorylation in mice heart
Eight to 12-week-old gender-matched β1AR knockout (β1AR KO) mice and β2AR KO mice51 were used for this study. Three to six animals were used for each experimental group based on previous experiments. Randomization and blinding were not performed. Mice were pretreated with vehicle or 25 μg per kg pertussis toxin (PTX) via intraperitoneal injection. After 48 h, mice were anesthetized with ketamine (100 mg per kg) and xylazine (2.5 mg per kg) for 10 min. Heart was then excised and, with aorta cannulated to needle, perfused with perfusion buffer (118 mM NaCl, 4.7 mM KCl, 1.2 mM MgSO4, 1.2 mM KH2PO4, 2.5 mM CaCl2, 25 mM NaHCO3, 0.5 mM Na-EDTA, 5.5 mM glucose) with O2 bubbling through Langendorff apparatus (Hugo Sachs Harvard Apparatus) set at 37 °C. After 10 min perfusion, buffer was changed to perfusion buffer with vehicle or 10 μM carvedilol, and perfused for another 10 min. Heart was then removed from the system and left ventricle was excised and snap frozen in liquid nitrogen. Animal experiments carried out for this study were handled according to approved protocols and animal welfare regulations the Animal Care and Use Committee of Duke University Medical Center.
Fluorescence resonance energy transfer measurement
FRET measurement was performed as previously described26. Briefly, HEK293 cells stably expressing β1AR-FRET sensor were cultured in glass-bottomed confocal dish. Cells were pretreated with vehicle or 200 ng per ml PTX for 16 h before experiment. On the day of experiment, cells were maintained in FRET buffer (10 mM HEPES, 0.2% BSA, 140 mM NaCl, 4.5 mM KCl, 2 mM CaCl2, 2 mM MgCl2, pH 7.4). FRET experiments were preformed using an Olympus IX-71 microscope. FRET was monitored as the emission ratio of YFP to Cerulean. Images were taken at 10 s interval and analyzed with ImageJ software.
In situ proximity ligation assay
β1AR or β2AR stable cells were cultured in 35 mm poly-d-lysine coated glass-bottom confocal dish (MatTek). Following stimulation, cells were fixed in 4% paraformaldehyde for 15 min and permeabilized with 0.2% Triton-X-100 for 10 min. After blocked with blocking buffer from Duolink Detection Kit (Sigma) at 37 °C for 30 min, cells were incubated overnight at 4 °C with anti-β1AR (or β2AR) antibody from rabbit (Santa Cruz) in conjunction with anti-Gαi antibody from mouse (New East Biosciences). The proximity ligation reaction was performed according to the manufacturer’s protocol using the Duolink Detection Kit (Sigma). Cells were mounted with DAPI Fluoromount-G (Southern Biotech). Images were recorded with Zeiss Axio Observer Z1 confocal microscope with ×40 objective. Data analysis was performed with ImageJ software. To quantify the mean PLA signal per cell, the red PLA fluorescence intensity was divided by the number of cells. The mean PLA signal of each data set was corrected by subtracting the background staining determined as the mean PLA signal of HEK293 cells without receptor overexpression. The relative fold over non-stimulation was normalized to the mean PLA signal of the unstimulated cells. In each experiment, 20–40 cells from three images were quantified for each condition.
EGFR internalization assessed by confocal microscopy
HEK293 cells stably expressing FLAG-tagged β1AR were transfected with EGFR-GFP together with control siRNA or β-arrestin siRNA as described below. After 24 h, the transfected cells were plated into glass-bottomed confocal dish and kept in culture for additional 24 h. Following pretreatment with PTX and stimulation with ligands, cells were washed with ice-cold PBS and fixed with 4% paraformaldehyde for 15 min. EGFR internalization was visualized with Zeiss Axio Observer Z1 confocal microscope with ×63 objective. In each experiment, 50 cells of each condition were counted under microscope. The percentage of cells showing EGFR internalization was determined by the number of cells showing the intracellular aggregate of EGFR-GFP.
