Abstract
Background/Objectives:
Studies concerning the glycaemic response to oral glucose, or meals in obesity have usually failed to account for gastric emptying. It has been suggested that the incretin effect may be diminished in obesity as a result of a reduction in glucagon-like peptide-1 (GLP-1) secretion. We sought to determine the effect of two different rates of intraduodenal glucose infusions on glycaemic, insulinaemic and incretin hormone responses in lean and obese subjects and compare the effects of oral and intraduodenal glucose in obese subjects.
Subjects/Methods:
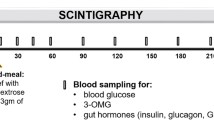
Eleven obese subjects (age 37.5±4.1 years, body mass index (BMI) 35.7±1.4 kg m−2) and 12 controls (age 34.7±4.0 years, BMI 23.9±0.7 kg m−2) received intraduodenal infusions of glucose at 1 or 3 kcal min−1, or saline for 60 min (t=0–60 min), followed by intraduodenal saline (t=60–120 min). In obese subjects, an oral glucose tolerance test was performed. Blood glucose, serum insulin, plasma total GLP-1 and total gastric inhibitory polypeptide (GIP) were measured.
Results:
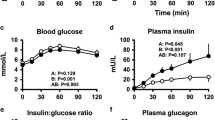
In both the groups (P<0.001), the incremental areas under the curve (iAUC)0–60 min for glucose was greater with the 3 kcal min−1 than the 1 kcal min−1 infusion; the iAUC0–120 min for glucose during 3 kcal min−1 was greater (P<0.05), in the obese. Insulin responses to 1 kcal min−1 and, particularly, 3 kcal min−1 were greater (P<0.001) in the obese. Stimulation of GLP-1 and GIP were greater (P<0.001) in response to 3 kcal min−1, compared with 1 kcal min−1 and saline, without any difference between the groups. In the obese, glycaemic, insulinaemic and GIP, but not GLP-1, responses to oral and intraduodenal glucose were related (P<0.05).
Conclusions:
The rate of duodenal glucose delivery is a major determinant of glycaemia, insulinaemia and incretin hormone release in obese subjects. Obesity is not apparently associated with impaired GLP-1 secretion.



Similar content being viewed by others
References
Utzschneider KM, Prigeon RL, Faulenbach MV, Tong J, Carr DB, Boyko EJ et al. Oral disposition index predicts the development of future diabetes above and beyond fasting and 2-h glucose levels. Diabetes Care 2009; 32: 335–341.
Aulinger BA, Vahl TP, Prigeon RL, D'Alessio DA, Elder DA . The incretin effect in obese adolescents with and without type 2 diabetes: impaired or intact? Am J Physiol Endocrinol Metab 2016; 310: E774–E781.
Muscelli E, Mari A, Casolaro A, Camastra S, Seghieri G, Gastaldelli A et al. Separate impact of obesity and glucose tolerance on the incretin effect in normal subjects and type 2 diabetic patients. Diabetes 2008; 57: 1340–1348.
Verdich C, Toubro S, Buemann B, Lysgard Madsen J, Juul Holst J, Astrup A . The role of postprandial releases of insulin and incretin hormones in meal-induced satiety—effect of obesity and weight reduction. Int J Obes Relat Metab Disord 2001; 25: 1206–1214.
Carr RD, Larsen MO, Jelic K, Lindgren O, Vikman J, Holst JJ et al. Secretion and dipeptidyl peptidase-4-mediated metabolism of incretin hormones after a mixed meal or glucose ingestion in obese compared to lean, nondiabetic men. J Clin Endocrinol Metab 2010; 95: 872–878.
Faerch K, Torekov SS, Vistisen D, Johansen NB, Witte DR, Jonsson A et al. GLP-1 response to oral glucose is reduced in prediabetes, screen-detected type 2 diabetes, and obesity and influenced by sex: the ADDITION-PRO Study. Diabetes 2015; 64: 2513–2525.
Chanoine JP, Mackelvie KJ, Barr SI, Wong AC, Meneilly GS, Elahi DH . GLP-1 and appetite responses to a meal in lean and overweight adolescents following exercise. Obesity (Silver Spring) 2008; 16: 202–204.
Vilsboll T, Krarup T, Sonne J, Madsbad S, Volund A, Juul AG et al. Incretin secretion in relation to meal size and body weight in healthy subjects and people with type 1 and type 2 diabetes mellitus. J Clin Endocrinol Metab 2003; 88: 2706–2713.
Sarson DL, Kopelman PG, Besterman HS, Pilkington TR, Bloom SR . Disparity between glucose-dependent insulinotropic polypeptide and insulin responses in obese man. Diabetologia 1983; 25: 386–391.
Stock S, Leichner P, Wong AC, Ghatei MA, Kieffer TJ, Bloom SR et al. Ghrelin, peptide YY, glucose-dependent insulinotropic polypeptide, and hunger responses to a mixed meal in anorexic, obese, and control female adolescents. J Clin Endocrinol Metab 2005; 90: 2161–2168.
