Abstract
Objective
This scoping review describes the nature and evidence base of internationally available guidelines for the introduction of oral feeding for preterm infants in neonatal units.
Study design
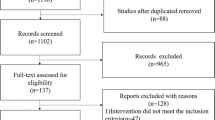
Thirty-nine current infant oral feeding introduction guidelines were obtained, and their recommendations contrasted with available scientific literature.
Result
Documents were primarily from the USA, UK, Canada, and Australia, from hospitals, regional health authorities, and journal articles. Specifics of nonnutritive sucking, gestational age at first feed, exclusions to oral feeding, suggested interventions, and the definition of full oral feeding varied between documents. There was variable use of scientific evidence to back up recommendations.
Conclusion
Guidelines for oral feeding, whether written by clinicians or researchers, vary greatly in their recommendations and details of interventions. Areas more widely researched were more commonly discussed. Recommendations varied more when evidence was not available or weak. Guideline developers need to synthesize evidence and local variability to create appropriate guidelines.


Similar content being viewed by others
References
Committee on Fetus and Newborn. Hospital discharge of the high-risk neonate. Pediatrics. 2008;122:1119–26.
Breton S, Steinwender S. Timing introduction and transition to oral feeding in preterm infants: current trends and practice. Newborn Infant Nurs Rev. 2008;8:153–9.
Holloway EM. The dynamic process of assessing infant feeding readiness. Newborn Infant Nurs Rev. 2014;14:119–23.
Ross K, Heiny E, Conner S, Spener P, Pineda R. Occupational therapy, physical therapy and speech-language pathology in the neonatal intensive care unit: Patterns of therapy usage in a level IV NICU. Res Dev Disabil. 2017;64:108–17.
Woolf SH, Grol R, Hutchinson A, Eccles M, Grimshaw J. Potential benefits, limitations, and harms of clinical guidelines. Br Med J. 1999;318:527–30.
Willis CD, Saul J, Bevan H, Scheirer MA, Best A, Greenhalgh T, et al. Sustaining organizational culture change in health systems. J Health Organ Manag. 2016;30:2–30.
Chantry CJ, Howard CR. Clinical protocols for management of breastfeeding. Pediatr Clin North Am. 2013;60:75–113.
Crouse-Hood JL. Implementing a cue based feeding protocol and staff education program in the neonatal intensive care unit. University of Delaware; 2019.
Briere CE, McGrath J, Cong X, Cusson R. State of the science: a contemporary review of feeding readiness in the preterm infant. J Perinat Neonatal Nurs. 2014;28:51–8.
Brouwers MC, Kho ME, Browman GP, Burgers JS, Cluzeau F, Feder G, et al. AGREE II: advancing guideline development, reporting and evaluation in health care. Can Med Assoc J. 2010;182:E839–42.
Aromataris E, Munn Z, editors. JBI manual for evidence synthesis. JBI; 2020. https://doi.org/10.46658/JBIMES-20-01.
Arvedson J, Clark H, Lazarus C, Schooling T, Frymark T. Evidence-based systematic review: effects of oral motor interventions on feeding and swallowing in preterm infants. Am J Speech Lang Pathol. 2010;19:321–40.
Asadollahpour F, Yadegari F, Soleimani F, Khalesi N. The effects of non-nutritive sucking and pre-feeding oral stimulation on time to achieve independent oral feeding for preterm infants. Iran J Pediatr. 2015;25:5.
Ziadi M, Heon M, Aita M. A critical review of interventions supporting transition from gavage to direct breastfeeding in hospitalized preterm infants. Newborn Infant Nurs Rev. 2016;16:78–91.
Lubbe W. Clinician’s guide for cue-based transition to oral feeding in preterm infants: an easy-to-use clinical guide. J Eval Clin Pr. 2018;24:80–8.
Rhooms L, Dow K, Brandon C, Zhao G, Fucile S. Effect of unimodal and multimodal sensorimotor interventions on oral feeding outcomes in preterm infants: an evidence-based systematic review. Adv Neonatal Care. 2019;19:E3–20.
