Abstract
Objective
Compare state policies with standards outlined in the 2012 AAP Policy Statement on Levels of Neonatal Care.
Study design
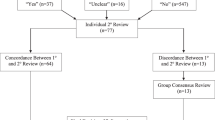
Systematic, web-based review of publicly available policies on levels of care in all states in 2014. Infant risk information, equipment capabilities, and specialty staffing were abstracted from published rules, statutes, and regulations.
Result
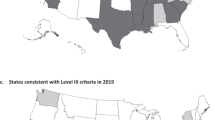
Twenty-two states had a policy on regionalized perinatal care. State policies vary in consistency with the AAP Policy, with 60% of states including standards consistent with Level I criteria, 48% Level II, 14% Level III, and one state with Level IV. Ventilation capability standards are highly consistent (66–100%), followed by imaging capability standards (50–90%). Policy language on specialty staffing (44–68%), and subspecialty staffing (39–50%) are moderately consistent.
Conclusion
State policies vary in consistency, a potentially significant barrier to monitoring, regulation, uniform care provision and measurement, and reporting of national-level measures on risk-appropriate care.

Similar content being viewed by others
References
MacDorman M, Matthews T, Mohagoo A, Zeitlin J. International comparisons of infant mortality and related factors: United States andEurope, 2010. Natl Vital Stat Rep. 2014;63:1–6.
Holmstrom S, Phibbs C. Regionalization and mortality in neonatal intensive care. Pediatr Clin North Am. 2009;56:617–30.
Goodman D, Fisher E, Little G, Stukel T, Chang C, Schoendorf K. The relation between the availability of neonatal intensive care and neonatal mortality. N Engl J Med. 2002;346:1538–44.
McCormick M, Richardson D. Access to neonatal intensive care. The Future of Children. 1995;5:162–75.
Toward Improving the Outcome of Pregnancy. Recommendations for the Regional Development of Maternal and Perinatal Health Services. White Plains, NY: March of Dimes; 1976.
Sloan F, Steinwald B. Effects of regulation on hospital costs and input use. J Law Econ. 1980;23:81–109.
Improving Health Care. A Dose of Competition: Department of Justice and Federal Trade Commision; 2004.
Gagnon D, Allison-Cooke S, Schwartz R. Perinatal care: the threat of deregionalization. Pediatr Ann. 1988;17:447–52.
Chung J, Phibbs C, Boscardin W, Kominski G, Ortega A, Needleman J. The effect of neonatal intensive care level and hospital volume on mortality of very low brith weight infants. Med Care. 2010;48:635–44.
Stark A. Levels of neonatal care. Pediatrics. 2004;114:1341–47.
Toward Improving the Outcome of Pregnancy. The 90s and Beyond. White Plains, NY: March of Dimes; 1993.
Toward Improving the Outcome of Pregnancy. Enhancing Perinatal Health Through Quality, Safety, and Performance Initiatives. White Plains, NY: March of Dimes; 2011.
Howell E, Richardson D, Ginsberg P, Foot B. Deregionalization of neonatal intensive care in urban areas. Am J Public Health 2002;92:119–24.
Guidelines for Perinatal Care, 5th Edition: American Academy of Pediatrics; 2002.
Guidelines for Perinatal Care, 6th Edition: American Academy of Pediatrics; 2007.
Guidelines for Perinatal Care, 7th Edition: American Academy of Pediatrics; 2012.
Levels of Neonatal Care: Committee on Fetus and Newborn. Pediatrics. 2012;130:587–597.
Healthy People 2020: Maternal, Infant, and Child Health Measure 33. http://www.healthypeople.gov/2020/topics-objectives/topic/maternal-infant-and-child-health/objectives. Accessed 26 Feb 2015.
Freeman V. Very low birth weight babies delivered at Facilities for high-risk neonates: a review of title v national performance measure 17: maternal and child health bureau, Health Resources and Services Administration; 2010; 1-41.
Blackmon L, Barfield W, Stark A. Hospital neonatal services in the united states: variation in definitions, criteria, and regulatory status, 2008. J Perinatol. 2009;29:788–94.
Phibbs C, Baker L, Caughey A, Danielsen B, Schmitt S, Phibbs R. Level and volume of neonatal intensive care and mortality in very-low-birth-weight infants. N Engl J Med. 2007;356:2165–75.
Lorch S, Baiocchi M, Ahlberg C, Small D. The differential impact of delivery hospital on the outcomes of premature infants. Pediatrics. 2012;130:270–78.
Synnes A, MacNab Y, Qiu Z, Ohlsson A, Gustafson P, Dean C, et al. Neonatal intensive care unit characteristics affect the incidence of severe intraventricular hemorrhage. Med Care. 2006;44:754–59.
Rogowski J, Horbar J, Pisek P, Baker L, Deterding J, Edwards W, et al. Economic implications of neonatal intensive care unit collaborative quality improvement. Pediatrics. 2001;107:23–29.
Horbar J, Rogowski J, Pisek P, Delmore P, Edwards W, Hocker J, et al. Collaborative quality improvement for neonatal intensive care. NIC/Q project investigators of the vermont oxford network. Pediatrics. 2001;107:14–22.
