Abstract
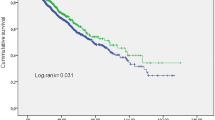
An intradialytic systolic blood pressure (SBP) decline, which defines intradialytic hypotension, may be associated with higher all-cause mortality. However, in Japanese patients on hemodialysis (HD), the association between intradialytic SBP decline and patient outcomes is unclear. This retrospective cohort study included 307 Japanese patients undergoing HD over 1 year in three dialysis clinics and evaluated the association between the mean annual intradialytic SBP decline (predialysis SBP-nadir intradialytic SBP) and clinical outcomes, including major adverse cardiovascular events (MACEs; cardiovascular death, nonfatal myocardial infarction or unstable angina, stroke, heart failure, and other severe cardiovascular events requiring hospitalization) by following up for 2 years. The mean annual intradialytic SBP decline was 24.2 (25–75th percentile, 18.3–35.0) mmHg. In the model fully adjusted for intradialytic SBP decline tertile group (T1, <20.4 mmHg; T2, 20.4 to <29.9 mmHg; T3, ≥29.9 mmHg), predialysis SBP, age, sex, HD vintage, Charlson comorbidity index, ultrafiltration rate, use of renin–angiotensin system inhibitors, corrected calcium, phosphorus, human atrial natriuretic peptide, geriatric nutritional risk index, normalized protein catabolism rate, C-reactive protein, hemoglobin, and use of pressor agents, Cox regression analyses showed that the hazard ratio (HR) was significantly higher for T3 than for T1 for MACEs (HR, 2.38; 95% confidence interval 1.12–5.09) and all-cause hospitalization (HR, 1.68; 95% confidence interval 1.03–2.74). Therefore, in Japanese patients on HD, a greater intradialytic SBP decline was associated with worse clinical outcomes. Further studies are warranted to investigate whether interventions to attenuate the intradialytic SBP decline will improve the prognosis of Japanese patients on HD.





Similar content being viewed by others
References
Hanafusa N, Abe M, Joki N, Hoshino J, Kikuchi K, Goto S, et al. 2020 Annual dialysis data report, JSDT Renal Data Registry. Nihon Toseki Igakkai Zasshi. 2021;54:611–57.
Kikuchi K, Hamano T, Wada A, Nakai S, Masakane I. Predilution online hemodiafiltration is associated with improved survival compared with hemodialysis. Kidney Int. 2019;95:929–38.
Cho A, Lee YK, Oh J, Yoon JW, Shin DH, Jeon HJ, et al. The relationship between intradialytic hypotension and vascular calcification in hemodialysis patients. PLoS One. 2017;12:e0185846.
Mc Causland FR, Brunelli SM, Waikar SS. Dialysis dose and intradialytic hypotension: results from the HEMO study. Am J Nephrol. 2013;38:388–96.
Mc Causland FR, Waikar SS. Association of predialysis calculated plasma osmolarity with intradialytic blood pressure decline. Am J Kidney Dis. 2015;66:499–506.
Okoye OC, Slater HE, Rajora N. Prevalence and risk factors of intra-dialytic hypotension: a 5 year retrospective report from a single Nigerian Centre. Pan Afr Med J. 2017;28:62.
Yu J, Liu Z, Shen B, Teng J, Zou J, Ding X. Intradialytic hypotension as an independent risk factor for long-term mortality in maintaining hemodialysis patients: a 5-year follow-up cohort study. Blood Purif. 2018;45:320–6.
Kanbay M, Ertuglu LA, Afsar B, Ozdogan E, Siriopol D, Covic A, et al. An update review of intradialytic hypotension: concept, risk factors, clinical implications and management. Clin Kidney J. 2020;13:981–93.
Uchiyama K, Shibagaki K, Yanai A, Kusahana E, Nakayama T, Morimoto K, et al. Seasonal variation and predictors of intradialytic blood pressure decline: a retrospective cohort study. Hypertens Res. 2021;44:1417–27.
Argilés A, Mourad G, Mion C. Seasonal changes in blood pressure in patients with end-stage renal disease treated with hemodialysis. N. Engl J Med. 1998;339:1364–70.
Tozawa M, Iseki K, Iseki C, Morita O, Yoshi S, Fukiyama K. Seasonal blood pressure and body weight variation in patients on chronic hemodialysis. Am J Nephrol. 1999;19:660–7.
Spósito M, Nieto FJ, Ventura JE. Seasonal variations of blood pressure and overhydration in patients on chronic hemodialysis. Am J Kidney Dis. 2000;35:812–8.
Cheung AK, Yan G, Greene T, Daugirdas JT, Dwyer JT, Levin NW, et al. Seasonal variations in clinical and laboratory variables among chronic hemodialysis patients. J Am Soc Nephrol. 2002;13:2345–52.
