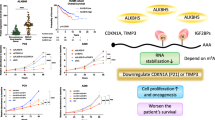
Abstract
Oncogenic KRAS mutations combined with the loss of the LKB1 tumor-suppressor gene (KL) are strongly associated with aggressive forms of lung cancer. N6-methyladenosine (m6A) in mRNA is a crucial epigenetic modification that controls cancer self-renewal and progression. However, the regulation and role of m6A modification in this cancer are unclear. We found that decreased m6A levels correlated with the disease progression and poor survival for KL patients. The correlation was mediated by a special increase in ALKBH5 (AlkB family member 5) levels, an m6A demethylase. ALKBH5 gain- or loss-of function could effectively reverse LKB1 regulated cell proliferation, colony formation, and migration of KRAS-mutated lung cancer cells. Mechanistically, LKB1 loss upregulated ALKBH5 expression by DNA hypermethylation of the CTCF-binding motif on the ALKBH5 promoter, which inhibited CTCF binding but enhanced histone modifications, including H3K4me3, H3K9ac, and H3K27ac. This effect could successfully be rescued by LKB1 expression. ALKBH5 demethylation of m6A stabilized oncogenic drivers, such as SOX2, SMAD7, and MYC, through a pathway dependent on YTHDF2, an m6A reader protein. The above findings were confirmed in clinical KRAS-mutated lung cancer patients. We conclude that loss of LKB1 promotes ALKBH5 transcription by a DNA methylation mechanism, reduces m6A modification, and increases the stability of m6A target oncogenes, thus contributing to aggressive phenotypes of KRAS-mutated lung cancer.
Similar content being viewed by others
Introduction
Recent global cancer statistics confirm that lung cancer is a commonly diagnosed malignancy and a leading cause of cancer-related deaths in both men and women1. Non-small cell lung cancer (NSCLC) accounts for about 85% of all lung cancers, and is not sensitive to most available treatment options. Approximately 10% of NSCLC cases involve concurrent KRAS mutation and LKB1 loss (KL)2,3,4. These cases are often more aggressive in terms of metastatic spread and drug resistance5,6,7,8,9 than those with neither mutation nor loss. However, the underlying molecular basis of these aggressive clinical behaviors is obscure.
Epigenetic modifications, including DNA/RNA methylation and histone methylation/ acetylation, have important roles in carcinogenesis10. KL cancer cells have higher levels of S-adenylmethionine (SAM) synthesis and DNA methylation11. SAM increases substrate supply to DNA and histone enzymes, such as DNMT1 and EZH2. Elevated SAM levels may also fuel RNA methylation12, suggesting that KL-mutations mediate a distinct form of epigenetic dysregulation. Nevertheless, reports are lacking on the regulation and role of RNA methylation in KL cancer cells.
N6-methyladenosine (m6A) mainly occurs at the consensus motif of GGm6ACC, and is the most prevalent internal chemical modification of mRNAs in eukaryotes13. Functionally, the reversible m6A modification of mRNAs is critical to cancer self-renewal and malignancy of several tumors14,15,16,17, including glioblastoma18, acute myeloid leukemia19, hepatocellular carcinoma20, and breast cancer21. In this regard, investigation of the landscapes and functions of m6A modification is an emerging research frontier known as RNA epigenetics or epitranscriptomics. AlkB homolog 5 (ALKBH5), a de-methyltransferase of m6A, is more highly expressed in most tissues than other m6A modulators8. ALKBH5 deficiency leads to compromised spermatogenesis in mice, and displays widespread mRNA methylation and global RNA instability22. Most recently, ALKBH5 was found to have oncogenic roles in glioblastoma and breast cancer cells17,20, suggesting it contributes to mRNA m6A methylation in cancer.
This study investigated the role and underlying mechanism of m6A modulation in aggressive KL mutant lung cancer cells. We found that loss of LKB1 activity promotes ALKBH5 transcription by a DNA methylation dependent mechanism. ALKBH5 demethylated and stabilized m6A modification target oncogenes in KRAS mutant cancers, which may influence how vulnerable the cancer is to therapy.
Results
Reduced m6A level was associated with aggressive KL lung cancer
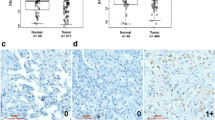
We first investigated the association between m6A RNA modification and aggressive KL lung cancer. IHC staining showed the reduced m6A level by loss of LKB1 in patients with KRAS mutation. And, the lowest of m6A level was found in KL tumor tissues when compared to wild type (WT), KRAS Wt; LKB1 Loss (L), or KRAS Mut; LKB1 Wt (K) tumor tissues (Fig. 1A, B). The m6A level was inversely correlated with TNM (Tumor, Node, and Metastasis) and clinical stage, whereas positively with tumor differentiation in KRAS mutant patients, but not in those with Kras wildtype (Fig. 1C). In addition, we found lower m6A level in K specimens that were null for thyroid transcription factor 1 (TTF1), a positive prognostic feature (Fig. 1D)23. Thus, reduced m6A modification is associated with aggressive KL lung cancer.
A, B Representation and quantification of LKB1 expression and m6A level in lung cancer patients. Data were mean ± SD. Bar = 50 µm. C Spearman correlation analysis of m6A level with the clinical characters of KRAS mutant or wild-type lung cancer patients. D The m6A level in lung cancer patients with TTF1 positive or negative. Boxes and whiskers represent the 10th to 90th percentiles, respectively; the median is the central line in each box. **P < 0.01, ***P < 0.001 by Student’s t-test. KRAS Mut; LKB1 Loss (KL); KRAS Mut; LKB1 Wt (K); KRAS Wt; LKB1 Loss (L) and KRAS Wt; LKB1 Wt (WT).
Loss of LKB1 enhanced ALKBH5 responses for m6A reduction in K lung cancer
To investigate how m6A is regulated in KL lung cancer, we compared the expression of proteins that act as the m6A writer complex (METTL3, METTL14, and WTAP) and erasers (ALKBH5 and FTO). IHC staining showed that only ALKBH5 expression was higher in KL than that of in K tumor tissues (Fig. 2A, B). ALKBH5 protein expression was negatively correlated with m6A level, in contrast to positive correlation with the tumor size, TNM and clinical stage in K lung cancer patients (Fig. 2C). However, LKB1 loss alone was not sufficient to change m6A level or ALKBH5 expression or their relationship with aggressive tumor phenotypes (Fig. S1 A–D).
