Abstract
Background
Acute cholangitis is an ominous complication in biliary atresia (BA) patients. We investigated the prevalence of small intestine bacterial overgrowth (SIBO) in BA patients and its role in predicting acute cholangitis.
Methods
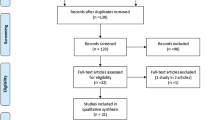
There are 69 BA patients with native liver recruited into this study prospectively. They received hydrogen and methane-based breath testing (HMBT) to detect SIBO after recruitment and were followed prospectively in our institute.
Results
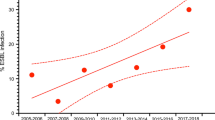
There are 16 (23.19%) subjects detected to have SIBO by HMBT. BA subjects with SIBO were noted to have higher serum alanine aminotransferase levels than others without SIBO (P = 0.03). The risk of acute cholangitis is significantly higher in BA patients with SIBO than in others without SIBO (62.50% vs. 15.09%, P < 0.001). The logistic regression analysis demonstrated that BA subjects with SIBO have a higher risk of acute cholangitis than others without SIBO (odds ratio = 9.38, P = 0.001). Cox’s proportional hazard analysis further confirmed the phenomena in survival analysis (hazard ratio = 6.43, P < 0.001).
Conclusions
The prevalence of SIBO in BA patients is 23.19% in this study. The presence of SIBO is associated with the occurrence of acute cholangitis in BA patients.
Impact
-
What is the key message of your article?
Acute cholangitis is common in BA, and is associated with SIBO after hepatoportoenterostomy in this study.
-
What does it add to the existing literature?
This study demonstrated that SIBO is common in BA after hepatoportoenterostomy, and is predictive of acute cholangitis and elevated serum ALT levels in BA.
-
What is the impact?
This prospective cohort study provides data regarding the significance of SIBO on the risk of acute cholangitis in BA patients.


Similar content being viewed by others
Data availability
Data are available on request and the approval of the local ethic committee.
References
Hartley, J. L., Davenport, M. & Kelly, D. A. Biliary atresia. Lancet 374, 1704–1713 (2009).
Hoofnagle, J. H. Biliary Atresia Research Consortium (BARC). Hepatology 39, 891 (2004).
Sokol, R. J. et al. Screening and outcomes in biliary atresia: summary of a National Institutes of Health workshop. Hepatology 46, 566–581 (2007).
Venkat, V. et al. Modeling outcomes in children with biliary atresia with native liver after 2 years of age. Hepatol. Commun. 4, 1824–1834 (2020).
Lien, T. H. et al. Effects of the infant stool color card screening program on 5-year outcome of biliary atresia in Taiwan. Hepatology 53, 202–208 (2011).
Sokol, R. J., Mack, C., Narkewicz, M. R. & Karrer, F. M. Pathogenesis and outcome of biliary atresia: current concepts. J. Pediatr. Gastroenterol. Nutr. 37, 4–21 (2003).
Ohi, R. Biliary atresia. A surgical perspective. Clin. Liver Dis. 4, 779–804 (2000).
Oh, M., Hobeldin, M., Chen, T., Thomas, D. W. & Atkinson, J. B. The Kasai procedure in the treatment of biliary atresia. J. Pediatr. Surg. 30, 1077–1080 (1995).
Chung, P. H. Y. et al. Life long follow up and management strategies of patients living with native livers after Kasai portoenterostomy. Sci. Rep. 11, 11207 (2021).
Pietrobattista, A. et al. Does the treatment after Kasai procedure influence biliary atresia outcome and native liver survival? J. Pediatr. Gastroenterol. Nutr. 71, 446–451 (2020).
Jain, V., Alexander, E. C., Burford, C., Verma, A. & Dhawan, A. Gut Microbiome: a potential modifiable risk factor in biliary atresia. J. Pediatr. Gastroenterol. Nutr. 72, 184–193 (2021).
Sakamoto, S., Fukahori, S., Hashizume, N. & Yagi, M. Measuring small intestinal bacterial overgrowth using the hydrogen breath test among postoperative patients with biliary atresia. Asian J. Surg. 43, 1130–1131 (2020).
Hitch, D. C. & Lilly, J. R. Identification, quantification, and significance of bacterial growth within the biliary tract after Kasai’s operation. J. Pediatr. Surg. 13, 563–569 (1978).
Yamamoto, T., Hamanaka, Y. & Suzuki, T. Bile acids and microorganisms in the jejunal lumen after biliary reconstruction in dogs. J. Am. Coll. Surg. 181, 525–529 (1995).
Rao, S. S. C. & Bhagatwala, J. Small intestinal bacterial overgrowth: clinical features and therapeutic management. Clin. Transl. Gastroenterol. 10, e00078 (2019).
Quigley, E. M. M., Murray, J. A. & Pimentel, M. AGA clinical practice update on small intestinal bacterial overgrowth: expert review. Gastroenterology 159, 1526–1532 (2020).