EGFR internalization assessed by flow cytometry
HEK293 cells (wildtype, β-arrestin1/2 knockout or Gαi knockout) were transfected with CFP-tagged β1AR. 48 h after transfection, cells were serum starved for 4 h before ligand stimulation. Following stimulation, cells were dissociated with accutase, washed with PBS and fixed in 4% formaldehyde for 15 min at room temperature. Fixed cells were enumerated, washed twice with staining buffer (PBS, 0.5% BSA, 2 mM EDTA) and blocked with 5% rat serum (Sigma) in staining buffer for 15 min. 1 × 106 cells for each sample were stained with equal concentrations of either PE-conjugated EGFR antibody (R&D systems) or isotype control (R&D systems; PE-conjugated rat IgG2A) for 30 min at room temperature. Following staining, cells were washed twice with staining buffer and resuspended in PBS for analysis utilizing a BD LSRII flow cytometer (BD Biosciences). Data analysis was performed with FlowJo software. Following doublet exclusion, single cells were gated for CFP positivity. To quantify relative EGFR internalization following ligand stimulation, the following formula was utilized: geometric mean fluorescence intensity of the PE-EGFR signal for each data set minus MFI of the isotype control. The resultant value was normalized to the MFI of the unstimulated cells to assess the relative percentage of EGFR internalization.
β-arrestin siRNA knockdown
SiRNAs targeting β-arrestin have been described previously13. A nonsilencing RNA duplex (5′-AAUUCUCCGAACGUGUCACGU-3′) was used as a control. HEK293 cells stably expressing FLAG-tagged β1AR were seeded into 10 cm dish on the day before to reach 30–40% confluence at the time of transfection. SiRNA were transfected using GeneSilencer Transfection Reagent (Genlantis) according to the manufacturer’s protocol. In brief, 20 μg siRNA and 240 μl siRNA dilution buffer were added into 180 μl serum-free medium, whereas 51 μl of transfection reagent was mixed with 300 μl serum-free medium. Both solutions were allowed to stand for 5 min at room temperature, then combined and incubated for additional 20 min. The mixture was then added to cells in the 10 cm dish with 4 ml serum-free medium. After 4 h incubation at 37 °C and 5% CO2, 5.5 ml of MEM containing 20% FBS and 2% penicillin–streptomycin were added into the dish. All assays were performed 3 d after siRNA transfection.
Statistical analysis
Data are expressed as mean ± SEM. Statistical comparisons were performed using two-tailed Student’s t-test or ANOVA with Bonferroni correction for multiple comparisons in Graphpad Prism. Normality test was performed with Shapiro-Wilk test. Outlier data points more than two standard deviations from the mean were excluded from analysis. Differences were considered statistically significant at P < 0.05.
Data availability
All data supporting the findings of this study are available from the authors upon request.
References
Lagerstrom, M. C. & Schioth, H. B. Structural diversity of G protein-coupled receptors and significance for drug discovery. Nat. Rev. Drug Discov. 7, 339–357 (2008).
Ma, P. & Zemmel, R. Value of novelty? Nat. Rev. Drug Discov. 1, 571–572 (2002).
Overington, J. P., Al-Lazikani, B. & Hopkins, A. L. How many drug targets are there? Nat. Rev. Drug Discov. 5, 993–996 (2006).
Woo, A. Y. & Xiao, R. P. beta-Adrenergic receptor subtype signaling in heart: from bench to bedside. Acta Pharmacol. Sin. 33, 335–341 (2012).
Wettschureck, N. & Offermanns, S. Mammalian G proteins and their cell type specific functions. Physiol. Rev. 85, 1159–1204 (2005).
Salazar, N. C., Chen, J. & Rockman, H. A. Cardiac GPCRs: GPCR signaling in healthy and failing hearts. Biochim. Biophys. Acta 1768, 1006–1018 (2007).