A, B Quantification and representation of LKB1 and m6A modulators in KL relative to K lung cancer patients. Boxes and whiskers represent the 10th to 90th percentiles, respectively; the median is the central line in each box. Bar = 50 µm. C Spearman correlation analysis of ALKBH5 expression with the KRAS mutant lung cancer pathological characters. D Venn diagram showing the differentially expressed genes (DEGs) of LKB1, m6A modulators, and readers between KL and K lung cancer. E Kaplan–Meier survival curve of patients with high and low ALKBH5 mRNA expression from the TCGA dataset. F Global m6A level regulation by LKB1 in lung cancer cell lines. G Western blot showing the LKB1 and ALKBH5 protein expression. H Co-immunofluorescence staining for LKB1 and ALKBH5 in A549 cells. Arrows show LKB1 positive and ALKBH5 negative cells. I LKB1 and m6A co-staining by LKB1 and/or ALKBH5 overexpression in A549 cells. Arrows show cells of LKB1 positive and m6A with strong (Second panel) or weak (Forth panel) intensity. Data were mean ± SD in F (n = 5). *P < 0.05 (Student’s t-test). Si-CN, SiRNA-A; OE-CN, OE-c-Flag pcDNA3; OE, overexpression. KRAS Mut; LKB1 Loss (KL); KRAS Mut; LKB1 Wt (K).
To confirm observations of clinical specimens, we screened for the differential expressions of m6A mediators and readers based on database queries. Analysis of TCGA, MTB8,24, and CCLE databases revealed that ALKBH5 mRNA expression was consistently higher in KL cancer tissues or cells, and negatively correlated with LKB1 expression (Figs. 2D and S2A–D). Furthermore, elevated ALKBH5 expression correlated with poor prognosis for patients with KRAS mutation (Fig. 2E). Additionally, ALKBH5 had the highest basal mRNA expression in human and mouse lung cancer tissues and cell lines (Fig. S2A–C). Taken together, these findings indicate that ALKBH5, a major regulator of m6A modification, contributes to aggressive phenotypes of KL lung tumors.
To investigate whether LKB1 loss affects ALKBH5 and m6A modification, we screened several lung cancer cell lines and categorized them based on KRAS mutation and LKB1 expression status. A549KL (KRASmut/LKB1loss), H1792K (KRASmut/LKB1high), H1299 (KRASwt/LKB1high), and H1703 (KRASwt/LKB1low) were selected from each category for further analyses (Fig. S3A). We then generated the loss of LKB1 function by siRNA-LKB1-transfection in H1299 and H1792 cells, while gain-of-function by LKB1 overexpression in H1703 and A549 cells. As expected, LKB1 expression positively regulated m6A levels in cells with KRAS mutation, but not with KRAS wild type (Fig. 2F). Consistent with clinical data, western blot and qRT-PCR assays showed that ALKBH5 was also the only m6A modulator negatively regulated by LKB1 in KRASmut cells, but was unaffected in KRASwt cells (Figs. 2G and S3B–E). These observations were supported by immunofluorescence staining that demonstrated negligible ALKBH5 signal in LKB1 overexpression A549 cells (Fig. 2H). Exogenous ALKBH5 expression blocked m6A staining in the presence of LKB1 (Fig. 2I). Furthermore, LKB1 expression negatively correlated with ALKBH5 expression was also found in KRAS-mutated pancreatic and colorectal cancer cell lines (Fig. S4A–E). Therefore, LKB1 expression directly affects the global m6A levels via ALKBH5 in KRAS-mutated cancer cells.
ALKBH5 negatively regulated LKB1 role for lung cancer cell proliferation and migration
Next, we explored functional relationships between LKB1 and ALKBH5 in KRAS mutant lung cancer cells. First, we established the transient ALKBH5 and/or LKB1 knockdown models in H1792 cells, as well as overexpression in A549 cells (Fig. 3A). As expected, ALKBH5 could fully release LKB1 repressed m6A levels in both cell lines (Fig. 3B, C). Functionally, ALKBH5 knockdown significantly inhibited cell proliferation, as shown by decreased colony formation in LKB1-silenced H1792 cells (Fig. 3D). We observed similar for H1792 cell migration in the transwell assay (Fig. 3E). Conversely, ALKBH5 overexpression promoted cell proliferation and migration in LKB1-transfected A549 cells (Fig. 3F, G). Thus, ALKBH5 negatively regulated LKB1 role for cell proliferation and migration in KRAS mutant cells.
A Western blot analysis shown that LKB1 and ALKBH5 were successfully knocked down in H1792 cells and overexpressed in A549 cells. B, C The measurement of global m6A by ELISA assay in H1792 (B) or A549 (C) cells, respectively. The colony formation ability (D) and cell migration (E) were reduced at both of basal level and LKB1 silenced level by ALKBH5 knockdown in H1792 cells, respectively. The reversible effect was found at both of basal level and LKB1 overexpressed level by ALKBH5 transfected in A549 cells using colony formation (F) and transwell assay (G). Data were mean ± SD (n = 5) and were analyzed by one-way ANOVA, followed by Bonferroni’s multiple comparison test for B–G. *P < 0.05. Bar = 5 mm in D and F; Bar = 50 µm in E and G.
Loss of LKB1 upregulated ALKBH5 via DNA hypermethylation in KRAS mutant cancer cells
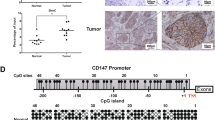
We then explored how LKB1 regulates ALKBH5 through DNA methylation. Consistent with previous studies in pancreatic ductal epithelial cells11, LKB1 alterations also negatively regulated the global 5mC DNA methylation in KRAS mutant lung cancer cells (Fig. 4A) but had no effect in KRAS wild-type cells. Specifically, ALKBH5 gene DNA methylation positively correlated with ALKBH5 mRNA expression in KRAS mutant lung, and colorectal cancer cell lines, based on the CLLE database (Fig. S5A–D). Subsequent treatment with 5-azacytidine (5-aza), an inhibitor of DNA methylation, reduced ALKBH5 mRNA and protein expression in a dose-dependent manner in H1792 and A549 cells, independent of LKB1 status (Fig. 4B–D). Based on ChIP-sequence analysis from the ENCODE database, we identified a single putative transcriptional repressor, CTCF (CCCTC-binding factor) and several activators, including H3K4me1, H3K4me2, H3K4me3, H3K9ac, and H3K27ac, on the ALKBH5 gene core promoter in A549 cells (Fig. S6). Interestingly, the CTCF peak region was colocated in the CpG island of ALKBH5 promoter (Fig. 4E). Further analysis by MeDIP assay indicated 5mC-methylation on the CTCF peak region was decreased with 5-aza treatment or exogenous LKB1-transfection in A549 cells (Fig. 4F). Lastly, bisulfite sequencing confirmed decreased DNA methylation on the CTCF peak region in 5-aza-treated or LKB1 overexpressed A549 cells (Fig. 4G, H). Thus, the data indicate that LKB1 loss induces DNA hypermethylation, thereby controlling ALKBH5 expression in KRAS mutant cancer cells.
