Abstract
Objective
To examine longitudinal pH-impedance characteristics from those infants who remained on proton pump inhibitors therapy for gastroesophageal reflux disease (GERD) as parents/providers refused to discontinue therapy after 4 weeks.
Study design
Eighteen infants with acid reflux index >3% underwent treatment, and pH-impedance data were compared prior to and on proton pump inhibitors at 42 ± 1 and 46 ± 1 weeks’ postmenstrual age, respectively. Esophageal acid and bolus exposure, symptoms and swallowing characteristics were examined.
Results
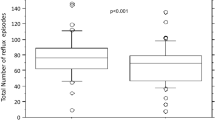
Proton pump inhibitors reduces the acid-mediated effects of reflux but modifies impedance and clearance mechanisms (P < 0.05). Prolonged therapy did not reduce symptoms (P > 0.05). Infants evaluated while on proton pump inhibitors were 1.8 times more likely to have swallows before and after reflux.
Conclusions
Prescription of proton pump inhibitors for objectively determined GERD should have time limits, as prolonged treatment can result in prolonged esophageal bolus clearance time without relieving symptoms.



Similar content being viewed by others
Data availability
The data that support the findings of this study are available upon reasonable request from the corresponding author. The data are not publicly available due to privacy and ethical restrictions.
References
Vandenplas Y, Rudolph CD, Di Lorenzo C, Hassall E, Liptak G, Mazur L, et al. Pediatric gastroesophageal reflux clinical practice guidelines: joint recommendations of the North American Society for Pediatric Gastroenterology, Hepatology, and Nutrition (NASPGHAN) and the European Society for Pediatric Gastroenterology, Hepatology, and Nutrition (ESPGHAN). J Pediatr Gastroenterol Nutr. 2009;49:498–547.
Rosen R, Vandenplas Y, Singendonk M, Cabana M, DiLorenzo C, Gottrand F, et al. Pediatric gastroesophageal reflux clinical practice guidelines: joint recommendations of the North American Society for pediatric gastroenterology, hepatology, and nutrition and the european society for pediatric gastroenterology, hepatology, and nutrition. J Pediatr Gastroenterol Nutr. 2018;66:516–54.
Orenstein SR, McGowan JD. Efficacy of conservative therapy as taught in the primary care setting for symptoms suggesting infant gastroesophageal reflux. J Pediatr. 2008;152:310–4.
Sultana Z, Hasenstab KA, Moore RK, Osborn EK, Yildiz VO, Wei L, et al. Symptom scores and pH-Impedance: secondary analysis of a randomized controlled trial in infants treated for gastroesophageal reflux. Gastro Hep Adv. 2022;1:869–81.
Levy EI, Salvatore S, Vandenplas Y, de Winter JP. Prescription of acid inhibitors in infants: an addiction hard to break. Eur J Pediatr. 2020;179:1957–61.
Jadcherla SR, Sultana Z, Hasenstab-Kenney KA, Prabhakar V, Gulati IK, Di Lorenzo C. Differentiating esophageal sensitivity phenotypes using pH-impedance in intensive care unit infants referred for gastroesophageal reflux symptoms. Pediatr Res. 2021;89:636–44.
Jadcherla SR, Slaughter JL, Stenger MR, Klebanoff M, Kelleher K, Gardner W. practice variance, prevalence, and economic burden of premature infants diagnosed with GERD. Hosp Pediatr. 2013;3:335–41.
Corsonello A, Lattanzio F, Bustacchini S, Garasto S, Cozza A, Schepisi R, et al. Adverse events of proton pump inhibitors: potential mechanisms. Curr Drug Metab. 2018;19:142–54.
Slaughter JL, Stenger MR, Reagan PB, Jadcherla SR. Neonatal Histamine-2 receptor antagonist and proton pump inhibitor treatment at United States Children’s Hospitals. J Pediatr. 2016;174:63–70.e3.
Davidson G, Wenzl TG, Thomson M, Omari T, Barker P, Lundborg P, et al. Efficacy and safety of once-daily esomeprazole for the treatment of gastroesophageal reflux disease in neonatal patients. J Pediatr. 2013;163:692–8.e1-2.
Loots CM, Benninga MA, Davidson GP, Omari TI. Addition of pH-impedance monitoring to standard pH monitoring increases the yield of symptom association analysis in infants and children with gastroesophageal reflux. J Pediatr. 2009;154:248–52.
