Abstract
Some reports have suggested that inflammation in perivascular adipose tissue (PVAT) may be implicated in vascular dysfunction by causing the disappearance of an anticontractile effect. The aim of this study was to investigate the effects of chronic melatonin treatment on the functional responses of the small mesenteric arteries and on the expression of markers of inflammation/oxidative stress in the aortas of senescence-accelerated prone mice (SAMP8), a model of age-related vascular dysfunction. We investigated seven SAMP8 and seven control senescence-accelerated resistant mice (SAMR1) treated for 10 months with melatonin, as well as equal numbers of age-matched untreated SAMP8 and SAMR1. The mesenteric small resistance arteries were dissected and mounted on a wire myograph, and the concentration–response to norepinephrine was evaluated in vessels with intact PVAT and after the removal of the PVAT. The expression of markers of oxidative stress, inflammation and aging in the aortas was evaluated by immunostaining. In addition, the adiponectin content and the expression of adiponectin receptor 1 were evaluated in the visceral adipose tissue. In untreated SAMP8 mice, we observed an overexpression of oxidative stress and inflammatory markers in the vasculature compared with the controls. No anticontractile effect of the PVAT was observed in untreated SAMP8 mice. Long-term treatment of SAMP8 mice with melatonin increased the expression of some markers of vasoprotection, decreased oxidative stress and inflammation and restored the anticontractile effect of the PVAT. Decreased expression of adiponectin and adiponectin receptor 1 was also observed in visceral fat of untreated SAMP8, whereas a significant increase was observed after melatonin treatment.
Similar content being viewed by others
Introduction
Physiological aging is associated with progressive changes in the mechanical properties of the large arteries, namely decreased distensibility and increased stiffness.1, 2, 3, 4 Alterations at the microvascular level may also occur, in terms of capillary rarefaction and the onset of vascular remodeling.4 The aging process is associated with changes in the vasculature at the cellular and molecular levels. Specifically, low-grade oxidative stress and inflammation are possible underlying mechanisms that may trigger physiological and early vascular aging.5, 6 The senescence-accelerated prone mouse (SAMP8) strain is a model of age-related vascular dysfunction and cognitive decline.7, 8, 9 Several studies have suggested that the SAMP8 strain is one of the most appropriate animal models for the study of vascular aging and age-associated diseases10, 11 because it shows pronounced morphological alterations, oxidative stress, inflammation, mechanical and endothelial dysfunctions10, 12, 13, 14, 15 and vascular alterations comparable to those induced by aging in humans.7, 14
Healthy adipose tissue produces a paracrine anticontractile effect through the release of vasodilator adipokines.16, 17, 18 Central to this action is the production of adiponectin.16, 19, 20, 21 However, the bioavailability of this vasodilatory molecule is compromised in obese subjects, in whom adipocyte hypertrophy is associated with increases in oxidative stress and local inflammation.16, 22, 23, 24, 25, 26, 27 Furthermore, fat accumulation may accelerate aging, at least at the tissue/organ levels, through oxidative stress-mediated processes.28, 29, 30 Aging is typically characterized by a decline in the fat-free mass and an altered adipose tissue distribution that is characterized by increased central and visceral adiposity.31, 32, 33
Melatonin is an endogenous indoleamine that has a well-demonstrated influence on circadian and seasonal rhythms,34, 35 sleep–wake cycles,36 the cardiovascular37, 38 and immune systems39 and endocrine regulation40, 41 with a broad spectrum of functions.6, 42, 43 In a previous study, significant improvements in the mesenteric small resistance artery structure and endothelial function have been observed in rats treated with melatonin.44 Similarly, melatonin restores the anticontractile activity of the perivascular adipose tissue (PVAT) in obese mice, possibly through an increase in adiponectin production/adiponectin receptor expression.27 Moreover, a decrease in the circulating melatonin levels and/or a dysfunction of melatonergic signaling are associated with a remarkable number of age-related diseases.45 In fact, the aging process in humans is associated with a progressive reduction in serum melatonin concentrations46 as well as the ability of endogenous melatonin to beneficially affect the circadian blood pressure profile.47 Thus, melatonin or synthetic melatonergic agonists are expected to be beneficial in normal or pathological aging.
For these reasons, aging may affect the anticontractile effects of PVAT through increased vascular inflammation/oxidative stress, whereas melatonin may have potentially beneficial effects.
Therefore, we sought to evaluate the anticontractile properties of PVAT in the mesenteric small resistance arteries together with indices of inflammation/oxidative stress/vascular damage in aortas by investigating an animal model of vascular aging (SAMP8) after chronic oral treatment with melatonin.
Materials and methods
Experimental Design
A total of 28 male mice (14 SAMP8 and 14 SAMR1) at 6 weeks of age were included in the study. The SAMP8 strain, which shows accelerated aging, was compared with its control (senescence-accelerated mouse resistant 1—SAMR1). The animals, which were obtained from Harlan Laboratories Srl (San Pietro Al Natisone, Udine, Italy), were housed in a temperature-controlled animal facility with a 12 h:12 h light–dark cycle and with free access to rodent chow and water. The body weight and water consumption of the animals were continuously monitored throughout the study.
The mice were randomly divided into four groups:
-
1
Control SAMR1 mice kept untreated and killed at 1 year of age (SAMR1);
-
2
Control SAMP8 mice kept untreated and killed at 1 year of age (SAMP8);
-
3
SAMR1 mice treated with melatonin from the 6th week to 1 year of age (SAMR1+MEL);
-
4
SAMP8 mice treated with melatonin from the 6th week to 1 year of age (SAMP8+MEL).