A 5mC DNA methylation was detected by ELISA assay. Data as mean ± SD (n = 5), *P < 0.05 (Student’s t-test). B–D Representation and quantification of ALKBH5 expression at protein (B, C) and mRNA levels (D) in response to 5-aza treatment in A549 and H1792 cells for 72 h. Error bars, SD (n = 4 for WB; n = 5 for qRT-PCR), *P < 0.05 as compared their corresponding controls (2-way ANOVA with Bonferroni multiple comparison post hoc test). E CTCF peak located in the CpGs Island of human ALKBH5 gene promoter. Bottom panel: the Methprimer histogram of CpG islands (CpGI, red box) and CpG dinucleotides (red vertical lines) in the regulatory region of ALKBH5. F MeDIP assay showing the decrease of 5mC enrichment on the ALKBH5 promoter containing CTCF motif fragment by treated with 5-aza and LKB1 overexpression. G, H Representative bisulfite sequencing of four clones (G) and quantification of DNA methylation (H) of ALKBH5 promoter containing CTCF motif. n = 4 in F and H, mean ± SD, * P < 0.05 vs. A549 DMSO by one-way ANOVA followed by Tukey’s test in F and H. Si-CN, Si-RNA-A. OE-CN, OE-c-Flag pcDNA3. OE overexpression.
DNA hypermethylation of the CTCF motif is critical for ALKBH5 upregulation
To determine whether CTCF directly represses ALKBH5, we used western blot and RT-qPCR. We found that silencing CTCF increased ALKBH5 protein and mRNA expression, and also rescued ALKBH5 repression by LKB1 overexpression (Fig. 5A–C). We next generated serial deletions, including CTCF motif deletion constructs based on the human ALKBH5 promoter, for the luciferase reporter assay. The CTCF-containing construct had lower ALKBH5 promoter activity than constructs that lacked the motif (Fig. 5D). Notably, CTCF motif deletion increased ALKBH5 promoter activity to levels similar to those in constructs without the CTCF motif. This evidence suggests that CTCF directly represses ALKBH5 transcriptional activity.
A–C Representative images and quantification of CTCF and ALKBH5 protein expression by WB and qRT-PCR in A549 cells with LKB1 overexpression and/or CTCF knockdown for 48 h. Error bars, SD (n = 4 for WB; n = 5 for qRT-PCR), *P < 0.05 vs. Si-CN or OE-CN (one-way ANOVA with Bonferroni multiple comparison post hoc test). D Luciferase reporter assay of A549 cells transfected with pGL3-basic constructs containing serial LKBH5 promoters or deletion of CTCF peak fragment. n = 8/group, mean ± SD. * P < 0.05 by one-way ANOVA followed by Tukey’s test. E Reduction of ALKBH5 Luc:-1168 bp wild-type (WT) construct activities by treatment of 5-aza or LKB1 overexpression in A549 cells, but not for ALKBH5 Luc:-1168 bp deletion (Del). Data as mean ± SD (n = 5), *P < 0.05 (Student’s t-test). F ChIP-qPCR showing that the ALKBH5-CTCF peak region was occupied by the suppressor of CTCF and activators of histone modulators in A549 cells. G–J ChIP-qPCR analyses of 5-aza treated or LKB1 overexpressed A549 cells. n = 5/group, mean ± SD. *P < 0.05 vs. IgG in F, vs. A549-DMSO in G–J by one-way ANOVA followed by Tukey’s test.
Next, we found that inhibition of DNA methylation by 5-aza treatment or by LKB1 overexpression reduced ALKBH5 promoter activity on the CTCF motif-containing construct, but had no effect on CTCF motif-deficient construct (Fig. 5E). Further ChIP-qPCR analysis indicated that histone activators, such as H3K4me1, H3K4me2, H3K4me3, H3K9ac, and H3K27ac, occupy the ALKBH5 gene promoter (Fig. 5F), consistent with ChIP-seq results (Fig. S6). Interestingly, 5-aza treatment or LKB1 overexpression promoted CTCF enrichment on ALKBH5, and also partially prevented enrichment of H3K4me3, H3K9ac, and H3K27ac (Fig. 5H–J). Therefore, loss of LKB1 promoted DNA hypermethylation in the CTCF peak region, thus preventing CTCF binding and releasing repression of ALKBH5 in KRAS mutant cells.
ALKBH5 demethylation of m6A increased expression and stability of SOX2, SMAD7, and MYC in a YTHDF2-dependent pathway
To identify downstream targets of ALKBH5-mediated m6A modification in lung cancer, we overlapped 2605 genes using the canonical m6A motif-enriched gene stop codon region based on m6A-sequence in A549 cells (16) (Fig. S7A). Gene ontology analysis revealed that the 2605 genes were significantly enriched in gene transcription regulation, mRNA splicing, cell cycle, and mRNA stability (Fig. S7B). KEGG pathway analysis revealed that the overlapping genes were closely associated with Hippo and TGF-β pathways (Fig. S7C). Using qRT-PCR, we confirmed that 45.2% (14/31) of Hippo-Yap pathway genes were directly regulated by ALKBH5 (Fig. S7D, E). Western blot assay further confirmed that ALKBH5 regulated SOX2, SMAD7, and MYC proteins in A549 and H1792 cells (Fig. 6A, B).
A, B Representative western blotting and quantification of SOX2, SMAD7, MYC, and ALKBH5 protein. Data as mean ± SD (n = 4). C Mutation of m6A site or ALKBH5 overexpression released the SOX2, SMAD7, and MYC gene posttranscriptional repression by LKB1 in A549 cells (n = 4). D m6A-RIP analysis demonstrated that SOX2, SMAD7, and MYC were subjected to ALKBH5-mediated m6A modifications (n = 5). E YTHDF2-RIP-qPCR shown that YTHDF2 could occupy m6A sites of SOX2, SMAD7, and MYC, which was mediated by ALKBH5 (n = 4). F qRT-PCR was performed to indicate that knockdown of YTHDF2 significantly upregulated SOX2, SMAD7, and MYC gene mRNA expression at basal level, LKB1 overexpressed or ALKBH5 silenced A549 cells (n = 6). Data as mean ± SD. *P < 0.05 by one-way ANOVA followed by Bonferroni multiple comparison post hoc test for B–F. Si-CN, Si-RNA-A. OE-CN, OE-c-Flag pcDNA3. OE overexpression.