Nauck MA, Heimesaat MM, Orskov C, Holst JJ, Ebert R, Creutzfeldt W . Preserved incretin activity of glucagon-like peptide 1 [7-36 amide] but not of synthetic human gastric inhibitory polypeptide in patients with type-2 diabetes mellitus. J Clin Invest 1993; 91: 301–307.
Knop FK, Aaboe K, Vilsboll T, Volund A, Holst JJ, Krarup T et al. Impaired incretin effect and fasting hyperglucagonaemia characterizing type 2 diabetic subjects are early signs of dysmetabolism in obesity. Diabetes Obes Metab 2012; 14: 500–510.
Horowitz M, Edelbroek MA, Wishart JM, Straathof JW . Relationship between oral glucose tolerance and gastric emptying in normal healthy subjects. Diabetologia 1993; 36: 857–862.
Marathe CS, Horowitz M, Trahair LG, Wishart JM, Bound M, Lange K et al. Relationships of early and late glycemic responses with gastric emptying during an oral glucose tolerance test. J Clin Endocrinol Metab 2015; 100: 3565–3571.
Jones KL, Horowitz M, Carney BI, Wishart JM, Guha S, Green L . Gastric emptying in early noninsulin-dependent diabetes mellitus. J Nucl Med 1996; 37: 1643–1648.
Trahair LG, Horowitz M, Marathe CS, Lange K, Standfield S, Rayner CK et al. Impact of gastric emptying to the glycemic and insulinemic responses to a 75-g oral glucose load in older subjects with normal and impaired glucose tolerance. Physiol Rep 2014; 2: e12204.
Collins PJ, Horowitz M, Cook DJ, Harding PE, Shearman DJ . Gastric emptying in normal subjects—a reproducible technique using a single scintillation camera and computer system. Gut 1983; 24: 1117–1125.
Corvilain B, Abramowicz M, Fery F, Schoutens A, Verlinden M, Balasse E et al. Effect of short-term starvation on gastric emptying in humans: relationship to oral glucose tolerance. Am J Physiol 1995; 269 (4 Pt 1): G512–G517.
Seimon RV, Brennan IM, Russo A, Little TJ, Jones KL, Standfield S et al. Gastric emptying, mouth-to-cecum transit, and glycemic, insulin, incretin, and energy intake responses to a mixed-nutrient liquid in lean, overweight, and obese males. Am J Physiol Endocrinol Metab 2013; 304: E294–E300.
Pilichiewicz AN, Chaikomin R, Brennan IM, Wishart JM, Rayner CK, Jones KL et al. Load-dependent effects of duodenal glucose on glycemia, gastrointestinal hormones, antropyloroduodenal motility, and energy intake in healthy men. Am J Physiol Endocrinol Metab 2007; 293: E743–E753.
Trahair LG, Horowitz M, Rayner CK, Gentilcore D, Lange K, Wishart JM et al. Comparative effects of variations in duodenal glucose load on glycemic, insulinemic, and incretin responses in healthy young and older subjects. J Clin Endocrinol Metab 2012; 97: 844–851.
Ma J, Pilichiewicz AN, Feinle-Bisset C, Wishart JM, Jones KL, Horowitz M et al. Effects of variations in duodenal glucose load on glycaemic, insulin, and incretin responses in type 2 diabetes. Diabet Med 2012; 29: 604–608.
Marathe CS, Feinle-Bisset C, Pilichiewicz A, Lange K, Jones KL, Rayner CK et al. The duodenal glucose load impacts the oral disposition index in healthy subjects. Diabet Med 2015; 32: 1500–1503.
Heddle R, Dent J, Toouli J, Read NW . Topography and measurement of pyloric pressure waves and tone in humans. Am J Physiol 1988; 255 (4 Pt 1): G490–G497.
Alberti KG, Zimmet PZ . Definition, diagnosis and classification of diabetes mellitus and its complications. Part 1: diagnosis and classification of diabetes mellitus provisional report of a WHO consultation. Diabet Med 1998; 15: 539–553.
Steinert RE, Landrock MF, Ullrich SS, Standfield S, Otto B, Horowitz M et al. Effects of intraduodenal infusion of the branched-chain amino acid leucine on ad libitum eating, gut motor and hormone functions, and glycemia in healthy men. Am J Clin Nutr 2015; 102: 820–827.
Levy JC, Matthews DR, Hermans MP . Correct homeostasis model assessment (HOMA) evaluation uses the computer program. Diabetes Care 1998; 21: 2191–2192.
Ghoos YF, Maes BD, Geypens BJ, Mys G, Hiele MI, Rutgeerts PJ et al. Measurement of gastric emptying rate of solids by means of a carbon-labeled octanoic acid breath test. Gastroenterology 1993; 104: 1640–1647.