Melatonin was dissolved in 1% ethanol and added to the drinking water for 10 months at a final dose of 10 mg kg−1 per day. It was administered in containers wrapped in aluminum foil, owing to the sensitivity of melatonin to light, and the drinking fluid was changed three times a week depending on the water consumption and the body weight of the animals.48 The dose and duration of treatment was chosen on the basis of previously published studies.1, 49, 50, 51 The protocols were approved by the Animal Care and Use Committee of the University of Brescia, Italy, and by the Italian Ministry of Health. At the end of the treatment, the animals were killed by cervical dislocation. The abdominal and thoracic aorta, including the aortic arch, the mesentery and the visceral perirenal adipose tissue were removed and washed briefly in phosphate-buffered saline with the following composition (in mmol l−1): (NaCl 137, KCl 2.7, Na2HPO4 10, KH2HPO4 2.0, pH 7.4). The aorta and the visceral adipose tissue were immediately fixed in 10% buffered formalin and embedded in paraffin wax according to a standard protocol; then, serial sections (7 μm thick) of each sample were cut with a microtome and used for morphometrical and immunostaining analyses. The mesenteric vascular bed was preserved for the micromyographic assay.
Morphometrical analyses
Alternate paraffin sections were deparaffinized, rehydrated and stained with hematoxylin–eosin, following a standard protocol. A minimum of 20 fields for five sections from each experimental animal were observed with an optical light microscope (Olympus, Hamburg, Germany) at a final magnification of × 400 by two observers blinded to the experimental treatment. Morphometric analysis was performed using a software program (Image Pro Premier 9.1, MediaCybernetics, Rockville, MD, USA) to evaluate the ratio of the areas of the tunica media/lumen (μm2) as a marker of vascular stenosis and hypertrophy.52
Immunofluorescence and immunohistochemical analysis
Alternate paraffin sections of both the aorta and visceral adipose tissue were deparaffinized, rehydrated and incubated in 1% bovine serum albumin (Sigma Aldrich, St Louis, MO, USA) for 1 h at room temperature. Then, the aorta sections were incubated for 1 h at room temperature and overnight at 4 °C with the following primary antibodies: rabbit polyclonal antibody against sirtuin 1 (SIRT1—final dilution 1:100; Santa Cruz Biotechnology, Santa Cruz,CA, USA); goat polyclonal antibody against endothelin-1 (ET-1—final dilution 1:500; Santa Cruz Biotechnology); mouse monoclonal antibody against cyclooxygenase 1 (COX-1—final dilution 1:600; Cayman Chemical, Ann Arbor, MI, USA); rabbit polyclonal antibody against cyclooxygenase 2 (COX2–final dilution 1: 1000; Cayman Chemical); rabbit polyclonal antibody against endothelial nitric oxide synthase (eNOS—final dilution 1:70; AnaSpec, San Josè, CA, USA); and rabbit polyclonal antibody against inducible nitric oxide synthase (iNOS—final dilution 1:250; Santa Cruz Biotechnology).
Furthermore, the alternate sections of the visceral adipose tissue were incubated with a rabbit polyclonal antibody against adiponectin (final dilution: 1:500; Abcam, Cambridge, UK) or a rabbit monoclonal antibody against adiponectin receptor 1 (ADIPOR1- final dilution: 1:400; Abcam). Thereafter, the sections, except for those used for the COX-1 assay, were labeled using anti-rabbit Alexa Fluor 488-, anti-goat Alexa Fluor 488- or anti-rabbit Alexa Fluor 546-conjugated secondary antibodies (final dilution 1:200; Invitrogen, Paisley, UK). Finally, the samples were counterstained with 4-6-diamidino-2-phenylindole, mounted and observed with a confocal microscope (LSM 510 Zeiss, Munich, Germany), as previously described.1, 27 For the COX-1 immunohistochemical analyses, after the incubation with the primary antibody, the aorta sections were sequentially incubated with a biotinylated anti-mouse immunoglobulin and then with an avidin–biotin peroxidase complex. The reaction products were visualized using 0.33% hydrogen peroxide with 0.05% 3,3′-diaminobenzidine tetrahydrochloride as the chromogen. The sections were finally counterstained with hematoxylin, mounted and observed with a light microscope (Olympus, Hamburg, Germany).53 The immunofluorescence and immunohistochemical negative controls were performed by replacing the primary antibodies with isotype-matched immunoglobulin G.
Twenty random fields, each with an area of 0.04 mm2, from a total of five sections for each experimental animal were analyzed, and the immunostaining for each primary antibody were calculated using an image analyzer (Image Pro Premier 9.1, MediaCybernetics, Rockville, MD, USA). The quantitative evaluation of each target of the immunostaining was performed by two blinded investigators, whose evaluation was assumed to be correct if the values were not significantly different. If there was disagreement concerning the interpretation, the case was reconsidered to reach a unanimous agreement. The levels of immunostaining were expressed as arbitrary units, except for the adiponectin and ADIPOR1 quantitative analyses, which were expressed as the immunostained percentage of the total area.
Wire micromyography
The mesenteric bed was immediately removed and placed in an ice-cold physiological salt solution (PSS) with the following composition (in mmol l−1): NaCl 119, NaHCO3 24, KCl 4.7, KH2PO4 1.18, MgSO4 1.17, CaCl2 2.5 and glucose 5.5. Second-order arteries were identified (diameter: 200–300 μm), and some of them were dissected away from the PVAT, whereas the remaining arteries were left with the surrounding PVAT intact. The mesenteric small arteries (2 mm length) with or without intact PVAT were mounted on 40-μm wires in a wire myograph (Danish Myo Technology, Aarhus, DK model 410A). After an initial 30-minute incubation, the vessel wall tension and diameter were normalized according to a standardized procedure54, 55, 56, 57, 58 and stabilized for 1 h.
Pharmacological assessment of contractility
The mesenteric small arteries with and without intact PVAT were studied using a wire myograph at 37 °C. The vessel bath was saturated by bubbling with 95% air/5% CO2 while the pH was maintained at 7.4, as described previously. The arterial viability was assessed by constriction with high-potassium (60 mmol l−1) PSS (KPSS), and the endothelial integrity was determined by addition of 1 × 10−5 mol l−1 acetylcholine. Constriction of the arteries with KPSS was performed after each dose response curve to norepinephrine (1 × 10−9 to 1 × 10−5 mol l−1), and the contractile responses were assessed as the percentage of maximum constriction with KPSS.