Rajagopal, S., Rajagopal, K. & Lefkowitz, R. J. Teaching old receptors new tricks: biasing seven-transmembrane receptors. Nat. Rev. Drug Discov. 9, 373–386 (2010).
Rockman, H. A., Koch, W. J. & Lefkowitz, R. J. Seven-transmembrane-spanning receptors and heart function. Nature 415, 206–212 (2002).
Noma, T. et al. Beta-arrestin-mediated beta1-adrenergic receptor transactivation of the EGFR confers cardioprotection. J. Clin. Invest. 117, 2445–2458 (2007).
Kim, I. M. et al. Beta-blockers alprenolol and carvedilol stimulate beta-arrestin-mediated EGFR transactivation. Proc. Natl Acad. Sci. USA 105, 14555–14560 (2008).
Luttrell, L. M. et al. Beta-arrestin-dependent formation of beta2 adrenergic receptor-Src protein kinase complexes. Science 283, 655–661 (1999).
Shenoy, S. K. et al. Beta-arrestin-dependent, G protein-independent ERK1/2 activation by the beta2 adrenergic receptor. J. Biol. Chem. 281, 1261–1273 (2006).
Ahn, S., Wei, H., Garrison, T. R. & Lefkowitz, R. J. Reciprocal regulation of angiotensin receptor-activated extracellular signal-regulated kinases by beta-arrestins 1 and 2. J. Biol. Chem. 279, 7807–7811 (2004).
Mangmool, S., Shukla, A. K. & Rockman, H. A. Beta-arrestin-dependent activation of Ca(2+)/calmodulin kinase II after beta(1)-adrenergic receptor stimulation. J. Cell. Biol. 189, 573–587 (2010).
Kahsai, A. W. et al. Multiple ligand-specific conformations of the beta2-adrenergic receptor. Nat. Chem. Biol. 7, 692–700 (2011).
Manglik, A. et al. Structural insights into the dynamic process of beta2-adrenergic receptor signaling. Cell 161, 1101–1111 (2015).
Ye, L., Van Eps, N., Zimmer, M., Ernst, O. P. & Prosser, R. S. Activation of the A2A adenosine G-protein-coupled receptor by conformational selection. Nature 533, 265–268 (2016).
Rajagopal, S. et al. Quantifying ligand bias at seven-transmembrane receptors. Mol. Pharmacol. 80, 367–377 (2011).
Wisler, J. W., Xiao, K., Thomsen, A. R. & Lefkowitz, R. J. Recent developments in biased agonism. Curr. Opin. Cell Biol. 27, 18–24 (2014).
Staus, D. P. et al. Allosteric nanobodies reveal the dynamic range and diverse mechanisms of G-protein-coupled receptor activation. Nature 535, 448–452 (2016).
Wisler, J. W. et al. A unique mechanism of beta-blocker action: carvedilol stimulates beta-arrestin signaling. Proc. Natl Acad. Sci. USA 104, 16657–16662 (2007).
Sauliere, A. et al. Deciphering biased-agonism complexity reveals a new active AT1 receptor entity. Nat. Chem. Biol. 8, 622–630 (2012).
Thomsen, A. R. et al. GPCR-G protein-beta-arrestin super-complex mediates sustained G protein signaling. Cell 166, 907–919 (2016).
Chruscinski, A. J. et al. Targeted disruption of the beta2 adrenergic receptor gene. J. Biol. Chem. 274, 16694–16700 (1999).
Rohrer, D. K. et al. Targeted disruption of the mouse beta1-adrenergic receptor gene: developmental and cardiovascular effects. Proc. Natl Acad. Sci. USA 93, 7375–7380 (1996).
Rochais, F. et al. Real-time optical recording of beta1-adrenergic receptor activation reveals supersensitivity of the Arg389 variant to carvedilol. J. Clin. Invest. 117, 229–235 (2007).