To investigate m6A modifications on SOX2, SMAD7, and MYC mRNA, we used firefly luciferase assay (Fig. 6C). We found their activities were significantly less than those of their mutant reporters, indicating that m6A represses gene activity. Moreover, overexpression of ALKBH5 increased luciferase activities of three m6A WT gene reporters, and also rescued the repressive activity mediated by LKB1-transfection. However, we observed no such effects for m6A mutant gene-fused reporters. Our m6A-RIP-qPCR assay showed significantly higher accumulation of m6A at mRNA fragments of all three genes than for the IgG control. However, this m6A enrichment was reduced by ALKBH5 overexpression. Also, ALKBH5 upregulation inhibited the increased m6A occupancy caused by LKB1 overexpression (Fig. 6D). Given that ALKBH5 overexpression or knockdown did not change the pre-mRNAs of SMAD7 and MYC (Fig. S8A–D), we predicted m6A reader protein YTHDF2 regulated their mRNA stability. Interestingly, actinomycin-D induced degradation of SMAD7, SOX2, and MYC mRNAs was partially prevented by silencing YTHDF2 in both A549 and H1792 cells. (Fig. S8E–J). RIP-qPCR assay showed that YTHDF2 also occupied SMAD7, SOX2, and MYC m6A regions, and this enrichment increased in the absence of ALKBH5 (Fig. 6E). Furthermore, YTHDF2 silencing rescued their gene expression upon LKB1 overexpression or ALKBH5 knockdown (Fig. 6F). Thus, ALKBH5-m6A-YTHDF2 signaling prevented SOX2, SMAD7, and MYC mRNA decay.
Confirmation of an axis of “LKB1-DNA methylation-ALKBH5-m6A” in clinical KRAS-mutated lung cancer patients
Next, we validated the underlying regulation of m6A by LKB1 using a panel of clinically relevant lung adenocarcinoma specimens. IHC staining showed that LKB1 loss increased the global 5-mC DNA methylation in lung cancer tissues with KRAS mutations, but not in tissues with WT KRAS (Fig. 7A). Similar pattern was found for both DNA methylation and mRNA expression of ALKBH5 (Fig. 7B, C). ALKBH5 protein expression negatively correlated with global m6A level, as well as the m6A levels for SOX2, SMAD7, and MYC genes only in KRAS mutant tissues (Fig. 7D–F). Furthermore, m6A levels of these three genes were negatively correlated with their mRNA expression (Fig. 7G–I). Notably, the protein levels of SOX2, SMAD7, and MYC were significantly increased by loss of LKB1 and correlated with ALKBH5 expression in KRAS mutant tissues (Fig. 7J, K). Thus, our clinical data further confirmed that LKB1 loss increased the DNA methylation and expression level of ALKBH5, which resulting in the demethylation of m6A modification on SOX2, SMAD7, and MYC, and maintaining their expression for KRAS mutant lung cancer.
A Representative immunostaining images and quantification of 5mC DNA in lung cancer patients with KW and KM. Boxes and whiskers represent the 10th to 90th percentiles, respectively; the median is the central line in each box. Bar = 50 µm. B, C High levels of ALKBH5 DNA methylation and mRNA expression in cases of LKB1 loss compared with that of LKB1 positive expression in KM patients. D–F The correlation of ALKBH5 protein with the global m6A modification (D), m6A levels of SOX2, SMAD7, and MYC genes (E, F) in KM and KW groups. G–I Negative correlations of the m6A enrichment with mRNA expressions of SOX2, SMAD7, and MYC in KM group. J Representative immunostaining images and quantification of SOX2, SMAD7, and MYC in KM group with LKB1 loss or not. K The positive correlations of ALKBH5 with SOX2, SMAD7, and MYC protein expression in KM group. Data as mean ± SD. KRAS mutation (KM). KRAS wild-type (KW). *P < 0.05 by one-way ANOVA followed by Bonferroni multiple comparison post hoc test for A, B, and C. Student’s t-test for J.
Discussion
Our findings describe m6A RNA modification by 5mC-DNA mechanism in KL tumors that supports tumorigenic growth and progression (Fig. 8). Here, we report that reduced m6A RNA modification increased stability and expression of critical oncogenes and contributed to aggressive cancer phenotypes. Loss of LKB1 specifically enhanced ALKBH5 expression and reduced m6A levels in KRAS-mutated cells. LKB1 inactivation could increase the 5-mC DNA methylation of the ALKBH5 promoter, which prevents CTCF binding and releases ALKBH5 suppression. Subsequently, reduced “m6A-YTHDF2” signaling promoted the expression and stability of critical tumor oncogenes, such as SOX2, SMAD7, and MYC. Our study indicates that LKB1 loss reduces m6A modification by upregulating ALKBH5, which contributes to aggressive tumor progression and poorer outcomes for KL lung cancer.
Loss of LKB1-induced DNA hypermethylation, which prevents CTCF binding on the ALKBH5 gene promoter, maintains ALKBH5 expression, and further represses global RNA methylation. Oncogenic SMAD7, SOX2, and MYC are crucial targets of m6A meditated by LKB1 deficiency, and are involved in KRAS mutation lung cancer progression.
Aberrant global m6A abundance has been increasingly reported in human cancers, and associates with cancer progression and clinical outcome25. Interestingly, m6A hypomethylation was reported in glioblastoma, bladder cancer, endometrial cancer26, melanoma, or breast carcinoma, whereas, m6A hypermethylation was found in gastric cancer and hepatocellular carcinoma27. Writing and erasing proteins regulate m6A levels, which enable the binding of m6A reader proteins and initiate a series of biological functions. For example, ALKBH5 demethylates m6A mRNAs, which modulates mRNA splicing, export, and stability. ALKBH5 deficiency leads to aberrant spermatogenesis and apoptosis in mouse testes, likely through regulating genes associated with the p53 network22. ALKBH5 often exerts an oncogenic role in GBM, pancreas, cervical, and breast cancer, but acts a tumor-suppressor in leukemia25. This two-sided role of ALKBH5, might relate with the complex and diverse function of m6A modification, which not only promotes the translation of related mRNAs but also reduces the mRNAs stability by binding with different reader proteins13,14,15,16. Thus, It would be important to determine how critical role of m6A and its regulator in each type of cancer.