Usvyat LA, Carter M, Thijssen S, Kooman JP, Van Der Sande FM, Zabetakis P, et al. Seasonal variations in mortality, clinical, and laboratory parameters in hemodialysis patients: a 5-year cohort study. Clin J Am Soc Nephrol. 2012;7:108–15.
Yamaguchi J, Hagiwara N, Ogawa H, Koyanagi R, Kasanuki H, Takagi A, et al. Effect of amlodipine+ candesartan on cardiovascular events in hypertensive patients with coronary artery disease (from The Heart Institute of Japan Candesartan Randomized Trial for Evaluation in Coronary Artery Disease [HIJ-CREATE] Study). Am J Cardiol. 2010;106:819–24.
Ogawa C, Tsuchiya K, Maeda K. High serum magnesium levels are associated with favorable prognoses in diabetic hemodialysis patients, retrospective observational study. PLoS One. 2020;15:e0238763.
Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40:373–83.
Mizuguchi J, Tomo T, Masakane I, Watanabe Y, Kawanishi H, Akiba T, et al. JSDT [Guidelines for maintenance hemodialysis: hemodialysis prescriptions]. J Jpn Soc Dial Ther. 2013;46:587–632.
Kanda Y. Investigation of the freely available easy-to-use software ‘EZR’ for medical statistics. Bone Marrow Transpl. 2013;48:452–8.
Goodkin DA, Bragg-Gresham JL, Koenig KG, Wolfe RA, Akiba T, Andreucci VE, et al. Association of comorbid conditions and mortality in hemodialysis patients in Europe, Japan, and the United States: the dialysis outcomes and practice patterns study (DOPPS). J Am Soc Nephrol. 2003;14:3270–7.
Okamura A, Okura H, Iwai S, Sakagami A, Kamon D, Hashimoto Y, et al. Incidence and prognostic impact of the calcified nodule in coronary artery disease patients with end-stage renal disease on dialysis. Heart Vessels. 2022;37:1662–8.
Shoji T, Tsubakihara Y, Fujii M, Imai E. Hemodialysis-associated hypotension as an independent risk factor for two-year mortality in hemodialysis patients. Kidney Int. 2004;66:1212–20.
Flythe JE, Xue H, Lynch KE, Curhan GC, Brunelli SM. Association of mortality risk with various definitions of intradialytic hypotension. J Am Soc Nephrol. 2015;26:724–34.
Lu J, Zhu M, Liu S, Zhu M, Pang H, Lin X, et al. The relationship between survival rate and intradialytic blood pressure changes in maintenance hemodialysis patients. Ren Fail. 2017;39:417–22.
Chou JA, Streja E, Nguyen DV, Rhee CM, Obi Y, Inrig JK, et al. Intradialytic hypotension, blood pressure changes and mortality risk in incident hemodialysis patients. Nephrol Dial Transpl. 2018;33:149–59.
Yu J, Chen X, Wang Y, Liu Z, Shen B, Teng J, et al. Intradialytic systolic blood pressure variation can predict long-term mortality in patients on maintenance hemodialysis. Int Urol Nephrol. 2021;53:785–95.
Burton JO, Jefferies HJ, Selby NM, McIntyre CW. Hemodialysis-induced cardiac injury: determinants and associated outcomes. Clin J Am Soc Nephrol. 2009;4:914–20.
Sars B, van der Sande FM, Kooman JP. Intradialytic hypotension: mechanisms and outcome. Blood Purif. 2020;49:158–67.
Magder SA. The highs and lows of blood pressure: toward meaningful clinical targets in patients with shock. Crit Care Med. 2014;42:1241–51.
Franssen CFM. Adenosine and dialysis hypotension. Kidney Int. 2006;69:789–91.
Mineshima M, Takahashi S, Tomo T, Kawanishi H, Kawaguchi H, Minakuchi J, et al. A clinical significance of intermittent infusion hemodiafiltration using backfiltration of ultrapure dialysis fluid compared to hemodialysis: a multicenter randomized controlled crossover trial. Blood Purif. 2019;48:368–81.
Acknowledgements
The authors thank all the participants of this research project.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Ethics
This study and all its protocols were reviewed and approved by the ethics committee of our hospital, and informed consent was obtained from all patients prior to their participation.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Takahashi, R., Uchiyama, K., Washida, N. et al. Mean annual intradialytic blood pressure decline and cardiovascular events in Japanese patients on maintenance hemodialysis. Hypertens Res 46, 1536–1546 (2023). https://doi.org/10.1038/s41440-023-01228-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-023-01228-8
- Springer Nature Singapore Pte Ltd.
Keywords
This article is cited by
-
Blood pressure management in hemodialysis patients
Hypertension Research (2023)