Daaka, Y., Luttrell, L. M. & Lefkowitz, R. J. Switching of the coupling of the beta2-adrenergic receptor to different G proteins by protein kinase A. Nature 390, 88–91 (1997).
Xiao, R. P., Ji, X. & Lakatta, E. G. Functional coupling of the beta 2-adrenoceptor to a pertussis toxin-sensitive G protein in cardiac myocytes. Mol. Pharmacol. 47, 322–329 (1995).
Martin, N. P., Whalen, E. J., Zamah, M. A., Pierce, K. L. & Lefkowitz, R. J. PKA-mediated phosphorylation of the beta1-adrenergic receptor promotes Gs/Gi switching. Cell. Signal. 16, 1397–1403 (2004).
Koch, W. J., Inglese, J., Stone, W. C. & Lefkowitz, R. J. The binding site for the beta gamma subunits of heterotrimeric G proteins on the beta-adrenergic receptor kinase. J. Biol. Chem. 268, 8256–8260 (1993).
Crespo, P., Cachero, T. G., Xu, N. & Gutkind, J. S. Dual effect of beta-adrenergic receptors on mitogen-activated protein kinase. Evidence for a beta gamma-dependent activation and a G alpha s-cAMP-mediated inhibition. J. Biol. Chem. 270, 25259–25265 (1995).
Nobles, K. N. et al. Distinct phosphorylation sites on the beta(2)-adrenergic receptor establish a barcode that encodes differential functions of beta-arrestin. Sci. Signal. 4, ra51 (2011).
Rapacciuolo, A. et al. Protein kinase A and G protein-coupled receptor kinase phosphorylation mediates beta-1 adrenergic receptor endocytosis through different pathways. J. Biol. Chem. 278, 35403–35411 (2003).
Ritter, S. L. & Hall, R. A. Fine-tuning of GPCR activity by receptor-interacting proteins. Nat. Rev. Mol. Cell Biol. 10, 819–830 (2009).
Rasmussen, S. G. et al. Crystal structure of the beta2 adrenergic receptor-Gs protein complex. Nature 477, 549–555 (2011).
Dohlman, H. G., Thorner, J., Caron, M. G. & Lefkowitz, R. J. Model systems for the study of seven-transmembrane-segment receptors. Annu. Rev. Biochem. 60, 653–688 (1991).
van Biesen, T., Luttrell, L. M., Hawes, B. E. & Lefkowitz, R. J. Mitogenic signaling via G protein-coupled receptors. Endocr. Rev. 17, 698–714 (1996).
Warne, T., Edwards, P. C., Leslie, A. G. & Tate, C. G. Crystal structures of a stabilized beta1-adrenoceptor bound to the biased agonists bucindolol and carvedilol. Structure 20, 841–849 (2012).
Rosenbaum, D. M. et al. Structure and function of an irreversible agonist-beta(2) adrenoceptor complex. Nature 469, 236–240 (2011).
Tilley, D. G., Kim, I. M., Patel, P. A., Violin, J. D. & Rockman, H. A. beta-Arrestin mediates beta1-adrenergic receptor-epidermal growth factor receptor interaction and downstream signaling. J. Biol. Chem. 284, 20375–20386 (2009).
Nuber, S. et al. beta-Arrestin biosensors reveal a rapid, receptor-dependent activation/deactivation cycle. Nature 531, 661–664 (2016).
Eichel, K., Jullie, D. & von Zastrow, M. beta-Arrestin drives MAP kinase signalling from clathrin-coated structures after GPCR dissociation. Nat. Cell Biol. 18, 303–310 (2016).
Oligny-Longpre, G. et al. Engagement of beta-arrestin by transactivated insulin-like growth factor receptor is needed for V2 vasopressin receptor-stimulated ERK1/2 activation. Proc. Natl Acad. Sci. USA 109, E1028–E1037 (2012).