The response curves to norepinephrine were assessed in the experimental groups in arteries with intact PVAT (WF) as well as in vessels without PVAT (NoF).
Statistical analysis
All of the data are expressed and presented as the mean±s.d. unless otherwise stated. The differences in responses to norepinephrine are expressed as a percentage of vasoconstriction to high-potassium PSS and analyzed using a two-way analysis of variance for repeated measures (ANOVA), using one within factor (concentrations of norepinephrine) and one between factor (groups of mice). Probability values less than 0.05 were considered significant. Multiple-comparison corrections were performed. The analyses were performed with SPSS software (SPSS, version 13.0).
Results
The body weights during and after the experimental protocol showed no significant differences among the groups (data not shown).
Anticontractile effect of PVAT in mesenteric small resistance arteries
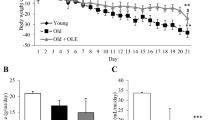
In SAMR1 control mice, an anticontractile effect of perivascular fat was present (WF vs. NoF: ANOVA P=0.04), whereas in aging SAMP8 mice, the effect was not detected (WF vs. NoF: ANOVA P=NS) (Figure 1). The long-term treatment with melatonin restored the anticontractile effect of PVAT in SAMP8 mice (WF vs. NoF ANOVA P=0.001), whereas in the melatonin-treated SAMR1 mice, the anticontractile effect of perivascular fat was similar to that observed in untreated SAMR1 mice (WF vs. NoF ANOVA P=0.04) (Figure 1). However, the contractile responses in the melatonin-treated SAMP8 mice were greater that those observed in untreated SAMP8 mice or in treated or untreated SAMR1 mice (ANOVA P<0.01).
(a) Concentration–response curve to norepinephrine in the mesenteric resistance arteries of SAMR1 mice. * SAMR1: Fat vs. No Fat: ANOVA P=0.04 (b) Concentration–response curve to norepinephrine in the mesenteric resistance arteries of SAMP8 mice. SAMP8 Fat vs. No Fat: ANOVA P=NS. (c) Concentration–response curve to norepinephrine in the mesenteric resistance arteries of SAMR1 mice: effect of melatonin. * SAMR1+MEL: Fat vs. No Fat: ANOVA P=0.04 (d) Concentration–response curve to norepinephrine in the mesenteric resistance arteries of SAMP8 mice: effect of melatonin. * SAMP8+MEL: Fat vs. No Fat: ANOVA P=0.001.
In SAMP8 mice that had been treated with melatonin, responses to KPSS were clearly reduced, particularly in the NoF vessels (untreated mice: SAMP8 WF: 2.12±1.37 mN mm−1, SAMP8 NoF: 3.11±2.66 mN mm−1, SAMR1 WF: 2.08±1.05 mN mm−1, SAMR1 NoF: 3.97±1.837 mN mm−1; after melatonin treatment: SAMP8 WF: 1.60±1.24 mN mm−1, SAMP8 NoF: 1.28±1.38 mN mm−1, P=0.04 vs. untreated SAMP8; P=0.0002 vs. untreated SAMR1, P=0.007 vs. SAMR1 treated with melatonin, SAMR1 WF 1.86±1.35 mN mm−1, SAMR1 NoF 3.47±2.24 mN mm−1).
Melatonin reduced aorta hypertrophy
The morphometrical analyses did not indicate differences among the three analyzed aorta segment locations (aortic arch, thoracic and abdominal aorta), so we defined all of these segments with the common term 'aorta'.
The histological appearance of the transverse aorta section showed that the tunica media thickness was significantly increased in the untreated SAMP8 group (Figure 2a), compared with treated and untreated SAMR1 mice (Figures 2b and c). The tunica media thickness in SAMP8 mice treated with melatonin was almost completely normalized, to a value similar to that measured in SAMR1 mice (Figures 2d and e).
Photomicrographs of the morphology of the aortas of untreated SAMP8 mice (a), untreated SAMR1 mice (b), SAMR1 mice treated with melatonin (c) and SAMP8 mice treated with melatonin (d) experimental groups. Hematoxylin–eosin staining. Bar: 20 μm. The graph shows the area of the tunica media/lumen ratio (e). MEL: melatonin; (l): lumen of the aorta. *P<0.05 vs. SAMP8.
Melatonin reduced markers of aging, oxidative stress and inflammation and restored the vasoactive factor balance in the aorta of aging mice
The SIRT1 content (identified in red) was significantly lower in untreated SAMP8 (Figure 3a) than in either the treated or untreated SAMR1 groups (Figures 3b and c). The melatonin treatment significantly increased SIRT1 expression in SAMP8 mice (Figure 3d). In particular, SIRT1 expression was very weak or absent in SAMP8 mice and moderate/strong in untreated and treated SAMR1 mice and in treated SAMP8 mice. The immunostaining was localized at the tunica intima and tunica media levels (at the nucleus and cytoplasm of endothelial and vascular smooth muscle cells). These observations were confirmed by the immunostaining measurements, which are summarized in Figure 3e.
Immunofluorescence photomicrographs of sirtuin 1 expression (SIRT1) (red staining) of the aortas of untreated SAMP8 mice (a), untreated SAMR1 mice (b), SAMR1 mice treated with melatonin (c) and SAMP8 mice treated with melatonin (d). The nuclei were stained with DAPI (blue). Bar 20 μm. The graph shows the histomorphometric analyses, expressed in arbitrary units (AU), for sirtuin 1 immunostaining (e). MEL: melatonin; (l): lumen of aorta. *P<0.05 vs. SAMP8.
A significant increase in the level of ET-1 (identified in green) was observed in untreated SAMP8 mice (Figure 4a) in which it was moderately/strongly expressed at the tunica media level compared with treated and untreated SAMR1 mice in which ET-1 was very weak/absent (Figures 4b and c). The expression of ET-1 was almost normalized in SAMP8 after treatment with melatonin (Figure 4d). ET-1 immunostaining was evident in the cytoplasm of the vascular smooth muscle cells of the tunica media, but there was no staining at the nuclear level. In Figure 4e, the morphometric analyses of ET-1 immunostaining are summarized.