Woodley FW, Moore-Clingenpeel M, Machado RS, Nemastil CJ, Jadcherla SR, Hayes D Jr, et al. Not all children with cystic fibrosis have abnormal esophageal neutralization during chemical clearance of acid reflux. Pediatr Gastroenterol Hepatol Nutr. 2017;20:153–9.
Gyawali CP, Kahrilas PJ, Savarino E, Zerbib F, Mion F, Smout A, et al. Modern diagnosis of GERD: the Lyon Consensus. Gut. 2018;67:1351–62.
Sivalingam M, Sitaram S, Hasenstab KA, Wei L, Woodley FW, Jadcherla SR. Effects of esophageal acidification on troublesome symptoms: an approach to characterize true acid GERD in dysphagic neonates. Dysphagia. 2017;32:509–19.
Jadcherla SR, Hanandeh N, Hasenstab KA, Nawaz S. Differentiation of esophageal pH-impedance characteristics classified by the mucosal integrity marker in human neonates. Pediatr Res. 2019;85:355–60.
Jadcherla SR, Peng J, Chan CY, Moore R, Wei L, Fernandez S, et al. Significance of gastroesophageal refluxate in relation to physical, chemical, and spatiotemporal characteristics in symptomatic intensive care unit neonates. Pediatr Res. 2011;70:192–8.
Weusten BL, Roelofs JM, Akkermans LM, Van Berge-Henegouwen GP, Smout AJ. The symptom-association probability: an improved method for symptom analysis of 24-hour esophageal pH data. Gastroenterology. 1994;107:1741–5.
Frazzoni M, Savarino E, de Bortoli N, Martinucci I, Furnari M, Frazzoni L, et al. Analyses of the post-reflux swallow-induced peristaltic wave index and nocturnal baseline impedance parameters increase the diagnostic yield of impedance-pH monitoring of patients with reflux disease. Clin Gastroenterol Hepatol. 2016;14:40–6.
Frazzoni M, de Bortoli N, Frazzoni L, Tolone S, Furnari M, Martinucci I, et al. The added diagnostic value of postreflux swallow-induced peristaltic wave index and nocturnal baseline impedance in refractory reflux disease studied with on-therapy impedance-pH monitoring. Neurogastroenterol Motil. 2017;29:e12947.
Castellani C, Huber-Zeyringer A, Bachmaier G, Saxena AK, Hollwarth ME. Proton pump inhibitors for reflux therapy in infants: effectiveness determined by impedance pH monitoring. Pediatr Surg Int. 2014;30:381–5.
Hemmink GJ, Bredenoord AJ, Weusten BL, Monkelbaan JF, Timmer R, Smout AJ. Esophageal pH-impedance monitoring in patients with therapy-resistant reflux symptoms: ‘on’ or ‘off’ proton pump inhibitor? Am J Gastroenterol. 2008;103:2446–53.
Turk H, Hauser B, Brecelj J, Vandenplas Y, Orel R. Effect of proton pump inhibition on acid, weakly acid and weakly alkaline gastro-esophageal reflux in children. World J Pediatr. 2013;9:36–41.
Gibbons TE, Gold BD. The use of proton pump inhibitors in children: a comprehensive review. Paediatr Drugs. 2003;5:25–40.
Welsh C, Kasirer MY, Pan J, Shifrin Y, Belik J. Pantoprazole decreases gastroesophageal muscle tone in newborn rats via rho-kinase inhibition. Am J Physiol Gastrointest Liver Physiol. 2014;307:G390–6.
Mitchell DJ, McClure BG, Tubman TR. Simultaneous monitoring of gastric and oesophageal pH reveals limitations of conventional oesophageal pH monitoring in milk fed infants. Arch Dis Child. 2001;84:273–6.
Borrelli O, Salvatore S, Mancini V, Ribolsi M, Gentile M, Bizzarri B, et al. Relationship between baseline impedance levels and esophageal mucosal integrity in children with erosive and non-erosive reflux disease. Neurogastroenterol Motil. 2012;24:828–e394.
Jadcherla SR, Helmick R, Hasenstab KA, Njeh M, Alshaikh E. Impact of esophageal mucosal permeability markers on provocation-induced esophageal reflexes in high-risk infants. Physiol Rep. 2022;10:e15366.