Thakkar PA, Rohit HR, Das RR, Thakkar UP, Singh A. Effect of oral stimulation on feeding performance and weight gain in preterm neonates: a randomised controlled trial. Paediatr Int Child Health. 2018;38:181–6.
Tubbs-Cooley HL, Pickler R, Meinzen-Derr J. Missed oral feeding opportunities and preterm infants’ time to achieve full oral feedings and neonatal intensive care unit discharge. Am J Perinatol. 2015;32:1–8.
Cormier DME. Impact of cue-based feeding protocol on premature infants’ outcomes and hospital length of stay. California State University; 2014.
Chrupcala KA, Edwards TM, Spatz DL. A continuous quality improvement project to implement infant-driven feeding as a standard of practice in the newborn/infant intensive care unit. J Obstet Gynecol Neonatal Nurs. 2015;44:654–64.
Fry TJ, Marfurt S, Wengier S. Systematic review of quality improvement initiatives related to cue-based feeding in preterm infants. Nurs Women’s Health. 2018;22:401–10.
Settle M, Francis K. Does the infant-driven feeding method positively impact preterm infant feeding outcomes? Adv Neonatal Care. 2019;19:51–55.
Watson J, McGuire W. Responsive versus scheduled feeding for preterm infants. Cochrane Database Syst Rev. 2016;1:CD005255.
Whetten CH. Cue-based feeding in the NICU. Nurs Women’s Health. 2016;20:507–10.
Pickler RH, Reyna BA, Wetzel PA, Lewis M. Effect of four approaches to oral feeding progression on clinical outcomes in preterm infants. Nurs Res Pract. 2015;2015:716828.
Wang YW, Hung HY, Lin CH, Wang CJ, Lin YJ, Chang YJ. Effect of a delayed start to oral feeding on feeding performance and physiological responses in preterm infants: a randomized clinical trial. J Nurs Res. 2018;26:324–31.
Jadcherla SR, Wang M, Vijayapal AS, Leuthner SR. Impact of prematurity and co-morbidities on feeding milestones in neonates: a retrospective study. Am J Perinatol. 2009;30:201.
Jackson BN, Kelly BN, McCann CM, Purdy SC. Predictors of the time to attain full oral feeding in late preterm infants. Acta Paediatr. 2016;105:e1–6.
Khan Z, Sitter C, Dunitz-Scheer M, Posch K, Avian A, Breseste I, et al. Full oral feeding is possible before discharge even in extremely preterm infants. Acta Paediatr. 2019;108:239–44.
Brumbaugh JE, Colaizy TT, Saha S, Van Meurs KP, Das A, Walsh MC, et al. Oral feeding practices and discharge timing for moderately preterm infants. Early Hum Dev. 2018;120:46–52.
Ferrara L, Bidiwala A, Sher I, Pirzada M, Barlev D, Islam S, et al. Effect of nasal continuous positive airway pressure on the pharyngeal swallow in neonates. Am J Perinatol. 2017;37:398.
Samson N, Michaud A, Othman R, Nadeau C, Nault S, Cantin D, et al. Nasal continuous positive airway pressure influences bottle-feeding in preterm lambs. Pediatr Res. 2017;82:926–33.
Samson N, Nadeau CN, Vincent L, Cantin D, Praud J-P. Effects of nasal continuous positive airway pressure and high-flow nasal cannula on sucking, swallowing, and breathing during bottle-feeding in lambs. Front Pediatr. 2018;5:296.
Glackin SJ, O’Sullivan A, George S, Semberova J, Miletin J. High flow nasal cannula versus NCPAP, duration to full oral feeds in preterm infants: a randomised controlled trial. Arch Dis Child Fetal Neonatal Ed. 2017;102:F329–32.
Taha DK, Kornhauser M, Greenspan JS, Dysart KC, Aghai ZH. High flow nasal cannula use is associated with increased morbidity and length of hospitalization in extremely low birth weight infants. J Pediatr. 2016;173:50–55.e1.