Limited literature is available to explain how m6A regulators could be modulated in cancers, although many studies have described roles for m6A regulators in cell fate and carcinogenesis20,28,29. This study identifies ALKBH5 as a functional target gene of 5-mC DNA methylation, which controls m6A RNA modification. Notably, ALKBH5 is one of the top five 5-mC DNA methylation biomarkers that helped distinguish patients with metastatic-lethal prostate cancer30, suggesting that DNA methylation of ALKBH5 may be a prognostic indicator. We also identified CTCF as an effective transcriptional suppressor that was highly sensitive to global 5-mC DNA methylation and required for ALKBH5 repression. Similarly, we previously showed that DNA hypomethylation facilitated CTCF binding to and suppression of hTERT expression in human endothelium31. Recent studies show 5-mC DNA hypermethylation facilitated tumorigenesis in KRAS/LKB1 co-mutated cancer11. LKB1 inactivation causes DNA hypermethylation and histone methylation, which facilitates immune escape in KL-mutated lung cancer and represses anti-oncogenic STING32. Consistent with those previous findings, our work indicates that oncogenic ALKBH5 is another target of LKB1 by a similar mechanism. Thus, loss of LKB1 reduces m6A modification also might via the linking of 5mC-DNA and histone modification in KL cancer.
Consistent with previous studies, our observations indicate that ALKBH5 is a lung cancer oncogene because it promoted cell proliferation and migration18,21. Increased ALKBH5 expression predicted poor survival in our analysis. Moreover, we identified three critical oncogenes, SOX2, SMAD7, and MYC, as targets of ALKBH5-mediated m6A modification. Mechanistically, LKB1 loss or ALKBH5 overexpression increased SAMD7, SOX2, and MYC stability via a YTHDF2-dependent mechanism. This result is supported by previously reported PAR-CLIP-Seq data in a Hela cell line13. YTHDF2-induced decay of m6A modified genes may be a common pathway across cell types. We also found that YTHDF1 occupied and promoted SAMD7 or MYC mRNA translation in an m6A-dependent manner33. Thus, it would be interesting to identify ALKBH5 targets by comparing the proteomic changes based on the differential level of ALKBH5.
Notably, LKB1 regulation of ALKBH5 via 5mC-DNA was not limited to KRAS mutant lung cancer, but extended to pancreatic and colorectal cancer, which are the top three causes of cancer death in the United States34. Aggressive lung tumorigenesis, tumor progression, and poor prognosis were observed in mice with Kras mutation combined with Lkb1 inactivation8. This tumor type is largely resistant to both standard-of-care treatments like docetaxel and combination treatment with a MEK inhibitor5,35. Co-mutations were also associated with an inert tumor immune microenvironment and poor clinical response to immune checkpoint blockade36,37,38. Thus, understanding molecular mechanisms may improve therapeutic strategies for cancer with KRAS and LKB1 co-mutations. Screening chemicals that may regulate m6A formation or removal is an effective approach for developing tumor therapeutics. For example, R-2HG, an ALKBH5 and FOT inhibitor, inhibits leukemia cell growth and induces apoptosis in mice39. m6A-YTHDF2 inactivity contributes to melanoma progression by enhancing the expression and stability of key immune checkpoint factors, including PD-1, CXCR4, and SOX1040. This implies that YTHDF2 modulation could be combined with an anti-PD-1/PD-L1 blockade to improve anticancer immunotherapy. In support of this idea, we identified the ALKBH5-m6A-YHTDF2 axis as a targetable molecular pathway to treat this aggressive cancer.
In conclusion, our results uncover the epigenetic reprogramming of DNA methylation and m6A RNA methylation during KRAS mutation/LKB1 loss induced lung carcinogenesis. We also reveal that histone modification was necessary for ALKBH5 upregulation, which in turn controlled m6A RNA modification. Our findings and other recent reports10,14,15,17 highlight the important linking of the global DNA methylation and m6A RNA modification in cancer. This epigenetic reprogramming indicates new therapeutic approaches to tumorigenesis, especially for the lung cancer with dual KRAS mutation/LKB1 loss.
Materials and methods
Human lung cancer specimens and cell lines
We randomly obtained fresh and paraffin-embedded lung adenocarcinoma specimens from 72 patients who underwent tumor resection surgery between January 2016 and September 2019 at the Cancer Hospital of Harbin University Medical College, China. Two pathologists performed blinded histological confirmation by hematoxylin and eosin (H&E) staining. KRAS mutations were detected by Cobas KRAS Mutation Test, which could detect 19 mutation sites based on a real-time PCR method. Exclusion criteria were patients who had received preoperative chemotherapy, radiation therapy, or had multiple metachronous or metastatic lesions. Clinical characteristics of patients were retrospectively analyzed and summarized in Table S1. We collected all clinical samples with informed consent according to Health Insurance Portability and Accountability Act (HIPAA)-approved protocols. This study was approved by the ethical review board of Cancer Hospital of Harbin University Medical College on October 22, 2018. All of the patients were given and accepted informed consent form prior to their enrollment.
MRC-9, H1299, H1650, H1703, H1795, H1792, A549, DLD-1, SW480, Panc-1, and MIA PaCa-2 cell lines were purchased from ATCC, USA. Cells were cultured in medium according to the manufacturer’s instructions and grown in a humidified incubator at 5% CO2. All cell lines were authenticated and confirmed negative for mycoplasma contamination by providers.
RNAi and protein overexpression transfection
To knockdown endogenous gene expression, we purchased si-RNAs targeting human LKB1 (sc-35816), ALKBH5 (sc-93856), YTHDF2 (sc-78661), and CTCF (sc-35124) from Santa Cruz and transiently transfected these si-RNAs into lung cancer cells for 48 h using Lipofectamine RNAiMAX (Invitrogen). We ordered LKB1 (#8590) and ALKBH5 (#38073) overexpressing vectors from Addgene and transfected them into human cancer cells using Lipofectamine 2000 (Invitrogen) for 24 h. Si-RNA-A (sc-37007, Santa Cruz) and c-Flag pcDNA3 (Plasmid #20011, Addgene) were served as transfect controls for genes knockdown and overexpression, respectively.
Quantitative reverse transcription polymerase chain reaction (qRT-PCR)
We extracted total cellular and tissue RNA using TRIzol Reagent (Thermo Fisher Scientific, USA) and used 1 µg total RNA for reverse transcription using the iScript™ cDNA Synthesis Kit (Bio-Rad). qRT-PCR was performed with 2× SYBR Green qPCR Master Mix (Bimake, USA) with a CFX96 Touch™ Real-Time PCR detection system (Bio-Rad Inc. USA). We calculated the relative gene expression using the comparative CT method and β-actin RNA sequences as a control. Primer sequences were listed in Table S2.