Immunofluorescence photomicrographs of endothelin-1 expression (ET-1) (green staining) of the aortas of untreated SAMP8 mice (a), untreated SAMR1 mice (b), SAMR1 mice treated with melatonin (c) and SAMP8 mice treated with melatonin (d). The nuclei were stained with DAPI (blue). Bar: 20 μm. The graph shows the histomorphometric analyses, expressed in arbitrary units (AU), of endothelin-1 immunostaining (e). MEL: melatonin; (l): lumen of aorta. *P<0.05 vs. SAMP8, #P<0.05 vs. SAMR1 and +P<0.05 vs. SAMR1+MEL.
The expression of COX-1 was significantly lower in untreated SAMP8 mice (weak expression) (Figure 5a) than in treated and untreated SAMR1 mice (strong expression) (Figures 5b and c), but the COX-1 expression was increased in melatonin-treated SAMP8 mice (moderate expression) (Figure 5d). However, the opposite pattern was observed for COX2 expression (identified in red) (Figures 5e–h). Both COX-1 and COX2 were expressed mainly in the cytoplasm of endothelial and vascular smooth muscle cells of the tunica intima and tunica media, respectively. The quantitative immunostaining data for COX-1 and COX2 are summarized in Figures 5i and l, respectively.
Immunohistochemistry and immunofluorescence photomicrographs of cyclooxygenase 1 (COX1) (a–d) and cyclooxygenase 2 (COX2) (e–h) (red staining) expression of the aortas of untreated SAMP8 mice (a, e), untreated SAMR1 mice (b, f), SAMR1 mice treated with melatonin (c, g) and SAMP8 mice treated with melatonin (d, h). The nuclei were stained with DAPI (blue). Bar: 20 μm. The graphs show the histomorphometric analyses, expressed in arbitrary units (AU), of cyclooxygenase 1 (i) and cyclooxygenase 2 (l) immunostaining. MEL: melatonin; (l): lumen of aorta. *P<0.05 vs. SAMP8, #P<0.05 vs. SAMR1 and +P<0.05 vs. SAMR1+MEL.
eNOS expression (identified in green) was significantly lower in the untreated SAMP8 mice (weak expression) (Figure 6a), compared with the treated or untreated SAMR1 mice (moderate/strong expression) (Figures 6b and c), whereas in melatonin-treated SAMP8 mice, eNOS expression was significantly increased (moderate/strong expression) (Figure 6d). In contrast, iNOS expression (identified in green) was higher in untreated SAMP8 mice, which had moderate immunostaining (Figure 6e), whereas in treated or untreated SAMR1 mice, the signal was almost absent (Figures 6f and g). The level of iNOS was significantly decreased in melatonin-treated SAMP8 mice (weak expression) (Figure 6h). Notably, eNOS expression was localized only at the tunica intima level, whereas iNOS was present at the cytoplasmic level of vascular smooth muscle cells of the tunica media. Figures 6i and l summarize the analyses of the immunostaining for eNOS and iNOS, respectively.
Immunofluorescence photomicrographs of endothelial nitric oxide synthase (eNOS) (a–d) and inducible nitric oxide synthase (iNOS) (e–h) expression (green stainings) of the aortas of untreated SAMP8 mice (a, e), untreated SAMR1 mice (b, f), SAMR1 mice treated with melatonin (c, g) and SAMP8 mice treated with melatonin (d, h). The nuclei were stained with DAPI (blue). Bar: 20 μm. The graphs show the histomorphometric analyses, expressed in arbitrary units (AU), of endothelial nitric oxide synthase (i) and inducible nitric oxide synthase (l) immunostaining. MEL: melatonin; (l): lumen of aorta. *P<0.05 vs. SAMP8, #P<0.05 vs. SAMR1 and +P<0.05 vs. SAMR1+MEL.
Adiponectin and adiponectin receptor 1 expression in visceral adipose tissue
The adiponectin immunostaining and the expression of ADIPOR1 in the visceral adipose tissue were reduced in untreated SAMP8 mice (Figures 7a: both proteins are identified with red staining) compared with the untreated and treated SAMR1 mice (Figures 7b). Treatment with melatonin significantly increased the production of both proteins in SAMP8 mice (Figures 7d). Both proteins were expressed at the membrane level of the white adipocytes, and no immunostaining was observed at the nuclear level. The quantitative analyses of adiponectin and ADIPOR1 immunostaining are summarized in Figure 7i.
Immunofluorescence photomicrographs of the visceral adipose tissue adiponectin and adiponectin receptor 1 expression (ADIPOR1) (red stainings) of the untreated SAMP8 mice (a, e), untreated SAMR1 mice (b, f), SAMR1 mice treated with melatonin (c, g) and SAMP8 mice treated with melatonin (d, h). The nuclei were stained with DAPI (blue). Bar: 20 μm. The graph shows the histomorphometric analyses, expressed as the percentage of the total area, of adiponectin and adiponectin receptor 1 immunostaining (i). MEL: melatonin. *P<0.05 vs. SAMP8, #P<0.05 vs. SAMR1 and +P<0.05 vs. SAMR1+MEL.