Packer, M. et al. Effect of carvedilol on survival in severe chronic heart failure. N. Engl. J. Med. 344, 1651–1658 (2001).
McMurray, J. J. & Pfeffer, M. A. Heart failure. Lancet 365, 1877–1889 (2005).
Poole-Wilson, P. A. et al. Comparison of carvedilol and metoprolol on clinical outcomes in patients with chronic heart failure in the Carvedilol Or Metoprolol European Trial (COMET): randomised controlled trial. Lancet 362, 7–13 (2003).
Ohlstein, E. H. et al. Carvedilol, a cardiovascular drug, prevents vascular smooth muscle cell proliferation, migration, and neointimal formation following vascular injury. Proc. Natl Acad. Sci. USA 90, 6189–6193 (1993).
DeGeorge, B. R. Jr et al. Targeted inhibition of cardiomyocyte Gi signaling enhances susceptibility to apoptotic cell death in response to ischemic stress. Circulation 117, 1378–1387 (2008).
Naga Prasad, S. V. et al. Phosphoinositide 3-kinase regulates beta2-adrenergic receptor endocytosis by AP-2 recruitment to the receptor/beta-arrestin complex. J. Cell Biol. 158, 563–575 (2002).
Ran, F. A. et al. Genome engineering using the CRISPR-Cas9 system. Nat. Protoc. 8, 2281–2308 (2013).
Rohrer, D. K., Chruscinski, A., Schauble, E. H., Bernstein, D. & Kobilka, B. K. Cardiovascular and metabolic alterations in mice lacking both beta1- and beta2-adrenergic receptors. J. Biol. Chem. 274, 16701–16708 (1999).
Acknowledgements
We thank Dr K. Xiao (University of Pittsburgh, USA) for intellectual input. We thank Dr R.J. Lefkowitz (Duke University, USA) for providing the β-arrestin antibodies. We thank Dr M. Bouvier (University of Montreal, Canada) and Dr J.S. Gutkind (University of California, San Diego, USA) for providing the T8-βARKct construct. This work was supported by National Institutes of Health grants HL056687 and HL075443 to H.A.R. and AHA Predoctoral Fellowship 14PRE20480352 to J.W.
Author information
Authors and Affiliations
Contributions
H.A.R. supervised the entire study; H.A.R., J.W. and D.P.S. wrote the manuscript with comments from all co-authors; J.W. designed and performed most of the experiments and analyzed data; K.H. performed the ERK phosphorylation assay in mice heart; M.A.M. assisted with flow cytometry assay; G.R.D. generated the Gαi and β-arrestin knockout cells; Q.C. assisted with co-immunoprecipitation experiments; A.A. and S.E. provided material and performed preliminary experiments for β1AR FRET-sensor.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Additional information
Publisher's note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commonslicense, unless indicated otherwise in a credit line to the material. If material is not included in the article’sCreative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visithttp://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Wang, J., Hanada, K., Staus, D.P. et al. Gαi is required for carvedilol-induced β1 adrenergic receptor β-arrestin biased signaling. Nat Commun 8, 1706 (2017). https://doi.org/10.1038/s41467-017-01855-z
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41467-017-01855-z
- Springer Nature Limited
This article is cited by
-
Membrane mediated mechanical stimuli produces distinct active-like states in the AT1 receptor
Nature Communications (2023)
-
Pepducin ICL1-9-Mediated β2-Adrenergic Receptor-Dependent Cardiomyocyte Contractility Occurs in a Gi Protein/ROCK/PKD-Sensitive Manner
Cardiovascular Drugs and Therapy (2023)
-
QR code model: a new possibility for GPCR phosphorylation recognition
Cell Communication and Signaling (2022)
-
Noradrenergic consolidation of social recognition memory is mediated by β-arrestin–biased signaling in the mouse prefrontal cortex
Communications Biology (2022)
-
Carvedilol targets β-arrestins to rewire innate immunity and improve oncolytic adenoviral therapy
Communications Biology (2022)