Western blot analysis
We lysed total protein from treated cells using RIPA buffer (Cell Signaling Technology) supplemented with Protease Inhibitor Cocktail (Thermo Fisher; 78430). Western blotting was performed as previously described41, and the primary antibodies included GAPDH (Santa Cruz, sc-137179), LKB1 (Santa Cruz, sc-32245), ALKBH5 (Proteintech, 16837-1-AP), CTCF (Santa Cruz, sc-271474), METTL3 (Abcam, ab195352), METTL14 (Abcam, ab220030), FTO (Abcam, ab126605), WTAP (Proteintech, 60188-1-Ig), SOX2 (Cell signaling, #3579), SMAD7 (Santa Cruz, sc-11392), and MYC (Cell signaling, #13987). We performed densitometric analyses of band intensity using ImageQuant TL 8.2 image analysis software (GE Healthcare Life Sciences, USA) and GAPDH was as an internal control.
Immunohistochemistry (IHC) staining
IHC analysis of paraffin-embedded lung cancer tissues containing primary tumors and matched normal lung tissues as previously described42,43. In brief, we de-paraffinized and rehydrated human tissue sections to retrieve antigens, and then incubating in 1% hydrogen peroxide. After blocking, we applied primary antibodies to the slides at 1:500 (anti-LKB1, METTL3, METTL14, WTAP, and FTO antibodies), 1:200 (anti-ALKBH5 antibody), and 1:1000 (anti-m6A and 5-mC antibody) dilutions and incubated at 4 °C overnight. We stained slides with EnVision+ Dual Link System-HRP (Dako) for 1 h at room temperature. Images of stained cells in four random fields were captured by using an optical microscope (Olympus, Japan). Relative protein expression was evaluated by a Histoscore (H-score) system. The results were evaluated by two independent pathologists.
Immunofluorescence staining
We performed immunofluorescence staining on cultured A549 cells transfected with siRNA or pcDNA. After treatment, we fixed cells with 4% paraformaldehyde (PFA), permeabilized with 0.3% Triton/phosphate-buffered saline (PBS), blocked in 1% bovine serum albumin (BSA), and then incubated with the indicated primary antibody for LKB1 (Santa Cruz, sc-32245), ALKBH5 (Proteintech, 16837-1-AP), or m6A (Synaptic Systems, 202111) overnight at 4 °C. The next day, cells were washed and incubated with secondary antibody conjugated to Alexa Fluor 555 (donkey anti-rabbit, Invitrogen) for 1 h at room temperature. We used DAPI (Sigma) staining to label nuclei. Fluorescence was observed under a Leica SP8 confocal laser scanning microscope.
Luciferase reporter assays
For the ALKBH5 promoter reporter assay, we generated serial ALKBH5 promoter reporters by PCR amplification and inserted into pGl3-basic plasmid, as we previously reported41. We deleted the CTCF region using the Q5 Site-Directed Mutagenesis Kit (NEB) per the manufacturer’s protocol. Firefly luciferase activity was used to evaluate the effect of m6A modification on SOX2, SMAD7, and MYC activation. We used the pmirGLO Dual-Luciferase miRNA target expression vector from Promega to construct the reporter plasmid, which contained both a firefly luciferase and a Renilla luciferase. We constructed mutant three reporter plasmids by replacing the adenosine bases within the m6A consensus sequences with cytosine. All constructs were confirmed by Sanger sequencing. Nucleotide sequences of primers were in Table S2. A549 cells grown in 96-well plates were transfected with reporter vectors and SV-40-Renilla-Luc in the presence of Lipofectamine 2000 Reagent (Invitrogen). Luminescence was measured with the Dual-Luciferase Reporter Assay System (Promega). We performed experiments for each vector as biological triplicates with six technical repeats.
Global 5-mC and m6A measurement
We measured total cellular and tissue 5-mC in DNA and m6A in mRNA levels by the MethylFlash Methylated DNA 5-mC Quantification Kit (Colorimetric) and EpiQuik m6A RNA Methylation Quantification ELISA kit (Colorimetric) (Epigentek Group Inc.), respectively. Total genomic DNA and RNA were isolated using the PureLink Genomic DNA Mini Kit and TRIzol Reagent (Thermo Fisher Scientific). We used 200 ng of DNA or RNA for additional global 5-mC and m6A measurement according to the manufacturer’s instructions. Measurements were performed in triplicate.
Bisulfite genome sequencing (BGS)
For DNA methylation analysis, we used BGS method, as previously described31,44. Briefly, 500 ng of genomic DNA was bisulfite converted using the BisulFlash DNA Modification Kit (Epigentek) following the manufacturer’s instructions. We amplified the fragment containing CTCF peak region of ALKBH5 promoter using primers listed in Table S2. PCR products were purified and cloned into a pCR4 TOPO vector using the TOPO TA Cloning Kit (Thermo Fisher Scientific, Rockford, IL, USA). We isolated and sequenced plasmid DNA from ten randomly selected clones (Genewiz, Piscataway, NJ, USA).
Methylated DNA immunoprecipitation (MeDIP) analysis
To confirm BGS results, we performed MeDIP using the Methylamp Methylated DNA Capture Kit (EpiGentek) according to the manufacturer’s instructions. Briefly, we extracted cellular and tissue chromatin DNA and digested to ~150–700 bp using a micrococcal nuclease (CST). The fragmented DNA was immunoprecipitated with anti-5-mC (Abcam, ab10805) at room temperature for 2 h. After washing and purifying the DNA, we quantified the methylation status using qPCR. Primers were listed in Table S2.
m6A-RNA Immunoprecipitation (m6A-RIP)
We extracted total RNA from treated A549 cells or tumor tissues, and incubated with DNase according to the TURBO DNA-free TM Kit (Thermo Fisher) protocol to avoid DNA contamination. Then, we chemically fragmented 1 µg/µl RNA and incubated with m6A antibody to immunoprecipitate according to the standard protocol for the EpiMark N6-Methyladenosine Enrichment Kit (NEB). Enrichment of m6A containing mRNA was then analyzed using qRT-PCR. Primers targeting m6A-enriched regions of SOX2, SMAD7, and MYC were listed in Table S2.