Discussion
This study provides the first demonstration that a prolonged oral administration of melatonin is able to improve the anticontractile activity of PVAT in the mesenteric small resistance arteries of aging mice; moreover, we observed that melatonin improved the morphological alterations, oxidative stress and inflammation in the aortas of aging mice (SAMP8). A vasculoprotective effect of melatonin has previously been observed in spontaneously hypertensive rats44 and in obese mice.27 Specifically, the vasculoprotective responses include regression of the remodeling processes in mesenteric small resistance arteries,44 restoration of the anticontractile activity of PVAT27 and reduction in the vascular expression of markers of inflammation/damage (endothelin-1, interleukin 6 and metalloprotease 2 ref. 27) and of adipocyte inflammation.27
It is therefore probable that among the mechanisms that might be involved in the vasculoprotective effects of melatonin, a major role is played by antioxidant/anti-inflammatory effects, as suggested by our observation of a dramatic reduction of oxidative stress and the expression of vascular inflammatory markers as well as the restoration of a normal morphology of aortas and increases in the vasoactive factors and markers of normal aging. As described above, melatonin has been shown to exert antioxidant and anti-inflammatory actions,59, 60, 61 and previous studies have demonstrated that increased oxidative stress is responsible for the loss of the anticontractile function of the PVAT.16, 23
In our study, chronic treatment with melatonin restored the correct morphology of the aorta as indicated by significant reductions in the thickness and hypertrophy of the tunica media in SAMP8 mice. This improvement in the aortic remodeling was paralleled by a significant reduction in the expression of ET-1, which is a marker of vasoconstriction and vascular hypertrophy/damage, and by the restoration of eNOS expression, which is associated with an increase in the production of nitric oxide, thus promoting and improving endothelial cell survival and counteracting the deleterious effects of ET-1.
Lloréns et al.14 have shown that eNOS antibody staining of the aortic endothelial cells of SAMP8 mice is similar to that observed in SAMR1 endothelial cells, but a greater thoracic aorta contractility is present in SAMP8 tissues compared with those of SAMR1 mice. They have also reported that the aortas of both strains show similar smooth muscle cell layers and no evident signs of tunica media/lumen ratio alterations, in contrast to the observations in the present study. However, these discrepancies are likely to be because the Lloréns study14 was performed in animals younger (6–7 month old) than those investigated in the present study. Furthermore, the Lloréns study, found that the endothelium of SAMP8 mice is dysfunctional, as indicated by a lack of a normal capacity to counteract smooth muscle contraction.14
iNOS is widely recognized as a marker of oxidative stress,62 whereas eNOS is associated with NO production and vascular protection.63 Similarly, elevated COX2 expression suggests the presence of oxidative stress, whereas the opposite is true for COX-1.64
In our study, elevated expression of iNOS and COX2 confirmed the presence of increased oxidative stress and inflammation in the vasculature of untreated aging SAMP8 mice.
As previously described, the choices of vascular ET-1, iNOS, eNOS, COX-1 and COX2 as markers of inflammation/oxidative stress/vascular damage were justified because ET-1 has relevant roles in inducing vascular hypertrophy, cell damage and oxidative stress, whereas iNOS, eNOS, COX-1 and COX2 provide insights into vascular mechanisms by virtue of their opposing effects on the production of reactive oxygen species, nitric oxide and inflammatory mediators.
In recent years, scientific interest regarding SIRT1 has substantially increased. SIRT1 is a protein with anti-aging properties that belongs to the histone-deacetylase family. SIRT1 is involved in the aging process and seems to be able to retard aging and increase cell life span, through apoptosis inhibition, cell repair, stem-cell proliferation and protection of cells from various types of stress.65, 66 The increase in SIRT1 observed in the aortas of melatonin-treated SAMP8 mice is an interesting observation with possible important therapeutic interest and implications.
Similarly to the observations in our previous study on obese mice, an improvement of the anticontractile activity of PVAT after melatonin treatment has been found to be associated with an increased expression of adiponectin/adiponectin receptor 1.27 These effects may be interpreted as a direct effect of melatonin or an indirect response that may be secondary to a reduction in oxidative stress/inflammation.
From a therapeutic perspective, our data suggest several potential translational approaches for the management of aging; in particular, it may be of interest to examine the use of biologic molecules with antioxidant/anti-inflammatory properties, such as melatonin, with the intent of delaying physiological and pathological aging with a particular focus on early vascular aging.
A surprising and partially unexplained finding of our study was the observation of increased contractility of the mesenteric small arteries of SAMP8 mice after treatment with melatonin compared with those from untreated SAMP8 mice and treated or untreated SAMR1 mice. We expressed our contractile responses as a percentage of maximum constriction with KPSS and therefore did not normalize for possible differences in media thickness. We did not perform morphological evaluations in these vessels.
However, after treatment with melatonin, no increases in the wall or media thickness would be expected, on the basis of the observation that there is a decrease in vascular remodeling after melatonin treatment at least in spontaneously hypertensive rats.44 Because melatonin exerted antioxidant and anti-inflammatory effects, these possible sources of increased contractility are probably not involved. We therefore do not have a good explanation for this finding, although a possible confounding effect is the reduced maximal response to KPSS that occurred only in the melatonin-treated SAMP8 mice. Therefore, the increased contractile response to norepinephrine in this group may be, to some extent, artifactual. When the concentration–response curves for norepinephrine were expressed as absolute wall tension, not corrected for the KPSS-induced contraction, no increase in the contractility in the melatonin-treated SAMP8 mice was observed.
The issues of vascular inflammation/oxidative stress as well as possible pharmacological modulation/vascular protection are complex. Vascular oxidative stress induced by angiotensin II may be reduced by exogenous H2S treatment in animal models,67 whereas in humans, smoking cessation has been shown to be helpful.68 The possible roles of endothelial progenitor cells, mononuclear cells and mesenchymal stem cells, vascular endothelial growth factor, fibroblast growth factor and hepatocyte growth factor have been thoroughly investigated in clinical settings.69 A possible role may also be played though an immunological mechanism. Specifically, toll-like receptor 4 has been demonstrated to have an essential role in regulating the angiotensin II-induced vascular reactive oxygen species levels by inhibiting the expression and activity of the antioxidant enzyme superoxide dismutase as well as by activating NADPH oxidase, which enhances inflammation, thereby facilitating the progression of vascular remodeling.70
In conclusion, we demonstrated that melatonin treatment is associated with protective effects in terms of the vascular morphological alterations, expression of oxidative stress, inflammatory and aging markers and modulation of vasoactive factors. Importantly, we also provide the first evidence that the anticontractile properties of PVAT can be restored by melatonin treatment in an experimental animal model of aging, possibly through an increase in adiponectin production/activity at the visceral adipose tissue level.