Dobrez D, Gerber S, Budetti P. Trends in perinatal regionalization and the role of managed care. Obstet Gynecol. 2006;108:839–45.
Lorch S, Martin A, Ranada R, Srinivas S, Grande D. Lessons for providers and hospitals from Philadelphia’s obstetric services closures and consolidations, 1997–2012. Health Aff. 2014;33:2162–69.
Lorch S. Ensuring acces to the appropriate health care professionals: regionalization and centralization in a new era of health care financing and delivery. J Am Med Assoc Pediatrics. 2015;169:11–12.
Lasswell S, Barfield W, Rochat R, Blackmon L. Perinatal regionalization for very low-birth-weight and very preterm infants: a meta-analysis. J Am Med Assoc. 2010;304:992–1000.
Profit J, Gould J, Bennett M, Goldstein B, Draper D, Phibbs C et al. The association of level of care with NICU quality. Pediatrics. 2016;137.
Profit J, Wise P, Lee H. Consequences of the affordable care act for sick newborns. Pediatrics. 2014;134:e1284–86.
Staebler S. Regionalized systems of perinatal care: health policy considerations. Adv Neonatal Care. 2011;11:37–42.
Nowakowski L, Barfield W, Kroelinger C, Lauver C, Lawler M, White V, et al. Assessment of state measures of risk appropriate care for very low birth weight infants and recommendations for enhancing regionalized systems. Matern Child Health J. 2012;16:217–27.
Bezner S, Bernstein I, Oldham K, Goldin A, Fischer A, Chen L. Pediatric surgeons’ attitudes toward regionalization of neonatal surgical care. J Pediatr Surg. 2014;49:1475–79.
Shah V, Warre R, Lee S. Quality improvement initiatives in neonatal intensive care unit networks: achievements and challenges. Acad Pediatr. 2013;13:S75–S83.
Hall R, Hall-Barrow J, Garcia-Rill E. Neonatal regionalization through telemedicine using a community based research and education core facility. Ethn Dis. 2010;20:136–40.
Kim E, Teague-Ross T, Greenfield W, Williams D, Kuo D, Hall R. Telemedicine collaboration improves perinatal regionalization and lowers statewide infant mortality. J Perinatol. 2013;33:725–30.
Okoroh E, Kroelinger C, Goodman D, Lasswell S, Williams A, Barfield W. United States and Territory policies supporting maternal and neonatal transfer: review of transport and reimbursement. J Perinatol. 2016;36:30–34.
Dukhovny D, Dukhovny S, Pursley D, Escobar G, McCormick M, Mao W. The impact of maternal characteristics on the moderately premature infant: an antenatal maternal transport clinical prediction rule. J Perinatol. 2012;32:532–38.
Gould J, Danielsen B, Bollman L, Hackel A, Murphy B. Estimating the quality of neonatal transport in California. J Perinatol. 2013;33:964–70.
Stroud M, Trautman M, Meyer K, Moss M, Schwartz H, Bigham M, et al. Pediatric and neonatal interfacility transport: results from a national consensus conference. Pediatrics. 2013;132:359–66.
McCoy M, Makkar A, Foulks A, Legako E. Establishing level II neonatal services in Southwestern Oklahoma. J Oklahoma Med Assoc. 2014;107:493–96.
Okoroh E, Kroelinger C, Smith A, Goodman D, Barfield W. US and territory telemedicine policies: identifying gaps in perinatal care. Am J Obstet Gynecol. 2016;215:772e.771–76.
Brantley M, Davis N, Goodman D, Callaghan W, Barfield W. Perinatal regionalization: a geospatial view of perinatal clinical care, United States, 2010–2013. Am J Obstet Gynecol. 2017;216:185e.181–185e.110.
Acknowledgements
We would like to acknowledge the data abstractors for contributing to the body of this work: Mary Charlotte Tate, Kim Tubbs Ramsay, Renyea M. Colvin, MPH, and Tracie Herold, LCSW. We would also like to thank Evelyn Interis, MPH, and Amy M. Williams, MPH, for the literature search and review, and Elizabeth Martin for facilitating management and coordination of the data abstractors and researchers. Finally, we would like to acknowledge the contributions of Alex Monroe Smith, who validated the data tables for this paper.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Kroelinger, C.D., Okoroh, E.M., Goodman, D.A. et al. Comparison of state risk-appropriate neonatal care policies with the 2012 AAP policy statement. J Perinatol 38, 411–420 (2018). https://doi.org/10.1038/s41372-017-0006-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-017-0006-6
- Springer Nature America, Inc.
This article is cited by
-
NICUs in the US: levels of acuity, number of beds, and relationships to population factors
Journal of Perinatology (2023)
-
Seven years later: state neonatal risk-appropriate care policy consistency with the 2012 American Academy of Pediatrics Policy
Journal of Perinatology (2022)
-
Trends in neonatal intensive care unit admissions by race/ethnicity in the United States, 2008–2018
Scientific Reports (2021)
-
Designation of neonatal levels of care: a review of state regulatory and monitoring policies
Journal of Perinatology (2020)