Cell proliferation and migration assay
For cell colony formation assay, A549 or H1792 cells were transfected with siRNA or pcDNA for 24 h and seeded into 6-well plates (500/well). After 1 week, we fixed formed colonies and stained with 0.1% crystal violet in 20% methanol, and counted colonies consisting of at least 50 cells. For the migration assay, we resuspended 5 × 105 cells in Opti-MEM Reduced Serum Media (Invitrogen) and seeded into the upper chamber of a transwell apparatus (8.0 μm, BD Biosciences), and added complete medium to the bottom chamber to provide chemoattractants for migration. To count migrated cells, we captured images of stained cells in five random fields by using an optical microscope (Olympus, Japan) and counted samples in triplicate.
Bioinformatics assay from database
The differentially expressed genes (DEGs) of m6A modulators (METTL3, METTL14, WTAP, FTO, and ALKBH5) and readers (YTHDF1, YTHDF2, YTHDF3, YTHDC1, and YTHDC2) between KL and K-lung cancer cell lines or tissues from the databases of the Cancer Genome Atlas (TCGA, https://portal.gdc.cancer.gov/), Mouse Tumor Biology (MTB, http://tumor.informatics.jax.org/mtbwi/index.do), and Cancer Cell Line Encyclopedia (CCLE, https://portals.broadinstitute.org/ccle/home).
m6A-seq data analysis
Based on the NCBI-GEO database (GEO: GSE76367), we determined the number of m6A-seq fragments mapped to each gene using HT-Seq. We overlapped the core m6A peaks based on functional m6A signal enriched around the stop codon (−5 to +5 kbp) of mRNAs and canonical m6A peaks45,46. Then, core m6A peaks were subjected to functional enrichment analysis by Ingenuity Pathway Analysis (IPA) (http://www.qiagen. com/ingenuity) and KEGG pathway (https://www.genome.jp/kegg/).
Statistics
All experiments were repeated at least four times, unless otherwise stated in the figure legend. We performed statistical analyses using the SPSS v20.0 software (SPSS Inc., Chicago, IL), and used Student’s t-test (two-tailed) or one-way ANOVA analysis followed by Tukey’s, Sidak’s, or Bonferroni test to assess statistical significance between or among groups. We calculated the survival rate using the log-rank (Mantel–Cox) test. Normality was assumed and variance was compared between or among groups. All numerical data were presented as mean ± standard deviation (SD) and a p value of <0.05 was considered significant.
References
Bray, F. et al. Global cancer statistics 2018, GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J. Clin. 68, 394–424 (2018).
Sanchez-Cespedes, M. et al. Inactivation of LKB1/STK11 is a common event in adenocarcinomas of the lung. Cancer Res. 62, 3659–3662 (2002).
Matsumoto, S. et al. Prevalence and specificity of LKB1 genetic alterations in lung cancers. Oncogene 26, 5911–5918 (2007).
Skoulidis, F. et al. Co-occurring genomic alterations define major subsets of KRAS-mutant lung adenocarcinoma with distinct biology, immune profiles, and therapeutic vulnerabilities. Cancer Disco. 5, 860–877 (2015).
Calles, A. et al. Immunohistochemical loss of LKB1 is a biomarker for more aggressive biology in KRAS-mutant lung adenocarcinoma. Clin. Cancer Res. 21, 2851–2860 (2015).
Gilbert-Ross, M. et al. Targeting adhesion signaling in KRAS, LKB1 mutant lung adenocarcinoma. JCI Insight 2, e90487 (2017).
Skoulidis, F. et al. STK11/LKB1 mutations and PD-1 inhibitor resistance in KRAS-mutant lung adenocarcinoma. Cancer Disco. 8, 822–835 (2018).
Ji, H. et al. LKB1 modulates lung cancer differentiation and metastasis. Nature 448, 807–810 (2007).
Wang, Y. et al. Mutant LKB1 confers enhanced radiosensitization in combination with trametinib in KRAS-mutant non-small cell lung cancer. Clin. Cancer Res. 24, 5744–5756 (2018).
Michalak, E. M., Burr, M. L., Bannister, A. J. & Dawson, M. A. The roles of DNA, RNA and histone methylation in ageing and cancer. Nat. Rev. Mol. Cell Biol. 20, 573–589 (2019).
Kottakis, F. et al. LKB1 loss links serine metabolism to DNA methylation and tumorigenesis. Nature 539, 390–395 (2016).
Stojkovic, V. & Fujimori, D. G. Radical SAM-mediated methylation of ribosomal RNA. Methods Enzymol. 560, 355–376 (2015).
Wang, X. et al. N6-methyladenosine-dependent regulation of messenger RNA stability. Nature 505, 117–120 (2014).
Pan, Y., Ma, P., Liu, Y., Li, W. & Shu, Y. Multiple functions of m(6)A RNA methylation in cancer. J. Hematol. Oncol. 11, 48 (2018).
Wang, S. et al. Roles of RNA methylation by means of N(6)-methyladenosine (m(6)A) in human cancers. Cancer Lett. 408, 112–120 (2017).
Lin, S., Choe, J., Du, P., Triboulet, R. & Gregory, R. I. The m(6)A methyltransferase METTL3 promotes translation in human cancer cells. Mol. Cell 62, 335–345 (2016).
Jaffrey, S. R. & Kharas, M. G. Emerging links between m(6)A and misregulated mRNA methylation in cancer. Genome Med. 9, 2 (2017).
Zhang, S. et al. m(6)A demethylase ALKBH5 maintains tumorigenicity of glioblastoma stem-like cells by sustaining FOXM1 expression and cell proliferation program. Cancer Cell 31, 591–606 (2017). e596.
Li, Z. et al. FTO plays an oncogenic role in acute myeloid leukemia as a N(6)-methyladenosine RNA demethylase. Cancer Cell 31, 127–141 (2017).
Chen, M. et al. RNA N6-methyladenosine methyltransferase-like 3 promotes liver cancer progression through YTHDF2-dependent posttranscriptional silencing of SOCS2. Hepatology 67, 2254–2270 (2018).
Zhang, C. et al. Hypoxia induces the breast cancer stem cell phenotype by HIF-dependent and ALKBH5-mediated m(6)A-demethylation of NANOG mRNA. Proc. Natl Acad. Sci. USA 113, E2047–E2056 (2016).
Zheng, G. et al. ALKBH5 is a mammalian RNA demethylase that impacts RNA metabolism and mouse fertility. Mol. Cell 49, 18–29 (2013).
Kim, J. H. et al. Prognostic impact of TTF-1 expression in non-squamous non-small-cell lung cancer, a meta-analysis. J. Cancer 9, 4279–4286 (2018).