Abdul-Ghani MA, Matsuda M, Balas B, DeFronzo RA . Muscle and liver insulin resistance indexes derived from the oral glucose tolerance test. Diabetes Care 2007; 30: 89–94.
Deacon CF, Ahren B . Physiology of incretins in health and disease. Rev Diabet Stud 2011; 8: 293–306.
Nguyen NQ, Debreceni TL, Bambrick JE, Chia B, Wishart J, Deane AM et al. Accelerated intestinal glucose absorption in morbidly obese humans: relationship to glucose transporters, incretin hormones, and glycemia. J Clin Endocrinol Metab 2015; 100: 968–976.
Park MI, Camilleri M, O'Connor H, Oenning L, Burton D, Stephens D et al. Effect of different macronutrients in excess on gastric sensory and motor functions and appetite in normal-weight, overweight, and obese humans. Am J Clin Nutr 2007; 85: 411–418.
Horner KM, Byrne NM, Cleghorn GJ, King NA . Influence of habitual physical activity on gastric emptying in healthy males and relationships with body composition and energy expenditure. Br J Nutr 2015; 114: 489–496.
Vazquez Roque MI, Camilleri M, Stephens DA, Jensen MD, Burton DD, Baxter KL et al. Gastric sensorimotor functions and hormone profile in normal weight, overweight, and obese people. Gastroenterology 2006; 131: 1717–1724.
Phillips WT . Gastric emptying in ethnic populations: possible relationship to development of diabetes and metabolic syndrome. Ethn Dis 2006; 16: 682–692.
Jagannathan R, Sevick MA, Li H, Fink D, Dankner R, Chetrit A et al. Elevated 1-hour plasma glucose levels are associated with dysglycemia, impaired beta-cell function, and insulin sensitivity: a pilot study from a real world health care setting. Endocrine 2016; 52: 172–175.
Abdul-Ghani MA, Abdul-Ghani T, Ali N, Defronzo RA . One-hour plasma glucose concentration and the metabolic syndrome identify subjects at high risk for future type 2 diabetes. Diabetes Care 2008; 31: 1650–1655.
Mignone LE, Wu T, Horowitz M, Rayner CK . Whey protein: the 'whey' forward for treatment of type 2 diabetes? World J Diabetes 2015; 6: 1274–1284.
Weiss R, D'Adamo E, Santoro N, Hershkop K, Caprio S . Basal alpha-cell up-regulation in obese insulin-resistant adolescents. J Clin Endocrinol Metab 2011; 96: 91–97.
Feinle C, Chapman IM, Wishart J, Horowitz M . Plasma glucagon-like peptide-1 (GLP-1) responses to duodenal fat and glucose infusions in lean and obese men. Peptides 2002; 23: 1491–1495.
Wu T, Ma J, Bound MJ, Checklin H, Deacon CF, Jones KL et al. Effects of sitagliptin on glycemia, incretin hormones, and antropyloroduodenal motility in response to intraduodenal glucose infusion in healthy lean and obese humans and patients with type 2 diabetes treated with or without metformin. Diabetes 2014; 63: 2776–2787.
Stengel A, Goebel-Stengel M, Teuffel P, Hofmann T, Busse P, Kobelt P et al. Obese patients have higher circulating protein levels of dipeptidyl peptidase IV. Peptides 2014; 61: 75–82.
Nauck MA, Vardarli I, Deacon CF, Holst JJ, Meier JJ . Secretion of glucagon-like peptide-1 (GLP-1) in type 2 diabetes: what is up, what is down? Diabetologia 2011; 54: 10–18.
Hausken T, Odegaard S, Matre K, Berstad A . Antroduodenal motility and movements of luminal contents studied by duplex sonography. Gastroenterology 1992; 102: 1583–1590.
Acknowledgements
We would like to acknowledge Mrs Rachael Tippett (Discipline of Medicine, University of Adelaide) for providing technical assistance with the studies. This study was supported by the National Health and Medical Research Council (NHMRC) of Australia (grant 627189). KLJ’s salary is funded by an NHMRC Senior Career Development Award (grant 627011) and CFB’s salary is funded by an NHMRC Senior Research Fellowship (grant 1103020). LGT was supported by an Australian Postgraduate Award and a Dawes scholarship from the Royal Adelaide Hospital.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
MH has participated in the advisory boards and/or symposia for Novo Nordisk, Sanofi, Novartis, Eli Lilly, Merck Sharp and Dohme, Boehringer Ingelheim and AstraZeneca, and has received honoraria for this activity. CKR has received research funding from Merck, AstraZeneca and Novartis. The remaining authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Trahair, L., Marathe, C., Standfield, S. et al. Effects of small intestinal glucose on glycaemia, insulinaemia and incretin hormone release are load-dependent in obese subjects. Int J Obes 41, 225–232 (2017). https://doi.org/10.1038/ijo.2016.202
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ijo.2016.202
- Springer Nature Limited