Abstract
Background/Objectives:
Idiopathic intracranial hypertension (IIH) is a condition of increased intracranial pressure (ICP) without identifiable cause. The majority of IIH patients are obese, which suggests a connection between ICP and obesity. The aim of the study was to compare ICP in lean and obese rats. We also aimed to clarify if any ICP difference could be attributed to changes in some well-known ICP modulators; retinol and arterial partial pressure of CO2 (pCO2). Another potential explanation could be differences in water transport across the choroid plexus (CP) epithelia, and thus we furthermore investigated expression profiles of aquaporin 1 (AQP1) and Na/K ATPase.
Methods:
ICP was measured in obese and lean Zucker rats over a period of 28 days. Arterial pCO2 and serum retinol were measured in serum samples. The CPs were isolated, and target messenger RNA (mRNA) and protein were analyzed by quantitative PCR and western blot, respectively.
Results:
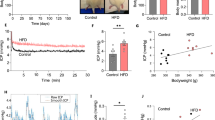
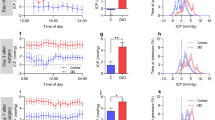
Obese rats had elevated ICP compared to lean controls on all recording days except day 0 (P<0.001). Serum retinol (P=0.35) and arterial pCO2 (P=0.16) did not differ between the two groups. Both AQP1 mRNA and protein levels were increased in the CP of the obese rats compared to lean rats (P=0.0422 and P=0.0281). There was no difference in Na/K ATPase mRNA or protein levels (P=0.2688 and P=0.1304).
Conclusion:
Obese Zucker rats display intracranial hypertension and increased AQP1 expression in CP compared to lean controls. The mechanisms behind these changes are still unknown, but appear to be unrelated to altered pCO2 levels or retinol metabolism. This indicates that the increase in ICP might be related to increased AQP1 levels in CP. Although further studies are warranted, obese Zucker rats could potentially model some aspects of the IIH pathophysiology.




Similar content being viewed by others
References
Friedman DI, Jacobson DM . Idiopathic intracranial hypertension. J Neuroophthalmol 2004; 24: 138–145.
Markey KA, Mollan SP, Jensen RH, Sinclair AJ . Understanding idiopathic intracranial hypertension: mechanisms, management, and future directions. Lancet Neurol 2016; 15: 78–91.
Sinclair AJ, Burdon MA, Nightingale PG, Ball AK, Good P, Matthews TD et al. Low energy diet and intracranial pressure in women with idiopathic intracranial hypertension: prospective cohort study. BMJ 2010; 341: c2701.
Skau M, Sander B, Milea D, Jensen R . Disease activity in idiopathic intracranial hypertension: a 3-month follow-up study. J Neurol 2011; 258: 277–283.
Sugerman HJ, Felton WL 3rd, Salvant JB Jr., Sismanis A, Kellum JM . Effects of surgically induced weight loss on idiopathic intracranial hypertension in morbid obesity. Neurology 1995; 45: 1655–1659.
Wong R, Madill SA, Pandey P, Riordan-Eva P . Idiopathic intracranial hypertension: the association between weight loss and the requirement for systemic treatment. BMC Ophthalmol 2007; 7: 15.
Warner JEA, Larson AJ, Bhosale P, Digre KB, Henley C, Alder SC et al. Retinol-binding protein and retinol analysis in cerebrospinal fluid and serum of patients with and without idiopathic intracranial hypertension. J Neuroophthalmol 2007; 27: 258–262.
Warner JE, Bernstein PS, Yemelyanov A, Alder SC, Farnsworth ST, Digre KB . Vitamin A in the cerebrospinal fluid of patients with and without idiopathic intracranial hypertension. Ann Neurol 2002; 52: 647–650.
Tabassi A, Salmasi AH, Jalali M . Serum and CSF vitamin A concentrations in idiopathic intracranial hypertension. Neurology 2005; 64: 1893–1896.
Selhorst JB, Kulkantrakorn K, Corbett JJ, Leira EC, Chung SM . Retinol-binding protein in idiopathic intracranial hypertension (IIH). J Neuroophthalmol 2000; 20: 250–252.
Jacobson DM, Berg R, Wall M, Digre KB, Corbett JJ, Ellefson RD . Serum vitamin A concentration is elevated in idiopathic intracranial hypertension. Neurology 1999; 53: 1114–1118.
Fishman RA . Polar bear liver, vitamin A, aquaporins, and pseudotumor cerebri. Ann Neurol 2002; 52: 531–533.
el Ouahabi A, Lorenzo AV, Black PM . Study of pseudotumor cerebri in vitamin A deficient rabbit. Eur J Pediatr Surg 1992; 2 (Suppl 1): 43–44.
Maddux GW, Foltz FM, Nelson SR . Effect of vitamin A intoxication on intracranial pressure and brain water in rats. J Nutr 1974; 104: 478–482.
Corey JE, Hayes KC . Cerebrospinal fluid pressure, growth, and hematology in relation to retinal status of the rat in acute vitamin A deficiency. J Nutr 1972; 102: 1585–1593.
Kuenzel WJ, Rowland AM, Pillai PB, O'Connor-Dennie TI, Emmert JL, Wideman RF . The use of vitamin A-deficient diets and jugular vein ligation to increase intracranial pressure in chickens (Gallus gallus. Poult Sci 2006; 85: 537–545.
Stiebel-Kalish H, Eyal S, Steiner I . The role of aquaporin-1 in idiopathic and drug-induced intracranial hypertension. Med Hypotheses 2013; 81: 1059–1062.
Damkier HH, Brown PD, Praetorius J . Cerebrospinal fluid secretion by the choroid plexus. Physiol Rev 2013; 93: 1847–1892.