Carretero, J. et al. Integrative genomic and proteomic analyses identify targets for Lkb1-deficient metastatic lung tumors. Cancer Cell 17, 547–559 (2010).
Huang, H., Weng, H. & Chen, J. m(6)A modification in coding and non-coding RNAs, roles and therapeutic implications in cancer. Cancer Cell 37, 270–288 (2020).
Liu, J. et al. m(6)A mRNA methylation regulates AKT activity to promote the proliferation and tumorigenicity of endometrial cancer. Nat. Cell Biol. 20, 1074–1083 (2018).
Lan, Q. et al. The critical role of RNA m(6)A methylation in cancer. Cancer Res. 79, 1285–1292 (2019).
Fu, Y., Dominissini, D., Rechavi, G. & He, C. Gene expression regulation mediated through reversible m(6)A RNA methylation. Nat. Rev. Genet. 15, 293–306 (2014).
Geula, S. et al. Stem cells. m6A mRNA methylation facilitates resolution of naive pluripotency toward differentiation. Science 347, 1002–1006 (2015).
Zhao, S. et al. Epigenome-wide tumor DNA methylation profiling identifies novel prognostic biomarkers of metastatic-lethal progression in men diagnosed with clinically localized prostate cancer. Clin. Cancer Res. 23, 311–319 (2017).
Zhang, D. et al. Homocysteine accelerates senescence of endothelial cells via DNA hypomethylation of human telomerase reverse transcriptase. Arterioscler. Thromb. Vasc. Biol. 35, 71–78 (2015).
Kitajima, S. et al. Suppression of STING associated with LKB1 loss in KRAS-driven lung cancer. Cancer Disco. 9, 34–45 (2019).
Wang, X. et al. N(6)-methyladenosine modulates messenger RNA translation efficiency. Cell 161, 1388–1399 (2015).
Rahib, L. et al. Projecting cancer incidence and deaths to 2030, the unexpected burden of thyroid, liver, and pancreas cancers in the United States. Cancer Res. 74, 2913–2921 (2014).
Meng, D. et al. Prognostic value of K-RAS mutations in patients with non-small cell lung cancer, a systematic review with meta-analysis. Lung Cancer 81, 1–10 (2013).
Moro, M. et al. Metformin enhances cisplatin-induced apoptosis and prevents resistance to cisplatin in co-mutated KRAS/LKB1 NSCLC. J. Thorac. Oncol. 13, 1692–1704 (2018).
Koyama, S. et al. STK11/LKB1 deficiency promotes neutrophil recruitment and proinflammatory cytokine production to suppress T-cell activity in the lung tumor microenvironment. Cancer Res. 76, 999–1008 (2016).
Schabath, M. B. et al. Differential association of STK11 and TP53 with KRAS mutation-associated gene expression, proliferation and immune surveillance in lung adenocarcinoma. Oncogene 35, 3209–3216 (2016).
Su, R. et al. R-2HG exhibits anti-tumor activity by targeting FTO/m(6)A/MYC/CEBPA signaling. Cell 172, 90–105 (2018).
Yang, S. et al. m(6)A mRNA demethylase FTO regulates melanoma tumorigenicity and response to anti-PD-1 blockade. Nat. Commun. 10, 2782 (2019).
Zhang, D. et al. Homocysteine upregulates soluble epoxide hydrolase in vascular endothelium in vitro and in vivo. Circ. Res. 110, 808–817 (2012).
Okon, I. S. et al. Protein kinase LKB1 promotes RAB7-mediated neuropilin-1 degradation to inhibit angiogenesis. J. Clin. Invest. 124, 4590–4602 (2014).
Wu, L. et al. FUN14 domain-containing 1 promotes breast cancer proliferation and migration by activating calcium-NFATC1-BMI1 axis. EBioMedicine 41, 384–394 (2019).
Zhang, D. et al. Non-CpG methylation by DNMT3B facilitates REST binding and gene silencing in developing mouse hearts. Nucleic Acids Res. 45, 3102–3115 (2017).
Linder, B. et al. Single-nucleotide-resolution mapping of m6A and m6Am throughout the transcriptome. Nat. Methods 12, 767–772 (2015).
Wang, Y. et al. N6-methyladenosine modification destabilizes developmental regulators in embryonic stem cells. Nat. Cell Biol. 16, 191–198 (2014).
Acknowledgements
We thank Laura Smales (BioMedEditing, Toronto, Canada) for critical reading and editing of the manuscript.
Funding
This study was funded by the National Heart, Lung, and Blood Institute (HL140954) and National Cancer Institute (NCI) (CA213022). Dr. Zou is the Eminent Scholar in Molecular and Translational Medicine of the Georgia Research Alliance.
Ethics statementThe study was performed in accordance with the Declaration of Helsinki. All of the patients were given and accepted an informed consent form prior to their enrollment. The use of human patient samples was approved by the Cancer Hospital of Harbin University Medical College Ethics Committee.
Author information
Authors and Affiliations
Contributions
Conception and design: M.Z., D. Z. Development of methodology: D.Z., J.N., I.O., Acquisition of data (provided cell lines, acquired and managed patients, provided facilities, etc.): J.N., I.O., X.Z., S.X., P.S., M.Z. Analysis and interpretation of data (e.g., statistical analysis, biostatistics, computational analysis): D.Z., J.N., I.O., X.Z., S.X., P.S. Writing, review, and/or revision of the manuscript: D.Z., I.O., X.Z., G.S., P.S., M.Z.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Edited by S. Inoue
Supplementary information
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Zhang, D., Ning, J., Okon, I. et al. Suppression of m6A mRNA modification by DNA hypermethylated ALKBH5 aggravates the oncological behavior of KRAS mutation/LKB1 loss lung cancer. Cell Death Dis 12, 518 (2021). https://doi.org/10.1038/s41419-021-03793-7
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41419-021-03793-7
- Springer Nature Limited
This article is cited by
-
FTO facilitates cancer metastasis by modifying the m6A level of FAP to induce integrin/FAK signaling in non-small cell lung cancer
Cell Communication and Signaling (2023)
-
RNA demethylase ALKBH5 in cancer: from mechanisms to therapeutic potential
Journal of Hematology & Oncology (2022)
-
m6A demethylase ALKBH5 promotes tumor cell proliferation by destabilizing IGF2BPs target genes and worsens the prognosis of patients with non-small-cell lung cancer
Cancer Gene Therapy (2022)
-
Pyroptosis correlates with tumor immunity and prognosis
Communications Biology (2022)
-
Crosstalk between m6A regulators and mRNA during cancer progression
Oncogene (2022)