Abstract
Background/Objectives:
The objective of this disease was to determine the prevalence of malnutrition in children with congenital heart disease (CHD).
Subjects/Methods:
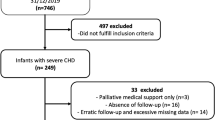
A total of 125 children with CHD, under 6 months of age, were divided into four groups: no pulmonary hypertension (PH) or cyanosis (group 1, n=47), isolated cyanosis (group 2, n=52), isolated PH (group 3, n=16), and PH and cyanosis (group 4, n=10). Six children died at 6 months (n=4), 12 months (n=1) and 19 months (n=1). The remaining children were followed-up for 24 months. Prevalence of moderate to severe malnutrition (weight/weight for height <80%), caloric intake and medications were compared between the four groups.
Results:
Moderate or severe malnutrition was more frequent in group 4 (100%) compared with others groups (group 1, 20%; group 2, 16.7% and group 3, 50%; P<0.05). Low oral caloric intake was more frequent in group 3 (71.4%) and group 4 (75%) than in group 1 (28%) and 2 (28.6%) (P<0.05). Food enrichment was practised in half of the children of group 4 and rarely in other groups (group 1, 15.8%; group 2, 8.6% and group 3, 11.1%; P<0.05). Enteral feeding was used more often in groups 3 (33.3%) and 4 (50%) than in groups 1 (15.8%) or 2 (14.3%; P<0.05).
Conclusions:
Moderate or severe malnutrition is present in 15% of children with CHD, and it is more frequent in case of PH. Half of these children demonstrate low caloric intake, whereas few have proper nutritional support.




Similar content being viewed by others
References
Hoffman JI, Kaplan S . The incidence of congenital heart disease. J Am Coll Cardiol 2002; 39: 1890–1900.
Salzer HR, Haschke F, Wimmer M, Heil M, Schilling R . Growth and nutritional intake of infants with congenital heart disease. Pediatr Cardiol 1989; 10: 17–23.
Da Silva VM, de Oliveira Lopes MV, de Araujo TL . Growth and nutritional status of children with congenital heart disease. J Cardiovasc Nurs 2007; 22: 390–396.
Barton JS, Hindmarsh PC, Scrimgeour CM, Rennie MJ, Preece MA . Energy expenditure in congenital heart disease. Arch Dis Child 1994; 70: 5–9.
Sy K, Dipchand A, Atenafu E, Chait P, Bannister L, Temple M et al. Safety and effectiveness of radiologic percutaneous gastrostomy and gastro jejunostomy in children with cardiac disease. Am J Roentgenol 2008; 191: 1169–1174.
Krieger I . Growth failure and congenital heart disease. Am J Dis Child 1970; 120: 497–502.
Kogon BE, Ramaswamy V, Todd K, Plattner C, Kirshbom PM, Kanter KR et al. Feeding difficulty in newborns following congenital heart surgery. Congenit Heart Dis 2007; 2: 332–337.
Nydegger A, Bines JE . Energy metabolism in infants with congenital heart disease. Nutrition 2006; 22: 697–704.
Forchielli ML, McColl R, Walker WA, Lo C . Children with congenital heart disease: a nutrition challenge. Nutr Rev 1994; 52: 348–353.
Varan B, Tokel K, Yilmaz G . Malnutrition and growth failure in cyanotic and acyanotic congenital heart disease with and without pulmonary hypertension. Arch Dis Child 1999; 81: 49–52.
Cribbs RK, Heiss KF, Clabby ML, Wulkan ML . Gastric fundoplication is effective in promoting weight gain in children with severe congenital heart defects. J Pediatr Surg 2008; 43: 283–289.
Steltzer M, Rudd N, Pick B . Nutrition care for newborns with congenital heart disease. Clin Perinatol 2005; 32: 1017–1030.
Jadcherla SR, Vijayapal AS, Leuthner S . Feeding abilities in neonates with congenital heart disease: a retrospective study. J Perinatol 2009; 29: 112–118.
Vaidyanathan B, Nair SB, Sundaram KR, Babu UK, Shivaprakasha K, Rao SG et al. Malnutrition in children with congenital heart disease (CHD) determinants and short term impact of corrective intervention. Indian Pediatr 2008; 45: 541–546.
Sempe M, Pedron G, Roy-Pernot MP . Auxologie Méthode et Séquences. Théraplix: Paris, 1979.
Martin A . Apports Nutritionnels Conseillés Pour la Population Française, 3rd edn, vol. 1, Tec and Doc: Paris, 2001, p 604.
Ratanachu-Ek S, Pongdara A . Nutritional status of pediatric patients with congenital heart disease: pre-and post-cardiac surgery. J Med Assoc Thai 2011; 94: S133–S137.