References
Rodella LF, Favero G, Rossini C, Foglio E, Bonomini F, Reiter RJ, Rezzani R . Aging and vascular dysfunction: beneficial melatonin effects. Age (Dordr) 2013; 35: 103–115.
Wang M, Shah AM . Age-associated pro-inflammatory remodeling and functional phenotype in the heart and large arteries. J Mol Cell Cardiol 2015; 83: 101–111.
Palombo C, Kozakova M . Arterial stiffness, atherosclerosis and cardiovascular risk: pathophysiologic mechanisms and emerging clinical indications. Vascul Pharmacol 2015; 77: 1–7.
Early vascular aging New directions in cardiovascular protection . Nilsson OM, Olsen MH, Laurent S (eds). ISBN 9780128016763, Elsevier: Amsterdam. 2015.
Chen B, Lu Y, Chen Y, Cheng J . The role of Nrf2 in oxidative stress-induced endothelial injuries. J Endocrinol 2015; 225: R83–R99.
Reiter RJ, Tan DX, Galano A . Melatonin: exceeding expectations. Physiology (Bethesda) 2014; 29: 325–333.
Hosokawa M, Abe T, Higuchi K, Shimakawa K, Omori Y, Matsushita T, Kogishi K, Deguchi E, Kishimoto Y, Yasuoka K, Takeda T . Management and design of the maintenance of SAM mouse strains: an animal model for accelerated senescence and age-associated disorders. Exp Gerontol 1997; 32: 111–116.
Takeda T, Hosokawa M, Takeshita S, Irino M, Higuchi K, Matsushita T, Tomita Y, Yasuhira K, Hamamoto H, Shimizu K, Ishii M, Yamamuro T . A new murine model of accelerated senescence. Mech Ageing Dev 1981; 17: 183–194.
Takeda T . Senescence-accelerated mouse (SAM): a biogerontological resource in aging research. Neurobiol Aging 1999; 20: 105–110.
Butterfield DA, Poon HF . The senescence-accelerated prone mouse (SAMP8): a model of age-related cognitive decline with relevance to alterations of the gene expression and protein abnormalities in Alzheimer's disease. Exp Gerontol 2005; 40: 774–783.
Miyamoto M . Characteristics of age-related behavioral changes in senescence-accelerated mouse SAMP8 and SAMP10. Exp Gerontol 1997; 32: 139–148.
Novella S, Dantas AP, Segarra G, Novensa L, Heras M, Hermenegildo C, Medina P . Aging enhances contraction to thromboxane A2 in aorta from female senescence-accelerated mice. Age (Dordr) 2013; 35: 117–128.
Fenton M, Huang HL, Hong Y, Hawe E, Kurz DJ, Erusalimsky JD . Early atherogenesis in senescence-accelerated mice. Exp Gerontol 2004; 39: 115–122.
Lloréns S, de Mera RM, Pascual A, Prieto-Martín A, Mendizábal Y, de Cabo C, Nava E, Jordán J . The senescence-accelerated mouse (SAM-P8) as a model for the study of vascular functional alterations during aging. Biogerontology 2007; 8: 663–672.
Novella S, Dantas AP, Segarra G, Novensà L, Bueno C, Heras M, Hermenegildo C, Medina P . Gathering of aging and estrogen withdrawal in vascular dysfunction of senescent accelerated mice. Exp Gerontol 2010; 45: 868–874.
Greenstein AS, Khavandi K, Withers SB, Sonoyama K, Clancy O, Jeziorska M, Laing I, Yates AP, Pemberton PW, Malik RA, Heagerty AM . Local inflammation and hypoxia abolish the protective anticontractile properties of perivascular fat in obese patients. Circulation 2009; 119: 1661–1670.
Ahima RS . Adipose tissue as an endocrine organ. Obesity 2006; 14:: 242S–249S.
Guerre-Millo M . Adipose tissue hormones. J Endocrinol Invest 2002; 25: 855–861.
Lohn M, Dubrovska G, Lauterbach B, Luft FC, Gollasch M, Sharma AM . Periadventitial fat releases a vascular relaxing factor. FASEB J 2002; 16: 1057–1063.
Dubrovska G, Verlohren S, Luft FC, Gollasch M . Mechanisms of ADRF release from rat aortic adventitial adipose tissue. Am J Physiol 2003; 286: H1107–H1113.
Verlohren S, Dubrovska G, Tsang SY, Essin K, Luft FC, Huang Y, Gollasch M . Visceral periadventitial adipose tissue regulates arterial tone of mesenteric arteries. Hypertension 2004; 44: 271–276.
Gao YJ, Lu C, Su LY, Sharma AM, Lee RMKW . Modulation of vascular function by perivascular adipose tissue: the role of endothelium and hydrogen peroxide. Br J Pharmacol 2007; 151: 323–331.
Withers SB, Agabiti Rosei C, Livingstone DM, Little MC, Aslam R, Malik RA, Heagerty AM . Studies in CD11b-DTR macrophage deficient mice prove that macrophage activation is responsible for the loss of anticontractile function in inflamed perivascular adipose tissue. Arterioscler Thromb Vascular Biol 2011; 31: 908–913.
Wang B, Wood IS, Trayhurn P . Dysregulation of the expression and secretion of inflammation-related adipokines by hypoxia in human adipocytes. Pflugers Arch 2007; 455: 479–492.
Pagé EL, Robitaille GA, Pouysségur J, Richard DE . Induction of hypoxia-inducible factor-1α by transcriptional and translational mechanisms. J Biol Chem 2002; 277: 48403–48409.
Aghamohammadzadeh R, Heagerty AM . Obesity-related hypertension: epidemiology, pathophysiology, treatments, and the contribution of perivascular adipose tissue. Ann Med 2012; 44 (Suppl 1): S74–S84.
