Abstract
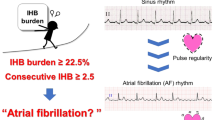
Hypertension is the most common risk factor for atrial fibrillation (AF). The ability to screen for potential AF during blood pressure (BP) measurement may be a valuable tool for early AF detection. This study evaluated the frequency of irregular pulse rates suggestive of AF in subjects undergoing ambulatory BP monitoring (ABPM) and compared the characteristics of patients at low risk of presumed AF vs. those at high risk. ABPM recordings were obtained in 4419 subjects aged ≥65 years visiting 304 community pharmacies, with clinically validated automated monitors equipped with an algorithm for detecting possible AF episodes during BP measurement. Subjects with <30% of the readings suggestive of AF were categorized as having a low risk of AF, and those with ≥30% of readings were classified as high risk. A total of 531 subjects (12.0%) were categorized as having a high risk of AF, with the risk increasing with advancing age. Subjects at high risk of AF had lower average systolic BP, higher average diastolic BP and pulse rate (PR), increased BP and PR variabilities, and blunted sleep-associated reductions in BP and PR. In repeated recordings, the reliability of the AF detection algorithm per se was good (kappa 0.476, p = 0.0001; intraclass correlation coefficient 0.56, p = 0.0001). Simultaneous BP measurement and screening for potential AF by ABPM in elderly people in clinical practice may help improve BP control and the detection of subjects at high risk of AF. However, a finding of presumed AF must always be confirmed by an electrocardiogram (ECG).



Similar content being viewed by others
Data availability
The data underlying this article are available in the article and its online supplementary material.
References
Chugh SS, Havmoeller R, Narayanan K, Singh D, Rienstra M, Benjamin EJ, et al. Worldwide epidemiology of atrial fibrillation: a Global Burden of Disease 2010 Study. Circulation. 2014;129:837–47.
Hindricks G, Potpara T, Dagres N, Arbelo E, Bax JJ, Blomstrom-Lundqvist C, et al. 2020 ESC Guidelines for the diagnosis and management of atrial fibrillation developed in collaboration with the European Association for Cardio-Thoracic Surgery (EACTS): The Task Force for the diagnosis and management of atrial fibrillation of the European Society of Cardiology (ESC) Developed with the special contribution of the European Heart Rhythm Association (EHRA) of the ESC. Eur Heart J. 2021;42:373–498.
Stergiou GS, Kyriakoulis KG, Stambolliu E, Destounis A, Karpettas N, Kalogeropoulos P, et al. Blood pressure measurement in atrial fibrillation: review and meta-analysis of evidence on accuracy and clinical relevance. J Hypertens. 2019;37:2430–41.
Kollias A, Destounis A, Kalogeropoulos P, Kyriakoulis KG, Ntineri A, Stergiou GS. Atrial fibrillation detection during 24-hour ambulatory blood pressure monitoring: comparison with 24-hour electrocardiography. Hypertension. 2018;72:110–5.
Huppertz N, Lip GYH, Lane DA. Validation of the modified Microlife blood pressure monitor in patients with paroxysmal atrial fibrillation. Clin Res Cardiol. 2020;109:802–9.
Omboni S, Mancinelli A, Rizzi F, Parati G, Group TP. Telemonitoring of 24-hour blood pressure in local pharmacies and blood pressure control in the community: the templar project. Am J Hypertens. 2019;32:629–39.
European Parliament and Council. Regulation (EU) 2016/679 of the European Parliament and of the Council of 27 April 2016 on the protection of natural persons with regard to the processing of personal data and on the free movement of such data, and repealing Directive 95/46/EC (General Data Protection Regulation). http://data.europa.eu/eli/reg/2016/679/oj. Accessed 28 Oct 2021.
Ragazzo F, Saladini F, Palatini P. Validation of the Microlife WatchBP O3 device for clinic, home, and ambulatory blood pressure measurement, according to the International Protocol. Blood Press Monit. 2010;15:59–62.
Stergiou GS, Tzamouranis D, Nasothimiou EG, Karpettas N, Protogerou A. Are there really differences between home and daytime ambulatory blood pressure? Comparison using a novel dual-mode ambulatory and home monitor. J Hum Hypertens. 2010;24:207–12.
Fania C, Lazzaretto I, Fontana U, Palatini P. Accuracy of the WatchBP O3 device for ambulatory blood pressure monitoring according to the new criteria of the ISO81060-2 2018 protocol. Blood Press Monit. 2020;25:285–90.
Parati G, Stergiou G, O’Brien E, Asmar R, Beilin L, Bilo G, et al. European Society of Hypertension practice guidelines for ambulatory blood pressure monitoring. J Hypertens. 2014;32:1359–66.
Omboni S, Campolo L, Panzeri E. Telehealth in chronic disease management and the role of the Internet-of-Medical-Things: the Tholomeus(R) experience. Expert Rev Med Devices. 2020;17:659–70.