Tokel K, Azak E, Ayabakan C, Varan B, Aşlamaci SA, Mercan S . Somatic growth after corrective surgery for congenital heart disease. Turk J Pediatr 2010; 52: 58–67.
Waterlow JC . Classification and definition of protein-calorie malnutrition. Br Med J 1972; 3: 566–569.
Vieira TC, Trigo M, Alonso RR, Ribeiro RH, Cardoso MR, Cardoso AC et al. Assessment of food intake in infants between 0 and 24 months with congenital heart disease. Arq Bras Cardiol 2007; 89: 219–224.
Medoff-Cooper B, Naim M, Torowicz D, Mott A . Feeding, growth, and nutrition in children with congenitally malformed hearts. Cardiol Young 2010; 20: 149–153.
Weintraub RG, Menahem S . Early surgical closure of a large ventricular septal defect: influence on long term growth. J Am Coll Cardiol 1991; 18: 552–558.
Cheung MM, Davis AM, Wilkinson JL, Weintraub RG . Long term somatic growth after repair of tetralogy of Fallot: evidence for restoration of genetic growth potential. Heart 2003; 89: 1340–1343.
Rhee EK, Evangelista JK, Nigrin DJ, Erickson LC . Impact of anatomic closure on somatic growth among small asymptomatic children with secundum atrial septal defect. Am J Cardiol 2000; 85: 1472–1475.
Unger R, DeKleermaeker M, Gidding SS, Christoffel KK . Calories count. Improved weight gain with dietary intervention in congenital heart disease. Am J Dis Child 1992; 146: 1078–1084.
Surmeli-Onay O, Cindik N, Kinik ST, Ozkan S, Bayraktar N, Tokel K . The effect of corrective surgery on serum IGF-1 and IGFBP-3 levels and growth in children with congenital heart disease. J Pediatr Endocrinol Metab 2011; 24: 483–487.
Chima CS, Barco K, Dewitt ML, Maeda M, Teran JC, Mullen KD . Relationship of nutritional status to length of stay, hospital costs, and discharge status of patients hospitalized in the medicine service. J Am Diet Assoc 1997; 97: 975–978.
Naber TH, Schermer T, de Bree A, Nusteling K, Eggink L, Kruimel JW et al. Prevalence of malnutrition in nonsurgical hospitalized patients and its association with disease complications. Am J Clin Nutr 1997; 66: 1232–1239.
Martyn CN, Winter PD, Coles SJ, Edington J . Effect of nutritional status on use of health care resources by patients with chronic disease living in the community. Clin Nutr 1998; 17: 119–123.
St Pierre A, Khattra P, Johnson M, Cender L, Manzano S, Holsti L . Content validation of the infant malnutrition and feeding checklist for congenital heart disease: a tool to identify risk of malnutrition and feeding difficulties in infants with congenital heart disease. J Pediatr Nurs 2010; 25: 367–374.
Jackson M, Poskitt EM . The effects of high-energy feeding on energy balance and growth in infants with congenital heart disease and failure to thrive. Br J Nutr 1991; 65: 131–143.
Schwarz SM, Gewitz MH, See CC, Berezin S, Glassman MS, Medow CM et al. Enteral nutrition in infants with congenital heart disease and growth failure. Pediatrics 1990; 86: 368–373.
Ciotti G, Holzer R, Pozzi M, Dalzell M . Nutritional support via percutaneous endoscopic gastrostomy in children with cardiac disease experiencing difficulties with feeding. Cardiol Young 2002; 12: 537–541.
Hofner G, Behrens R, Koch A, Singer H, Hofbeck M . Enteral nutrition support by percutaneous endoscopic gastrostomy in children with congenital heart disease. Pediatr Cardiol 2000; 21: 341–346.
Acknowledgements
The first draft was written by TL. No honorarium or grant has been received by any of the authors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Blasquez, A., Clouzeau, H., Fayon, M. et al. Evaluation of nutritional status and support in children with congenital heart disease. Eur J Clin Nutr 70, 528–531 (2016). https://doi.org/10.1038/ejcn.2015.209
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2015.209
- Springer Nature Limited
This article is cited by
-
Decreased lipid levels in adult with congenital heart disease: a systematic review and Meta-analysis
BMC Cardiovascular Disorders (2023)
-
Enteral access and reflux management in neonates with severe univentricular congenital heart disease: literature review and proposed algorithm
European Journal of Pediatrics (2023)
-
Reliability and validity of the FFQ and feeding index for 7-to 24-month-old children after congenital heart disease surgery
BMC Pediatrics (2022)
-
Effect of feeding with standard or higher-density formulas on anthropometric measures in children with congenital heart defects after corrective surgery: a randomized clinical trial
European Journal of Clinical Nutrition (2022)
-
Prevalence and Associated Factors of Long-term Growth Failure in Infants with Congenital Heart Disease Who Underwent Cardiac Surgery Before the Age of One
Pediatric Cardiology (2022)