Cohen Sabban J, Bertoldi GD, Ussher F, Christiansen S, Lifschitz C, Orsi M. Low-impedance baseline values predict severe esophagitis. J Pediatr Gastroenterol Nutr. 2017;65:278–80.
Xu H, Ye B, Ding Y, Wang M, Lin L, Jiang L. Factors of reflux episodes with post-reflux swallow-induced peristaltic wave in gastroesophageal reflux disease. J Neurogastroenterol Motil. 2020;26:378–83.
Frazzoni M, Manta R, Mirante VG, Conigliaro R, Frazzoni L, Melotti G. Esophageal chemical clearance is impaired in gastro-esophageal reflux disease-a 24-h impedance-pH monitoring assessment. Neurogastroenterol Motil. 2013;25:399–406.e295.
Gupta A, Gulati P, Kim W, Fernandez S, Shaker R, Jadcherla SR. Effect of postnatal maturation on the mechanisms of esophageal propulsion in preterm human neonates: primary and secondary peristalsis. Am J Gastroenterol. 2009;104:411–9.
Jadcherla SR, Duong HQ, Hoffmann RG, Shaker R. Esophageal body and upper esophageal sphincter motor responses to esophageal provocation during maturation in preterm newborns. J Pediatr. 2003;143:31–8.
Collins CR, Hasenstab KA, Nawaz S, Jadcherla SR. Mechanisms of aerodigestive symptoms in infants with varying acid reflux index determined by esophageal manometry. J Pediatr. 2019;206:240–7.
Zerbib F, Duriez A, Roman S, Capdepont M, Mion F. Determinants of gastro-oesophageal reflux perception in patients with persistent symptoms despite proton pump inhibitors. Gut. 2008;57:156–60.
Herregods TV, Bredenoord AJ, Smout AJ. Pathophysiology of gastroesophageal reflux disease: new understanding in a new era. Neurogastroenterol Motil. 2015;27:1202–13.
Zoizner-Agar G, Rotsides JM, Shao Q, Rickert S, Ward R, Greifer M, et al. Proton pump inhibitor administration in neonates and infants. Lack of consensus - An ASPO survey. Int J Pediatr Otorhinolaryngol. 2020;137:110200.
Safe M, Chan WH, Leach ST, Sutton L, Lui K, Krishnan U. Widespread use of gastric acid inhibitors in infants: Are they needed? Are they safe? World J Gastrointest Pharm Ther. 2016;7:531–9.
Eichenwald EC, Committee On F, Newborn. Diagnosis and Management of Gastroesophageal Reflux in Preterm Infants. Pediatrics. 2018;142:e20181061.
Jadcherla SR, Hasenstab KA, Gulati IK, Helmick R, Ipek H, Yildiz V, et al. Impact of feeding strategies with acid suppression on esophageal reflexes in human neonates with gastroesophageal reflux disease: a single-blinded randomized clinical trial. Clin Transl Gastroenterol. 2020;11:e00249.
Levy EI, Hoang DM, Vandenplas Y. The effects of proton pump inhibitors on the microbiome in young children. Acta Paediatr. 2020;109:1531–8.
Jadcherla SR, Hasenstab KA, Wei L, Osborn EK, Viswanathan S, Gulati IK, et al. Role of feeding strategy bundle with acid-suppressive therapy in infants with esophageal acid reflux exposure: a randomized controlled trial. Pediatr Res. 2021;89:645–52.
Funding
Supported by the National Institutes of Health (RO1 DK 068158 [to SRJ]) and the National Center for Advancing Translational Sciences (UL1TR002733 [to The Ohio State University Center for Clinical and Translational Science for REDCap support]).
Author information
Authors and Affiliations
Contributions
ZS and SRJ performed studies. ZS, and VOY analyzed data. ZS and SRJ drafted the initial manuscript. SRJ conceptualized study, obtained funding, and IRB approvals. ZS, VOY, and SRJ validated and interpreted data, critically reviewed, and revised the manuscript, approved the final version, and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sultana, Z., O. Yildiz, V. & Jadcherla, S.R. Characteristics of esophageal refluxate and symptoms in infants compared between pre-treatment and on treatment with proton pump inhibitors. J Perinatol 44, 87–93 (2024). https://doi.org/10.1038/s41372-023-01825-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-023-01825-y
- Springer Nature America, Inc.