Hanin M, Nuthakki S, Malkar MB, Jadcherla SR. Safety and efficacy of oral feeding in infants with BPD on nasal CPAP. Dysphagia. 2015;30:121–7.
Clark L, Kennedy G, Pring T, Hird M. Improving bottle feeding in preterm infants: investigating the elevated side-lying position. Infant. 2007;3:154–8.
Park J, Thoyre S, Knafl GJ, Hodges EA, Nix WB. Efficacy of semielevated side-lying positioning during bottle-feeding of very preterm infants: a pilot study. J Perinat Neonatal Nurs. 2014;28:69–79.
Park J, Pados BF, Thoyre SM. Systematic review: what is the evidence for the side-lying position for feeding preterm infants? Adv Neonatal Care. 2018;18:285–94.
McGrath JM, Braescu AV. State of the science: feeding readiness in the preterm infant. J Perinat Neonatal Nurs. 2004;18:353–68.
Einarsson-Backes LM, Deitz J, Price R, Glass R, Hays R. The effect of oral support on sucking efficiency in preterm infants. Am J Occup Ther. 1994;48:490–8.
Hill AS, Kurkowski TB, Garcia J. Oral support measures used in feeding the preterm infant. Nurs Res. 2000;49:2–10.
Ross ES, Browne JV. Developmental progression of feeding skills: an approach to supporting feeding in preterm infants. Semin Neonatol. 2002;7:469–75.
American Speech-Language-Hearing Association. Pediatric dysphagia. 2020. http://www.asha.org/Practice-Portal/Clinical-Topics/Pediatric-Dysphagia.
Rustam LB, Masri S, Atallah N, Tamim H, Charafeddine L. Sensorimotor therapy and time to full oral feeding in <33 weeks infants. Early Hum Dev. 2016;99:1–5.
Kirk AT, Alder SC, King JD. Cue-based oral feeding clinical pathway results in earlier attainment of full oral feeding in premature infants. J Perinatol. 2007;27:572–8.
Viswanathan S, Jadcherla S. Transitioning from gavage to full oral feeds in premature infants: When should we discontinue the nasogastric tube? J Perinatol. 2019;39:1257–62.
Hwang YS, Ma MC, Tseng YM, Tsai WH. Associations among perinatal factors and age of achievement of full oral feeding in very preterm infants. Pediatr Neonatol. 2013;54:309–14.
Embleton ND. Nutrition and growth. In: Phillip M, Turck D, Shamir R, editors. World review of nutrition and dietetics. S. Karger: Basel; 2013.
Andrews JC, Schünemann HJ, Oxman AD, Pottie K, Meerpohl JJ, Coello PA, et al. GRADE guidelines: 15. Going from evidence to recommendation—determinants of a recommendation’s direction and strength. J Clin Epidemiol. 2013;66:726–35.
Acknowledgements
Dr Huub Bakker for support with manuscript preparation and proofreading.
Author information
Authors and Affiliations
Contributions
LB conceived the study design, identified and analyzed the documents, and wrote the manuscript. BJ and AM conceived the study design, provided support for document identification and analysis, and edited and approved the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Bakker, L., Jackson, B. & Miles, A. Oral-feeding guidelines for preterm neonates in the NICU: a scoping review. J Perinatol 41, 140–149 (2021). https://doi.org/10.1038/s41372-020-00887-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-020-00887-6
- Springer Nature America, Inc.
This article is cited by
-
The effect of oropharyngeal mother’s milk on nutritional outcomes in preterm infants: a randomized controlled trial
BMC Pediatrics (2024)
-
Factors associated with post NICU discharge exclusive breastfeeding rate and duration amongst first time mothers of preterm infants in Shanghai: a longitudinal cohort study
International Breastfeeding Journal (2022)
-
Neonatal Abstinence Syndrome: Management Advances and Therapeutic Approaches
Current Addiction Reports (2021)