Omboni S, Palatini P, Parati G. Working Group on Blood Pressure Monitoring of the Italian Society of H. Standards for ambulatory blood pressure monitoring clinical reporting in daily practice: recommendations from the Italian Society of Hypertension. Blood Press Monit. 2015;20:241–4.
Mena L, Pintos S, Queipo NV, Aizpurua JA, Maestre G, Sulbaran T. A reliable index for the prognostic significance of blood pressure variability. J Hypertens. 2005;23:505–11.
Altman DG. Practical statistics for medical research. New York, NY: Chapman & Hall/CRC Press; 1999.
Koo TK, Li MY. A guideline of selecting and reporting intraclass correlation coefficients for reliability research. J Chiropr Med. 2016;15:155–63.
Schnabel RB, Sullivan LM, Levy D, Pencina MJ, Massaro JM, D’Agostino RB Sr., et al. Development of a risk score for atrial fibrillation (Framingham Heart Study): a community-based cohort study. Lancet. 2009;373:739–45.
Olbers J, Jacobson E, Viberg F, Witt N, Ljungman P, Rosenqvist M, et al. Systolic blood pressure increases in patients with atrial fibrillation regaining sinus rhythm after electrical cardioversion. J Clin Hypertens. 2019;21:363–8.
Wasmund SL, Li JM, Page RL, Joglar JA, Kowal RC, Smith ML, et al. Effect of atrial fibrillation and an irregular ventricular response on sympathetic nerve activity in human subjects. Circulation. 2003;107:2011–5.
Segerson NM, Sharma N, Smith ML, Wasmund SL, Kowal RC, Abedin M, et al. The effects of rate and irregularity on sympathetic nerve activity in human subjects. Heart Rhythm. 2007;4:20–26.
Olbers J, Gille A, Ljungman P, Rosenqvist M, Ostergren J, Witt N. High beat-to-beat blood pressure variability in atrial fibrillation compared to sinus rhythm. Blood Press. 2018;27:249–55.
Parati G, Torlasco C, Pengo M, Bilo G, Ochoa JE. Blood pressure variability: its relevance for cardiovascular homeostasis and cardiovascular diseases. Hypertens Res. 2020;43:609–20.
Khan AA, Lip GYH, Shantsila A. Heart rate variability in atrial fibrillation: the balance between sympathetic and parasympathetic nervous system. Eur J Clin Investig. 2019;49:e13174.
Stergiou GS, Kollias A, Destounis A, Tzamouranis D. Automated blood pressure measurement in atrial fibrillation: a systematic review and meta-analysis. J Hypertens. 2012;30:2074–82.
Clark CE, McDonagh STJ, McManus RJ. Accuracy of automated blood pressure measurements in the presence of atrial fibrillation: systematic review and meta-analysis. J Hum Hypertens. 2019;33:352–64.
Park SH, Choi YK. Measurement reliability of automated oscillometric blood pressure monitor in the elderly with atrial fibrillation: a systematic review and meta-analysis. Blood Press Monit. 2020;25:2–12.
Xie F, Xu J, Liu H, Li X, Wu Y, Su H. Different impact factors for accurate oscillometric blood pressure measurement between sinus rhythm and atrial fibrillation. J Hum Hypertens. 2021;35:785–90.
Acknowledgements
The authors wish to thank all the pharmacists for providing patient data for the present study.
Author contributions
All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this manuscript, take responsibility for the integrity of the work as a whole, and have given final approval to the version to be published. SO ran the analysis and drafted the manuscript. All authors critically revised and approved the final manuscript.
Funding
This is an investigator-initiated academic study. The study coordinator, the Italian Institute of Telemedicine (a not-for-profit organization), is the promoter and main sponsor of the study and made available its resources and facilities for conducting the trial. The work was also in part supported by the Karolinska Institutet Research Foundations (Stockholm, Sweden), which provided funding to TK, and the Swedish Society of Medicine, which provided funding to KL.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
SO is a scientific consultant of Biotechmed Ltd, provider of telemedicine services. All other authors declare no conflicts of interest regarding the publication of this paper.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Omboni, S., Ballatore, T., Rizzi, F. et al. 24-hour ambulatory blood pressure telemonitoring in patients at risk of atrial fibrillation: results from the TEMPLAR project. Hypertens Res 45, 1486–1495 (2022). https://doi.org/10.1038/s41440-022-00932-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-022-00932-1
- Springer Nature Singapore Pte Ltd.
Keywords
This article is cited by
-
Blood pressure in atrial fibrillation and in sinus rhythm during ambulatory blood pressure monitoring: data from the TEMPLAR project
Hypertension Research (2024)
-
Lifetime home BP-centered approach is the core from onset to aggravation of hypertension
Hypertension Research (2023)
-
New concept of pulse irregularity for the detection of atrial fibrillation during blood pressure measurement
Hypertension Research (2022)