Agabiti-Rosei C, De Ciuceis C, Rossini C, Porteri E, Rodella LF, Withers SB, Heagerty AM, Favero G, Agabiti-Rosei E, Rizzoni D, Rezzani R . Anticontractile activity of perivascular fat in obese mice and the effect of long-term treatment with melatonin. J Hypertens 2014; 32: 1264–1274.
Liu R, Pulliam DA, Liu Y, Salmon AB . Dynamic differences in oxidative stress and the regulation of metabolism with age in visceral versus subcutaneous adipose. Redox Biol 2015; 6: 401–408.
Findeisen HM, Pearson KJ, Gizard F, Zhao Y, Qing H, Jones KL, Cohn D, Heywood EB, de Cabo R, Bruemmer D . Oxidative stress accumulates in adipose tissue during aging and inhibits adipogenesis. PLoS ONE 2011; 6: e18532.
Zhang Y, Fischer KE, Soto V, Liu Y, Sosnowska D, Richardson A, Salmon AB . Obesity-induced oxidative stress, accelerated functional decline with age and increased mortality in mice. Arch Biochem Biophys 2015; 576: 39–48.
Kuk JL, Lee S, Heymsfield SB, Ross R . Waist circumference and abdominal adipose tissue distribution: influence of age and sex. Am J Clin Nutr 2005; 81: 1330–1334.
Kuk JL, Saunders TJ, Davidson LE, Ross R . Age-related changes in total and regional fat distribution. Ageing Res Rev 2009; 8: 339–348.
Pararasa C, Bailey CJ, Griffiths HR . Ageing, adipose tissue, fatty acids and inflammation. Biogerontology 2015; 16: 235–248.
Goldman BD . Mammalian photoperiodic system: formal properties and neuroendocrine mechanisms of photoperiodic time measurement. J Biol Rhythms 2001; 16: 283–301.
Johnston JD, Skene DJ . Regulation of mammalian neuroendocrine physiology and rhythms by melatonin. J Endocrinol 2015; 226: T187–T198.
Claustrat B, Leston J . Melatonin: physiological effects in humans. Neurochirurgie 2015; 61: 77–84.
Favero G, Rodella LF, Reiter RJ, Rezzani R . Melatonin and its atheroprotective effects: a review. Mol Cell Endocrinol 2014; 382: 926–937.
Reiter RJ, Tan DX, Paredes SD, Fuentes-Broto L . Beneficial effects of melatonin in cardiovascular disease. Ann Med 2010; 42: 276–285.
Acuña-Castroviejo D, Escames G, Venegas C, Díaz-Casado ME, Lima-Cabello E, López LC, Rosales-Corral S, Tan DX, Reiter RJ . Extrapineal melatonin: sources, regulation, and potential functions. Cell Mol Life Sci 2014; 71: 2997–3025.
Ferreira DS, Amaral FG, Mesquita CC, Barbosa AP, Lellis-Santos C, Turati AO, Santos LR, Sollon CS, Gomes PR, Faria JA, Cipolla-Neto J, Bordin S, Anhê GF . Maternal melatonin programs the daily pattern of energy metabolism in adult offspring. PLoS ONE 2012; 7: e38795.
Reiter RJ, Tan DX, Fuentes-Broto L . Melatonin: a multitasking molecule. Prog Brain Res 2010; 181: 127–151.
Hardeland R, Cardinali DP, Srinivasan V, Spence DW, Brown GM, Pandi-Perumal SR . Melatonin–a pleiotropic, orchestrating regulator molecule. Prog Neurobiol 2011; 93: 350–384.
Mendes C, Lopes AM, do Amaral FG, Peliciari-Garcia RA, Turati Ade O, Hirabara SM, Scialfa Falcão JH, Cipolla-Neto J . Adaptations of the aging animal to exercise: role of daily supplementation with melatonin. J Pineal Res 2013; 55: 229–239.
Rezzani R, Porteri E, De Ciuceis C, Bonomini F, Rodella LF, Paiardi S, Boari GE, Platto C, Pilu A, Avanzi D, Rizzoni D, Agabiti Rosei E . Effects of melatonin and Pycnogenol on small artery structure and function in spontaneously hypertensive rats. Hypertension 2010; 55: 1373–1380.
Hardeland R . Melatonin in aging and disease - multiple consequences of reduced secretion, options and limits of treatment. Aging Dis 2012; 3: 194–225.
Karasek M . Melatonin, human aging, and age-related diseases. Exp Gerontol 2004; 39: 1723–1729.
Obayashi K, Saeki K, Tone N, Kurumatani N . Relationship between melatonin secretion and nighttime blood pressure in elderly individuals with and without antihypertensive treatment: a cross-sectional study of the HEIJO-KYO cohort. Hypertens Res 2014; 37: 908–913.
Favero G, Lonati C, Giugno L, Castrezzati S, Rodella LF, Rezzani R . Obesity-related dysfunction of the aorta and prevention by melatonin treatment in ob/ob mice. Acta Histochem 2013; 115: 783–788.
Rodríguez MI, Carretero M, Escames G, López LC, Maldonado MD, Tan DX, Reiter RJ, Acuña-Castroviejo D . Chronic melatonin treatment prevents age-dependent cardiac mitochondrial dysfunction in senescence-accelerated mice. Free Radic Res 2007; 41: 15–24.
Forman K, Vara E, García C, Kireev R, Cuesta S, Acuña-Castroviejo D, Tresguerres JA . Beneficial effects of melatonin on cardiological alterations in a murine model of accelerated aging. J Pineal Res 2010; 49: 312–320.
Forman K, Vara E, García C, Kireev R, Cuesta S, Escames G, Tresguerres JA . Effect of a combined treatment with growth hormone and melatonin in the cardiological aging on male SAMP8 mice. J Gerontol A Biol Sci Med Sci 2011; 66: 823–834.