Rezaie, A. et al. Hydrogen and methane-based breath testing in gastrointestinal disorders: The North American Consensus. Am. J. Gastroenterol. 112, 775–784 (2017).
Ghoshal, U. C. How to interpret hydrogen breath tests. J. Neurogastroenterol. Motil. 17, 312–317 (2011).
Pande, C., Kumar, A. & Sarin, S. K. Small-intestinal bacterial overgrowth in cirrhosis is related to the severity of liver disease. Aliment Pharm. Ther. 29, 1273–1281 (2009).
Lakshmi, C. P. et al. Frequency and factors associated with small intestinal bacterial overgrowth in patients with cirrhosis of the liver and extra hepatic portal venous obstruction. Dig. Dis. Sci. 55, 1142–1148 (2010).
Abu-Shanab, A. & Quigley, E. M. The role of the gut microbiota in nonalcoholic fatty liver disease. Nat. Rev. Gastroenterol. Hepatol. 7, 691–701 (2010).
Quigley, E. M., Abu-Shanab, A., Murphy, E. F., Stanton, C. & Monsour, H. P. Jr. The metabolic role of the microbiome: implications for NAFLD and the metabolic syndrome. Semin Liver Dis. 36, 312–316 (2016).
Wu, J. F. et al. Transient elastography is useful in diagnosing biliary atresia and predicting prognosis after hepatoportoenterostomy. Hepatology 68, 616–624 (2018).
Shen, Q. L. et al. Assessment of liver fibrosis by Fibroscan as compared to liver biopsy in biliary atresia. World J. Gastroenterol. 21, 6931–6936 (2015).
Belei, O., Olariu, L., Dobrescu, A., Marcovici, T. & Marginean, O. The relationship between non-alcoholic fatty liver disease and small intestinal bacterial overgrowth among overweight and obese children and adolescents. J. Pediatr. Endocrinol. Metab. 30, 1161–1168 (2017).
Cares, K. et al. Risk of small intestinal bacterial overgrowth with chronic use of proton pump inhibitors in children. Eur. J. Gastroenterol. Hepatol. 29, 396–399 (2017).
Wang, L. et al. Hydrogen breath test to detect small intestinal bacterial overgrowth: a prevalence case–control study in autism. Eur. Child Adolesc. Psychiatry 27, 233–240 (2018).
Augustyn, M., Grys, I. & Kukla, M. Small intestinal bacterial overgrowth and nonalcoholic fatty liver disease. Clin. Exp. Hepatol. 5, 1–10 (2019).
Ferolla, S. M., Armiliato, G. N. A., Couto, G. A. & Ferrari, T. C. A. The role of intestinal bacteria overgrowth in obesity-related nonalcoholic fatty liver disease. Nutrients 6, 5583–5599 (2014).
Wu, J. F. et al. Serum bile acid levels assist the prediction of biliary stricture and survival after liver transplantation in children. Eur. J. Pediatr. 180, 2539–2547 (2021).
Ramírez-Pérez, O., Cruz-Ramón, V., Chinchilla-López, P. & Méndez-Sánchez, N. The role of the gut microbiota in bile acid metabolism. Ann. Hepatol. 16, S21–S26 (2017).
Larsen, H. M. et al. Chronic loose stools following right-sided hemicolectomy for colon cancer and the association with bile acid malabsorption and small intestinal bacterial overgrowth. Colorectal Dis. 25, 600–607 (2023).
Funding
This work is supported by grants from the National Taiwan University Hospital (NTUH.110-T05, NTUH.111-T0009, NTUH. 112-E0009). The funding agencies had no role in the design, and conduct of the study; in the collection, analysis and interpretation of the data; or in the preparation, review, or approval of the manuscript.
Author information
Authors and Affiliations
Contributions
J.-F.W., the first author of the study, is responsible for the study design, data management, and manuscript writing. P.-H.T., H.-H.C., C.-M.C., W.-H.L., W.-M.H., and M.-H.C. are responsible for long-term patient follow, recruitment, and critical review of the manuscript. P.-H.T. is responsible for the study design, hydrogen breath test interpretation, and critical review of the manuscript. M.-H.C., the corresponding author, is responsible for patient recruitment, study design, critical review of the article, and is the principal investigator of this study. All authors have seen and approved the final version. The corresponding author had full access to all the data in this study and had final responsibility for the decision to submit it for publication.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethics approval and consent to participate
The study protocol was approved by the institutional review board of National Taiwan University Hospital. All participants or their parents signed the informed consent approved by the institutional review board.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wu, JF., Tseng, PH., Chang, HH. et al. The prevalence and impact of small intestine bacterial overgrowth in biliary atresia patients. Pediatr Res 95, 302–307 (2024). https://doi.org/10.1038/s41390-023-02818-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41390-023-02818-5
- Springer Nature America, Inc.