Zhang YY, Proenca R, Maffei M, Barone M, Leopold L, Friedman JM . Positional cloning of the mouse obese gene and its human homolog. Nature 1994; 372: 425–432.
Chua SC, White DW, WuPeng XS, Liu SM, Okada N, Kershaw EE et al. Phenotype of fatty due to Gln269Pro mutation in the leptin receptor (Lepr). Diabetes 1996; 45: 1141–1143.
Chua SC Jr., Chung WK, Wu-Peng XS, Zhang Y, Liu SM, Tartaglia L et al. Phenotypes of mouse diabetes and rat fatty due to mutations in the OB (leptin) receptor. Science 1996; 271: 994–996.
Uldall M, Juhler M, Skjolding AD, Kruuse C, Jansen-Olesen I, Jensen R . A novel method for long-term monitoring of intracranial pressure in rats. J Neurosci Methods 2014; 227: 1–9.
Gevers EF, Wit JM, Robinson IC . Effects of long-term gonadotrophin-releasing hormone analog treatment on growth, growth hormone (GH) secretion, GH receptors, and GH-binding protein in the rat. Pediatr Res 1998; 43: 111–120.
Arakaki X, McCleary P, Techy M, Chiang J, Kuo L, Fonteh AN et al. Na,K-ATPase alpha isoforms at the blood-cerebrospinal fluid-trigeminal nerve and blood-retina interfaces in the rat. Fluids Barriers CNS 2013; 10: 14.
Deborah I, Friedman PI, Crabtree P Comparison of Intracranial Pressure in Zucker Fatty Rats and Sprague-Dawley Rats. North American Neuro-Ophthalmology Society Annual Meeting #23, 1997. Poster presentation, 10 (session 2).
Delamere NA, Tamiya S . Expression, regulation and function of Na,K-ATPase in the lens. Prog Retin Eye Res 2004; 23: 593–615.
van Hulst RA, Hasan D, Lachmann B . Intracranial pressure, brain PCO2, PO2, and pH during hypo- and hyperventilation at constant mean airway pressure in pigs. Intensive Care Med 2002; 28: 68–73.
Brian JE Jr . Carbon dioxide and the cerebral circulation. Anesthesiology 1998; 88: 1365–1386.
Zhou W, Liu W . Hypercapnia and hypocapnia in neonates. World J Pediatr 2008; 4: 192–196.
Dennis LJ, Mayer SA . Diagnosis and management of increased intracranial pressure. Neurol India 2001; 49 (Suppl 1): S37–S50.
Osmond JM, Mintz JD, Stepp DW . Preventing increased blood pressure in the obese Zucker rat improves severity of stroke. Am J Physiol Heart Circ Physiol 2010; 299: H55–H61.
Institoris A, Snipes JA, Katakam PV, Domoki F, Boda K, Bari F et al. Impaired vascular responses of insulin-resistant rats after mild subarachnoid hemorrhage. Am J Physiol Heart Circ Physiol 2011; 300: H2080–H2087.
Bouma GJ, Muizelaar JP, Bandoh K, Marmarou A . Blood pressure and intracranial pressure-volume dynamics in severe head injury: relationship with cerebral blood flow. J Neurosurg 1992; 77: 15–19.
Lilja A, Andresen M, Hadi A, Christoffersen D, Juhler M . Clinical experience with telemetric intracranial pressure monitoring in a Danish neurosurgical center. Clin Neurol Neurosurg 2014; 120: 36–40.
Headache Classification Committee of the International Headache Society (IHS).. The International Classification of Headache Disorders, 3rd edition (beta version). Cephalalgia 2013; 33: 629–808.
Rangel-Castilla L, Gopinath S, Robertson CS . Management of intracranial hypertension. Neurol Clin 2008; 26: 521–541, x.
Dunn LT . Raised intracranial pressure. J Neurol Neurosurg Psychiatry 2002; 73 (Suppl 1): i23–i27.
Brosche TM . Intracranial pressure and cerebral perfusion pressure ranges. Crit Care Nurse 2011; 31: 18–19 author's reply 9.
Andresen M, Juhler M . Intracranial pressure following complete removal of a small demarcated brain tumor: a model for normal intracranial pressure in humans. J Neurosurg 2014; 121: 797–801.
Fellmann L, Nascimento AR, Tibirica E, Bousquet P . Murine models for pharmacological studies of the metabolic syndrome. Pharmacol Ther 2013; 137: 331–340.
Acknowledgements
The current study was funded by the University of Copenhagen, The Research Foundation of The Capital Region, The A.P Møller Foundation for the Advancement of Medical Science, Aase and Ejnar Danielsen Foundation, and Foundation for Research in Neurology.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Uldall, M., Bhatt, D., Kruuse, C. et al. Choroid plexus aquaporin 1 and intracranial pressure are increased in obese rats: towards an idiopathic intracranial hypertension model?. Int J Obes 41, 1141–1147 (2017). https://doi.org/10.1038/ijo.2017.83
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2017.83
- Springer Nature Limited
This article is cited by
-
CSF hyperdynamics in rats mimicking the obesity and androgen excess characteristic of patients with idiopathic intracranial hypertension
Fluids and Barriers of the CNS (2024)
-
Modelling idiopathic intracranial hypertension in rats: contributions of high fat diet and testosterone to intracranial pressure and cerebrospinal fluid production
Fluids and Barriers of the CNS (2023)
-
The impact of obesity-related raised intracranial pressure in rodents
Scientific Reports (2022)
-
Understanding the link between obesity and headache- with focus on migraine and idiopathic intracranial hypertension
The Journal of Headache and Pain (2021)
-
Long-term monitoring of intracranial pressure in freely-moving rats; impact of different physiological states
Fluids and Barriers of the CNS (2020)