Ketonen J, Shi J, Martonen E, Mervaala E . Periadventitial adipose tissue promotes endothelial dysfunction via oxidative stress in diet-induced obese C57Bl/6 mice. Circ J 2010; 74: 1479–1487.
Stacchiotti A, Favero G, Giugno L, Lavazza A, Reiter RJ, Rodella LF, Rezzani R . Mitochondrial and metabolic dysfunction in renal convoluted tubules of obese mice: protective role of melatonin. PLoS ONE 2014; 9: e111141.
Aalkjaer C, Heagerty AM, Petersen KK, Swales JD, Mulvany MJ . Evidence for increased media thickness, increased neural amine uptake, and depressed excitation-contraction coupling in isolated resistance vessels from essential hypertensives. Circ Res 1987; 61: 181–186.
Mulvany MJ, Hansen PK, Aalkjaer C . Direct evidence that the greater contractility of resistance vessels in spontaneously hypertensive rats is associated with a narrowed lumen, a thickened media, and an increased number of smooth muscle cell layers. Circ Res 1978; 43: 854–864.
Rizzoni D, Porteri E, Guelfi D, Muiesan ML, Valentini U, Cimino A, Girelli A, Rodella L, Bianchi R, Sleiman I, Agabiti Rosei E . Structural alterations in subcutaneous small arteries of normotensive and hypertensive patients with not insulin dependent diabetes mellitus. Circulation 2001; 103: 1238–1244.
Rizzoni D, Porteri E, Castellano M, Bettoni G, Muiesan ML, Muiesan P, Giulini SM, Agabiti-Rosei E . Vascular hypertrophy and remodeling in secondary hypertension. Hypertension 1996; 28: 785–790.
Mulvany MJ, Halpern W . Contractile properties of small arterial resistance vessels in spontaneously hypertensive and normotensive rats. Circ Res 1977; 41: 19–26.
Koziróg M, Poliwczak AR, Duchnowicz P, Koter-Michalak M, Sikora J, Broncel M . Melatonin treatment improves blood pressure, lipid profile, and parameters of oxidative stress in patients with metabolic syndrome. J Pineal Res 2011; 50: 261–266.
Bonnefont-Rousselot D, Collin F, Jore D, Gardès-Albert M . Reaction mechanism of melatonin oxidation by reactive oxygen species in vitro. J Pineal Res 2011; 50: 328–335.
Radogna F, Diederich M, Ghibelli L . Melatonin: a pleiotropic molecule regulating inflammation. Biochem Pharmacol 2010; 80: 1844–1852.
Geller DA, Lowenstein CJ, Shapiro RA, Nussler AK, Di Silvio M, Wang SC, Nakayama DK, Simmons RL, Snyder SH, Billiar TR . Molecular cloning and expression of inducible nitric oxide synthase from human hepatocytes. Proc Natl Acad Sci USA 1993; 90: 3491–3495.
Knowles RG, Moncada S . Nitric oxide synthases in mammals. Biochem J 1994; 298: 249–258.
Mitchell JA, Akarasereenont P, Thiemermann C, Flower RJ, Vane JR . Selectivity of nonsteroidal antiinflammatory drugs as inhibitors of constitutive and inducible cyclooxygenase. Proc Natl Acad Sci USA 1993; 90: 11693–11697.
Favero G, Franceschetti L, Rodella LF, Rezzani R . Sirtuins, aging, and cardiovascular risks. Age (Dordr) 2015; 37: 9804.
Ota H, Eto M, Ogawa S, Iijima K, Akishita M, Ouchi Y . SIRT1/eNOS axis as a potential target against vascular senescence, dysfunction and atherosclerosis. J Atheroscler Thromb 2010; 17: 431–435.
Al-Magableh MR, Kemp-Harper BK, Hart JL . Hydrogen sulfide treatment reduces blood pressure and oxidative stress in angiotensin II-induced hypertensive mice. Hypertens Res 2015; 38: 13–20.
Kato T, Umeda A, Miyagawa K, Takeda H, Adachi T, Toyoda S, Taguchi I, Inoue T, Node K . Varenicline-assisted smoking cessation decreases oxidative stress and restores endothelial function. Hypertens Res 2014; 37: 655–658.
Suzuki J, Shimamura M, Suda H, Wakayama K, Kumagai H, Ikeda Y, Akazawa H, Isobe M, Komuro I, Morishita R . Current therapies and investigational drugs for peripheral arterial disease. Hypertens Res 2016; 39: 183–191.
Nakashima T, Umemoto S, Yoshimura K, Matsuda S, Itoh S, Murata T, Fukai T, Matsuzaki M . TLR4 is a critical regulator of angiotensin II-induced vascular remodeling: the roles of extracellular SOD and NADPH oxidase. Hypertens Res 2015; 38: 649–655.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Agabiti-Rosei, C., Favero, G., De Ciuceis, C. et al. Effect of long-term treatment with melatonin on vascular markers of oxidative stress/inflammation and on the anticontractile activity of perivascular fat in aging mice. Hypertens Res 40, 41–50 (2017). https://doi.org/10.1038/hr.2016.103
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2016.103
- Springer Nature Singapore Pte Ltd.
This article is cited by
-
The evolving functions of the vasculature in regulating adipose tissue biology in health and obesity
Nature Reviews Endocrinology (2023)
-
Possible benefits of exogenous melatonin for individuals on dialysis: a narrative review on potential mechanisms and clinical implications
Naunyn-Schmiedeberg's Archives of Pharmacology (2021)
-
Expression of Melatonin Receptor 1 in Rat Mesenteric Artery and Perivascular Adipose Tissue and Vasoactive Action of Melatonin
Cellular and Molecular Neurobiology (2021)
-
Perivascular adipose tissue dysfunction aggravates adventitial remodeling in obese mini pigs via NLRP3 inflammasome/IL-1 signaling pathway
Acta Pharmacologica Sinica (2019)
-
Association between epicardial adipose tissue thickness and parameters of target organ damage in patients undergoing coronary angiography
Hypertension Research (2019)